Key Points
-
Highlights the principles of mouth stick design, including patient selection and treatment planning considerations.
-
Presents two recent clinical cases where mouth sticks have been indicated, detailing the clinical and laboratory stages involved.
-
Discusses the future of mouth sticks, in particular, the influence of technological advances on mouth stick design.
Abstract
Patients with physical disabilities precluding functional use of their limbs can benefit enormously from the expertise of the dental profession. The dental clinician is able to not only meet the routine oral health needs of these patients, but possesses the unique skills and knowledge to provide specialised oral prosthetic appliances which can facilitate a range of independent activities. Mouth sticks, as they are commonly known, are dental prostheses that are held intra-orally by the patient and manipulated to perform numerous actions such as drawing, writing and painting. They have been well documented within dental and occupational therapy literature and reports of their fabrication date back over 150 years, albeit in a very rudimentary form. The enduring value of mouth sticks to the physically disabled population is that they can provide a degree of self-reliance which would otherwise not be afforded to them. This article discusses the evolution of mouth sticks, principles of mouth stick design, patient selection criteria and treatment planning considerations. We present two recent clinical cases where mouth sticks have been indicated and have been indispensable to the user, detailing the clinical and laboratory stages involved.
Similar content being viewed by others
Introduction
The dental profession has a long-standing history of providing tailored oral healthcare for patients with physical disabilities. One of the more ingenious and inventive aspects of this specialised care has involved fabricating oral prostheses which aid activities of daily living. Injuries to the spinal cord or certain debilitating systemic conditions such as cerebral palsy or poliomyelitis may leave the head and neck regions as the only neurologically intact parts of the body.1 Likewise congenital abnormalities or trauma of the limbs can render the individual restricted in their range of movements. In such cases where limb function is either absent or minimal, muscles of the head, neck, face, jaws and tongue can be used to compensate.2 A prosthetic mouth-held appliance, which can use these muscle groups, may therefore be valuable for such patients.
The mouth-held appliance, bite stick, mouth-operated device or mouth stick, as it is commonly known, essentially comprises three basic connected components: an intra-oral mouthpiece, a rod and a functional tip. When used by patients with dysfunctional limb capabilities, they can provide the means to perform multiple practical tasks such as writing, drawing, turning pages of a book and grasping objects. In this way these prostheses can foster a sense of independence and self-sufficiency in those with physical disabilities and may be instrumental in assisting their rehabilitation.
The evolution of mouth sticks
The early mouth stick
Mouth sticks for those with physical disabilities have been well reported within dental literature. Frankel et al.3 cited one of the earliest references to such a prosthesis from a text by Dampier in 1875.4 Dampier described a Mr John Carter, who had sustained quadriplegia following an alcohol-induced fall from a tree, and his subsequent rehabilitation using a simple mouth stick to facilitate his desire to paint.4 Many of the first mouth sticks, such as this, involved a rigid rod to which a simple occlusal bite plane was formed at one end and a writing or similar implement was attached at the other end. Since then mouth sticks have undergone much modification and adaptation over the years, in both their design and material composition.
Mouthpiece design and material
The earliest appliances, as outlined by Dampier in 1874, were maintained in position by the patient simply occluding on to the mouthpiece.5,6 As one can imagine, and as Frankel et al.3 stated, such appliances required a great deal of muscular effort and left the patient unable to eat or talk during its use. Thus a natural progression of the mouth stick led to custom-made, close-fitting intra-oral components. Design variations of the mouthpiece component are numerous and initially these were adapted to only cover the anterior teeth and lips.7,8 As expected this design was short lived given their propensity to cause posterior overeruption of the uncovered molar teeth and reduced stability.1,9,10,11,12,13 Thereafter mouthpieces were designed to make use of the entire arch and well documented designs include: splints covering occlusal and incisal aspects of maxillary and mandibular teeth (similar to the appearance of interocclusal records);1,14,15,16 splints covering the palatal aspects of the maxillary teeth and hard palate;13 splints covering occlusal, palatal, incisal aspects and a small overlap of the buccal surfaces of maxillary teeth (resembling diagnostic splints);17 splints covering the occlusal and incisal surfaces of both maxillary and mandibular teeth with an overlap of buccal surfaces in both arches;11,18,19,20 unique splints which only covered the palate and gingivae with no tooth coverage;21 and, lastly, full coverage maxillary or mandibular splints (akin to mouthguards).2,3,22,23 Where appropriate, patients' existing dentures have also been adapted to form the intra-oral component of mouth sticks.24 Use of these customised, self-retaining mouthpieces improved retention and stability of the mouth stick and reduced patient fatigue.
The mouthpiece material itself has likewise developed over time. Latex and silicone have been used to fabricate mouthpieces and additionally used as soft liners within mouthpieces. However, these have been observed to absorb odours and staining,17 leading to the preferential use of self-curing or heat cured acrylic resin.1,8,12,13,14,17,18,20,22,25,26 Case reports have also documented the use of thermoplastic material used for mouthguards,2,19 and, more recently polyvinyl acetate-polyethylene copolymer (PVAC.PE) has been utilised.9 The majority of mouthpieces described are invariably reinforced with either a metal base plate or mesh work.13,17,20,22,27
Functional tip design and material
Concurrent to developments in the mouthpiece design were advances in the functional capability of mouth sticks. A logical evolution for the mouth stick was to incorporate the feature of holding a number of different interchangeable tips to increase its 'multifunctionality'. Many have used the design of having a female receptacle at the end of the rod to which a number of different implements such as a pen, pencil or rubber stop can be attached, once modified with the corresponding male counterpart.1,18,22 The mechanism of attachment may be snap-lock/friction-grip1,14,19,24 or magnetic.22 Other systems have used screw mechanisms at the rod end to hold various implements;20 however, these require an assistant when changing tips, limiting the degree of independence they can provide. Regardless of the mechanism of attachment, the ability to change functional tips extends the range of the users' activities considerably to include writing, drawing, painting, typewriting, using push buttons, hooking objects and turning the pages of a book.
Rod design and material
The rod components of mouth sticks were initially a rigid design and fabricated from a variety of materials such as wood,8 aluminium,3,17,28 acrylic,1,2 plastic6, stainless steel,22 Lucite13,28 and fibreglass.18 Rod design has consisted of a horizontal straight body,2,3,5,6,8,13,16,18,24,27,28 a straight downward incline1,25 or those with a principally straight horizontal body and an angled distal tip pointed towards the floor14,17,22 Literature suggests an obtuse angle of 130 degrees17,22 applied to the rod will provide the patient with a user-friendly appliance. The length of the rod is normally adjusted for the preference of the patient with particular attention to their visual acuity.1,17 The average reported length of rigid rods are between 25–50cm.2,17,29
Dynamic and advanced mouth sticks
The period from the 1960s to the 1980s saw an outburst of imaginative and sophisticated technology employed within mouth stick manufacture and heralded the so-called dynamic mouth sticks. This marked a significant evolution in the design and function of mouth sticks. Dynamic mouth sticks have been indicated for those with high-level quadriplegia where there is an absence of functional neck muscles or lack of sufficient neck musculature, precluding the use of the aforementioned static mouth sticks with a fixed length.7,9,15 These mouth sticks conform to the same basic component design as the previously described static mouth sticks, but each of the three parts may incorporate a movable feature extending the range of activities it can perform.9 These appliances often have a telescopic/projecting feature built into the rod to give the ability to extend and reduce the length of the mouth stick as required.7,15,19,22,25,26,30 Adjustment of the length can be achieved by protrusion of the tongue onto a button or groove within the mouthpiece, which in turn is connected to a mechanism within the telescopic rod causing extension7,15 More simple dynamic mouthpieces have employed a telescopic shaft that is adjusted in length by another individual and then fixed in place using a set screw,22 or incorporate a projecting strut on the telescopic rod shaft which can be pulled or pushed against a stationary object by the patient to adjust the length.19
Some clinicians have taken the dynamic mouth stick one step further. O'Donnel et al.26 amalgamated a ball and socket joint together with a rack and pinion mechanism within the intra-oral mouthpiece. When this inventive device was manipulated by the tongue and by retrusive and protrusive movements of the mandible, it allowed for controlled vertical and lateral movements of the mouth stick.26 Beder23 likewise used vertical excursions of the mandible to increase the range of movements achievable by mouth sticks; his design used mandibular forces to control a grasping motion at the tip via two spring-loaded 'fingers'. This appliance was purported to afford the user grasping and lifting capabilities. Similarly, devices which use protrusive/retrusive movements of the mandible to control 'fingerlike' extensions at the functional tip to perform grasping actions, have also been fabricated.31,32 Stow's29 comparable design incorporated a design whereby occlusal biting forces directed onto the mouthpiece component closed and opened a 'pincer foot' functional tip.
Battery-operated mouth sticks
The static and dynamic mouthpieces described so far may broadly be considered mechanical devices. Battery-operated or electric devices have also been designed.30 Their principle mechanism involves incorporating buttons into the mouthpiece which, when depressed by the tongue, activates an electrically operated control box built into the mouth stick resulting in a telescoping action. Their use has not been widespread and it has been reported this was likely because their utilisation depends on a supply of current (via recharging the battery pack), and also due to their delicate and complicated operation, which makes them more liable to malfunction.17
Review of historical mouth stick designs
The assortment of designs related to mouth stick construction have been previously reviewed and criticised, with some being described as too crude and 'unifunctional' and others as highly specific and difficult to fabricate.1 However, the diversity of mouth stick design over the years is a likely reflection that a 'one size fits all' is impractical. It is also a reflection of more sophisticated materials and techniques becoming available. This said, despite the design chosen, there are key basic principles which should be considered and adhered to when constructing a mouth stick.
Principles of mouth stick design
Guiding principles regarding mouth-held appliances have been mentioned in many early case reports of mouth sticks. In 1973, requirements for mouth sticks were formalised by Blaine and Nelson13 to address some of the previous issues that had been identified such as over eruption of teeth associated with partial coverage intra-oral mouthpieces, poor retention, lateral instability of the mouthpiece, creation of a gagging sensation due to strain on the muscles of mastication and fatiguing of the patients. A summary of these 14 principles can be seen in Table 1 and serve as a useful reference when designing mouth sticks.
Patient selection and treatment planning considerations for mouth sticks
In addition to the normal considerations which are borne in mind when providing removable prostheses for patients, such as a sound dentition, a healthy and stable periodontal status and adequate neuromuscular control etc, there are some additional areas to consider to ensure the success of the device.
First and foremost, it is important to ascertain what the patient would like to be able to accomplish with their mouth stick. This will determine what sort(s) of functional tip is provided, such as a writing implement, paintbrush or a rubber stub to turn pages, and if a dynamic or static design should be used, if, for example, the patient wishes to grasp or hold objects.
An assessment should be made of the patient's functional capacity. Their physical ability to control head, neck and shoulder muscle groups is important in the selection of the appropriate mouth stick.27 If there were limited ability in using head and neck muscles a dynamic mouth stick would be the more useful choice. Should there be difficulty in assessing or predicting the patient's range of motion, a static mouth stick could always be trialled first. The patient's cognitive ability should also be taken into account. As with any removable prosthesis there is a learning period required before full and comfortable function is attained. With a mouth stick it is likely this accommodation process would be more prolonged and challenging. Ruff27 usefully suggested caregivers may be instrumental in helping to guide the selection process of mouth sticks for patients where there is limited mental capacity. Physiotherapists and occupational therapists, in particular, may be helpful in this regard. These healthcare professionals can offer valuable insight into the personal limitations of the patient and thus aid mouth stick design, as well as be integral in supporting the patient to successfully adapt to these devices once delivered.12,27
Once it has been decided that a mouth stick is indicated, key to its stability will be the state of the patient's existing dentition. Patients who have limited use of their limbs may be more likely to suffer from dental disease due to an impairment of performing thorough at-home cleaning. Thus, a more robust and intensive preventive oral hygiene programme will first need to be in place, compared to the routine prosthodontic patient.
Clinical case study 1
Background
Patient A, 49 years old, sustained quadriplegia as a result of a rugby injury. He is a long time user of mouth sticks and has worn mouth sticks since his late teens to aid both work-related and leisure activities, such as typing on a computer keyboard, using a telephone key pad and reading. His first mouth sticks were designed such that the intra-oral acrylic mouthpieces were not self-retentive and required occlusal pressure to be maintained in place, similar to the designs of the very early documented intra-oral mouthpieces. As can be seen in Figure 1 these were constructed of an acrylic mouthpiece, aluminium rod and a rubber tip.
Presenting complaint
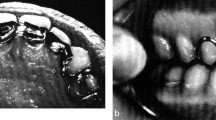
Patient A's presenting complaint was that his existing mouth stick kept breaking, with the area of weakness manifesting as fracture at the join between the mouthpiece and the rod component (Fig. 2). His existing mouth stick incorporated the design of a lower occlusal mouthguard as the mouthpiece, made of Molloplast B, with a cobalt-chrome backing (Fig. 2). The rod aluminium portion (not shown) was simply soldered onto the mouthpiece and suffered continual fracture.
Clinical examination
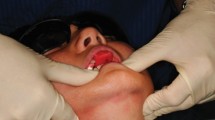
Clinical examination revealed poor oral hygiene with BPE scores of 111/222. The patient has a moderately restored dentition with several cast and direct restorations. Abrasive tooth surface loss of 14 to 24 was observed (Fig. 3) and special investigation revealed these teeth to be positive to vitality testing, in line with control teeth. Extra-orally, the patient displayed full and controlled movement of the head by the neck musculature.
Examination of current and previous mouth stick
Examination of the current mouth stick (Fig. 2) revealed the aluminium rod, which was simply soldered to the mouthpiece, had fractured away. Other design issues show the intra-oral mouthpiece material used was not stain resistant or highly cleansable. Finally, the causative factor of the observed tooth surface loss is undoubtedly the result of the cobalt-chrome backing of the mouthpiece.
The main issues with the patient's historic mouth sticks (Fig. 1) were the intra-oral mouthpiece component which was not self-retentive and led to patient fatigue and they were also prone to fracture as they were made in thin sections. Like the patient's current mouth stick they also had fractured at the joint between the mouthpiece and the rod. It is important to examine the features of failed mouth sticks so that positive features can be incorporated into new designs and unsuccessful features can be actively removed, just as is the case when making removable prostheses for patients who have experienced previous difficulties.
Diagnosis and treatment plan
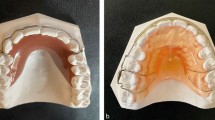
Patient A was diagnosed with gingivitis, abrasive tooth surface loss of anterior maxillary teeth from existing cobalt-chrome mouth stick and a history of failed mouth sticks. The treatment plan advised included oral hygiene instruction, full mouth supraginigival scaling and to design a new optimised static mouth stick. As the patient was happy with the rubber functional tip on his previous mouth sticks, this was to be retained in the new version.
Clinical and laboratory stages of constructing Patient A's mouth stick
See Table 2 and Figures 5 to 18 for a summary of the clinical and laboratory stages used to construct both Patient A's and B's mouth sticks. Minor variations in construction have been included for both cases.
Clinical case study 2
Background
Patient B, 45 years old, was involved in a train accident when he was eight, which resulted in loss of his right arm and limited function in his left hand. He had so far managed to complete all of his daily activities using just his mouth, such as holding utensils, opening packaging and grasping objects, including very heavy items such as his children! The patient had no previous experience of a mouth stick and the mainstay of the dental care he received had been targeted at treating his high caries rate. As a result of his disability the patient had difficulty performing effective at-home plaque control and in combination with a highly cariogenic diet this had resulted in the extraction of a number teeth and their replacement with implants and conventional bridges. He was on a high fluoride regimen and had received intensive oral hygiene instruction and dietary advice, together with being provided with a wall mounted toothbrush to ensure more effective cleaning.
Presenting complaint
Patient B was keen to explore the possibility of having an oral prosthesis which could extend the range of actions he could perform, in particular, to aid his use of a touch screen smart phone and tablet. He was also concerned about finding a solution in order to limit any further damage to his existing dentition.
Clinical examination
Clinical examination revealed poor levels of oral hygiene with BPE scores of 2 in all sextants. The patient has an extensively restored dentition with two implant supported bridges and a single unit implant in the lower arch, and a nine unit fixed-fixed conventional bridge in the upper arch extending from the upper right first molar to the upper left canine and a separate three unit fixed-fixed conventional bridge extending from the upper left second premolar to the upper left second molar (Fig. 4). The extensive amount of metal work seen on Patient B's cast restorations (Fig. 4) had been a deliberate design feature to help facilitate all of his daily activities, which, as mentioned, were accomplished using just his mouth. Extra-orally, Patient B displayed full and controlled movement of the head by the neck musculature.
Diagnosis and treatment plan
The patient was diagnosed with a high caries risk, gingivitis and overuse of his dentition to perform daily activities. The recommended treatment plan was for the patient to continue to receive oral hygiene reinforcement and to trial a static mouth stick prosthesis to help perform daily activities more comfortably. The design of which was to incorporate a stylus functional tip for operation with touch screens.
Clinical and laboratory stages of constructing Patient B's mouth stick
See Table 2 and Figures 5 to 18 for a summary of the clinical and laboratory stages used to construct both Patient A's and B's mouth sticks. Minor variations in construction have been included for both cases.
Patient feedback
Both Patient A and Patient B have reported overwhelming satisfaction with their mouth sticks. For Patient A, a long-time mouth stick user, his new and improved mouth stick has meant he has been able to perform his daily activities more comfortably and efficiently. While for Patient B, his first ever mouth stick has expanded his range of actions enormously and reduced the demands he previously placed on his natural dentition. Patient B has, however, found the weight of his mouth stick to be an issue and would prefer a heavier, more robust feel. We are thus fabricating a second mouth stick, incorporating the use of a weightier stainless steel rod.
Mouth sticks: their future
Mouth sticks have existed, been adapted and sophisticated for over a century now. Such intra-oral prostheses will continue to be useful to our patient population who have congenitally lost functional use of their limbs or acquired such disabilities. Undoubtedly, as materials and techniques develop, mouth sticks will so too develop. External technological advances will also spur on evolutions in mouth stick design. As has been presented with Patient B, the advent of touch screens for smart devices has significantly affected how we interact with the modern world and thus resulted in the novel incorporation of a stylus tip. It should be borne in mind, however, what is key that the design of these devices be dictated by the requirements of the individual and be tailored to fit their needs accordingly.
The success and use of these devices will further be ensured by improved links with other members of the patient's care team, and in particular, their physiotherapists and occupational therapists, as already mentioned. Smith12 noted collaboration between dentists and therapists is especially important in mouth stick provision and training, although rarely seen in clinical practice with both groups showing a limited awareness of each other's skills. Holistic treatment planning is arguably more important for the groups of patient likely to benefit from mouth sticks compared to other patient groups and close liaison with all healthcare professionals involved is no doubt useful.
Conclusion
The fabrication of mouth sticks involves the use of routine prosthodontic skills in combination with uncomplicated laboratory manufacturing processes, effected by excellent communication with skilled dental technicians and auxiliary healthcare professionals. Mouth sticks are thus prosthetic devices which all dental professionals are able and best placed to provide to those in need.16 The satisfaction in this clinical work is in delivering autonomy and self-reliance to the patients who require it the most. This reward alone surely makes provision of dental mouth sticks a worthwhile endeavour for any clinician.
References
Lutwak E . A new mouthstick prosthesis for handicapped patients. J Prosthet Dent 1977; 37: 61–66.
O'Donnell D, Robinson W . A simple self-retaining appliance for physically disabled individuals. Quintessence Int 1988; 19: 63–65.
Frankel M A, Hawkesford, Simonson J. A new pattern mouth stick. Paraplegia 1975; 13: 66–69.
Dampier W J . A memoir of John Carter. London: Simpkin, Marshall & Co, 1875.
Moore J C . Reading aids for a quadriplegic patient. Am J Occup Therap 1956; 10: 119–120.
Bastable A D . Typewriter frame and mouthstick for the quadriplegic with neck involvement. Am J Occup Therap 1956; 10: 7–8.
Mildred E Y . Ejectable mouth stick. Am J Occup Therap 1956; 10: 121.
Sniderman M, Hollis L I . The use of self-curing acrylic in the making of a mouthpiece to aid the upper extremity paralytic patient. Am J Occup Therap 1954; 8: 115–116.
Nunn J H, Wood I . The use of vacuum-molded polyvinyl acetate-polyethylene copolymer (PVAC.PE) for a handicapped patient. Spec Care Dentist 1992; 12: 122–124.
Hemley S . Bite planes, their application and action. Am J Orthod 1938; 24: 721–736.
Buckely R R, Slominski A H . The acrylic mouthpiece. Am J Occup Therap 1958; 12: 23–25.
Smith R . Mouth stick design for the client with spinal cord injury. Am J Occup Therap 1988; 43: 251–254.
Blaine H L, Nelson E P . A mouthstick for quadriplegic patients. J Prosthet Dent 1973; 29: 317–322.
Brown J P, Chapman R P, Mellor C W . Interchangeable mouth-held appliances for the physically handicapped child. J Int Dent Child 1975; 6: 27–28.
Garcia S, Greenfield J . Dynamic protractible mouthstick. Am J Occup Therap 1981; 35: 529–530.
King W C . Mouthstick habilitation. J Am Dent Assoc 1973; 87: 839–842.
Zalkind M, Mitrani A, Stern N . mouth-operated devices for handicapped persons. J Prosthet Dent 1975; 34: 652–658.
Olsen R A, Prentke E M, Olsen D . A versatile and easily fabricated mouthstick. J Prosthet Dent 1986; 55: 247–249.
Kozole K P, Gordon R E, Hurst P S . Modular mouthstick system. J Prosthet Dent 1985; 53: 831–835.
Mulligan R . A physiologic bitestick appliance for quadriplegics. Spec Care Dentist 1983; 3: 24–29.
Yeakel M H, Margetis P M . A new technique for fabricating temporary mouthstick appliances. Am J Occup Therap 1968; 22: 168–173.
Smokler J, Rappaport S C . Mouthstick prosthesis for a patient with arthrogryposis multiplex congenital. J Prosthet Dent 1979; 42: 316–321.
Beder O E . Manipulative appliances for quadriplegics. J Prosthet Dent 1964; 14: 785–788.
Garsud O . Therapeutic dental aid for patient with multiple sclerosis. Br Dent J 1981; 150: 356.
Cloran A J . Telescopic mouth instruments for severely handicapped patients. J Prosthet Dent 1974; 32: 435–438.
O'Donnel D, Yen P K J, Robinson W . A mouth-controlled appliance for severely physically handicapped patients. Br Dent J 1985; 159: 186–188.
Ruff J C . Selection criteria for static and dynamic mouthsticks. Gen Dent 1990: 414–416.
Grisius R J, Firtell D N . Mouth-controlled devices to assist the handicapped. J Hosp Dent Pract 1978; 13: 107–108.
Stow R W . Grasping mouthstick. Arch Phys Med Rehab 1966; 47: 31–33.
Cloran A J, Lotz J W, Campbell H D, Wiechess D O . Oral telescoping orthosis: an aid to functional rehabilitation of quadriplegic patients. J Am Dent Assoc 1980; 100: 876–879.
Donnelly M W, Beder O E . A manipulative appliance. J Prosthet Dent 1972; 28: 309–312.
Georgia Warm Springs Foundation. The pincer mouthstick. Am J Occup Therap 1957; 11: 288–289.
Evans B A, Cooley A M . Writing, typing and painting aids for the respirator patient. Am J Occup Therap 1956; 10: 85–87.
Acknowledgements
The authors would like to sincerely thank Claire Grant, former dental technician at Guy's Dental Hospital, and Andrew Kirk, dental technician at Royal London Dental Hospital, for their dedication to patient care, expert technical skills and photographs and notes on the manufacturing processes of the mouth sticks presented in this paper.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Toor (nee Bachoo), I., Tabiat-Pour, S. & Critchlow, S. Mouth sticks: their past, present and future. Br Dent J 219, 209–215 (2015). https://doi.org/10.1038/sj.bdj.2015.681
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2015.681