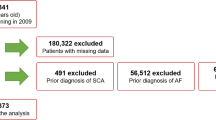
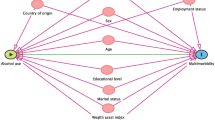
Studying short-term relationships between acute alcohol consumption and discrete atrial fibrillation (AF) episodes has proven difficult given the need for AF assessments shortly after acute and excessive drinking1,2,3,4. Here, we analyzed breathalyzer data and identified eight recurrent and nationally recognized events associated with increased alcohol consumption. Using these events as instrumental variables, we analyzed data from emergency department (ED) visits for AF in California. Using multivariable adjusted Poisson regression models to compare rates of AF and new-onset AF during and 6 d after instrumental variable events compared with all other days of the year, alcohol consumption inferred from these events was associated with a statistically significant increase in ED visits for AF and for new-onset AF. Our data suggest that acute alcohol consumption in the general population is associated with a higher risk of discrete AF episodes as well as for new-onset (incident) AF.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Investigators interested in using OSHPD data can apply at https://oshpd.ca.gov/data-and-reports/request-data. These administrative data are publicly available through the established processes of the OSHPD.
References
Ettinger, P. O. et al. Arrhythmias and the ‘holiday heart’: alcohol-associated cardiac rhythm disorders. Am. Heart J. 95, 555–562 (1978).
Engel, T. R. & Luck, J. C. Effect of whiskey on atrial vulnerability and ‘holiday heart’. J. Am. Coll. Cardiol. 1, 816–818 (1983).
Thornton, J. R. Atrial fibrillation in healthy non-alcoholic people after an alcoholic binge. Lancet 2, 1013–1015 (1984).
Greenspon, A. J. & Schaal, S. F. The ‘holiday heart’: electrophysiologic studies of alcohol effects in alcoholics. Ann. Intern. Med. 98, 135–139 (1983).
Chugh, S. S., Blackshear, J. L., Shen, W. K., Hammill, S. C. & Gersh, B. J. Epidemiology and natural history of atrial fibrillation: clinical implications. J. Am. Coll. Cardiol. 37, 371–378 (2001).
Middeldorp, M. E., Ariyaratnam, J., Lau, D. & Sanders, P. Lifestyle modifications for treatment of atrial fibrillation. Heart 106, 325–332 (2020).
Chung, M. K. et al. Lifestyle and risk factor modification for reduction of atrial fibrillation: a scientific statement from the American Heart Association. Circulation 141, e750–e772 (2020).
Kodama, S. et al. Alcohol consumption and risk of atrial fibrillation: a meta-analysis. J. Am. Coll. Cardiol. 57, 427–436 (2011).
Whitman, I. R. et al. Alcohol abuse and cardiac disease. J. Am. Coll. Cardiol. 69, 13–24 (2017).
Dukes, J. W. et al. Access to alcohol and heart disease among patients in hospital: observational cohort study using differences in alcohol sales laws. BMJ 353, i2714 (2016).
Dixit, S. et al. Past alcohol consumption and incident atrial fibrillation: the Atherosclerosis Risk in Communities (ARIC) Study. PLoS ONE 12, e0185228 (2017).
Voskoboinik, A. et al. Alcohol abstinence in drinkers with atrial fibrillation. N. Engl. J. Med. 382, 20–28 (2020).
Groh, C. A. et al. Patient-reported triggers of paroxysmal atrial fibrillation. Heart Rhythm 16, 996–1002 (2019).
Mandyam, M. C. et al. Alcohol and vagal tone as triggers for paroxysmal atrial fibrillation. Am. J. Cardiol. 110, 364–368 (2012).
Marcus, G. M. et al. A randomized, double-blind, placebo-controlled trial of intravenous alcohol to assess changes in atrial electrophysiology. JACC Clin. Electrophysiol. 7, 662–670 (2021).
Brunner, S. et al. Alcohol consumption, sinus tachycardia, and cardiac arrhythmias at the Munich Octoberfest: results from the Munich Beer Related Electrocardiogram Workup Study (MunichBREW). Eur. Heart J. 38, 2100–2106 (2017).
Adams, J. Consideration of immediate and future consequences, smoking status, and body mass index. Health Psychol. 31, 260–263 (2012).
Hernán, M. A. & Robins, J. M. Instruments for causal inference: an epidemiologist’s dream? Epidemiology 17, 360–372 (2006).
Zhang, Z., Uddin, M. J., Cheng, J. & Huang, T. Instrumental variable analysis in the presence of unmeasured confounding. Ann. Transl. Med. 6, 182 (2018).
Mäkelä, P., Martikainen, P. & Nihtilä, E. Temporal variation in deaths related to alcohol intoxication and drinking. Int. J. Epidemiol. 34, 765–771 (2005).
Poikolainen, K., Leppänen, K. & Vuori, E. Alcohol sales and fatal alcohol poisonings: a time-series analysis. Addiction 97, 1037–1040 (2002).
Dearing, R. L. et al. Super Bowl Sunday: risky business for at-risk (male) drinkers? Subst. Use Misuse 49, 1359–1363 (2014).
Patrick, M. E. & Azar, B. High-intensity drinking. Alcohol Res. 39, 49–55 (2018).
Syed-Abdul, M. M. et al. The Tailgate Study: differing metabolic effects of a bout of excessive eating and drinking. Alcohol 90, 45–55 (2021).
Neal, D. J. & Fromme, K. Hook ‘em horns and heavy drinking: alcohol use and collegiate sports. Addict. Behav. 32, 2681–2693 (2007).
Christensen, M. A. et al. Sleep characteristics that predict atrial fibrillation. Heart Rhythm 15, 1289–1295 (2018).
Genuardi, M. V. et al. Association of short sleep duration and atrial fibrillation. Chest 156, 544–552 (2019).
Hsieh, C. G. & Martin, J. L. Short sleep, insomnia, and cardiovascular disease. Curr. Sleep Med. Rep. 5, 234–242 (2019).
Wuopio, J., Orho-Melander, M., Ärnlöv, J. & Nowak, C. Estimated salt intake and risk of atrial fibrillation in a prospective community-based cohort. J. Intern. Med. 289, 700–708 (2020).
Pääkkö, T. J. W. et al. Dietary sodium intake is associated with long-term risk of new-onset atrial fibrillation. Ann. Med. 50, 694–703 (2018).
Aschbacher K. et al. Machine learning prediction of blood alcohol concentration: a digital signature of smart-breathalyzer behavior. NPG Digit. Med. 4, 74 (2021).
Riordan, B. C. et al. The accuracy and promise of personal breathalysers for research: steps toward a cost-effective reliable measure of alcohol intoxication? Digit. Health 3, 2055207617746752 (2017).
Author information
Authors and Affiliations
Contributions
S.A., C.A.G., C.D.F. and G.M.M. conceived and designed the study. S.A., E.V., G.N. and G.M.M. performed data analysis and statistical analysis. S.A. and G.M.M. wrote the first manuscript draft. Critical revision, editing and approval of the final manuscript was carried out by all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review information
Nature Cardiovascular Research thanks Abhishek Deshmukh, Ben Freedman and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Supplementary information
Source data
Source Data Fig. 1
Statistical source data for Fig. 1.
Rights and permissions
About this article
Cite this article
Aung, S., Nah, G., Vittinghoff, E. et al. Population-level analyses of alcohol consumption as a predictor of acute atrial fibrillation episodes. Nat Cardiovasc Res 1, 23–27 (2022). https://doi.org/10.1038/s44161-021-00003-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s44161-021-00003-7
This article is cited by
-
Changes in alcohol consumption during the COVID-19 pandemic: a longitudinal cohort study using smart-breathalyzer data
Scientific Reports (2024)
-
Alcohol binge drinking and delirium cordis
Nature Cardiovascular Research (2022)