Abstract
Mitochondrial diseases represent a spectrum of disorders caused by impaired mitochondrial function, ranging in severity from mortality during infancy to progressive adult-onset disease. Mitochondrial dysfunction is also recognized as a molecular hallmark of the biological ageing process. Rapamycin, a drug that increases lifespan and health during normative ageing, also increases survival and reduces neurological symptoms in a mouse model of the severe mitochondrial disease Leigh syndrome. The Ndufs4 knockout (Ndufs4−/−) mouse lacks the complex I subunit NDUFS4 and shows rapid onset and progression of neurodegeneration mimicking patients with Leigh syndrome. Here we show that another drug that extends lifespan and delays normative ageing in mice, acarbose, also suppresses symptoms of disease and improves survival of Ndufs4−/− mice. Unlike rapamycin, acarbose rescues disease phenotypes independently of inhibition of the mechanistic target of rapamycin. Furthermore, rapamycin and acarbose have additive effects in delaying neurological symptoms and increasing maximum lifespan in Ndufs4−/− mice. We find that acarbose remodels the intestinal microbiome and alters the production of short-chain fatty acids. Supplementation with tributyrin, a source of butyric acid, recapitulates some effects of acarbose on lifespan and disease progression, while depletion of the endogenous microbiome in Ndufs4−/− mice appears to fully recapitulate the effects of acarbose on healthspan and lifespan in these animals. To our knowledge, this study provides the first evidence that alteration of the gut microbiome plays a significant role in severe mitochondrial disease and provides further support for the model that biological ageing and severe mitochondrial disorders share underlying common mechanisms.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The data used to generate the figures in this manuscript are publicly available and published along with the paper. Further information and requests for resources and reagents should be directed to and will be fulfilled by Alessandro Bitto (ab62@uw.edu). Source data are provided with this paper.
References
Janssen, R. J., Nijtmans, L. G., van den Heuvel, L. P. & Smeitink, J. A. Mitochondrial complex I: structure, function and pathology. J. Inherit. Metab. Dis. 29, 499–515 (2006).
Wallace, D. C. Mitochondrial DNA mutations in disease and aging. Environ. Mol. Mutagen. 51, 440–450 (2010).
Bannwarth, S. et al. Prevalence of rare mitochondrial DNA mutations in mitochondrial disorders. J. Med. Genet. 50, 704–714 (2013).
Fassone, E. & Rahman, S. Complex I deficiency: clinical features, biochemistry and molecular genetics. J. Med. Genet. 49, 578–590 (2012).
Budde, S. M. et al. Combined enzymatic complex I and III deficiency associated with mutations in the nuclear encoded NDUFS4 gene. Biochem. Biophys. Res. Commun. 275, 63–68 (2000).
Kruse, S. E. et al. Mice with mitochondrial complex I deficiency develop a fatal encephalomyopathy. Cell Metab. 7, 312–320 (2008).
Johnson, S. C. et al. mTOR inhibition alleviates mitochondrial disease in a mouse model of Leigh syndrome. Science 342, 1524–1528 (2013).
Johnson, S. C. et al. Dose-dependent effects of mTOR inhibition on weight and mitochondrial disease in mice. Front. Genet. 6, 247 (2015).
Kim, S. H. et al. Multi-organ abnormalities and mTORC1 activation in zebrafish model of multiple acyl-CoA dehydrogenase deficiency. PLoS Genet. 9, e1003563 (2013).
Peng, M. et al. Inhibiting cytosolic translation and autophagy improves health in mitochondrial disease. Hum. Mol. Genet. 24, 4829–4847 (2015).
Ito, T. K. et al. Hepatic S6K1 partially regulates lifespan of mice with mitochondrial complex I deficiency. Front. Genet. 8, 113 (2017).
Martin-Perez, M. et al. PKC downregulation upon rapamycin treatment attenuates mitochondrial disease. Nat. Metab. 2, 1472–1481 (2020).
Johnson, S. C. et al. mTOR inhibitors may benefit kidney transplant recipients with mitochondrial diseases. Kidney Int. 95, 455–466 (2019).
Sage-Schwaede, A. et al. Exploring mTOR inhibition as treatment for mitochondrial disease. Ann. Clin. Transl. Neurol. 6, 1877–1881 (2019).
Powers, R. W. 3rd, Kaeberlein, M., Caldwell, S. D., Kennedy, B. K. & Fields, S. Extension of chronological life span in yeast by decreased TOR pathway signaling. Genes Dev. 20, 174–184 (2006).
Robida-Stubbs, S. et al. TOR signaling and rapamycin influence longevity by regulating SKN-1/Nrf and DAF-16/FoxO. Cell Metab. 15, 713–724 (2012).
Bjedov, I. et al. Mechanisms of life span extension by rapamycin in the fruit fly Drosophila melanogaster. Cell Metab. 11, 35–46 (2010).
Harrison, D. E. et al. Rapamycin fed late in life extends lifespan in genetically heterogeneous mice. Nature 460, 392–395 (2009).
Anisimov, V. N. et al. Rapamycin increases lifespan and inhibits spontaneous tumorigenesis in inbred female mice. Cell Cycle 10, 4230–4236 (2011).
Komarova, E. A. et al. Rapamycin extends lifespan and delays tumorigenesis in heterozygous p53+/− mice. Aging (Albany NY) 4, 709–714 (2012).
Wilkinson, J. E. et al. Rapamycin slows aging in mice. Aging Cell 11, 675–682 (2012).
Livi, C. B. et al. Rapamycin extends life span of Rb1+/− mice by inhibiting neuroendocrine tumors. Aging (Albany NY) 5, 100–110 (2013).
Neff, F. et al. Rapamycin extends murine lifespan but has limited effects on aging. J. Clin. Investig. 123, 3272–3291 (2013).
Fok, W. C. et al. Mice fed rapamycin have an increase in lifespan associated with major changes in the liver transcriptome. PLoS ONE 9, e83988 (2014).
Miller, R. A. et al. Rapamycin-mediated lifespan increase in mice is dose and sex dependent and metabolically distinct from dietary restriction. Aging Cell 13, 468–477 (2014).
Popovich, I. G. et al. Lifespan extension and cancer prevention in HER-2/neu transgenic mice treated with low intermittent doses of rapamycin. Cancer Biol. Ther. 15, 586–592 (2014).
Bitto, A. et al. Transient rapamycin treatment can increase lifespan and healthspan in middle-aged mice. eLife 5, e16351 (2016).
Miller, R. A. et al. Rapamycin, but not resveratrol or simvastatin, extends life span of genetically heterogeneous mice. J. Gerontol. A Biol. Sci. Med. Sci. 66, 191–201 (2011).
Zhang, Y. et al. Rapamycin extends life and health in C57BL/6 mice. J. Gerontol. A Biol. Sci. Med. Sci. 69, 119–130 (2014).
Halloran, J. et al. Chronic inhibition of mammalian target of rapamycin by rapamycin modulates cognitive and non-cognitive components of behavior throughout lifespan in mice. Neuroscience 223, 102–113 (2012).
Majumder, S. et al. Lifelong rapamycin administration ameliorates age-dependent cognitive deficits by reducing IL-1β and enhancing NMDA signaling. Aging Cell 11, 326–335 (2012).
Zaseck, L. W., Miller, R. A. & Brooks, S. V. Rapamycin attenuates age-associated changes in tibialis anterior tendon viscoelastic properties. J. Gerontol. A Biol. Sci. Med. Sci. 71, 858–865 (2016).
Chiao, Y. A. et al. Rapamycin transiently induces mitochondrial remodeling to reprogram energy metabolism in old hearts. Aging (Albany NY) 8, 314–327 (2016).
Dai, D. F. et al. Altered proteome turnover and remodeling by short-term caloric restriction or rapamycin rejuvenate the aging heart. Aging Cell 13, 529–539 (2014).
Flynn, J. M. et al. Late-life rapamycin treatment reverses age-related heart dysfunction. Aging Cell 12, 851–862 (2013).
Chen, C., Liu, Y. & Zheng, P. mTOR regulation and therapeutic rejuvenation of aging hematopoietic stem cells. Sci. Signal. 2, ra75 (2009).
Shavlakadze, T. et al. Short-term low-dose mTORC1 inhibition in aged rats counter-regulates age-related gene changes and blocks age-related kidney pathology. J. Gerontol. A Biol. Sci. Med. Sci. 73, 845–852 (2018).
An, J. Y. et al. Rapamycin rejuvenates oral health in aging mice. eLife 9, e54318 (2020).
An, J. Y. et al. Rapamycin treatment attenuates age-associated periodontitis in mice. Geroscience 39, 457–463 (2017).
Yilmaz, O. H. et al. mTORC1 in the Paneth cell niche couples intestinal stem-cell function to calorie intake. Nature 486, 490–495 (2012).
Garcia, D. N. et al. Effect of caloric restriction and rapamycin on ovarian aging in mice. Geroscience 41, 395–408 (2019).
Urfer, S. R. et al. A randomized controlled trial to establish effects of short-term rapamycin treatment in 24 middle-aged companion dogs. Geroscience 39, 117–127 (2017).
Mannick, J. B. et al. mTOR inhibition improves immune function in the elderly. Sci. Transl. Med. 6, 268ra179 (2014).
Mannick, J. B. et al. TORC1 inhibition enhances immune function and reduces infections in the elderly. Sci. Transl. Med. 10, eaaq1564 (2018).
Lopez-Otin, C., Blasco, M. A., Partridge, L., Serrano, M. & Kroemer, G. The hallmarks of aging. Cell 153, 1194–1217 (2013).
Srivastava, S. The mitochondrial basis of aging and age-related disorders. Genes (Basel) 8, 398 (2017).
Trifunovic, A. & Larsson, N. G. Mitochondrial dysfunction as a cause of ageing. J. Intern. Med. 263, 167–178 (2008).
Berry, B. J. & Kaeberlein, M. An energetics perspective on geroscience: mitochondrial protonmotive force and aging. Geroscience 43, 1591–1604 (2021).
Bitto, A. Is aging an acquired mitochondrial disease? Innov. Aging 3, S394–S395 (2019).
Hoffmann, J. & Spengler, M. Efficacy of 24-week monotherapy with acarbose, metformin, or placebo in dietary-treated NIDDM patients: the Essen-II Study. Am. J. Med. 103, 483–490 (1997).
Harrison, D. E. et al. Acarbose improves health and lifespan in aging HET3 mice. Aging Cell 18, e12898 (2019).
Strong, R. et al. Longer lifespan in male mice treated with a weakly estrogenic agonist, an antioxidant, an α-glucosidase inhibitor or a Nrf2-inducer. Aging Cell 15, 872–884 (2016).
Quintana, A., Kruse, S. E., Kapur, R. P., Sanz, E. & Palmiter, R. D. Complex I deficiency due to loss of Ndufs4 in the brain results in progressive encephalopathy resembling Leigh syndrome. Proc. Natl Acad. Sci. USA 107, 10996–11001 (2010).
Kayser, E. B., Sedensky, M. M. & Morgan, P. G. Region-specific defects of respiratory capacities in the Ndufs4(KO) mouse brain. PLoS ONE 11, e0148219 (2016).
Harrison, D. E. et al. Acarbose, 17-α-estradiol, and nordihydroguaiaretic acid extend mouse lifespan preferentially in males. Aging Cell 13, 273–282 (2014).
DiNicolantonio, J. J., Bhutani, J. & O’Keefe, J. H. Acarbose: safe and effective for lowering postprandial hyperglycaemia and improving cardiovascular outcomes. Open Heart 2, e000327 (2015).
Lembcke, B., Loser, C., Folsch, U. R., Wohler, J. & Creutzfeldt, W. Adaptive responses to pharmacological inhibition of small intestinal α-glucosidases in the rat. Gut 28, 181–187 (1987).
Wick, A. N., Drury, D. R., Nakada, H. I. & Wolfe, J. B. Localization of the primary metabolic block produced by 2-deoxyglucose. J. Biol. Chem. 224 963–969 (1957).
Gordon, H. A. & Pesti, L. The gnotobiotic animal as a tool in the study of host microbial relationships. Bacteriol. Rev. 35, 390–429 (1971).
Reikvam, D. H. et al. Depletion of murine intestinal microbiota: effects on gut mucosa and epithelial gene expression. PLoS ONE 6, e17996 (2011).
Savage, D. C. & Dubos, R. Alterations in the mouse cecum and its flora produced by antibacterial drugs. J. Exp. Med. 128, 97–110 (1968).
Smith, B. J. et al. Changes in the gut microbiome and fermentation products concurrent with enhanced longevity in acarbose-treated mice. BMC Microbiol. 19, 130 (2019).
Koh, A., De Vadder, F., Kovatcheva-Datchary, P. & Backhed, F. From dietary fiber to host physiology: short-chain fatty acids as key bacterial metabolites. Cell 165, 1332–1345 (2016).
Bourassa, M. W., Alim, I., Bultman, S. J. & Ratan, R. R. Butyrate, neuroepigenetics and the gut microbiome: can a high fiber diet improve brain health? Neurosci. Lett. 625, 56–63 (2016).
Han, J., Lin, K., Sequeira, C. & Borchers, C. H. An isotope-labeled chemical derivatization method for the quantitation of short-chain fatty acids in human feces by liquid chromatography-tandem mass spectrometry. Anal. Chim. Acta 854, 86–94 (2015).
Kennedy, B. K. et al. Geroscience: linking aging to chronic disease. Cell 159, 709–713 (2014).
Kaeberlein, M. Translational geroscience: a new paradigm for 21st century medicine. Transl. Med. Aging 1, 1–4 (2017).
Leiser, S. F., Fletcher, M., Begun, A. & Kaeberlein, M. Life-span extension from hypoxia in Caenorhabditis elegans requires both HIF-1 and DAF-16 and is antagonized by SKN-1. J. Gerontol. A Biol. Sci. Med. Sci. 68, 1135–1144 (2013).
Mehta, R., Chandler-Brown, D., Ramos, F. J., Shamieh, L. S. & Kaeberlein, M. Regulation of mRNA translation as a conserved mechanism of longevity control. Adv. Exp. Med. Biol. 694, 14–29 (2010).
Asadi Shahmirzadi, A. et al.Alpha-ketoglutarate, an endogenous metabolite, extends lifespan and compresses morbidity in aging mice.Cell Metab. 32, 447–456.e6 (2020).
Mills, K. F. et al. Long-term administration of nicotinamide mononucleotide mitigates age-associated physiological decline in mice. Cell Metab. 24, 795–806 (2016).
Jain, I. H. et al. Hypoxia as a therapy for mitochondrial disease. Science 352, 54–61 (2016).
Ferrari, M. et al. Hypoxia treatment reverses neurodegenerative disease in a mouse model of Leigh syndrome. Proc. Natl Acad. Sci. USA 114, E4241–E4250 (2017).
Lee, C. F., Caudal, A., Abell, L., Nagana Gowda, G. A. & Tian, R. Targeting NAD+ metabolism as interventions for mitochondrial disease. Sci. Rep. 9, 3073 (2019).
Strong, R. et al. Lifespan benefits for the combination of rapamycin plus acarbose and for captopril in genetically heterogeneous mice. Aging Cell 21, e13724 (2022).
Weimer, S. et al. d-Glucosamine supplementation extends life span of nematodes and of ageing mice. Nat. Commun. 5, 3563 (2014).
Singh, S. et al. Chronic dietary administration of the glycolytic inhibitor 2-deoxy-d-glucose (2-DG) inhibits the growth of implanted Ehrlich’s ascites tumor in mice. PLoS ONE 10, e0132089 (2015).
Johnson, S. C. et al. Regional metabolic signatures in the Ndufs4(KO) mouse brain implicate defective glutamate/α-ketoglutarate metabolism in mitochondrial disease. Mol. Genet. Metab. 130, 118–132 (2020).
Gu, Y. et al. Analyses of gut microbiota and plasma bile acids enable stratification of patients for antidiabetic treatment. Nat. Commun. 8, 1785 (2017).
Perry, E. A. et al. Tetracyclines promote survival and fitness in mitochondrial disease models. Nat. Metab. 3, 33–42 (2021).
Rios-Covian, D., Salazar, N., Gueimonde, M. & de Los Reyes-Gavilan, C. G. Shaping the metabolism of intestinal Bacteroides population through diet to improve human health. Front. Microbiol. 8, 376 (2017).
MacLean, B. et al. Skyline: an open source document editor for creating and analyzing targeted proteomics experiments. Bioinformatics 26, 966–968 (2010).
Ritchie, M. E. et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 43, e47 (2015).
Smyth, G. K. Linear models and empirical Bayes methods for assessing differential expression in microarray experiments. Stat. Appl. Genet. Mol. Biol. 3, Article3 (2004).
Pang, Z. et al. MetaboAnalyst 5.0: narrowing the gap between raw spectra and functional insights. Nucleic Acids Res. 49, W388–W396 (2021).
Benjamini, Y. & Hochberg, Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J. R. Stat. Soc. Series B Stat. Methodol. 57, 289–300 (1995).
Acknowledgements
We acknowledge funding from the Nathan Shock Center of Excellence for the Biology of Aging (grant no. 3 P30 AG 013280) and from grant no. 1 R01 NS98329 Mechanisms of Mitochondrial Disease Suppression in Ndufs4 Knockout Mice.
Author information
Authors and Affiliations
Contributions
A.B. and M.K. devised the study. A.B., A.S.G., B.M.G.N., H.T., K.S., N.T.,G.V., J.B. and A.S. administered treatments, collected weight data and scored neurological phenotypes and survival. A.B., H.T., K.S., A.S. and N.T. collected tissues and ran western blot analyses. A.B., A.S.G., B.M.G.N., H.T., K.S., N.T., G.V. and S.R.U. helped maintain the mouse colony and genotyped animals. I.B.S. and W.D. helped with the design, execution and analysis of microbiome sequencing data. K.Y. and L.W. helped with the analysis of metabolomics data. E.-B.K. helped with the design and collection of samples for metabolomics analysis. J.M.S. performed all histopathology scoring. D.L.S. Jr. contributed acarbose and scientific rationale for the study. J.W.T. and L.D. measured the abundance of SCFAs. T.K.I. measured survival and neurological symptoms onset in mice treated with antibiotics. A.B. and M.K. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Metabolism thanks Albert Quintana and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Primary Handling Editor: Christoph Schmitt, in collaboration with the Nature Metabolism team.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Acarbose reduces brain inflammation in Ndufs4−/− mice.
(a) Semi-quantitative immunohistochemistry for GFAP (b) and Iba1 (c) in several brain regions. Data are presented as individual values (closed circles wild type untreated, closed triangles Ndufs4−/− untreated, open triangles Ndufs4−/− acarbose-treated), superimposed on mean +/− standard deviation. Mixed-Effect Model p-values; GFAP; wild type untreated vs Ndufs4−/− untreated =0.0003 (mean difference −1.333, 95% CI −1.992 to −0.6751), Striatum =0.0088 (mean difference = −0.7333, 95% CI −1.282 to −0.1851), Thalamus/Hippocampus =0.0002 (mean difference = −0.9167, 95% CI −1.387 to −0.4461), Cerebellum/Brainstem =0.0001 (mean difference −1.283, 95% CI −1.907 to −0.6598), Ndufs4−/− untreated vs. Ndufs4−/− acarbose-treated, olfactory bulb = 0.0026 (mean difference =1.3, 95% CI interval 0.4992 to 2.101), Thalamus/Hippocampus =0.0378 (mean difference =0.75, 95% CI 0.04374 to 1.456), cerebellum/brainstem, <0.0001 (mean difference =1.557, 95% CI 1.013 to 2.101); Iba1; wild type untreated vs Ndufs4−/− untreated, olfactory bulb <0.0001 (mean difference −1.75, −2.223 to −1.277), striatum =0.0303 (mean difference −0.5333, 95% CI −1.019 to −0.0475), Thalamus/Hippocampus =0.0307 (mean difference =−0.5833, 95% CI −1.117 to −0.04932), cerebellum =0.0134 (mean difference −0.8182, 95% CI −1.473 to −0.1630), cerebellum/brainstem =0.0003 (mean difference =−1.038, 95% CI −1.584 to −0.4916), wild type untreated vs Ndufs4−/− acarbose-treated, thalamus/hippocampus =0.0031 (mean difference =−0.9167, 95% CI −1.488 to −0.3457). N = 12/group wild type and Ndufs4−/− untreated, N = 7 Ndufs4−/− acarbose-treated. d. Western blot and e. densitometric analysis of Trem-2 expression in 50 days old brain lysates from wild type untreated (dark blue), Ndufs4−/− untreated (light blue), and acarbose-treated Ndufs4−/− mice (red). Bars are mean +/− standard deviation. N = 4/group, One-way ANOVA.
Extended Data Fig. 2 Acarbose effects are independent of sex.
A. and B. Individual survival curves of control-chow and acarbose-chow fed Ndufs4−/− mice. A. Log-rank p < 0.0001 N = 13/group B. Log-rank p < 0.001 N = 13 untreated, N = 12 acarbose-treated C. Pooled lifespan curves divided by sex. Log-rank p < 0.5944, N = 14 acarbose-treated males, N = 11 acarbose-treated females. D. Weight progression from weaning until post-natal day 81. Solid dark blue: female wild type mice fed control chow. Dotted dark blue: male wild type mice fed control chow. Solid dark red: female wild type mice fed acarbose chow. Dotted dark red: male wild type mice fed acarbose chow. Solid light blue: female Ndufs4−/− mice fed control chow Dotted light blue: male Ndufs4−/− mice fed control chow. Solid light red: female Ndufs4−/− mice fed acarbose chow. Dotted light red: male Ndufs4−/− mice fed acarbose chow. N = 8 female wild type untreated, N = 9 male wild type untreated, N = 5 females Ndufs4−/− untreated, N = 7 males Ndufs4−/− untreated, N = 4 females wild type acarbose, N = 4 males wild type acarbose, N = 7 females Ndufs4−/− acarbose, N = 6 males Ndufs4−/− acarbose. E. Comparison of weights at 35 days post-natal for control-chow fed wild type, Ndufs4−/− mice, acarbose-chow fed wild type, and Ndufs4−/− mice, divided by sex. *** p < 0.001 one way ANOVA. N = 8 female wild type untreated, N = 9 male wild type untreated, N = 5 females Ndufs4−/− untreated, N = 7 males Ndufs4−/− untreated, N = 4 females wild type acarbose, N = 4 males wild type acarbose, N = 7 females Ndufs4−/− acarbose, N = 6 males Ndufs4−/− acarbose.
Extended Data Fig. 3 Acarbose does not inhibit mTORc1 signaling but does not further extend lifespan in Ndufs4−/− mice treated with rapamycin.
a. Western blots of ribosomal protein S6 phosphorylation at serine 235/236. b. c. Densitometric analysis of the western blots in panel A. Data are mean +/− standard deviation. One-way ANOVA adjusted p-values: wild type untreated vs. wild type rapamycin =0.0148 (mean difference =1.813, 95% CI 0.3369 to 3.289), Ndufs4−/− untreated vs Ndufs4−/− rapamycin treated =0.0092 (mean difference= 2.048. 95% CI 0.4927 to 3.604). N = 4 wild type and Ndufs4−/− untreated, N = 5 wild type and Ndufs4−/− acarbose or rapamycin treated. d. Onset of neurological symptoms (clasping) measured in days after birth in control-chow (blue,) 0.1% acarbose-chow (red) fed, 8 mg/kg/day I.P. rapamycin-treated (green,) acarbose-chow fed and every other day rapamycin treated (orange) Ndufs4−/− mice. Data are mean +/− standard deviation. One-way ANOVA adjusted p-values: Ndufs4−/− untreated vs acarbose-treated =0.0005 (mean difference −12.32, 95% CI −19.97 to −4.667), Ndufs4−/− untreated vs. rapamycin-treated =0.0186 (mean difference =−9.071, 95% CI −16.98 to −1.163), Ndufs4−/− untreated vs double-treated <0.0001 (mean difference = −19.85, 95% CI −27.50 to −12.20), acarbose-treated Ndufs4−/− vs double treated =0.0375 (mean difference =−7.533, 95% CI −14.75 to −0.3207), rapamycin-treated Ndufs4−/− vs double treated =0.0020 (mean difference =−10.78, 95% CI −18.26 to −3.295). N = 12 Ndufs4−/− untreated, N = 15 Ndufs4−/− acarbose, N = 13 Ndufs4−/− rapamycin, N = 15 Ndufs4−/− double treated e. Survival curves of Ndufs4−/− mice fed either control (blue,) 0.1% acarbose diet (red,) treated with 8 mg/kg daily intraperitoneal rapamycin (orange,) acarbose diet + every other day rapamycin (orange). Median lifespan was 52 days for control-chow fed, 76.5 days for acarbose-chow fed mice (log-rank p < 0.05), 80 for rapamycin treated mice (log-rank p < 0.05), and 74 for double treatment regimens (log-rank p < 0.01). Double treatment with acarbose and every other day rapamycin also increased maximum lifespan, Mann-Whitney U, p < 0.05. N = 13 Ndufs4−/− untreated, N = 12 Ndufs4−/− acarbose, N = 16 Ndufs4−/− rapamycin, N = 15 Ndufs4−/− double treated f. Comparison of body weight progression at 35 days post-natal for untreated wt (dark blue), untreated Ndufs4−/− (light blue), acarbose treated wt (dark red), acarbose treated Ndufs4−/− (light red), rapamycin treated wt (dark green), rapamycin treated Ndufs4−/− (light green), double treated wt (dark orange), and double treated Ndufs4−/− mice (light orange). One-way ANOVA adjusted p-values: wild type untreated vs Ndufs4−/− untreated <0.0001 (mean difference =4.958, 95% CI 2.436 to 7.480), Ndufs4−/− untreated vs rapamycin-treated =0.0029 (mean difference =2.880, 95% CI 0.6592 to 5.101), Ndufs4−/− untreated vs double-treated =0.0119 (mean difference = 2.604, 95% CI 0.3549 to 4.853), acarbose-treated Ndufs4−/− vs rapamycin-treated =0.0229 (mean difference =2.199. 95% CI 0.1792 to 4.220). N = 10 wild type untreated, N = 13 Ndufs4−/− untreated, N = 11 wild type acarbose-treated, N = 17 Ndufs4−/− acarbose-treated, N = 9 wild type rapamycin-treated, N = 16 Ndufs4−/− rapamycin-treated, N = 10 wild type double treated, N = 15 Ndufs4−/− double treated, sex: both. G. Weight progression from weaning until post-natal day 81. Solid dark blue: wild type mice fed control chow. Solid dark red: wild type mice fed acarbose chow. Dotted light blue: Ndufs4−/− mice fed control chow. Dotted light red: Ndufs4−/− mice fed acarbose chow. Solid dark green: wt rapamycin. Dotted light green: Ndufs4−/− rapamycin. Solid dark orange: wt double treated. Dotted light orange: Ndufs4−/− double treated. N = 10 wild type untreated, N = 13 Ndufs4−/− untreated, N = 11 wild type acarbose-treated, N = 17 Ndufs4−/− acarbose-treated, N = 9 wild type rapamycin-treated, N = 16 Ndufs4−/− rapamycin-treated, N = 10 wild type double treated, N = 15 Ndufs4−/− double treated, sex: both.
Extended Data Fig. 4 Combination therapy with acarbose and rapamycin in Ndufs4−/− mice.
A. Western blot and B. densitometric analysis of ribosomal protein S6 phosphorylation in brains from 50 days old wild type untreated, Ndufs4−/− untreated, and acarbose treated Ndufs4−/− mice. Data are mean +/− standard deviation N = 4/group, One-way ANOVA. C. Daily double treatment with acarbose and rapamycin prevents growth and ultimately causes death in newly weaned mice. Solid lines indicate weight progression individual animals on daily double treatment with rapamycin and acarbose from weaning. Dark orange squares: wild type animals, light orange triangles: Ndufs4−/− animals Dotted lines are average weights of untreated animals, dark blue squares: wild type untreated, light blue triangles, Ndufs4−/− untreated. D. Onset of neurological symptoms (clasping) measured in days after birth in control-chow (blue,) 0.1% acarbose-chow (red) fed, 8 mg/kg/day I.P. rapamycin-treated (green,) acarbose-chow fed from weaning and daily rapamycin treated from post natal (p.n.) day 28 (grey) Ndufs4−/− mice. Data are mean +/− standard deviation. One-way ANOVA adjusted p-values: Ndufs4−/− untreated vs acarbose-treated =0.0004 (mean difference −12.32, 95% CI −20.08 to −4.550), Ndufs4−/− untreated vs. rapamycin-treated =0.0196 (mean difference =−9.071, 95% CI −17.10 to −10.43), Ndufs4−/− untreated vs double-treated <0.0001 (mean difference = −21.28, 95% CI −29.65 to −12.91), acarbose-treated Ndufs4−/− vs double treated =0.0202 (mean difference =−8.964, 95% CI −16.92 to −1.004), rapamycin-treated Ndufs4−/− vs double treated =0.0011 (mean difference =−12.21, 95% CI −20.42 to −3.995). N = 12 Ndufs4−/− untreated, N = 15 Ndufs4−/− acarbose, N = 13 Ndufs4−/− rapamycin, N = 11 Ndufs4−/− double treated. E. Survival curves of Ndufs4-/- mice fed either control (blue), 0.1% acarbose diet (red), treated with 8 mg/kg daily intraperitoneal rapamycin (orange), acarbose diet + every other day rapamycin (orange). Median lifespan was 52 days for control-chow fed, 76.5 days for acarbose-chow fed mice (log-rank p < 0.05), 80 for rapamycin treated mice (log-rank p < 0.05), and 74 for double treatment regimens (log-rank p < 0.01). Double treatment with acarbose and every other day rapamycin also increased maximum lifespan, Mann-Whitney U, p < 0.05. N = 13 Ndufs4-/- untreated, N = 12 Ndufs4-/- acarbose, N = 16 Ndufs4-/- rapamycin, N = 15 Ndufs4-/- double treated F. Comparison of body weight progression at 35 days post-natal for untreated wt (dark blue), untreated Ndufs4-/- (light blue), acarbose treated wt (dark red), acarbose treated Ndufs4-/- (light red), rapamycin treated wt (dark green), rapamycin treated Ndufs4-/- (light green), double treated wt (dark orange), and double treated Ndufs4-/- mice (light orange). One-way ANOVA adjusted p-values: wild type untreated vs Ndufs4-/- untreated <0.0001 (mean difference = 4.958, 95% CI 2.436 to 7.480), Ndufs4-/- untreated vs rapamycin-treated = 0.0029 (mean difference = 2.880, 95% CI 0.6592 to 5.101), Ndufs4-/- untreated vs double-treated = 0.0119 (mean difference = 2.604, 95% CI 0.3549 to 4.853), acarbose-treated Ndufs4-/- vs rapamycin-treated = 0.0229 (mean difference = 2.199. 95% CI 0.1792 to 4.220). N = 10 wild type untreated, N = 13 Ndufs4-/- untreated, N = 11 wild type acarbose-treated, N = 17 Ndufs4-/- acarbose-treated, N = 9 wild type rapamycin-treated, N = 16 Ndufs4-/- rapamycin-treated, N = 10 wild type double treated, N = 15 Ndufs4-/- double treated, sex: both. G. Weight progression from weaning until post-natal day 81. Solid dark blue: wild type mice fed control chow. Solid dark red: wild type mice fed acarbose chow. Dotted light blue: Ndufs4-/- mice fed control chow. Dotted light red: Ndufs4-/- mice fed acarbose chow. Solid dark green: wt rapamycin. Dotted light green: Ndufs4-/- rapamycin. Solid dark orange: wt double treated. Dotted light orange: Ndufs4-/- double treated. N = 10 wild type untreated, N = 13 Ndufs4-/- untreated, N = 11 wild type acarbose-treated, N = 17 Ndufs4-/- acarbose-treated, N = 9 wild type rapamycin-treated, N = 16 Ndufs4-/- rapamycin-treated, N = 10 wild type double treated, N = 15 Ndufs4-/- double treated, sex: both.
Extended Data Fig. 5 Metabolic profiling of brain regions in Ndufs4−/− mice treated with acarbose.
a. Schematic diagram of the metabolomics assay. b. Volcano plot of metabolic features in the olfactory bulb of untreated Ndufs4−/− mice compared to wild type littermates. Red dots are significantly altered metabolites. Linear model adjusted p-value (Benjamini-Hochberg FDR correction) <0.05. Individual metabolites p-values available in metabolomics dataset. c. Heat map of the relative abundance of selected significantly altered metabolites in the olfactory bulb of wild type untreated (WT-U), Ndufs4−/− untreated (KO-U), and acarbose-treated Ndufs4−/− mice (KO-A). d. and e. Specific Pathway Analysis of glycolysis intermediates in the olfactory bulb of untreated (D.) and acarbose-treated (E.) Ndufs4−/− mice. Red metabolites are significantly more abundant compared to untreated wild type; blue metabolites are significantly less abundant. Linear model adjusted p-value (Benjamini-Hochberg FDR correction) <0.05. Individual metabolites p-values available in metabolomics dataset. N = 4-5 per group.
Extended Data Fig. 6 Metabolomics reveals glucose dishomeostasis in Ndufs4−/− brains.
a Principal component analysis of the metabolomics dataset described in Fig. 4a. Light blue squares and circles, wild type untreated; red squares and circles, Ndufs4−/− untreated; dark blue squares and circles, acarbose-treated Ndufs4−/−. b. Metabolites Set Enrichment Analysis (MSEA) of metabolic pathways enriched in the olfactory bulb of untreated Ndufs4−/− compared to wild type animals. c. Metabolites Pathway Analysis (MPA) of metabolic pathways enriched in the olfactory bulb of untreated Ndufs4−/− compared to wild type animals. Color denotes p-value, same scale as in panel B., size of circles denotes impact. N = 4-5 per group for panels A to C. d. 1 h post-prandial blood glucose levels in wild type and Ndufs4−/− mice untreated or treated with acarbose. Data are mean +/− standard deviation. One-way ANOVA adjusted p-values: wild type untreated vs. Ndufs4−/− untreated =0.0018 (mean difference= 51.6, 95% CI 17.64 to 85.56), wild type untreated vs wild type acarbose =0.0428 (mean difference =30.2, 95% CI 0.7883 to 59.61). N = 5 wild type and Ndufs4−/− untreated, N = 10 wild type N = 13 Ndufs4−/− acarbose-treated. e. Survival plot of Ndufs4−/− mice treated with 0.2%, 0.4% 2-deoxyglucose (2DG) or 1%, 10% glucosamine (GlcN) mixed in the food. N = 26 untreated, N = 9 0.2% 2-deoxyglucose, N = 11 0.4% 2-deoxyglucose, N = 25 1% glucosamine, N = 13 10% glucosamine. F. Onset of clasping in Ndufs4−/− mice treated with 2-deoxyglucose (2DG) or glucosamine (GlcN). Data are mean +/− standard deviation. N = 12 untreated, N = 9 0.2% and 0.4% deoxyglucose, N = 21 1% glucosamine, N = 8 10% glucosamine.
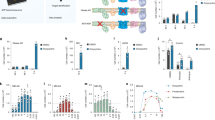
Extended Data Fig. 7 Acarbose alters the intestinal microbiome in Ndufs4−/− mice.
a. Centered log-ratio normalized proportion of Bacteroides divided by genotype and treatment. Linear regression p-value by treatment adjusted by genotype =0.001. N = 9-11 per group b-e. Center log-ratio normalized proportion of Prevotella (B.) Alistipes (C.) Clostridium (D.) and Rikenella (E.) divided by treatment. Linear regression p-value by treatment= 0.023 (B), 0.026 (C), 0.036 (D), 0.038 (E), FDR = 0.136.
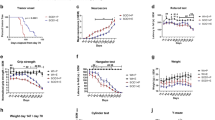
Extended Data Fig. 8 Tributyrin supplementation improves survival in Ndufs4−/− mice.
a. Survival plot of Ndufs4−/− treated with 50 mg/kg or 100 g/kg tributyrin. N = 25 untreated, N = 12 50 g/kg tributyrin, N = 16 100 g/kg tributyrin. b. Weight progression from weaning until post-natal day 81. Solid dark blue: wild type mice fed control chow (dark blue), Ndufs4−/− untreated (light blue), and tributyrin (shades of brown). Data are mean +/− standard deviation. N = 13 wild type and Ndufs4−/− untreated, N = 12 wild type 10 g/kg tributyrin, N = 18 Ndufs4−/− 10 g/kg tributyrin, N = 13 wild type and Ndufs4−/− 50 g/kg tributyrin, N = 12 wild type 100 g/kg tributyrin, N = 15 100 g/kg tributyrin. N = 20/group c-d. Linear trend of Ndufs4−/− (C.) and wild type mice (D.) weight after treatment with increasing doses of tributyrin at post-natal day 35. Data are mean +/− standard deviation. One-way ANOVA test for linear trend p-value = 0.0003 (Ndufs4−/−), 0.0005 (wild type). N = 13 wild type and Ndufs4−/− untreated, N = 12 wild type 10 g/kg tributyrin, N = 18 Ndufs4−/− 10 g/kg tributyrin, N = 13 wild type and Ndufs4−/− 50 g/kg tributyrin, N = 12 wild type 100 g/kg tributyrin, N = 15 100 g/kg tributyrin. e. Weight progression from weaning until post-natal day 70. Solid: wild type mice, dotted: Ndufs4−/− mice fed control chow (blue), tributyrin (brown), or rapamycin (green). Data are mean +/− standard deviation. f. Comparison of weights at 35 days post-natal for wild type and Ndufs4−/− fed either chow (blue), chow supplemented with 10 g/kg tributyrin (brown), injected with rapamycin (green), or fed chow supplemented with 10 g/kg tributyrin and injected with rapamycin (orange). Data are mean +/− standard deviation. One-way ANOVA, adjusted p-values: wt untreated vs Ndufs4−/− untreated =0.0112 (mean difference 4.5, 95% CI 0.8824 to 8.119), Ndufs4−/− untreated vs. Ndufs4−/− rapamycin-treated <0.0001 (mean difference 3.533, 95% CI 1.807 to 5.260), Ndufs4−/− untreated vs Ndufs4−/− tributyrin+rapamycin-treated =0.007 (mean difference 2.330, 95% CI 0.4753 to 4.184). N = 11 wild type untreated, N = 21 Ndufs4−/− untreated, N = 12 wild type 10 g/kg tributyrin, N = 18 Ndufs4−/− 10 g/kg tributyrin, N = 9 wt rapamycin, N = 17 Ndufs4−/− rapamycin, N = 7 wt tributyrin + rapamycin, N = 13 Ndufs4−/− tributyrin + rapamycin. g. Onset of clasping in untreated (blue), tributyrin-treated (brown), rapamycin treated (green), or tributyrin and rapamycin-treated Ndufs4−/− mice. Data are mean +/− standard deviation. One-way ANOVA, adjusted p-value untreated vs tributyrin =0.0486 (mean difference −5.888, 95% CI −11.75 to −0.02388), untreated vs. rapamycin =0.0126 (mean difference =−7.354, 95% CI −13.54 to −1.172), untreated vs. tributyrin+rapamycin <0.0001 (mean difference = −11.43, 95% CI −17.61 to −5.248). N = 15 untreated, N = 16 tributyrin-treated, N = 13 rapamycin-treated, N = 13 tributyrin and rapamycin treated. h. Survival plot of Ndufs4-/- untreated (blue), tributyrin-treated (brown), rapamycin treated (green), or tributyrin and rapamycin-treated Ndufs4-/- mice. N = 12 untreated, N = 18 tributyrin, N = 16 rapamycin, N = 13 tributyrin + rapamycin. Log-rank p<0.0001.
Supplementary information
Source data
Source Data Fig. 1
Histology panels and source scans values tables.
Source Data Fig. 2
Source data tables.
Source Data Fig. 3
Photograph of caeca and source data tables.
Source Data Fig. 4
Source data tables.
Source Data Extended Data Fig. 1
Histology panels, source data tables and western blots scans.
Source Data Extended Data Fig. 2
Source data tables.
Source Data Extended Data Fig. 3
Western blot scans and source data tables.
Source Data Extended Data Fig. 4
Western blot scans and source data tables.
Source Data Extended Data Fig. 5
Source data tables and metabolomics dataset.
Source Data Extended Data Fig. 6
Source data tables.
Source Data Extended Data Fig. 7
Source data tables.
Source Data Extended Data Fig. 8
Source data tables.
Rights and permissions
About this article
Cite this article
Bitto, A., Grillo, A.S., Ito, T.K. et al. Acarbose suppresses symptoms of mitochondrial disease in a mouse model of Leigh syndrome. Nat Metab 5, 955–967 (2023). https://doi.org/10.1038/s42255-023-00815-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s42255-023-00815-w