Abstract
Carriers of a premutation allele (PM) in the FMR1 gene are at risk of developing a number of Fragile X premutation asssociated disorders (FXPAC), including Fragile X-associated Tremor/Ataxia Syndrome (FXTAS), Fragile X-associated Primary Ovarian Insufficiency (FXPOI), and Fragile X-associated neuropsychiatric disorders (FXAND). We have recently reported somatic CGG allele expansion in female PM; however, its clinical significance remains unclear. The aim of this study was to examine the potential clinical association between somatic FMR1 allele instability and PM associated disorders. Participants comprised of 424 female PM carriers age 0.3– 90 years. FMR1 molecular measures and clinical information on the presence of medical conditions, were determined for all subjects for primary analysis. Two sub-groups of participants (age ≥ 25, N = 377 and age ≥ 50, N = 134) were used in the analysis related to presence of FXPOI and FXTAS, respectively. Among all participants (N = 424), the degree of instability (expansion) was significantly higher (median 2.5 vs 2.0, P = 0.026) in participants with a diagnosis of attention deficit hyperactivity disorder (ADHD) compared to those without. FMR1 mRNA expression was significantly higher in subjects with any psychiatric disorder diagnosis (P = 0.0017); specifically, in those with ADHD (P = 0.009), and with depression (P = 0.025). Somatic FMR1 expansion was associated with the presence of ADHD in female PM and FMR1 mRNA levels were associated with the presence of mental health disorders. The findings of our research are innovative as they suggest a potential role of the CGG expansion in the clinical phenotype of PM and may potentially guide clinical prognosis and management.
Similar content being viewed by others

Introduction
The fragile X premutation carrier status has received growing recognition as a distinct clinical and molecular entity beyond Fragile X syndrome (FXS) over the past two decades. PM individuals have between 55 to 200 CGG repeats in the 5’ region of the FMR1 gene and typically pass on the mutation to their offspring, with a propensity for expansion to the full mutation state (> 200 CGG repeats) in each subsequent generation1. While FXS is one of the most common single gene disorders causing intellectual disability, the premutation status is more common and occurs in approximately 1 in 400 males and 1 in 200 females2. We now know that the premutation status is associated with specific clinical conditions including Fragile X-associated Tremor/Ataxia Syndrome (FXTAS), Fragile X-associated Primary Ovarian Insufficiency (FXPOI), and Fragile X-associated Neuropsychiatric Disorders (FXAND)3,4,5. Other research groups have referred to these neuropsychiatric and other conditions associated with the premutation as Fragile X-premutation associated conditions (FXPAC) due to concerns of stigma associated with the term ‘disorder’. Regardless, it is important to recognize the presence and burden of these conditions in PM carriers as many of them are associated with significant comorbidity.
Occurrence of these disorders varies across PM with gender differences as well. For instance, FXTAS is seen in 40–75% of male PM and 8–16% of females6,7. Common FXAND conditions include anxiety (occurring in 50–70% of carriers) and depression (40–65% of carriers) but increasingly, attention deficit hyperactivity disorder (ADHD) and autism spectrum disorder (ASD) have also been reported to be more common in PM, with reported prevalence rates of 30–45% and 8% respectively8,9,10,11,12. The molecular basis behind these disorders is attributed to the toxicity related to elevated levels of FMR1 mRNA seen in PM13,14. This is proposed to interfere with various cellular functions through mitochondrial dysfunction, calcium dysregulation and cell/DNA damage repair functions13,15,16,17.
Instability of the FMR1 premutation allele has recently been described for the first time by our group on a large sample of female PM18. Specifically, we characterized the presence of a series of unstable expanded alleles in ~ 94% of peripheral blood samples differing from the major premutation allele by one or more repeat units. The degree of expansion was directly proportional to the number of CGG repeats in the original allele with an indication that the extent of the expansion increased with age as well. Expansion was also inversely proportional to the number of AGG anchors which are considered to be ‘stabilizers’ that prevent CGG expansion across generations. However, the clinical implications of the presence and degree of this somatic expansion is, as yet, unclear. Indeed, given that this observation was based on peripheral blood sample, how this translates to brain tissue and its possible implications especially in the pathophysiology of neurologic premutation associated conditions like FXAND and FXTAS are important areas for further studies.
The aim of this study was to examine the potential clinical associations between somatic expansion in female PM and premutation associated conditions. We hypothesized that a higher degree of expansion will be associated with a greater occurrence of disorders; and hence planned for separate sub-group analysis by age-range of the cohort a priori.
Methods
Subjects
Participants in this study included 424 female PM age 0.3–90 years whose premutation status (CGG repeat size 55–200) was confirmed by PCR/Southern blot testing. FMR1 molecular measures and clinical information, were determined for all 424 subjects and used in the primary analysis. In addition, participants were divided in two additional sub-groups for the analysis related to the presence of FXPOI and FXTAS (age ≥ 25, N = 377, and age ≥ 50, N = 134 respectively).
Participants were enrolled either as part of a dedicated research visit or following cascade testing after consultation for a child or sibling with fragile X syndrome. The study and all research protocols were carried out in accordance with and was approved by the Institutional Review Board at the University of California, Davis. All participants gave written informed consent before participating in the study.
Clinical information
Clinical information on the presence and severity of FXTAS, presence of FXPOI, presence of FXAND disorders, neurological symptoms, chronic medical problems and auto-immune conditions and demographic variables including weight, height, history of smoking and education level were documented on a data sheet filled out in taking the medical history. Ascertainment of presence and stage (range 1–5) of FXTAS was made by an experienced physician (RJH) who has several years of experience with PM patients, following detailed medical examination and review of Magnetic Resonance Imaging images of patients. Presence of FXPOI was defined as occurrence of early menopause prior to 40 years of age.
Presence of FXAND disorders was determined based on DSM-5 criteria for respective FXAND conditions, following evaluation by a trained medical provider or psychologist. FXAND disorders examined, specifically included anxiety, depression, ASD and ADHD and standardized assessments such as the Autism Diagnostic Observation Schedule (ADOS)19, the Structured Clinical Interview for DSM-5 (SCID-5)20, and the Kiddie Schedule for Affective Disorders and Schizophrenia (K-SADS)21, for younger patients, were used. Information on results of the SCID-5 In terms of presence of at least 1 psychiatric disorder (e.g. specific phobias, social phobia, generalized anxiety disorder, major depressive disorder) was obtained. A cognitive assessment based on standardized testing was carried out. Given the wide age-range of participants, a variety of standardized cognitive assessments were used across study participants. These included the Wechsler Intelligence Scale for Children, Third or Fourth Edition (WISC-III or WISC-IV)22, the Stanford Binet Intelligence Scales, Fifth Edition (SB-5)23, and the Wechsler Adult Intelligence Scale, Third or Fourth Edition (WAIS-III or WAIS-IV)24, as per participant age.
Specific chronic medical conditions of interest comprised hyper or hypothyroidism, diabetes mellitus, migraine, osteoporosis, seizures and autonomic dysfunction such as urinary incontinence. Information on these conditions were collapsed into a single category titled chronic medical conditions with presence of at least 1 condition and number of conditions collected. Specific auto-immune conditions included systemic lupus erythematosus, rheumatoid arthritis, fibromyalgia, autoimmune thyroid conditions and multiple sclerosis. Similarly, presence of at least 1 auto-immune condition and number of such conditions was collected under the category of auto-immune conditions.
Molecular data
Molecular data, including CGG allele repeat size, AGG interruptions and expansion were obtained from DNA samples isolated from 3 mL of whole blood using the Gentra Puregene Blood Kit (Qiagen, Valencia, CA, USA). FMR1 allele size was assessed through PCR and Southern blot analysis as previously described25,26. PCR used specific FMR1 primers (AmplideX PCR/CE, Asuragen) and PCR products were visualized by capillary electrophoresis (CE). Southern blot analysis was used to determine the methylation status of the FMR1 alleles (Activation ratio, AR and percent of methylation) as reported in Tassone et al.27 The AR value indicates the percentage of cells carrying the normal allele on the active X-chromosome. The number of AGG interruptions were quantified with a triplet primed PCR protocol as reported in Yrigollen et al.28,29, which was then visualized with CE and analyzed with Peak Scanner Software 2.0. To quantify the degree of expansion in each participant, the original size allele (Peak 1) and the modal expanded allele (Peak 2) needed to be identified, in which identification of Peak 1 was facilitated by X-inactivation in females. The expanded peak with the highest relative fluorescence units (RFU) value was selected as Peak 2. Expansion was calculated using the formula (Peak 2–Peak 1), more details can be found in Hwang et al.18. Total RNA was isolated from 2.5 ml of peripheral blood collected in PAXgene (Qiagen, Valencia, CA, United States) and quantified using the Agilent 2100 Bioanalyzer system. To measure FMR1 transcript expression levels, qRT-PCR used Assays-On-Demand (Applied Biosystems, Foster City, CA, USA) and custom TaqMan primers and probe assays as specified by Tassone et al.13.
Statistical analysis
All analysis was conducted using R version 4.0.5 (2021-03-31). Analysis was conducted on all participants (0.3–90 years old) as well as on those age ≥ 25 years (FXPOI group) and those ≥ 50 years (FXTAS group) as separate sub-groups. Specific measures analyzed in the FXPOI group was the age at menopause and the presence of FXPOI while that in the FXTAS group was the presence and the stage of FXTAS. Expansion was measured as described in our previous paper18 but in essence, instability was represented by ∆Rpts, which, in a repeat profile, represents the difference in the number of repeats between the modal expanded allele (Peak 2) and modal stable allele (Peak 1). Spearman test of correlation were used to examine CGG repeat length, FMR1 mRNA expression, and expansion (measured as peak 2—peak 1) against IQ measures. CGG repeat length, FMR1 mRNA expression, and expansion, were compared between subjects with and without a given clinical condition using Wilcoxon rank sum tests. FMR1 was modelled by CGG, adjusting for activation ratio (AR), using a linear regression model with FMR1 as the response and CGG and AR as covariates. Analyses of associations between expansion and clinical phenotype was not adjusted for CGG repeat number as none of the clinical conditions were significantly associated with the number of CGG repeats and CGG repeats furthermore did not differ meaningfully between subjects with and without a given condition.
Ethics approval and consent to participate
The study and all research protocols were carried out in accordance with the Institutional Review Board at the University of California, Davis. All participants gave written informed consent before participating in the study.
Results
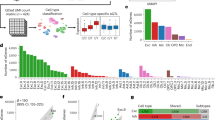
The final number of participants consisted of 424 female PM with an age range of 0.3 to 90 years. The mean number of CGG repeats was 92.1 (SD 23.0); premutation expansion, was present in all 424 participants and somatic instability, as illustrated in Fig. 1, was present in ~ 92% of them. Average full-scale IQ of participants was 119.8 (SD 19.0). Table 1 shows the descriptive molecular and clinical data of the three groups of participants. There was a large range of clinical conditions present within participants with the most common ones being anxiety (77.3% of those who had available data) and depression (63.6%). The majority of the participants (84.0%) had at least one FXAND condition. Among the 43 participants who had FXPOI within the \(\ge\) 25 years old sub-group, 36 (85.7%) had anxiety, 30 (71.4%) had depression, 13 (30.2%) had autoimmune conditions.
Example of a PCR profile (visualized by a Capillary Electrophoretogram) observed in a female PM showing somatic allelic instability. The degree of CGG instability is shown as a shoulder pattern (serial of peaks) located to the right side of the premutation allele peak. Instability is calculated as Peak 2 (unstable premutation allele size, highest peak size of the shoulder pattern) minus Peak 1 (stable premutation allele size on the left of the shoulder pattern) as described in Hwang et al. 2022.
Looking at the entire cohort, the degree of expansion was significantly higher in participants with a diagnosis of ADHD (median difference 2.5) compared to those without the diagnosis (median difference 2.0, P = 0.026) (Table 2). A sensitivity analyses of the association between instability and ADHD, adjusting for age, yielded the same conclusions as the unadjusted analysis. Expansion was not associated with any other clinical condition. FMR1 mRNA expression was significantly higher in participants with at least 1 SCID-5 diagnosis (median difference 1.98 vs 0.87, P = 0.0017), in those with ADHD (2.30 vs 2.04, P = 0.009), in those with depression (2.19 vs 1.98, P = 0.025) and in those with at least 1 FXAND condition (2.16 vs 1.94, P = 0.005). (Table 3 and Fig. 2). Full-scale IQ was not significantly correlated with either expansion, FMR1 mRNA or number of CGG repeats.
Analysis was also done to look at the presence of clinical conditions by other molecular measures namely number of CGG repeat numbers, number of AGG anchors and the AR. CGG repeat length did not differ significantly with presence of any clinical condition. However, among those with > 105 CGG repeats, there was a greater proportion of participants with ADHD compared to those with < 105 CGG repeats; although this was not statistically significant. The proportion of participants with ADHD was also highest in those with an AR between 0.21 and 0.40 as compared to other ranges. There were no other significant associations with CGG repeat numbers or AR for any clinical condition. Lastly, although in our analysis we observed differences in the number of AGG anchors, they did not reach significance with the presence of any clinical condition. As expected, after adjusting for AR, FMR1 mRNA levels increased significantly with increasing number of CGG repeats (B = 0.016, SE = 0.002, P = < 0.001) (Fig. 3). Further, the increase in levels of FMR1 mRNA was clearly modulated by the AR, with participants who had a higher ratio having lower increase in FMR1 mRNA levels.
Looking at demographic variables associated with clinical conditions, participants who had ADHD were significantly younger than those without the condition, as expected (mean age 47.0 years vs 52.0; P = 0.037). Those who had anxiety were much more likely to have a lower educational status as compared to those who did not have anxiety (47.0% with college education or higher vs 75.0%, P = 0.034). Age, educational attainment, or history of smoking were not associated with any other clinical condition.
Among the FXPOI sub-group, there was no significant association noted between presence of FXPOI and degree of expansion (median expansion in those with FXPOI vs those without FXPOI 2.0 vs 2.0, P = 0.875). The rate of FXPOI was associated with number of CGG repeats as shown in the bar plots in Fig. 4) with the highest prevalence observed in those carrying an allele in the mid-premutation range as previously reported30. Furthermore, CGG repeat length was significantly larger (median 3.0 vs 2.0, P = 0.020) and allelic expansion higher in subjects with ADHD (median 92.5 vs 87.0, P = 0.027). In the FXTAS sub-group, expansion was not associated with the presence or the stage of FXTAS. Interestingly, degree of expansion was lower in subjects with at least 1 diagnosis on the SCID-5 (0.0 vs 2.5, P = 0.0428), although this was based on a small number of subjects (N = 18).
Discussion
This study sought to assess the clinical implications, if any, of somatic allelic expansion in a large cohort of female PM participants. Our main findings suggest that expansion is associated with significantly higher occurrence of ADHD among female PM. Further, higher levels of FMR1 mRNA are associated with an occurrence of neuropsychiatric conditions including depression and ADHD. Lastly, levels of FMR1 mRNA were significantly predicted by number of CGG repeats and by AR amongst female PM, confirming findings from previous studies31,32,33.
Our findings with respect to FMR1 mRNA levels likely reflect the toxicity of elevated levels of mRNA, which has been shown to interfere with mitochondrial function, calcium regulation and cellular repair mechanisms as well as contributing to gain of function mutations13,15,16,17. These disruptions at the molecular level are thought to contribute to the increased pathology seen in PM, resulting in white matter disease in those with FXTAS and other psychiatric problems associated with FXAND. The positive association between FMR1 mRNA levels and number of CGG repeats is not surprising and is consistent with previous literature13. Elevated levels of FMR1 mRNA have also been shown to be associated with increased levels of psychological symptoms previously31,34; our findings add to this in terms of specific psychiatric conditions associated with mRNA levels. We further demonstrate here the crucial role played by the AR as the more favorable the ratio, with greater proportion of the non-mutated allele being active, the lower the excess mRNA produced.
It has also been shown that PM carriers who have higher repeat numbers (> 120 CGG) tend to have lower FMRP levels as well, likely due to the inefficiency of the translational process35,36. This combination of elevated mRNA levels and lowered FMRP levels could create a ‘double-hit’ phenomenon resulting in greater occurrence of disorders associated with both the reduced FMRP expression because translation inefficiency and RNA toxicity due to the presence of elevated levels of FMR1 mRNA37. Indeed, a series of cases including PM with CGG repeats in the upper premutation range has previously demonstrated a high occurrence of affective mood disorders, anxiety and psychotic thinking37. The combined pathology resultant of both increased mRNA and lowered FMRP is thought to contribute to this occurrence.
ADHD is a common neurodevelopmental disorder that seen in children and adolescents with a population prevalence rate of typically around 5.0% to 9.8%38,39,40. Elevated levels of ADHD have been demonstrated in PM in several studies10,12,41,42. Consistent with these reports, in our cohort of 424 participants, we observed that 26.2% of carriers had a diagnosis of ADHD; and this was more likely in younger participants in keeping with ADHD traditionally being considered a predominantly childhood neurodevelopmental disorder and limited awareness and diagnosis of ADHD in adults in the past. Although the exact reasons for elevated rates of ADHD in PM are not yet clear, neuro-imaging of PM has demonstrated changes in grey matter voxel density in the amygdala, insula and caudate and this may be related to executive function challenges43. Furthermore, the increased vulnerability of PM neurons related to mRNA toxicity as discussed above is possibly related to attentional and emotional regulation difficulties15. The presence of expansion could be a further modulator of this effect within the nervous system. Importantly, given what is seen in a mouse model of the FXDs44, and in patients with other repeat expansion diseases45,46, the degree of expansion may be higher in the brain compared to peripheral blood from which this study’s samples were obtained. As we previously showed, given that expansion increases with the number of CGG repeats and that the latter correlates with FMR1 mRNA levels, the presence of expansion could be a marker for elevated mRNA related toxicity. This may explain the greater occurrence of ADHD within our cohort. However, one of the limitation of our study is that our data was restricted in terms of subtypes of severity and ADHD (inattentive vs hyperactive-impulsive). Thus, future research into the implications of expansion on the nature of ADHD is warranted to shed light on possible associative mechanisms. Further, this study includes a small sample size especially for some for the clinical conditions investigated at various age points, which was related to data availability in medical record review. Consequently, the study may have had limited statistical power for detection of significant associations. Increasing the overall sample size and targeted recruitment of PM of specific age groups could help overcome this in future studies. In addition, participants included were not a population sample but rather a mixture of PM seen for clinical concerns and identified by cascade testing. Hence prevalence of clinical conditions such as FXAND conditions could be higher than true prevalence values. However, this preliminary data suggest a potential role of allelic somatic expansion as a biomarker that may be useful for assessing prognosis and clinical management of patients PM.
Conclusion
Somatic FMR1 allele expansion was associated with the presence of ADHD in female PM. In addition, higher FMR1 mRNA levels were associated with the presence of multiple neuropsychiatric conditions as well as increased number of CGG repeats. As such, this work is of relevance as it indicates that somatic allelic CGG expansion could be a potential molecular marker for the manifestation of neuropsychiatric conditions in PM. It is, therefore, original, as it constitutes the first study where somatic instability of the FMR1 CGG repeat has been associated with clinical conditions in a large cohort of female PM. Further research on the clinical implications of expansion could potentially help to discern the clinical phenotype and guide prognostication and management of these conditions in these individuals.
Data availability
Data can be made available on reasonable request to the corresponding author.
Abbreviations
- PM:
-
Premutation
- ADHD:
-
Attention deficit hyperactivity disorder
- FXTAS:
-
Fragile X-associated Tremor/Ataxia Syndrome
- FXPOI:
-
Fragile X-associated Primary Ovarian Insufficiency
- FXAND:
-
Fragile X-associated Neuropsychiatric Disorders
- ASD:
-
Autism spectrum disorder
- CE:
-
Capillary electrophoresis
- RFU:
-
Relative fluorescence units
References
Hagerman, R.J.H., P. J., Fragile X Syndrome and Premutation Disorders. 2020, Mac Keith Press.
Tassone, F. et al. FMR1 CGG allele size and prevalence ascertained through newborn screening in the United States. Genome Med. 4(12), 100 (2012).
Jacquemont, S. et al. Fragile X premutation tremor/ataxia syndrome: Molecular, clinical, and neuroimaging correlates. Am. J. Hum. Genet. 72(4), 869–878 (2003).
Sullivan, A. K. et al. Association of FMR1 repeat size with ovarian dysfunction. Hum. Reprod. 20(2), 402–412 (2005).
Hagerman, R. J. et al. Fragile X-associated neuropsychiatric disorders (FXAND). Front. Psychiatry 9, 564 (2018).
Hagerman, R. J. & Hagerman, P. Fragile X-associated tremor/ataxia syndrome-features, mechanisms and management. Nat. Rev. Neurol. 12(7), 403–412 (2016).
Hagerman, R. & Hagerman, P. Fragile X-associated tremor/ataxia syndrome: Pathophysiology and management. Curr. Opin. Neurol. 34(4), 541–546 (2021).
Cordeiro, L. et al. Anxiety disorders in fragile X premutation carriers: Preliminary characterization of probands and non-probands. Intractable Rare Dis. Res. 4(3), 123–130 (2015).
Bourgeois, J. A. et al. Cognitive, anxiety and mood disorders in the fragile X-associated tremor/ataxia syndrome. Gen. Hosp. Psychiatry 29(4), 349–356 (2007).
Farzin, F. et al. Autism spectrum disorders and attention-deficit/hyperactivity disorder in boys with the fragile X premutation. J. Dev. Behav. Pediatr. 27(2 Suppl), S137–S144 (2006).
Clifford, S. et al. Autism spectrum phenotype in males and females with fragile X full mutation and premutation. J. Autism. Dev. Disord. 37(4), 738–747 (2007).
Bailey, D. B. Jr. et al. Co-occurring conditions associated with FMR1 gene variations: Findings from a national parent survey. Am. J. Med. Genet. A 146A(16), 2060–2069 (2008).
Tassone, F. et al. Elevated levels of FMR1 mRNA in carrier males: A new mechanism of involvement in the fragile-X syndrome. Am. J. Hum. Genet. 66(1), 6–15 (2000).
Galloway, J. N. & Nelson, D. L. Evidence for RNA-mediated toxicity in the fragile X-associated tremor/ataxia syndrome. Fut. Neurol. 4(6), 785–798 (2009).
Chen, Y. et al. Murine hippocampal neurons expressing Fmr1 gene premutations show early developmental deficits and late degeneration. Hum. Mol. Genet. 19(1), 196–208 (2010).
Robin, G. et al. Calcium dysregulation and Cdk5-ATM pathway involved in a mouse model of fragile X-associated tremor/ataxia syndrome. Hum. Mol. Genet. 26(14), 2649–2666 (2017).
Napoli, E. et al. Altered zinc transport disrupts mitochondrial protein processing/import in fragile X-associated tremor/ataxia syndrome. Hum. Mol. Genet. 20(15), 3079–3092 (2011).
Hwang, Y. H. et al. Both cis and trans-acting genetic factors drive somatic instability in female carriers of the FMR1 premutation. Sci. Rep. 12(1), 10419 (2022).
Lord, C., et al., Autism Diagnostic Observation Schedule Second Edition (ADOS-2) Manual (Part 1): Modules 1–4. Torrance, CA: Western Psychological Services, 2012.
First, M.B., Structured clinical interview for the DSM (SCID). The encyclopedia of clinical psychology, 2014: p. 1–6.
Kaufman, J. et al. Schedule for affective disorders and schizophrenia for school-age children-present and lifetime version (K-SADS-PL): Initial reliability and validity data. J. Am. Acad. Child Adolesc. Psychiatry 36(7), 980–988 (1997).
Wechsler, D., Wechsler abbreviated scale of intelligence. 1999: Psychological Corporation.
Roid, G.H. and M. Pomplun, The Stanford-Binet Intelligence Scales. 2012: The Guilford Press.
Wechsler, D., Wechsler adult Intelligence Scale. Archives of Clinical Neuropsychology, 1955.
Tassone, F. et al. A rapid polymerase chain reaction-based screening method for identification of all expanded alleles of the fragile X (FMR1) gene in newborn and high-risk populations. J. Mol. Diagn. 10(1), 43–49 (2008).
Filipovic-Sadic, S. et al. A novel FMR1 PCR method for the routine detection of low abundance expanded alleles and full mutations in fragile X syndrome. Clin. Chem. 56(3), 399–408 (2010).
Tassone, F. et al. FMRP expression as a potential prognostic indicator in fragile X syndrome. Am. J. Med. Genet. 84(3), 250–261 (1999).
Yrigollen, C. M. et al. AGG interruptions within the maternal FMR1 gene reduce the risk of offspring with fragile X syndrome. Genet. Med. 14(8), 729–736 (2012).
Villate, O. et al. Effect of AGG interruptions on FMR1 maternal transmissions. Front. Mol. Biosci. 7, 135 (2020).
Allen, E. G. et al. Refining the risk for fragile X-associated primary ovarian insufficiency (FXPOI) by FMR1 CGG repeat size. Genet. Med. 23(9), 1648–1655 (2021).
Johnson, D., et al., Increased pain symptomatology among females vs. males with fragile X-associated tremor/ataxia syndrome. Front. Psychiatry, 2021. 12.
Tassone, F. et al. Transcription of the FMR1 gene in individuals with fragile X syndrome. Am. J. Med. Genet. 97(3), 195–203 (2000).
Yrigollen, C. M. et al. The role of AGG interruptions in the transcription of FMR1 premutation alleles. PLoS ONE 6(7), e21728 (2011).
Hessl, D. et al. Abnormal elevation of FMR1 mRNA is associated with psychological symptoms in individuals with the fragile X premutation. Am. J. Med. Genet. B Neuropsychiatr. Genet. 139(1), 115–121 (2005).
Ludwig, A. L. et al. CNS expression of murine fragile X protein (FMRP) as a function of CGG-repeat size. Hum. Mol. Genet. 23(12), 3228–3238 (2014).
Pretto, D. I. et al. Differential increases of specific FMR1 mRNA isoforms in premutation carriers. J. Med. Genet. 52(1), 42–52 (2015).
Schneider, A. et al. Elevated FMR1-mRNA and lowered FMRP–a double-hit mechanism for psychiatric features in men with FMR1 premutations. Transl. Psychiatry 10(1), 1–8 (2020).
Ghandour, R. M. et al. Prevalence and treatment of depression, anxiety, and conduct problems in US children. J. Pediatr. 206, 256-267.e3 (2019).
Bitsko, R. H. et al. Mental health surveillance among children-United States, 2013–2019. MMWR Suppl. 71(2), 1–42 (2022).
Sayal, K. et al. ADHD in children and young people: Prevalence, care pathways, and service provision. Lancet Psychiatry 5(2), 175–186 (2018).
Dorn, M. B., Mazzocco, M. M. & Hagerman, R. J. Behavioral and psychiatric disorders in adult male carriers of fragile X. J. Am. Acad. Child Adolesc. Psychiatry 33(2), 256–264 (1994).
Hunter, J. E. et al. The FMR1 premutation and attention-deficit hyperactivity disorder (ADHD): Evidence for a complex inheritance. Behav. Genet. 42(3), 415–422 (2012).
Moore, C. J. et al. The effect of pre-mutation of X chromosome CGG trinucleotide repeats on brain anatomy. Brain 127(Pt 12), 2672–2681 (2004).
Zhao, X.-N. & Usdin, K. Timing of expansion of fragile X premutation alleles during intergenerational transmission in a mouse model of the fragile X-related disorders. Front. Genet. 9, 314 (2018).
Kacher, R. et al. Propensity for somatic expansion increases over the course of life in Huntington disease. Elife 10, e64674 (2021).
Campion, L. N. et al. Tissue-specific and repeat length-dependent somatic instability of the X-linked dystonia parkinsonism-associated CCCTCT repeat. Acta Neuropathol. Commun. 10(1), 1–16 (2022).
Acknowledgements
We thank the families who have participated in our studies and also the Fragile X team including students at the MIND Institute for their excellent collaboration.
Funding
This research was supported by the National Center for Advancing Translational Sciences, National Institutes of Health, through grant number P50 HD103526 and HD036071. The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Author information
Authors and Affiliations
Contributions
R.A. conceptualized the article and wrote the first draft. Y.H. carried out the molecular measures described in the study and was a major contributor to the manuscript. E.S. was involved in clinical data measurements and contributed to versions of the manuscript. B.H. and K.U. carried out measures of instability. B.J. conducted all the statistical analysis involved and reported in the manuscript. R.H. contributed to study data collection and critically reviewed the manuscript. F.T. conceptualized the study, oversaw all the molecular measures involved, critically reviewed and revised versions of the manuscript. All authors read, reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Aishworiya, R., Hwang, Y.H., Santos, E. et al. Clinical implications of somatic allele expansion in female FMR1 premutation carriers. Sci Rep 13, 7050 (2023). https://doi.org/10.1038/s41598-023-33528-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-33528-x
This article is cited by
-
Comment on: “Somatic CAG repeat instability in intermediate alleles of the HTT gene and its potential association with a clinical phenotype” by Ruiz de Sabando et al.
European Journal of Human Genetics (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.