Abstract
Upper extremity functioning is important for achieving independence in activities of daily living (ADL). A better understanding of relationships between different aspects of independence in ADL after spinal cord injury (SCI) and upper extremity functioning is required to guide rehabilitation practices. To determine which aspects of independence in ADL are correlated with upper extremity functioning in individuals with cervical or thoracic SCI. A total of 25 adults (mean age 58.4 years, 72% men) with established cervical or thoracic SCI were recruited. Independence in ADL was assessed by Spinal Cord Independence Measure (SCIM-III) and upper extremity functioning by kinematic measures (movement time, smoothness, and wrist angle during drinking task), grip strength, Upper Extremity Motor and Sensory Score, Box and Block Test (BBT), Action Research Arm Test (ARAT), and Upper Extremity Basic Data Set (ISCI-Hand and ISCI-Shoulder). Spearman correlation coefficients were used for data analyses. The SCIM-self-care subscale, particularly the feeding and dressing items, correlated moderately (r ≥ 0.5) with movement time and smoothness, grip strength, ARAT, BBT, and ISCI-Hand. The SCIM-respiration/sphincter subscale and the SCIM-mobility showed very low and low correlations with upper extremity assessments. However, at item level, respiration and bed/wheelchair mobility showed moderate correlations. Independence in self-care as domain and feeding/dressing, respiration and bed/wheelchair mobility as separate items were dependent on upper extremity functioning in individuals with cervical or thoracic SCI. Movement time and smoothness along with BBT, grip strength, ARAT, and ISCI-Hand can be used as indicators of independence in ADL. These findings can provide guidance to clinical practice in selection of upper extremity assessments in the context for ADL in individuals with SCI.
Similar content being viewed by others
Introduction
Spinal cord injury (SCI) results not only in impairment of the extremities, but also in impairment of the trunk below the neurological level of injury. The management of SCI relies on an in-depth understanding of impairments, based fundamentally on the American Spinal Injury Association (ASIA) examination and classification1,2,3. However, although ASIA is the gold standard for clinical assessment, it has been criticized for problems with the psychometric properties of sensory function assessment of incomplete injuries, lack of sensitivity regarding functioning, and exclusion of certain segments (upper cervical, thoracic, and sacral), which in turn leads to gaps in the understanding of impairment in, for example, trunk motor function4,5,6.
In the later phases after SCI, both clinicians and patients tend to focus on activity limitations and independence in activities of daily living (ADL) rather than impairments3,6. According to the International Classification of Functioning, Disability and Health (ICF), the domain of activity can be divided into activity capacity (capacity to perform tasks and activities) and activity performance (actual use of the upper extremity in ADL)7. Assessment in different ICF domains is recommended8 because specific impairments (e.g., neurological injury level or grade of completeness) are not directly indicative of expected limitations in activity3,6,9.
To improve the clinical relevance of activity performance assessment, the Spinal Cord Independence Measure (SCIM)10 was developed, and the revised version of the SCIM (SCIM-III)11,12 is now recommended as a primary, valid, and reliable measure, specific for individuals with SCI4,6. For activity performance and independence in real life, the upper extremity plays a fundamental role3,13 and its restoration is ranked as one of the main priorities for individuals with cervical SCI14,15. Upper extremity activity performance assessed with the SCIM self-care subscale in individuals with cervical SCI has been shown to correlate with upper extremity functioning (i.e., including body functions-strength and activity capacity)16. The SCIM self-care subscale has also been used as an indirect indicator of upper extremity activity17,18,19,20,21,22. Activity performance assessed with the SCIM correlates with movement smoothness of reach-to-grasp23. Upper extremity activity capacity can be explained (between 59 and 81% of the variation) by kinematic measures of wrist angle, movement time, and smoothness24.
Although previous studies have examined some aspects of independence in ADL in respect with upper extremity functioning16, a more detailed understanding of the relationships between independence in activities at different levels and upper extremity functioning assessed with both objective kinematic measures and clinical assessments is still lacking6,13. This knowledge would guide clinicians in selection of appropriate upper extremity assessments when the goal is to measure outcomes related to independence in daily life.
Thus, the aim of this study was to determine which aspects of independence in ADL are correlated with upper extremity functioning in individuals with cervical or thoracic SCI.
Methods
Study design and participants
In this observational cross-sectional study, participants were recruited from an outpatient clinic at Sahlgrenska University Hospital in Gothenburg, Sweden, in 2018. Inclusion criteria were: cervical or thoracic SCI with grade of severity A, B, C, or D according to the ASIA Impairment Scale (AIS)1,2, injury present for more than 1 year, age ≥ 18 years, limited independence (SCIM-total score less than 100), and ability to use the upper extremity to some degree for everyday task such as drinking from a glass. Exclusion criteria were inability to communicate in Swedish and other psychological, neurological, or musculoskeletal comorbidities that could affect upper extremity use in ADL. The neurological level of the SCI was determined according to the International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI) developed by ASIA and the completeness of injury according to the ASIA Impairment Scale (AIS; A-E)1,2. This study was performed in accordance with the Declarations of Helsinki and approved by the Swedish Ethical Review Authority (registration number 408-17). All participants gave informed, written consent before recruitment in the study. The study was registered at researchweb.org (https://www.researchweb.org/is/vgr/project/260901) prior to participant enrollment. The reporting of this study conforms to the Strengthening the Reporting of Observational studies in Epidemiology (STROBE) statement25.
Independence in ADL
Activity performance in the form of independence in ADL was assessed using SCIM-III11,12. SCIM-III includes 19 items divided into three subscales: (i) Self-care (SCIM-self-care), (ii) Respiration and Sphincter management (SCIM-respiration/sphincter) (iii) Mobility (SCIM-mobility). A score of 100 indicates independence in all SCIM-III areas. The SCIM-self-care, with a maximum score of 20, includes 6 items assessing feeding, upper and lower body bathing as well as dressing, and grooming. Both the SCIM-respiration/sphincter subscale (respiration, sphincter management-bladder and bowel, toileting) and the SCIM-mobility subscale (bed mobility; transfers and mobility indoors and outdoors) include 9 items with a maximum score of 40 points.
Upper extremity functioning
The assessments of upper extremity covered different aspects of functioning according to the ICF framework7. The ASIA Upper Extremity Motor Score, the ASIA Upper Extremity Sensory Score, the grip strength as well as the kinematic variables of movement time (MT), number of movement units (NMU) also called smoothness, and wrist dorsiflexion angle covered the ICF domain of body functions. The Action Research Arm Test (ARAT), the International Spinal Cord Injury Upper Extremity Basic Data Set Form, and the Box and Block Test (BBT) covered the ICF domain of activity. For all assessments, data from the most affected upper extremity were included in the analysis. ARAT was used to determine the most affected arm, and when ARAT scores were equal in both arms, the pre-injury nondominant arm was considered the most affected arm.
Clinical assessment of body functions
Grip strength was measured with a Jamar hydraulic hand dynamometer with analog readout in sitting position with elbow flexed 90 degrees and wrist between 0 and 30 dorsiflexion. The gravity of the dynamometer was supported by the tester or table. An average of three trials was calculated26. Grip strength has been shown to be associated with SCIM-total score27. According to the ASIA examination, strength in key muscles of the upper extremity was assessed with the manual muscle test with grades between 0 and 5 and summarized for each upper extremity in the Upper Extremity Motor Score with a maximum of 25 points1,2. Sensation in key points (according to the ASIA examination) in the upper extremity was rated on a scale ranging from 0 to 2 and summarized for each upper extremity in the Upper Extremity Sensory Score with a maximum of 32 points1,2. The grade of completeness was also assessed according to ASIA, and the data for this were derived from the medical records.
Kinematic measures of body functions
For the kinematic analysis of the standardized drinking task, a 5-camera optoelectronic motion capture system (Pro Reflex Motion Capture System, MCU240 Hz, Qualisys AB, Gothenburg, Sweden) was used28,29. The infrared light signals emitted by the cameras reflected by spherical markers placed at anatomical landmarks on the upper extremities (third metacarpophalangeal joint, styloid process of ulna, lateral epicondyle, upper middle part of acromion), forehead (notch between the eyebrows), upper part of sternum, and on a hard-plastic drinking glass (Fig. 1). The marker positions in 3D space were automatically identified and transferred for offline analysis using MATLAB (The Math Works Inc) software. The kinematic data were filtered using a 6 Hz second-order Butterworth filter in the forward and backward directions, resulting in a zero-phase distortion and fourth-order filtering before analysis. The drinking glass containing 100 ml of water was placed 30 cm from the edge of the table at the midline of the body (about 75% of the arm length). The standardized sitting position comprised approximately 90° knee, hip, and elbow flexion, the wrist in line with the edge of the table, and the back resting against the back of the chair. Trunk movement was not constrained and the participants using wheelchair were allowed to sit in their own chairs30 (Fig. 1). Participants were instructed to unimanually perform the task 8–10 times in a convenient speed as naturally as possible. For statistical analysis the mean of all performed trials were used31.
The drinking task comprised five phases: (i) reaching (including grasping), (ii) forward transport of the glass to the mouth, (iii) drinking, (iv) backward transport of the glass to the table, (v) and returning the hand to the starting position28,29. Movement time (MT) was measured for the entire drinking task including all movement phases28,29. The start and end of the movement was detected when the velocity of the hand marker exceeded or returned to 2% of the maximum velocity28,29. The number of movement units (NMU) was calculated by the tangential velocity profile of the hand marker for all transport phases except the drinking phase. A movement unit was defined as the difference between a local minimum and the next maximum velocity value that exceeded the amplitude limit of 20 mm/s, with a time between two consecutive peaks of at least 150 ms28,29. The NMU captures the repeated sub-accelerations and sub-decelerations during movement performance and can be defined as movement smoothness. The minimum NMU for the drinking task is 4 (one unit for each movement phase) and a higher NMU indicates a less smooth movement30. The maximum joint angle of dorsiflexion of the wrist was determined by the angle between the vectors connecting the hand and wrist as well as the elbow and wrist markers and was calculated for the reaching and forward transport phase28,29.
Clinical assessments of activity capacity
Upper extremity activity capacity was assessed using the ARAT32. The ARAT includes 19 items hierarchically organised into 4 subscales (grasp, grip, pinch, and gross movement)32. The sum score ranges from 0 to 57, with higher scores indicating better performance32. The ARAT has been increasingly used in individuals with SCI33,34 and has showed moderate to good correlation with kinematic variables of movement time, smoothness, and maximum wrist angle24.
Gross manual dexterity was quantified using the BBT. The test score was the number of wooden blocks (2.5 cm) moved unimanually over a wooden divider from one compartment to another within one minute. The BBT is a reliable and simple assessment that measures the efficiency of movement regardless of the compensatory strategies used35,36,37,38.
The hand and shoulder classification scales from the International Spinal Cord Injury Upper Extremity Basic Data Set Form39, version 1.140, developed by the International Spinal Cord Society (ISCoS), were used. The "Basic hand-upper extremity function" (ISCI-Hand) uses a 5-level scoring system based on the voluntary motor function of the upper extremity muscles required to perform common arm and hand movements such as reaching, grasping and manipulation39,40. The "Shoulder function classification" (ISCI-Shoulder) uses a 4-level scoring system based on observed shoulder and upper extremity function during arm positioning39,40. The ISCI Upper Extremity Basic Data Set Form has been tested and has shown excellent inter-rater reliability for evaluating cervical SCI41. ISCI-Hand has shown moderate correlation with kinematic measure of wrist angle24.
Statistical analysis
Statistical analyses were performed using the IBM Statistical Package for Social Sciences™ (SPSS, version 24). Descriptive statistics were calculated for demographic and clinical characteristics. The two-sided significance level (alpha value) was set at p < 0.05. When both arms could perform the drinking task, data only from the more-affected arm (i.e., less total ARAT score) or the non-dominant arm was used. The preliminary analyses of included outcome measures showed non-normal distribution of all upper extremity assessments except for BBT. Therefore, Spearman correlation coefficient was used for correlation analysis between independence in ADL (i.e., SCIM-total, SCIM subscales, and each item) and upper extremity assessments (kinematic measures, clinical scales). The strength of correlation was interpreted as 0.00–0.25 (very low), 0.26–0.49 (low), 0.50–0.69 (moderate), 0.70–0.89 (high), and 0.90–1.00 (very high)42.
Ethics approval and consent to participate
The study was approved by the Swedish Ethical Review Authority (registration number 408-17). We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research.
Results
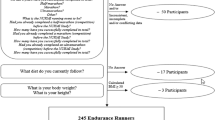
Of the 411 medical records screened, 216 individuals with SCI were eligible for the current study. Of those who responded to the telephone call (n = 134), 32 were interested in participating and 25 met the inclusion criteria and were included in the study24. The mean age of the study group was 58.4 years (range 44.6–72.2), 72% were men, and the mean time since injury was 17.5 (range 2.1–32.9) years. Of all participants, 80% had a traumatic injury and 68% had a cervical injury. The majority had motor complete injury (56%), although all grades of severity (injury level and completeness) were included except AIS E (Table 1). Four individuals with thoracic injuries and two individuals with cervical incomplete injury had full points in arm functioning according to the ARAT total score. Participants with incomplete AIS type D injuries all but one had a cervical SCI (Table 1).
According to the inclusion criteria, none of the participants was fully independent in ADL as assessed by the SCIM total score. Total SCIM scores ranged from 41.8 to 84.82 (mean 63.3, median 65). The scores of the SCIM subscales (self-care, respiration/sphincter, mobility) and the results of all upper extremity assessments are shown in Table 2.
The Spearman correlation coefficients between the upper extremity assessments and the total SCIM score and the SCIM sub scores are reported in Table 3. In the ICF domain of body functions, kinematic measures of smoothness and movement time (r ≥ 0.6) as well as grip strength (r ≥ 0.5) showed moderate correlations with SCIM-self-care. In the ICF domain of activity, clinical assessments of ARAT, BBT, and ISCI-Hand showed moderate correlations (r ≥ 0.5). Correlations with SCIM-respiration/sphincter subscale were non-significant and low or very low. For the SCIM-mobility subscale, statistically significant but low correlations (r 0.3–0.5) were observed for grip strength and ISCI-Hand. SCIM-total showed low but statistically significant correlations with the kinematic measure of movement time and the ISCI-Hand classification score.
Respective Spearman correlation coefficients between the upper extremity assessments and the total SCIM score and the SCIM sub scores only in participants with cervical SCI (n = 17) are reported in the Supplementary Table 1. A separate statistical analysis with thoracic SCI alone lacked statistical power due to the small (n = 8) sample size.
Table 4 shows the correlation coefficients between the upper extremity assessments and each item of the SCIM-self-care subscale. Moderate and high correlations were observed for feeding and for the upper and lower body dressing items with the kinematic measures of movement time and smoothness, grip strength, ARAT, and BBT. The Upper Extremity Motor Score and the ISCI-Hand showed moderate correlations with the feeding and upper body dressing items. The kinematic measure of wrist angle, the Upper Extremity Sensory Score, and the ISCI-Shoulder showed moderate correlations with dressing of the upper body alone. The upper body dressing correlated with all upper extremity functioning assessments. The SCIM self-care items of bathing and grooming showed statistically significant but low correlations with some upper extremity assessments.
Table 5 shows the correlation coefficients between the upper extremity assessments and each item of the SCIM-respiration/sphincter subscale. The kinematic measures of movement time and smoothness as well as BBT showed moderate correlations with the respiration item. Movement time was also moderately correlated with toilet use item. The bladder and bowel items had non-significantly low or very low correlations with upper extremity functioning.
As for the SCIM-mobility subscale, the bed mobility and wheelchair mobility items showed moderate correlations with the kinematic measure of movement time (Table 6). Moderate correlations were also found between smoothness of movement, grip strength, ARAT, BBT, ISCI-Hand, and the bed mobility item. ISCI-Hand also correlated moderately with ground wheelchair mobility.
Discussion
The results of this cross-sectional study showed that independence in activities of daily living and, especially, independence in self-care correlated with upper extremity functioning as measured in the ICF domain of body functions and activity. The SCIM-self-care subscale and, especially the feeding and dressing items correlated with kinematic measures of movement time and smoothness, grip strength, ARAT, BBT, and ISCI-Hand. Correlations with the SCIM-respiration/sphincter subscale were low and not statistically significant. However, at the item level, moderate correlations were observed for movement time, smoothness, and BBT with respiration item and for movement time with toilet use item. The SCIM-mobility subscale showed low but statistically significant correlations with grip strength and ISCI-Hand. At the item level, moderate correlations were observed for the items bed mobility and wheelchair transfers with movement time, smoothness, grip strength, ARAT, BBT, and ISCI-Hand.
Our results showed that independence in self-care, rather than independence in mobility and in respiration and sphincter management, correlated with upper extremity functioning in individuals with cervical or thoracic SCI. This finding is in line with previous research that mainly included individuals with tetraplegia, even though the strength of correlations varies between different study populations16,20,21,43. One possible explanation for these differences could be the degree of independence in ADL in each specific study population. For example, correlations between upper extremity functioning and the SCIM-self-care subscale were stronger in studies that included only participants with tetraplegia, in which the participants’ degree of independence in ADL was lower16,44, compared with studies such as ours that also included participants with paraplegia20, in which the participants’ degree of independence was higher.
In the current study, the SCIM-self-care items of feeding and dressing showed the strongest correlations with upper extremity functioning. Similar results were also reported by Rudhe et al.16, who found that the upper body dressing and grooming items correlated with motor score and hand capacity tests16. In addition to the self-care items, the bed and wheelchair mobility items also showed moderate correlations with upper extremity functioning in the current study. This finding is consistent with a study in individuals with cervical complete or incomplete SCI after hand surgery, in which the feeding and wheelchair mobility items were selected as indicators of functional independence45. On the SCIM-respiration/sphincter subscale, at the item level, our study showed that the independence in respiration item correlated significantly with several upper extremity assessments. This interesting finding is clinically relevant considering the role of muscles stabilizing the shoulder girdle, such as the latissimus dorsi and serratus muscles, in respiration.
In the current study, kinematic measures were included to objectively characterize and quantify upper extremity movements during a purposeful task. Among the upper extremity assessments, measures of movement time and smoothness showed the strongest correlations with the SCIM-self-care subscale. In addition, at the item level, independence in feeding, dressing, wheelchair/bed mobility, respiration and toilet use correlated with movement time and smoothness. These results are novel and show that independence in these activities is closely related to the smoothness of arm movements and the time required to perform a standardized everyday task, such as drinking from a glass. While movement time is easily captured in clinical settings, movement smoothness is a measure that requires more advanced camera-based analysis. Previous research has shown strong correlation between movement time and smoothness24. This suggests that standardized, timed everyday tasks, such as the drinking task, could probably be used as a potential indicator of independence in ADL.
Grip strength is another simple clinical test that showed moderate correlation with independence in self-care and at the item level with independence in feeding, dressing, and mobility in bed. Grip strength has been previously reported to correlate with SCIM-total score27. In the ICF domain of activity, the clinical assessments BBT, ARAT, and ISCI-Hand correlated moderately with independence in self-care and at the item level with independence in feeding, dressing, mobility in bed, and respiration. Given these results, all clinical assessments that showed moderate correlations with independence in ADL can be recommended as clinical proxies for independence in ADL. Considering that all participants in this study were able to move at least one block on the BBT, while four participants scored 0 on the grip strength test, and that the ARAT requires a longer administration time, the BBT could be recommended as a quick and easy clinical assessment after SCI, especially if the focus is on independence in ADL and not on movement quality or strategy used36,46.
Strengths and limitations
In this study, the ICF framework was used to guide the selection of upper extremity assessments, which strengthens the study by providing clinicians with a more nuanced picture of the correlations across different functioning domains and measures. Most of the assessments used in the current study are well established, which increases the clinical validity of the results. Our approach of examining independence at the item level can also be considered a strength, as it provides further insight into the different domains and categories of independence in ADL. When item scores are summed in the SCIM total score or subscale scores, some information is lost16. In addition, our study is strengthened by kinematic analysis during a daily task, which adds a novel perspective to the results in relation to independence30.
The results in this study can only be generalized to a population of individuals with complete or incomplete SCI at the cervical or thoracic level with a relatively high degree of independence (mean SCIM score of 63 out of 100). The study sample was heterogeneous and included both cervical and thoracic injuries with varying completeness and severity of injury, which may be considered a limitation when the focus is on impairment. However, the focus of the current study was on independence in ADL and upper extremity functioning after SCI. Therefore, dependence in ADL rather than neurological level was selected as one of the inclusion criteria. Based on these criteria, 8 participants with thoracic injuries were also included in the study because they had a lower SCIM total score than 100. Of these 8 participants with decreased SCIM due to thoracic injuries, 4 had limitations in upper extremity functioning. This is not surprising given the importance of trunk stabilization to upper extremity motor control47. Future studies with larger samples are needed to determine the extent to which upper extremity functioning may be limited in individuals with thoracic SCI.
Conclusions
Independence in self-care including feeding, dressing as well as respiration, and mobility in bed and wheelchair correlates with upper extremity functioning in individuals with cervical or thoracic SCI. In clinical settings, grip strength, BBT, ARAT, and ISCI-Hand as well as timed tests of functional tasks, such as drinking, can be used as indicators of independence in ADL. This new, deeper understanding of upper extremity functioning in the context of independence can guide the selection of assessments and rehabilitation interventions in clinical practice.
Data availability
The data that support the findings of this study are available via corresponding author on a reasonable request.
Abbreviations
- ADL:
-
Activities of Daily Living
- ASIA:
-
American Spinal Injury Association
- AIS:
-
ASIA Impairment scale
- ARAT:
-
Action Research Arm Test
- BBT:
-
Box and Block Test
- BMI:
-
Body Mass Index
- ICF:
-
International Classification of Functioning, Disability and Health
- ISCI:
-
International Spinal Cord Injury Upper Extremity Data Set
- ISCI-Hand:
-
Basic Hand variable of the International Spinal Cord Injury Upper Extremity Data Set
- ISCI-Shoulder:
-
Shoulder variable of the International Spinal Cord Injury Upper Extremity Data Set
- ISCoS:
-
International Spinal Cord Society
- ISNCSCI:
-
International Standards for Neurological Classification of Spinal Cord Injury
- NMU:
-
Number of Movement Units
- MT:
-
Movement Time
- SCI:
-
Spinal Cord Injury
- SCIM-III:
-
Spinal Cord Independence Measure version III
- SCIM-self-care:
-
Spinal Cord Independence Measure self-care subscale
- SCIM-respiration/sphincter:
-
Spinal Cord Independence Measure respiration and sphincter management subscale
- SCIM-mobility:
-
Spinal Cord Independence Measure mobility subscale
- SCIM-total:
-
Spinal Cord Independence Measure total score
- STROBE:
-
Strengthening the Reporting of Observational studies in Epidemiology
- UEMS:
-
Upper Extremity Motor Score
- UESS:
-
Upper Extremity Sensory Score
References
Kirshblum, S. C. et al. International standards for neurological classification of spinal cord injury (revised 2011). J. Spinal Cord Med. 34, 535–546 (2011).
Kirshblum, S. C. et al. Reference for the 2011 revision of the International Standards for Neurological Classification of Spinal Cord Injury. J. Spinal Cord Med. 34, 547–554 (2011).
Outcomes Following Traumatic Spinal Cord Injury: Clinical practice guidelines for health-care professionals. J. Spinal Cord Med. 23, 289–289 (2000)
Alexander, M. S. et al. Outcome measures in spinal cord injury: Recent assessments and recommendations for future directions. Spinal Cord 47, 582–591 (2009).
Hales, M., Biros, E. & Reznik, J. E. Reliability and validity of the sensory component of the international standards for neurological classification of spinal cord injury (ISNCSCI): A systematic review. Top Spinal Cord Inj. Rehabil. 21, 241–249 (2015).
Anderson, K. et al. Functional recovery measures for spinal cord injury: An evidence-based review for clinical practice and research. J. Spinal Cord Med. 31, 133–144 (2008).
Organization, W. H. International classification of functioning, disability and health: ICF. (World Health Organization, 2001).
Burridge, J. et al. A systematic review of international clinical guidelines for rehabilitation of people with neurological conditions: What recommendations are made for upper limb assessment?. Front. Neurol. 10, 567. https://doi.org/10.3389/fneur.2019.00567 (2019).
Steeves, J. D. et al. Guidelines for the conduct of clinical trials for spinal cord injury (SCI) as developed by the ICCP panel: Clinical trial outcome measures. Spinal Cord 45, 206–221. https://doi.org/10.1038/sj.sc.3102008 (2007).
Catz, A., Itzkovich, M., Agranov, E., Ring, H. & Tamir, A. SCIM–spinal cord independence measure: A new disability scale for patients with spinal cord lesions. Spinal Cord 35, 850–856 (1997).
Almeida, C., Coelho, J. N. & Riberto, M. Applicability, validation and reproducibility of the Spinal Cord Independence Measure version III (SCIM III) in patients with non-traumatic spinal cord lesions. Disabil. Rehabil. 38, 2229–2234. https://doi.org/10.3109/09638288.2015.1129454 (2016).
Bluvshtein, V. et al. SCIM III is reliable and valid in a separate analysis for traumatic spinal cord lesions. Spinal Cord 49, 292–296. https://doi.org/10.1038/sc.2010.111 (2011).
Starkey, M. L. & Curt, A. in Neurorehabilitation Technology, Second Edition 107–138 (2016).
Snoek, G. J., Mj, I. J., Hermens, H. J., Maxwell, D. & Biering-Sorensen, F. Survey of the needs of patients with spinal cord injury: Impact and priority for improvement in hand function in tetraplegics. Spinal Cord 42, 526–532. https://doi.org/10.1038/sj.sc.3101638 (2004).
Anderson, K. D. Targeting recovery: Priorities of the spinal cord-injured population. J Neurotrauma 21, 1371–1383. https://doi.org/10.1089/neu.2004.21.1371 (2004).
Rudhe, C. & van Hedel, H. J. A. Upper extremity function in persons with tetraplegia: Relationships between strength, capacity, and the spinal cord independence measure. Neurorehabil. Neural Repair 23, 413–421. https://doi.org/10.1177/1545968308331143 (2009).
Rudhe, C., Albisser, U., Starkey, M. L., Curt, A. & Bolliger, M. Reliability of movement workspace measurements in a passive arm orthosis used in spinal cord injury rehabilitation. J. Neuro Eng. Rehabil. 9, 37. https://doi.org/10.1186/1743-0003-9-37 (2012).
Kalsi-Ryan, S. et al. The graded redefined assessment of strength sensibility and prehension version 2 (GV2): Psychometric properties. J. Spinal Cord Med. 42, 149–157. https://doi.org/10.1080/10790268.2019.1616950 (2019).
Popovic, M. R. et al. Functional electrical stimulation therapy of voluntary grasping versus only conventional rehabilitation for patients with subacute incomplete tetraplegia: A randomized clinical trial. Neurorehabili. Neural Repair 25, 433–442. https://doi.org/10.1177/1545968310392924 (2011).
Marino, R. J., Kern, S. B., Leiby, B., Schmidt-Read, M. & Mulcahey, M. J. Reliability and validity of the capabilities of upper extremity test (CUE-T) in subjects with chronic spinal cord injury. J. Spinal Cord Med. 38, 498–504. https://doi.org/10.1179/2045772314Y.0000000272 (2015).
Dent, K. et al. Evaluation of the capabilities of upper extremity test (CUE-T) in children with tetraplegia. Top Spinal Cord Inj. Rehabil. 24, 239–251. https://doi.org/10.1310/sci2403-239 (2018).
Lu, X., Battistuzzo, C. R., Zoghi, M. & Galea, M. P. Effects of training on upper limb function after cervical spinal cord injury: A systematic review. Clin. Rehabil. 29, 3–13. https://doi.org/10.1177/0269215514536411 (2015).
Cacho, E. W., de Oliveira, R., Ortolan, R. L., Varoto, R. & Cliquet, A. Jr. Upper limb assessment in tetraplegia: Clinical, functional and kinematic correlations. Int. J. Rehabil. Res. 34, 65–72. https://doi.org/10.1097/MRR.0b013e32833d6cf3 (2011).
Lili, L., Sunnerhagen, K. S., Rekand, T. & Alt Murphy, M. Associations between upper extremity functioning and kinematics in people with spinal cord injury. J. Neuroeng. Rehabil. 18, 147. https://doi.org/10.1186/s12984-021-00938-9 (2021).
von Elm, E. et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. J. Clin. Epidemiol. 61, 344–349. https://doi.org/10.1016/j.jclinepi.2007.11.008 (2008).
Mathiowetz, V., Rennells, C. & Donahoe, L. Effect of elbow position on grip and key pinch strength. J. Hand Surg. 10, 694–697. https://doi.org/10.1016/S0363-5023(85)80210-0 (1985).
Neto, F. R. et al. Handgrip strength cutoff points for functional independence and wheelchair ability in men with spinal cord Injury. Top Spinal Cord Inj Rehabil. 27, 60–69 (2021).
Alt, M. M., Willen, C. & Sunnerhagen, K. S. Kinematic variables quantifying upper-extremity performance after stroke during reaching and drinking from a glass. Neurorehabil. Neural Repair 25, 71–80. https://doi.org/10.1177/1545968310370748 (2011).
Au-Alt, M. M., Au-Murphy, S., Au-Persson, H. C., Au-Bergström, U.-B. & Au-Sunnerhagen, K. S. Kinematic analysis using 3D motion capture of drinking task in people with and without upper-extremity impairments. JoVE 5, e57228 (2018).
Lili, L., Sunnerhagen, K. S., Rekand, T. & Alt Murphy, M. Quantifying an upper extremity everyday task with 3D kinematic analysis in people with spinal cord injury and non-disabled controls. Front. Neurol. 12, 755790. https://doi.org/10.3389/fneur.2021.755790 (2021).
Frykberg, G. E., Grip, H. & Alt Murphy, M. How many trials are needed in kinematic analysis of reach-to-grasp?—A study of the drinking task in persons with stroke and non-disabled controls. J. Neuro Eng. Rehabil. 18, 101. https://doi.org/10.1186/s12984-021-00895-3 (2021).
Yozbatiran, N., Der-Yeghiaian, L. & Cramer, S. C. A standardized approach to performing the action research arm test. Neurorehabil. Neural Repair 22, 78–90. https://doi.org/10.1177/1545968307305353 (2007).
Kowalczewski, J., Chong, S. L., Galea, M. & Prochazka, A. In-home tele-rehabilitation improves tetraplegic hand function. Neurorehabil. Neural Repair 25, 412–422. https://doi.org/10.1177/1545968310394869 (2011).
Harvey, L. A., Dunlop, S. A., Churilov, L. & Galea, M. P. Early intensive hand rehabilitation is not more effective than usual care plus one-to-one hand therapy in people with sub-acute spinal cord injury ('Hands On’): A randomised trial. J. Physiother. 63, 197–204. https://doi.org/10.1016/j.jphys.2017.08.005 (2017).
Cortes, M. et al. Improved grasp function with transcranial direct current stimulation in chronic spinal cord injury. NeuroRehabil. 41, 51–59. https://doi.org/10.3233/nre-171456 (2017).
Mathiowetz, V., Volland, G., Kashman, N. & Weber, K. Adult norms for the box and block test of manual dexterity. Am. J. Occup. Therapy 39, 386–391. https://doi.org/10.5014/ajot.39.6.386 (1985).
Platz, T. et al. Reliability and validity of arm function assessment with standardized guidelines for the Fugl-Meyer test, action research arm test and box and block test: A multicentre study. Clin. Rehabil. 19, 404–411. https://doi.org/10.1191/0269215505cr832oa (2005).
Trumbower, R. D., Hayes, H. B., Mitchell, G. S., Wolf, S. L. & Stahl, V. A. Effects of acute intermittent hypoxia on hand use after spinal cord trauma: A preliminary study. Neurology 89, 1904–1907. https://doi.org/10.1212/wnl.0000000000004596 (2017).
Biering-Sørensen, F. et al. International spinal cord injury upper extremity basic data set. Spinal Cord 52, 652–657. https://doi.org/10.1038/sc.2014.87 (2014).
Biering-Sørensen, F. et al. International spinal cord injury upper extremity basic data set version 1.1. Spinal Cord 53, 890. https://doi.org/10.1038/sc.2015.101 (2015).
Tongprasert, S., Namchandee, A., Sotthipoka, K. & Kammuang-Lue, P. Reliability of the international spinal cord injury upper extremity basic data set. Spinal Cord 56, 913–918. https://doi.org/10.1038/s41393-018-0154-3 (2018).
Ugarte, M. D. Vol. 32 320 (Abingdon: Taylor & Francis Ltd, Abingdon, 2005).
Velstra, I. M. et al. Prediction and stratification of upper limb function and self-care in acute cervical spinal cord injury with the graded redefined assessment of strength, sensibility, and prehension (GRASSP). Neurorehabil. Neural Repair 28, 632–642. https://doi.org/10.1177/1545968314521695 (2014).
Kalsi-Ryan, S. et al. The graded redefined assessment of strength sensibility and prehension: Reliability and validity. J. Neurotrauma 29, 905–914. https://doi.org/10.1089/neu.2010.1504 (2012).
Dengler, J. et al. Evaluation of functional independence in cervical spinal cord injury: Implications for surgery to restore upper limb function. J. Hand Surg. 46, 621. https://doi.org/10.1016/j.jhsa.2020.10.036 (2021).
Platz, T. et al. Reliability and validity of arm function assessment with standardized guidelines for the fugl-meyer test, action research arm test and box and block test: A multicentre study. Clin. Rehabil. 19, 404–411. https://doi.org/10.1191/0269215505cr832oa (2005).
Peeters, L. H. C., de Groot, I. J. M. & Geurts, A. C. H. Trunk involvement in performing upper extremity activities while seated in neurological patients with a flaccid trunk-A review. Gait Posture 62, 46–55. https://doi.org/10.1016/j.gaitpost.2018.02.028 (2018).
Acknowledgements
The authors would like to thank all participants who volunteered to participate in this study.
Funding
Open access funding provided by University of Gothenburg. This work was supported by the Swedish Society for Medical Research (S19-0074), the Swedish state under an agreement between the Swedish government and the county councils, the ALF agreement (ALFGBG-718711, ALFGBG-879111, ALFGBG-932697), Promobilia, Norrbacka-Eugeniastiftelsen (802/19, 803/20), the local Research and Development Board for Gothenburg and Södra Bohuslän (VGFOUGSB-868941), Sahlgrenska University Hospital Research Foundation (SU-793851).
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to concept, design, and interpretation of data. LL conducted the data collection, performed data analysis, and drafted the manuscript. MAM contributed to the data collection, analysis and drafting. MAM, TK and KSS revised the manuscript critically for intellectual content. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lili, L., Sunnerhagen, K.S., Rekand, T. et al. Independence and upper extremity functioning after spinal cord injury: a cross-sectional study. Sci Rep 13, 3148 (2023). https://doi.org/10.1038/s41598-023-29986-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-29986-y
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.