Abstract
The increase in neuronal activity induced by a single seizure is supported by a rise in the cerebral blood flow and tissue oxygenation, a mechanism called neurovascular coupling (NVC). Whether cerebral and systemic hemodynamics are able to match neuronal activity during recurring seizures is unclear, as data from rodent models are at odds with human studies. In order to clarify this issue, we used an invasive brain and systemic monitoring to study the effects of chemically induced non-convulsive seizures in sheep. Despite an increase in neuronal activity as seizures repeat (Spearman’s ρ coefficient 0.31, P < 0.001), ictal variations of cerebral blood flow remained stable while it progressively increased in the inter-ictal intervals (ρ = 0.06, P = 0.44 and ρ = 0.22; P = 0.008). We also observed a progressive reduction in the inter-ictal brain tissue oxygenation (ρ = − 0.18; P = 0.04), suggesting that NVC was unable to compensate for the metabolic demand of these closely repeating seizures. At the systemic level, there was a progressive reduction in blood pressure and a progressive rise in cardiac output (ρ = − 0.22; P = 0.01 and ρ = 0.22; P = 0.01, respectively), suggesting seizure-induced autonomic dysfunction.
Similar content being viewed by others
Introduction
Seizures, including non-convulsive seizures (NCSz), cause a dramatic increase in cortical neuronal activity, metabolism and oxygen consumption that is normally supported by a rise in regional cerebral blood flow (CBF)1, owing to the mechanisms of neurovascular coupling (NVC)2. The effect of recurrent seizures on local and systemic hemodynamic response, and in particular the behavior of NVC to repeated solicitation, however, has not been widely investigated. It is also known that seizures affect blood–brain barrier (BBB) integrity3,4,5. A recent study in a rodent model of recurrent seizures showed that BBB permeability changes and pericytes dysfunction were associated with a progressive reduction in vessels vasodilation, probably because of a disruption of the neurovascular unit6. Although human BBB disruption was demonstrated in vitro3,7, the effects of recurrent seizures on the cerebrovascular response remain a matter a discussion since invasive brain monitoring is justifiable only in pathologic conditions which are sources of confounding factors. For example, during seizures, an abnormal neurovascular coupling, associated with a BBB dysfunction, was shown in a patient presenting a subarachnoid hemorrhage8 which can independently alter the NVC9. Moreover, this progressive reduction in vasodilation was not confirmed by human studies that, instead, showed an increase of CBF in case of non-convulsive status epilepticus10,11,12. The reasons for the discrepancy between animals and humans studies are unclear but might be related to the differences in the models (induced seizures in healthy animals vs. spontaneous seizures in brain injured patients) and to the known limits of rodent models to reproduce human pathology if compared to gyrencephalic mammalian brains16. Furthermore, little is known about the effect of recurrent NCSz on systemic hemodynamics, although a flattening of seizure-induced mean arterial pressure (MAP) variations has been observed13,14 possibly due to a progressive alteration in the function of the autonomic nervous system15. Finally, whether the hypothesized impairment in NVC and in systemic hemodynamic induced by recurrent seizures leads to a reduction in CBF and brain tissue oxygenation remains unknown.
In this study, we aimed to study the cerebral hemodynamic and systemic cardiovascular effects of repeated chemically-induced NCSz in a healthy ovine model, as sheep is considered a promising surrogate for modelling human brain diseases16 and it has already been employed as model for epilepsy17,18 and to study brain microcirculation19,20. Moreover, a sheep model offers numerous technical and theoretical advantages over small animals since it provides a unique opportunity for the transfer of techniques (neuromonitoring and neurosurgical) between animals and humans, making the results more applicable in a clinical setting17.
Results
The study included 7 sheep (median weight: 29 [range 26–35] kgs). Systemic parameters at time of penicillin application are summarized in Table 1. A median of 27 [range: 8–109] seizures were induced per animal, with a latency of 85 [42–150] min and after a cumulative dose of 1 × 106 [0.5–1.6 × 106] UI of penicillin (Table 1). Figures 1 and 2 show local cerebral and systemic cardiovascular effects of seizures repetition.
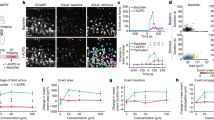
Variation of ictal and interictal cerebral parameters with seizure recurrence. Eγ EEG gamma envelope power, CBFv Cerebral blood flow velocity, PbtO2 Partial tissue oxygen pressure. For inter-ictal and ictal peak calculation please refer to the text. In abscissa, the seizure rank and the number of animals whose seizure was available for each rank. Data are presented as median ± median absolute deviation. The indicated Spearman’s rank-order correlation coefficient ρ and the corresponding p value are calculated using all available seizures. An increase in time was recorded for Eγ (ρ = 0.31, P < 0.001; (a) and ictal PbtO2 change (ρ = 0.21, P = 0.01; (c) whereas ictal CBFv change was not influenced by seizure recurrence (b). A positive statistically significant trend was noticed in the inter-ictal CBFv change as seizures recurred (ρ = 0.22, P < 0.01; (d). Conversely inter-ictal PbtO2 decreased (ρ = − 0.18, P = 0.04; (e).
Variation of inter-ictal and ictal systemic parameters with seizure recurrence. MAP Mean arterial pressure, HR Heart rate, COEST Cardiac output estimation using the Liljestrand–Zander method. For inter-ictal and ictal peak calculation please refer to the text. In abscissa, the seizure rank and the number of animals whose seizure was available for each rank. Data are presented as median ± median absolute deviation. The indicated Spearman’s rank-order correlation coefficient ρ and the corresponding p value are calculated using all available seizures. A non-significant decrease in the median value of both ictal MAP (ρ = − 0.14, P = 0.11; (a) and ictal HR (ρ = − 0.17, P = 0.06; (b) occurred while the ictal COEST response was not influenced by seizure recurrence (c). The inter-ictal MAP value significantly decreased as seizures recurred (ρ = − 0.22, P = 0.01; (d). Conversely a positive trend was observed for the inter-ictal COEST (ρ = 0.22, P = 0.01, (f).
Between seizures, periodic inter-ictal spikes were recorded with a stable median frequency of 0.8 [IQR 0.6–1.1] Hz.
Cerebral measures
The ictal Eγ increased of a median of + 11 [7–17] % of the pre-ictal value and a statistically significant positive trend was noticed with recurring seizures (Spearman’s ρ coefficient 0.31, P < 0.001, Fig. 1a). An increase in the ictal CBFv was recorded in 79/133 (60%) of seizures. The median ictal variation of CBFv was + 6 [− 6 to + 15] % of the pre-ictal value, but we did not observe a significant variation with recurring seizures (ρ = 0.06; P = 0.44; Fig. 1b). An ictal increase in PbtO2 occurred in 75/135 (55%) of seizures. The median ictal variation was + 0.3 [− 0.4 to + 0.7] % and it significantly increased with recurring seizures (ρ = 0.21; P = 0.01; Fig. 1c). Regarding the variation of the inter-ictal measures with recurring seizures, we observed a progressive increase in the inter-ictal CBFv and a progressive decrease in the inter-ictal PbtO2 values (ρ = 0.22; P = 0.008 and − 0.18; P = 0.04, respectively, Fig. 1d,e).
Systemic measures
After an initial increase until the eighth seizure, the ictal MAP and HR variations both showed a progressive decrease as seizures recurred, yielding an overall negative, albeit non-significant, trend (ρ = − 0.14; P = 0.11 and − 0.17; P = 0.06, respectively; Fig. 2a,b). The ictal COEST variation was more heterogonous and there was no significant correlation with seizure recurrence (Fig. 2c).
The inter-ictal MAP and COEST showed an opposite behavior, with a clear negative (ρ = − 0.22; P = 0.01) and a positive (ρ = 0.22; P = 0.01) correlation, respectively, as seizures recurred (Fig. 2d,f). The inter-ictal HR did not significantly change with recurring seizures (ρ = − 0.005, P = 0.99; Fig. 2e).
Discussion
In this experimental study, we showed that NVC is partially maintained during recurring penicillin-induced seizures in healthy animals, with stable relative ictal variations of both CBFv and PbtO2. This was accompanied by a progressive increase in the inter-ictal CBFv but also by a progressive decrease in the inter-ictal PbtO2.
Our results are thus in line with previous clinical studies that reported an increase of CBF, and a consequent rise in intracranial pressure, following repetitive NCSz10,11,12. Recurrent seizures also cause blood–brain barrier (BBB) permeability changes and vascular leakage4,6 leading to cerebral inflammation and brain edema, which is associated with enhanced mass effect and midline shift in brain injured patients21. These events might alter the neurovascular unit22 and potentially increase the risk of intracranial hypertension. In case of preexisting NVC alteration, as in subarachnoid hemorrhage patients, brain hypoxia might occur even during seizures10. As previously demonstrated10,23, the metabolic uncoupling during the inter-ictal phase and the seizure-induced intracranial hypertension may be a cause of secondary brain injury in critically ill patients experiencing recurrent seizures.
Prior animal studies have shown that the increased O2 consumption, necessary to restore basal intracellular Na+ and K+ concentrations after neuronal firing, exceeds seizure duration24,25,26, lasting up to 2 min after discharge cessation. Our results suggest that NVC cannot fully compensate for the post-ictal energy demand, resulting in progressive reduction in cerebral oxygenation, as seizures repeat. Functional hyperemia would be less efficient in restoring tissue oxygenation because of the above-mentioned seizure-induced BBB and brain extracellular milieu alterations which may worsen oxygen delivery to the tissue.
At the same time, the ictal variation in PbtO2 increased with recurrent seizures. It has been suggested that mitochondrial dysfunction occurs with seizure repetition6. Consequently, the impaired oxidative respiration could explain the reduction in O2 consumption and the rise in PbtO2 we observed as seizures repeat. Furthermore, as the lack of substrate is the rate limiting factor for oxygen consumption28, the inadequate inter-ictal perfusion we observed could play a role in reducing mitochondrial activity. It has to be noted that the extent of these events was not sufficient to impair neuronal function since the last seizures had a prominent EEG power and lasted longer than the early ones. As proposed by others authors, in the context of pathologic stress, auxiliary sources of energy than mitochondrial oxidative respiration, such as glycolysis, might support neuronal activity27,29.
Local changes at the cerebral level are further influenced by progressive hemodynamic changes at the systemic level. With recurring seizures, we observed a transient increase followed by a progressive decrease in interictal MAP variation and a progressive increase in interictal CO variation, while the ictal MAP and HR progressively decreased, albeit non significantly. As opposed to convulsive seizures and status epilepticus (SE), the systemic effects of NCSz and NCSE are not fully understood. Cardiovascular changes in epilepsy models vary accordingly to activation of different cortical (such as cingulate gyrus, insular cortex, prefrontal cortex)30 or subcortical (such as thalamus, hypothalamus)31 structures involved in cardiovascular function regulation. However, sympathetic outflow is commonly enhanced during seizures15. In our model, ictal-induced sympathetic stimulation resulted into an initial predominant rise in MAP associated with a chronotropic cardiac effect. Our findings are at odds with previous animal studies, which found a decrease in cardiac function responsible for a progressive reduction in ictal changes of CO and consequently MAP changes14. In fact, even if MAP changes show a negative tendency in both ictal and inter-ictal measures, the inter-ictal CO trend is clearly positive. Differences in species (rat vs. sheep), in the mode of administration (IV vs. in situ) and type of pro-convulsant (pentylenetetrazole vs. penicillin) may account for these discrepancies. The inter-ictal decrease in MAP and increase in CO might be explained by a differential desensitization of vascular and cardiac adrenergic receptors (AR) to persistent sympathetic activation. In different settings, α AR vascular desensitization was shown to occur in term of few hours32 whereas β cardiac receptors internalization might take much longer33. It was for instance shown that sympathetic activation during continuous NCSE only had a transient effect over peripheral vessels, as opposed to a more persistent cardiac effect34. This study, as well as most prior studies investigating the systemic effect of NCSE or NCSz, used IV administration of pro-convulsant agents to induce generalized seizures14,34.
Our study seem to suggest that seizures might progressively alter the autonomic response, in the absence of a potential direct effect of PTZ on the autonomic system. It is well known that an autonomic dysregulation occurs in epileptic patients35 and that it is related to the development of fatal arrhythmias and sudden death36.
Our study provides some leads for future clinical applications. We showed that significant changes in the cerebrovascular regulation take place after a relatively small number of seizures that might likely occur in a limited period in predisposed patients. This might suggest that, in selected cases, especially in those presenting a preexisting condition known to alter the NVC performance (i.e. traumatic brain injury37, ischemic stroke38, subarachnoid hemorrhage10), a real 24/7 (daytime and night time) continuous EEG (cEEG) monitoring should be provided in order to stop seizure recurrence as soon as possible and prevent their potential deleterious effects. In this sense, our results stress the importance of increasing the availability of the cEEG, in order to provide a prompt seizure treatment. In fact, cEEG is the only available tool to detect NCSz, and it is associated with a lower in-hospital mortality39. Unfortunately, cEEG demands high humans and technical resources and it is seldom limited to bigger health structures39. In order to deceive this issue, recent literature compared cEEG vs repeated routine (20 min) EEG and seemed to suggest that, even the latter was less performant in seizure detection, mortality was not influenced by recording duration40. Due to important methodological limitations41, evidences are lacking to prefer routine to continuous EEG and our results seem to suggest that efforts should be pursuit to spread cEEG use in order to maximize seizure recognition and treatment.
Our study has some limitations. First, the ictal variations in tissue oxygenation we recorded are smaller than those reported in other animals studies42,43. Although we positioned Clark and EEG electrodes as close as possible to each other, our measures might represent the average of PbtO2 variations in the focus and its surrounding tissue, which are not superimposable42,44, and might thus underestimate their magnitude. Second, we did not directly quantify intracranial pressure; as a consequence, we cannot confirm previous studies that found a correlation between prolonged seizure and intracranial hypertension10,11,12 and our conclusions are speculative on this point. Since animals were anesthetized, the question of whether the influence of anesthesia on NVC arises. At this moment, this effect is unclear; even if sedative drugs can alter CBF45, preliminary studies did not show a negative influence on NVC46. Whether the chosen model of epilepsy could interfere with the NVC also has to be considered. Penicillin exerts its pro-convulsant effect by inhibiting gamma-aminobutyric acid (GABA)-gated chloride ion influx47. GABA released from interneurons might play a role in the NVC since it has a direct effect on vascular smooth cells48. Blocking GABA receptors might increase neurotransmitter extracellular concentration and facilitate its interaction with vascular cells receptors. The high variability of the ictal CBFv responses is questioning. It has already been shown that the direction (increase vs decrease) of the initial vascular response to seizure depend from the distance of the recording probe from the ictal focus, since an initial decrease in the CBFv occurs in the vicinity of the seizure focus42. It has to be noted that an absolute increase in ictal CBFv is plausible despite the stable relative ictal variations because of an increase in the CBFv inter-ictal value, since this value was taken to calculate the ictal change. As vascular measurements were made at the brain surface, results concern mainly pial vessels and they might not be generalizable to other vascular compartments. Due to the frequently recurring seizures, it was not possible to find a suitable stationary period, as suggested by the Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology35,49, to quantify heart rate variability and baroreflex sensitivity measurements in order to deeply analyze autonomic function. Thus, the seizure-induced autonomic dysfunction remains speculative. Finally, it has to be noticed that, in this acute setting, seizures recurrence was more frequent than what usually occurs in human patients; this precludes an entire translation of our results to clinical practice.
In conclusion, our study suggests a deleterious effect of recurrent seizures in both cerebral and systemic vascular system. The NVC is only partially maintained since it is finally unable to compensate for the metabolic demand of closely repeating seizures, leading to a reduction in brain tissue oxygenation despite a hyperemia which, at long term, might be associated with an increasing intracranial pressure that may further impair cortical perfusion. Systemic cardiovascular response changes might fail to support cerebral hemodynamics and may suggest a seizure-induced autonomic dysfunction.
Materials and methods
General procedure
Animal model procedures have been previously described50. Briefly, the Institutional Review Board for Animal Care of the Free University of Brussels (Belgium) approved all experimental procedures (approval number 675 N), which were also in compliance with ARRIVE guidelines. Care and handling of the animals were in accord with National Institutes of Health guidelines (Institute of Laboratory Animal Resources). The protocol was performed on seven anesthetized, mechanically ventilated, healthy Ovis Aries female sheep. Right-side craniotomy was performed using a high-speed drill (Wuhu Ruijin Medical instrument, Wuhu, China) and a 2.5 cm2 bone hole was opened in the frontal-parietal bone using a laminectomy tool (Aesculap-WerkeAG, Tuttlingen, Germany). The dura mater was opened with scissors and a 4-contact electrocorticography (ECOG) electrodes (Dixi Medical, Besançon, France) was slipped beneath the dura over the cortex surface of the post-central gyrus and taped to the skull. Within 1 cm from the ECOG electrode, the dura mater was subsequently punctured to insert a laser-Doppler flowmetry probe (OxyFlow 4000, Oxford Optronic, UK) for local cerebral blood flow velocity (CBFv) measurement and a Clark electrode (Licox; Integra Lifesciences, Zaventem, Belgium) for brain tissue oxygen partial pressure (PbtO2) measurement. All catheters were placed under sterile conditions at a depth of 0.5 cm into the brain parenchyma as close as possible one to each other (Supplementary Fig. S1), as previously described50.
Monitoring and measurements
A continuous intravenous (IV) infusion of ketamine, morphine, and midazolam was used as general anesthesia throughout the entire experiment adjusting initial doses in order to achieve a nearly continuous background51. Muscular blockade was achieved using 10 μg/kg/h of rocuronium. Ventilator parameters were adjusted to maintain PaO2 and PaCO2 values in the normal (90–120 mmHg and 35–45 mmHg respectively) ranges. Mean arterial pressure (SC 9000 monitor; Siemens, Berlin, Germany), heart rate (HR), core-temperature and cardiac output (CO) (Vigilance II monitor; Edwards Lifesciences, Irvine, California, United-States) were monitored continuously. Systemic hemodynamic parameters, ECOG, PbtO2, and CBFv were recorded continuously and simultaneously with a sampling rate of 250 Hz (Notocord-hem, Instern Company, France). Measurements of mean pulmonary arterial pressure were collected every 1.5 h. Cardiac index (CI) was calculated using standard formulas52; the body surface area was estimated from Mitchell’s sheep-specific formula53.
Experimental protocol
After surgical procedures, the animal was allowed to stabilize. Seizures were induced by topical application of penicillin G (Kela Pharma, Sint-Niklass, Belgium) on the cerebral cortex beneath the ECOG electrode. 105 penicillin UI, diluted in 0.1 mL of CNS perfusion fluid (Perfusion Fluid CNS, CMA Microdialysis AB, Sweden), were applied every 15 min until seizures were induced. After data collection, animals were euthanized using IV high dose of potassium chloride (40 mEq).
Data analysis
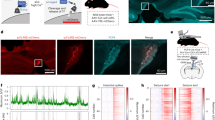
All analyses were performed offline, using built-in and custom functions in Matlab (The MathWorks, Natick, MA, USA). Physiologically implausible measures and outliers, defined according to Chauvenet’s criteria54, were removed. Seizure onsets were defined as rhythmic discharges with a frequency ≥ 3 Hz, according to consensus criteria51; seizure offsets corresponded to post-ictal ECOG signal attenuation or when discharge frequency dropped below 3 Hz. For each detected seizure, ECOG epochs from 30 s before to 60 s after seizure onset were selected (Fig. 3); if the inter-ictal interval between two consecutive seizures was shorter than 60 s, both seizures were discarded. The envelope of the gamma frequency band (30–50 Hz) (Eγ) was extracted from the ECOG signal using wavelet transform spectral density estimate (cwt, icwt and envelope functions in Matlab); this frequency band was chosen because it best reflects neurons’ activity55. Physiological variables (MAP, HR, CBFv, PbtO2 and CO) were simultaneously recorded; since the sampling frequency of the CO monitor was too low to identify rapid variations, the Liljestrand-Zander method56 was employed to estimate CO from the pulse waveform (COEST). The CBFv signal was high-pass filtered with a cut-off frequency of 0.25 Hz. Since the number of seizures varied between animals, data analysis was limited to the first 22 seizures per animal in order to maximize the available variables. Of note, since animals were curarized, seizures were non-convulsive.
Multimodal cerebral and systemic recording in an animal with penicillin-induced seizures. Eγ EEG gamma envelope power, CBFv Cerebral blood flow velocity, PbtO2 Partial tissue oxygen pressure, MAP Mean arterial pressure, HR Heart rate, COEST Cardiac output estimation using the Liljestrand–Zander method. Time = 0 corresponds to the last penicillin application before seizure occurrence. Peaks in the gamma envelope of the ECOG signal corresponds to induced seizures on electrocorticography (Eγ—top row). Seizures are associated with time-locked variations in local CBFv (second row), PbtO2 (third row) and systemic parameters (MAP—forth row, HR—fifth row, and COEST—last row). The epoch around a seizure is presented as example (grey rectangle); for more details, please refer to the text.
Ictal versus pre-ictal variations
For each seizure of each animal, all variables were expressed as percentage variations from the baseline mean, calculated on the pre-ictal 15 s epoch, as previously described10. The peak values of the normalized ictal measures for each seizure were pooled together across animals and used for further statistical analysis.
Variations of pre-ictal values
For each seizure of each animal, pre-ictal values were also expressed as percentage variations of the pre-ictal mean of the first seizure; each animal was used as its own baseline reference. These normalized pre-ictal values for each seizure were pooled together across all animals and used for further statistical analysis.
Statistical analysis
Statistical analyses were performed using Matlab (MathWorks). A p value < 0.05 was considered statistically significant. Data are presented as median ± median absolute deviation or median [range]. The Spearman’s rank-order correlation coefficient was used to measure the strength of the association between all available repeating seizures and variations of local (Eγ, CBG, PbtO2) and systemic (MAP, HR, COEST) parameters.
To ensure that measured parameters were stable over time, they were recorded in four control animals in which seizures were not induced. Results are presented in Supplementary Fig. S2.
Ethical publication statement
We confirm that we have read the Journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
References
Kobayashi, E., Hawco, C. S., Grova, C., Dubeau, F. & Gotman, J. Widespread and intense BOLD changes during brief focal electrographic seizures. Neurology 66, 1049–1055 (2006).
Attwell, D. et al. Glial and neuronal control of brain blood flow. Nature 468, 232–243 (2010).
van Vliet, E. A. et al. Blood-brain barrier leakage may lead to progression of temporal lobe epilepsy. Brain 130, 521–534 (2007).
van Vliet, E. A., Aronica, E. & Gorter, J. A. Blood–brain barrier dysfunction, seizures and epilepsy. Semin. Cell Dev. Biol. 38, 26–34 (2015).
Löscher, W. & Friedman, A. Structural, molecular, and functional alterations of the blood-brain barrier during epileptogenesis and epilepsy: A cause, consequence, or both?. Int. J. Mol. Sci. 21, 591 (2020).
Prager, O. et al. Seizure-induced microvascular injury is associated with impaired neurovascular coupling and blood–brain barrier dysfunction. Epilepsia 60, 322–336 (2019).
Sharp, C. D. et al. N-methyl-d-aspartate receptor activation in human cerebral endothelium promotes intracellular oxidant stress. Am. J. Physiol. Heart Circ. Physiol. 288, H1893–H1899 (2005).
Winkler, M. K. L. et al. Impaired neurovascular coupling to ictal epileptic activity and spreading depolarization in a patient with subarachnoid hemorrhage: Possible link to blood-brain barrier dysfunction: BBB and Impaired Neurovascular Coupling. Epilepsia 53, 22–30 (2012).
Balbi, M., Koide, M., Wellman, G. C. & Plesnila, N. Inversion of neurovascular coupling after subarachnoid hemorrhage in vivo. J. Cereb. Blood Flow Metab. 37, 3625–3634 (2017).
Claassen, J. et al. Nonconvulsive seizures after subarachnoid hemorrhage: Multimodal detection and outcomes: Claassen et al: Effects of seizures after SAH. Ann. Neurol. 74, 53–64 (2013).
Vespa, P. M. et al. Nonconvulsive electrographic seizures after traumatic brain injury result in a delayed, prolonged increase in intracranial pressure and metabolic crisis. Crit. Care Med. 35, 2830–2836 (2007).
Ko, S.-B. Status epilepticus-induced hyperemia and brain tissue hypoxia after cardiac arrest. Arch. Neurol. 68, 1323 (2011).
Kreisman, N. R., Magee, J. C. & Brizzee, B. L. Relative hypoperfusion in rat cerebral cortex during recurrent seizures. J. Cereb. Blood Flow Metab. 11, 77–87 (1991).
Kreisman, N. R., Gauthier-Lewis, M. L., Conklin, S. G., Voss, N. F. & Barbee, R. W. Cardiac output and regional hemodynamics during recurrent seizures in rats. Brain Res. 626, 295–302 (1993).
Nass, R. D., Hampel, K. G., Elger, C. E. & Surges, R. Blood pressure in seizures and epilepsy. Front. Neurol. 10, 501 (2019).
Kaiser, E. & West, F. Large animal ischemic stroke models: Replicating human stroke pathophysiology. Neural Regen. Res. 15, 1377 (2020).
Opdam, H. I. et al. A sheep model for the study of focal epilepsy with concurrent intracranial EEG and functional MRI. Epilepsia 43, 779–787 (2002).
Johnston, S. C., Horn, J. K., Valente, J. & Simon, R. P. The role of hypoventilation in a sheep model of epileptic sudden death. Ann. Neurol. 37, 531–537 (1995).
Taccone, F. S. et al. Sepsis is associated with altered cerebral microcirculation and tissue hypoxia in experimental peritonitis. Crit. Care Med. 42, e114 (2014).
Taccone, F. S. et al. Cerebral microcirculation is impaired during sepsis: An experimental study. Crit. Care 14, 1–10 (2010).
Vespa, P. M. et al. Acute seizures after intracerebral hemorrhage: A factor in progressive midline shift and outcome. Neurology 60, 1441–1446 (2003).
Bankstahl, M. et al. Blood–brain barrier leakage during early epileptogenesis is associated with rapid remodeling of the neurovascular unit. eneuro 5, ENEURO.0123-18.2018 (2018).
Claassen, J. et al. Nonconvulsive seizures in subarachnoid hemorrhage link inflammation and outcome: Seizures in SAH. Ann. Neurol. 75, 771–781 (2014).
Lewis, D. V. & Schuette, W. H. NADH fluorescence and [K+]o changes during hippocampal electrical stimulation. J. Neurophysiol. 38, 405–417 (1975).
Lewis, D. V., O’Connor, M. J. & Schuette, W. H. Oxidative metabolism during recurrent seizures in the penicillin treated hippocampus. Electroencephalogr. Clin. Neurophysiol. 36, 347–356 (1974).
Lothman, E., LaManna, J., Cordingley, G., Rosenthal, M. & Somjen, G. Responses of electrical potential, potassium levels, and oxidative metabolic activity of the cerebral neocortex of cats. Brain Res. 88, 15–36 (1975).
Vespa, P. et al. Metabolic crisis without brain ischemia is common after traumatic brain injury: A combined microdialysis and positron emission tomography study. J. Cereb. Blood Flow Metab. 25, 763–774 (2005).
Jöbsis, F. F., O’Connor, M., Vitale, A. & Vreman, H. Intracellular redox changes in functioning cerebral cortex. I. Metabolic effects of epileptiform activity. J. Neurophysiol. 34, 735–749 (1971).
Yang, H. et al. Glycolysis in energy metabolism during seizures. Neural Regen. Res. 8, 1316–1326 (2013).
Sevcencu, C. & Struijk, J. J. Autonomic alterations and cardiac changes in epilepsy: Cardiac Effects in Epilepsy. Epilepsia 51, 725–737 (2010).
Kaya, C. A., Ozkaynakci, A. E., Goren, M. Z. & Onat, F. Y. Changes in baroreflex responses of kindled rats. Epilepsia 46, 367–371 (2005).
Bünemann, M., Lee, K. B., Pals-Rylaarsdam, R., Roseberry, A. G. & Hosey, M. M. Desensitization of G-protein–coupled receptors in the cardiovascular system. Annu. Rev. Physiol. 61, 169–192 (1999).
Tang, C., Yang, J., Wu, L.-L., Dong, L.-W. & Liu, M.-S. Phosphorylation of β-adrenergic receptor leads to its redistribution in rat heart during sepsis. Am. J. Physiol.-Regul. Integr. Comp. Physiol. 274, R1078–R1086 (1998).
Benowitz, N. L., Simon, R. P. & Copeland, J. R. Status epilepticus: Divergence of sympathetic activity and cardiovascular response. Ann. Neurol. 19, 197–199 (1986).
Myers, K. A., Sivathamboo, S. & Perucca, P. Heart rate variability measurement in epilepsy: How can we move from research to clinical practice?. Epilepsia 59, 2169–2178 (2018).
Jefferys, J. G. R., Ashby-Lumsden, A. & Lovick, T. A. Cardiac effects of repeated focal seizures in rats induced by intrahippocampal tetanus toxin: Bradyarrhythmias, tachycardias, and prolonged interictal QT interval. Epilepsia 61, 798–809 (2020).
Toth, P. et al. Traumatic brain injury-induced autoregulatory dysfunction and spreading depression-related neurovascular uncoupling: Pathomechanisms, perspectives, and therapeutic implications. Am. J. Physiol. Heart Circ. Physiol. 311, H1118–H1131 (2016).
Salinet, A. S. M., Robinson, T. G. & Panerai, R. B. Cerebral blood flow response to neural activation after acute ischemic stroke: A failure of myogenic regulation?. J. Neurol. 260, 2588–2595 (2013).
Hill, C. E. et al. Continuous EEG is associated with favorable hospitalization outcomes for critically ill patients. Neurology 92, e9–e18 (2019).
Rossetti, A. O. et al. Continuous vs routine electroencephalogram in critically ill adults with altered consciousness and no recent seizure: A multicenter randomized clinical trial. JAMA Neurol. 77, 1225 (2020).
Gaspard, N., Westover, M. B. & Hirsch, L. J. Assessment of a study of continuous vs repeat-spot electroencephalography in patients with critical illness. JAMA Neurol. 78, 369 (2021).
Zhao, M., Ma, H., Suh, M. & Schwartz, T. H. Spatiotemporal dynamics of perfusion and oximetry during ictal discharges in the rat neocortex. J. Neurosci. 29, 2814–2823 (2009).
Bahar, S., Suh, M., Zhao, M. & Schwartz, T. H. Intrinsic optical signal imaging of neocortical seizures: The ‘epileptic dip’. NeuroReport 17, 499–503 (2006).
Zhao, M. et al. Preictal and ictal neurovascular and metabolic coupling surrounding a seizure focus. J. Neurosci. 31, 13292–13300 (2011).
Zeiler, F. A. et al. The cerebrovascular response to ketamine: A systematic review of the animal and human literature. J. Neurosurg. Anesthesiol. 28, 123–140 (2016).
Franceschini, M. A. et al. The effect of different anesthetics on neurovascular coupling. Neuroimage 51, 1367–1377 (2010).
Tsuda, A. et al. Effect of penicillin on GABA-gated chloride ion influx. Neurochem. Res. 19, 1–4 (1994).
Cauli, B. Cortical GABA interneurons in neurovascular coupling: Relays for subcortical vasoactive pathways. J. Neurosci. 24, 8940–8949 (2004).
Heart rate variability: standards of measurement, physiological interpretation and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Circulation 93, 1043–1065 (1996).
Ferlini, L., Su, F., Creteur, J., Taccone, F. S. & Gaspard, N. Cerebral autoregulation and neurovascular coupling are progressively impaired during septic shock: An experimental study. Intensive Care Med. Exp. 8, 44 (2020).
Hirsch, L. J. et al. American Clinical Neurophysiology Society’s standardized critical care EEG terminology: 2012 version. J. Clin. Neurophysiol. 30, 1–27 (2013).
Patel, N., Durland, J. & Makaryus, A. N. Physiology, cardiac index. in StatPearls (StatPearls Publishing, 2021). https://www.statpearls.com/ArticleLibrary/viewarticle/18897 PMID: 30969727.
Berman, A. Effects of body surface area estimates on predicted energy requirements and heat stress. J. Dairy Sci. 86, 3605–3610 (2003).
Zerbet, A. & Nikulin, M. A new statistic for detecting outliers in exponential case. Commun. Stat. Theory Methods 32, 573–583 (2003).
Manning, J. R., Jacobs, J., Fried, I. & Kahana, M. J. Broadband shifts in local field potential power spectra are correlated with single-neuron spiking in humans. J. Neurosci. 29, 13613–13620 (2009).
Caillard, A. et al. Comparison of cardiac output measured by oesophageal Doppler ultrasonography or pulse pressure contour wave analysis. Br. J. Anaesth. 114, 893–900 (2015).
Acknowledgements
This work was supported by the Fonds Erasme pour la Recherche Médicale–Convention de Recherche d’Excellence and the Fonds National pour la Recherche Scientifique.
Author information
Authors and Affiliations
Contributions
N.G., F.S.T., and J.C. conceived the original idea and designed the model. L.F. and F.S. carried out the experiments. L.F. collected the data, performed the analytic calculations and interpretation, and wrote the manuscript directly supervised by N.G. All authors discussed the results, commented on the manuscript, and approved the final version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ferlini, L., Su, F., Creteur, J. et al. Cerebral and systemic hemodynamic effect of recurring seizures. Sci Rep 11, 22209 (2021). https://doi.org/10.1038/s41598-021-01704-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-01704-6
This article is cited by
-
Xylazine effects on opioid-induced brain hypoxia
Psychopharmacology (2023)
-
Sepsis modulates cortical excitability and alters the local and systemic hemodynamic response to seizures
Scientific Reports (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.