Abstract
Carbon dioxide (CO2) is commonly used to kill laboratory rats. Rats find CO2 aversive and aversion varies between individuals, indicating that rats vary in CO2 sensitivity. Healthy humans experience feelings of anxiety at concentrations similar to those avoided by rats, and these feelings are diminished by the administration of benzodiazepines. Our aim was to assess the effects of the benzodiazepine midazolam on individual thresholds of rat aversion to CO2. Six female Sprague Dawley rats were repeatedly exposed to CO2 gradual-fill in approach-avoidance testing. The first three exposures were to a control-treatment followed by three exposures to midazolam (0.375 mg/kg). Within each treatment aversion to CO2 was not affected by exposure number; however, tolerance increased from an average of 10.7% CO2 avoided during control sessions, to 15.5% CO2 avoided when treated with midazolam. These results indicate that rats experience anxiety when exposed to CO2, and that variation in rat CO2 sensitivity is driven by individual differences in the onset of these feelings of anxiety. No rat tolerated CO2 concentrations required to induce loss of consciousness.
Similar content being viewed by others
Introduction
Carbon dioxide (CO2) is one of the most used methods to kill laboratory rats1, but mounting evidence indicates that CO2 elicits negative emotions. Rats are highly motivated to avoid CO2 in aversion tests2,3,4,5,6,7,8, and these animals express a wide range defence behaviours – e.g. rearing, pushing the cage lid, increased locomotion, vocalizations and freezing – when exposed to this agent9,10,11. Recent work from our research group indicates that rats vary in CO2 sensitivity. Aversion to CO2 consistently varied among individuals across repeated exposures12.
Voluntary inhalation of CO2 is widely used in human research to induce feelings of anxiety, fear and panic13,14. Humans vary in CO2 sensitivity, with panic disorder patients being sensitive to even low concentrations15,16,17. In healthy volunteers, self-reported feelings of fear, anxiety and panic increase with CO2 concentration18,19. It has been proposed that human CO2 sensitivity is mediated by the GABAergic system20. Healthy subjects and panic disorder patients that are pre-treated with benzodiazepines (thus increasing GABAA receptor functioning) experience less fear, anxiety and panic due to CO2 inhalation21,22. In rats, exposure to higher CO2 concentrations decreases GABAA function23,24, and enhances anxiety-like behaviours in the Vogel conflict25 and social interaction tests26; effects that are counteracted by the administration of benzodiazepines23,24,25,26.
Emotions can be defined as observable stimuli-elicited responses (behavioral, neurobiological and physiological), whereas the subjective experience of emotions (i.e. felt emotions) are the animals’ conscious awareness of these responses27. Felt emotions can be inferred in animals from a combination of evidence from behavioral, neurobiological and physiological responses28, functional homology29, and the use of specific drug treatments that target feelings of emotions in humans30. The aim of this study was to assess the effects of the benzodiazepine midazolam on rat individual thresholds of aversion to CO2. We hypothesized that rat aversion to CO2 is caused by feelings of anxiety, and predicted that aversion to CO2 would decrease when rats were pre-treated with midazolam. We further hypothesized that individual differences in rat CO2 sensitivity are driven by variation in the onset of feelings of anxiety, and predicted that an increase in CO2 tolerance due to midazolam treatment would reduce individual differences in the threshold of aversion.
Results
Locomotor effects
Control and midazolam treatments did not differ in the rate of line crossing (control: 0.2 ± 0.06 crossings s−1; midazolam: 0.4 ± 0.10 crossings s−1; t = −2.06, df = 5, p = 0.09).
Anxiolytic effects
No rat produced fecal boli in the elevated plus maze. Rats spent more time in the open arms in the midazolam treatment (23 ± 4.1 s) compared to the control (13 ± 3.9 s; t = −2.70, df = 5, p < 0.05). The number of open arm entries did not differ between control (2.3 ± 0.56 entries) and midazolam treatments (4.0 ± 0.86 entries; t = −1.89, df = 5, p = 0.12).
Aversion to CO2
During training (with air) rats left the bottom cage after 364 ± 15 s and ate all 20 rewards. During test sessions with air, we found a significant interaction between exposure number and treatment on latency to exit the cage (F = 5.87, df = 1,27, p < 0.05). The average latency to leave the bottom cage when rats were treated with midazolam was 391 ± 28 s, while during control sessions rats left after 420 ± 27 s. In the control treatment, latency to exit the cage decreased with exposure number (β = −20.25, standard error = 9.13, t = −2.22, df = 11, p = 0.05). In the midazolam treatment there was no evidence for a change in latency to exit the cage as a function of exposure number (β = 10.33, standard error = 9.14, t = 1.13, df = 11, p = 0.28). Again, rats ate all 20 sweet rewards (in both treatments) when exposed to air.
We found a significant effect of treatment on the latency to avoid CO2 and number of rewards consumed (latency to avoid CO2: F = 21.59, df = 1,25, p < 0.001; rewards consumed: F = 14.55, df = 1,25, p < 0.001). Rats tolerated CO2 for longer and consumed more rewards when treated with midazolam than they did during control sessions (Fig. 1a,b). Rats exited the cage when CO2 concentrations reached on average 10.7 ± 1.14% CO2 during control sessions, versus 15.5 ± 1.41% CO2 when rats were treated with midazolam. Exposure number and its interaction with treatment did not affect the latency to avoid CO2 (exposure number: F = 0.1, df = 1,25, p = 0.75; interaction between exposure number and treatment: F < 0.001, df = 1,25, p = 0.98) or the number of rewards consumed (exposure number: F = 0.53, df = 1,25, p = 0.47; interaction between exposure number and treatment: F = 0.14, df = 1,25, p = 0.71).
Effect of midazolam on rat aversion to CO2. Rat responses showing treatment effects and consistency in individual rat responses between control- and midazolam-treatment (each line corresponds to an individual rat; n = 6 rats; dots and error bars represent the mean ± standard error). (a) Latency to avoid CO2 and (b) number of rewards consumed.
Individual differences in the latency to avoid CO2 were consistent across the two treatments (Pearson correlation test: r = 0.83, df = 4, p < 0.05; Fig. 1a). The CO2 concentrations at which rats exited the cage ranged between 6.2 and 13.6% CO2 among rats during control sessions, versus between 10.9 and 19.3% CO2 when rats were treated with midazolam. Number of rewards consumed was consistent across the two treatments (r = 0.78, df = 4, p = 0.07; Fig. 1b).
Discussion
We found no effect of midazolam on locomotion in the open field, indicating that midazolam at the dose provided did not impair activity and in this way reduced avoidance behaviour. Moreover, during air trials all rats exited the bottom cage in every test. These results are consistent with previous work showing that low doses do not interfere with normal activity in rats31,32,33. Studies have shown a dose dependent effect of midazolam on activity34; doses in excess of 1 mg/kg can reduce locomotion31 and doses in excess of 10 mg/kg can induce anaesthesia35,36.
Previous studies have shown that midazolam increases open arm exploration in the elevated plus maze31,37,38,39, reduces defensive burying40, predator odour avoidance32,33, and freezing due to place conditioning31. In the current study, pre-treated rats spent more time in the open arms of the elevated plus maze, adding to the existing evidence that midazolam has an anxiolytic effect.
In combination, we conclude that oral administration of 0.375 mg/kg midazolam decreases anxiety without impairing motor function. The pharmacodynamics of this drug do not appear to differ between oral and intravenous administration. Midazolam is absorbed rapidly (reaching peak plasma concentration 5 to 15 min after administration) with a systemic availability and metabolic clearance of 45% and 27 min (t1/2), respectively, and a terminal half-life of 67 ml min−1 kg−1 41. In the current study, all rats rapidly and willingly consumed the pudding mixed with midazolam, without the need for handling, restraint, or injection – these procedures have shown to induce stress in rats42,43,44,45, and can alter responses in behavioural tests46,47,48.
When treated with midazolam, rats showed a 45% increase in tolerance of CO2 (i.e. tolerance increased from 10.7 to 15.5% CO2). It is unlikely that order accounts for this result given that we found no within-treatment effect of exposure order on aversion to CO2, and that rats used in the current study were already familiar with CO2 exposure in approach-avoidance testing. Familiarity with CO2 and the testing environment likely reduced within-individual variation in responses49. A previous study using the same experimental setting (i.e. approach-avoidance testing with similar flow rates of CO2) showed that tolerance of CO2 does not increase with consecutive exposures12. Hence we argue that the observed increase in tolerance to CO2 was due to midazolam and not habituation.
It has been reported that benzodiazepines increase food palatability and intake50 so it is possible that rat motivation to consume the sweet rewards increased with midazolam. However, the effect of midazolam on sucrose consumption is dose dependent; midazolam affects sucrose consumption at doses higher than 3.0 mg/kg but it is reported to have negligible effects at doses similar to that used in the current study51. In addition, rat aversion to CO2 in approach-avoidance tests is not related to food motivation8. Since midazolam also reduced evidence of anxiety in the elevated plus maze, it is reasonable to conclude that the increased CO2 tolerance was due to the anxiolytic effect of midazolam. Future work should consider the use of motivation trade-offs that are not food related, for example, the use of a light-dark apparatus.
During control trials rats tolerated concentrations of CO2 averaging 10.7%; similar concentrations of CO2 elicit feelings of anxiety in humans. When inhaling 7.5% CO2 healthy humans show an increase in escape responses (i.e. request to stop the test) and feelings related to anxiety (e.g. alertness, anxiety, fear, feel like leaving the room, feeling paralysed, tense, irritable, nervous, worried)52,53, but panic responses are rare at this concentration. Gorman and colleagues15 reported a panic rate of 5% in healthy people when inhaling 7% CO2 for 20 min. In contrast, a single inhalation of 35% CO2 results in panic in 23 to 41% of healthy volunteers17,53,54,55. Inhalation of lower concentrations (~7% CO2) elicits feelings similar to those experienced by people with generalized anxiety disorder21,53,56,57, whereas the emotional experience felt at higher concentrations (35% CO2) resembles naturally occurring panic attacks54. When inhaling 7.5% CO2, healthy individuals pretreated with the benzodiazepine lorazepam experienced fewer feelings related to anxiety21,57. Pre-treatment with the benzodiazepine alprazolam – an anti-panic drug – reduced feelings and somatic symptoms associated with panic elicited by 7 and 35% CO2 inhalation53,56. In the current study, providing midazolam before CO2 exposure increased the average threshold of aversion to 15.5% CO2. This increase indicates that rat aversion to lower concentrations of CO2 is elicited by feelings of anxiety, and that these feelings are reduced by midazolam.
It is important to note that all rats avoided CO2 at concentrations far lower than those needed to induce unconsciousness. This result suggests that higher concentrations of CO2 evoke emotional experiences (e.g. air hunger or panic) that are not sensitive to the anxiolytic effect of midazolam at this dose.
Previous studies have shown that thresholds of aversion vary among rats, ranging between 5.6 and 18.3% CO212. In agreement with these results, we found that during control tests the threshold of aversion ranged from 6.2 to 13.6% CO2 among rats. In contrast, the CO2 concentrations avoided when rats were treated with midazolam ranged between 10.9 and 19.3%, values substantially higher than reported for non-medicated rats6,12. Individual differences in CO2 aversion were consistent within rats across treatments. Variation in rat CO2 responsiveness has been linked to the activity of neurons involved in the mediation of anxiety and panic experiences (i.e. orexin neurons in the lateral hypothalamus)58,59. These results indicate that individual differences in rat CO2 sensitivity are due to differences in the onset of feelings of anxiety.
A limitation of the current study was the sample size of only 6 rats, likely limiting our ability to detect differences between treatments60. That we were still able to detect clear treatment effects with this sample size suggests that these effects are robust. Other limitations include that we used only females, from a single strain, and that these animals were older than those typically used in laboratory research. We encourage work using a larger and more diverse sample. Another limitation is that our design intentionally confounded order and treatment. To reduce the risk of order effects we used animals that were highly habituated to CO2 and the test apparatus, and tested for order effects within treatment. That said, we encourage future studies to employ an A-B-A (return to baseline) design to further account for order effects.
One strength of the current study was that animals were highly experienced with testing procedures. Behavioural responses can be affected by low familiarity with the testing environment, and with uncontrolled contingencies before and during testing46,61,62. We suggest that future studies also use animals that are highly habituated to CO2, the experimental setting and handling procedures but caution that this requires a considerable investment in training.
Conclusion
Midazolam treatment reduced anxiety and increased individual rat thresholds of aversion to CO2 in female Sprague Dawley rats. These results suggest that rat aversion to CO2 is driven by feelings of anxiety, with an onset that varies among individuals. Even with midazolam treatment all rats avoided CO2 before loss of consciousness, indicating that even with this refinement CO2 will induce negative affective states.
Methodology
All procedures were approved by the Animal Care Committee of The University of British Columbia (protocol A15-0071), following the guidelines on care and use of rodents in research established by the Canadian Council on Animal Care.
Subjects and housing
Previous studies using approach-avoidance testing have detected a treatment effect with a sample of 8 rats6. Therefore, we used eight 16-month-old female Sprague-Dawley rats that, in an effort to reduce the total number of animals used, were transferred from another study (obtained from the University of British Columbia surplus stock). Rats were housed two groups of three and one group of two. All rats were clinically healthy at the time of enrolment, but two rats reached humane end points (due mammary tumor development) and were euthanized before the study was completed. The two euthanized rats were both from groups of three so by the end of the study all rats were pair housed with their original cage mates and no regrouping was needed. The remaining rats average 642 ± 46 g (mean ± standard deviation). Rats were marked with a permanent marker (Ketchum Manufacturing Inc., ON, Canada) for individual identification. Each of the three pairs were housed in two cages (20 cm × 50 cm × 40 cm) connected by a red tinted polycarbonate tube (7.6 cm diameter, 15 cm long). The caging contained bedding (1/4 inch Enrichment Bedding, Biofresh, Absorption Corp, WA, USA) and environmental enrichment (e.g. cardboard boxes, hammocks, PVC pipes, and shredded paper towels). Animals were kept on a 12-h light/dark cycle, under controlled temperature and humidity (22 ± 0.15 °C and 57 ± 0.44%, respectively). Rats were provided ad libitum food (Rat Diet PMI 5012, Lab Diets, Land O’Lakes, Inc., MN, USA) and tap water, and provided 30 min of daily access to a large enriched cage63,64 (Supplementary Methods S1: Rat playpens).
Handling and transport
Rats were habituated to handling and transport for 6 months before the study (following, Supplementary Methods S2: Agency-based handling and transport). All trials were performed in an experimental room during the light cycle between 900 h and 1700 h; a cage covered with black plastic was used to transport animals. Subjects were habituated, trained or tested only once per day at similar hours each day. Rats were isolated from cage-mates for a maximum of 40 min per day during habituation, training or testing. Before the beginning of each trial, the apparatus was cleaned with Quatricide (Pharmacal Research Laboratories, Naugatuck, CT, USA).
Experimental design
Rats had been repeatedly exposed to CO2 in the approach-avoidance apparatus before the study and were thus habituated to both the agent and the apparatus. To reduce potential carry over effects from the drug, rats were exposed to CO2 gradual-fill (20% CO2 cage vol. min−1) three times for the control treatment and three times for the midazolam treatment. One air exposure (air flow of 4 L min−1) was run between every CO2 trial, providing data for three control and three midazolam air trials. Two days before the first exposure to CO2 rats were tested in an open field and an elevated plus maze under both treatment conditions (Fig. 2). The anxiolytic effects of benzodiazepines are inconsistently detected when assessed in the open field test65. Hence, the open field test was used to assess effects of midazolam on locomotion, and the elevated plus maze was used to assess anxiolytic effects.
Midazolam administration
Midazolam (5 mg/ml, Sandoz, Boucherville, Qc, Canada) was mixed with 1 ml of vanilla pudding (Vanilla Flavored Pudding Cup, Western Family, Overwaitea Food Group LP, BC, Canada) and administered orally at 0.375 mg/kg33 30 min before testing. For the control treatment, rats received 1 ml of untreated vanilla pudding, also 30 min before testing.
Locomotor effect
Apparatus
The open field consisted of a white acrylic glass arena (100 cm long × 100 cm wide × 61 cm high) placed on a wooden base (52 cm high). The arena was visually divided into 25 squares (20 cm × 20 cm; defined by black lines on the floor) to quantify movement (Supplementary Methods S3: Open field arena and elevated plus maze).
Habituation, training and testing procedures
To control for changes in locomotion due to habituation66,67, rats were exposed to the open field arena twice before testing (Fig. 2). We tested rats once in the control treatment and once in the midazolam treatment. The rat was placed in the center of the open field arena at the beginning of each trial. Trials lasted 5 min and rats could move freely within the arena during this time. All open field trials were video recorded, and recordings were scored (using Boris software, Version 7.0.9)68 by observers blind to rat identity and treatment for frequency of line-crossing (i.e. rat’s shoulders and head crossing any line that divided the floor of the arena). To measure interobserver reliability, 50% of the trials were rescored by an independent observer; the two sets of scores were highly related (r = 0.99).
Anxiolytic effect
Apparatus
An elevated plus maze was used to measure the anxiolytic effects of midazolam. The apparatus was made of two open and two closed black acrylic glass arms (each arm 50 cm long and 10 cm wide; closed arms each had two walls 61 cm high) arranged in a cross shape with a square (10 cm × 10) cm in the center, and placed on a wooden base (52 cm high; Supplementary Methods S3: open field arena and elevated plus maze).
Habituation, training and testing
Open arm behaviour in the elevated plus maze is known to change from the first to second exposure (i.e. one-trial-tolerance), but not between the second and subsequent exposures67,69,70. Thus we exposed rats twice to the elevated plus maze prior to the experiment, and then retested rats once in each treatment condition (Fig. 2). Trials lasted 5 min; at the beginning of each trial subjects were placed at the center of the elevated plus maze and were left to explore the apparatus. All elevated plus maze were video recorded and fecal boli were counted at the end of each trial. Behaviours were scored from video as described above. Again, interobserver reliability was assessed by rescoring 50% of the trials by an independent observer, and again scores were highly consistent (time in the open arms: r = 0.82; open arms entries: r = 0.83).
Aversion to CO2
Apparatus
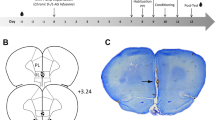
To assess the effect of midazolam on aversion to CO2 we used an approach-avoidance apparatus. The approach-avoidance apparatus consisted of a top cage from the subject’s home caging system placed 20 cm above a bottom cage (20 cm × 45 cm × 24 cm). Both cages contained bedding. Cages were connected by a transparent acrylic glass tube (10 cm diameter, 45 cm long), with cleats on the inside for traction. The connecting tube contained a plastic sliding door (10 cm × 10 cm) at the top cage entrance. The lid for the top cage was made of wire, and the bottom cage lid was made of clear acrylic glass with two scavenging outlets and a gas inlet (Fig. 3).
CO2 and air were delivered from compressed gas cylinders (Praxair, BC, Canada), and the gas flow was regulated through flow meters (CO2: Western Medica, OH, USA; air: Dwyer instruments, Inc., NI, USA).
Habituation, training and testing procedures
Rats had been trained in the approach-avoidance apparatus for another study (in which they had been repeatedly exposed to CO2 in approach-avoidance testing). Rats were not food deprived before testing. Previous work has shown no effect of hunger on motivation for sweet rewards when rats are tested with CO2 in approach-avoidance tests8. At the beginning of the current study these rats were re-trained to go down the tube of the apparatus to enter the bottom cage and eat 20 sweet rewards (Cheerio; Honey Nut Cheerios, General Mills Inc., MN, USA) in the presence of air flow (4 L min−1). First, we placed a rat in the top cage of the apparatus and allowed it to explore for 5 min. Then, we delivered a sweet reward in the top cage and closed the sliding door while the rat ate the reward, blocking access to the bottom cage. We placed 20 sweet rewards in a dish in the bottom cage. After 60 s, we opened the sliding door allowing the rat to descend into the bottom cage to consume the sweet rewards. As soon as the rat’s shoulders crossed into the tube to exit the bottom cage the training session ended; rats were not allowed to return to the bottom cage. Rats were considered to have met the training criterion if they stayed in the bottom cage for 5 min or consumed all 20 sweet rewards for three consecutive training trials.
Once trained, rats were exposed to CO2 in the approach-avoidance apparatus. For CO2 trials, we substituted the flow of air for CO2 as soon as the rat started eating the rewards. We measured the latency (s) to exit the bottom cage and the number of rewards consumed by direct observation.
Assessment of CO2 concentrations
We ran twelve CO2 flow trials in the approach-avoidance apparatus to estimate CO2 concentrations during gradual-fill (18.5% CO2 chamber vol. min−1). No animal was present during these trials. A clear plastic sampling tube was introduced into the cage through an inlet placed in the opposite side of the scavenging outlets, but equidistant to the gas inlet (Fig. 3). The clear tube was attached to an oxygen analyzer (Series 200, Alpha Omega Instrument Corporation, RI, USA). We estimated changes in CO2 concentrations every 0.2 s from the readings of oxygen concentrations using the formula CO2(t=x) = 100 − ([O2(t=x) * 100]/O2(t=0).
Data analysis
Analyses were carried out with R (R Development Core Team, Version 3.4.1) and RStudio (RStudio, Inc., Version 1.0.136). Normality of the residuals and differences of matched pairs were visually assessed. Results are reported as mean ± standard error.
Locomotor effects
We estimated the rate of line crossing per second and then compared treatments using a paired t-test.
Anxiolytic effects
Treatment differences in the time spent in the open arms of the elevated plus maze and the number of open arm entries were tested with paired t-tests.
Aversion to CO2
Response variables (latency to leave the bottom chamber during CO2 and air trials, and the number of rewards eaten during CO2 trials) were analyzed with linear mixed models. The models included treatment (control and midazolam) as fixed factor, exposure number (1st, 2nd and 3rd within each treatment) as a covariate, the interaction between treatment and exposure number, and rat identity as random intercept. For CO2 trials, we also estimated CO2 concentration at the time when rats exited the bottom chamber. Concentrations were estimated using the average CO2 concentration at each time point (measured every 0.2 s) during the 12 CO2 flow trials.
For each rat in each treatment, we estimated the average (from the three trials) latency to leave the bottom chamber and the number of rewards eaten during CO2 trials. Consistency of individual differences in the average latency to leave the bottom chamber and number of rewards eaten between treatments were assessed with Pearson correlation tests.
Data availability
All data generated or analysed during this study is included as Supplementary Data.
References
Hawkins, P. et al. A good death? Report of the second Newcastle meeting on laboratory animal euthanasia. Animals 6, 50 (2016).
Leach, M. C., Bowell, V. A., Allan, T. F. & Morton, D. B. Aversion to gaseous euthanasia agents in rats and mice. Comp. Med. 52, 249–257 (2002).
Leach, M. C., Bowell, V. A., Allan, T. F. & Morton, D. B. Measurement of aversion to determine humane methods of anaesthesia and euthanasia. Anim. Welfare 13, S77–S86 (2004).
Niel, L. & Weary, D. M. Rats avoid exposure to carbon dioxide and argon. Appl. Anim. Behav. Sci. 107, 100–109 (2007).
Niel, L., Kirkden, R. D. & Weary, D. M. Effects of novelty on rats’ responses to CO2 exposure. Appl. Anim. Behav. Sci. 111, 183–194 (2008).
Niel, L., Stewart, S. A. & Weary, D. M. Effect of flow rate on aversion to gradual-fill carbon dioxide exposure in rats. Appl. Anim. Behav. Sci. 109, 77–84 (2008).
Wong, D., Makowska, I. J. & Weary, D. M. Rat aversion to isoflurane versus carbon dioxide. Biol. Lett. 9, 20121000 (2013).
Kirkden, R. D. et al. The validity of using an approach-avoidance test to measure the strength of aversion to carbon dioxide in rats. Appl. Anim. Behav. Sci. 114, 216–34 (2008).
Chisholm, J., De Rantere, D., Fernandez, N. J., Krajacic, A. & Pang, D. S. Carbon dioxide, but not isoflurane, elicits ultrasonic vocalizations in female rats. Lab. Anim. 47, 324–327 (2013).
Niel, L. & Weary, D. M. Behavioural responses of rats to gradual-fill carbon dioxide euthanasia and reduced oxygen concentrations. Appl. Anim. Behav. Sci. 100, 295–308 (2006).
Winter, A., Ahlbrand, R., Naik, D. & Sah, R. Differential behavioral sensitivity to carbon dioxide (CO2) inhalation in rats. Neuroscience 346, 423–433 (2017).
Améndola, L. & Weary, D. M. Evidence for consistent individual differences in rat sensitivity to carbon dioxide. PloS One 14, e0215808 (2019).
Esquivel, G., Schruers, K. R., Maddock, R. J., Colasanti, A. & Griez, E. J. Acids in the brain: a factor in panic? J. Psychopharmacol. 24, 639–647 (2010).
Liu, J. J., Ein, N., Gervasio, J. & Vickers, K. Subjective and physiological responses to the 35% carbon dioxide challenge in healthy and non-clinical control populations: a meta-analysis and systematic review. Anxiety Stress Coping 32, 216–230 (2019).
Gorman, J. M. et al. Physiological changes during carbon dioxide inhalation in patients with panic disorder, major depression, and premenstrual dysphoric disorder: evidence for a central fear mechanism. Arch. Gen. Psychiatry. 58, 125–131 (2001).
Kent, J. M. et al. Specificity of panic response to CO2 inhalation in panic disorder: a comparison with major depression and premenstrual dysphoric disorder. Am. J. Psychiatry. 158, 58–67 (2001).
Monkul, E. S. et al. History of suffocation, state-trait anxiety, and anxiety sensitivity in predicting 35% carbon dioxide-induced panic. Psychiatry Res. 179, 194–197 (2010).
Griez, E. J., Colasanti, A., Van Diest, R., Salamon, E. & Schruers, K. Carbon dioxide inhalation induces dose-dependent and age-related negative affectivity. PLoS One 2, e987 (2007).
Leibold, N. K. et al. Carbon dioxide inhalation as a human experimental model of panic: the relationship between emotions and cardiovascular physiology. Biol. Psychol. 94, 331–340 (2013).
Bailey, J. E. & Nutt, D. J. GABA-A receptors and the response to CO2 inhalation-A translational trans-species model of anxiety? Pharmacol. Biochem. Behav. 90, 51–57 (2008).
Bailey, J. E., Kendrick, A., Diaper, A., Potokar, J. P. & Nutt, D. J. A validation of the 7.5% CO2 model of GAD using paroxetine and lorazepam in healthy volunteers. J. Psychopharmacol. 21, 42–49 (2007).
Nardi, A. E., Valença, A. M., Zin, W. & Nascimento, I. Carbon dioxide induced panic attacks and short term clonazepam treatment: preliminary study. Arq. Neuropsiquiatr. 57, 361–365 (1999).
Concas, A., Sanna, E., Cuccheddu, T. & Paola, M. Carbon dioxide inhalation, stress and anxiogenic drugs reduce the function of GABA A receptor complex in the rat brain. Prog. Neuropsychopharmacol. Biol. Psychiatry 17, 651–661 (1993).
Sanna, E., Cuccheddu, T., Serra, M., Concas, A. & Biggio, G. Carbon dioxide inhalation reduces the function of GABAA receptors in the rat brain. Eur. J. Pharmacol. 216, 457–458 (1992).
Cuccheddu, T. et al. Proconflict effect of carbon dioxide inhalation in rats. Life. Sc. 56, PL321–PL324 (1995).
Johnson, P. L. et al. Orexin 1 and 2 receptor involvement in CO2-induced panic-associated behavior and autonomic responses. Depress. Anxiety 32, 671–683 (2015).
Damasio, A. R. Emotions and feelings (eds Manstead, A. S., Frijda, N. & Fischer, A.) (Cambridge University Press, 2004).
Adolphs, R. The biology of fear. Curr. Biol. 23, R79–R93 (2013).
Panksepp, J. The affective brain and core consciousness: How does neural activity generate emotional feelings? (eds Lewis, M., Haviland-Jones, J. M. & Barrett, L. F.) (Guilford Press 2008).
Weary, D. M., Droege, P. & Braithwaite, V. A. Evidence of Felt Emotions: Approaches, Inferences, and Refinements. Adv. Stud. Behav. 49, 27–48 (2017).
Miao, Y. L. et al. Midazolam ameliorates the behavior deficits of a rat posttraumatic stress disorder model through dual 18 kDa translocator protein and central benzodiazepine receptor and neurosteroidogenesis. PLoS One 9, e101450 (2014).
McGregor, I. S., Hargreaves, G. A., Apfelbach, R. & Hunt, G. E. Neural correlates of cat odor-induced anxiety in rats: region-specific effects of the benzodiazepine midazolam. J. Neurosc. 24, 4134–4144 (2004).
Dielenberg, R. A., Arnold, J. C. & McGregor, I. S. Low-dose midazolam attenuates predatory odor avoidance in rats. Pharmacol. Biochem. Behav. 62, 197–201 (1999).
Yerbury, R. E. & Cooper, S. J. The benzodiazepine partial agonists, Ro16-6028 and Ro17-1812, increase palatable food consumption in nondeprived rats. Pharmacol. Biochem. Behav. 28, 427–431 (1987).
Pain, L., Oberling, P., Sandner, G. & Di Scala, G. Effect of midazolam on propofol-induced positive affective state assessed by place conditioning in rats. Anesthesiology 87, 935–943 (1997).
Kissin, I., Brown, P. T. & Bradley, J. E. Locomotor activity after recovery from hypnosis: midazolam-morphine versus midazolam. Anesth. Analg. 75, 929–931 (1992).
Bertoglio, L. J. & Carobrez, A. P. Prior maze experience required to alter midazolam effects in rats submitted to the elevated plus-maze. Pharmacol. Biochem. Behav. 72, 449–455 (2002).
Ramos, A. Animal models of anxiety: do I need multiple tests? Trends Pharmacol. Sc. 29, 493–498 (2008).
Salonen, M., Onaivi, E. S. & Maze, M. Dexmedetomidine synergism with midazolam in the elevated plus-maze test in rats. Psychopharmacology 108, 229–234 (1992).
Treit, D. A comparison of anxiolytic and nonanxiolytic agents in the shock-probe/burying test for anxiolytics. Pharmacol. Biochem. Behav. 36, 203–205 (1990).
Mandema, J. W., Tukker, E. & Danhof, M. Pharmacokinetic-pharmacodynamic modelling of the EEG effects of midazolam in individual rats: influence of rate and route of administration. Br. J. Pharmacol 102, 663–668 (1991).
Balcombe, J. P., Barnard, N. D. & Sandusky, C. Laboratory routines cause animal stress. J. Am. Assoc. Lab. Anim. Sci. 43, 42–51 (2004).
Andrews, N., Zharkovsky, A. & File, S. E. Acute handling stress downregulates benzodiazepine receptors: reversal by diazepam. Eur. J. Pharmacol. 210, 247–251 (1992).
Gruen, R. J., Wenberg, K., Elahi, R. & Friedhoff, A. J. Alterations in GABA A receptor binding in the prefrontal cortex following exposure to chronic stress. Brain. Res. 684, 112–114 (1995).
Vinkers, C. H. et al. Stress-induced hyperthermia is reduced by rapid-acting anxiolytic drugs independent of injection stress in rats. Pharmacol. Biochem. Behav. 93, 413–418 (2009).
Davis, H. & Pérusse, R. Human-based social interaction can reward a rat’s behavior. Anim. Learn. Behav. 16, 89–92 (1988).
Lapin, I. P. Only controls: effect of handling, sham injection, and intraperitoneal injection of saline on behavior of mice in an elevated plus-maze. J. Pharmacol. Toxicol. Methods. 34, 73–77 (1995).
Pritchard, L. M., Van Kempen, T. A. & Zimmerberg, B. Behavioral effects of repeated handling differ in rats reared in social isolation and environmental enrichment. Neurosci. Lett. 536, 47–51 (2013).
Biro, P. A. Do rapid assays predict repeatability in labile (behavioural) traits? Anim. Behav. 83, 1295–1300 (2012).
Berridge, K. C. & Peciña, S. Benzodiazepines, appetite, and taste palatability. Neurosci. Biobehav. Rev. 19, 121–131 (1995).
Shimura, T., Kamada, Y. & Yamamoto, T. Ventral tegmental lesions reduce overconsumption of normally preferred taste fluid in rats. Behav. Brain. Res. 134, 123–130 (2002).
Bailey, J. E., Argyropoulos, S. V., Kendrick, A. H. & Nutt, D. J. Behavioral and cardiovascular effects of 7.5% CO2 in human volunteers. Depress. Anxiety 21, 18–25 (2005).
Poma, S. Z. et al. Anxiolytic effects of vestipitant in a sub-group of healthy volunteers known to be sensitive to CO2 challenge. J. Psychopharmacol. 28, 491–497 (2014).
van Beek, N. & Griez, E. Reactivity to a 35% CO2 challenge in healthy first-degree relatives of patients with panic disorder. Biol. Psychiatry 47, 830–835 (2000).
Verburg, K., Pols, H., de Leeuw, M. & Griez, E. Reliability of the 35% carbon dioxide panic provocation challenge. Psychiatry. Res. 78, 207–214 (1998).
Bailey, J. E., Papadopoulos, A., Seddon, K. & Nutt, D. J. A comparison of the effects of a subtype selective and non-selective benzodiazepine receptor agonist in two CO2 models of experimental human anxiety. J. Psychopharmacol. 23, 117–122 (2009).
Diaper, A. et al. The effect of a clinically effective and non-effective dose of lorazepam on 7.5% CO2-induced anxiety. Hum. Psychopharmacol. 27, 540–548 (2012).
Johnson, P. L. et al. Activation of the orexin 1 receptor is a critical component of CO2-mediated anxiety and hypertension but not bradycardia. Neuropsychopharmacology 37, 1911–1922 (2012).
Monfils, M. H. et al. Predicting extinction phenotype to optimize fear reduction. Psychopharmacology 236, 99–110 (2019).
Button, K. S. et al. Power failure: why small sample size undermines the reliability of neuroscience. Nat. Rev. Neurosci. 14, 365 (2013).
Archer, J. Tests for emotionality in rats and mice: a review. Anim. Behav. 21, 205–235 (1973).
Eilam, D. Open-field behavior withstands drastic changes in arena size. Behav. Brain Res. 142, 53–62 (2003).
Makowska, I. J. & Weary, D. M. Differences in anticipatory behaviour between rats (Rattus norvegicus) housed in standard versus semi-naturalistic laboratory environments. PloS One 11, e0147595 (2016).
Makowska, I. J. & Weary, D. M. The importance of burrowing, climbing and standing upright for laboratory rats. R. Soc. Open. Sci. 3, 160136 (2016).
Prut, L. & Belzung, C. The open field as a paradigm to measure the effects of drugs on anxiety-like behaviors: a review. Eur. J. Pharmacol. 463, 3–33 (2003).
Romero, R. D. & Chen, W. J. A. Gender-related response in open-field activity following developmental nicotine exposure in rats. Pharmacol. Biochem. Behav. 78, 675–681 (2004).
Wehrmeister, T. D., Izídio, G. S., Pereira, E., Izídio, G. & Ramos, A. Absence of repeated-trial tolerance to the anxiolytic-like effects of chlordiazepoxide in the rat triple test. Pharmacol. Biochem. Behav. 97, 301–309 (2010).
Friard, O. & Gamba, M. BORIS: a free, versatile open-source event-logging software for video/audio coding and live observations. Methods. Ecol. Evol. 7, 1325–1330 (2016).
Fernandes, C. & File, S. E. The influence of open arm ledges and maze experience in the elevated plus-maze. Pharmacol. Biochem. Behav. 54, 31–40 (1996).
Treit, D., Menard, J. & Royan, C. Anxiogenic stimuli in the elevated plus-maze. Pharmacol. Biochem. Behav. 44, 463–469 (1993).
Acknowledgements
We thank Marina Von Keyserlingk, Becca Franks and Joanna Makowska for their helpful comments and suggestions. We are especially grateful to Catherine Schuppli for her help with all stages of this study. We also thank Delea Carrillo and Jackson Lai for assistance in caring for our rats. This research was funded by an NSERC Discovery grant to D.M.W. L.A. was supported by the CONACyT PhD scholarship (no. 381124) and the Charles River Scholarship in Animal Welfare.
Author information
Authors and Affiliations
Contributions
Conceptualization and experimental design (L.A., A.R. and D.M.W.). Performed the experiment (L.A. and A.R.). Data curation (L.A.). Statistical analyses (L.A. and D.M.W.). Funding acquisition (D.M.W.). Writing of the manuscript (L.A., A.R. and D.M.W.).
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Améndola, L., Ratuski, A. & Weary, D.M. Variation in the onset of CO2-induced anxiety in female Sprague Dawley rats. Sci Rep 9, 19007 (2019). https://doi.org/10.1038/s41598-019-55493-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-55493-0
This article is cited by
-
Understanding rat emotional responses to CO2
Translational Psychiatry (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.