Abstract
This systematic review and meta-analysis was designed to investigate whether maternal psychological stress and recent life events are associated with an increased risk of miscarriage. A literature search was conducted to identify studies reporting miscarriage in women with and without history of exposure to psychological stress (the only exposure considered). The search produced 1978 studies; 8 studies were suitable for analysis. A meta-analysis was performed using a random-effects model with effect sizes weighted by the sampling variance. The risk of miscarriage was significantly higher in women with a history of exposure to psychological stress (OR 1.42, 95% CI 1.19–1.70). These findings remained after controlling for study type (cohort and nested case-control study OR 1.33 95% CI 1.14–1.54), exposure types (work stress OR 1.27, 95% CI 1.10–1.47), types of controls included (live birth OR 2.82 95% CI: 1.64–4.86). We found no evidence that publication bias or study heterogeneity significantly influenced the results. Our finding provides the most robust evidence to date, that prior psychological stress is harmful to women in early pregnancy.
Similar content being viewed by others
Introduction
Spontaneous pregnancy loss is the most common complication of pregnancy1, 2; it occurs before 24 weeks of gestation in around 20% of pregnancies3,4,5 and in 12–15% of clinically recognized pregnancies6. However, many cases of miscarriage are unreported; especially those involving early fetal loss, so the incidence may be even higher7. Only a small proportion (<10%) of women who experience miscarriage report recurrent pregnancy loss7 and as many as a third of pregnancy losses are not linked to chromosomal abnormalities5. Miscarriage is often associated with high levels of distress for women, their partners and families; therefore, every potential cause of miscarriage should be investigated. The evidence relating stress to spontaneous miscarriage is conflicting. Women reporting one or more recent negative life events prior to miscarriage were twice as likely to have a chromosomally normal spontaneous abortion8, even after adjusting for life-style factors9 and a similar two-fold increase in miscarriage was found in women with a history of exposure to psychological stress1. Stress (e.g. financial or marital problems, death, divorce, physical and nonphysical abuse inflicted on a woman by her partner and loss of social support) was also associated with the likelihood of miscarriage among women reporting to an emergency department or admission to hospital10, 11.Psychological challenges can include the experience of emotional trauma, social problems, concerns about money, marital/partnership disharmony, work pressure, significant change in personal circumstances as well as prior pregnancy loss12. In addition, retrospective studies link increase in workplace demands with adverse pregnancy outcomes including miscarriage7, 13.
On the other hand, possibly because of a desire not to exacerbate women’s concerns, many doctors discount any association between stress and miscarriage. In the UK for example, an NHS website (http://www.nhs.uk/Conditions/Miscarriage/Pages/Causes.aspx) advises mothers that the risk of miscarriage being related to a mother’s emotional state is a “common misconception”. Perhaps because of a lack of evidence, opposing opinions regarding stress as a cause of miscarriage are widely held.
Further evidence of a link between stress and adverse reproductive outcomes comes from animal studies; for example, among non-domesticated animals, re-location and exposure to unfamiliar conspecifics can lead to sufficient stress to cause miscarriage14. The negative effect of stress on the nervous, endocrine and immune systems of mice is also associated with abortion15.
The belief that stress at the time of conception or during pregnancy can harm their baby, causing problems such as miscarriage, is widely held amongst women. For example, 76% of women attending an antenatal clinic in the USA, thought that a mother’s stress can negatively affect pregnancy outcome, with 35% believing that pregnant women should avoid upsetting things like violent programs or funerals16. Women in that study were interpreting the term “stress” in its psychological form i.e. they experience negative emotionality when their physical or psychological well-being is threatened. Some doctors and midwives share this view although they know that fetal chromosomal abnormality is present in around two thirds of cases of early pregnancy failure5. Other risk factors for miscarriage include increased maternal age, obesity, caffeine17, alcohol7, 18, 19, cigarette smoke20, 21 and exercise22.
The diverse views held by women and healthcare professionals demonstrate the need for evidence in this vital area of human wellbeing. Awareness of the effects of psychosocial stress could lead to improved strategies for screening psychological support and changes in employment practices. This systematic review and meta-analysis as therefore designed to investigate whether maternal psychological stress is associated with an increased risk of miscarriage.
Results
Characteristics of included studies
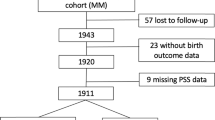
The search strategy produced 1978 studies; of which, 1896 studies with irrelevant title and/or abstract were excluded. Full text papers were retrieved for 82 studies and 74 studies were further excluded in compliance with the criteria defined in methods section. A final number of 8 studies were included for the meta-analysis. Details of the study selection process were presented in Fig. 1.
Characteristics of all studies included in the systematic review were shown as Table 1. Of the 8 included studies, 4 are case-control studies, 3 are cohort studies, and 1 is a nested case-control study. The sample size in these studies ranged from 96 to 6945. All of the 8 included studies reported odds ratio (OR) with 95% confidence interval (CI) as the outcome measure of the association between psychological stress and miscarriage1, 2, 7, 8, 10, 11, 13, 23.
Quality assessment and publication bias
Results from Newcastle-Ottawa Scale (NOS) indicated that six of our included studies were rated7–9 stars whereas two studies were rated 6 stars (shown as Supplementary Table S1). Seven studies achieved high comparability by adjusting for or matching on at least one of the following confounders: maternal age, gestational age, pregnancy history, caffeine and tobacco consumption, and social support. Begg’s rank correlation test (p = 0.536), Egger’s linear regression test (p = 0.170) and the funnel plot (shown as Supplementary Figure S1) suggested that there was no significant publication bias.
Effect size analysis
We evaluated for the outliers before starting the analysis, and found no extreme values. As presented in Fig. 2, the overall pooled OR was 1.42 (95% CI 1.19 to 1.70) with moderate heterogeneity (I2 = 35.6%), indicating that maternal psychological stress is significantly associated with an increased risk of miscarriage.
Subgroup analysis was conducted to explore the sources of the heterogeneity (presented in Table 2). There was positive association between psychological stress and miscarriage for the type of study (OR: 1.69 for case-control studies; 1.33 for cohort and nested case-control study).However, the OR was statistically significant only for cohort and nested case-control studies (OR, 1.33; 95% CI, 1.14–1.54; P < 0.001). Moreover, substantial heterogeneity (I2 = 62.1%) was reported for case-control studies, whereas for cohort and nested case-control study, heterogeneity was low (I2 = 0.0%).
Exposures in the included studies were divided into three types: psychological stress, life events and work stress. In terms of subgroup analysis based on exposure factors, we found that there was no heterogeneity (I2 = 0.0%) between studies concerning work stress7, 13, 23. We found that work stress was significantly associated with an increased risk of miscarriage (OR, 1.27; 95% CI, 1.10–1.47; P = 0.001).
In subgroup analysis according to the types of controls, psychological stress was observed to have the greatest impact on miscarriage when the comparison group consisted of women who had a live birth (OR, 2.82; 95% CI, 1.64–4.86; P < 0.001)1, 11.
We further categorized the eight included studies by NOS scores; heterogeneity decreased (I2 = 21.7%) when the two lower quality studies were excluded1, 13. After removing the study not controlling for potential confounding factors1, the pooled OR slightly decreased to 1.34 (95% CI 1.16 to 1.54; I2 = 9.2%). Results from sensitivity analysis (i.e. excluding one study at a time) demonstrated that none of the studies caused significant heterogeneity compared with the rest, or strongly influenced the results (shown as Supplementary Figure S2).
Discussion
The results of this meta-analysis support the belief that psychological stress before and during pregnancy is associated with miscarriage. A view held by some medical practitioners and around three quarters of pregnant women, but most often dismissed by doctors and other health care professionals. Whilst chromosomal abnormalities underlie many cases of early pregnancy loss, the present results show that these psychological factors can increase the risk by approximately 42%.
Psychological stress can influence well-being through associated health-impairing behaviors and through physiological responses which affect vascular, immune, metabolic or neuroendocrine functions24. The experience of stress can originate in a wide range of circumstances and is defined as “any situation that overwhelms our ability to cope”25. Therefore, the experience of stress varies, not only by an individual’s internal resources but also by the social and material support which is available to them. Effects are difficult to assess as physiological responses to stress vary with its intensity and duration, and are contingent on the genetic vulnerability and life history of the affected individual26. For example, the degree of stress experienced in infancy and childhood have implications for the individual’s subsequent physiological response to stress25. Persistent stressors, which are perceived as uncontrollable, are the most damaging to physical and mental health25. However, as far as the authors are aware, different classes of stress do not systematically elicit differential physiological responses.
Because of the complexity of the mechanisms and the degree of individual variation in the response to stressors, accurate measurement and comparisons of the experience of stress between individuals or groups of individuals is challenging. Psychological stress is also likely to co-occur with other psychological factors such as anxiety and depression27 and may be chronic, acute or transient. A variety of relevant scales have been applied in specific studies, for example, the Perceived Stress Scale28, the Pre-natal Social Environment Inventory29 and Index of Spousal Abuse30 and others pertaining more generally to life events and stress symptoms, thus making simple comparisons between studies difficult. Retrospective reports, both from focal groups and controls, may be especially vulnerable to recall bias. Even a small indicator of prospective miscarriage, or history of previous miscarriage, is likely to produce stress, therefore confounding the direction of effects. In addition, many miscarriages are managed at home and never reported7. Estimating miscarriage risk is further complicated by the difficulty in distinguishing the effect of stress from the effects of substances like alcohol, tobacco and caffeine which are taken to relieve stress.
Based on the considerations described above, interpretation of the findings from this meta-analysis is subject to some caution; the included studies also vary by the types of stress under focus and their prospective or retrospective design. The measures of stress vary between studies and do not always assess symptoms directly8, 13 and some scales do not specify cut-off points between high and low stress (e.g. Perceived Stress Scale). Participant self-reports are often retrospective with an associated risk of recall bias, as authors generally acknowledge11, 13. Whilst the NOS assessment provided a means to assess non-randomized studies, the scoring system itself is not without its drawbacks and criticisms31. Study quality is also variable: some offer limited detail on assessment1, 7, 23, on case selection procedures1 and on timing of assessment in relation to outcome1. Therefore we propose the need for high quality research into an association between the experience of stress in a variety of contexts and miscarriage risk.
In the present meta-analysis, on sub analysis, six studies with higher quality showed a significantly increased miscarriage risk in women suffering from psychological stress, but this was not found in the two studies with lower NOS scores. An increased miscarriage risk was found on analysis of cohort and nested case-control but not in case-control studies. For case-controls, the variability is also much larger (leading to an interval including 0). The explanation for this possibly relates to the smaller number of studies (hence larger variability), or perhaps the increased level of heterogeneity intrinsic in case-controls. However inclusion or exclusion of confounders did not affect the results.
The association between psychological stress and miscarriage could result, at least in part, from activation of the hypothalamic-pituitary-adrenal axis by recruitment of hypothalamic neurones which secrete corticotrophin-releasing hormone, increasing pituitary secretion of adrenocorticotrophic hormone secretion and hence of adrenal cortisol32. This hormone has direct effects on decidual and placental metabolism but also interacts with progesterone signalling32. Stress-related early pregnancy failure could also result from suppression of the hypothalamic-pituitary-gonadal axis32,33,34,35. Although generally considered a “stress hormone”, prolactin production is decreased by stress in early pregnancy14, 32, 36. Since prolactin stimulates progesterone secretion, the reduced levels will decrease progesterone synthesis37, 38. Stress also inhibits pituitary human chorionic gonadotropin secretion compounding the effect of prolactin on progesterone release from the corpus luteum32, 39, 40. These mechanisms are relevant because progesterone activity is crucial for the maintenance of pregnancy; low levels in early of gestation predicting miscarriage32. Among its multiple effects, this hormone contributes to the suppression of maternal immune response to the conceptus32.
In summary, the result of this systematic review and meta-analysis support the belief that psychological stress, including life events and occupational stress, in pregnancy is associated with an increased risk of miscarriage and indicates a critical need for further high quality research into the relationship between miscarriage and stress experienced prior to pregnancy and in the early gestational period. Taken together with the serious morbidities already known to be associated with stress (pregnancy induced hypertension, preterm birth and low birth weight), this finding also highlights the need to include a structured psychological assessment in early pregnancy into routine antenatal care. This demonstration that stress contributes to early pregnancy failure could provide the basis for novel and effective interventions in this field. As far as we are aware there have been no randomized trials of psychological therapy to prevent miscarriage, however Liddell, Pattison and Zanderigo41 reported a live birth rate of 86% in women with recurrent (≥3) miscarriages who were enrolled into a program of emotional support, compared to 33% in similar women who had no formal supportive care. Twenty-five years later, the results of our meta-analysis, highlight the potential to identify and treat psychological factors which contribute to adverse pregnancy outcomes in the human.
Methods
Literature search
We searched the following databases for published articles and conference abstracts and proceedings in consultation with a search methodologist, using the Medline search strategy below (with minor modifications to account for different controlled vocabularies and syntax): MEDLINE (Ovid, 1946 – June, 2016), EMBASE (Ovid, 1980 – June, 2016), PsycINFO (Ovid, 1806 – June, 2016), CINAHL plus (EBSCO, 1937 – June, 2016), Maternity & Infant Care (Ovid, 1971 – June, 2016), and Conference Proceedings Citation Index - Science (CPCI-S, 1990 – June, 2016). No language or date restrictions were applied.
Search strategy: (1) exp abortion, spontaneous/; (2) ((tubal or threatened or missed or spontaneous or recurrent or incomplete or inevitable or habitual or septic) adj abortion*).mp;(3) miscarr*.ti,ab;(4) ((pregnancy or embryo) adj3 (loss or failure)).mp; (5) blighted ovum.mp;(6)misbirth.mp; (7) exp fetal death/; (8) ((fetal or foetal or fetus or foetus or intrauterine or antepartum or prenatal) adj (death or resorption or mummification)).ti,ab; (9)or/1–8; (10) exp stress, psychological/;(11)anxiety/; (12)exp stress disorders, traumatic/; (13) panic disorder/; (14)((stress* or distress* or anxiety or PTSD or panic) not oxidative).ti,ab;(15)life change events/; (16) (life adj2 event*).ti,ab;(17)or/10–16; (18) exp risk factors/or exp risk/; (19) risk*.ti,ab;(20) 18 or 19; (21) 9 and 17 and 20.
We only included case-control, cohort (retrospective or prospective) and nested case-control studies for this review and for studies that reported similar or overlapping data, only the latest or those with a larger sample size were considered.
Only studies that included women who had miscarriage (cases) and women with ongoing pregnancy or live birth (controls) were considered for eligibility. Miscarriage or pregnancy loss occurring before the first 22 weeks gestation is defined as the natural death of an embryo or fetus before it is able to survive independently. The following exclusion criteria were applied: (i) psychological stress was induced by miscarriage; (ii) psychological stress and/or miscarriage-related data could not be retrieved; (iii) women had mental or psychological disorders before pregnancy; (iv) no relevant comparison or available control were present; (v) psychological stress before miscarriage (including anxiety, depression, life event, work/job stress, etc.) was not the only exposure factor.
Three authors(F.Q., Y.W., and Y.Z) independently reviewed and selected the articles in compliance with the inclusion/exclusion criteria. Disagreement was resolved by consensus or arbitration.
Study coding
The following information was recorded or coded for each article: country, year, study design, study population characteristics, total sample size, stress measurement methods of the studies, sample size related to our meta-analysis and outcome data. All the reviewers cross-checked the extracted data repeatedly and any disagreements were resolved by consensus. Authors were contacted for further details if necessary.
The quality of the included studies was assessed independently by three authors (F.Q., Y.W. and Y.Z.) using NOS42. Different assessment items were applied to case-control and cohort studies, respectively. For each type of study, eight criteria were used in the assessment, namely (1) for cohort studies: representativeness of exposed cohort, selection of non-exposed cohort, ascertainment of exposure, outcome not present at baseline, comparability of cohorts, assessment of outcome, sufficient follow-up duration, and adequate follow-up; (2) for case-control studies: adequate definition of cases, representativeness of cases, selection of controls, definition of controls, comparability of cases and controls, ascertainment of exposure, same method of ascertainment for cases and controls, and non-response rate. The total score for each study was obtained by summing up stars from each item. More than six stars indicate good quality, whereas 5–6 stars indicate acceptable quality. Disagreements were resolved by consensus.
Meta-analysis procedures
Data were all presented as OR with 95% confidence interval CI. We firstly evaluated for the outliers, defining as that the individual ORs were more than 2 standard deviations from the mean of all the effect sizes, to see if replacement of extreme values is necessary. The statistical analysis was performed in STATA 12.0 software (StataCorp, College Station, USA). This provided effect sizes weighted by the sampling variance, with a 95% confidence interval and a measure of heterogeneity. DerSimonian and Laird random-effects model was employed, as our effect sizes were assumed to be sampled from a large number of possible sample sizes. Heterogeneity between studies was evaluated using homogeneity statistic (Q), which follows a Chi-square distribution with a degree of freedom of (n-1) where n is the total number of studies included43. I2 statistic was also used to evaluate the heterogeneity, and results were deemed significance in correspondence of a Chi-squared test with p < 0.10 or I2 > 50%43, 44. Subgroup analysis was conducted to explore the sources of the heterogeneity, and sensitivity analysis was performed to examine the effect of excluding each study. Publication bias was examined through visual inspection of a funnel plot, and further evaluated by Begg’s and Egger’s tests45 (p < 0.05 indicated a significant publication bias).
References
Bashour, H. & Abdul Salam, A. Psychological stress and spontaneous abortion. Int J Gynaecol Obstet. 73, 179–181 (2001).
Meaney, S. et al. Perceived maternal stress and emotional wellbeing as risk factors for miscarriage. J Epidemiol Community Health. 68, A31–A32 (2014).
Garcia-Enguidanos, A., Calle, M. E., Valero, J., Luna, S. & Dominguez-Rojas, V. Risk factors in miscarriage: a review. Eur J Obstet Gynecol Reprod Biol. 102, 111–119 (2002).
Savitz, D. A., Hertz-Picciotto, I., Poole, C. & Olshan, A. F. Epidemiologic measures of the course and outcome of pregnancy. Epidemiol Rev. 24, 91–101 (2002).
Wilcox, A. J. et al. Incidence of early loss of pregnancy. N Engl J Med. 319, 189–194 (1988).
Regan, L., Braude, P. R. & Trembath, P. L. Influence of past reproductive performance on risk of spontaneous abortion. BMJ. 299, 541–545 (1989).
Maconochie, N., Doyle, P., Prior, S. & Simmons, R. Risk factors for first trimester miscarriage–results from a UK-population-based case-control study. BJOG. 114, 170–186 (2007).
Boyles, S. H. et al. Life event stress and the association with spontaneous abortion in gravid women at an urban emergency department. Health Psychol. 19, 510–514 (2000).
Neugebauer, R. et al. Association of stressful life events with chromosomally normal spontaneous abortion. Am J Epidemiol. 143, 588–596 (1996).
Nelson, D. B. et al. Does stress influence early pregnancy loss? Ann Epidemiol. 13, 223–229 (2003).
O’Hare, T. & Creed, F. Life events and miscarriage. Br J Psychiatry. 167, 799–805 (1995).
Kicia, M., Skurzak, A., Wiktor, K., Iwanowicz-Palus, G. & Wiktor, H. Anxiety and stress in miscarriage. Pol J Public Health. 125, 162–165 (2015).
Brandt, L. P. & Nielsen, C. V. Job stress and adverse outcome of pregnancy: a causal link or recall bias? Am J Epidemiol. 135, 302–311 (1992).
Li, X., Liu, X. & Yu, S. Psychological Stress-Derived Prolactin Modulates Occludin Expression in Vaginal Epithelial Cells to Compromise Barrier Function. Cell Physiol Biochem. 37, 153–161 (2015).
Arck, P. C. Stress and pregnancy loss: role of immune mediators, hormones and neurotransmitters. Am J Reprod Immunol. 46, 117–123 (2001).
Schaffir, J. Do patients associate adverse pregnancy outcomes with folkloric beliefs? Arch Womens Ment Health. 10, 301–304 (2007).
Weng, X., Odouli, R. & Li, D. K. Maternal caffeine consumption during pregnancy and the risk of miscarriage: a prospective cohort study. Am J Obstet Gynecol. 198, 279 e271-278 (2008).
Kesmodel, U., Wisborg, K., Olsen, S. F., Henriksen, T. B. & Secher, N. J. Moderate alcohol intake in pregnancy and the risk of spontaneous abortion. Alcohol Alcohol. 37, 87–92 (2002).
Windham, G. C., Fenster, L. & Swan, S. H. Moderate maternal and paternal alcohol consumption and the risk of spontaneous abortion. Epidemiology. 3, 364–370 (1992).
George, L., Granath, F., Johansson, A. L., Anneren, G. & Cnattingius, S. Environmental tobacco smoke and risk of spontaneous abortion. Epidemiology. 17, 500–505 (2006).
Venners, S. A. Paternal Smoking and Pregnancy Loss: A Prospective Study Using a Biomarker of Pregnancy. Am J Epidemiol. 159, 993–1001 (2004).
Madsen, M. et al. Leisure time physical exercise during pregnancy and the risk of miscarriage: a study within the Danish National Birth Cohort. BJOG. 114, 1419–1426 (2007).
Fenster, L. et al. Psychologic stress in the workplace and spontaneous abortion. Am J Epidemiol. 142, 1176–1183 (1995).
McEwen, B. S. Central effects of stress hormones in health and disease: Understanding the protective and damaging effects of stress and stress mediators. Eur J Pharmacol. 583, 174–185 (2008).
Gerhardt, S. Why love matters: How affection shapes a baby’s brain. Infant Observation. 9, 305–309 (2006).
DeRijk, R. H., Kitraki, E. & de Kloet, E. R. Corticosteroid Hormones in Stress and Anxiety–Role of Receptor Variants and Environmental Inputsin. Stress-From Molecules to Behavior: A Comprehensive Analysis of the Neurobiology of Stress Responses (eds Soreq, H., Friedman, A. & Kaufer, D.) 117–150 (WILEY-VCH, 2009).
DiPietro, J. A., Novak, M. F., Costigan, K. A., Atella, L. D. & Reusing, S. P. Maternal psychological distress during pregnancy in relation to child development at age two. Child Dev. 77, 573–587 (2006).
Cohen, S., Kamarck, T. & Mermelstein, R. A global measure of perceived stress.J Health Soc Behav. 385–396 (1983).
Orr, S. T., James, S. A. & Casper, R. Psychosocial stressors and low birth weight: development of a questionnaire. J Dev Behav Pediatr. 13, 343–347 (1992).
Hudson, W. W. & McIntosh, S. R. The assessment of spouse abuse: Two quantifiable dimensions. J Marriage Fam. 873–888 (1981).
Stang, A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 25, 603–605 (2010).
Parker, V. J. & Douglas, A. J. Stress in early pregnancy: maternal neuro-endocrine-immune responses and effects. J Reprod Immunol. 85, 86–92 (2010).
Stergiakouli, E., Sterne, J. A. & Smith, G. D. Failure to replicate the association of glucocorticoid and type 1 corticotropin-releasing hormone receptors gene variants with risk of depression during pregnancy and post-partum reported by. J Psychiatr Res. 56, 168–170 (2014).
Castelo-Branco, C. et al. Unintended pregnancy after gonadal failure chemoprevention with gonadotropin-releasing hormone agonist in women with hematologic malignancies. Fertil Steril. 92, 1260–1263 (2009).
Takahashi, K., Ozaki, T., Kanasaki, H. & Miyazaki, K. Successful pregnancy in a woman with ovarian failure associated with mutation in the beta-subunit of luteinizing hormone. Horm Res. 55, 258–263 (2001).
Labad, J. et al. Stress biomarkers as predictors of transition to psychosis in at-risk mental states: roles for cortisol, prolactin and albumin. J Psychiatr Res. 60, 163–169 (2015).
Pennacchio, G. E., Neira, F. J., Soaje, M., Jahn, G. A. & Valdez, S. R. Effect of hyperthyroidism on circulating prolactin and hypothalamic expression of tyrosine hydroxylase, prolactin signaling cascade members and estrogen and progesterone receptors during late pregnancy and lactation in the rat. Mol Cell Endocrinol. 442, 40–50 (2016).
Varas, S. M. & Jahn, G. A. The expression of estrogen, prolactin, and progesterone receptors in mammary gland and liver of female rats during pregnancy and early postpartum: regulation by thyroid hormones. Endocr Res. 31, 357–370 (2005).
Surico, D. et al. Human Chorionic Gonadotropin Protects Vascular Endothelial Cells from Oxidative Stress by Apoptosis Inhibition, Cell Survival Signalling Activation and Mitochondrial Function Protection. Cell Physiol Biochem. 36, 2108–2120 (2015).
Kajihara, T. et al. Human chorionic gonadotropin confers resistance to oxidative stress-induced apoptosis in decidualizing human endometrial stromal cells. Fertil Steril. 95, 1302–1307 (2011).
Liddell, H. S., Pattison, N. S. & Zanderigo, A. Recurrent Miscarriage - Outcome after Supportive Care in Early-Pregnancy. Aust N Z J Obstet Gynaecol. 31, 320–322 (1991).
Wells, G. et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses, http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (2011) (Date of access: 22/06/2016).
Hedges, L. V. & Olkin, I. Statistical methods for meta-analysis. (Academic press, 2014).
Lipsey, M. W. & Wilson, D. B. Practical meta-analysis. (Sage Publications, Inc, 2001).
Egger, M., Smith, G. D., Schneider, M. & Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 315, 629–634 (1997).
Author information
Authors and Affiliations
Contributions
P.H. conceived and designed the study. F.Q., J.B., R.M. and P.H. developed the search strategy for the identification of articles and identified the articles. F.Q., Y.W., Y.Z., T.D. and G.B. acquired and analysed the data. F.Q., Y.W., Y.Z., J.B., B.T. and P.H. drafted the manuscript. F.W. helped to revise the manuscript with all the other authors. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Qu, F., Wu, Y., Zhu, YH. et al. The association between psychological stress and miscarriage: A systematic review and meta-analysis. Sci Rep 7, 1731 (2017). https://doi.org/10.1038/s41598-017-01792-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-01792-3
This article is cited by
-
Effects of improved on-farm crop storage on DNA methylation of mothers and their infants: evidence from a randomized controlled trial in Kenya
Clinical Epigenetics (2024)
-
Reproductive health of Syrian refugee women in Lebanon: a descriptive analysis of the Sijilli electronic health records database
BMC Women's Health (2023)
-
Psychosocial adaptation, marital satisfaction and meaning in life between women with high and low-risk pregnancies
Current Psychology (2023)
-
Resilience, stress and anxiety in pregnancy before and throughout the pandemic: a structural equation modelling approach
Current Psychology (2023)
-
Risk factors for miscarriage in Syrian refugee women living in non-camp settings in Jordan: results from the Women ASPIRE cross-sectional study
Conflict and Health (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.