Abstract
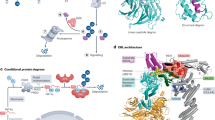
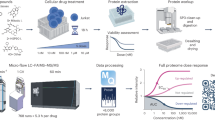
Despite decades of research, little is known about the cellular targets and the mode of action of the vast majority of antimalarial drugs. We recently demonstrated that the cellular thermal shift assay (CETSA) protocol in its two variants: the melt curve and the isothermal dose-response, represents a comprehensive strategy for the identification of antimalarial drug targets. CETSA enables proteome-wide target screening for unmodified antimalarial compounds with undetermined mechanisms of action, providing quantitative evidence about direct drug–protein interactions. The experimental workflow involves treatment of P. falciparum–infected erythrocytes with a compound of interest, heat exposure to denature proteins, soluble protein isolation, enzymatic digestion, peptide labeling with tandem mass tags, offline fractionation, and liquid chromatography–tandem mass spectrometry analysis. Methodological optimizations necessary for the analysis of this intracellular parasite are discussed, including enrichment of parasitized cells and hemoglobin depletion strategies to overcome high hemoglobin abundance in the host red blood cells. We outline an effective data processing workflow using the mineCETSA R package, which enables prioritization of drug–target candidates for follow-up studies. The entire protocol can be completed within 2 weeks.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
mineCETSA has been deposited on GitHub (https://github.com/nkdailingyun/mineCETSA) and is covered under the GNU General Public License, v.3.0 (GPL-3.0). The code in this protocol has been peer-reviewed.
References
World Health Organization. World Malaria Report 2019 (2019).
Leang, R. et al. Evidence of Plasmodium falciparum malaria multidrug resistance to artemisinin and piperaquine in Western Cambodia: dihydroartemisinin-piperaquine open-label multicenter clinical assessment. Antimicrob. Agents Chemother. 59, 4719–4726 (2015).
Dondorp, A. M. et al. Artemisinin resistance in Plasmodium falciparum malaria. N. Engl. J. Med. 361, 455–467 (2009).
Amaratunga, C. et al. Artemisinin-resistant Plasmodium falciparum in Pursat province, western Cambodia: a parasite clearance rate study. Lancet Infect. Dis. 12, 851–858 (2012).
Thriemer, K. et al. Delayed parasite clearance after treatment with dihydroartemisinin-piperaquine in Plasmodium falciparum malaria patients in central Vietnam. Antimicrob. Agents Chemother. 58, 7049–7055 (2014).
Phyo, A. P. et al. Declining efficacy of artemisinin combination therapy against P. Falciparum malaria on the Thai-Myanmar border (2003-2013): the role of parasite genetic factors. Clin. Infect. Dis. 63, 784–791 (2016).
Muller, I. B. & Hyde, J. E. Antimalarial drugs: modes of action and mechanisms of parasite resistance. Future Microbiol. 5, 1857–1873 (2010).
Schlitzer, M. Malaria chemotherapeutics part I: history of antimalarial drug development, currently used therapeutics, and drugs in clinical development. ChemMedChem. 2, 944–986 (2007).
Corey, V. C. et al. A broad analysis of resistance development in the malaria parasite. Nat. Commun. 7, 11901 (2016).
Flannery, E. L., Fidock, D. A. & Winzeler, E. A. Using genetic methods to define the targets of compounds with antimalarial activity. J. Med. Chem. 56, 7761–7771 (2013).
Pradhan, A. et al. Chemogenomic profiling of Plasmodium falciparum as a tool to aid antimalarial drug discovery. Sci. Rep. 5, 15930 (2015).
Hu, G. et al. Transcriptional profiling of growth perturbations of the human malaria parasite Plasmodium falciparum. Nat. Biotechnol. 28, 91–98 (2010).
Ismail, H. M. et al. Artemisinin activity-based probes identify multiple molecular targets within the asexual stage of the malaria parasites Plasmodium falciparum 3D7. Proc. Natl Acad. Sci. USA 113, 2080–2085 (2016).
Allman, E. L., Painter, H. J., Samra, J., Carrasquilla, M. & Llinas, M. Metabolomic profiling of the malaria box reveals antimalarial target pathways. Antimicrob. Agents Chemother. 60, 6635–6649 (2016).
Creek, D. J. et al. Metabolomics-based screening of the malaria box reveals both novel and established mechanisms of action. Antimicrob. Agents Chemother. 60, 6650–6663 (2016).
Edwards, R. L. & Odom John, A. R. Muddled mechanisms: recent progress towards antimalarial target identification. F1000Res. 5, 2514 (2016).
Jafari, R. et al. The cellular thermal shift assay for evaluating drug target interactions in cells. Nat. Protoc. 9, 2100–2122 (2014).
Martinez Molina, D. et al. Monitoring drug target engagement in cells and tissues using the cellular thermal shift assay. Science 341, 84–87 (2013).
Martinez Molina, D. & Nordlund, P. The cellular thermal shift assay: a novel biophysical assay for in situ drug target engagement and mechanistic biomarker studies. Annu. Rev. Pharmacol. Toxicol. 56, 141–161 (2016).
Savitski, M. M. et al. Tracking cancer drugs in living cells by thermal profiling of the proteome. Science 346, 1255784 (2014).
Dziekan, J. M. et al. Identifying purine nucleoside phosphorylase as the target of quinine using cellular thermal shift assay. Sci. Transl. Med. 11, eaau3174 (2019).
Franken, H. et al. Thermal proteome profiling for unbiased identification of direct and indirect drug targets using multiplexed quantitative mass spectrometry. Nat. Protoc. 10, 1567–1593 (2015).
Pasini, E. M. et al. In-depth analysis of the membrane and cytosolic proteome of red blood cells. Blood 108, 791–801 (2006).
Ringrose, J. H. et al. Highly efficient depletion strategy for the two most abundant erythrocyte soluble proteins improves proteome coverage dramatically. J. Proteome Res. 7, 3060–3063 (2008).
D’Amici, G. M., Rinalducci, S. & Zolla, L. An easy preparative gel electrophoretic method for targeted depletion of hemoglobin in erythrocyte cytosolic samples. Electrophoresis 32, 1319–1322 (2011).
Roux-Dalvai, F. et al. Extensive analysis of the cytoplasmic proteome of human erythrocytes using the peptide ligand library technology and advanced mass spectrometry. Mol. Cell. Proteomics 7, 2254–2269 (2008).
Walpurgis, K. et al. Validated hemoglobin-depletion approach for red blood cell lysate proteome analysis by means of 2D PAGE and Orbitrap MS. Electrophoresis 33, 2537–2545 (2012).
Klont, F. et al. Assessment of sample preparation bias in mass spectrometry-based proteomics. Anal. Chem. 90, 5405–5413 (2018).
Shaw, J. et al. Positioning high-throughput CETSA in early drug discovery through screening against B-Raf and PARP1. SLAS Discovery 24, 121–132 (2019).
Yang, S. M. et al. Discovery of orally bioavailable, quinoline-based aldehyde dehydrogenase 1A1 (ALDH1A1) inhibitors with potent cellular activity. J. Med. Chem. 61, 4883–4903 (2018).
Page, B. D. G. et al. Targeted NUDT5 inhibitors block hormone signaling in breast cancer cells. Nat. Commun. 9, 250 (2018).
Ishii, T. et al. CETSA quantitatively verifies in vivo target engagement of novel RIPK1 inhibitors in various biospecimens. Scientific Rep. 7, 13000 (2017).
Reinhard, F. B. et al. Thermal proteome profiling monitors ligand interactions with cellular membrane proteins. Nat. Methods 12, 1129–1131 (2015).
Kitagawa, M. et al. Dual blockade of the lipid kinase PIP4Ks and mitotic pathways leads to cancer-selective lethality. Nat. Commun. 8, 2200 (2017).
Corpas-Lopez, V. et al. Pharmacological validation of N-myristoyltransferase as a drug target in Leishmania donovani. ACS Infect. Dis. 5, 111–122 (2019).
Schenone, M., Dancik, V., Wagner, B. K. & Clemons, P. A. Target identification and mechanism of action in chemical biology and drug discovery. Nat. Chem. Biol. 9, 232–240 (2013).
Becher, I. et al. Thermal profiling reveals phenylalanine hydroxylase as an off-target of panobinostat. Nat. Chem. Biol. 12, 908–910 (2016).
Lim, Y. T. et al. An efficient proteome-wide strategy for discovery and characterization of cellular nucleotide-protein interactions. PLoS One 13, e0208273 (2018).
Dai, L. et al. Horizontal cell biology: monitoring global changes of protein interaction states with the proteome-wide cellular thermal shift assay (CETSA). Annu. Rev. Biochem. 88, 383-408 (2019).
Huber, K. V. et al. Proteome-wide drug and metabolite interaction mapping by thermal-stability profiling. Nat. Methods 12, 1055–1057 (2015).
Tan, C. S. H. et al. Thermal proximity coaggregation for system-wide profiling of protein complex dynamics in cells. Science 359, 1170–1177 (2018).
Dai, L. et al. Modulation of protein-interaction states through the cell cycle. Cell 173, 1481–1494.e1413 (2018).
Becher, I. et al. Pervasive protein thermal stability variation during the cell cycle. Cell 173, 1495–1507.e1418 (2018).
Sun, W. et al. Monitoring structural modulation of redox-sensitive proteins in cells with MS-CETSA. Redox Biol. 24, 101168 (2019).
Gunjan, S. et al. Mefloquine induces ROS mediated programmed cell death in malaria parasite: Plasmodium. Apoptosis 21, 955–964 (2016).
Rocamora, F. et al. Oxidative stress and protein damage responses mediate artemisinin resistance in malaria parasites. PLoS Pathog. 14, e1006930 (2018).
Bridgford, J. L. et al. Artemisinin kills malaria parasites by damaging proteins and inhibiting the proteasome. Nat. Commun. 9, 3801 (2018).
Meshnick, S. R. Artemisinin: mechanisms of action, resistance and toxicity. Int. J. Parasitol. 32, 1655–1660 (2002).
Cui, L., Mharakurwa, S., Ndiaye, D., Rathod, P. K. & Rosenthal, P. J. Antimalarial drug resistance: literature review and activities and findings of the ICEMR Network. Am. J. Trop. Med. Hyg. 93, 57–68 (2015).
Birth, D., Kao, W. C. & Hunte, C. Structural analysis of atovaquone-inhibited cytochrome bc1 complex reveals the molecular basis of antimalarial drug action. Nat. Commun. 5, 4029 (2014).
Summers, R. L. et al. Diverse mutational pathways converge on saturable chloroquine transport via the malaria parasite’s chloroquine resistance transporter. Proc. Natl Acad. Sci. USA 111, E1759–E1767 (2014).
Haldar, K. & Mohandas, N. Erythrocyte remodeling by malaria parasites. Curr. Opin. Hematol. 14, 203–209 (2007).
Maier, A. G., Cooke, B. M., Cowman, A. F. & Tilley, L. Malaria parasite proteins that remodel the host erythrocyte. Nat. Rev. Microbiol. 7, 341–354 (2009).
Moxon, C. A., Grau, G. E. & Craig, A. G. Malaria: modification of the red blood cell and consequences in the human host. Br. J. Haematol. 154, 670–679 (2011).
Luth, M. R., Gupta, P., Ottilie, S. & Winzeler, E. A. Using in vitro evolution and whole genome analysis to discover next generation targets for antimalarial drug discovery. ACS Infect. Dis. 4, 301–314 (2018).
Cowell, A. N. et al. Mapping the malaria parasite druggable genome by using in vitro evolution and chemogenomics. Science 359, 191–199 (2018).
Baragana, B. et al. A novel multiple-stage antimalarial agent that inhibits protein synthesis. Nature 522, 315–320 (2015).
Hoepfner, D. et al. Selective and specific inhibition of the Plasmodium falciparum lysyl-tRNA synthetase by the fungal secondary metabolite cladosporin. Cell Host Microbe 11, 654–663 (2012).
Istvan, E. S. et al. Validation of isoleucine utilization targets in I. Proc. Natl Acad. Sci. USA 108, 1627–1632 (2011).
Herman, J. D. et al. The cytoplasmic prolyl-tRNA synthetase of the malaria parasite is a dual-stage target of febrifugine and its analogs. Sci. Transl. Med. 7, 288ra277 (2015).
Lukens, A. K. et al. Harnessing evolutionary fitness in Plasmodium falciparum for drug discovery and suppressing resistance. Proc. Natl Acad. Sci. USA 111, 799–804 (2014).
Rottmann, M. et al. Spiroindolones, a potent compound class for the treatment of malaria. Science 329, 1175–1180 (2010).
Vaidya, A. B. et al. Pyrazoleamide compounds are potent antimalarials that target Na+ homeostasis in intraerythrocytic Plasmodium falciparum. Nat. Commun. 5, 5521 (2014).
Flannery, E. L. et al. Mutations in the P-type cation-transporter ATPase 4, PfATP4, mediate resistance to both aminopyrazole and spiroindolone antimalarials. ACS Chem. Biol. 10, 413–420 (2015).
Cowell, A. N. & Winzeler, E. A. Advances in omics-based methods to identify novel targets for malaria and other parasitic protozoan infections. Genome Med. 11, 63 (2019).
Kuhen, K. L. et al. KAF156 is an antimalarial clinical candidate with potential for use in prophylaxis, treatment, and prevention of disease transmission. Antimicrob. Agents Chemother. 58, 5060–5067 (2014).
Drewes, G. & Knapp, S. Chemoproteomics and chemical probes for target discovery. Trends Biotechnol. 36, 1275–1286 (2018).
Ong, S. E. et al. Identifying the proteins to which small-molecule probes and drugs bind in cells. Proc. Natl Acad. Sci. USA 106, 4617–4622 (2009).
Wang, J. et al. Haem-activated promiscuous targeting of artemisinin in I. Nat. Commun. 6, 10111 (2015).
Paquet, T. et al. Antimalarial efficacy of MMV390048, an inhibitor of Plasmodium phosphatidylinositol 4-kinase. Sci. Transl. Med. 9, eaad9735 (2017).
Pai, M. Y. et al. Drug affinity responsive target stability (DARTS) for small-molecule target identification. Methods Mol. Biol. 1263, 287–298 (2015).
Sun, W. et al. Chemical signatures and new drug targets for gametocytocidal drug development. Sci. Rep. 4, 3743 (2014).
Lomenick, B. et al. Target identification using drug affinity responsive target stability (DARTS). Proc. Natl Acad. Sci. USA 106, 21984–21989 (2009).
Siwo, G. H. et al. An integrative analysis of small molecule transcriptional responses in the human malaria parasite Plasmodium falciparum. BMC Genomics 16, 1030 (2015).
Famin, O. & Ginsburg, H. Differential effects of 4-aminoquinoline-containing antimalarial drugs on hemoglobin digestion in Plasmodium falciparum–infected erythrocytes. Biochem. Pharmacol. 63, 393–398 (2002).
Zarchin, S., Krugliak, M. & Ginsburg, H. Digestion of the host erythrocyte by malaria parasites is the primary target for quinoline-containing antimalarials. Biochem. Pharmacol. 35, 2435–2442 (1986).
Loria, P., Miller, S., Foley, M. & Tilley, L. Inhibition of the peroxidative degradation of haem as the basis of action of chloroquine and other quinoline antimalarials. Biochem. J. 339(Pt 2), 363–370 (1999).
Wilson, D. W., Langer, C., Goodman, C. D., McFadden, G. I. & Beeson, J. G. Defining the timing of action of antimalarial drugs against Plasmodium falciparum. Antimicrob. Agents Chemother. 57, 1455–1467 (2013).
Tilley, L., Straimer, J., Gnadig, N. F., Ralph, S. A. & Fidock, D. A. Artemisinin action and resistance in Plasmodium falciparum. Trends Parasitol. 32, 682–696 (2016).
Delves, M. J. et al. Routine in vitro culture of P. falciparum gametocytes to evaluate novel transmission-blocking interventions. Nat. Protoc. 11, 1668–1680 (2016).
Duffy, S., Loganathan, S., Holleran, J. P. & Avery, V. M. Large-scale production of Plasmodium falciparum gametocytes for malaria drug discovery. Nat. Protoc. 11, 976–992 (2016).
Mikolajczak, S. A. et al. Plasmodium vivax liver stage development and hypnozoite persistence in human liver-chimeric mice. Cell Host Microbe 17, 526–535 (2015).
Klonis, N. et al. Altered temporal response of malaria parasites determines differential sensitivity to artemisinin. Proc. Natl Acad. Sci. USA 110, 5157–5162 (2013).
Dogovski, C. et al. Targeting the cell stress response of Plasmodium falciparum to overcome artemisinin resistance. PLoS Biol. 13, e1002132 (2015).
Inyushin, M. et al. Superparamagnetic properties of hemozoin. Sci. Rep. 6, 26212 (2016).
Jackson, K. E. et al. Selective permeabilization of the host cell membrane of I-infected red blood cells with streptolysin O and equinatoxin II. Biochem. J. 403, 167–175 (2007).
Prive, G. G. Detergents for the stabilization and crystallization of membrane proteins. Methods 41, 388–397 (2007).
Alexandrov, A. I., Mileni, M., Chien, E. Y., Hanson, M. A. & Stevens, R. C. Microscale fluorescent thermal stability assay for membrane proteins. Structure 16, 351–359 (2008).
Guettou, F. et al. Selectivity mechanism of a bacterial homolog of the human drug-peptide transporters PepT1 and PepT2. Nat. Struct. Mol. Biol. 21, 728–731 (2014).
Kawatkar, A. et al. CETSA beyond soluble targets: a broad application to multipass transmembrane proteins. ACS Chem. Biol. 14, 1913-1920 (2019).
Djimde, A. et al. A molecular marker for chloroquine-resistant falciparum malaria. N. Engl. J. Med. 344, 257–263 (2001).
Price, R. N. et al. Mefloquine resistance in Plasmodium falciparum and increased pfmdr1 gene copy number. Lancet 364, 438–447 (2004).
Kone, A. et al. Quinine treatment selects the pfnhe-1 ms4760-1 polymorphism in Malian patients with Falciparum malaria. J. Infect. Dis. 207, 520–527 (2013).
Menard, D. et al. Global analysis of Plasmodium falciparum Na(+)/H(+) exchanger (pfnhe-1) allele polymorphism and its usefulness as a marker of in vitro resistance to quinine. Int. J. Parasitol. 3, 8–19 (2013).
Mok, S. et al. Structural polymorphism in the promoter of pfmrp2 confers Plasmodium falciparum tolerance to quinoline drugs. Mol. Microbiol. 91, 918–934 (2014).
Bellanca, S. et al. Multiple drugs compete for transport via the Plasmodium falciparum chloroquine resistance transporter at distinct but interdependent sites. J. Biol. Chem. 289, 36336–36351 (2014).
Sanchez, C. P. et al. Differences in trans-stimulated chloroquine efflux kinetics are linked to PfCRT in Plasmodium falciparum. Mol. Microbiol. 64, 407–420 (2007).
Sanchez, C. P., Stein, W. & Lanzer, M. Trans stimulation provides evidence for a drug efflux carrier as the mechanism of chloroquine resistance in Plasmodium falciparum. Biochemistry 42, 9383–9394 (2003).
Christophers, S. R. & Fulton, J. D. Experiments with isolated malaria parasites (Plasmodium knowlesi) free from red cells. Ann. Trop. Med. Parasitol. 33, 161–170 (1939).
Ribaut, C. et al. Concentration and purification by magnetic separation of the erythrocytic stages of all human Plasmodium species. Malar. J. 7, 45 (2008).
Cimmperman, P. et al. A quantitative model of thermal stabilization and destabilization of proteins by ligands. Biophys. J. 95, 3222–3231 (2008).
Rappsilber, J., Mann, M. & Ishihama, Y. Protocol for micro-purification, enrichment, pre-fractionation and storage of peptides for proteomics using StageTips. Nat. Protoc. 2, 1896–1906 (2007).
Zecha, J. et al. TMT labeling for the masses: a robust and cost-efficient, in-solution labeling approach. Mol. Cell. Proteomics 18, 1468-1478 (2019).
Childs, D. et al. TPP: Analyze Thermal Proteome Profiling (TPP) Experiments. R package version 3.14.0 http://bioconductor.org/packages/release/bioc/html/TPP.html (2019).
Childs, D. et al. Nonparametric analysis of thermal proteome profiles reveals novel drug-binding proteins. Mol. Cell. Proteomics 18, 2506–2515 (2019).
Borras, E. & Sabido, E. What is targeted proteomics? A concise revision of targeted acquisition and targeted data analysis in mass spectrometry. Proteomics 17, 1700180 (2017).
Pacold, M. E. et al. A PHGDH inhibitor reveals coordination of serine synthesis and one-carbon unit fate. Nat. Chem. Biol. 12, 452–458 (2016).
Dai, R., Wilson, D. J., Geders, T. W., Aldrich, C. C. & Finzel, B. C. Inhibition of Mycobacterium tuberculosis transaminase BioA by aryl hydrazines and hydrazides. Chembiochem. 15, 575–586 (2014).
Botelho, H. M., Koch, M., Fritz, G. & Gomes, C. M. Metal ions modulate the folding and stability of the tumor suppressor protein S100A2. The FEBS J. 276, 1776–1786 (2009).
Miettinen, T. P. et al. Thermal proteome profiling of breast cancer cells reveals proteasomal activation by CDK4/6 inhibitor palbociclib. EMBO J. 37, e98359 (2018).
Mateus, A. et al. Thermal proteome profiling in bacteria: probing protein state in vivo. Mol. Syst. Biol. 14, e8242 (2018).
Acknowledgements
This work was supported by NMRC MS-CETSA platform grant MOH/IAFCAT2/004/2015 to Z.B., P.N. and R.M.S.; Singapore Ministry of Education Tier 2 grant MOE2015-T2-2-108 to Z.B.; a Young Investigator Grant (YIG2015 A-STAR) to R.M.S.; an NTU Presidential Postdoctoral Fellowship Grant (NTU/PPF/2019) to J.M.D.; a startup grant from NTU to P.N.; and grants from the Swedish Research Council and the Knut och Alice Wallenberg Foundation to P.N.
Author information
Authors and Affiliations
Contributions
Z.B. and P.N. conceived and developed the idea for this article. J.M.D., G.W. and L.D. wrote the manuscript and performed the data analysis. L.D. developed the mineCETSA package. J.M.D., G.W., K.D.G. and H.Y. carried out experimental work for the experiments presented. J.M.D., G.W., L.D., K.D.G., H.Y., Y.T.L., L.C., L.C.W., B.P., R.M.S. and N.P. contributed to the development of the experimental protocol in this article. R.M.S. set up the mass spectrometry workflow. All authors provided feedback and changes to the manuscript. J.M.D., G.W. and Z.B., brought together the text and finalized the manuscript.
Corresponding authors
Ethics declarations
Competing interests
P.N. is the cofounder and a member of the board of directors of Pelago Bioscience AB and an inventor on a patent series originating from PTC/GB2012/050853, held by Pelago Bioscience AB, which covers MS-CETSA.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
Key reference using this protocol
Dziekan et al. Sci. Transl. Med. 11, eaau3174 (2019): https://doi.org/10.1126/scitranslmed.aau3174
Integrated supplementary information
Supplementary Figure 1 Sensitivity, specificity and false-discovery analysis of hit-calling metric used in ‘mineCETSA’ package.
(a) Pseudo-ROC analysis for a published data set of ATP melt curve MS-CETSA (or TPP) experiment. The dataset was downloaded from Childs et al.105 where the list (558 proteins) of expected ATP-binding proteins was annotated based on Gene Ontology Consortium annotations via the Bioconductor annotation packages org.Hs.eg.db (version 3.4.0) and GO.db (version 3.4.0). The hit calling based on EDscore in mineCETSA package is presented in a pseudo-ROC curve, where the expected ATP-binding proteins according to GO annotation was used as proxy true positives. The result is also compared to the ΔTm based hit calling method22. It should be noted that although the overall AUC is higher in ΔTm approach compared to EDscore approach, when the false positive rate is controlled (say <10%), EDscore approach performs better. (b) False discovery curve analysis of the ATP dataset as (a), where the protein hits were ranked on x-axis according to hit calling measures (EDscore or ΔTm), and the y-axis counts the number of false positives among the top N hits, for varying values of N. The asterisks indicate a threshold of 0.01 of the Benjamini-Hochberg adjusted p-values from the EDscore approach or the ΔTm approach (for each of the two replicates). The EDscore preforms much better than ΔTm, is probably because the formula of EDscore takes into consideration the extent of apparent shift, as well as the reproducibility of replicated measurements. (c) Similar to (a), the pseudo-ROC comparative analysis was done on a published MS-CETSA (or TPP) data set of the ATP-competitive pan-kinase inhibitor staurosporine, where 187 proteins were annotated as target proteins, also retrieved from Childs et al.105. (d) Similar to (b), the false discovery curve analysis of the staurosporine data set. In this case, according to the overall curve shape, the EDscore approach seems only slightly better than the ΔTm approach, but does much better in FDR control. (e) The pseudo-ROC analysis for the NADPH ITDR-CETSA experiment38,39, where two biological replicates were acquired and analyzed separately. The expected list of human NADP-binding protein was retrieved from the protein database UniProtKB based on the annotation in “Nucleotide binding” column, where 108 out of 20431 proteins were annotated NADP-binding proteins. (f) Scatterplot of the protein thermal shifts in NADPH ITDR-CETSA experiment as (e). The NADPH-responsive proteins were annotated with the known associated cofactors or substrates in different colors as shown. Most of the NADPH-responsive proteins that are consistently identified from two biological replicates are the known NAD(P)H-binding proteins. Of note, the two effected phosphotyrosine phosphatases, PTPN1 and PTPN11, are likely due to the generation of superoxide at high NADPH concentrations. Panel (f) is adapted from Dai et al.39.
Supplementary Figure 2 General overview of proteome coverage in different ITDR sample preparation types.
(a) Number of P. falciparum and non-hemoglobin H. sapiens proteins detected (PSM>3) across lysate (green), intact-cell (purple) and hemodepleted (‘Hb-‘) intact-cell (blue) ITDR 37 °C samples. Average values derived from 3 biological replicates are indicated on the graph with error bars representing Standard Deviation (SD). (b) Global hemoglobin content of Intact-cell ITDR 37 °C samples before and after the hemodepletion step, demonstrating successful removal of >90% of hemoglobin from the sample. Values indicated above each plot are an average of 8 biological replicates and error bars represent SD. Hemoglobin concentration was measured with Human Hb ELISA kit (Abcam, cat.no. ab 157707). (c) Peptide spectra match (PSM) counts for P. falciparum and non-hemoglobin H. sapiens proteins with PSM>3 detected in MS/MS analysis of three different sample preparation types: lysate (green), intact-cell (purple) and hemodepleted (‘Hb-‘) intact-cell (blue) ITDR 37 °C samples. Values are based on 3 biological replicates show significant increase in PSM in hemodepleted intact-cell samples. Error bars represent SD and p-values indicated on the plot were obtained from unpaired t-test. (d) Bland-Altman plot of PSM per protein difference in Hb- and non-depleted intact-cell sample preparation, demonstrating that hemodepletion results in higher average signal intensity for Plasmodium proteins identified in MS analysis (observed as the change in PSM number per protein in hemodepleted samples, relative to non-depleted samples). Plotted values are derived from overlapping proteins found in at least 1 biological replicate from each sample preparation type and possess PSM>3. (e) Venn diagram representing the overlap in proteins with PSM>3 identified between different sample preparation types. Data is based on confident protein identification in at least one out of three biological replicates of each sample type, demonstrating superior proteome coverage attained in lysate experiments and no bias in proteome coverage between intact-cell sample preparation variants. Figure is drawn based on unpublished data (experiments carried out by J.M.D., G.W. and K.D.).
Supplementary Figure 3 The influence of hemodepletion on target identification in intact-cell ITDR CETSA with quinine.
(a-b) P. falciparum proteome analysis of Intact-cell ITDR experiments under 0–10 μM quinine treatment with thermal challenges at 51 °C (blue dots) or 57 °C (red triangles) without hemoglobin depletion step (a) or with its inclusion (b). All proteins confidently identified in each condition and the non-denaturing control (n) are plotted on the graph as a function ΔAUC (relative shift in protein abundance under drug treatment in heat-challenged sample normalized against the non-denaturing 37 °C control, e.g., see panels C-F) and R squared value (signifying adherence of protein stabilization profile to the dose-response trend). Hit selection cut-offs of two and three times the MAD of ΔAUC in each dataset (i.e., MAD*2 and MAD*3) and R squared=0.8 are indicated on the graph. Significantly stabilized proteins, passing both hit selection cut-offs are located in the top right corner of the plot. (c) Protein stabilization curve of the top candidate target identified in panel A. (d-f) Protein stabilization curves of the top candidate targets identified in panel B. The extent of stabilization, depicted as the remaining soluble protein level after thermal challenge relative to no-drug control (y-axis) is plotted for replicate measurements along the drug concentration gradient (x-axis). The non-denaturing 37 °C control condition is plotted in black, whilst two denaturing conditions 51 °C and 57 °C are plotted in the shades of blue and red, respectively. Increased soluble protein abundance under drug exposure after heat challenge is suggestive of drug-induced protein stabilization. Panels B, D, E, F are based on unpublished data (experiments carried out by J.M.D., G.W. and K.D.) and panels A and C are adapted from Dziekan et al.21.
Supplementary information
Supplementary Information
Supplementary Figs. 1–3 and Supplementary Results and Discussion.
Supplementary Data 1
Plasmodium_DB_Human.fasta.
Supplementary Data 2
CESTA training datasets.
Rights and permissions
About this article
Cite this article
Dziekan, J.M., Wirjanata, G., Dai, L. et al. Cellular thermal shift assay for the identification of drug–target interactions in the Plasmodium falciparum proteome. Nat Protoc 15, 1881–1921 (2020). https://doi.org/10.1038/s41596-020-0310-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41596-020-0310-z
This article is cited by
-
Deep learning based CETSA feature prediction cross multiple cell lines with latent space representation
Scientific Reports (2024)
-
The toxic natural product tutin causes epileptic seizures in mice by activating calcineurin
Signal Transduction and Targeted Therapy (2023)
-
Antimalarial drug discovery: progress and approaches
Nature Reviews Drug Discovery (2023)
-
The novel CDK9 inhibitor, XPW1, alone and in combination with BRD4 inhibitor JQ1, for the treatment of clear cell renal cell carcinoma
British Journal of Cancer (2023)
-
Potent acyl-CoA synthetase 10 inhibitors kill Plasmodium falciparum by disrupting triglyceride formation
Nature Communications (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.