Abstract
Inhibitory extracellular matrices form around mature neurons as perineuronal nets containing chondroitin sulfate proteoglycans that limit axonal sprouting after CNS injury. The enzyme chondroitinase (Chase) degrades inhibitory chondroitin sulfate proteoglycans and improves axonal sprouting and functional recovery after spinal cord injury in rodents. We evaluated the effects of Chase in rhesus monkeys that had undergone C7 spinal cord hemisection. Four weeks after hemisection, we administered multiple intraparenchymal Chase injections below the lesion, targeting spinal cord circuits that control hand function. Hand function improved significantly in Chase-treated monkeys relative to vehicle-injected controls. Moreover, Chase significantly increased corticospinal axon growth and the number of synapses formed by corticospinal terminals in gray matter caudal to the lesion. No detrimental effects were detected. This approach appears to merit clinical translation in spinal cord injury.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
The custom-written ImageJ scripts are available from the corresponding author upon reasonable request.
References
Schwab, M. E. Nogo and axon regeneration. Curr. Opin. Neurobiol. 14, 118–124 (2004).
Fitch, M. T. & Silver, J. CNS injury, glial scars, and inflammation: inhibitory extracellular matrices and regeneration failure. Exp. Neurol. 209, 294–301 (2008).
Kwok, J. C. F., Afshari, F., García-Alías, G. & Fawcett, J. W. Proteoglycans in the central nervous system: plasticity, regeneration and their stimulation with chondroitinase ABC. Restor. Neurol. Neurosci. 26, 131–145 (2008).
Tran, A. P., Warren, P. M. & Silver, J. The biology of regeneration failure and success after spinal cord injury. Physiol. Rev. 98, 881–917 (2018).
Dou, C. L. & Levine, J. M. Inhibition of neurite growth by the NG2 chondroitin sulfate proteoglycan. J. Neurosci. 14, 7616–7628 (1994).
Levine, J. M. & Nishiyama, A. The NG2 chondroitin sulfate proteoglycan: a multifunctional proteoglycan associated with immature cells. Perspect. Dev. Neurobiol. 3, 245–259 (1996).
Jones, L. L., Yamaguchi, Y., Stallcup, W. B. & Tuszynski, M. H. NG2 Is a major chondroitin sulfate proteoglycan produced after spinal cord injury and is expressed by macrophages and oligodendrocyte progenitors. J. Neurosci. 22, 2792–2803 (2002).
Grimpe, B. & Silver, J. A novel DNA enzyme reduces glycosaminoglycan chains in the glial scar and allows microtransplanted dorsal root ganglia axons to regenerate beyond lesions in the spinal cord. J. Neurosci. 24, 1393–1397 (2004).
Wang, D. & Fawcett, J. The perineuronal net and the control of CNS plasticity. Cell Tissue Res. 349, 147–160 (2012).
Alilain, W. J., Horn, K. P., Hu, H., Dick, T. E. & Silver, J. Functional regeneration of respiratory pathways after spinal cord injury. Nature 475, 196–200 (2011).
Filous, A. R. et al. Entrapment via synaptic-like connections between NG2 proteoglycan+ cells and dystrophic axons in the lesion plays a role in regeneration failure after spinal cord injury. J. Neurosci. 34, 16369–16384 (2014).
Lang, B. T. et al. Modulation of the proteoglycan receptor PTPσ promotes recovery after spinal cord injury. Nature 518, 404–408 (2015).
Moon, L. D., Asher, R. A., Rhodes, K. E. & Fawcett, J. W. Regeneration of CNS axons back to their target following treatment of adult rat brain with chondroitinase ABC. Nat. Neurosci. 4, 465–466 (2001).
Bradbury, E. J. et al. Chondroitinase ABC promotes functional recovery after spinal cord injury. Nature 416, 636–640 (2002).
García-Alías, G., Barkhuysen, S., Buckle, M. & Fawcett, J. W. Chondroitinase ABC treatment opens a window of opportunity for task-specific rehabilitation. Nat. Neurosci. 12, 1145–1151 (2009).
Caggiano, A. O., Zimber, M. P., Ganguly, A., Blight, A. R. & Gruskin, E. A. Chondroitinase ABCI improves locomotion and bladder function following contusion injury of the rat spinal cord. J. Neurotrauma 22, 226–239 (2005).
Galtrey, C. M., Asher, R. A., Nothias, F. & Fawcett, J. W. Promoting plasticity in the spinal cord with chondroitinase improves functional recovery after peripheral nerve repair. Brain 130, 926–939 (2007).
Starkey, M. L., Bartus, K., Barritt, A. W. & Bradbury, E. J. Chondroitinase ABC promotes compensatory sprouting of the intact corticospinal tract and recovery of forelimb function following unilateral pyramidotomy in adult mice. Eur. J. Neurosci. 36, 3665–3678 (2012).
Houle, J. D. et al. Combining an autologous peripheral nervous system “bridge” and matrix modification by chondroitinase allows robust, functional regeneration beyond a hemisection lesion of the adult rat spinal cord. J. Neurosci. 26, 7405–7415 (2006).
James, N. D. et al. Chondroitinase gene therapy improves upper limb function following cervical contusion injury. Exp. Neurol. 271, 131–135 (2015).
Soleman, S., Yip, P. K., Duricki, D. A. & Moon, L. D. F. Delayed treatment with chondroitinase ABC promotes sensorimotor recovery and plasticity after stroke in aged rats. Brain 135, 1210–1223 (2012).
Hill, J. J., Jin, K., Mao, X. O., Xie, L. & Greenberg, D. A. Intracerebral chondroitinase ABC and heparan sulfate proteoglycan glypican improve outcome from chronic stroke in rats. Proc. Natl Acad. Sci. USA 109, 9155–9160 (2012).
Gherardini, L., Gennaro, M. & Pizzorusso, T. Perilesional treatment with chondroitinase ABC and motor training promote functional recovery after stroke in rats. Cereb. Cortex 25, 202–212 (2015).
Tester, N. J. & Howland, D. R. Chondroitinase ABC improves basic and skilled locomotion in spinal cord injured cats. Exp. Neurol. 209, 483–496 (2008).
Mondello, S. E., Jefferson, S. C., Tester, N. J. & Howland, D. R. Impact of treatment duration and lesion size on effectiveness of chondroitinase treatment post-SCI. Exp. Neurol. 267, 64–77 (2015).
Ginsberg, M. D. Neuroprotection for ischemic stroke: past, present and future. Neuropharmacology 55, 363–389 (2008).
Howells, D. W., Sena, E. S. & Macleod, M. R. Bringing rigour to translational medicine. Nat. Rev. Neurol. 10, 37–43 (2014).
Schumacher, M., Denier, C., Oudinet, J.-P., Adams, D. & Guennoun, R. Progesterone neuroprotection: the background of clinical trial failure. J. Steroid Biochem. Mol. Biol. 160, 53–66 (2016).
Tator, C. H. Review of treatment trials in human spinal cord injury: issues, difficulties, and recommendations. Neurosurgery 59, 957–982 (2006).
Rosenzweig, E. S. et al. Extensive spontaneous plasticity of corticospinal projections after primate spinal cord injury. Nat. Neurosci. 13, 1505–1510 (2010).
Lawrence, D. G. & Kuypers, H. G. The functional organization of the motor system in the monkey. I. The effects of bilateral pyramidal lesions. Brain 91, 1–14 (1968).
Hepp-Reymond, M. C., Trouche, E. & Wiesendanger, M. Effects of unilateral and bilateral pyramidotomy on a conditioned rapid precision grip in monkeys (Macaca fascicularis). Exp. Brain Res. 21, 519–527 (1974).
Bunge, R. P., Puckett, W. R., Becerra, J. L., Marcillo, A. & Quencer, R. M. Observations on the pathology of human spinal cord injury. A review and classification of 22 new cases with details from a case of chronic cord compression with extensive focal demyelination. Adv. Neurol. 59, 75–89 (1993).
Kakulas, B. A. A review of the neuropathology of human spinal cord injury with emphasis on special features. J. Spinal Cord Med. 22, 119–124 (1999).
Nout, Y. S. et al. Animal models of neurologic disorders: a nonhuman primate model of spinal cord injury. Neurotherapeutics 9, 380–392 (2012).
Weidner, N., Ner, A., Salimi, N. & Tuszynski, M. H. Spontaneous corticospinal axonal plasticity and functional recovery after adult central nervous system injury. Proc. Natl Acad. Sci. USA 98, 3513–3518 (2001).
Brus-Ramer, M., Carmel, J. B., Chakrabarty, S. & Martin, J. H. Electrical stimulation of spared corticospinal axons augments connections with ipsilateral spinal motor circuits after injury. J. Neurosci. 27, 13793–13801 (2007).
Ghosh, A. et al. Functional and anatomical reorganization of the sensory-motor cortex after incomplete spinal cord injury in adult rats. J. Neurosci. 29, 12210–12219 (2009).
Friedli, L. et al. Pronounced species divergence in corticospinal tract reorganization and functional recovery after lateralized spinal cord injury favors primates. Sci. Transl. Med. 7, 302ra134 (2015).
Liu, K. et al. PTEN deletion enhances the regenerative ability of adult corticospinal neurons. Nat. Neurosci. 13, 1075–1081 (2010).
Lee, J. K. et al. Assessing spinal axon regeneration and sprouting in Nogo-, MAG-, and OMgp-deficient mice. Neuron 66, 663–670 (2010).
Nout, Y. S. et al. Methods for functional assessment after C7 spinal cord hemisection in the rhesus monkey. Neurorehabil. Neural Repair 26, 556–569 (2012).
Shank, C. D., Walters, B. C. & Hadley, M. N. Management of acute traumatic spinal cord injuries. Handb. Clin. Neurol. 140, 275–298 (2017).
Salegio, E. A. et al. A unilateral cervical spinal cord contusion injury model in non-human primates (Macaca mulatta). J. Neurotrauma 33, 439–459 (2016).
Rosenzweig, E. S. et al. Extensive spinal decussation and bilateral termination of cervical corticospinal projections in rhesus monkeys. J. Comp. Neurol. 513, 151–163 (2009).
Leanza, G., Perez, S., Pellitteri, R., Russo, A. & Stanzani, S. Branching serotonergic and non-serotonergic projections from caudal brainstem to the medial preoptic area and the lumbar spinal cord, in the rat. Neurosci. Lett. 200, 5–8 (1995).
Haefeli, J. et al. A data-driven approach for evaluating multi-modal therapy in traumatic brain injury. Sci. Rep. 7, 42474 (2017).
International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for human use. ICH harmonised tripartite guideline. Statistical principles for clinical trials. International Conference on Harmonisation E9 Expert Working Group. Stat. Med. 18, 1905–1942 (1999).
Rasmussen, M. A., Colding‐Jørgensen, M., Hansen, L. T. & Bro, R. Multivariate evaluation of pharmacological responses in early clinical trials: a study of rIL-21 in the treatment of patients with metastatic melanoma. Br. J. Clin. Pharmacol. 69, 379–390 (2010).
Raghavan, N. et al. The ADAS-Cog revisited: novel composite scales based on ADAS-Cog to improve efficiency in MCI and early AD trials. Alzheimers Dement. 9, S21–S31 (2013).
García-Alías, G. et al. Therapeutic time window for the application of chondroitinase ABC after spinal cord injury. Exp. Neurol. 210, 331–338 (2008).
Lin, R., Kwok, J. C. F., Crespo, D. & Fawcett, J. W. Chondroitinase ABC has a long-lasting effect on chondroitin sulphate glycosaminoglycan content in the injured rat brain. J. Neurochem. 104, 400–408 (2008).
Hu, H. Z., Granger, N., Pai, S. B., Bellamkonda, R. V. & Jeffery, N. D. Therapeutic efficacy of microtube-embedded chondroitinase ABC in a canine clinical model of spinal cord injury. Brain 141, 1017–1027 (2018).
Iseda, T. et al. Single, high-dose intraspinal injection of chondroitinase reduces glycosaminoglycans in injured spinal cord and promotes corticospinal axonal regrowth after hemisection but not contusion. J. Neurotrauma 25, 334–349 (2008).
Jefferson, S. C., Tester, N. J. & Howland, D. R. Chondroitinase ABC promotes recovery of adaptive limb movements and enhances axonal growth caudal to a spinal hemisection. J. Neurosci. 31, 5710–5720 (2011).
Steinmetz, M. P. et al. Chronic enhancement of the intrinsic growth capacity of sensory neurons combined with the degradation of inhibitory proteoglycans allows functional regeneration of sensory axons through the dorsal root entry zone in the mammalian spinal cord. J. Neurosci. 25, 8066–8076 (2005).
Rosenzweig, E. S. et al. Restorative effects of human neural stem cell grafts on the primate spinal cord. Nat. Med. 24, 484–490 (2018).
Linting, M., Meulman, J. J., Groenen, P. J. F. & van der Koojj, A. J. Nonlinear principal components analysis: introduction and application. Psychol. Methods 12, 336–358 (2007).
Lever, J., Krzywinski, M. & Altman, N. Principal component analysis. Nat. Methods 14, 641–642 (2017).
Ferguson, A. R. et al. Derivation of Multivariate Syndromic Outcome Metrics for Consistent Testing across Multiple Models of Cervical Spinal Cord Injury in Rats. PLoS One 8, e59712 (2013).
Gifi, A. Nonlinear Multivariate Analysis. (Wiley, 1990).
Cnaan, A., Laird, N. M. & Slasor, P. Using the general linear mixed model to analyse unbalanced repeated measures and longitudinal data. Stat. Med. 16, 2349–2380 (1997).
Acknowledgements
This work was supported by the National Institutes of Health (NIH, grant no. NS042291 to M.H.T.) and Acorda Therapeutics. Core infrastructure support for the primate spinal cord research facility was provided by the Veterans Administration (Gordon Mansfield Spinal Cord Injury Collaborative Consortium grant nos. IP50RX001045 and RR&D B7332R to M.H.T. and grant no. RR&D 1I01RX002245 to A.R.F.). The California National Primate Research Center is funded by the NIH (grant no. NCRR P51 OD011107-56). Funding was also provided by the Craig H. Neilsen Foundation (M.H.T.), the Bernard and Anne Spitzer Charitable Trust (M.H.T.), the Dr. Miriam and Sheldon G. Adelson Medical Research Foundation (M.H.T.), the British Medical Research Council (J.W.F.) and the Christopher & Dana Reeve Foundation (J.W.F.).
Author information
Authors and Affiliations
Contributions
E.S.R., E.A.S., J.H.B., J.F.I., A.O.C., A.R.B., J.R.H., L.A.H., J.F.I., A.O.C., A.R.B., Y.S.N-L., A.R.F., M.S.B., J.C.B. and M.H.T. designed the experiments. E.S.R., E.A.S., R.M., S.H., R.P., C.L.C., J.F.I., A.O.C., A.R.B., Y.S.N.-L., J.C.B. and M.H.T. carried out the experiments. E.S.R., E.A.S., J.J.L., J.L.W., C.A.W., J.H.B., B.H., J.R.H., J.W.F., A.R.F., M.S.B., J.C.B. and M.H.T. analyzed the data. E.S.R. and M.H.T. wrote the manuscript. E.S.R., E.A.S., J.J.L., J.L.W., C.A.W., J.H.B., R.M., S.H., R.P., C.L.C., J.F.I., A.O.C., A.R.B., B.H., J.R.H., L.A.H., Y.S.N.-L., J.W.F., A.R.F., M.S.B., J.C.B. and M.H.T. edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
J.F.I., A.O.C. and A.R.B. are employees of Acorda Therapeutics; J.W.F. and M.H.T. were members of the Acorda scientific advisory board at the time that these studies were performed. All other authors declare no competing interests.
Additional information
Journal peer review information: Nature Neuroscience thanks J. Andrew Pruszynski, Jerry Silver, and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Fig. 1 Intrathecal Chase Infusions in the Pig Do Not Degrade Gray Matter Chondroitin Sulfate Proteoglycans.
(a) 2B6 labeling of digested stubs of chondroitin sulfate proteoglycans (CSPGs) in transverse spinal cord sections of the porcine spinal cord at C8. Following intrathecal Chase infusions, there is an approximate 1 mm rim of CSPG degradation in the peripheral white matter of Chase-treated subjects. (b) Saline-infused control. (c) Wisteria Floribunda Agglutinin (WFA) labeling of peri-neuronal net CSPGs in gray matter reveals intact peri-neuronal net CSPGs in all Chase-infused subjects, which appear identical to (d) saline-infused controls. Labeling experiments included 6 Chase-infused and 1 saline-infused animals. Scale bars: 500 μm.
Supplementary Fig. 2 Parenchymal Integrity at Chase Injection Sites – Nissl.
Intraparenchymal injections of Chase in the monkey spinal cord do not cause extensive damage or inflammation. Images of transverse sections very near injection sites at C8-T1. Left column of images is from a short-term Chase subject (2 wks post injection, 6 wks post SCI); middle column is from a saline-injected subject (4 mos post injection, 5 mos post SCI); right column is from a Chase-injected subject (4 mos post injection, 5 mos post SCI). (A) Labeling for Nissl substance reveals mild hypercellularity along the injection track (arrowheads) 2 weeks after Chase injection. (B-C) By 4 months after injections, there are no evident differences in Nissl stains comparing saline and Chase injection sites. (D-F) Higher magnifications of sections in A-C. (G-I) Further magnification of panels D-F. Labeling experiments included 2 short-term Chase subjects, 4 saline-injected subjects, and 6 Chase-injected subjects. Scale bars: A-C, 500 μm; D-F, 100 μm; G-I, 50 μm.
Supplementary Fig. 3 Parenchymal Integrity at Chase Injection Sites – CD8, GFAP, Motor Neurons.
Intraparenchymal injections of Chase in the monkey spinal cord do not cause extensive damage or inflammation. Images of transverse sections midway between injection sites at C8-T1. (A-C) CD8 labeling in gray matter reveals rare T-cells 2 weeks after Chase injection; these cells are not detected 4 months after injection. CD3 and CD45 labeling showed the same pattern (data not shown). (D-F) Labeling for GFAP (astrocytes) in gray matter shows no qualitative differences between short-term Chase, long-term saline, and long-term Chase. Immunolabeling experiments included 2 short-term Chase subjects, 4 saline-injected subjects, and 6 Chase-injected subjects. (G) Injections of either Chase or saline resulted in no loss of spinal motor neurons (MNs) on injected vs. uninjected sides of the spinal cord (expected proportion is 0.5). Moreover, there was no drop in MN numbers at the actual injection site, nor when comparing motor neuron numbers in Chase vs. control animals (Chase proportion: 0.53±0.04; Control proportion: 0.51±0.01; ANOVA: F(1, 0.00055) = 0.11, P=0.75). N=6 Chase and N=5 controls. Lines show group means, bars show SEM, data points are individual tissue sections, 5-6 total sections per subject (up to one section per x-axis position). Scale bars: 100 μm.
Supplementary Fig. 4 Temporary Microglial Activation at Chase Injection Sites.
Images of transverse sections immediately adjacent to injection sites (or similar regions in C8-T1 spinal cord for uninjected subjects), labeled for IBA1 (microglia) at the indicated time points. There are significant differences in density of IBA1 labeling across groups (Overall ANOVA: F(5, 197.30) = 4.43, P = 0.009). Analyses include sections from animals involved in a previous study (;30 N=3 Intact subjects, N=4 Lesion 2wk subjects, N=3 Lesion 5mo subjects). Main panels show example actual images used for quantification; insets are 3x zooms. Images shown are from subjects whose results were closest to their group’s mean value. Quantifications in panel G. (A) Intact subjects show the baseline level of microglial labeling. (B) Two weeks after lesion, a trend toward increased microglial labeling is observed compared to baseline (N=4 subjects, ANOVA: F(1, 144.57) = 2.79, P = 0.16, compared to N=3 Intact subjects). (C) Two weeks after Chase injections (six weeks after lesion), increased IBA1 labeling is evident immediately adjacent to the injection site (arrow) (N=2 subjects). (D-F) At longer time points after lesions, increased IBA1 labeling remains evident and statistically significant compared to intact baseline (Lesion 5mo, N=5 subjects, ANOVA: F(1, 435.10) = 6.74, P = 0.04; Saline 4mo, N=3 subjects, ANOVA: F(1, 277.44) = 10.34, P = 0.03; Chase 4mo, N=6 subjects, ANOVA: F(1, 479.47) = 35.19, P = 0.0006; all compared to N=3 Intact subjects). However, there are no significant differences among animals with lesions alone, Saline injections or Chase injections (Lesion 5mo vs. Saline 4mo, vs. Chase 4mo, ANOVA: F(2, 3.78) = 0.11, P=0.89). (G) Bar graphs show means, data points are individual subjects, error bars represent SEM, asterisks indicate statistical difference from intact baseline, statistical results described above. Scale bar: 200 μm.
Supplementary Fig. 5 Chase Injections Degrade Chondroitin Sulfate Proteoglycans up to the Caudal Lesion Border.
(a) 2 wk after Chase administration (1 mo after lesion), WFA labeling reveals that CSPGs are intact at the rostral end of the lesion site. (b) In contrast, CSPG degradation is evident up to the caudal lesion border. However, because no “bridge” was placed in the lesion site to allow the growth of axons through the lesion, this CSPG degradation likely had no impact on experimental outcomes. Approximate zone of peri-neuronal net CSPG degradation indicated by dashed lines. Labeling experiment included 6 control subjects, and 6 Chase-injected subjects. Scale bar: 1 mm.
Supplementary Fig. 6 Object Manipulation.
(a) Intact subject manipulating an apple bimanually. Note palmar contact of right hand (arrow) with object, digit extension and thumb apposition, all features of normal object manipulation. (b) Manipulation by a lesioned subject early after injury. Note the flexed digits of the impaired right hand (arrows). (c) Partial recovery of the impaired right hand during object manipulation. The hand is more normally positioned and less tightly flexed, but the dorsal aspect of the digits are still in contact with the fruit, and the thumb remains close to digit two (arrows). The score for object manipulations is based on these features in combination with evaluations of movement of the wrist and fingers during manipulation, and the presence of pincer grasp42,44.
Supplementary Fig. 7 Lesion Reconstructions.
Extent of lesion is shown in red shading. Control subject #7 was considered an ‘overlesion’ and was excluded from behavioral analyses (but not CST anatomical analysis, as the left dorsolateral tract, which carries nearly all of the spared CST axons, was unaffected by the overlesion). Control subject #3 did not receive cortical tracer due to weight loss, and was therefore excluded from CST density analyses.
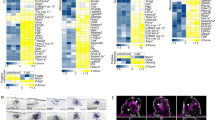
Supplementary Fig. 8 Behavioral Task Loadings on Principal Components Analysis.
Non-linear principal components analysis of all behavioral tasks (open-field tasks and Brinkman board) across all time points revealed strong loadings of all behavioral components on PC1, which accounted for 67.7% of the variance. For PC1, positive loadings (in red) indicate increased behavioral score, and negative loadings (in blue) are found on Brinkman board clearance time measurements (where lower values indicate improved performance). The loading pattern for PC1 indicates that this component broadly reflects improved behavioral performance. Two more principal components were extracted, with much lower percent variance accounted for (10.4% for PC2 and 5.1% for PC3). The loading patterns for these components did not indicate clearly definable eigenmodules, and scores on these components were therefore not tested. N = 11 subjects, with results confirmed through 1000 iterations of bootstrap subsampling at 60%.
Supplementary Fig. 9 Chase Also Increases Density of Axons Originating in Right Motor Cortex.
(a) A488-traced CST axons originating in the right motor cortex; 90% of these axons cross midline at the medullary pyramids and descend in the intact left hemicord, hence the greater density of descending axons compared to Fig 4. (b) Some of the axons cross midline near the central canal (CC) and (c) terminate primarily in the ventromedial gray matter. (d) Ventromedial gray matter from control subject. (e) Quantification shows that, just as with axons originating in the left motor cortex, Chase increases the density of these CST axons caudal to the spinal cord hemisection (total length in lesion-side GM per 40 μm section; P=0.001, linear mixed model). Immunolabeling and quantification included N=6 Chase and N=5 controls. Bars represent means, data points are individual subjects, error bars represent linear mixed model SEM. Scale bars: A,1 mm; B-D, 100 μm.
Supplementary Fig. 10 No Chase Effect on Raphespinal Density.
Serotonin labeling (5HT) in lesion-side gray matter in transverse sections at C8 in (A) control and (B) Chase-treated subjects. Higher magnification shown in insets. (C) Quantification reveals no differences between treated and control subjects in raphespinal density in motor neuron pools (P=0.924, generalized estimating equation). N=5 Chase and N=4 controls. Bars represent means, data points are individual subjects, error bars represent generalized estimating equation SEM. Scale bars: 200 μm.
Supplementary Fig. 11 Non-linear Principal Components Analysis Workflow.
Analysis was divided into two distinct stages. In Stage I, we compiled the full behavioral data outcome matrix (open-field measures and Brinkman board measures), and created a cross-correlation matrix of data from from all animals at each timepoint, regardless of condition. Non-linear principal component analysis then determined the extent to which each outcome measure correlated with the variance explained by the principal component (PC Loadings). The PC loadings were then examined and cross-validated to confirm the resulting PC scores serve as legitimate multidimensional outcome metrics. A PC score was then generated for each animal at each timepoint. In Stage II, we performed a directed, single hypothesis test (linear mixed model), unblinded to the effect of Chase on PC1 score.
Supplementary information
Supplementary Video 1
Forelimb function in open field—control subject. Subject 5 had the median object manipulation score in the control group. The video was taken 122 d after SCI. Object manipulation is scored during manipulation of the Kong toy filled with food objects (vegetable pieces, dried fruit, for example raisins, and nuts) and during retrieval of those pieces from the floor with the impaired hand, as well as during manipulation and eating of a large piece of fruit (for example, apple or orange). Hand use during other times contributed to scores for over-ground locomotion and climbing (but not to the object manipulation score), and also reflected recovery of hand use during spontaneous behavior. Highlights, focused on hand use: 0:08 Consistent weight-supported stepping on the two left limbs (un-affected side); the right limbs barely touch the perch surface. 00:14 As the animal sits, the right forelimb accepts some weight on the dorsal surface of the hand. 00:31 Initial contact of the right (impaired) forelimb with dorsal (non-volar) surface of impaired hand for support/stabilization of the Kong on-ground; this occurred for more than half the time the object was being manipulated on the ground. 00:37 The impaired hand was fully flexed with the wrist overextended. 1:07 Non-volar contact off-ground; this occurred for more than half the time. 1:27 Slight wrist movements during manipulation.
Supplementary Video 2
Forelimb function in open field—chase subject. Subject 6 had the median object manipulation score in the Chase group. The video was taken 121 d after SCI. Scoring as described in Supplementary Video 1. There is more and better use of the hand by this subject (Chase group) than the median control group subject (Supplementary Video 1). Highlights, focused on hand use: 00:08 Consistent weight-supported stepping on all four limbs. 00:15 Palmar placement of the impaired hand on the perch bar. 00:19 Non-volar contact with Kong on-ground; wrist extended, metacarpal-phalangeal (MCP) joint extended, proximal and distal inter-phalangeal joints (PIP and DIP) flexed. The distal aspect of the fingers are flexed and so their dorsal aspects (non-volar surfaces) are in contact with the Kong. 00:23 Wrist movements. 01:13 Volar contact with apple off-ground; some D1-2 (digit 1-2) space. 01:23 Volar contact off-ground; D2-5 movement. 01:47 Some D1-2 space. 02:05 Some D1-2 space. 02:34 Finger movements.
Rights and permissions
About this article
Cite this article
Rosenzweig, E.S., Salegio, E.A., Liang, J.J. et al. Chondroitinase improves anatomical and functional outcomes after primate spinal cord injury. Nat Neurosci 22, 1269–1275 (2019). https://doi.org/10.1038/s41593-019-0424-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41593-019-0424-1
This article is cited by
-
Opportunities and challenges in design and optimization of protein function
Nature Reviews Molecular Cell Biology (2024)
-
Regulation of axonal regeneration after mammalian spinal cord injury
Nature Reviews Molecular Cell Biology (2023)
-
Neurocognitive impact of Zika virus infection in adult rhesus macaques
Journal of Neuroinflammation (2022)
-
Natural and targeted circuit reorganization after spinal cord injury
Nature Neuroscience (2022)
-
Gene-Modified Stem Cells for Spinal Cord Injury: a Promising Better Alternative Therapy
Stem Cell Reviews and Reports (2022)