Abstract
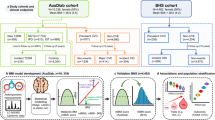
The state of intermediate hyperglycemia is indicative of elevated risk of developing type 2 diabetes1. However, the current definition of prediabetes neither reflects subphenotypes of pathophysiology of type 2 diabetes nor is predictive of future metabolic trajectories. We used partitioning on variables derived from oral glucose tolerance tests, MRI-measured body fat distribution, liver fat content and genetic risk in a cohort of extensively phenotyped individuals who are at increased risk for type 2 diabetes2,3 to identify six distinct clusters of subphenotypes. Three of the identified subphenotypes have increased glycemia (clusters 3, 5 and 6), but only individuals in clusters 5 and 3 have imminent diabetes risks. By contrast, those in cluster 6 have moderate risk of type 2 diabetes, but an increased risk of kidney disease and all-cause mortality. Findings were replicated in an independent cohort using simple anthropomorphic and glycemic constructs4. This proof-of-concept study demonstrates that pathophysiological heterogeneity exists before diagnosis of type 2 diabetes and highlights a group of individuals who have an increased risk of complications without rapid progression to overt type 2 diabetes.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
For TUEF/TULIP data, all requests for data and materials will be promptly reviewed by the Data Access Steering Committee of the Institute of Diabetes and Metabolic Research, Tübingen, to verify whether the request is subject to any intellectual property or confidentiality obligations. Individual-level data may be subject to confidentiality. Any data and materials that can be shared will be released via a Material Transfer Agreement. Access to individual-level data of the Whitehall II study is subject to a separate data-sharing agreement according to the data-sharing policy of Whitehall II. This policy conforms to the MRC Policy on Research Data Sharing. More details can be found on the Whitehall II webpage: https://www.ucl.ac.uk/epidemiology-health-care/research/epidemiology-and-public-health/research/whitehall-ii/data-sharing.
Code availability
The R code used to generate all results of this manuscript is available upon request. Requests will be reviewed by the Data Access Steering Committee of the Institute of Diabetes and Metabolic Research, Tübingen.
References
Tabák, A. G., Herder, C., Rathmann, W., Brunner, E. J. & Kivimäki, M. Prediabetes: a high-risk state for diabetes development. Lancet 379, 2279–2290 (2012).
Stumvoll, M. et al. Association of the T-G polymorphism in adiponectin (exon 2) with obesity and insulin sensitivity: interaction with family history of type 2 diabetes. Diabetes 51, 37–41 (2002).
Schmid, V. et al. Non-alcoholic fatty liver disease and impaired proinsulin conversion as newly identified predictors of the long-term non-response to a lifestyle intervention for diabetes prevention: results from the TULIP study. Diabetologia https://doi.org/10.1007/s00125-017-4407-z (2017).
Marmot, M. & Brunner, E. Cohort profile: the Whitehall II study. Int J. Epidemiol. 34, 251–256 (2005).
Davidson, M. B. Diagnosing diabetes with glucose criteria: worshipping a false god. Diabetes Care 34, 524–526 (2011).
Ahlqvist, E. et al. Novel subgroups of adult-onset diabetes and their association with outcomes: a data-driven cluster analysis of six variables. Lancet Diabetes. Endocrinol. 6, 361–369 (2018).
Stidsen, J. V. et al. Pathophysiology-based phenotyping in type 2 diabetes: a clinical classification tool. Diabetes Metab. Res. Rev. 0, e3005 (2018).
Unger, R. & Grundy, S. Hyperglycaemia as an inducer as well as a consequence of impaired islet cell function and insulin resistance: implications for the management of diabetes. Diabetologia 28, 119–121 (1985).
O’Connor, L. J. & Price, A. L. Distinguishing genetic correlation from causation across 52 diseases and complex traits. Nat. Genet. 50, 1728–1734 (2018).
Stefan, N., Schick, F. & Häring, H.-U. Causes, characteristics, and consequences of metabolically unhealthy normal weight in humans. Cell Metab. 26, 292–300 (2017).
Mahajan, A. et al. Refining the accuracy of validated target identification through coding variant fine-mapping in type 2 diabetes. Nat. Genet. 50, 559 (2018).
Udler, M. S. et al. Type 2 diabetes genetic loci informed by multi-trait associations point to disease mechanisms and subtypes: A soft clustering analysis. PLoS Med. 15, e1002654 (2018).
Hulman, A. et al. Pathophysiological characteristics underlying different glucose response curves: a latent class trajectory analysis from the prospective EGIR-RISC study. Diabetes Care https://doi.org/10.2337/dc18-0279 (2018).
Wagner, R. et al. Exercise-induced albuminuria is associated with perivascular renal sinus fat in individuals at increased risk of type 2 diabetes. Diabetologia 55, 2054–2058 (2012).
DeFronzo, R. A. & Ferrannini, E. Insulin resistance: a multifaceted syndrome responsible for NIDDM, obesity, hypertension, dyslipidemia, and atherosclerotic cardiovascular disease. Diabetes Care 14, 173–194 (1991).
Yip, J. et al. Insulin resistance in insulin-dependent diabetic patients with microalbuminuria. Lancet 342, 883–887 (1993).
Parvanova, A. I. et al. Insulin resistance and microalbuminuria: a cross-sectional, case-control study of 158 patients with type 2 diabetes and different degrees of urinary albumin excretion. Diabetes 55, 1456–1462 (2006).
Gerst, F. et al. Metabolic crosstalk between fatty pancreas and fatty liver: effects on local inflammation and insulin secretion. Diabetologia 60, 2240–2251 (2017).
El-Atat, F. A., Stas, S. N., McFarlane, S. I. & Sowers, J. R. The relationship between hyperinsulinemia, hypertension and progressive renal disease. J. Am. Soc. Nephrol. 15, 2816–2827 (2004).
Ausk, K. J., Boyko, E. J. & Ioannou, G. N. Insulin resistance predicts mortality in nondiabetic individuals in the U.S. Diabetes Care 33, 1179–1185 (2010).
Artunc, F. et al. The impact of insulin resistance on the kidney and vasculature. Nat. Rev. Nephrol. 12, 721–737 (2016).
Wannamethee, S. G., Shaper, A. G. & Perry, I. J., British Regional Heart Study. Smoking as a modifiable risk factor for type 2 diabetes in middle-aged men. Diabetes Care 24, 1590–1595 (2001).
Hogan, S. L. et al. Association of cigarette smoking with albuminuria in the United States: the third national health and nutrition examination survey. Ren. Fail. 29, 133–142 (2007).
Cirillo, M. et al. Microalbuminuria in nondiabetic adults: relation of blood pressure, body mass index, plasma cholesterol levels, and smoking: The Gubbio Population Study. Arch. Intern. Med. 158, 1933–1939 (1998).
Stefan, N. et al. Identification and characterization of metabolically benign obesity in humans. Arch. Intern. Med. 168, 1609–1616 (2008).
Stefan, N., Häring, H.-U. & Schulze, M. B. Metabolically healthy obesity: the low-hanging fruit in obesity treatment? Lancet Diabetes Endocrinol. 6, 249–258 (2018).
Heni, M. et al. Pancreatic fat is negatively associated with insulin secretion in individuals with impaired fasting glucose and/or impaired glucose tolerance: a nuclear magnetic resonance study. Diabetes Metab. Res. Rev. 26, 200–205 (2010).
Jaghutriz, B. A. et al. Metabolomic characteristics of fatty pancreas. Exp. Clin. Endocrinol. Diabetes https://doi.org/10.1055/a-0896-8671 (2019).
Dennis, J. M., Shields, B. M., Henley, W. E., Jones, A. G. & Hattersley, A. T. Disease progression and treatment response in data-driven subgroups of type 2 diabetes compared with models based on simple clinical features: an analysis using clinical trial data. Lancet Diabetes Endocrinol. 7, 442–451 (2019).
Zaharia, O. P. et al. Risk of diabetes-associated diseases in subgroups of patients with recent-onset diabetes: a 5-year follow-up study. Lancet Diabetes Endocrinol. 7, 684–694 (2019).
Weyer, C., Bogardus, C., Mott, D. M. & Pratley, R. E. The natural history of insulin secretory dysfunction and insulin resistance in the pathogenesis of type 2 diabetes mellitus. J. Clin. Invest. 104, 787–794 (1999).
Matsuda, M. & DeFronzo, R. A. Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes Care 22, 1462–1470 (1999).
Herzberg-Schäfer, S. et al. Evaluation of fasting state-/oral glucose tolerance test-derived measures of insulin release for the detection of genetically impaired β-cell function. PloS ONE 5, e14194 (2010).
Wagner, R. et al. A novel insulin sensitivity index particularly suitable to measure insulin sensitivity during gestation. Acta Diabetol. 53, 1037–1044 (2016).
Siegel-Axel, D. I. & Häring, H. U. Perivascular adipose tissue: an unique fat compartment relevant for the cardiometabolic syndrome. Rev. Endocr. Metab. Disord. 17, 51–60 (2016) .
Stefan, N., Kantartzis, K. & Häring, H.-U. Causes and metabolic consequences offatty liver. Endocr. Rev. 29, 939–960 (2008).
Eckel, R. H., Grundy, S. M. & Zimmet, P. Z. The metabolic syndrome. Lancet 365, 1415–1428 (2005).
Vilhjálmsson, B. J. et al. Modeling linkage disequilibrium increases accuracy of polygenic risk scores. Am. J. Hum. Genet. 97, 576–592 (2015).
Stumvoll, M., Van Haeften, T., Fritsche, A. & Gerich, J. Oral glucose tolerance test indexes for insulin sensitivity and secretion based on various availabilities of sampling times. Diabetes Care 24, 796–797 (2001).
Bouillon, K. et al. Decline in low-density lipoprotein cholesterol concentration: lipid-lowering drugs, diet, or physical activity? Evidence from the Whitehall II study. Heart 97, 923–930 (2011).
Machann, J. et al. Standardized assessment of whole body adipose tissue topography by MRI. J. Magn. Reson. Imaging 21, 455–462 (2005).
Stefan, N. et al. Inhibition of 11β-HSD1 with RO5093151 for non-alcoholic fatty liver disease: a multicentre, randomised, double-blind, placebo-controlled trial. Lancet Diabetes Endocrinol. 2, 406–416 (2014).
Bots Michiel, L., Hoes Arno, W., Koudstaal Peter, J., Albert, H. & Grobbee Diederick, E. Common carotid intima-media thickness and risk of stroke and myocardial infarction. Circulation 96, 1432–1437 (1997).
Touboul, P.-J. et al. Mannheim carotid intima-media thickness and plaque consensus (2004–2006–2011). Cerebrovasc. Dis. 34, 290–296 (2012).
Levey, A. S. et al. A new equation to estimate glomerular filtration rate. Ann. Intern Med 150, 604–612 (2009).
Levey, A. S. et al. Definition and classification of chronic kidney disease: a position statement from Kidney Disease: Improving Global Outcomes (KDIGO). Kidney Int. 67, 2089–2100 (2005).
Ferrie, J. E., Kivimäki, M., Shipley, M. J., Smith, G. D. & Virtanen, M. Job insecurity and incident coronary heart disease: the Whitehall II prospective cohort study. Atherosclerosis 227, 178–181 (2013).
R Core Team. R: A Language and Environment for Statistical Computing. (R Foundation for Statistical Computing, 2015).
Reynolds, A. P., Richards, G., de la Iglesia, B. & Rayward-Smith, V. J. Clustering rules: a comparison of partitioning and hierarchical clustering algorithms. J. Math. Model Algor. 5, 475–504 (2006).
Hennig, C. Cluster-wise assessment of cluster stability. Comput. Stat. Data Anal. 52, 258–271 (2007).
Acknowledgements
We thank all the research volunteers for their participation. We thank all participants in the Whitehall II Study, Whitehall II researchers and support staff who made the study possible. We gratefully acknowledge the excellent technical assistance of the Diabetes Research Unit Diabetes Research and Metabolic Diseases of the Helmholtz Center Munich at the University of Tübingen, Germany. We thank J. Kriebel and H. Grallert (Molecular Epidemiology, Helmholtz Center Munich) for generating the Global Screening Array data. This study was supported in part by a grant (01GI0925) from the Federal Ministry of Education and Research (BMBF) to the German Center for Diabetes Research (DZD e.V.) and from the state of Baden-Württemberg to R.W. and A.F. (32-5400/58/2, Forum Gesundheitsstandort Baden-Württemberg). The UK Medical Research Council (MR/K013351/1; G0902037), British Heart Foundation (RG/13/2/30098) and the US National Institutes of Health (R01HL36310, R01AG013196) have supported collection of data in the Whitehall II Study.
Author information
Authors and Affiliations
Contributions
R.W. analyzed the data and wrote the manuscript. M.H., A.G.T., J.M., F.S., E.R. and A.F. contributed to data acquisition and the interpretation of data, and edited the manuscript. M.H.d.A., A.P. A.L.B. and N.S. contributed to the interpretation of data and edited the manuscript. H.-U.H. and A.F. contributed to the concept of the work and edited the manuscript. All authors have reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Jennifer Sargent was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Assignment of proxy variables from the Whitehall II cohort to the original clustering variables.
Assignment of proxy variables from the Whitehall II cohort (variables that were both assessed in Whitehall-II and the original clustering cohort TUEF/TULIP) to the original clustering variables. Clusters were identified in Whitehall II using the Euclidean distances of the subjects computed from these variables to the cluster medians in TUEF/TULIP. The upper row shows the original clustering variables available in TUEF/TULIP, the lower row the variables in Whitehall-II. Arrows show the physiological connection between the variables.
Extended Data Fig. 2 Key features of the clusters.
NGT: normal glucose tolerance, IFG: impaired fasting glucose, IGT: impaired glucose tolerance, T2D: type 2 diabetes.
Extended Data Fig. 3 Transitions into Ahlqvist-diabetes-classes for subjects who were assigned to clusters in the Whitehall II study and developed diabetes during follow-up.
Transitions into Ahlqvist-diabetes-classes (right hand side) for subjects who were assigned to clusters in the Whitehall II study and developed diabetes during follow-up (left hand side, N = 201).
Extended Data Fig. 4 Kaplan-Meier curves to compare the risk discrimination between Hulman-classes and clusters.
Kaplan-Meier curves to compare the risk discrimination between Hulman-classes (A, n = 416 individuals with follow-up) and clusters (B, n = 421 individuals with follow-up) showing probabilities of remaining diabetes free in the TUEF/TULIP cohort. P-values indicate two-sided log-rank tests.
Extended Data Fig. 5 Kaplan-Meier curves to compare the risk discrimination between quintiles of baseline glucose AUC levels and clusters.
Kaplan-Meier curves to compare the risk discrimination between quintiles of baseline glucose AUC levels (A, n = 6643 individuals with follow-up) and clusters (B, n = 6643 individuals with follow-up) for diabetes development in the Whitehall II study. P-values indicate two-sided log-rank tests.
Extended Data Fig. 6 Cumulative incidence of chronic kidney disease stage 3 or worse.
Cumulative incidence of chronic kidney disease stage 3 or worse in the Whitehall-II study (N = 5182).
Extended Data Fig. 7 Cluster-stratified carotid intima media thickness.
Cluster-stratified carotid intima media thickness (IMT) in the subset with ultrasound measurements (N = 479) in the TUEF/TULIP study. IMT was measured in 60%, 37%, 46%, 72%, 45% and 55% of the participants of cluster 1 through 6, respectively. Boxes (hinges) denote the 25th and 75th percentiles with an additional horizontal line indicating the median. Whiskers show the highest and lowest data points excluding outliers (defined as at least 1.5×interquartile range below the lower or above the upper hinge).
Extended Data Fig. 8 Cluster stability plot.
Cluster stability plot showing all consecutive cluster transitions in the iterative re-clustering of repeated measurements in TUEF/TULIP (N = 429 individuals with repeated measurements).
Supplementary information
Supplementary Information
Supplementary Tables 1–15
Rights and permissions
About this article
Cite this article
Wagner, R., Heni, M., Tabák, A.G. et al. Pathophysiology-based subphenotyping of individuals at elevated risk for type 2 diabetes. Nat Med 27, 49–57 (2021). https://doi.org/10.1038/s41591-020-1116-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-020-1116-9
This article is cited by
-
The clinical relevance of a polygenic risk score for type 2 diabetes mellitus in the Korean population
Scientific Reports (2024)
-
Inter-organ crosstalk during development and progression of type 2 diabetes mellitus
Nature Reviews Endocrinology (2024)
-
Effectiveness of a cognitive behavioral therapy-integrated, hospital-based program for prediabetes: a matched cohort study
Scientific Reports (2024)
-
Definition, Klassifikation, Diagnostik und Differenzialdiagnostik des Diabetes mellitus: Update 2023
Die Diabetologie (2024)
-
The insulin resistant brain: impact on whole-body metabolism and body fat distribution
Diabetologia (2024)