Abstract
The carbohydrate–insulin model of obesity posits that high-carbohydrate diets lead to excess insulin secretion, thereby promoting fat accumulation and increasing energy intake. Thus, low-carbohydrate diets are predicted to reduce ad libitum energy intake as compared to low-fat, high-carbohydrate diets. To test this hypothesis, 20 adults aged 29.9 ± 1.4 (mean ± s.e.m.) years with body mass index of 27.8 ± 1.3 kg m−2 were admitted as inpatients to the National Institutes of Health Clinical Center and randomized to consume ad libitum either a minimally processed, plant-based, low-fat diet (10.3% fat, 75.2% carbohydrate) with high glycemic load (85 g 1,000 kcal−1) or a minimally processed, animal-based, ketogenic, low-carbohydrate diet (75.8% fat, 10.0% carbohydrate) with low glycemic load (6 g 1,000 kcal−1) for 2 weeks followed immediately by the alternate diet for 2 weeks. One participant withdrew due to hypoglycemia during the low-carbohydrate diet. The primary outcomes compared mean daily ad libitum energy intake between each 2-week diet period as well as between the final week of each diet. We found that the low-fat diet led to 689 ± 73 kcal d−1 less energy intake than the low-carbohydrate diet over 2 weeks (P < 0.0001) and 544 ± 68 kcal d−1 less over the final week (P < 0.0001). Therefore, the predictions of the carbohydrate–insulin model were inconsistent with our observations. This study was registered on ClinicalTrials.gov as NCT03878108.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The study protocol, de-identified individual data, and statistical analysis code for the results reported in this manuscript will be posted on the Open Science Framework website (https://osf.io/fjykq/) and is freely available without restrictions.
References
Hall, K. D. Did the food environment cause the obesity epidemic? Obesity 26, 11–13 (2018).
Ludwig, D. S. & Ebbeling, C. B. The carbohydrate-insulin model of obesity: beyond “calories in, calories out”. JAMA Intern. Med. 178, 1098–1103 (2018).
Ludwig, D. S. & Friedman, M. I. Increasing adiposity: consequence or cause of overeating? JAMA 311, 2167–2168 (2014).
Blundell, J. E. & MacDiarmid, J. I. Fat as a risk factor for overconsumption: satiation, satiety, and patterns of eating. J. Am. Diet. Assoc. 97, S63–S69 (1997).
Blundell, J. E. & Macdiarmid, J. I. Passive overconsumption. Fat intake and short-term energy balance. Ann. NY Acad. Sci. 827, 392–407 (1997).
Bray, G. A. & Popkin, B. M. Dietary fat intake does affect obesity! Am. J. Clin. Nutr. 68, 1157–1173 (1998).
Stubbs, R. J. Nutrition Society Medal Lecture. Appetite, feeding behaviour and energy balance in human subjects. Proc. Nutr. Soc. 57, 341–356 (1998).
Hopkins, M., Gibbons, C., Caudwell, P., Blundell, J. E. & Finlayson, G. Differing effects of high-fat or high-carbohydrate meals on food hedonics in overweight and obese individuals. Br. J. Nutr. 115, 1875–1884 (2016).
Freedhoff, Y. & Hall, K. D. Weight loss diet studies: we need help not hype. Lancet 388, 849–851 (2016).
Das, S. K. et al. Long-term effects of 2 energy-restricted diets differing in glycemic load on dietary adherence, body composition, and metabolism in CALERIE: a 1-y randomized controlled trial. Am. J. Clin. Nutr. 85, 1023–1030 (2007).
Hall, K. D., Guo, J. & Speakman, J. R. Do low-carbohydrate diets increase energy expenditure? Int. J. Obes. https://doi.org/10.1038/s41366-019-0456-3 (2019).
Stinson, E. J. et al. Is dietary nonadherence unique to obesity and weight loss? Results from a randomized clinical trial. Obesity 28, 2020–2027 (2020).
Boden, G., Sargrad, K., Homko, C., Mozzoli, M. & Stein, T. P. Effect of a low-carbohydrate diet on appetite, blood glucose levels, and insulin resistance in obese patients with type 2 diabetes. Ann. Intern. Med. 142, 403–411 (2005).
Lissner, L., Levitsky, D. A., Strupp, B. J., Kalkwarf, H. J. & Roe, D. A. Dietary fat and the regulation of energy intake in human subjects. Am. J. Clin. Nutr. 46, 886–892 (1987).
Stubbs, R. J., Harbron, C. G., Murgatroyd, P. R. & Prentice, A. M. Covert manipulation of dietary fat and energy density: effect on substrate flux and food intake in men eating ad libitum. Am. J. Clin. Nutr. 62, 316–329 (1995).
Gibson, A. A. et al. Do ketogenic diets really suppress appetite? A systematic review and meta-analysis. Obes. Rev. 16, 64–76 (2015).
Paoli, A., Bosco, G., Camporesi, E. M. & Mangar, D. Ketosis, ketogenic diet and food intake control: a complex relationship. Front. Psychol. 6, 27 (2015).
Stubbs, R. J., Ritz, P., Coward, W. A. & Prentice, A. M. Covert manipulation of the ratio of dietary fat to carbohydrate and energy density: effect on food intake and energy balance in free-living men eating ad libitum. Am. J. Clin. Nutr. 62, 330–337 (1995).
Hall, K. D. et al. Ultra-processed diets cause excess calorie intake and weight gain: an inpatient randomized controlled trial of ad libitum food intake. Cell Metab. 30, 67–77.e63 (2019).
Shintani, T. T., Hughes, C. K., Beckham, S. & O’Connor, H. K. Obesity and cardiovascular risk intervention through the ad libitum feeding of traditional Hawaiian diet. Am. J. Clin. Nutr. 53, 1647s–1651s (1991).
Johnstone, A. M., Horgan, G. W., Murison, S. D., Bremner, D. M. & Lobley, G. E. Effects of a high-protein ketogenic diet on hunger, appetite, and weight loss in obese men feeding ad libitum. Am. J. Clin. Nutr. 87, 44–55 (2008).
Shimy, K. J. et al. Effects of dietary carbohydrate content on circulating metabolic fuel availability in the postprandial state. J. Endocr. Soc. https://doi.org/10.1210/jendso/bvaa062 (2020).
Sherrier, M. & Li, H. The impact of keto-adaptation on exercise performance and the role of metabolic-regulating cytokines. Am. J. Clin. Nutr. 110, 562–573 (2019).
Hall, K. D. et al. Energy expenditure and body composition changes after an isocaloric ketogenic diet in overweight and obese men. Am. J. Clin. Nutr. 104, 324–333 (2016).
Mohorko, N. et al. Weight loss, improved physical performance, cognitive function, eating behavior, and metabolic profile in a 12-week ketogenic diet in obese adults. Nutr. Res. 62, 64–77 (2019).
Phinney, S. D., Bistrian, B. R., Evans, W. J., Gervino, E. & Blackburn, G. L. The human metabolic response to chronic ketosis without caloric restriction: preservation of submaximal exercise capability with reduced carbohydrate oxidation. Metabolism 32, 769–776 (1983).
Phinney, S. D. et al. Capacity for moderate exercise in obese subjects after adaptation to a hypocaloric, ketogenic diet. J. Clin. Invest. 66, 1152–1161 (1980).
Georgiou, E. et al. Body composition changes in chronic hemodialysis patients before and after hemodialysis as assessed by dual-energy X-ray absorptiometry. Metabolism 46, 1059–1062 (1997).
Going, S. B. et al. Detection of small changes in body composition by dual-energy X-ray absorptiometry. Am. J. Clin. Nutr. 57, 845–850 (1993).
Horber, F. F., Thomi, F., Casez, J. P., Fonteille, J. & Jaeger, P. Impact of hydration status on body composition as measured by dual energy X-ray absorptiometry in normal volunteers and patients on haemodialysis. Br. J. Radiol. 65, 895–900 (1992).
Toomey, C. M., McCormack, W. G. & Jakeman, P. The effect of hydration status on the measurement of lean tissue mass by dual-energy X-ray absorptiometry. Eur. J. Appl. Physiol. 117, 567–574 (2017).
Taylor, J. R. An Introduction to Error Analysis: the Study of Uncertainties in Physical Measurements. (University Science Books, 1982).
Hall, K. D. et al. Methodologic considerations for measuring energy expenditure differences between diets varying in carbohydrate using the doubly labeled water method. Am. J. Clin. Nutr. https://doi.org/10.1093/ajcn/nqy390 (2019).
Hall, K. D. et al. Calorie for calorie, dietary fat restriction results in more body fat loss than carbohydrate restriction in people with obesity. Cell Metab. 22, 427–436 (2015).
Leidy, H. J. et al. The role of protein in weight loss and maintenance. Am. J. Clin. Nutr. 101, 1320S–1329S (2015).
Sandesara, P. B., Virani, S. S., Fazio, S. & Shapiro, M. D. The forgotten lipids: triglycerides, remnant cholesterol, and atherosclerotic cardiovascular disease risk. Endocr. Rev. 40, 537–557 (2019).
Xia, J. & Yin, C. Glucose variability and coronary artery disease. Heart Lung Circ. 28, 553–559 (2019).
Sun, S., Li, H., Chen, J. & Qian, Q. Lactic acid: no longer an inert and end-product of glycolysis. Physiology 32, 453–463 (2017).
Raubenheimer, D. & Simpson, S. J. Protein leverage: theoretical foundations and ten points of clarification. Obesity 27, 1225–1238 (2019).
Clark, M. J. & Slavin, J. L. The effect of fiber on satiety and food intake: a systematic review. J. Am. Coll. Nutr. 32, 200–211 (2013).
Hervik, A. K. & Svihus, B. The role of fiber in energy balance. J. Nutr. Metab. 2019, 4983657 (2019).
Smethers, A. D. & Rolls, B. J. Dietary management of obesity: cornerstones of healthy eating patterns. Med. Clin. North Am. 102, 107–124 (2018).
Rolls, B. J. The relationship between dietary energy density and energy intake. Physiol. Behav. 97, 609–615 (2009).
Ledikwe, J. H. et al. Dietary energy density determined by eight calculation methods in a nationally representative United States population. J. Nutr. 135, 273–278 (2005).
Martinez Steele, E. et al. Ultra-processed foods and added sugars in the US diet: evidence from a nationally representative cross-sectional study. BMJ Open 6, e009892 (2016).
Rauber, F. et al. Ultra-processed food consumption and chronic non-communicable diseases-related dietary nutrient profile in the UK (2008–2014). Nutrients https://doi.org/10.3390/nu10050587 (2018).
de Graaf, C. & Kok, F. J. Slow food, fast food and the control of food intake. Nat. Rev. Endocrinol. 6, 290–293 (2010).
Forde, C. G., Mars, M. & de Graaf, K. Ultra-processing or oral processing? A role for energy density and eating rate in moderating energy intake from processed foods. Curr. Dev. Nutr. 4, nzaa019 (2020).
Monteiro, C. A. et al. Ultra-processed foods: what they are and how to identify them. Public Health Nutr. 22, 936–941 (2019).
Flood, A. et al. Methodology for adding glycemic load values to the National Cancer Institute diet history questionnaire database. J. Am. Diet. Assoc. 106, 393–402 (2006).
Harris, P. A. et al. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inform. 42, 377–381 (2009).
Ouwerkerk, R., Pettigrew, R. I. & Gharib, A. M. Liver metabolite concentrations measured with 1H MR spectroscopy. Radiology 265, 565–575 (2012).
Freedson, P. S., Melanson, E. & Sirard, J. Calibration of the Computer Science and Applications Inc. accelerometer. Med. Sci. Sports Exerc. 30, 777–781 (1998).
Schoffelen, P. F. & Westerterp, K. R. Intra-individual variability and adaptation of overnight- and sleeping metabolic rate. Physiol. Behav. 94, 158–163 (2008).
Tarasuk, V. & Beaton, G. H. Day-to-day variation in energy and nutrient intake: evidence of individuality in eating behaviour? Appetite 18, 43–54 (1992).
Bray, G. A., Flatt, J. P., Volaufova, J., Delany, J. P. & Champagne, C. M. Corrective responses in human food intake identified from an analysis of 7-d food-intake records. Am. J. Clin. Nutr. 88, 1504–1510 (2008).
Edholm, O. G. et al. Food intake and energy expenditure of army recruits. Br. J. Nutr. 24, 1091–1107 (1970).
Acknowledgements
This work was supported by the Intramural Research Program of the NIH, National Institute of Diabetes & Digestive & Kidney Diseases under award number 1ZIADK013037. P.V.J. is supported by the National Institute of Nursing Research under award number 1ZIANR000035-01, The Office of Workforce Diversity and the Rockefeller University Heilbrunn Nurse Scholar Award. We thank the nursing and nutrition staff at the NIH Metabolic Clinical Research Unit for their invaluable assistance with this study. We thank K. Klatt, J. Speakman and E. Weiss for helpful comments. We thank the study participants who volunteered to participate in this demanding protocol.
Author information
Authors and Affiliations
Contributions
K.D.H. designed the study. K.D.H. and J.G. analyzed the data. A.C. and S.Y. designed the diets and measured food and beverage intake with the assistance of J.B. and S.T. R.B. and K.Y.C. performed the indirect calorimetry measurements. C.G.F. assisted with the appetitive and eating rate measurements and their interpretation. A.M.G. and R.O. performed the liver fat measurements. M.W. and P.W. analyzed the blood and urine samples. S.T.C., I.R. and M.S. were responsible for the clinical care of the research participants and supervised the day-to-day operation and coordination of the study by V.D., I.G., R.H., L.M., P.V.J., K.R. and A.S. K.D.H. wrote the manuscript and is the guarantor of this work and has full access to all data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors critically revised the draft and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
C.G. Forde has received reimbursement for speaking at conferences sponsored by companies selling nutritional products, serves on the scientific advisory council for Kerry Taste and Nutrition and is part of an academic consortium that has received research funding from Abbott Nutrition, Nestec and Danone. The other authors declare no competing interests.
Additional information
Peer review information Jennifer Sargent was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Oral glucose tolerance.
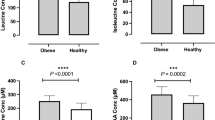
Mean blood concentrations in response to 75g oral glucose tolerance tests conducted at the end of the LC and LF diet periods (n=20) with respect to a) glucose, b) insulin, c) lactate, and d) free fatty acids. Data are presented as mean ± SEM.
Supplementary information
Supplementary Information
Descriptions and photographs of seven daily menus for LC and LF diets plus snacks.
Rights and permissions
About this article
Cite this article
Hall, K.D., Guo, J., Courville, A.B. et al. Effect of a plant-based, low-fat diet versus an animal-based, ketogenic diet on ad libitum energy intake. Nat Med 27, 344–353 (2021). https://doi.org/10.1038/s41591-020-01209-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-020-01209-1
This article is cited by
-
Changes in the chronic and postprandial blood lipid profiles of trained competitive cyclists and triathletes following a ketogenic diet: a randomized crossover trial
BMC Sports Science, Medicine and Rehabilitation (2024)
-
Differential peripheral immune signatures elicited by vegan versus ketogenic diets in humans
Nature Medicine (2024)
-
Metabolic Messengers: ketone bodies
Nature Metabolism (2023)
-
Ad libitum meal energy intake is positively influenced by energy density, eating rate and hyper-palatable food across four dietary patterns
Nature Food (2023)
-
Determining the metabolic effects of dietary fat, sugars and fat-sugar interaction using nutritional geometry in a dietary challenge study with male mice
Nature Communications (2023)