Abstract
Autologous induced pluripotent stem cells (iPSCs) constitute an unlimited cell source for patient-specific cell-based organ repair strategies. However, their generation and subsequent differentiation into specific cells or tissues entail cell line-specific manufacturing challenges and form a lengthy process that precludes acute treatment modalities. These shortcomings could be overcome by using prefabricated allogeneic cell or tissue products, but the vigorous immune response against histo-incompatible cells has prevented the successful implementation of this approach. Here we show that both mouse and human iPSCs lose their immunogenicity when major histocompatibility complex (MHC) class I and II genes are inactivated and CD47 is over-expressed. These hypoimmunogenic iPSCs retain their pluripotent stem cell potential and differentiation capacity. Endothelial cells, smooth muscle cells, and cardiomyocytes derived from hypoimmunogenic mouse or human iPSCs reliably evade immune rejection in fully MHC-mismatched allogeneic recipients and survive long-term without the use of immunosuppression. These findings suggest that hypoimmunogenic cell grafts can be engineered for universal transplantation.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
All data supporting the findings of this study are available in the paper and its Supplementary Information files.
Change history
16 September 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41587-022-01426-8
References
Gyongyosi, M. et al. Meta-analysis of cell-based CaRdiac stUdiEs (ACCRUE) in patients with acute myocardial infarction based on individual patient data. Circ. Res. 116, 1346–1360 (2015).
Fisher, S. A., Doree, C., Mathur, A. & Martin-Rendon, E. Meta-analysis of cell therapy trials for patients with heart failure. Circ. Res. 116, 1361–1377 (2015).
Kandala, J. et al. Meta-analysis of stem cell therapy in chronic ischemic cardiomyopathy. Am. J. Cardiol. 112, 217–225 (2013).
Fernandez-Aviles, F. et al. Global position paper on cardiovascular regenerative medicine. Eur. Heart J. 38, 2532–2546 (2017).
Lipsitz, Y. Y., Timmins, N. E. & Zandstra, P. W. Quality cell therapy manufacturing by design. Nat. Biotechnol. 34, 393–400 (2016).
Blair, N. F. & Barker, R. A. Making it personal: the prospects for autologous pluripotent stem cell-derived therapies. Regen. Med. 11, 423–425 (2016).
Chakradhar, S. An eye to the future: researchers debate best path for stem cell-derived therapies. Nat. Med. 22, 116–119 (2016).
Smith, D. M. Assessing commercial opportunities for autologous and allogeneic cell-based products. Regen. Med. 7, 721–732 (2012).
Lipsitz, Y. Y., Bedford, P., Davies, A. H., Timmins, N. E. & Zandstra, P. W. Achieving efficient manufacturing and quality assurance through synthetic cell therapy design. Cell. Stem. Cell. 20, 13–17 (2017).
van Berlo, J. H. & Molkentin, J. D. An emerging consensus on cardiac regeneration. Nat. Med. 20, 1386–1393 (2014).
Arck, P. C. & Hecher, K. Fetomaternal immune cross-talk and its consequences for maternal and offspring’s health. Nat. Med. 19, 548–556 (2013).
Jaiswal, S. et al. CD47 is upregulated on circulating hematopoietic stem cells and leukemia cells to avoid phagocytosis. Cell 138, 271–285 (2009).
Diecke, S. et al. Novel codon-optimized mini-intronic plasmid for efficient, inexpensive, and xeno-free induction of pluripotency. Sci. Rep. 5, 8081 (2015).
Chang, C. H., Fontes, J. D., Peterlin, M. & Flavell, R. A. Class II transactivator (CIITA) is sufficient for the inducible expression of major histocompatibility complex class II genes. J. Exp. Med. 180, 1367–1374 (1994).
Elsner, L. et al. The heat shock protein HSP70 promotes mouse NK cell activity against tumors that express inducible NKG2D ligands. J. Immunol. 179, 5523–5533 (2007).
Maddaluno, M. et al. Murine aortic smooth muscle cells acquire, though fail to present exogenous protein antigens on major histocompatibility complex class II molecules. Biomed. Res. Int. 2014, 949845 (2014).
Didie, M., Galla, S., Muppala, V., Dressel, R. & Zimmermann, W. H. Immunological properties of murine parthenogenetic stem cell-derived cardiomyocytes and engineered heart muscle. Front. Immunol. 8, 955 (2017).
Wunderlich, M. et al. AML xenograft efficiency is significantly improved in NOD/SCID-IL2RG mice constitutively expressing human SCF, GM-CSF and IL-3. Leukemia 24, 1785–1788 (2010).
Shultz, L. D., Ishikawa, F. & Greiner, D. L. Humanized mice in translational biomedical research. Nat. Rev. Immunol. 7, 118–130 (2007).
Billerbeck, E. et al. Development of human CD4+ FoxP3+ regulatory T cells in human stem cell factor-, granulocyte-macrophage colony-stimulating factor-, and interleukin-3-expressing NOD-SCID IL2Rgamma(null) humanized mice. Blood 117, 3076–3086 (2011).
Melkus, M. W. et al. Humanized mice mount specific adaptive and innate immune responses to EBV and TSST-1. Nat. Med. 12, 1316–1322 (2006).
Deuse, T. et al. Human leukocyte antigen I knockdown human embryonic stem cells induce host ignorance and achieve prolonged xenogeneic survival. Circulation 124, S3–S9 (2011).
Wang, D., Quan, Y., Yan, Q., Morales, J. E. & Wetsel, R. A. Targeted disruption of the beta2-microglobulin gene minimizes the immunogenicity of human embryonic stem cells. Stem Cells Transl. Med. 4, 1234–1245 (2015).
Dressel, R. et al. Pluripotent stem cells are highly susceptible targets for syngeneic, allogeneic, and xenogeneic natural killer cells. FASEB J. 24, 2164–2177 (2010).
Kruse, V. et al. Human induced pluripotent stem cells are targets for allogeneic and autologous natural killer (NK) cells and killing is partly mediated by the activating NK Receptor DNAM-1. PLoS ONE 10, e0125544 (2015).
Gornalusse, G. G. et al. HLA-E-expressing pluripotent stem cells escape allogeneic responses and lysis by NK cells. Nat. Biotechnol. 35, 765–772 (2017).
Zhao, L., Teklemariam, T. & Hantash, B. M. Heterelogous expression of mutated HLA-G decreases immunogenicity of human embryonic stem cells and their epidermal derivatives. Stem Cell Res. 13, 342–354 (2014).
Hou, S., Doherty, P. C., Zijlstra, M., Jaenisch, R. & Katz, J. M. Delayed clearance of Sendai virus in mice lacking class I MHC-restricted CD8+ T cells. J. Immunol. 149, 1319–1325 (1992).
Shiba, Y. et al. Allogeneic transplantation of iPS cell-derived cardiomyocytes regenerates primate hearts. Nature 538, 388–391 (2016).
Kawamura, T. et al. Cardiomyocytes derived from MHC-homozygous induced pluripotent stem cells exhibit reduced allogeneic immunogenicity in MHC-matched non-human primates. Stem Cell Rep. 6, 312–320 (2016).
Acknowledgements
We thank C. Pahrmann for cell culture work, imaging experiments and overall assistance and L. Li for his assistance. The in vivo BLI experiments were performed at the UCSF Pre-clinical Therapeutics Core (A. Fries; with special thanks to B.C. Hann). Special thanks go to J. Wu (Stanford Cardiovascular Institute, Stanford University School of Medicine) for providing the miPSCs and the help of his laboratory with developing the protocol for hiPSC differentiation into cardiomyocytes. We thank J.-F. Garcia-Gomez (City of Hope, Duarte) for the HLA typing of humanized BLT mice. We also thank E. Maltepe and H. Pektas for providing the syncytiotrophoblast cells. D.W. was supported by the Max Kade Foundation. A.W. received funding from the National Institutes of Health (grant AI123010). J.V.G. received funding from the National Institutes of Health (AI111899 and MH108179). The cardiomyocyte research was partly made possible by a grant from the California Institute for Regenerative Medicine (Grant Number DISC1-09984). Research related to cardiomyocyte immunobiology reported in this publication was supported by National Heart, Lung, and Blood Institute of the National Institutes of Health under award number R01HL140236. L.L.L. is an American Cancer Society Professor funded by NIH AI068129 and in part by the Parker Institute for Cancer Immunotherapy. S.S. and T.D. received funding for the cardiomyocyte research from the California Institute for Regenerative Medicine (Grant Number DISC1-09984) and for the immunobiology work from the National Heart, Lung, and Blood Institute of the National Institutes of Health under award number R01HL140236. The contents of this publication are solely the responsibility of the authors and do not necessarily represent the official views of the NIH, CIRM and other agencies of the State of California.
Author information
Authors and Affiliations
Contributions
T.D. and S.S. designed the experiments, supervised the project, and wrote the manuscript. X.H. performed the adaptive and innate immunobiology experiments, molecular biology and imaging studies and cell culture work and analyzed the data. A.G. performed imaging studies and analyzed the data. D.W. performed the in vivo and immunofluorescence imaging studies (confocal microscopy) and histopathology. G.T. performed imaging studies and cell injections. C.D. and W.O.T. generated BLT mice and performed the BLT imaging experiments. A.W. and J.V.G. designed and supervised the experiments using BLT mice. W.O.T. and C.D. performed the experiments using BLT mice. H.R., M.M.D. and L.L.L. gave technical support and conceptual advice. All authors contributed to editing the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 The immune phenotype of syncytiotrophoblast cells.
a, The syncytiotrophoblast is the immediate interface between maternal blood and the fetal side of the placenta. b, Mouse syncytiotrophoblast cells were isolated and cultured (representative picture of two independent experiments). c, RT-PCR showed depleted MHC class I and II expression, but positive Cd47 expression (representative gel of three independent experiments). d-f, The surface expression of MHC class I (d), MHC class II (e), and Cd47 (f) was assessed by flow cytometry (mean ±s.d., 4 independent experiments per group). Representative histograms are shown.
Supplementary Figure 2 The generation of miPSCs.
a, Mouse tail tip fibroblasts were re-programmed using a plasmid expressing the four reprogramming factors Oct4, KLF4, Sox2, and c-Myc. b, The miPSCs showed a normal 40, XX mouse karyotype in one analysis. c, miPSCs showed the typical gene expression profile of pluripotent stem cells (representative gel of two independent experiments). d, In immunofluorescence, miPSC cultures were positive for Sox2, Oct4, SSEA-1, and alkaline phosphatase (representative pictures of three independent experiments). e, When transplanted into immunodeficient SCID-beige mice, they formed teratomas containing (neuro-) ectoderm, mesoderm, and endoderm (representative pictures of three independent experiments). f, Endodermal (cytokeratin 8), mesodermal (brachyury), and ectodermal (GFAP) lineages were demonstrated by confocal immunofluorescence microscopy (representative pictures of three independent experiments).
Supplementary Figure 3 Immune phenotype and pluripotency of engineered miPSCs.
a, Mouse iPSCs underwent three editing steps to disrupt B2m, Ciita, and over-express Cd47 to achieve a hypoimmunogenic phenotype. Every step included rigorous testing for quality control. b-d, MHC class I (b), MHC class II (c), and Cd47 expression (d) by flow cytometry is shown for each engineering step, confirming successful gene editing (box 25th to 75th percentile with median, whiskers min-max, 4 independent experiments per graph, ANOVA with Bonferroni’s post-hoc test). e-g, During the engineering process, all edited miPSCs maintained expression of the pluripotent gene expression signature (representative gel of two independent PCR experiments). h, B2m−/−Ciita−/− Cd47 tg miPSCs exhibited Sox2, Oct4, and SSEA-1 expression in confocal immunofluorescence stainings, as well as alkaline phosphatase in immunohistochemistry (representative pictures of three independent experiments).
Supplementary Figure 4 Survival of gene-engineered miPSCs.
a, C57BL/6 B2m−/− miPSCs were transplanted into either syngeneic C57BL/6 (blue) mice or allogeneic (red) BALB/c mice. b, The thigh volume of all five C57BL/6 and ten BALB/c animals is shown over time. The overall percentage of cell grafts that survived and formed teratomas in BALB/c was 60%. c, IFN-γ Elispots and IL-4 Elispots are shown with splenocytes recovered 5 days after the transplantation and B2m−/− miPSCs stimulator cells (box 25th to 75th percentile with median, whiskers min-max, 8 animals per group, two-tailed Student’s t-test). d, Mean fluorescence (MFI) of IgM binding to B2m−/− miPSCs incubated with recipient serum after 5 days (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). e, C57BL/6 B2m−/−Ciita−/− miPSCs were transplanted into syngeneic C57BL/6 or allogeneic BALB/c mice. f, The thigh volume of all 5 C57BL/6 and 12 BALB/c animals is shown over time. The overall percentage of cell grafts that survived and formed teratomas in BALB/c was 91.7%. g, IFN-γ Elispots and IL-4 Elispots are shown with splenocytes recovered 5 days after the transplantation and B2m−/−Ciita−/− miPSCs stimulator cells (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). h, Mean fluorescence (MFI) of IgM binding to B2m−/−Ciita−/− miPSCs incubated with recipient serum after 5 days (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). i, The expression of stimulatory NKG2D ligands and NKp46 ligands on miPSC lines and YAC-1 was assessed using receptor Fc chimera proteins in flow cytometry (mean ± s.d., 3 independent experiments per group, ANOVA with Bonferroni’s post-hoc test). j, IFN-γ spot frequencies of miPSC lines and YAC-1 in Elispot assays with BALB/c NK cells (box 25th to 75th percentile with median, whiskers min-max, 6 independent experiments, ANOVA with Bonferroni’s post-hoc test).
Supplementary Figure 5 Interaction between CD47 and NK cells.
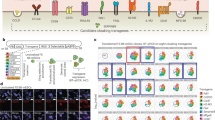
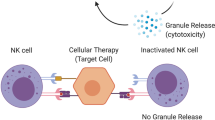
a, In vivo innate immune clearance was assessed by injecting a 1 : 1 mixture of CFSE-labeled wt miPSCs and either B2m−/−Ciita−/− or B2m−/−Ciita−/− Cd47 tg miPSCs into the peritoneum of syngeneic C57BL/6 mice. After 48 h, CSFE-labeled peritoneal miPSCs were recovered and the percentages of both fractions assessed by flow cytometry (mean ± s.d., 4 animals per group). While B2m−/−Ciita−/− miPSCs were rapidly cleared, B2m−/−Ciita−/− Cd47 tg miPSCs were spared. b, Mice were pretreated with clodronate to deplete macrophages, making this model more specific to NK cell killing and again only B2m−/−Ciita−/− Cd47 tg miPSCs were spared from NK cell killing (mean ± s.d., 4 animals per group). c, When a Cd47-blocking antibody was co-injected into the peritoneum, the protection was abolished and B2m−/−Ciita−/− Cd47 tg miPSCs were killed (mean ± s.d., 4 animals per group). d, In vitro real-time NK cell killing was assessed on confluent wt, B2m−/−Ciita−/−, and B2m−/−Ciita−/− Cd47 tg miECs in three different effector : target cell ratios. Using allogeneic BALB/c mouse NK (mNK) cells, B2m−/−Ciita−/− miECs were rapidly killed, and wt and B2m−/−Ciita−/− Cd47 tg miECs permanently survived (mean ± s.d., 3 independent experiments per group). e, Similarly, using syngeneic C57BL/6 mNK cells, B2m−/−Ciita−/− miECs were rapidly killed, and wt and B2m−/−Ciita−/− Cd47 tg miECs permanently survived (mean ± s.d., 3 independent experiments per group). f, When a Cd47-blocking antibody was added to syngeneic C57BL/6 mNK cells, B2m−/−Ciita−/− Cd47 tg miECs were swiftly killed (mean ± s.d., 3 independent experiments per group). g, When human NK (hNK) cells were used, both B2m−/−Ciita−/− and B2m−/−Ciita−/− Cd47 tg miECs were rapidly killed (mean ± s.d., 3 independent experiments per group). h, When hNK cells were used with human wt, B2M−/−CIITA−/−, and B2M−/−CIITA−/− CD47 tg hiECs, only B2M−/−CIITA−/− hiECs were rapidly killed and wt and B2M−/−CIITA−/− CD47 tg hiECs were spared (mean ± s.d., 3 independent experiments per group). i, With a CD47-blocking antibody, B2M−/−CIITA−/− CD47 tg hiECs were then swiftly killed (mean ± s.d., 3 independent experiments per group).
Supplementary Figure 6 Differentiation of miPSCs into miECs, miSMCs and miCMs.
a-b, B2m−/− Ciita−/− Cd47 tg miPSCs (a) and wt miPSCs (b) were successfully differentiated into corresponding miEC, miSMC, and miCM derivatives (representative pictures of three independent experiments). miECs were positive for Cd31 and VE-cadherin, miSMCs were positive for Sma and Sm22, miCMs were positive for Troponin I and Sarcomeric alpha-actinin by confocal immunofluorescence. All derivatives lost their expression of pluripotency genes (representative pictures of two independent PCR experiments).
Supplementary Figure 7 Immune phenotype of wt and engineered miPSC derivatives.
a, wt miECs showed high MHC class I and MHC class II expression, while B2m−/−Ciita−/− Cd47 tg miECs were MHC class I and MHC class II depleted and showed increased Cd47 expression (box 25th to 75th percentile with median, whiskers min-max, 4 independent experiments per graph, two-tailed Student’s t-test). b, wt miSMCs showed moderate MHC class I and MHC class II expression, while B2m−/−Ciita−/− Cd47 tg miSMCs were MHC class I and MHC class II depleted and showed increased Cd47 expression (box 25th to 75th percentile with median, whiskers min-max, 4 independent experiments per graph, two-tailed Student’s t-test). c, wt miCMs showed moderate MHC class I and low MHC class II expression; B2m−/−Ciita−/− Cd47 tg miCMs were MHC class I and MHC class II depleted and showed increased Cd47 expression (box 25th to 75th percentile with median, whiskers min-max, 4 independent experiments per graph, two-tailed Student’s t-test). d-e, The expression of stimulatory NKG2D ligands (d) and NKp46 ligands (e) on wt and B2m−/−Ciita−/− λCd47 tg miECs, miSMCs, miCMs, and YAC-1 was assessed using receptor Fc chimera proteins in flow cytometry (mean ± s.d., 3 independent experiments per group, two-tailed Student’s t-test).
Supplementary Figure 8 Immune response against miPSC derivatives.
a-c, Five days after the injection of wt miPSC-derived miECs (a), miSMCs (b), or miCMs (c) into C57BL/6 or BALB/c recipients, splenocytes were recovered for IFN-γ Elispot assays (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). The IFN-γ response was vastly stronger in all allogeneic recipients. Mean fluorescence (MFI) of IgM binding to wt miPSC-derived miECs (a), miSMCs (b), and miCMs (c), incubated with recipient serum after 5 days (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). There was a markedly stronger IgM response in all allogeneic recipients. d-f, Similarly, B2m−/−Ciita−/− Cd47 tg miPSC-derived miECs (d), miSMCs (e), or miCMs (f) were injected into C57BL/6 or BALB/c recipients and IFN-γ Elispots were performed after 5 days (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). Mean fluorescence (MFI) of IgM binding to B2m−/− Ciita−/− Cd47 tg miPSC-derived miECs (d), miSMCs (e), and miCMs (f), incubated with recipient serum after 5 days (box 25th to 75th percentile with median, whiskers min-max, 6 animals per group, two-tailed Student’s t-test). There was no measurable IFN-γ response or IgM response in allogeneic recipients. g-i, To assess the inhibitory effect of Cd47 overexpression on NK cell killing, IFN-γ Elispots with NK cells were performed with miECs (g), miSMCs (h), or miCMs (i) derived from B2m−/−Ciita−/− miPSC or B2m−/−Ciita−/− Cd47 tg miPSC (box 25th to 75th percentile with median, whiskers min-max, 6 independent experiments, ANOVA with Bonferroni’s post-hoc test) Only derivatives from B2m−/−Ciita−/− miPSC were susceptible for NK cell killing. j-l, In vivo innate immune clearance was assessed by injecting a 1 : 1 mixture of wt derivative engineered derivative into the peritoneum of C57BL/6 mice. After 48 h, peritoneal miECs (j), miSMCs (k), and miCMs (l) were recovered and the percentage assessed by flow cytometry (mean ± s.d., 4 animals per group).
Supplementary Figure 9 Immune cell infiltration and cytokine expression in miEC grafts.
a, Matrigel plugs containing either wt miECs or B2m−/−Ciita−/− Cd47 tg miECs were implanted in allogeneic BALB/c recipients. Cell-free matrigel plugs served as controls. b, Immunofluorescence stainings detected immune cell infiltration in wt iEC-plaques containing CD3+ T lymphocytes, CD335+ NK cells, and sparse F4/80+ macrophages. Co-staining of CD3 and VE-cadherin confirmed CD3+ lymphocyte infiltration in EC grafts in the wt group. Practically no immune cells were found in plugs containing B2m−/−Ciita−/− Cd47 tg miECs (representative pictures of three independent experiments). c, The cytokine profile in wt miEC plugs was shifted towards a pro-inflammatory milieu. Multiple significantly upregulated cytokines were typical of activated cytotoxic CD8+ T cells, CD4+ T helper-1 cells, and CD4+ T helper-2 cells, as well as macrophages (mean ± s.d., 12 animals per group, two-tailed Student’s t-test; dashed red lines show levels of cell-free matrigel).
Supplementary Figure 10 Morphology of transplanted B2m–/–Ciita–/– Cd47 tg miPSC derivatives in allogeneic hosts.
a-c, B2m−/−Ciita−/− Cd47 tg miEC (a), miSMC (b), or miCM (c) grafts in matrigel were transplanted subcutaneously into allogeneic BALB/c mice to investigate whether these hypoimmunogenic derivatives further mature in vivo or change their morphology over time in allogeneic recipients. Matrigel plugs were recovered after different time points for hematoxylin and eosin and immunofluorescence stainings (representative pictures of two independent experiments). Transplanted miECs started to organize in circular structures around day 14 and formed primitive vessels that contained erythrocytes around day 35 (a). Transplanted miSMCs (b) maintained their typical spindle-shape appearance and loose arrangement, whereas miCMs retained their immature round progenitor morphology (c). Both latter cell types did not show a higher degree of three-dimensional organization, which may be attributed to the lack of mechanical stimulus necessary for maturation of any type of muscle cell.
Supplementary Figure 11 Pluripotency of wt and B2M–/–CIITA–/– CD47 tg hiPSCs.
a, wt hiPSCs showed a normal human 46, XX karyotype in one analysis. b, wt hiPSCs were positive for TRA-1-60, TRA-1-81, SOX 2, OCT4, and SSEA-4 in confocal immunofluorescence and positive for alkaline phosphatase in immunohistochemistry (representative pictures of three independent experiments). c, wt hiPSCs expressed typical pluripotency genes (representative gel of two independent PCR experiments). d, B2M−/−CIITA−/− CD47 tg hiPSCs maintained the normal human 46, XX karyotype in one analysis. e, B2M−/−CIITA−/− CD47 tg hiPSCs were also positive for TRA-1-60, TRA-1-81, SOX 2, OCT4, and SSEA-4 in confocal immunofluorescence and positive for alkaline phosphatase in immunohistochemistry (representative pictures of three independent experiments). f, B2M−/−CIITA−/− CD47 tg hiPSCs continued to express the typical pluripotency genes (representative gel of two independent PCR experiments). g-j, wt hiPSCs (g, h) and B2M−/− CIITA−/− CD47 tg hiPSCs (i, j) gave rise to cell types of all 3 germ layers after transplantation into SCID-beige mice. Endodermal (cytokeratin 8), mesodermal (brachyury), and ectodermal lineages (GFAP) were also demonstrated by confocal immunofluorescence microscopy (representative pictures of three independent experiments).
Supplementary Figure 12 Differentiation of hiPSCs into hiECs and hiCMs.
a-b, wt hiPSCs (a) and B2M−/−CIITA−/− CD47 tg hiPSCs (b) were successfully differentiated into corresponding miEC and miCM derivatives (representative pictures of three independent experiments). miECs were positive for CD31 and VE-cadherin and miCMs were positive for Troponin I and Sarcomeric alpha-actinin by confocal immunofluorescence. All derivatives lost their expression of pluripotency genes (representative pictures of two independent experiments). c-g, The expression of stimulatory NK cell ligands was assessed on hiPSCs and their derivatives using receptor Fc chimera proteins in flow cytometry (mean ± s.d., 3 independent experiments per group, ANOVA with Bonferroni’s post-hoc test (hiPSCs) or two-tailed Student’s t-test (hiECs and hiCMs)). Ligands for NKG2D (c), NKp30 (d), NKp44 (e), NKp46 (f), and NKp80 (g) were compared between wt and engineered hiPSCs, hiECs, hiCMs, and K562. h-i, The expression of specific human natural cytotoxicity receptor ligands was evaluated by flow cytometry (mean ± s.d., 3 independent experiments per group, ANOVA with Bonferroni’s post-hoc test (hiPSCs) or two-tailed Student’s t-test (hiECs and hiCMs)). Surface expression of B7-H6 (h), and AICL (i) was compared between wt and engineered hiPSCs and derivatives, and K562. j, The HLA-A mismatches in transplant experiments with wt and B2M−/−CIITA−/− CD47 tg hiPSCs, hiECs, and hiCMs in allogeneic humanized NSG-HGM3 recipients (mean ± s.d., 5 animals per group, two-tailed Student’s t-test).
Supplementary Figure 13 CD3 reconstitution and HLA matching in humanized mice.
a, Percentage of CD3+ cells among the reconstituted human CD45+ cell population in NSG-SGM3 mice receiving hiPSC grafts (n=7 per group), hiEC grafts (n=3 per group), or hiCM grafts (n=3 per group) in the Elispot groups or hiPSC grafts, hiEC grafts, or hiCM grafts (n=5 per group) in the BLI groups (mean ± s.d., two-tailed Student’s t-test). b, All NSG-SGM3 mice were typed for HLA-A and the number of HLA-A mismatches (MM) was calculated for every single animal used in this study. 2 MM are coded in red, 1 MM in orange, and zero MM in green. c, Percentage of CD3+ cells among the reconstituted human CD45+ cell population in BLT mice receiving iEC grafts in the Elispot groups (n=4 per group) or BLI groups (n=5) (mean ± s.d., two-tailed Student’s t-test).
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–13
Rights and permissions
About this article
Cite this article
Deuse, T., Hu, X., Gravina, A. et al. Hypoimmunogenic derivatives of induced pluripotent stem cells evade immune rejection in fully immunocompetent allogeneic recipients. Nat Biotechnol 37, 252–258 (2019). https://doi.org/10.1038/s41587-019-0016-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41587-019-0016-3
This article is cited by
-
Current status of stem cell therapy for type 1 diabetes: a critique and a prospective consideration
Stem Cell Research & Therapy (2024)
-
Generation and optimization of off-the-shelf immunotherapeutics targeting TCR-Vβ2+ T cell malignancy
Nature Communications (2024)
-
synNotch-programmed iPSC-derived NK cells usurp TIGIT and CD73 activities for glioblastoma therapy
Nature Communications (2024)
-
Hypoimmune cells resist rejection in monkeys
Nature Biotechnology (2024)
-
Stem Cell-Based Strategies: The Future Direction of Bioartificial Liver Development
Stem Cell Reviews and Reports (2024)