Abstract
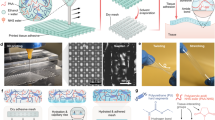
Two dry surfaces can instantly adhere upon contact with each other through intermolecular forces such as hydrogen bonds, electrostatic interactions and van der Waals interactions1,2. However, such instant adhesion is challenging when wet surfaces such as body tissues are involved, because water separates the molecules of the two surfaces, preventing interactions3,4. Although tissue adhesives have potential advantages over suturing or stapling5,6, existing liquid or hydrogel tissue adhesives suffer from several limitations: weak bonding, low biological compatibility, poor mechanical match with tissues, and slow adhesion formation5,6,7,8,9,10,11,12,13. Here we propose an alternative tissue adhesive in the form of a dry double-sided tape (DST) made from a combination of a biopolymer (gelatin or chitosan) and crosslinked poly(acrylic acid) grafted with N-hydrosuccinimide ester. The adhesion mechanism of this DST relies on the removal of interfacial water from the tissue surface, resulting in fast temporary crosslinking to the surface. Subsequent covalent crosslinking with amine groups on the tissue surface further improves the adhesion stability and strength of the DST. In vitro mouse, in vivo rat and ex vivo porcine models show that the DST can achieve strong adhesion between diverse wet dynamic tissues and engineering solids within five seconds. The DST may be useful as a tissue adhesive and sealant, and in adhering wearable and implantable devices to wet tissues.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All data are available in the main text or the Supplementary Information.
References
Creton, C. Pressure-sensitive adhesives: an introductory course. MRS Bull. 28, 434–439 (2003).
Chung, J. Y. & Chaudhury, M. K. Soft and hard adhesion. J. Adhes. 81, 1119–1145 (2005).
Peppas, N. A. & Buri, P. A. Surface, interfacial and molecular aspects of polymer bioadhesion on soft tissues. J. Control. Release 2, 257–275 (1985).
Lee, H., Lee, B. P. & Messersmith, P. B. A reversible wet/dry adhesive inspired by mussels and geckos. Nature 448, 338–341 (2007).
Reece, T. B., Maxey, T. S. & Kron, I. L. A prospectus on tissue adhesives. Am. J. Surg. 182, S40–S44 (2001).
Coulthard, P. et al. Tissue adhesives for closure of surgical incisions. Cochrane Database Syst. Rev. 11, CD004287 (2014).
Vakalopoulos, K. A. et al. Mechanical strength and rheological properties of tissue adhesives with regard to colorectal anastomosis: an ex vivo study. Ann. Surg. 261, 323–331 (2015).
Rose, S. et al. Nanoparticle solutions as adhesives for gels and biological tissues. Nature 505, 382–385 (2014).
Lee, B. P., Messersmith, P. B., Israelachvili, J. N. & Waite, J. H. Mussel-inspired adhesives and coatings. Annu. Rev. Mater. Res. 41, 99–132 (2011).
Annabi, N., Yue, K., Tamayol, A. & Khademhosseini, A. Elastic sealants for surgical applications. Eur. J. Pharm. Biopharm. 95, 27–39 (2015).
Karp, J. M. A slick and stretchable surgical adhesive. N. Engl. J. Med. 377, 2092–2094 (2017).
Li, J. et al. Tough adhesives for diverse wet surfaces. Science 357, 378–381 (2017).
LeMaire, S. A. et al. The threat of adhesive embolization: BioGlue leaks through needle holes in aortic tissue and prosthetic grafts. Ann. Thorac. Surg. 80, 106–111 (2005).
Maier, G. P., Rapp, M. V., Waite, J. H., Israelachvili, J. N. & Butler, A. Adaptive synergy between catechol and lysine promotes wet adhesion by surface salt displacement. Science 349, 628–632 (2015).
Zhao, Q. et al. Underwater contact adhesion and microarchitecture in polyelectrolyte complexes actuated by solvent exchange. Nat. Mater. 15, 407–412 (2016).
Singla, S., Amarpuri, G., Dhopatkar, N., Blackledge, T. A. & Dhinojwala, A. Hygroscopic compounds in spider aggregate glue remove interfacial water to maintain adhesion in humid conditions. Nat. Commun. 9, 1890 (2018).
Gong, J. P., Katsuyama, Y., Kurokawa, T. & Osada, Y. Double-network hydrogels with extremely high mechanical strength. Adv. Mater. 15, 1155–1158 (2003).
Zhao, X. Multi-scale multi-mechanism design of tough hydrogels: building dissipation into stretchy networks. Soft Matter 10, 672–687 (2014).
Yuk, H., Zhang, T., Lin, S., Parada, G. A. & Zhao, X. Tough bonding of hydrogels to diverse non-porous surfaces. Nat. Mater. 15, 190–196 (2016).
Yuk, H., Zhang, T., Parada, G. A., Liu, X. & Zhao, X. Skin-inspired hydrogel–elastomer hybrids with robust interfaces and functional microstructures. Nat. Commun. 7, 12028 (2016).
Yuk, H., Lu, B. & Zhao, X. Hydrogel bioelectronics. Chem. Soc. Rev. 48, 1642–1667 (2019).
Gorgieva, S. & Kokol, V. Preparation, characterization, and in vitro enzymatic degradation of chitosan-gelatine hydrogel scaffolds as potential biomaterials. J. Biomed. Mater. Res. A 100A, 1655–1667 (2012).
Barnes, S., Spencer, M., Graham, D. & Johnson, H. B. Surgical wound irrigation: a call for evidence-based standardization of practice. Am. J. Infect. Control 42, 525–529 (2014).
Lang, N. et al. A blood-resistant surgical glue for minimally invasive repair of vessels and heart defects. Sci. Transl. Med. 6, 218ra6 (2014).
Yang, J., Bai, R. & Suo, Z. Topological adhesion of wet materials. Adv. Mater. 30, 1800671 (2018).
Whyte, W. et al. Sustained release of targeted cardiac therapy with a replenishable implanted epicardial reservoir. Nat. Biomed. Eng. 2, 416–428 (2018).
Jiang, W. W., Su, S. H., Eberhart, R. C. & Tang, L. Phagocyte responses to degradable polymers. J. Biomed. Mater. Res. A 82A, 492–497 (2007).
Yamagishi, K. et al. Tissue-adhesive wirelessly powered optoelectronic device for metronomic photodynamic cancer therapy. Nat. Biomed. Eng. 3, 27–36 (2019).
Feiner, R. et al. Engineered hybrid cardiac patches with multifunctional electronics for online monitoring and regulation of tissue function. Nat. Mater. 15, 679–685 (2016).
Roche, E. T. et al. Soft robotic sleeve supports heart function. Sci. Transl. Med. 9, eaaf3925 (2017).
VanDelinder, V. et al. Simple, benign, aqueous-based amination of polycarbonate surfaces. ACS Appl. Mater. Interfaces 7, 5643–5649 (2015).
Darnell, M. C. et al. Performance and biocompatibility of extremely tough alginate/polyacrylamide hydrogels. Biomaterials 34, 8042–8048 (2013).
Yuk, H. & Zhao, X. A new 3D printing strategy by harnessing deformation, instability, and fracture of viscoelastic inks. Adv. Mater. 30, 1704028 (2018).
Jamshidi, A., Beigi, F. A. K., Kabiri, K. & Zohuriaan-Mehr, M. Optimized HPLC determination of residual monomer in hygienic SAP hydrogels. Polym. Test. 24, 825–828 (2005).
Wang, C., Yan, Q., Liu, H.-B., Zhou, X.-H. & Xiao, S.-J. Different EDC/NHS activation mechanisms between PAA and PMAA brushes and the following amidation reactions. Langmuir 27, 12058–12068 (2011).
Lim, C. Y. et al. Succinimidyl ester surface chemistry: implications of the competition between aminolysis and hydrolysis on covalent protein immobilization. Langmuir 30, 12868–12878 (2014).
Acknowledgements
We thank J. Hu and M. Guo in the Massachusetts Institute of Technology (MIT) Mechanical Engineering Department for their help with the cell viability test; T. McClure in the MIT Materials Research Laboratory for help with the FTIR measurement; and S. Ngoy in the Brigham and Women’s Hospital (BHW) Rodent Cardiovascular Physiology Core for technical support with rodent surgery. This work is supported by the US National Science Foundation (NSF; grant CMMI-1661627) and Office of Naval Research (N00014-17-1-2920). H.Y. acknowledges financial support from a Samsung Scholarship. C.E.V. acknowledges financial support from the NSF Graduate Research Fellowship Program.
Author information
Authors and Affiliations
Contributions
H.Y. conceived the idea. H.Y. developed the materials and methods for the DST. H.Y. and C.S.N. designed the in vitro and ex vivo experiments. H.Y. conducted the in vitro and ex vivo experiments. C.E.V., H.Y. and E.T.R. designed the in vivo experiments. C.E.V. and H.Y. conducted the in vivo experiments. X.M., H.Y. and X.Z. developed the quantitative model for the DST. R.F.P. conducted histological assessments. H.Y., C.E.V., R.F.P., E.T.R. and X.Z. analysed the results. H.Y. and X.Z. wrote the manuscript with input from all authors. X.Z. supervised the study.
Corresponding author
Ethics declarations
Competing interests
H.Y. and X.Z. are inventors of a patent application (US patent 62/845,976) that covers the dry-crosslinking mechanism and the design of DST.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 The overall process of DST application.
The DST can be applied directly onto wet tissue surfaces after removing the backing, without any other preparation process. Upon contact with the wet surfaces, the DST dries them by quickly swelling and absorbing the interfacial water. Simultaneously, the carboxylic acid groups in the DST form temporary crosslinks through intermolecular bonds with the tissue surfaces, followed by covalent crosslinking between NHS ester groups in the DST and primary amine groups on the tissues. After adhering on tissues, the swollen DST becomes a thin layer of tough hydrogel which provides robust adhesion between the surfaces. Dissipation indicates the mechanical energy dissipation from the DST during deformation by the applied force, F.
Extended Data Fig. 2 Presence of NHS ester and surface amine coupling of the DST.
a, Transmission FTIR spectrum of the DST with NHS ester. The carboxylic acid C=O stretch at 1,710 cm−1 is associated with PAAc in the DST. The symmetric C–N–C stretch at 1,219 cm−1 and asymmetric C–N–C stretch at 1,307 cm−1 are associated with NHS ester in the DST35,36. b, Schematic illustration of covalent crosslinking between amine-coupled fluorescent microbeads (µ-beads) with the DST. c, Fluorescence microscopy images of covalently crosslinked microbeads with DST with NHS ester (left) and DST without NHS ester (right).
Extended Data Fig. 3 Swelling of the DST.
a, Swelling ratio and thickness of the chitosan-based DST as a function of time after pressing between two wet porcine skins. b, Dark-field microscopic image and bright-field image overlaid with green fluorescence of porcine skins adhered by the chitosan-based DST 5 min after application. c, Dark-field microscopic image and bright-field image overlaid with green fluorescence of porcine skins adhered by the chitosan-based DST 24 h after application. The sample was kept in a wet environment throughout the measurement.
Extended Data Fig. 4 Properties of the dry DST.
a, The DST is initially prepared as a thin dry film that can conform to tissue surfaces. b, Nominal stress versus engineering strain for the dry DST. The measured Young’s modulus of the dry DST is 5.7 GPa.
Extended Data Fig. 5 Quantification of residual monomer in the DST by HPLC.
a, Standard calibration curve of acrylic acid for HPLC. b, Results of HPLC characterization of the DST extraction solution. The DST has a very low concentration of residual acrylic acid monomers: 74 ng per 1 mg of the DST.
Extended Data Fig. 6 Setups for mechanical testing of adhesion performance.
a, Setup for measurement of interfacial toughness, based on the standard 180-degree peel test (ASTM F2256). b, Setup for measurement of shear strength, based on the standard lap-shear test (ASTM F2255). c, Setup for measurement of tensile strength, based on the standard tensile test (ASTM F2258). F, force; Fplateau, plateau force in peel test; Fmax, maximum force in lap-shear and tensile test; L, length; W, width.
Extended Data Fig. 7 Effect of covalent crosslinks on the long-term stability of adhesion by the DST.
a, Interfacial toughness and shear and tensile strength versus pressing time for wet porcine skins adhered by the DST without NHS ester. Note that these adhesion tests were performed immediately after the initial pressing. b, Interfacial toughness and shear and tensile strength versus time after pressing for wet porcine skins adhered by the DST without NHS ester. Note that all samples for b were kept in wet environments before the mechanical tests. Values represent the mean and the standard deviation (n = 3–5).
Extended Data Fig. 8 Adhesion performances of the DST and various existing tissue adhesives.
Shown are typical values for interfacial toughness, shear and tensile strength, and application time required for adhesion formation, for the DST (adhered between hydrogel and porcine skin) and various existing tissue adhesives. The interfacial toughness, shear strength and tensile strength for all commercially available adhesives were measured according to the application manual provided for each product. The application time for commercially available adhesives was based on the application manuals provided. The data for ultraviolet-curable surgical glue24, nanoparticle solution8 and tough hydrogel adhesive12 were obtained from the literature. Values represent the mean and the standard deviation (n = 3–5).
Extended Data Fig. 9 Surface functionalization of engineering solids.
a, Primary amine functionalization of silicon, titanium and PDMS, and subsequent covalent coupling between the primary amine groups and the NHS ester groups in the DST. b, Primary amine functionalization of polycarbonate, and subsequent covalent coupling between the primary amine groups and the NHS ester groups in the DST. c, Primary amine functionalization of polyimide, and subsequent covalent coupling between the primary amine groups and the NHS ester groups in the DST.
Extended Data Fig. 10 Sealing of ex vivo porcine trachea and small intestine by the DST.
a, Sealing of an air-leaking, lacerated ex vivo porcine trachea by a hydrogel patch adhered by the DST. b, Anastomosis of a dissected ex vivo porcine small intestine by the DST.
Supplementary information
Supplementary Information
This file contains Supplementary Texts, Supplementary Figs. 1 to 16, and Supplementary References.
Supplementary Video 1
Overall process of adhesion formation between wet porcine skins by the DST.
Supplementary Video 2
Adhesion formation between various wet porcine tissues by the DST.
Supplementary Video 3
Adhesion formation between wet porcine skins and engineering solids by the DST.
Supplementary Video 4
Adhesion of DST-TPU patch on beating rat heart in vivo.
Supplementary Video 5
Sealing of an air-leaking ex vivo porcine lung by adhesion of a hydrogel patch by the DST.
Supplementary Video 6
Sealing of a fluid-leaking ex vivo stomach by adhesion of a hydrogel patch by the DST.
Supplementary Video 7
Anastomosis of a dissected ex vivo small intestine by the DST.
Supplementary Video 8
Adhesion of a drug patch on a beating ex vivo porcine heart by the DST.
Supplementary Video 9
Adhesion of a strain sensor on a beating ex vivo porcine heart by the DST.
Rights and permissions
About this article
Cite this article
Yuk, H., Varela, C.E., Nabzdyk, C.S. et al. Dry double-sided tape for adhesion of wet tissues and devices. Nature 575, 169–174 (2019). https://doi.org/10.1038/s41586-019-1710-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-019-1710-5
This article is cited by
-
Mussel-inspired resilient hydrogels with strong skin adhesion and high-sensitivity for wearable device
Nano Convergence (2024)
-
Swim bladder-derived biomaterials: structures, compositions, properties, modifications, and biomedical applications
Journal of Nanobiotechnology (2024)
-
A magnetic multi-layer soft robot for on-demand targeted adhesion
Nature Communications (2024)
-
Surface hydrophobization of hydrogels via interface dynamics-induced network reconfiguration
Nature Communications (2024)
-
A 3D printable tissue adhesive
Nature Communications (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.