Abstract
Dysfunctional breathing is the main cause of morbidity and mortality after traumatic injury of the cervical spinal cord1,2 and often necessitates assisted ventilation, thus stressing the need to develop strategies to restore breathing. Cervical interneurons that form synapses on phrenic motor neurons, which control the main inspiratory muscle, can modulate phrenic motor output and diaphragmatic function3,4,5. Here, using a combination of pharmacogenetics and respiratory physiology assays in different models of spinal cord injury, we show that mid-cervical excitatory interneurons are essential for the maintenance of breathing in mice with non-traumatic cervical spinal cord injury, and are also crucial for promoting respiratory recovery after traumatic spinal cord injury. Although these interneurons are not necessary for breathing under normal conditions, their stimulation in non-injured animals enhances inspiratory amplitude. Immediately after spinal cord injury, pharmacogenetic stimulation of cervical excitatory interneurons restores respiratory motor function. Overall, our results demonstrate a strategy to restore breathing after central nervous system trauma by targeting a neuronal subpopulation.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All quantification data from figures are provided in the Supplementary Information and all raw data are available upon reasonable request.
References
Jackson, A. B. & Groomes, T. E. Incidence of respiratory complications following spinal cord injury. Arch. Phys. Med. Rehabil. 75, 270–275 (1994).
Berlly, M. & Shem, K. Respiratory management during the first five days after spinal cord injury. J. Spinal Cord Med. 30, 309–318 (2007).
Palisses, R., Perségol, L. & Viala, D. Evidence for respiratory interneurones in the C3-C5 cervical spinal cord in the decorticate rabbit. Exp. Brain Res. 78, 624–632 (1989).
Lane, M. A. et al. Cervical prephrenic interneurons in the normal and lesioned spinal cord of the adult rat. J. Comp. Neurol. 511, 692–709 (2008).
Cregg, J. M. et al. A latent propriospinal network can restore diaphragm function after high cervical spinal cord injury. Cell Reports 21, 654–665 (2017).
Como, J. J. et al. Characterizing the need for mechanical ventilation following cervical spinal cord injury with neurologic deficit. J. Trauma 59, 912–916, discussion 916 (2005).
Lane, M. A. et al. Respiratory function following bilateral mid-cervical contusion injury in the adult rat. Exp. Neurol. 235, 197–210 (2012).
Brown, R., DiMarco, A. F., Hoit, J. D. & Garshick, E. Respiratory dysfunction and management in spinal cord injury. Respir. Care 51, 853–868, discussion 869–870 (2006).
DeVivo, M. J., Black, K. J. & Stover, S. L. Causes of death during the first 12 years after spinal cord injury. Arch. Phys. Med. Rehabil. 74, 248–254 (1993).
Alilain, W. J., Horn, K. P., Hu, H., Dick, T. E. & Silver, J. Functional regeneration of respiratory pathways after spinal cord injury. Nature 475, 196–200 (2011).
Grassner, L. et al. Nontraumatic spinal cord injury at the neurological intensive care unit: spectrum, causes of admission and predictors of mortality. Ther. Adv. Neurol. Disord. 9, 85–94 (2016).
New, P. W. et al. International retrospective comparison of inpatient rehabilitation for patients with spinal cord dysfunction epidemiology and clinical outcomes. Arch. Phys. Med. Rehabil. 96, 1080–1087 (2015).
Nouri, A., Tetreault, L., Singh, A., Karadimas, S. K. & Fehlings, M. G. Degenerative cervical myelopathy: epidemiology, genetics, and pathogenesis. Spine 40, E675–E693 (2015).
Toyoda, H., Nakamura, H., Konishi, S., Terai, H. & Takaoka, K. Does chronic cervical myelopathy affect respiratory function? J. Neurosurg. Spine 1, 175–178 (2004).
Bhagavatula, I. D. et al. Subclinical respiratory dysfunction in chronic cervical cord compression: a pulmonary function test correlation. Neurosurg. Focus 40, E3 (2016).
Karadimas, S. K. et al. Riluzole blocks perioperative ischemia-reperfusion injury and enhances postdecompression outcomes in cervical spondylotic myelopathy. Sci. Transl. Med. 7, 316ra194 (2015).
Karadimas, S. K. et al. A novel experimental model of cervical spondylotic myelopathy (CSM) to facilitate translational research. Neurobiol. Dis. 54, 43–58 (2013).
Yu, W. R., Liu, T., Kiehl, T. R. & Fehlings, M. G. Human neuropathological and animal model evidence supporting a role for Fas-mediated apoptosis and inflammation in cervical spondylotic myelopathy. Brain 134, 1277–1292 (2011).
Malone, A., Meldrum, D. & Bolger, C. Gait impairment in cervical spondylotic myelopathy: comparison with age- and gender-matched healthy controls. Eur. Spine J. 21, 2456–2466 (2012).
Ono, K. et al. Myelopathy hand. New clinical signs of cervical cord damage. J. Bone Joint Surg. Br. 69, 215–219 (1987).
Kullander, K. et al. Role of EphA4 and EphrinB3 in local neuronal circuits that control walking. Science 299, 1889–1892 (2003).
Bezdudnaya, T., Hormigo, K. M., Marchenko, V. & Lane, M. A. Spontaneous respiratory plasticity following unilateral high cervical spinal cord injury in behaving rats. Exp. Neurol. 305, 56–65 (2018).
Goshgarian, H. G. The crossed phrenic phenomenon and recovery of function following spinal cord injury. Respir. Physiol. Neurobiol. 169, 85–93 (2009).
Alilain, W. J. & Goshgarian, H. G. MK-801 upregulates NR2A protein levels and induces functional recovery of the ipsilateral hemidiaphragm following acute C2 hemisection in adult rats. J. Spinal Cord Med. 30, 346–354 (2007).
Golder, F. J. et al. Respiratory motor recovery after unilateral spinal cord injury: eliminating crossed phrenic activity decreases tidal volume and increases contralateral respiratory motor output. J. Neurosci. 23, 2494–2501 (2003).
Fuller, D. D. et al. Modest spontaneous recovery of ventilation following chronic high cervical hemisection in rats. Exp. Neurol. 211, 97–106 (2008).
Huang, R. et al. Modulation of respiratory output by cervical epidural stimulation in the anesthetized mouse. J. Appl. Physiol. 121, 1272–1281 (2016).
Streeter, K. A. et al. Intermittent hypoxia enhances functional connectivity of midcervical spinal interneurons. J. Neurosci. 37, 8349–8362 (2017).
Satkunendrarajah, K. et al. Riluzole promotes motor and respiratory recovery associated with enhanced neuronal survival and function following high cervical spinal hemisection. Exp. Neurol. 276, 59–71 (2016).
Klironomos, G. et al. New experimental rabbit animal model for cervical spondylotic myelopathy. Spinal Cord 49, 1097–1102 (2011).
Mantilla, C. B., Zhan, W. Z. & Sieck, G. C. Retrograde labeling of phrenic motoneurons by intrapleural injection. J. Neurosci. Methods 182, 244–249 (2009).
Bilney, B., Morris, M. & Webster, K. Concurrent related validity of the GAITRite walkway system for quantification of the spatial and temporal parameters of gait. Gait Posture 17, 68–74 (2003).
Farr, T. D., Liu, L., Colwell, K. L., Whishaw, I. Q. & Metz, G. A. Bilateral alteration in stepping pattern after unilateral motor cortex injury: a new test strategy for analysis of skilled limb movements in neurological mouse models. J. Neurosci. Methods 153, 104–113 (2006).
Whishaw, I. Q. & Pellis, S. M. The structure of skilled forelimb reaching in the rat: a proximally driven movement with a single distal rotatory component. Behav. Brain Res. 41, 49–59 (1990).
Minic, Z. et al. Nanoconjugate-bound adenosine A1 receptor antagonist enhances recovery of breathing following acute cervical spinal cord injury. Exp. Neurol. 292, 56–62 (2017).
Montandon, G., Horner, R. L., Kinkead, R. & Bairam, A. Caffeine in the neonatal period induces long-lasting changes in sleep and breathing in adult rats. J. Physiol. (Lond.) 587, 5493–5507 (2009).
McKay, L. C. & Feldman, J. L. Unilateral ablation of pre-Botzinger complex disrupts breathing during sleep but not wakefulness. Am. J. Respir. Crit. Care Med. 178, 89–95 (2008).
Acknowledgements
This research was supported by grant 2987 from the PVA Research Foundation (M.G.F. and K.S.), CIHR Grant MOP13683 (M.G.F.), AOSPINE Young Investigator Research Grant (K.S.); the Halbert Chair (M.G.F.) and the DeZwirek Foundation (M.G.F.). S.K.K. was supported by the Onassis Foundation. We thank A. Andreopoulou and J. Kallitsis for the ntSCI compression material; J. Austin for logistical support; C. Castro and L. Li for technical assistance; L. Teves (M. Tymianski’s laboratory) for assistance with blood gas measurement. We thank our colleagues for constructive feedback.
Reviewer information
Nature thanks J. Feldman and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
Study conception: K.S., S.K.K. and M.G.F. Experimental design: K.S. and S.K.K. ntSCI surgeries: S.K.K. (A.M.L. for Extended Data Fig. 2). SCI surgeries: K.S. Viral intraspinal injections: K.S. and S.K.K. Electrophysiological experiments and analysis: K.S. Plethysmography: K.S. and G.M. Anatomical experiments: S.K.K. and K.S. Neurobehavioural and blood gas experiments: K.S. and S.K.K. Molecular and viral work: A.M.L. Statistics: A.M.L. Supervision: M.G.F. All authors discussed the results and participated in writing the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 MRI of the cervical spine of a patient with ntSCI due to degenerative cervical myelopathy.
Arrows point to an area of severe compression of the cervical spinal cord at the C3–C5 levels, the area that houses the PMNs. Of note, this patient did not have clinical respiratory deficits.
Extended Data Fig. 2 ntSCI mice demonstrate notable compression of the cervical spinal cord.
a, Sagittal 3D view of a reconstructed cervical spinal cord of a ntSCI mouse extending from C1 (rostral, r) to C8 (caudal, c) demonstrates the compressive injury at C4–C6 spinal level (arrow). b, Cervical spinal cord sections of ntSCI and sham mice stained with haematoxylin and eosin and luxol fast blue (representative of 4 biological replicates). Scale bar, 600 μm.
Extended Data Fig. 3 Mice and humans with ntSCI display similar gait dysfunction.
Representative footprint images from both a mouse (hindpaws only are displayed) and a human ntSCI subject demonstrating decreased stride length and increased base of support during walking relative to control subjects.
Extended Data Fig. 4 ntSCI mice display a significant loss of manual dexterity.
a, Representative position–time graph of forepaw movements during skilled walking on a horizontal ladder. b, Bar graph demonstrating an increased number of incorrect forepaw placements as a percentage of total placements in ntSCI mice during ladder walk (P = 0.0012, 95% CI = 16.02 to 39.69). c, Representative image showing reaching and grasping by a ntSCI mouse. d, The number of unsuccessful reaches was greater in ntSCI versus sham mice (P = 0.0025, 95% CI = 5.126 to 15.01). e, The time taken (seconds) to consume a whole length of pasta during the Capellini handling test was increased in ntSCI mice (P = 5.71 × 10−5, 95% CI = 59.06 to 97.21). f, The number of grip adjustments made by the mice during the consumption of the pasta (P = 0.0063, 95% CI = 13.34 to 52.66). Statistical significance was determined using an independent samples two-tailed t-test in b, d–f; n = 3 mice for sham and n = 5 mice for ntSCI. Data are mean ± s.e.m. *P < 0.05.
Extended Data Fig. 5 Functional plasticity of the cervical respiratory network under ntSCI.
a, Stacked column graph demonstrating the number of animals with recovered ipsilateral (left) hemidiaphragmatic electromyography (EMG) activity immediately after left C2 hemisection (n = 4 mice per group). Length of compression in the ntSCI animals was related to the proportion of animals with ipsilateral inspiratory activity after C2 hemisection (P = 0.0034, chi-square test for trend). b, Representative EMG recordings from the left hemidiaphragm immediately after left C2 hemisection in sham as well as in 2-, 4- and 8-week ntSCI mice.
Extended Data Fig. 6 C2 hemisection.
Haematoxylin and eosin-stained cervical spinal cord section from a mouse subjected to a left C2 hemisection injury. Scale bar, 600 μm. Staining was performed on 22 separate C2 hemisection samples with similar results.
Extended Data Fig. 7 Anatomical plasticity of the cervical respiratory network in ntSCI.
a, Schematic demonstrating the injection paradigm to assess the anatomical plasticity of the cervical respiratory network after ntSCI. b, c, Bar graphs demonstrating a greater number of cervical interneurons connected to the preserved PMNs (P = 2.0 × 10−4, 95% CI = 96.44 to 183.8, unpaired t-test, two-tailed), and more specifically, a greater number of contralateral cervical interneurons in 8-week ntSCI mice (P = 0.0024, 95% CI = −166.2230 to −40.71032, repeated-measures ANOVA with Sidak’s post hoc test for ipsilateral and contralateral comparisons; n = 3 mice for sham group and n = 5 mice for ntSCI). d, Confocal image of 30-μm-thick transverse cervical spinal cord section demonstrating PRV-traced PMNs on the left (ipsilateral) and prephrenic interneurons in the contralateral ventromedial region; the area where most prephrenic interneurons were located. e, Projections of the PRV152-traced pre-phrenic interneurons to the contralateral area housing the PMNs. Visualization of PRV152 was performed for all samples (n = 3 mice for sham and n = 5 mice for ntSCI) with similar results. Data are mean ± s.e.m. *P < 0.05, **P < 0.001.
Extended Data Fig. 8 Expression of PSAM in midcervical excitatory neurons.
High magnification confocal images demonstrate the expression of PSAM (GFP+) in only the excitatory cells (tdTomato+) of the intermediate grey matter. The images were taken from the same sections depicted in Fig. 2c, and are representative of results from 6 biological replicates. Scale bar, 50 μm.
Extended Data Fig. 9 Stimulation of cervical eINs enhances respiratory output.
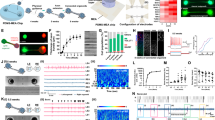
a, Scheme demonstrating the approach used to express hM3Dq–mCherry in the eINs of the intermediate grey matter of C4–C5 spinal level. The Cre-dependent AAV-DIO-hM3Dq-mCherry viral construct was injected in the intermediate grey matter area of the cervical spinal cord of uninjured Vglut2::cre mice (VGLUT2-hM3Dq). b, Representative confocal image demonstrating the expression of hM3Dq–mCherry in the glutamatergic cells of the area of interest (based on 8 biological replicates). Note the lack of expression in the area of motor neurons. CC denotes the central canal. Scale bar, 100 μm. c, Respiratory measurements showed increased inspiratory amplitude but no change in respiratory frequency following stimulation of the cervical eINs (P = 0.9042, repeated-measures ANOVA; n = 8 mice for saline control and CNO groups). The interaction between the change in respiratory amplitude after injection, and treatment (saline versus CNO) was highly significant (P = 0.0002, repeated-measures ANOVA), indicating that the relative change after saline injection is not equal to the relative change after CNO (n = 8 mice for saline control and CNO groups). d, CNO did not change either the inspiratory amplitude (P = 0.3513, paired two-tailed t-test, 95% CI = −0.1077 to 0.04301, n = 9 mice) or the respiratory frequency (P = 0.6906, paired two-tailed t-test, 95% CI = −10.70 to 15.37, n = 9 mice) in Vglut2::cre mice lacking the AAV-DIO-hM3Dq-mCherry injections. e, Representative respiratory activity from VGLUT2-hM3Dq mice before and after saline or CNO administration. f, Representative respiratory activity from Vglut2::cre mice lacking AAV-DIO-hM3Dq-mCherry injection, before and after CNO administration.
Supplementary information
Rights and permissions
About this article
Cite this article
Satkunendrarajah, K., Karadimas, S.K., Laliberte, A.M. et al. Cervical excitatory neurons sustain breathing after spinal cord injury. Nature 562, 419–422 (2018). https://doi.org/10.1038/s41586-018-0595-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-018-0595-z
Keywords
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.