Abstract
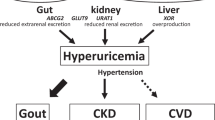
Asymptomatic hyperuricaemia affects ~20% of the general population in the USA, with variable rates in other countries. Historically, asymptomatic hyperuricaemia was considered a benign laboratory finding with little clinical importance in the absence of gout or kidney stones. Yet, increasing evidence suggests that asymptomatic hyperuricaemia can predict the development of hypertension, obesity, diabetes mellitus and chronic kidney disease and might contribute to disease by stimulating inflammation. Although urate has been classically viewed as an antioxidant with beneficial effects, new data suggest that both crystalline and soluble urate activate various pro-inflammatory pathways. This Review summarizes what is known about the role of urate in the inflammatory response. Further research is needed to define the role of asymptomatic hyperuricaemia in these pro-inflammatory pathways.
Key points
-
Hyperuricaemia is a common laboratory finding that precedes gout and is associated with gout, as well as with hypertension, acute and chronic kidney disease, obesity, metabolic syndrome, fatty liver and diabetes mellitus.
-
The causative role of elevated serum urate in these inflammatory conditions is controversial, but several urate-driven inflammatory mechanisms and other mechanisms have been described.
-
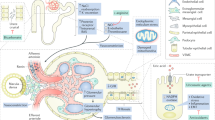
Urate crystals activate the NLRP3 inflammasome and contribute to IL-1β activation through autophagy dysfunction, diminished clearance of damaged organelles, altered redox status and/or AMP-activated protein kinase (AMPK) inhibition.
-
Urate crystals can promote inflammasome-independent mechanisms, such as serine protease-dependent activation of pro-inflammatory cytokines, formation of neutrophil extracellular traps and resolution of inflammation.
-
Soluble urate also has pro-oxidative effects in several cell types and induces inflammatory signalling through several mechanisms, such as MAPK pathway activation, AKT-mTOR activation or AMPK inhibition.
-
Soluble urate and hyperuricaemia exposure could alter the epigenetic programme of innate immune cells and contribute to common adult diseases by promoting persistent inflammatory hyperresponsiveness.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bursill, D. et al. Gout, hyperuricemia, and crystal-associated disease network consensus statement regarding labels and definitions for disease elements in gout. Arthritis Care Res. 71, 427–434 (2019).
Zhu, Y., Pandya, B. J. & Choi, H. K. Prevalence of gout and hyperuricemia in the US general population: the National Health and Nutrition Examination Survey 2007–2008. Arthritis Rheum. 63, 3136–3141 (2011).
Richette, P. et al. 2016 updated EULAR evidence-based recommendations for the management of gout. Ann. Rheum. Dis. 76, 29–42 (2017).
Sivera, F. et al. Multinational evidence-based recommendations for the diagnosis and management of gout: integrating systematic literature review and expert opinion of a broad panel of rheumatologists in the 3e initiative. Ann. Rheum. Dis. 73, 328–335 (2014).
Dalbeth, N. et al. Discordant American College of Physicians and international rheumatology guidelines for gout management: consensus statement of the Gout, Hyperuricemia and Crystal-Associated Disease Network (G-CAN). Nat. Rev. Rheumatol. 13, 561–568 (2017).
Khanna, D. et al. 2012 American College of Rheumatology guidelines for management of gout. Part 1: systematic nonpharmacologic and pharmacologic therapeutic approaches to hyperuricemia. Arthritis Care Res. 64, 1431–1446 (2012).
Neogi, T. & Mikuls, T. R. To treat or not to treat (to target) in gout. Ann. Intern. Med. 166, 71–72 (2017).
Jensen, T. et al. Fructose and sugar: a major mediator of non-alcoholic fatty liver disease. J. Hepatol. 68, 1063–1075 (2018).
Johnson, R. J. et al. Hyperuricemia, acute and chronic kidney disease, hypertension, and cardiovascular disease: report of a scientific workshop organized by the national kidney foundation. Am. J. Kidney Dis. 71, 851–865 (2018).
Grayson, P. C., Kim, S. Y., LaValley, M. & Choi, H. K. Hyperuricemia and incident hypertension: a systematic review and meta-analysis. Arthritis Care Res. 63, 102–110 (2011).
Johnson, R. J. et al. Sugar, uric acid, and the etiology of diabetes and obesity. Diabetes 62, 3307–3315 (2013).
Lv, Q. et al. High serum uric acid and increased risk of type 2 diabetes: a systemic review and meta-analysis of prospective cohort studies. PLOS ONE 8, e56864 (2013).
Kuwabara, M. et al. Asymptomatic hyperuricemia without comorbidities predicts cardiometabolic diseases: five-year Japanese cohort study. Hypertension 69, 1036–1044 (2017).
Yamanaka, H. Japanese Society of Gout and Nucleic Acid Metabolism. Japanese guideline for the management of hyperuricemia and gout: second edition. Nucleosides Nucleotides Nucleic Acids 30, 1018–1029 (2011).
Bursill, D., Taylor, W. J., Terkeltaub, R. & Dalbeth, N. The nomenclature of the basic disease elements of gout: a content analysis of contemporary medical journals. Semin. Arthritis Rheum. 48, 456–461 (2018).
Kahn, K., Serfozo, P. & Tipton, P. A. Identification of the true product of the urate oxidase reaction. J. Am. Chem. Soc. 119, 5435–5442 (1997).
Smith, H. W. From Fish to Philosopher. (Little, Brown and Co, 1953).
Poulson, T. L. et al. Uric acid: the main nitrogenous excretory product of birds. Science 170, 98–99 (1970).
Kratzer, J. T. et al. Evolutionary history and metabolic insights of ancient mammalian uricases. Proc. Natl Acad. Sci. USA 111, 3763–3768 (2014).
Oda, M., Satta, Y., Takenaka, O. & Takahata, N. Loss of urate oxidase activity in hominoids and its evolutionary implications. Mol. Biol. Evol. 19, 640–653 (2002).
Johnson, R. J. et al. Theodore E. Woodward Award: the evolution of obesity: insights from the mid-Miocene. Trans. Am. Clin. Climatol. Assoc. 121, 295–308 (2010).
Tan, P. K., Farrar, J. E., Gaucher, E. A. & Miner, J. N. Coevolution of URAT1 and uricase during primate evolution: implications for serum urate homeostasis and gout. Mol. Biol. Evol. 33, 2193–2200 (2016).
Orowan, E. The origin of man. Nature 175, 683–684 (1955).
Brooks, G. W. & Mueller, E. Serum urate concentrations among university professors; relation to drive, achievement, and leadership. JAMA 195, 415–418 (1966).
Sutin, A. R. et al. Impulsivity is associated with uric acid: evidence from humans and mice. Biol. Psychiatry 75, 31–37 (2014).
Ames, B. N., Cathcart, R., Schwiers, E. & Hochstein, P. Uric acid provides an antioxidant defense in humans against oxidant- and radical-caused aging and cancer: a hypothesis. Proc. Natl Acad. Sci. USA 78, 6858–6862 (1981).
Sevanian, A., Davies, K. J. & Hochstein, P. Serum urate as an antioxidant for ascorbic acid. Am. J. Clin. Nutr. 54, 1129S–1134S (1991).
Watanabe, S. et al. Uric acid, hominoid evolution, and the pathogenesis of salt-sensitivity. Hypertension 40, 355–360 (2002).
Johnson, R. J. & Andrews, P. Fructose, uricase, and the back-to-Africa hypothesis. Evol. Anthropol. 19, 250–257 (2010).
Cicerchi, C. et al. Uric acid-dependent inhibition of AMP kinase induces hepatic glucose production in diabetes and starvation: evolutionary implications of the uricase loss in hominids. FASEB J. 28, 3339–3350 (2014).
Gersch, C. et al. Inactivation of nitric oxide by uric acid. Nucleosides Nucleotides Nucleic Acids 27, 967–978 (2008).
Imaram, W. et al. Radicals in the reaction between peroxynitrite and uric acid identified by electron spin resonance spectroscopy and liquid chromatography mass spectrometry. Free Radic. Biol. Med. 49, 275–281 (2010).
Johnson, R. J., Titte, S., Cade, J. R., Rideout, B. A. & Oliver, W. J. Uric acid, evolution and primitive cultures. Semin. Nephrol. 25, 3–8 (2005).
Kottgen, A. et al. Genome-wide association analyses identify 18 new loci associated with serum urate concentrations. Nat. Genet. 45, 145–154 (2013).
Nakatochi, M. et al. Genome-wide meta-analysis identifies multiple novel loci associated with serum uric acid levels in Japanese individuals. Commun. Biol. 2, 115 (2019).
Major, T. J., Dalbeth, N., Stahl, E. A. & Merriman, T. R. An update on the genetics of hyperuricaemia and gout. Nat. Rev. Rheumatol. 14, 341–353 (2018).
Tin, A. et al. Large-scale whole-exome sequencing association studies identify rare functional variants influencing serum urate levels. Nat. Commun. 9, 4228 (2018).
Johnson, R. J. et al. Is there a pathogenetic role for uric acid in hypertension and cardiovascular and renal disease? Hypertension 41, 1183–1190 (2003).
Neogi, T. Gout. Ann. Intern. Med. 165, ITC1–ITC16 (2016).
Choi, H. K., Atkinson, K., Karlson, E. W., Willett, W. & Curhan, G. Purine-rich foods, dairy and protein intake, and the risk of gout in men. N. Engl. J. Med. 350, 1093–1103 (2004).
Quinones, G. A. et al. Effect of insulin on uric acid excretion in humans. Am. J. Physiol. 268, E1–E5 (1995).
Kahn, A. M. Effect of diuretics on the renal handling of urate. Semin. Nephrol. 8, 305–314 (1988).
Lee, S. M. et al. Low serum uric acid level is a risk factor for death in incident hemodialysis patients. Am. J. Nephrol. 29, 79–85 (2009).
Suliman, M. E. et al. J-shaped mortality relationship for uric acid in CKD. Am. J. Kidney Dis. 48, 761–771 (2006).
Kuo, C. F., Grainge, M. J., Zhang, W. & Doherty, M. Global epidemiology of gout: prevalence, incidence and risk factors. Nat. Rev. Rheumatol. 11, 649–662 (2015).
Faires, J. S. & McCarty, D. J. Acute arthritis in man and dog after intrasynovial injection of sodium urate crystals. Lancet 280, 682–685 (1962).
Shimizu, T., Hori, H., Umeyama, M. & Shimizu, K. Characteristics of gout patients according to the laterality of nephrolithiasis: a cross-sectional study using helical computed tomography. Int. J. Rheum. Dis. 22, 567–573 (2019).
Landgren, A. J. et al. Incidence of and risk factors for nephrolithiasis in patients with gout and the general population, a cohort study. Arthritis Res. Ther. 19, 173 (2017).
Marchini, G. S., Sarkissian, C., Tian, D., Gebreselassie, S. & Monga, M. Gout, stone composition and urinary stone risk: a matched case comparative study. J. Urol. 189, 1334–1339 (2013).
Hahn, K., Kanbay, M., Lanaspa, M. A., Johnson, R. J. & Ejaz, A. A. Serum uric acid and acute kidney injury: a mini review. J. Adv. Res. 8, 529–536 (2017).
Shimada, M. et al. A novel role for uric acid in acute kidney injury associated with tumour lysis syndrome. Nephrol. Dial. Transpl. 24, 2960–2964 (2009).
Roncal-Jimenez, C. et al. Heat stress nephropathy from exercise-induced uric acid crystalluria: a perspective on Mesoamerican nephropathy. Am. J. Kidney Dis. 67, 20–30 (2016).
Ryu, E. S. et al. Uric acid-induced phenotypic transition of renal tubular cells as a novel mechanism of chronic kidney disease. Am. J. Physiol. Ren. Physiol. 304, F471–F480 (2013).
Zhou, Y. et al. Uric acid induces renal inflammation via activating tubular NF-κB signaling pathway. PLOS ONE 7, e39738 (2012).
Verzola, D. et al. Uric acid promotes apoptosis in human proximal tubule cells by oxidative stress and the activation of NADPH oxidase NOX 4. PLOS ONE 9, e115210 (2014).
Keenan, T. et al. Causal assessment of serum urate levels in cardiometabolic diseases through a mendelian randomization study. J. Am. Coll. Cardiol. 67, 407–416 (2016).
White, J. et al. Plasma urate concentration and risk of coronary heart disease: a Mendelian randomisation analysis. Lancet Diabetes Endocrinol. 4, 327–336 (2016).
Jordan, D. M. et al. No causal effects of serum urate levels on the risk of chronic kidney disease: a Mendelian randomization study. PLOS Med. 16, e1002725 (2019).
Johnson, R. J., Merriman, T. & Lanaspa, M. A. Causal or noncausal relationship of uric acid with diabetes. Diabetes 64, 2720–2722 (2015).
Su, X., Xu, B., Yan, B., Qiao, X. & Wang, L. Effects of uric acid-lowering therapy in patients with chronic kidney disease: a meta-analysis. PLOS ONE 12, e0187550 (2017).
Qu, L. H., Jiang, H. & Chen, J. H. Effect of uric acid-lowering therapy on blood pressure: systematic review and meta-analysis. Ann. Med. 49, 142–156 (2017).
Martinon, F., Petrilli, V., Mayor, A., Tardivel, A. & Tschopp, J. Gout-associated uric acid crystals activate the NALP3 inflammasome. Nature 440, 237–241 (2006).
Dinarello, C. A. A clinical perspective of IL-1β as the gatekeeper of inflammation. Eur. J. Immunol. 41, 1203–1217 (2011).
Dinarello, C. A. The history of fever, leukocytic pyrogen and interleukin-1. Temperature 2, 8–16 (2015).
Gross, O., Thomas, C. J., Guarda, G. & Tschopp, J. The inflammasome: an integrated view. Immunol. Rev. 243, 136–151 (2011).
Kelley, N., Jeltema, D., Duan, Y. & He, Y. The NLRP3 inflammasome: an overview of mechanisms of activation and regulation. Int. J. Mol. Sci. 20, E3328 (2019).
Netea, M. G. et al. Differential requirement for the activation of the inflammasome for processing and release of IL-1β in monocytes and macrophages. Blood 113, 2324–2335 (2009).
Misawa, T. et al. Microtubule-driven spatial arrangement of mitochondria promotes activation of the NLRP3 inflammasome. Nat. Immunol. 14, 454–460 (2013).
Joosten, L. A. et al. Engagement of fatty acids with Toll-like receptor 2 drives interleukin-1β production via the ASC/caspase 1 pathway in monosodium urate monohydrate crystal-induced gouty arthritis. Arthritis Rheum. 62, 3237–3248 (2010).
Jhang, J. J., Cheng, Y. T., Ho, C. Y. & Yen, G. C. Monosodium urate crystals trigger Nrf2- and heme oxygenase-1-dependent inflammation in THP-1 cells. Cell Mol. Immunol. 12, 424–434 (2015).
Kim, S. K., Choe, J. Y. & Park, K. Y. Enhanced p62 is responsible for mitochondrial pathway-dependent apoptosis and interleukin-1β production at the early phase by monosodium urate crystals in murine macrophage. Inflammation 39, 1603–1616 (2016).
Wang, Y., Viollet, B., Terkeltaub, R. & Liu-Bryan, R. AMP-activated protein kinase suppresses urate crystal-induced inflammation and transduces colchicine effects in macrophages. Ann. Rheum. Dis. 75, 286–294 (2014).
Vazirpanah, N. et al. mTOR inhibition by metformin impacts monosodium urate crystal-induced inflammation and cell death in gout: a prelude to a new add-on therapy? Ann. Rheumat. Dis. 78, 663–671 (2019).
Cumpelik, A., Ankli, B., Zecher, D. & Schifferli, J. A. Neutrophil microvesicles resolve gout by inhibiting C5a-mediated priming of the inflammasome. Ann. Rheum. Dis. 75, 1236–1245 (2016).
Russell, I. J., Mansen, C., Kolb, L. M. & Kolb, W. P. Activation of the fifth component of human complement (C5) induced by monosodium urate crystals: C5 convertase assembly on the crystal surface. Clin. Immunol. Immunopathol. 24, 239–250 (1982).
Netea, M. G., van de Veerdonk, F. L., van der Meer, J. W., Dinarello, C. A. & Joosten, L. A. Inflammasome-independent regulation of IL-1-family cytokines. Ann. Rev. Immunol. 33, 49–77 (2015).
Cho, J. S. et al. Neutrophil-derived IL-1β is sufficient for abscess formation in immunity against Staphylococcus aureus in mice. PLOS Pathog. 8, e1003047 (2012).
Schreiber, A. et al. Neutrophil serine proteases promote IL-1β generation and injury in necrotizing crescentic glomerulonephritis. J. Am. Soc. Nephrol. 23, 470–482 (2012).
Joosten, L. A. et al. Alpha-1-anti-trypsin-Fc fusion protein ameliorates gouty arthritis by reducing release and extracellular processing of IL-1β and by the induction of endogenous IL-1Ra. Ann. Rheumat. Dis. 75, 1219–1227 (2015).
Hahn, J. et al. Aggregated neutrophil extracellular traps resolve inflammation by proteolysis of cytokines and chemokines and protection from antiproteases. FASEB J. 33, 1401–1414 (2018).
Schauer, C. et al. Aggregated neutrophil extracellular traps limit inflammation by degrading cytokines and chemokines. Nat. Med. 20, 511–517 (2014).
Schorn, C. et al. Bonding the foe-NETting neutrophils immobilize the pro-inflammatory monosodium urate crystals. Front. Immunol. 3, 376 (2012).
Reber, L. L., Gaudenzio, N., Starkl, P. & Galli, S. J. Neutrophils are not required for resolution of acute gouty arthritis in mice. Nat. Med. 22, 1382–1384 (2016).
Reinwald, C. et al. Reply to “Neutrophils are not required for resolution of acute gouty arthritis in mice”. Nat. Med. 22, 1384–1386 (2016).
Desai, J., Steiger, S. & Anders, H. J. Molecular pathophysiology of gout. Trends Mol. Med. 23, 756–768 (2017).
Manfredi, A. A., Ramirez, G. A., Rovere-Querini, P. & Maugeri, N. The neutrophil’s choice: phagocytose vs make neutrophil extracellular traps. Front. Immunol. 9, 288 (2018).
Gersch, C. et al. Reactions of peroxynitrite with uric acid: formation of reactive intermediates, alkylated products and triuret, and in vivo production of triuret under conditions of oxidative stress. Nucleosides Nucleotides Nucleic Acids 28, 118–149 (2009).
Meotti, F. C. et al. Urate as a physiological substrate for myeloperoxidase: implications for hyperuricemia and inflammation. J. Biol. Chem. 286, 12901–12911 (2011).
Corry, D. B. et al. Uric acid stimulates vascular smooth muscle cell proliferation and oxidative stress via the vascular renin-angiotensin system. J. Hypertens. 26, 269–275 (2008).
Yu, M. A., Sanchez-Lozada, L. G., Johnson, R. J. & Kang, D. H. Oxidative stress with an activation of the renin-angiotensin system in human vascular endothelial cells as a novel mechanism of uric acid-induced endothelial dysfunction. J. Hypertens. 28, 1234–1242 (2010).
Sautin, Y. Y., Nakagawa, T., Zharikov, S. & Johnson, R. J. Adverse effects of the classic antioxidant uric acid in adipocytes: NADPH oxidase-mediated oxidative/nitrosative stress. Am. J. Physiol. Cell Physiol. 293, C584–C596 (2007).
Lanaspa, M. A. et al. Uric acid induces hepatic steatosis by generation of mitochondrial oxidative stress: potential role in fructose-dependent and -independent fatty liver. J. Biol. Chem. 287, 40732–40744 (2012).
Roncal-Jimenez, C. A. et al. Sucrose induces fatty liver and pancreatic inflammation in male breeder rats independent of excess energy intake. Metabolism 60, 1259–1270 (2011).
Cirillo, P. et al. Ketohexokinase-dependent metabolism of fructose induces proinflammatory mediators in proximal tubular cells. J. Am. Soc. Nephrol. 20, 545–553 (2009).
Choi, Y. J. et al. Uric acid induces endothelial dysfunction by vascular insulin resistance associated with the impairment of nitric oxide synthesis. FASEB J. 28, 3197–3204 (2014).
Sanchez-Lozada, L. G. et al. Uric acid-induced endothelial dysfunction is associated with mitochondrial alterations and decreased intracellular ATP concentrations. Nephron Exp. Nephrol. 121, e71–e78 (2012).
Martinon, F. Signaling by ROS drives inflammasome activation. Eur. J. Immunol. 40, 616–619 (2010).
Crisan, T. O. et al. Uric acid priming in human monocytes is driven by the AKT-PRAS40 autophagy pathway. Proc. Natl Acad. Sci. USA 114, 5485–5490 (2017).
Alberts, B. M. et al. Secretion of IL-1β from monocytes in gout is redoxindependent. Front. Immunol. 10, 70 (2019).
Kang, D. H., Park, S. K., Lee, I. K. & Johnson, R. J. Uric acid-induced C-reactive protein expression: implication on cell proliferation and nitric oxide production of human vascular cells. J. Am. Soc. Nephrol. 16, 3553–3562 (2005).
Kanellis, J. et al. Uric acid stimulates monocyte chemoattractant protein-1 production in vascular smooth muscle cells via mitogen-activated protein kinase and cyclooxygenase-2. Hypertension 41, 1287–1293 (2003).
Xu, C. et al. Activation of renal (Pro)renin receptor contributes to high fructose-induced salt sensitivity. Hypertension 69, 339–348 (2017).
Kang, D. H. et al. A role for uric acid in the progression of renal disease. J. Am. Soc. Nephrol. 13, 2888–2897 (2002).
Rao, G. N., Corson, M. A. & Berk, B. C. Uric acid stimulates vascular smooth muscle cell proliferation by increasing platelet-derived growth factor A-chain expression. J. Biol. Chem. 266, 8604–8608 (1991).
Braga, T. T. et al. Soluble uric acid activates the NLRP3 inflammasome. Sci. Rep. 7, 39884 (2017).
Netea, M. G., Kullberg, B. J., Blok, W. L., Netea, R. T. & van der Meer, J. W. The role of hyperuricemia in the increased cytokine production after lipopolysaccharide challenge in neutropenic mice. Blood 89, 577–582 (1997).
Jia, L. et al. Hyperuricemia causes pancreatic β-cell death and dysfunction through NF-κB signaling pathway. PLOS ONE 8, e78284 (2013).
Lu, W. et al. Uric acid produces an inflammatory response through activation of NF-κB in the hypothalamus: implications for the pathogenesis of metabolic disorders. Sci. Rep. 5, 12144 (2015).
Crisan, T. O. et al. Soluble uric acid primes TLR-induced proinflammatory cytokine production by human primary cells via inhibition of IL-1Ra. Ann. Rheum. Dis. 75, 755–762 (2015).
Cheng, Z. The FoxO-autophagy axis in health and disease. Trends Endocrinol. Metab. 30, 658–671 (2019).
Wiza, C., Nascimento, E. B. & Ouwens, D. M. Role of PRAS40 in Akt and mTOR signaling in health and disease. Am. J. Physiol. Endocrinol. Metab. 302, E1453–E1460 (2012).
Dunlop, E. A. & Tee, A. R. mTOR and autophagy: a dynamic relationship governed by nutrients and energy. Semin. Cell Dev. Biol. 36, 121–129 (2014).
Saitoh, T. et al. Loss of the autophagy protein Atg16L1 enhances endotoxin-induced IL-1β production. Nature 456, 264–268 (2008).
Crisan, T. O. et al. Inflammasome-independent modulation of cytokine response by autophagy in human cells. PLOS ONE 6, e18666 (2011).
Harris, J. et al. Autophagy controls IL-1β secretion by targeting pro-IL-1β for degradation. J. Biol. Chem. 286, 9587–9597 (2011).
Buffen, K. et al. Autophagy suppresses host adaptive immune responses toward Borrelia burgdorferi. J. Leukoc. Biol. 100, 589–598 (2016).
Garcia, D. & Shaw, R. J. AMPK: mechanisms of cellular energy sensing and restoration of metabolic balance. Mol. Cell 66, 789–800 (2017).
O’Neill, L. A. & Hardie, D. G. Metabolism of inflammation limited by AMPK and pseudo-starvation. Nature 493, 346–355 (2013).
Lanaspa, M. A. et al. Counteracting roles of AMP deaminase and AMP kinase in the development of fatty liver. PLOS ONE 7, e48801 (2012).
Luo, C. et al. High uric acid activates the ROS-AMPK pathway, impairs CD68 expression and inhibits OxLDL-induced foam-cell formation in a human monocytic cell line, THP-1. Cell Physiol. Biochem. 40, 538–548 (2016).
Yuan, H. et al. Metformin ameliorates high uric acid-induced insulin resistance in skeletal muscle cells. Mol. Cell Endocrinol. 443, 138–145 (2017).
Netea, M. G., Quintin, J. & van der Meer, J. W. Trained immunity: a memory for innate host defense. Cell Host Microbe 9, 355–361 (2011).
Saeed, S. et al. Epigenetic programming of monocyte-to-macrophage differentiation and trained innate immunity. Science 345, 1251086 (2014).
Novakovic, B. et al. β-glucan reverses the epigenetic state of LPS-induced immunological tolerance. Cell 167, 1354–1368.e14 (2016).
Blok, B. A., Arts, R. J., van Crevel, R., Benn, C. S. & Netea, M. G. Trained innate immunity as underlying mechanism for the long-term, nonspecific effects of vaccines. J. Leukoc. Biol. 98, 347–356 (2015).
Crisan, T. O., Netea, M. G. & Joosten, L. A. Innate immune memory: implications for host responses to damage-associated molecular patterns. Eur. J. Immunol. 46, 817–828 (2016).
Rajasekar, P., O’Neill, C. L., Eeles, L., Stitt, A. W. & Medina, R. J. Epigenetic changes in endothelial progenitors as a possible cellular basis for glycemic memory in diabetic vascular complications. J. Diabetes Res. 2015, 436879 (2015).
Bekkering, S. et al. Oxidized low-density lipoprotein induces long-term proinflammatory cytokine production and foam cell formation via epigenetic reprogramming of monocytes. Arterioscler. Thromb. Vasc. Biol. 34, 1731–1738 (2014).
Bekkering, S. et al. Treatment with statins does not revert trained immunity in patients with familial hypercholesterolemia. Cell Metab. 30, 1–2 (2019).
Ruggiero, C. et al. Uric acid and inflammatory markers. Eur. Heart J. 27, 1174–1181 (2006).
Grainger, R., McLaughlin, R. J., Harrison, A. A. & Harper, J. L. Hyperuricaemia elevates circulating CCL2 levels and primes monocyte trafficking in subjects with inter-critical gout. Rheumatology 52, 1018–1021 (2013).
Gao, L. et al. Male asymptomatic hyperuricemia patients display a lower number of NKG2D+ NK cells before and after a low-purine diet. Medicine 97, e13668 (2018).
Mylona, E. E. et al. Enhanced interleukin-1β production of PBMCs from patients with gout after stimulation with Toll-like receptor-2 ligands and urate crystals. Arthritis Res. Ther. 14, R158 (2012).
Tanaka, T. et al. A double blind placebo controlled randomized trial of the effect of acute uric acid changes on inflammatory markers in humans: a pilot study. PLOS ONE 12, e0181100 (2017).
Abhishek, A., Valdes, A. M., Zhang, W. & Doherty, M. Association of serum uric acid and disease duration with frequent gout attacks: a case-control study. Arthritis Care Res. 68, 1573–1577 (2016).
Griffith, J. W., Sun, T., McIntosh, M. T. & Bucala, R. Pure hemozoin is inflammatory in vivo and activates the NALP3 inflammasome via release of uric acid. J. Immunol. 183, 5208–5220 (2009).
Orengo, J. M. et al. Uric acid is a mediator of the Plasmodium falciparum-induced inflammatory response. PLOS ONE 4, e5194 (2009).
Shriner, D. et al. Evolutionary context for the association of γ-globin, serum uric acid, and hypertension in African Americans. BMC Med. Genet. 16, 103 (2015).
Spaetgens, B. et al. Risk of infections in patients with gout: a population-based cohort study. Sci. Rep. 7, 1429 (2017).
Bardin, T. & Richette, P. Definition of hyperuricemia and gouty conditions. Curr. Opin. Rheumatol. 26, 186–191 (2014).
Inaba, S., Sautin, Y., Garcia, G. E. & Johnson, R. J. What can asymptomatic hyperuricaemia and systemic inflammation in the absence of gout tell us? Rheumatology 52, 963–965 (2013).
Dalbeth, N. et al. Urate crystal deposition in asymptomatic hyperuricaemia and symptomatic gout: a dual energy CT study. Ann. Rheumat. Dis. 74, 908–911 (2015).
Perez-Ruiz, F., Marimon, E. & Chinchilla, S. P. Hyperuricaemia with deposition: latest evidence and therapeutic approach. Ther. Adv. Musculoskelet. Dis. 7, 225–233 (2015).
Asghar, Z. A. et al. Maternal fructose drives placental uric acid production leading to adverse fetal outcomes. Sci. Rep. 6, 25091 (2016).
Sato, Y. et al. The case for uric acid- lowering treatment in patients with hyperuricaemia and CKD. Nat. Rev. Nephrol. 15, 767–775 (2019).
Acknowledgements
The work by L.A.B.J. and T.O.C. is supported by a Competitiveness Operational Programme grant of the Romanian Ministry of European Funds (P_37_762, MySMIS 103587). The work of P.B. is supported by the National Institute of Health (NIH)/National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), the Diabetic Complications Consortium (DiaComp), the Juvenile Diabetes Research Foundation (JDRF), the Thrasher Research Fund, Center for Women’s Health Research and the International Society for Paediatric and Adolescent Diabetes (ISPAD). The work by R.J.J. is supported by grants from the NIH (NIDDK 1RO1DK109408-01A1 and NIDDK R01 DK108859-01)
Author information
Authors and Affiliations
Contributions
The authors contributed equally to all aspects of the article.
Corresponding authors
Ethics declarations
Competing interests
R.J.J. declares that he is an inventor on several patents and patent applications related to the role of fructose and urate metabolism in hypertension, metabolic syndrome and kidney disease. He also has equity with XORTX therapeutics, which is developing novel xanthine oxidase inhibitors, and Colorado Research Partners LLC, which is developing inhibitors of fructose metabolism. Finally, he has received honoraria from Astra Zeneca, Eli Lilly and Horizon Pharmaceuticals. P.B. declares that he has received consulting fees or speaking honoraria or both from Horizon Pharma, Boehringer Ingelheim, Bayer, and Bristol-Myers Squibb. He also serves on a scientific advisory board for XORTX Therapeutics. L.A.B.J. and T.O.C. declare that they have no competing interests.
Additional information
Peer review information
Nature Reviews Rheumatology thanks P. Richette and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Joosten, L.A.B., Crişan, T.O., Bjornstad, P. et al. Asymptomatic hyperuricaemia: a silent activator of the innate immune system. Nat Rev Rheumatol 16, 75–86 (2020). https://doi.org/10.1038/s41584-019-0334-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41584-019-0334-3
This article is cited by
-
Association between anthropometric indices and hyperuricemia: a nationwide study in China
Clinical Rheumatology (2024)
-
Endovascular Interventional Procedure is a Significant Risk Factor of Postsurgical Gout: A Retrospective Cohort Study
Rheumatology and Therapy (2024)
-
GWAS-identified hyperuricemia-associated IGF1R variant rs6598541 has a limited role in urate mediated inflammation in human mononuclear cells
Scientific Reports (2024)
-
Lactobacillus rhamnosus GG ameliorates hyperuricemia in a novel model
npj Biofilms and Microbiomes (2024)
-
Gegen Qinlian Decoction treatment of asymptomatic hyperuricemia by targeting circadian immune function
Chinese Medicine (2023)