Abstract
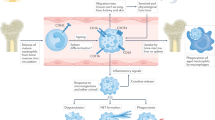
Rheumatic diseases are a collection of disorders defined by the presence of inflammation and destruction of joints and internal organs. A common feature of these diseases is the presence of autoantibodies targeting molecules commonly expressed in neutrophils. These preformed mediators are released by neutrophils but not by other immune cells such as macrophages. Neutrophils, major players in the host innate immune response, initiate a cell death mechanism termed neutrophil extracellular trap (NET) formation as a way to ensnare pathogens. NETs are also a source of released self-molecules found in rheumatic diseases. Subsequently, research on the role of NETs in the onset, progression and resolution of inflammation in rheumatic diseases has intensified. This Review has two aims. First, it aims to highlight the mechanisms required for the generation of NETs, the research landscape of which is rapidly changing. Second, it aims to discuss the role of neutrophils and NETs in systemic lupus erythematosus, vasculitis (specifically anti-neutrophil cytoplasmic autoantibody-associated vasculitis), rheumatoid arthritis and gout. Our goal is to clarify the field of NET research in rheumatic diseases in the hope of improving the therapeutic approaches utilized for these diseases.
Key points
-
Molecules released during neutrophil extracellular trap (NET) formation can often become autoantigens in systemic lupus erythematosus, small vessel vasculitis, rheumatoid arthritis and gout.
-
Damaged tissues and organs in these rheumatic diseases are prone to containing NET-derived material.
-
Neutrophils from patients with some rheumatic diseases spontaneously undergo NETosis in vitro, reflecting the pre-activation of neutrophils during chronic inflammation.
-
To date, whether NET formation is deleterious to progression of all rheumatic diseases is unclear.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Goldblatt, F. & O’Neill, S. G. Clinical aspects of autoimmune rheumatic diseases. Lancet 382, 797–808 (2006).
Diamond, B., Bluestone, J. & Wofsy, D. The immune tolerance network and rheumatic disease: immune tolerance comes to the clinic. Arthritis Rheum. 44, 1730–1735 (2001).
Brinkmann, V. et al. Neutrophil extracellular traps kill bacteria. Science 303, 1532–1535 (2004).
Gupta, S. & Kaplan, M. J. The role of neutrophils and NETosis in autoimmune and renal diseases. Nat. Rev. Nephrol. 12, 402–413 (2016).
Kolaczkowska, E. & Kubes, P. Neutrophil recruitment and function in health and inflammation. Nat. Rev. Immunol. 13, 159–175 (2013).
Borregaard, N. Neutrophils, from marrow to microbes. Immunity 33, 657–670 (2010).
Amulic, B., Cazalet, C., Hayes, G. L., Metzler, K. D. & Zychlinsky, A. Neutrophil function: from mechanisms to disease. Annu. Rev. Immunol. 30, 459–489 (2012).
Tak, T., Tesselaar, K., Pillay, J., Borghans, J. A. M. & Koenderman, L. What’s your age again? Determination of human neutrophil half-lives revisited. J. Leukoc. Biol. 94, 595–601 (2013).
Tecchio, C., Micheletti, A. & Cassatella, M. A. Neutrophil-derived cytokines: facts beyond expression. Front. Immunol. 5, 508 (2014).
Mantovani, A., Cassatella, M. A., Costantini, C. & Jaillon, S. Neutrophils in the activation and regulation of innate and adaptive immunity. Nat. Rev. Immunol. 11, 519–531 (2011).
Kenny, E. F. et al. Diverse stimuli engage different neutrophil extracellular trap pathways. eLife 6, e24437 (2017).
Papayannopoulos, V., Metzler, K. D., Hakkim, A. & Zychlinsky, A. Neutrophil elastase and myeloperoxidase regulate the formation of neutrophil extracellular traps. J. Cell Biol. 191, 677–691 (2010).
Metzler, K. D., Goosmann, C., Lubojemska, A., Zychlinsky, A. & Papayannopoulos, V. A myeloperoxidase-containing complex regulates neutrophil elastase release and actin dynamics during NETosis. Cell Rep. 8, 883–896 (2014).
Amulic, B. et al. Cell-cycle proteins control production of neutrophil extracellular traps. Dev. Cell 43, 449–462 (2017).
Martinod, K. et al. Neutrophil elastase-deficient mice form neutrophil extracellular traps in an experimental model of deep vein thrombosis. J. Thromb. Haemost. 14, 551–558 (2016).
Bruhns, P. Properties of mouse and human IgG receptors and their contribution to disease models. Blood 119, 5640–5649 (2012).
Kaplan, M. J. & Radic, M. Neutrophil extracellular traps: double-edged swords of innate immunity. J. Immunol. 189, 2689–2695 (2012).
Bryan, N. et al. Reactive oxygen species (ROS) — a family of fate deciding molecules pivotal in constructive inflammation and wound healing. Eur. Cell. Mater. 24, 249–265 (2012).
Hirsch, J. G. Bactericidal action of histone. J. Exp. Med. 108, 925–944 (1958).
Lee, J. J. & Pope, J. E. A meta-analysis of the risk of venous thromboembolism in inflammatory rheumatic diseases. Arthritis Res. Ther. 16, 435 (2014).
Rahman, A. & Isenberg, D. A. Systemic lupus erythematosus. N. Engl. J. Med. 358, 929–939 (2008).
Wilhelm, A. J. & Major, A. S. Accelerated atherosclerosis in SLE: mechanisms and prevention approaches. Int. J. Clin. Rheumtol. 7, 527–539 (2012).
Stojan, G. & Petri, M. Atherosclerosis in systemic lupus erythematosus. J. Cardiovasc. Pharmacol. 62, 255–262 (2013).
Anders, H.-J. J. & Vielhauer, V. Renal co-morbidity in patients with rheumatic diseases. Arthritis Res. Ther. 13, 222 (2011).
Hargraves, M. M., Richmond, H. & Morton, R. Presentation of two bone marrow elements; the tart cell and the L. E. cell. Proc. Staff Meet. Mayo Clin. 23, 25–28 (1948).
Carli, L., Tani, C., Vagnani, S., Signorini, V. & Mosca, M. Leukopenia, lymphopenia, and neutropenia in systemic lupus erythematosus: prevalence and clinical impact — a systematic literature review. Semin. Arthritis Rheum. 45, 190–194 (2015).
Hakkim, A. et al. Impairment of neutrophil extracellular trap degradation is associated with lupus nephritis. Proc. Natl Acad. Sci. USA 107, 9813–9818 (2010).
Villanueva, E. et al. Netting neutrophils induce endothelial damage, infiltrate tissues, and expose immunostimulatory molecules in systemic lupus erythematosus. J. Immunol. 187, 538–552 (2011).
Wang, H., Li, T., Chen, S., Gu, Y. & Ye, S. Neutrophil extracellular trap mitochondrial DNA and its autoantibody in systemic lupus erythematosus and a proof-of-concept trial of metformin. Arthritis Rheumatol. 67, 3190–3200 (2015).
Lande, R. et al. Neutrophils activate plasmacytoid dendritic cells by releasing self-DNA-peptide complexes in systemic lupus erythematosus. Sci. Transl. Med. 3, 73ra19 (2011).
Garcia-Romo, G. S. et al. Netting neutrophils are major inducers of type I IFN production in pediatric systemic lupus erythematosus. Sci. Transl. Med. 3, 73ra20 (2011).
Arandjelovic, S. & Ravichandran, K. S. Phagocytosis of apoptotic cells in homeostasis. Nat. Immunol. 16, 907–917 (2015).
Farrera, C. & Fadeel, B. Macrophage clearance of neutrophil extracellular traps is a silent process. J. Immunol. 191, 2647–2656 (2013).
Ren, Y. et al. Increased apoptotic neutrophils and macrophages and impaired macrophage phagocytic clearance of apoptotic neutrophils in systemic lupus erythematosus. Arthritis Rheum. 48, 2888–2897 (2003).
Shao, W.-H. H. & Cohen, P. L. Disturbances of apoptotic cell clearance in systemic lupus erythematosus. Arthritis Res. Ther. 13, 202 (2011).
Midgley, A. & Beresford, M. W. Cellular localization of nuclear antigen during neutrophil apoptosis: mechanism for autoantigen exposure? Lupus 20, 641–646 (2011).
Leffler, J. et al. Neutrophil extracellular traps that are not degraded in systemic lupus erythematosus activate complement exacerbating the disease. J. Immunol. 188, 3522–3531 (2012).
Fang, Y., Xu, C., Fu, Y. X., Holers, V. M. & Molina, H. Expression of complement receptors 1 and 2 on follicular dendritic cells is necessary for the generation of a strong antigen-specific IgG response. J. Immunol. 160, 5273–5279 (1998).
Maletto, B. A. et al. Presence of neutrophil-bearing antigen in lymphoid organs of immune mice. Blood 108, 3094–3102 (2006).
Duffy, D. et al. Neutrophils transport antigen from the dermis to the bone marrow, initiating a source of memory CD8+ T Cells. Immunity 37, 917–929 (2012).
Abi Abdallah, D. S., Egan, C. E., Butcher, B. A. & Denkers, E. Y. Mouse neutrophils are professional antigen-presenting cells programmed to instruct Th1 and Th17 T cell differentiation. Int. Immunol. 23, 317–326 (2011).
Friou, G. J. Clinical application of a test for lupus globulin-nucleohistone interaction using fluorescent antibody. Yale J. Biol. Med. 31, 40–47 (1958).
Fritzler, M. J. & Tan, E. M. Antibodies to histones in drug-induced and idiopathic lupus erythematosus. J. Clin. Invest. 62, 560–567 (1978).
Nässberger, L., Jonsson, H., Sjöholm, A. G., Sturfelt, G. & Heubner, A. Circulating anti-elastase in systemic lupus erythematosus. Lancet 1, 509 (1989).
Spronk, P. E. et al. Antineutrophil cytoplasmic antibodies in systemic lupus erythematosus. Br. J. Rheumatol. 35, 625–631 (1996).
Cervera, R. et al. Anti-chromatin antibodies in systemic lupus erythematosus: a useful marker for lupus nephropathy. Ann. Rheum. Dis. 62, 431–434 (2003).
Carmona-Rivera, C., Zhao, W., Yalavarthi, S. & Kaplan, M. J. Neutrophil extracellular traps induce endothelial dysfunction in systemic lupus erythematosus through the activation of matrix metalloproteinase-2. Ann. Rheum. Dis. 74, 1417–1424 (2015).
Lood, C. et al. Neutrophil extracellular traps enriched in oxidized mitochondrial DNA are interferogenic and contribute to lupus-like disease. Nat. Med. 22, 146–153 (2016).
Hirose, O., Itabashi, M., Takei, T., Honda, K. & Nitta, K. Antineutrophil cytoplasmic antibody-associated glomerulonephritis with immunoglobulin deposition. Clin. Exp. Nephrol. 21, 643–650 (2017).
Skiljevic, D. et al. Serum DNase I activity in systemic lupus erythematosus: correlation with immunoserological markers, the disease activity and organ involvement. Clin. Chem. Lab. Med. 51, 1083–1091 (2013).
Bodaño, A., Amarelo, J., González, A., Gómez-Reino, J. J. & Conde, C. Novel DNASE I mutations related to systemic lupus erythematosus. Arthritis Rheum. 50, 4070–4071 (2004).
Al-Mayouf, S. M. et al. Loss-of-function variant in DNASE1L3 causes a familial form of systemic lupus erythematosus. Nat. Genet. 43, 1186–1188 (2011).
Napirei, M. et al. Features of systemic lupus erythematosus in Dnase1-deficient mice. Nat. Genet. 25, 177–181 (2000).
Sisirak, V. et al. Digestion of chromatin in apoptotic cell microparticles prevents autoimmunity. Cell 166, 88–101 (2016).
Gehrke, N. et al. Oxidative damage of DNA confers resistance to cytosolic nuclease TREX1 degradation and potentiates STING-dependent immune sensing. Immunity 39, 482–495 (2013).
Frost, P. G. & Lachmann, P. J. The relationship of desoxyribonuclease inhibitor levels in human sera to the occurrence of antinuclear antibodies. Clin. Exp. Immunol. 3, 447–455 (1968).
Yeh, T.-M. M., Chang, H.-C. C., Liang, C.-C. C., Wu, J.-J. J. & Liu, M.-F. F. Deoxyribonuclease-inhibitory antibodies in systemic lupus erythematosus. J. Biomed. Sci. 10, 544–551 (2003).
Trofimenko, A. S., Gontar, I. P., Zborovsky, A. B. & Paramonova, O. V. Anti-DNase I antibodies in systemic lupus erythematosus: diagnostic value and share in the enzyme inhibition. Rheumatol. Int. 36, 521–529 (2016).
Hooks, J. J. et al. Immune interferon in the circulation of patients with autoimmune disease. N. Engl. J. Med. 301, 5–8 (1979).
Preble, O. T., Black, R. J., Friedman, R. M., Klippel, J. H. & Vilcek, J. Systemic lupus erythematosus: presence in human serum of an unusual acid-labile leukocyte interferon. Science 216, 429–431 (1982).
Banchereau, J. & Pascual, V. Type I interferon in systemic lupus erythematosus and other autoimmune diseases. Immunity 25, 383–392 (2006).
Crow, M. K. Type I interferon in the pathogenesis of lupus. J. Immunol. 192, 5459–5468 (2014).
Lande, R. et al. Plasmacytoid dendritic cells sense self-DNA coupled with antimicrobial peptide. Nature 449, 564–569 (2007).
Caielli, S. et al. Oxidized mitochondrial nucleoids released by neutrophils drive type I interferon production in human lupus. J. Exp. Med. 213, 697–713 (2016).
Lartigue, A. et al. Role of TLR9 in anti-nucleosome and anti-DNA antibody production in lpr mutation-induced murine lupus. J. Immunol. 177, 1349–1354 (2006).
Nickerson, K. M., Cullen, J. L., Kashgarian, M. & Shlomchik, M. J. Exacerbated autoimmunity in the absence of TLR9 in MRL. Fas(lpr) mice depends on Ifnar1. J. Immunol. 190, 3889–3894 (2013).
Kahlenberg, J. M., Carmona-Rivera, C., Smith, C. K. & Kaplan, M. J. Neutrophil extracellular trap-associated protein activation of the NLRP3 inflammasome is enhanced in lupus macrophages. J. Immunol. 190, 1217–1226 (2013).
Denny, M. F. et al. A distinct subset of proinflammatory neutrophils isolated from patients with systemic lupus erythematosus induces vascular damage and synthesizes type I IFNs. J. Immunol. 184, 3284–3297 (2010).
Hacbarth, E. & Kajdacsy-Balla, A. Low density neutrophils in patients with systemic lupus erythematosus, rheumatoid arthritis, and acute rheumatic fever. Arthritis Rheum. 29, 1334–1342 (1986).
Bennett, L. et al. Interferon and granulopoiesis signatures in systemic lupus erythematosus blood. J. Exp. Med. 197, 711–723 (2003).
Midgley, A. & Beresford, M. W. Increased expression of low density granulocytes in juvenile-onset systemic lupus erythematosus patients correlates with disease activity. Lupus 25, 407–411 (2016).
Macanovic, M. et al. The treatment of systemic lupus erythematosus (SLE) in NZB/W F1 hybrid mice; studies with recombinant murine DNase and with dexamethasone. Clin. Exp. Immunol. 106, 243–252 (1996).
Davis, J. C. et al. Recombinant human Dnase I (rhDNase) in patients with lupus nephritis. Lupus 8, 68–76 (1999).
Winkelstein, J. A. et al. Chronic granulomatous disease. Report on a national registry of 368 patients. Medicine 79, 155–169 (2000).
Campbell, A. M., Kashgarian, M. & Shlomchik, M. J. NADPH oxidase inhibits the pathogenesis of systemic lupus erythematosus. Sci. Transl. Med. 4, 157ra141 (2012).
Jacob, C. O. et al. Haploinsufficiency of NADPH oxidase subunit neutrophil cytosolic factor 2 is sufficient to accelerate full-blown lupus in NZM 2328 mice. Arthritis Rheumatol. 69, 1647–1660 (2017).
Kienhöfer, D. et al. Experimental lupus is aggravated in mouse strains with impaired induction of neutrophil extracellular traps. JCI insight 2, 92920 (2017).
Knight, J. S. et al. Peptidylarginine deiminase inhibition is immunomodulatory and vasculoprotective in murine lupus. J. Clin. Invest. 123, 2981–2993 (2013).
Knight, J. S. et al. Peptidylarginine deiminase inhibition disrupts NET formation and protects against kidney, skin and vascular disease in lupus-prone MRL/lpr mice. Ann. Rheum. Dis. 74, 2199–2206 (2015).
Gordon, R. A. et al. Lupus and proliferative nephritis are PAD4 independent in murine models. JCI insight 2, e92926 (2017).
Elefante, E. et al. One year in review 2017: systemic vasculitis. Clin. Exp. Rheumatol. 35 (Suppl. 1), 5–26 (2017).
Kallenberg, C. G. M., Heeringa, P. & Stegeman, C. A. Mechanisms of disease: pathogenesis and treatment of ANCA-associated vasculitides. Nat. Rev. Rheumatol. 2, 661–670 (2006).
Muñoz-Grajales, C. & Pineda, J. C. Pathophysiological relationship between infections and systemic vasculitis. Autoimmune Dis. 2015, 1–8 (2015).
Jennette, J. C. & Falk, R. J. Small-vessel vasculitis. N. Engl. J. Med. 337, 1512–1523 (1997).
Söderberg, D. & Segelmark, M. Neutrophil extracellular traps in ANCA-Associated vasculitis. Front. Immunol. 7, 256 (2016).
Falk, R. J. & Jennette, J. C. Anti-neutrophil cytoplasmic autoantibodies with specificity for myeloperoxidase in patients with systemic vasculitis and idiopathic necrotizing and crescentic glomerulonephritis. N. Engl. J. Med. 318, 1651–1657 (1988).
Niles, J. L., McCluskey, R. T., Ahmad, M. F. & Arnaout, M. A. Wegener’s granulomatosis autoantigen is a novel neutrophil serine proteinase. Blood 74, 1888–1893 (1989).
Charles, L. A., Caldas, M. L., Falk, R. J., Terrell, R. S. & Jennette, J. C. Antibodies against granule proteins activate neutrophils in vitro. J. Leukoc. Biol. 50, 539–546 (1991).
Brogan, P. & Eleftheriou, D. Vasculitis update: pathogenesis and biomarkers. Pediatr. Nephrol. 33, 187–198 (2017).
Falk, R. J., Terrell, R. S., Charles, L. A. & Jennette, J. C. Anti-neutrophil cytoplasmic autoantibodies induce neutrophils to degranulate and produce oxygen radicals in vitro. Proc. Natl Acad. Sci. USA 87, 4115–4119 (1990).
Kessenbrock, K. et al. Netting neutrophils in autoimmune small-vessel vasculitis. Nat. Med. 15, 623–625 (2009).
Söderberg, D. et al. Increased levels of neutrophil extracellular trap remnants in the circulation of patients with small vessel vasculitis, but an inverse correlation to anti-neutrophil cytoplasmic antibodies during remission. Rheumatology 54, 2085–2094 (2015).
Cheadle, C. et al. Transcription of proteinase 3 and related myelopoiesis genes in peripheral blood mononuclear cells of patients with active Wegener’s granulomatosis. Arthritis Rheum. 62, 1744–1754 (2010).
Lyons, P. A. et al. Novel expression signatures identified by transcriptional analysis of separated leucocyte subsets in systemic lupus erythematosus and vasculitis. Ann. Rheum. Dis. 69, 1208–1213 (2010).
Grayson, P. C. et al. Neutrophil-related gene expression and low-density granulocytes associated with disease activity and response to treatment in antineutrophil cytoplasmic antibody-associated vasculitis. Arthritis Rheumatol. 67, 1922–1932 (2015).
Sangaletti, S. et al. Neutrophil extracellular traps mediate transfer of cytoplasmic neutrophil antigens to myeloid dendritic cells toward ANCA induction and associated autoimmunity. Blood 120, 3007–3018 (2012).
Kumar, S. V. et al. Neutrophil extracellular trap-related extracellular histones cause vascular necrosis in severe GN. J. Am. Soc. Nephrol. 26, 2399–2413 (2015).
Kusunoki, Y. et al. Peptidylarginine deiminase inhibitor suppresses neutrophil extracellular trap formation and MPO-ANCA production. Front. Immunol. 7, 227 (2016).
Jiménez-Alcázar, M. et al. Host DNases prevent vascular occlusion by neutrophil extracellular traps. Science 358, 1202–1206 (2017).
Deane, K. D. Preclinical rheumatoid arthritis (autoantibodies): an updated review. Curr. Rheumatol. Rep. 16, 419 (2014).
Chaudhari, K., Rizvi, S. & Syed, B. A. Rheumatoid arthritis: current and future trends. Nat. Rev. Drug Discov. 15, 305–306 (2016).
Smolen, J. S., Aletaha, D. & McInnes, I. B. Rheumatoid arthritis. Lancet 388, 2023–2038 (2016).
Angelotti, F. et al. One year in review 2017: pathogenesis of rheumatoid arthritis. Clin. Exp. Rheumatol. 35, 368–378 (2017).
Edwards, S. W. & Hallett, M. B. Seeing the wood for the trees: the forgotten role of neutrophils in rheumatoid arthritis. Immunol. Today 18, 320–324 (1997).
Ottonello, L. et al. Delayed neutrophil apoptosis induced by synovial fluid in rheumatoid arthritis: role of cytokines, estrogens, and adenosine. Ann. N. Y Acad. Sci. 966, 226–231 (2002).
Eggleton, P., Wang, L., Penhallow, J., Crawford, N. & Brown, K. A. Differences in oxidative response of subpopulations of neutrophils from healthy subjects and patients with rheumatoid arthritis. Ann. Rheum. Dis. 54, 916–923 (1995).
Corsiero, E., Pratesi, F., Prediletto, E., Bombardieri, M. & Migliorini, P. NETosis as source of autoantigens in rheumatoid arthritis. Front. Immunol. 7, 485 (2016).
Khandpur, R. et al. NETs are a source of citrullinated autoantigens and stimulate inflammatory responses in rheumatoid arthritis. Sci. Transl. Med. 5, 178ra40 (2013).
Wegner, N. et al. Autoimmunity to specific citrullinated proteins gives the first clues to the etiology of rheumatoid arthritis. Immunol. Rev. 233, 34–54 (2010).
Carmona-Rivera, C. et al. Synovial fibroblast-neutrophil interactions promote pathogenic adaptive immunity in rheumatoid arthritis. Sci. Immunol. 2, eaag3358 (2017).
Wright, H. L., Makki, F. A., Moots, R. J. & Edwards, S. W. Low-density granulocytes: functionally distinct, immature neutrophils in rheumatoid arthritis with altered properties and defective TNF signalling. J. Leukoc. Biol. 101, 599–611 (2017).
Kouskoff, V. et al. Organ-specific disease provoked by systemic autoimmunity. Cell 87, 811–822 (1996).
Korganow, A. S. et al. From systemic T cell self-reactivity to organ-specific autoimmune disease via immunoglobulins. Immunity 10, 451–461 (1999).
Ji, H. et al. Genetic influences on the end-stage effector phase of arthritis. J. Exp. Med. 194, 321–330 (2001).
Wipke, B. T. & Allen, P. M. Essential role of neutrophils in the initiation and progression of a murine model of rheumatoid arthritis. J. Immunol. 167, 1601–1608 (2001).
Christensen, A. D., Haase, C., Cook, A. D. & Hamilton, J. A. K/BxN serum-transfer arthritis as a model for human inflammatory arthritis. Front. Immunol. 7, 213 (2016).
Karsunky, H. et al. Inflammatory reactions and severe neutropenia in mice lacking the transcriptional repressor Gfi1. Nat. Genet. 30, 295–300 (2002).
Monach, P. A. et al. Neutrophils in a mouse model of autoantibody-mediated arthritis: critical producers of Fc receptor gamma, the receptor for C5a, and lymphocyte function-associated antigen 1. Arthritis Rheum. 62, 753–764 (2010).
Maicas, N. et al. Deficiency of Nrf2 accelerates the effector phase of arthritis and aggravates joint disease. Antioxid. Redox Signal. 15, 889–901 (2011).
Rohrbach, A. S., Hemmers, S., Arandjelovic, S., Corr, M. & Mowen, K. A. PAD4 is not essential for disease in the K/BxN murine autoantibody-mediated model of arthritis. Arthritis Res. Ther. 14, R104 (2012).
Owlia, M. B., Newman, K. & Akhtari, M. Felty’s syndrome, insights and updates. Open Rheumatol. J. 8, 129–136 (2014).
Dwivedi, N. & Radic, M. Citrullination of autoantigens implicates NETosis in the induction of autoimmunity. Ann. Rheum. Dis. 73, 483–491 (2014).
Nuki, G. & Simkin, P. A. A concise history of gout and hyperuricemia and their treatment. Arthritis Res. Ther. 8, S1 (2006).
Malawista, S. E., de Boisfleury, A. C. & Naccache, P. H. Inflammatory gout: observations over a half-century. FASEB J. 25, 4073–4078 (2011).
Kuo, C.-F., Grainge, M. J., Mallen, C., Zhang, W. & Doherty, M. Comorbidities in patients with gout prior to and following diagnosis: case-control study. Ann. Rheum. Dis. 75, 210–217 (2014).
Kuo, C.-F., Grainge, M. J., Zhang, W. & Doherty, M. Global epidemiology of gout: prevalence, incidence and risk factors. Nat. Rev. Rheumatol. 11, 649–662 (2015).
Rada, B. Neutrophil extracellular traps and microcrystals. J. Immunol. Res. 2017, 1–7 (2017).
Amaral, F. A. A. et al. NLRP3 inflammasome-mediated neutrophil recruitment and hypernociception depend on leukotriene B(4) in a murine model of gout. Arthritis Rheum. 64, 474–484 (2012).
Mitroulis, I., Kambas, K. & Ritis, K. Neutrophils, IL-1β, and gout: is there a link? Semin. Immunopathol. 35, 501–512 (2013).
Martinon, F., Pétrilli, V., Mayor, A., Tardivel, A. & Nature, T.-J. Gout-associated uric acid crystals activate the NALP3 inflammasome. Nature 440, 237–241 (2006).
Ryckman, C. et al. Role of S100A8 and S100A9 in neutrophil recruitment in response to monosodium urate monohydrate crystals in the air-pouch model of acute gouty arthritis. Arthritis Rheum. 48, 2310–2320 (2003).
Popa-Nita, O. & Naccache, P. H. Crystal-induced neutrophil activation. Immunol. Cell Biol. 88, 32–40 (2010).
Mitroulis, I. et al. Neutrophil extracellular trap formation is associated with IL-1β and autophagy-related signaling in gout. PLoS ONE 6, e29318 (2011).
Schauer, C. et al. Aggregated neutrophil extracellular traps limit inflammation by degrading cytokines and chemokines. Nat. Med. 20, 511–517 (2014).
Chatfield, S. M. et al. Monosodium urate crystals generate nuclease-resistant neutrophil extracellular traps via a distinct molecular pathway. J. Immunol. 200, 1802–1816 (2018).
Chhana, A. & Dalbeth, N. The gouty tophus: a review. Curr. Rheumatol. Rep. 17, 19 (2015).
Reber, L. L., Gaudenzio, N., Starkl, P. & Galli, S. J. Neutrophils are not required for resolution of acute gouty arthritis in mice. Nat. Med. 22, 1382–1384 (2016).
Clain, J. M., Cartin-Ceba, R., Fervenza, F. C. & Specks, U. Experience with rituximab in the treatment of antineutrophil cytoplasmic antibody associated vasculitis. Ther. Adv. Musculoskelet. Dis. 6, 58–74 (2013).
Mok, C. C. Current role of rituximab in systemic lupus erythematosus. Int. J. Rheum. Dis. 18, 154–163 (2015).
Flossmann, O. et al. Long-term patient survival in ANCA-associated vasculitis. Ann. Rheum. Dis. 70, 488–494 (2011).
Ragab, G., Elshahaly, M. & Bardin, T. Gout: an old disease in new perspective – a review. J. Adv. Res. 8, 495–511 (2017).
Willis, V. C. et al. N-Α-benzoyl-N5-(2-chloro-1-iminoethyl)-L-ornithine amide, a protein arginine deiminase inhibitor, reduces the severity of murine collagen-induced arthritis. J. Immunol. 186, 4396–4404 (2011).
McDonald, B., Urrutia, R., Yipp, B. G., Jenne, C. N. & Kubes, P. Intravascular neutrophil extracellular traps capture bacteria from the bloodstream during sepsis. Cell Host Microbe 12, 324–333 (2012).
Kolaczkowska, E. et al. Molecular mechanisms of NET formation and degradation revealed by intravital imaging in the liver vasculature. Nat. Commun. 6, 6673 (2015).
Brinkmann, V., Abu Abed, U., Goosmann, C. & Zychlinsky, A. Immunodetection of NETs in paraffin-embedded tissue. Front. Immunol. 7, 513 (2016).
Papayannopoulos, V., Staab, D. & Zychlinsky, A. Neutrophil elastase enhances sputum solubilization in cystic fibrosis patients receiving DNase therapy. PLoS ONE 6, e28526 (2011).
Caudrillier, A. et al. Platelets induce neutrophil extracellular traps in transfusion-related acute lung injury. J. Clin. Invest. 122, 2661–2671 (2012).
Reviewer information
Nature Reviews Rheumatology thanks M. Herrmann, M. Radic and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
All authors contributed to substantial discussion of content, researching data, writing and reviewing and/or editing the manuscript before submission.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Apel, F., Zychlinsky, A. & Kenny, E.F. The role of neutrophil extracellular traps in rheumatic diseases. Nat Rev Rheumatol 14, 467–475 (2018). https://doi.org/10.1038/s41584-018-0039-z
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41584-018-0039-z
This article is cited by
-
Cayratia albifolia C.L.Li exerts anti-rheumatoid arthritis effect by inhibiting macrophage activation and neutrophil extracellular traps (NETs)
Chinese Medicine (2024)
-
Clinical features and prognosis of ANCA-associated vasculitis patients who were double-seropositive for myeloperoxidase-ANCA and proteinase 3-ANCA
Clinical and Experimental Medicine (2024)
-
Neutrophilic Activity Biomarkers (Plasma Neutrophil Extracellular Traps and Calprotectin) in Established Patients with Rheumatoid Arthritis Receiving Biological or JAK Inhibitors: A Clinical and Ultrasonographic Study
Rheumatology and Therapy (2024)
-
Ozone alleviates MSU-induced acute gout pain via upregulating AMPK/GAS6/MerTK/SOCS3 signaling pathway
Journal of Translational Medicine (2023)
-
Neutrophil extracellular trap-induced intermediate monocytes trigger macrophage activation syndrome in adult-onset Still’s disease
BMC Medicine (2023)