Abstract
The opioid crisis constitutes a public health challenge at the intersection of two interrelated medical problems — opioid addiction and chronic pain. Overlap of the reward and pain circuits in the brain underlies the frequent comorbidity of chronic pain and opioid addiction, whereas inadequate support, treatment and health-care reimbursement for both of these conditions are major contributors underlying the magnitude of the problem. Neurologists are uniquely positioned to help address the opioid crisis, not only through their involvement in the management of chronic pain conditions but also because they can screen for and manage opioid use disorders. The new NIH Helping to End Addiction Long-term (HEAL) Initiative will support research into pain and opioid use disorders to help address the opioid crisis. Neurologists’ involvement in basic, translational and clinical research is needed for the development of new pain therapeutics and biomarkers and interventions to prevent chronic pain and to prevent and treat opioid addiction.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
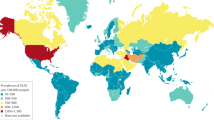
Dahlhamer, J. et al. Prevalence of chronic pain and high-impact chronic pain among adults — United States, 2016. MMWR Morb. Mortal. Wkly Rep. 67, 1001–1006 (2018).
Shupler, M. S., Kramer, J. K., Cragg, J. J., Jutzeler, C. R. & Whitehurst, D. G. T. Pan-Canadian estimates of chronic pain prevalence from 2000 to 2014: a repeated cross-sectional survey analysis. J. Pain. https://doi.org/10.1016/j.jpain.2018.10.010 (2018).
Breivik, H., Collett, B., Ventafridda, V., Cohen, R. & Gallacher, D. Survey of chronic pain in Europe: prevalence, impact on daily life, and treatment. Eur. J. Pain 10, 287–333 (2006).
Jackson, T. et al. A systematic review and meta-analysis of the global burden of chronic pain without clear etiology in low- and middle-income countries: trends in heterogeneous data and a proposal for new assessment methods. Anesth. Analg. 123, 739–748 (2016).
Shipton, E. A., Shipton, E. E. & Shipton, A. J. A. Review of the opioid epidemic: what do we do about it? Pain Ther. 7, 23–36 (2018).
Clark, D. J. & Schumacher, M. A. America’s opioid epidemic: supply and demand considerations. Anesth. Analg. 125, 1667–1674 (2017).
Lamvu, G., Feranec, J. & Blanton, E. Perioperative pain management: an update for obstetrician-gynecologists. Am. J. Obstet. Gynecol. 218, 193–199 (2018).
Barratt, M. J., Latimer, J., Jauncey, M., Tay, E. & Nielsen, S. Urine drug screening for early detection of unwitting use of fentanyl and its analogues among people who inject heroin in Sydney, Australia. Drug Alcohol Rev. 37, 847–850 (2018).
Pergolizzi, J. V. Jr., LeQuang, J. A., Berger, G. K. & Raffa, R. B. The basic pharmacology of opioids informs the opioid discourse about misuse and abuse: a review. Pain Ther. 6, 1–16 (2017).
Chou, R. et al. The effectiveness and risks of long-term opioid treatment of chronic pain. Evid. Rep. Technol. Assess (Full Rep.). https://doi.org/10.23970/AHRQEPCERTA218 (2014).
Yi, P. & Pryzbylkowski, P. Opioid induced hyperalgesia. Pain Med. 16 (Suppl. 1), S32–S36 (2015).
Volkow, N. D. & McLellan, A. T. Mitigation strategies for opioid abuse. N. Engl. J. Med. 375, 96 (2016).
Jonnes, J. The rise of the modern addict. Am. J. Publ. Health 85, 1157–1162 (1995).
Kandall, S. R. Women and drug addiction: a historical perspective. J. Addict. Dis. 29, 117–126 (2010).
Van Zee, A. The promotion and marketing of oxycontin: commercial triumph, public health tragedy. Am. J. Publ. Health 99, 221–227 (2009).
Fauber, J. Painkiller boom fueled by networking: doctors, researchers with financial ties to drug makers set stage for surge in prescriptions. archive.jsonline http://archive.jsonline.com/watchdog/watchdogreports/painkiller-boom-fueled-by-networking-dp3p2rn-139609053.html (2012).
Government Accounting Office. Prescription drugs: OxyContin abuse and diversion and efforts to address the problem. govinfo https://www.govinfo.gov/app/details/GAOREPORTS-GAO-04-110 (2004).
Mezei, L. & Murinson, B. B., Johns Hopkins Pain Curriculum Development Team. Pain education in North American medical schools. J. Pain 12, 1199–1208 (2011).
Yanni, L. M. et al. Preparation, confidence, and attitudes about chronic noncancer pain in graduate medical education. J. Grad. Med. Educ. 2, 260–268 (2010).
Guy, G. P. Jr et al. Vital signs: changes in opioid prescribing in the United States, 2006–2015. MMWR Morb. Mortal. Wkly Rep. 66, 697–704 (2017).
Centers for Disease Control and Prevention. Synthetic opioid overdose data. CDC https://www.cdc.gov/drugoverdose/data/fentanyl.html (updated 19 Dec 2018).
National Institutes of Health Interagency Pain Research Coordinating Committee. National pain strategy: a comprehensive population health-level strategy for pain. NIH https://iprcc.nih.gov/sites/default/files/HHSNational_Pain_Strategy_508C.pdf (2017).
International Narcotics Control Board. Narcotic drugs. Report 2016: estimated world requirements for 2017 - statistics for 2015. INCB https://www.incb.org/incb/en/narcotic-drugs/Technical_Reports/2016/narcotic-drugs-technical-report-2016.html (2016).
Fischer, B. & Rehm, J. Revisiting the ‘paradigm shift’ in opioid use: developments and implications 10 years later. Drug Alcohol Rev. 37 (Suppl. 1), S199–S202 (2018).
Volkow, N., Benveniste, H. & McLellan, A. T. Use and misuse of opioids in chronic pain. Annu. Rev. Med. 69, 451–465 (2018).
Krebs, E. E. et al. Effect of opioid versus nonopioid medications on pain-related function in patients with chronic back pain or hip or knee osteoarthritis pain: the SPACE randomized clinical trial. JAMA 319, 872–882 (2018).
Potter, J. S. et al. The multi-site prescription opioid addiction treatment study: 18-month outcomes. J. Subst. Abuse Treat. 48, 62–69 (2015).
Weiss, R. D. et al. Long-term outcomes from the National Drug Abuse Treatment Clinical Trials Network prescription opioid addiction treatment study. Drug Alcohol Depend. 150, 112–119 (2015).
Dugosh, K. et al. A systematic review on the use of psychosocial interventions in conjunction with medications for the treatment of opioid addiction. J. Addict. Med. 10, 93–103 (2016).
National Institutes of Health National Institute on Drug Abuse. Principles of drug addiction treatment: a research-based guide (third edition). drugabuse https://www.drugabuse.gov/publications/principles-drug-addiction-treatment-research-based-guide-third-edition/preface (2018).
Department of Health and Human Services: Substance Abuse and Mental Health Services Administration. Treatment episode data set (TEDS) 2005–2015. National admissions to substance abuse treatment services. SAMHSA https://wwwdasis.samhsa.gov/dasis2/teds_pubs/2015_teds_rpt_natl.pdf (2017).
Thomas, C. P. et al. Medication-assisted treatment with buprenorphine: assessing the evidence. Psychiatr. Serv. 65, 158–170 (2014).
Brooklyn, J. R. & Sigmon, S. C. Vermont Hub-and-Spoke model of care for opioid use disorder: development, implementation, and impact. J. Addict. Med. 11, 286–292 (2017).
Wang, H. et al. Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 388, 1459–1544 (2016).
Institute of Medicine (US) Committee on Advancing Pain Research, Care, and Education. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research (National Academies Press (US), 2011).
Blackwell, D. L., Lucas, J. W. & Clarke, T. C. Summary Health Statistics for U.S. Adults: National Health Interview Survey, 2012. Vital and Health Statistics: Series 10, Number 260 (Centers for Disease Control and Prevention, 2014).
Blondell, R. D. et al. A clinical trial comparing tapering doses of buprenorphine with steady doses for chronic pain and co-existent opioid addiction. J. Addict. Med. 4, 140–146 (2010).
Neumann, A. M. et al. A preliminary study comparing methadone and buprenorphine in patients with chronic pain and coexistent opioid addiction. J. Addict. Dis. 32, 68–78 (2013).
Tsui, J. I., Herman, D. S., Kettavong, M., Anderson, B. J. & Stein, M. D. Escitalopram is associated with reductions in pain severity and pain interference in opioid dependent patients with depressive symptoms. Pain 152, 2640–2644 (2011).
Koroschetz, W. The NIH HEAL initiative and pain research. NIH https://www.ninds.nih.gov/News-Events/Directors-Messages/All-Directors-Messages/NIH-HEAL-Initiative-and-Pain-Research (updated 28 Aug 2018).
National Institutes of Health. Brain Initiative https://www.braininitiative.nih.gov/ (2019).
National Institutes of Health. Stimulating Peripheral Activity to Relieve Conditions (SPARC) https://commonfund.nih.gov/sparc (updated 15 Jan 2019).
Acknowledgements
The authors thank R. Baler and J. Ward for their valuable editorial help with the manuscript.
Reviewer information
Nature Reviews Neurology thanks G. Fischer and other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
Both authors contributed equally to all aspects of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Volkow, N.D., Koroshetz, W.J. The role of neurologists in tackling the opioid epidemic. Nat Rev Neurol 15, 301–305 (2019). https://doi.org/10.1038/s41582-019-0146-8
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41582-019-0146-8