Abstract
Chimeric antigen receptors (CARs) have shown remarkable ability to re-direct T cells to target CD19-expressing tumours, resulting in remission rates of up to 90% in individuals with paediatric acute lymphoblastic lymphoma. Lessons learned from these clinical trials of adoptive T cell therapy for cancer, as well as investments made in manufacturing T cells at commercial scale, have inspired researchers to develop CARs for additional applications. Here, we explore the challenges and opportunities of using this technology to target infectious diseases such as with HIV and undesired immune responses such as autoimmunity and transplant rejection. Despite substantial obstacles, the potential of CAR T cells to enable cures for a wide array of disease settings could be transformational for the medical field.
Similar content being viewed by others
Introduction
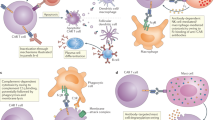
Two broad categories of T cells work together to ensure specific and long-term immunity against pathogens and tumours while protecting the body from aberrant responses against self. The first subset comprises effector T cells, which eliminate pathogens and tumours; regulatory T (Treg) cells make up the second subset and function to prevent an immune response against self. Although effector T cell responses are generally potent, some infectious organisms and tumours have evolved a large variety of escape mechanisms to bypass T cell control1. Similarly, the incidence of autoimmune diseases, such as type 1 diabetes, highlights that Treg cells are not always successful in preventing aberrant immune responses. Moreover, in organ transplantation, Treg cells often fail to protect life-saving tissues from immune rejection.
Chimeric antigen receptor (CAR) technology has emerged as a promising approach to reprogramme T cells to overcome the barriers that confront naturally occurring T cells. Because CARs alter how T cells recognize antigen by directly binding to cell surface proteins without requiring peptide presentation by MHC molecules, there are fewer available targets for CARs to recognize relative to T cell receptors (TCRs). However, CAR targeting has more specificity and no HLA restriction, and it avoids many of the T cell escape mechanisms that are used by infectious agents and tumours, which are no longer effective against CAR T cells. Although clinical success is somewhat new to the CAR T cell field, the concept first emerged in the 1990s when investigators showed that T cell specificity could be redirected by fusing a targeting moiety that recognizes a cell surface protein with a T cell activation domain such as the CD3ζ cytoplasmic tail. The first example of this technology fused CD4 to the CD3ζ chain (CD4ζCAR). When expressed in effector T cells, this construct redirected T cell specificity to HIV-infected cells by taking advantage of the interaction between HIV envelope protein (Env) and CD4 (ref.2). This concept was brought to the clinic in the late 1990s; although it was shown to be safe and feasible, durable control of virus infection was not observed3,4,5,6. In the intervening years, our understanding of how to engineer potent effector CAR T cells to target tumours has flourished7,8,9. In addition, pharmaceutical companies have promoted the transition of effector CAR T cell therapy from a boutique phase I single-centre clinical trial to a Food and Drug Administration (FDA)-approved therapy that can be used to treat thousands of patients across the United States and elsewhere10.
As T cells have pivotal roles in controlling infectious disease and autoimmunity, many in the field are considering how CAR T cell therapy could provide long-term solutions to diseases outside of cancer in which traditional medical approaches have not provided a cure. We focus our discussion on both the progress and the remaining challenges of making CAR T cell therapy a reality for individuals suffering from chronic infectious disease (with HIV), autoimmune disease and transplant rejection. Given the abundance of T cell subsets and their high levels of heterogeneity11, we refer to broad groups of T cell populations without delving into the possible advantages or disadvantages of more nuanced T cell subsets. Moreover, we concentrate on the issues that are unique to treating HIV infection with effector CAR T cells and the challenges facing the field before engineered CAR Treg cells can be safely infused into patients. Without doubt, advances in these two areas will also fuel new ideas about how to enhance CAR T cell function in cancer and beyond.
CAR T cells for the clearance of HIV
Although HIV infection induces robust antiviral immunity, the immune system fails to clear all of the HIV-infected cells. In part, this is because a small fraction of infected cells avoids immunosurveillance by expressing low to no amounts of viral antigen. These latently infected cells (often referred to as the HIV reservoir) can remain dormant for many years only to sporadically start producing infectious virus, which necessitates lifelong antiviral therapy. It is clear from several studies that although early initiation of combination antiretroviral therapy (cART) reduces the size of the HIV reservoir, it does not eliminate its formation, as HIV can still emerge after years of undetectable viraemia12,13. In addition, other factors — such as virus escape, HIV-specific T cell dysfunction and/or exhaustion and the physical segregation between immune effectors and infected cells — contribute to the inability of endogenous immune responses to eradicate infection14.
Together, these factors indicate that successful HIV cure strategies will require potent and persistent cellular immune surveillance that remains poised to suppress virus re-emergence for perhaps decades. The adoptive transfer of effector T cells genetically modified with a CAR may transcend the limitations of virus-specific cytotoxic T lymphocytes (CTLs) that develop during natural infection to control disease and prevent latency reactivation from becoming a clinically important event. The advantages of CAR T cells compared with naturally occurring HIV-specific CTLs are summarized in Table 1.
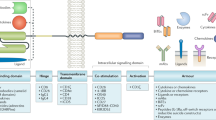
As noted above, between 1995 and 2005, several clinical trials investigated the safety and efficacy of using CD4ζCAR T cells in HIV-infected individuals. The outcomes of these studies reinforced the safety and feasibility of ex vivo adoptive T cell gene therapy, but ultimately treatment failed to durably reduce the viral burden within blood and tissue reservoirs4,5,6. These findings raised concerns about the ability of first-generation CAR T cells, which contain only the CD3ζ signalling domain, to function in vivo. Following these initial clinical trials, the cancer immunotherapy field has advanced the design and manufacturing of effector CAR T cells to generate optimal antitumour responses15,16. A key improvement in design from first-generation to second-generation CARs has been the inclusion of co-stimulatory signalling domains, such as those from 4-1BB (also known as TNFRSF9) and CD28, that modulate T cell function, persistence and susceptibility to exhaustion17,18. Co-stimulatory domains can also influence memory development and metabolism of CAR T cells. For example, signalling from a CAR containing a 4-1BB domain promotes a central memory phenotype in T cells and reliance on oxidative phosphorylation for energy, whereas signalling from a CAR containing a CD28 domain promotes an effector memory phenotype in T cells and an augmented rate of glycolysis19,20. These findings help to reconcile the differential persistence of CAR T cells that has been observed in vivo, whereby different types of co-stimulation can reprogramme T cell metabolism to generate long-lived memory cells or short-term effector cells.
Recently, we re-engineered the CD4ζCAR used in the original clinical trials by altering the vector backbone, the promoter and the structural and signalling domains. Optimized CD4-based CAR T cells containing the 4-1BB–CD3ζ signalling domain (Fig. 1a) were at least 50-fold more potent at suppressing HIV replication in vitro than were T cells expressing the original CD4ζCAR. Moreover, when the optimized CAR T cells were evaluated in a humanized mouse model of HIV infection, they preserved the CD4+ T cell count, reduced the HIV burden and expanded in response to HIV to a much greater extent than did first-generation CD4ζCAR T cells21.
Extracellular antigen recognition domains of chimeric antigen receptors (CARs) determine their specificity for HIV-1 by targeting different regions of the HIV envelope protein (Env). a | The full-length extracellular domain of CD4 comprises four domains (D1–D4). D1 and D2 are crucial for binding to the glycoprotein 120 (gp120) component of the HIV Env trimer. b | CARs containing broadly neutralizing antibody (bNAb)-derived single-chain variable fragments (scFvs) have been produced from antibodies such as VRCO1 and PG9, which differentially bind the Env trimer at the CD4-binding site and second variable (V2) loop, respectively. c,d | Bispecific CARs confer dual specificity for HIV through the CD4–gp120 interaction and either binding of the scFv to an alternative region in Env or binding of the carbohydrate recognition domain (CRD) of a C-type lectin to glycan motifs on Env. VH, variable heavy chain; VL, variable light chain.
Several groups have explored targeting HIV-infected cells using second-generation CARs with alternative antigen-binding moieties. CARs containing single-chain variable fragments (scFvs) derived from broadly neutralizing antibodies (bNAbs) have been developed that target conserved sites within the Env protein, including the CD4-binding site, the glycoprotein 41 (gp41) membrane-proximal external region and variable region glycans21,22,23 (Fig. 1b). Despite the antiviral capacity of scFv-based CAR T cells in vitro, several factors may limit their therapeutic potential in humans. To become a broadly applicable therapy, scFv-based CAR T cells must overcome HIV escape, be effective against the diversity of HIV strains and be non-immunogenic so that they can persist for decades.
Furthermore, bispecific CARs were recently developed that fuse a CD4 segment to either a bNAb-based scFv24 (Fig. 1c) or the carbohydrate recognition domain (CRD) of a human C-type lectin25 (Fig. 1d). These bispecific CARs have dual specificity for HIV through binding of the CD4 fragment to the gp120 subunit of Env and, in the case of the CRD, binding to conserved glycans on Env. However, C-type lectins can bind endogenous cell components such as normal cell-associated glycans26,27, which raises the possibility of on-target, off-tissue reactivity. Despite the advantages and potential drawbacks of each type of antigen-targeting moiety, it is clearly possible that highly potent HIV-specific T cells can be generated by improving CAR design. This will likely impact the durability and function of CAR T cells in HIV-infected individuals going forward into clinical trials.
Enhancing CAR T cell persistence in vivo
CAR T cells that target CD19-expressing cells (CD19CAR T cells) can induce long-term remission in some patients with specific B cell malignancies28,29. Importantly, the durability of remission has been shown to correlate with the maintenance of functional CAR T cells30. Several studies showed that total CD19 antigen burden in patients (from both malignant and nonmalignant cells) is a crucial factor driving the proliferation and persistence of CAR T cells in vivo. For example, individuals with a high level of CD19+ cells in the bone marrow before CAR T cell therapy had a greater magnitude of CAR T cell persistence post-remission, which correlated with a reduced risk of CD19+ disease relapse31,32,33. This suggests that a high antigen load upon CAR T cell infusion is required to achieve durable remission.
HIV infection poses a unique challenge because the quantity of virus-infected cells in cART-treated individuals is substantially less than the number of cancer cells in patients with leukaemia. As a result, strategies such as therapeutic immunization and/or multiple infusions of HIV-specific CAR T cells should be implemented to augment the persistence of CAR T cells after infusion. This will be essential to ensure that a sufficient number of CAR T cells are ready to respond to HIV rebound after treatment interruption and to maintain a persistent CAR T cell population that is poised to react when virus reappears from latently infected cells.
Therapeutic immunization
The immunological memory generated by traditional vaccines mediates resistance to infection upon re-exposure. Often, booster immunizations are administered subsequently to maintain a sufficiently large population of antigen-specific memory cells34. The same rationale for vaccination against infection is actively being applied to CAR T cell therapy. For example, investigators have manufactured dual-specific T cells by transducing the CD19CAR into T cells specific for Epstein–Barr virus, adenovirus or cytomegalovirus (CMV)35,36,37. In this manner, vaccines expressing viral epitopes that are targeted by these T cells can be administered to reinvigorate CAR T cells through endogenous TCR signalling.
As a proof of concept, tumour-bearing mice were infused with CD19CAR-transduced, CMV-specific T cells and then vaccinated with CMV pp65 peptide alone or with peptide-loaded antigen-presenting T cells (T-APCs). Both vaccination regimens elicited robust CAR T cell proliferation and augmented antitumour activity in vivo35. Similar approaches are being applied in clinical trials using the CD19CAR38,39,40. However, repetitive TCR stimulation of virus-specific memory T cells induces terminal T cell differentiation and reduces their replicative capacity34. Thus, optimum re-stimulation may be achieved in vivo by directly stimulating through the CAR and by using less-differentiated T cells as source material. To this end, a pilot study is in progress to evaluate episodic administration of CD19+ T-APCs, which are designed to increase the number of CD19CAR T cells after remission and hopefully reduce the incidence of disease relapse32,41.
The HIV research community has developed numerous prophylactic vaccines that could be adapted for use in non-human primates or humanized mice to evaluate their impact on CAR T cell persistence in vivo42. Ultimately, CAR T cells for HIV cure will need to persist in environments with low antigen burden, and it is hoped that existing vaccination strategies or candidates in preclinical evaluation can be used to augment the long-term survival of functional CAR T cells.
CAR T cell resistance to HIV
The ability of CAR T cells to mediate a functional HIV cure is likely to depend on T cell persistence following adoptive transfer. However, the persistence of CAR T cells will be limited if they become infected; thus, protecting these engineered T cells from infection will be crucial. Preventing viral entry is the most effective strategy for engineering HIV-resistant CAR T cells43. This approach blocks virus propagation and, importantly, precludes integration of the virus into the host genome, where it could persist in a latent state. Several ex vivo gene-editing strategies have been clinically investigated to abrogate HIV entry, including targeted disruption of the gene encoding the HIV co-receptor CC-chemokine receptor 5 (CCR5) using zinc-finger nucleases44,45. Recently, new gene-editing strategies have been developed that enable high rates of homology-directed repair (HDR) of gene cassettes into specific genomic loci46,47,48. One study simultaneously disrupted CCR5 using a site-directed megaTAL nuclease and drove HDR using an adeno-associated virus donor template encoding an scFv-based CAR23. This method produced functional HIV-specific CAR T cells lacking CCR5 expression that suppressed virus replication in vitro to a greater extent than did CAR T cells generated by lentiviral transduction that were not protected from infection. Furthermore, concurrent CCR5 disruption and targeted CAR integration by HDR offer several advantages. For example, the efficiency of CCR5 disruption using good manufacturing practice (GMP)-compatible approaches is modest45,49, so by encouraging CAR integration into CCR5, the number of CAR T cells that are also CCR5 deficient increases. Also, although there have not been any reported oncogenic insertional events caused by lentivirus integration into the genome of T cells, HDR potentially adds another degree of safety owing to its targeted integration of gene cassettes into the genome23.
Despite the potential advantages of HDR, this technology is fairly new, and it remains unclear so far whether safe and sufficient editing of T cells can be achieved at the clinical scale. As an alternative method, other groups have incorporated protection from HIV infection into T cells by either co-transduction or the integration of resistance genes into the lentiviral vector containing the HIV-specific CAR. For example, constructs have co-expressed sequence variations of the gp41 heptad repeat 2 domain, which inhibits HIV fusion at the virological synapse, or small hairpin RNA (shRNA) molecules targeting CCR5 and the HIV long terminal repeat (LTR) sequence50,51,52,53. CCR5-targeting shRNAs downregulate expression of CCR5 by CAR T cells to prevent virus entry, and, as a secondary measure, the LTR-targeting shRNAs mediate HIV RNA degradation, thus blunting a productive infection within CAR T cells.
It is important to note that most of these HIV resistance strategies were initially developed to protect CD4+ T cells from viral infection43. HIV-specific CAR T cells may prove to be a more difficult population to protect owing to the ability of the CAR construct to bind and concentrate HIV on the T cell surface. In addition, many CAR T cells have a persistent, low level of activation owing to tonic signalling through the CAR17,21,54. Given that T cell activation influences the rate of HIV infection55,56,57,58,59, basal activation of CAR T cells may inadvertently increase their susceptibility to infection. Moreover, as new HIV resistance strategies are being developed, it is uncertain how additional T cell engineering will affect the fitness of CAR T cells in vivo and what sacrifice in antiviral function might be incurred to achieve resistance to virus infection.
HSPC-derived CAR T cells
Haematopoietic stem and/or progenitor cell (HSPC)-based gene therapy may overcome the limited persistence of peripheral T cell-based products in environments with a low antigen burden. HSPCs have the inherent ability to self-renew, proliferate and produce mature, multilineage immune cells that egress into the blood and tissues60. As a result, HSPCs modified with an HIV-specific TCR or CAR could provide long-term production and maintenance of HIV-specific T cells and other immune effectors61,62. To evaluate this approach, immunodeficient mice were engrafted with first-generation CD4ζCAR-modified HSPCs, and human immune cell reconstitution was shown to occur63. After HIV challenge, CD4ζCAR T cells retained effector function, proliferated and suppressed virus replication to a greater extent than did T cells from control mice64. Interestingly, CAR-modified HSPCs underwent altered T cell development by suppressing endogenous TCR recombination. Although the implication of this finding remains unclear, the use of HSPC-based gene editing may therefore prevent the generation of cross-reactive T cells that maintain dual specificity imparted by the CAR and the mature TCR.
Subsequent to this study, the authors evaluated the persistence and function of HSPC-derived CAR-modified cells in a non-human primate model of HIV infection52. Similar to the mouse study, CD4ζCAR-modified HSPCs engrafted and differentiated into multiple haematopoietic lineages that expressed the CAR, including natural killer cells, which have the cellular machinery to integrate signals through the TCR CD3ζ chain and may contribute to HIV-specific immunity65. However, in other lineages such as B cells, CAR expression has no obvious benefit, and it may render these cells susceptible to HIV infection. Thus, the overall benefit of CAR expression by non-T cells remains unclear. To evaluate the protective effect of CAR-modified cells, animals were infected with a simian–human immunodeficiency virus (SHIV) variant for 24 weeks, followed by 28 weeks of cART before treatment interruption. Ultimately, CAR-modified cells failed to prevent SHIV replication in the absence of cART, but there was a marked reduction in the magnitude of rebound viraemia following treatment cessation in CAR-expressing primates, which was concurrent with the expansion of CAR-modified cell populations52. Despite the absence of durable SHIV control, this study showed the safety of HSPC-based gene therapy in a preclinical animal model and, importantly, therapy resulted in the stable production of antiviral cells for nearly 2 years. These findings underscore the possibility that HSPC-based CAR therapy could overcome the poor persistence that is associated with peripheral-based effector CAR T cell products.
Purging the latent HIV reservoir
The central challenge to HIV cure efforts is the persistence of a latent viral reservoir despite effective cART66. The ‘shock and kill’ strategy aims to purge this reservoir by using latency-reversing agents (LRAs) to disrupt HIV quiescence67. It is hoped that reactivated cells will die as a result of virus-induced cytopathic effects and/or be lysed by immune effectors68. However, LRAs alone have not measurably reduced the size of the latent reservoir, potentially because of insufficient virus reactivation and/or because existing immunity fails to clear reactivated cells69,70,71. Recently, it has been suggested that additional mechanisms contribute to this phenomenon. CD4+ T cells harbouring intact replication-competent HIV provirus, which are the source of recrudescent viraemia after cART interruption, evade CD8+ T cell-mediated clearance, possibly by dysregulating antigen presentation through HIV negative regulatory factor (Nef)72. Unlike naturally occurring virus-specific CTLs, CAR T cells may be uniquely well equipped to target CD4+ T cells harbouring intact provirus, as CAR T cells do not require antigen presentation by MHC molecules to elicit an immune response. Also, defective proviruses can be expressed and recognized by virus-specific CTLs, which may distract the immune response from targeting the latent reservoir73. However, defective proviruses often contain deletions in env that probably abrogate expression of the full-length protein74; this could mean that CAR T cells are poised to specifically recognize and lyse infected CD4+ T cells containing intact provirus. Despite these advantages over naturally occurring virus-specific CTLs, CAR T cells must still overcome several challenges to purge the latent reservoir.
Infected CD4+ T follicular helper cells (TFH cells) in B cell follicles of lymphoid tissue are a major compartment for persistent virus replication during cART75,76. Although virus-specific CTLs have been detected in lymph nodes, they are largely absent from the B cell follicles because they lack expression of CXC-chemokine receptor 5 (CXCR5), which is responsible for the trafficking of cells into the B cell zone along a CXC-chemokine ligand 13 (CXCL13) concentration gradient77,78. As a result, the paucity of CXCR5 expression on virus-specific CTLs is one mechanism that promotes the persistence of infected CD4+ TFH cells within an immune-privileged site79. In addition to the physical segregation of virus-specific CTLs from infected CD4+ TFH cells, recent data suggest that these CTLs have markedly reduced cytotoxic potential in lymphoid tissue and are characterized by low levels of expression of perforin and granzymes80. This finding implies the existence of an unknown phenomenon that blunts CTL-mediated immunopathology in lymph nodes, which may be important for the unimpeded development of adaptive immune responses, but creates a unique anatomical niche with immune privilege that can enable pathogens such as HIV to proliferate, unrestricted by virus-specific CTLs. Consequently, CAR T cells must overcome the immune privilege of the B cell follicle and maintain cytolytic function to cure HIV infection.
One approach is to engineer effector CAR T cells to express the follicular homing receptor CXCR5, which will mediate the entry of CAR T cells into the B cell follicle, where they can target HIV-infected CD4+ TFH cells (Fig. 2). As a proof of concept, CXCR5 has been ectopically expressed in peripheral blood-derived CD8+ T cells from simian immunodeficiency virus (SIV)-infected rhesus macaques81. After infusion, these CXCR5+CD8+ T cells preferentially homed to B cell follicles in both spleen and lymph nodes and colocalized with SIV-infected cells. This approach could be applied to effector CAR T cells alone or in conjunction with LRAs to promote virus reactivation from latently infected cells (Fig. 2). Recent data indicate that the IL-15 superagonist complex ALT-803 can reverse HIV latency and promote CD8+ T cell entry into follicular regions82,83. Systemic treatment with ALT-803 in SIV-infected rhesus macaques induced the accumulation of virus-specific CD8+ T cells within the B cell follicle. Infiltration of virus-specific T cells into the follicles of elite controller rhesus macaques was concurrent with a reduction in the number of SIV-infected cells82. Together, these findings highlight how additional T cell engineering and/or LRA treatment could synergize with effector CAR T cell therapy to alter the trafficking of CAR T cells into sites of cryptic virus replication to purge persistently infected cells (Fig. 2).
The trafficking of chimeric antigen receptor (CAR)-expressing T cells into the B cell follicles of lymphoid tissue could facilitate the elimination of CD4+ T follicular helper (TFH) cells that are persistently infected with HIV-1. a | Naturally occurring HIV-specific CD8+ cytotoxic T lymphocytes (CTLs) are present in the extrafollicular region of a lymph node. However, many CTLs fail to access the B cell follicle because they lack expression of the follicular homing receptor CXC-chemokine receptor 5 (CXCR5), which can mediate chemotaxis along a CXC-chemokine ligand 13 (CXCL13) concentration gradient. b | However, CXCR5 gene engineering could enable HIV-specific CAR T cells to enter into the B cell follicle. Upon entry, CAR T cells could eliminate infected CD4+ TFH cells and reduce the population size of cells that contribute to recrudescent viraemia after interruption of combination antiretroviral therapy (cART). In addition, before cART interruption, administration of latency-reversing agents, such as an IL-15 superagonist complex, could synergize with CAR T cells to eliminate the pool of infected CD4+ T cells that exist in lymphoid and peripheral tissues.
Summary
The field of cancer immunotherapy has made important advances in CAR technology, which have resulted in remissions of a subset of treatment-refractory malignancies. Recently, the HIV field has applied these advances to generate functional HIV-specific effector CAR T cells that could be used in an immunotherapeutic strategy to eradicate disease. Toxicity has been, and will continue to be, a crucial issue for CAR T cell therapy in patients with cancer. It is not yet known to what extent toxicity induced by HIV-specific CARs will limit their clinical use. Fortunately, HIV Env is a non-self molecule, and thus faithful targeting of HIV-infected cells by CAR T cells should be achieved. An additional concern of CAR therapy is the onset of a cytokine storm, which has been observed in patients with cancer, particularly in those with large tumour burden84. However, CAR T cells for the treatment of HIV infection will probably be infused into the body during cART, when minimal amounts of antigen are present; therefore, the initial threat of a cytokine storm is unlikely. In the event that HIV-specific CAR T cells fail to control viral rebound after treatment interruption, the cytokine storm may become a problem. As the excess cytokine production is driven by antigen, cART as well as IL-6-specific antibodies may be effective approaches to halt this adverse event85. Furthermore, the high cost of CAR T cell therapies is a concern in both cancer and HIV infection, but if durable remission can be achieved, we are confident that an economical way to administer these life-saving, life-changing therapies will emerge. These issues of toxicity and cost are discussed in greater detail elsewhere10,43,66.
The new generation of CAR T cells are equipped to overcome many of the failures of endogenous virus-specific CTLs to control infection. So far, second-generation CAR T cells have proved safe and have been shown to have antiviral activity in both mouse and non-human primate models of HIV infection. However, successful CAR T cell therapy in humans will likely depend on the long-term maintenance of functional T cells that remain poised to respond to latent HIV reactivation for months or years after infusion. Thus, research emphasis must be placed on augmenting the survival of CAR T cells in environments with a low antigen burden and developing strategies to protect CAR T cells from HIV infection. Furthermore, future investigation could examine the synergistic effects of CAR T cells with LRAs and other immunomodulatory drugs to eliminate the latent HIV reservoir. Together, these studies highlight the immense promise of CAR T cells to be used alone or in combination with other therapies to cure HIV infection in humans.
CAR T cells for autoimmune disease
Many state-of-the-art treatments for autoimmune diseases are not curative, have marked side effects and do not treat all of the disease-related complications. Thus, disruptive therapies, such as CAR T cell-based therapies, are desperately needed. For example, effector CAR T cells could be directed to kill the pathological immune cells of an autoimmune disease. Alternatively, as many autoimmune diseases can be attributed to a combination of suboptimal function, trafficking, stability and abundance of Treg cells, CARs could be used to guide Treg cells to the autoimmune milieu where they can be activated, proliferate and exert their suppressive function. We discuss both approaches below.
Chimeric autoantibody receptors
In chimeric autoantibody receptors (CAARs), the extracellular portion of the receptor consists of the protein target of self-reactive antibodies, which enables CAAR T cells to destroy autoimmune B cells in a manner analogous to the way in which CD19CAR T cells target and destroy B cell leukaemia cells. Thus, when the B cell receptor (BCR) of an autoimmune B cell from the polyclonal pool encounters an effector CAAR T cell, it is destroyed and cannot produce autoantibodies. Preclinical proof of concept was obtained from a humanized mouse model of pemphigus vulgaris, in which autoimmune B cells target desmogleins causing skin and other mucous membranes to blister. Patients with this disease have traditionally been treated with corticosteroids and other broadly immunosuppressive agents that reduce whole-body immunosurveillance. Effector T cells expressing a CAAR that consists of desmoglein 3 fused to a second-generation 4-1BB–CD3ζ signalling domain interacted with cognate BCRs and induced the lysis of pathogenic B cells86. Because effector CAAR T cells function by killing their cognate cellular targets, the lessons learned from ongoing clinical and laboratory studies of effector CAR T cells for cancer therapy are likely to apply to effector CAAR T cell therapy also. The use of effector CAAR T cells could be extended to treat other B cell-mediated pathologies, such as systemic lupus erythematosus or rheumatoid arthritis. Furthermore, CAAR T cells targeting a CAR molecule could be used as a safety switch to eliminate autoimmunity caused by a previous infusion of effector CAR T cells87.
Re-directing regulatory T cells
Recently, several phase I clinical trials have been completed testing the safety and feasibility of using polyclonal Treg cells to delay the progression of type 1 diabetes and prevent graft-versus-host disease (GVHD) after bone marrow transplantation88,89,90,91. These pioneering studies have shown that generating very large numbers of Treg cells in a GMP-compliant manner is feasible92,93 and that large Treg cell infusions are well tolerated by patients with no evidence of global immunosuppression. Importantly, the incidence of acute GVHD observed in patients treated with expanded Treg cells was reduced. Furthermore, in the study of patients with type 1 diabetes, Treg cells were found up to a year after infusion, which indicates that infused Treg cells can persist and thus may be capable of promoting long-term tolerance.
Introducing CARs into Treg cells is an attractive way to generate antigen-specific Treg cells. In addition to reducing the number of Treg cells that are required for an effective response94, antigen specificity should restrict the trafficking and off-target suppression of injected Treg cells. However, there are key differences in the biology of Treg cells and effector T cells, including their responses to TCR stimulation95, co-receptor ligation96 and cytokines97, that bring into question how applicable the axioms established from the use of effector CAR T cells in patients with cancer will be to CAR Treg cells.
Compared with CAR-based therapies for HIV infection and cancer, the use of CAR Treg cells to fight autoimmunity is a relatively new concept. In a landmark study, CAR Treg cells specific for 2,4,6-trinitrobenzene sulfonic acid (TNBS) were used in a mouse model of TNBS-induced colitis98. The authors showed that CAR Treg cells could proliferate in an antigen-specific manner; traffic and accumulate at the target organ; prevent or ameliorate TNBS-induced colitis at suboptimal doses at which polyclonal Treg cells had no effect; and promote bystander suppression of a different form of colitis in the presence of target antigen. Later studies built on these findings by showing the ability of CAR Treg cells to prevent and/or ameliorate disease in other mouse models of colitis99, colitis-associated cancer100 and experimental autoimmune encephalomyelitis101. These mouse studies provide a strong rationale to move CAR Treg cell therapy into preclinical studies. In Box 1, we discuss why MHC-mismatched transplantation is an attractive indication to first test CAR Treg cells in the clinic.
Target selection
Similar to the use of CAR T cells in patients with cancer, the ideal antigen target for CAR Treg cells in autoimmune disease will be highly expressed on the cell surface, and expression will be limited to the cell type or tissue of interest (see Table 2 for a comparison between the properties of effector CAR T cells and CAR Treg cells). Unfortunately, the difficulty of identifying the ideal target for cancer-specific effector CAR T cells is also shared for CAR Treg cells. However, the consequences of off-target recognition are very different. Reactivity of effector CAR T cells against on-target, off-tumour tissue can have serious effects. For example, human epidermal growth factor receptor 2 (HER2; also known as ERBB2)-specific effector CAR T cells caused fatal acute respiratory distress syndrome in one patient owing to a low level of expression of the target antigen in the lung102. By contrast, the off-tissue reactivity of CAR Treg cells will probably have less severe consequences, as it is known that the infusion of polyclonal Treg cells does not cause opportunistic infection or cancer88,89,90,91. However, the tonic signalling that has been observed for some CAR constructs54 may give CAR Treg cells constitutive suppressive activity; thus, the safety profile of unmodified Treg cells may not predict the safety profile of CAR Treg cells. One concern with on-target, off-tissue recognition by CAR Treg cells is that these cells may preferentially home to the off-tissue site at the expense of where they are needed, and thus these off-tissue sinks may limit the effectiveness of antigen-specific Treg cell therapy. Moreover, the accumulation of Treg cells in otherwise healthy tissue may create a milieu that is favourable for tumour formation or pathogen survival, but to the best of our knowledge, this has not been experimentally addressed as yet.
Cell stability
If an effector CAR T cell converts to either an exhausted T cell or a Treg cell, this is unlikely to raise any safety concerns. This conversion may decrease the efficacy of the therapy and, in theory, if most of the effector CAR T cells were to convert to Treg cells, then this could hasten disease progression, but this has not been observed in the cancer trials so far. By contrast, substantial safety concerns would be raised if CAR Treg cells convert to effector T cells, as this has the potential to exacerbate disease progression.
Evidence from mouse studies shows that when Treg cells are exposed to inflammatory conditions, some cells lose expression of forkhead box protein P3 (FOXP3) and gain pro-inflammatory function103. Thus, the conversion of β cell-specific CAR Treg cells into effector T cells will likely potentiate the killing of pancreatic islet β cells and accelerate, rather than delay, the progression of type 1 diabetes. Another way in which effector T cells bearing CARs could arise is if they contaminate the isolation of Treg cells that are used for source material. As stated earlier, Treg cells are a rare population, and achieving 100% purity will be near impossible using current GMP reagents on a clinical scale. As we do not fully understand how effector CAR T cells and CAR Treg cells differentially proliferate and traffic in vivo, it is possible that a small population of effector CAR T cells could expand or traffic104 much faster than CAR Treg cells, with devastating consequences. The opposite is also a concern in that Treg cells could contaminate effector CAR T cell infusion products. However, Treg cells can be easily removed from the infusion product by selection on anti-CD25 beads before transduction, and the culture conditions that are used to proliferate effector T cells in vitro do not favour Treg cell proliferation105.
Safety
Several strategies have been proposed to minimize the possibility that effector T cells will express CARs that are intended to be expressed by Treg cells. First, the choice of initial starting material will be important. Engineered Treg cells derived from cord blood, rather than from adult peripheral blood mononuclear cells (PBMCs), will likely be safest as a starting material because they lack effector T cells that arise later in life, are easily isolated relative to Treg cells from peripheral blood and have a naive phenotype that is associated with Treg cell lineage stability and function106,107,108. In most scenarios for which a patient does not have cryopreserved autologous cord blood, third-party cord blood Treg cells are a viable, safe alternative that is already being used in clinical trials for the treatment of GVHD89,90,93,109. However, for applications other than GVHD, it is unclear how potential MHC mismatches might affect the long-term persistence and function of infused Treg cells. In the absence of a suitable source of cord blood cells, adult PBMCs could be sorted for naive Treg cell markers106,110,111 provided that a GMP-compatible sorter becomes commercially available.
To test the stability of an expanded Treg cell product, methylation of the Treg cell-specific demethylated region can function as a marker for effector T cell conversion potential112. This test can be carried out in fewer than 24 hours and has been included in the product release criteria of expanded Treg cells for patient infusion113. Finally, we have shown that a TCR with too low affinity to function in effector T cells was able to confer potent, antigen-specific suppression when expressed in a Treg cell114, which suggests that the signal strength required to activate a Treg cell is less than that required to activate effector T cells. Thus, one way in which the safety of CAR Treg cell therapy could be improved would be to engineer the CAR so that it has the signal strength to function in a Treg cell but not an effector T cell.
Once the cell therapy has been administered to a patient, the ability to induce apoptosis of engineered cells could mitigate adverse effects. Several suicide switches have been described, whereby administration of an otherwise inert drug causes controlled apoptosis of the infused CAR T cell product115. More complex switches could be envisioned in the future, such as ones that induce cell death autonomously when FOXP3 expression is lost by CAR Treg cells or when expression of IL-17 and/or another pro-inflammatory cytokine is turned on.
Studies have shown that Treg cells can induce effector T cells to become suppressive cells also, through a process known as infectious tolerance116. Thus, the CAR Treg cells might not be necessary for all of the therapeutic effect, provided that they induce the generation of a durable oligoclonal population of local Treg cells. Last, introduction of FOXP3 into CAR Treg cells under the control of a heterologous promoter may help to maintain FOXP3 expression and suppressive activity even if natural FOXP3 expression is lost117,118,119. At a minimum, this approach would help to ensure that if antigen-specific Treg cells lost suppressive activity, the ectopically expressed FOXP3 would minimize the activity of the resulting effector T cells.
Signalling
Because effector T cells and Treg cells have distinct co-stimulatory requirements, it is possible that the co-stimulatory domain that gives Treg cells the most suppressive activity will be distinct from the co-stimulatory domain that yields the most potent effector T cell activity. Moreover, CAR Treg cells might need to be uniquely designed for each targeted autoimmune disease, as the choice of co-stimulation domain might affect trafficking, metabolism and/or survival of the CAR Treg cells. However, mounting evidence indicates that CD28-mediated co-stimulation will be necessary for CAR Treg cells120. So far, each published CAR has included the CD28 signalling domain98,99,100,101,121,122,123,124,125 as CD28 signalling is known to be essential for proper Treg cell maintenance, proliferation and function126,127. No comprehensive study comparing CD28 with other co-stimulation domains has been carried out; thus, other co-stimulation domains alone or in combination with CD28 may be of benefit. For example, the intracellular domains of cytotoxic T lymphocyte antigen 4 (CTLA4)128, CD27 (ref.129) and inducible T cell co-stimulator (ICOS)130 could be useful as part of a CAR on the basis of their demonstrated roles in the proliferation and development of Treg cells.
Dosing and persistence
Understanding the optimal T cell dose to infuse into a patient specific for each application of CAR T cells will improve the safety, efficacy and economic feasibility of this approach131,132. However, CAR T cells function as a ‘living’ drug whose half-life is difficult to ascertain, and as most of our knowledge of CAR T cell persistence comes from measuring their abundance in the peripheral blood and not tissues, determining the optimal dose of T cells will at best be complicated and disease dependent. For initial studies that used expanded Treg cell populations to prevent acute GVHD, patients who received a larger dose of expanded Treg cells benefited more than patients who received a smaller dose; 43% of patients developed low-grade GVHD in an earlier, low-dose trial, whereas only 9% of patients developed GVHD in the higher-dose trial (compared with 63% for controls)90,133. As Treg cells are a rare population of cells, highly efficient culture systems may be needed to reach the target dose for CAR Treg cells92,105. For transplant applications, in which there is an abundance of antigen, a relatively small dose of CAR Treg cells may be sufficient if the therapeutic population can be expanded in the patient.
A successful effector CAR T cell therapy is designed to kill every cancer or virus-infected cell in the patient, thereby eliminating the persistence of its target antigen. When target antigen becomes limiting, the pool of infused CAR T cells may retract to a size where it cannot then respond to a recurrence of cancer cells. By contrast, properly functioning CAR Treg cell therapy will protect its target cells from elimination, and these cells will function as a source of antigen to maintain CAR Treg cell persistence. Thus, successful CAR Treg cell therapy will positively support the maintenance of engineered T cells and thus may have an advantage over effector CAR T cells in terms of generating a durable cure.
Summary
Ultimately, the adaptation of CAR technology to treat autoimmune diseases and to facilitate organ transplantation has shown promise in the laboratory and in small animal models, which sets the stage for organ transplant studies in MHC-mismatched non-human primates. Yet, we must determine the optimal extracellular binding domains, intracellular signalling domains and manufacturing protocols for these CARs before investigating cell dosage, timing and route of administration in the clinic to maximize the safety, efficacy and durability of a cure. Owing to inherent differences between the biology of Treg cells and the biology of effector T cells, as well as disease-specific requirements, much work remains to be done in developing the prime therapeutic product of CAR Treg cells.
Concluding remarks
T cells have a pivotal role in controlling cancer, infectious disease and autoimmunity. Thus, it seems likely that engineered, re-directed T cells will also be able to control these disease indications when naturally occurring T cells fail. As we better understand the biology of naturally occurring T cells, these advances will help the field to engineer better T cells to function in a wide array of disease areas. We have highlighted many hurdles that remain to broaden the scope of CAR T cell therapy from patients with cancer, which may give the impression that these other therapies will be a long time coming. However, it is important to keep in mind how the initial clinical success that was seen in just three patients who received CD19CARs84 ignited a firestorm of activity that led to FDA approval a mere 6 years later. If early clinical success of CAR T cells is observed in patients infected with HIV or with autoimmune disease, then the path to FDA approval may be quicker as a result of the path blazed by the approval of CD19CAR T cell therapies.
References
McMichael, A. T cell responses and viral escape. Cell 93, 673–676 (1998).
Roberts, M. R. et al. Targeting of human immunodeficiency virus-infected cells by CD8 + T lymphocytes armed with universal T cell receptors. Blood 84, 2878–2889 (1994).
Scholler, J. et al. Decade-long safety and function of retroviral-modified chimeric antigen receptor T cells. Sci. Transl Med. 4, 132ra153 (2012).
Castelli, J. C., Deeks, S. G., Shiboski, S. & Levy, J. A. Relationship of CD8+ T cell noncytotoxic anti-HIV response to CD4+ T cell number in untreated asymptomatic HIV-infected individuals. Blood 99, 4225–4227 (2002).
Mitsuyasu, R. T. et al. Prolonged survival and tissue trafficking following adoptive transfer of CD4zeta gene-modified autologous CD4+ and CD8+ T cells in human immunodeficiency virus-nfected subjects. Blood 96, 785–793 (2000).
Walker, R. E. et al. Long-term in vivo survival of receptor-modified syngeneic T cells in patients with human immunodeficiency virus infection. Blood 96, 467–474 (2000).
June, C. H., O’Connor, R. S., Kawalekar, O. U., Ghassemi, S. & Milone, M. C. CAR T cell immunotherapy for human cancer. Science 359, 1361–1365 (2018).
Lim, W. A. & June, C. H. The principles of engineering immune cells to treat cancer. Cell 168, 724–740 (2017).
June, C. H., Blazar, B. R. & Riley, J. L. Engineering lymphocyte subsets: tools, trials and tribulations. Nat. Rev. Immunol. 9, 704–716 (2009).
Barrett, D. M., Grupp, S. A. & June, C. H. Chimeric antigen receptor- and TCR-modified T cells enter main street and wall street. J. Immunol. 195, 755–761 (2015).
Cheng, Y., Wong, M. T., van der Maaten, L. & Newell, E. W. Categorical analysis of human T cell heterogeneity with one-dimensional soli-expression by nonlinear stochastic embedding. J. Immunol. 196, 924–932 (2016).
Rainwater-Lovett, K., Uprety, P. & Persaud, D. Advances and hope for perinatal HIV remission and cure in children and adolescents. Curr. Opin. Pediatr. 28, 86–92 (2016).
Saez-Cirion, A. et al. Post-treatment HIV-1 controllers with a long-term virological remission after the interruption of early initiated antiretroviral therapy ANRS VISCONTI Study. PLOS Pathog. 9, e1003211 (2013).
Jones, R. B. & Walker, B. D. HIV-specific CD8+ T cells and HIV eradication. J. Clin. Invest. 126, 455–463 (2016).
Fesnak, A. D., June, C. H. & Levine, B. L. Engineered T cells: the promise and challenges of cancer immunotherapy. Nat. Rev. Cancer 16, 566–581 (2016).
van der Stegen, S. J., Hamieh, M. & Sadelain, M. The pharmacology of second-generation chimeric antigen receptors. Nat. Rev. Drug Discov. 14, 499–509 (2015).
Long, A. H. et al. 4-1BB costimulation ameliorates T cell exhaustion induced by tonic signaling of chimeric antigen receptors. Nat. Med. 21, 581–590 (2015).
Gomes-Silva, D. et al. Tonic 4-1BB costimulation in chimeric antigen receptors impedes T cell survival and is vector-dependent. Cell Rep. 21, 17–26 (2017).
Kawalekar, O. U. et al. Distinct signaling of coreceptors regulates specific metabolism pathways and impacts memory development in CAR T cells. Immunity 44, 380–390 (2016).
Frauwirth, K. A. et al. The CD28 signaling pathway regulates glucose metabolism. Immunity 16, 769–777 (2002).
Leibman, R. S. et al. Supraphysiologic control over HIV-1 replication mediated by CD8 T cells expressing a re-engineered CD4-based chimeric antigen receptor. PLOS Pathog. 13, e1006613 (2017).
Liu, B. et al. Chimeric antigen receptor T cells guided by the single-chain Fv of a broadly neutralizing antibody specifically and effectively eradicate virus reactivated from latency in CD4+ T lymphocytes isolated from HIV-1-infected individuals receiving suppressive combined antiretroviral therapy. J. Virol. 90, 9712–9724 (2016).
Hale, M. et al. Engineering HIV-resistant, anti-HIV chimeric antigen receptor T cells. Mol. Ther. 25, 570–579 (2017).
Liu, L. et al. Novel CD4-based bispecific chimeric antigen receptor designed for enhanced anti-HIV potency and absence of HIV entry receptor activity. J. Virol. 89, 6685–6694 (2015).
Ghanem, M. H. et al. Bispecific chimeric antigen receptors targeting the CD4 binding site and high-mannose Glycans of gp120 optimized for anti-human immunodeficiency virus potency and breadth with minimal immunogenicity. Cytotherapy 20, 407–419 (2018).
Figdor, C. G., van Kooyk, Y. & Adema, G. J. C-Type lectin receptors on dendritic cells and Langerhans cells. Nat. Rev. Immunol. 2, 77–84 (2002).
Ip, W. K., Takahashi, K., Ezekowitz, R. A. & Stuart, L. M. Mannose-binding lectin and innate immunity. Immunol. Rev. 230, 9–21 (2009).
Lee, D. W. et al. T cells expressing CD19 chimeric antigen receptors for acute lymphoblastic leukaemia in children and young adults: a phase 1 dose-escalation trial. Lancet 385, 517–528 (2015).
Brentjens, R. J. et al. CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci. Transl Med. 5, 177ra138 (2013).
Porter, D. L. et al. Chimeric antigen receptor T cells persist and induce sustained remissions in relapsed refractory chronic lymphocytic leukemia. Sci. Transl Med. 7, 303ra139 (2015).
Turtle, C. J. et al. CD19 CAR-T cells of defined CD4+:CD8+ composition in adult B cell ALL patients. J. Clin. Invest. 126, 2123–2138 (2016).
Gardner, R. A. et al. Intent-to-treat leukemia remission by CD19 CAR T cells of defined formulation and dose in children and young adults. Blood 129, 3322–3331 (2017).
Maude, S. L. et al. Chimeric antigen receptor T cells for sustained remissions in leukemia. N. Engl. J. Med. 371, 1507–1517 (2014).
Sallusto, F., Lanzavecchia, A., Araki, K. & Ahmed, R. From vaccines to memory and back. Immunity 33, 451–463 (2010).
Wang, X. et al. CMVpp65 vaccine enhances the antitumor efficacy of adoptively transferred CD19-redirected CMV-specific T cells. Clin. Cancer Res. 21, 2993–3002 (2015).
Sun, J. et al. Early transduction produces highly functional chimeric antigen receptor-modified virus-specific T cells with central memory markers: a Production Assistant for Cell Therapy (PACT) translational application. J. Immunother. Cancer 3, 5 (2015).
Nakazawa, Y. et al. PiggyBac-mediated cancer immunotherapy using EBV-specific cytotoxic T cells expressing HER2-specific chimeric antigen receptor. Mol. Ther. 19, 2133–2143 (2011).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/show/NCT01430390 (2011).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/show/NCT00709033 (2008).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/show/NCT01109095 (2010).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/show/NCT03186118 (2017).
Gray, G. E., Laher, F., Lazarus, E., Ensoli, B. & Corey, L. Approaches to preventative and therapeutic HIV vaccines. Curr. Opin. Virol. 17, 104–109 (2016).
Leibman, R. S. & Riley, J. L. Engineering T cells to functionally cure HIV-1 infection. Mol. Ther. 23, 1149–1159 (2015).
Perez, E. E. et al. Establishment of HIV-1 resistance in CD4+ T cells by genome editing using zinc-finger nucleases. Nat. Biotechnol. 26, 808–816 (2008).
Tebas, P. et al. Gene editing of CCR5 in autologous CD4 T cells of persons infected with HIV. N. Engl. J. Med. 370, 901–910 (2014).
Eyquem, J. et al. Targeting a CAR to the TRAC locus with CRISPR/Cas9 enhances tumour rejection. Nature 543, 113–117 (2017).
Sather, B. D. et al. Efficient modification of CCR5 in primary human hematopoietic cells using a megaTAL nuclease and AAV donor template. Sci. Transl Med. 7, 307ra156 (2015).
Wang, J. et al. Highly efficient homology-driven genome editing in human T cells by combining zinc-finger nuclease mRNA and AAV6 donor delivery. Nucleic Acids Res. 44, e30 (2016).
Maier, D. A. et al. Efficient clinical scale gene modification via zinc finger nuclease-targeted disruption of the HIV co-receptor CCR5. Hum. Gene Ther. 24, 245–258 (2013).
MacLean, A. G. et al. A novel real-time CTL assay to measure designer T cell function against HIV Env+ cells. J. Med. Primatol. 43, 341–348 (2014).
Kamata, M. et al. Ectopic expression of anti-HIV-1 shRNAs protects CD8+ T cells modified with CD4zeta CAR from HIV-1 infection and alleviates impairment of cell proliferation. Biochem. Biophys. Res. Commun. 463, 216–221 (2015).
Zhen, A. et al. Long-term persistence and function of hematopoietic stem cell-derived chimeric antigen receptor T cells in a nonhuman primate model of HIV/AIDS. PLOS Pathog. 13, e1006753 (2017). This paper reports HIV-specific CAR T cell therapy using haematopoietic stem cells in a non-human primate model of HIV infection.
Leslie, G. J. et al. Potent and broad inhibition of HIV-1 by a peptide from the gp41 heptad repeat-2 domain conjugated to the CXCR4 amino terminus. PLOS Pathog. 12, e1005983 (2016).
Frigault, M. J. et al. Identification of chimeric antigen receptors that mediate constitutive or inducible proliferation of T cells. Cancer Immunol. Res. 3, 356–367 (2015).
Levine, B. L. et al. Antiviral effect and ex vivo CD4+ T cell proliferation in HIV-positive patients as a result of CD28 costimulation. Science 272, 1939–1943 (1996).
Richardson, M. W., Jadlowsky, J., Didigu, C. A., Doms, R. W. & Riley, J. L. Kruppel-like factor 2 modulates CCR5 expression and susceptibility to HIV-1 infection. J. Immunol. 189, 3815–3821 (2012).
Riley, J. L. et al. Modulation of susceptibility to HIV-1 infection by the cytotoxic T lymphocyte antigen 4 costimulatory molecule. J. Exp. Med. 191, 1987–1997 (2000).
Riley, J. L. et al. Intrinsic resistance to T cell infection with HIV type 1 induced by CD28 costimulation. J. Immunol. 158, 5545–5553 (1997).
Carroll, R. G. et al. Differential regulation of HIV-1 fusion cofactor expression by CD28 costimulation of CD4+ T cells. Science 276, 273–276 (1997).
Mendelson, A. & Frenette, P. S. Hematopoietic stem cell niche maintenance during homeostasis and regeneration. Nat. Med. 20, 833–846 (2014).
Zhen, A. & Kitchen, S. Stem-cell-based gene therapy for HIV infection. Viruses 6, 1–12 (2013).
Kitchen, S. G. et al. In vivo suppression of HIV by antigen specific T cells derived from engineered hematopoietic stem cells. PLOS Pathog. 8, e1002649 (2012).
Zhen, A. et al. Stem-cell based engineered immunity against HIV infection in the humanized mouse model. J. Vis. Exp. 113, e54048 (2016).
Zhen, A. et al. HIV-specific immunity derived from chimeric antigen receptor-engineered stem cells. Mol. Ther. 23, 1358–1367 (2015).
Tran, A. C., Zhang, D., Byrn, R. & Roberts, M. R. Chimeric zeta-receptors direct human natural killer (NK) effector function to permit killing of NK-resistant tumor cells and HIV-infected T lymphocytes. J. Immunol. 155, 1000–1009 (1995).
Riley, J. L. & Montaner, L. J. Cell-mediated immunity to target the persistent human immunodeficiency virus reservoir. J. Infect. Dis. 215, S160–S171 (2017).
Shan, L. et al. Stimulation of HIV-1-specific cytolytic T lymphocytes facilitates elimination of latent viral reservoir after virus reactivation. Immunity 36, 491–501 (2012).
Deeks, S. G. HIV: shock and kill. Nature 487, 439–440 (2012).
Rasmussen, T. A. et al. Panobinostat, a histone deacetylase inhibitor, for latent-virus reactivation in HIV-infected patients on suppressive antiretroviral therapy: a phase 1/2, single group, clinical trial. Lancet HIV 1, e13–e21 (2014).
Sogaard, O. S. et al. The depsipeptide romidepsin reverses HIV-1 latency in vivo. PLOS Pathog. 11, e1005142 (2015).
Spivak, A. M. et al. A pilot study assessing the safety and latency-reversing activity of disulfiram in HIV-1-infected adults on antiretroviral therapy. Clin. Infect. Dis. 58, 883–890 (2014).
Huang, S. H. et al. Latent HIV reservoirs exhibit inherent resistance to elimination by CD8+ T cells. J. Clin. Invest. 128, 876–889 (2018).
Pollack, R. A. et al. Defective HIV-1 proviruses are expressed and can be recognized by cytotoxic T lymphocytes, which shape the proviral landscape. Cell Host Microbe 21, 494–506 (2017).
Bruner, K. M. et al. Defective proviruses rapidly accumulate during acute HIV-1 infection. Nat. Med. 22, 1043–1049 (2016).
Banga, R. et al. PD-1+ and follicular helper T cells are responsible for persistent HIV-1 transcription in treated aviremic individuals. Nat. Med. 22, 754–761 (2016).
Perreau, M. et al. Follicular helper T cells serve as the major CD4 T cell compartment for HIV-1 infection, replication, and production. J. Exp. Med. 210, 143–156 (2013).
Ansel, K. M. et al. A chemokine-driven positive feedback loop organizes lymphoid follicles. Nature 406, 309–314 (2000).
Forster, R. et al. A putative chemokine receptor, BLR1, directs B cell migration to defined lymphoid organs and specific anatomic compartments of the spleen. Cell 87, 1037–1047 (1996).
Fukazawa, Y. et al. B cell follicle sanctuary permits persistent productive simian immunodeficiency virus infection in elite controllers. Nat. Med. 21, 132–139 (2015). This paper shows that B cell follicles in lymphoid tissue are sanctuary sites for persistent SIV replication despite the presence of SIV-specific CD8 + T cells.
Reuter, M. A. et al. HIV-specific CD8+ T cells exhibit reduced and differentially regulated cytolytic activity in lymphoid tissue. Cell Rep. 21, 3458–3470 (2017). This paper highlights that HIV-specific CD8 + T cells in lymphoid tissue have reduced cytolytic activity, which indicates that lymph nodes are a site of immune privilege against CD8 + T cell-mediated cytotoxicity.
Ayala, V. I. et al. CXCR5-dependent entry of CD8 T cells into Rhesus Macaque B-cell follicles achieved through T-cell engineering. J. Virol. 91, e02507-16 (2017).
Webb, G. M. et al. The human IL-15 superagonist ALT-803 directs SIV-specific CD8+ T cells into B cell follicles. Blood Adv. 2, 76–84 (2018).
Jones, R. B. et al. A subset of latency-reversing agents expose HIV-infected resting CD4+ T-cells to recognition by cytotoxic T-lymphocytes. PLOS Pathog. 12, e1005545 (2016).
Porter, D. L., Levine, B. L., Kalos, M., Bagg, A. & June, C. H. Chimeric antigen receptor-modified T cells in chronic lymphoid leukemia. N. Engl. J. Med. 365, 725–733 (2011).
Chen, F. et al. Measuring IL-6 and sIL-6R in serum from patients treated with tocilizumab and/or siltuximab following CAR T cell therapy. J. Immunol. Methods 434, 1–8 (2016).
Ellebrecht, C. T. et al. Reengineering chimeric antigen receptor T cells for targeted therapy of autoimmune disease. Science 353, 179–184 (2016). This paper provides a description of CAAR T cells, which showed specific killing of autoimmune B cells.
Jena, B. et al. Chimeric antigen receptor (CAR)-specific monoclonal antibody to detect CD19-specific T cells in clinical trials. PLOS One 8, e57838 (2013).
Trzonkowski, P. et al. First-in-man clinical results of the treatment of patients with graft versus host disease with human ex vivo expanded CD4+CD25+CD127− T regulatory cells. Clin. Immunol. 133, 22–26 (2009).
Brunstein, C. G. et al. Infusion of ex vivo expanded T regulatory cells in adults transplanted with umbilical cord blood: safety profile and detection kinetics. Blood 117, 1061–1070 (2011).
Brunstein, C. G. et al. Umbilical cord blood-derived T regulatory cells to prevent GVHD: kinetics, toxicity profile, and clinical effect. Blood 127, 1044–1051 (2016). This study shows that large-scale, GMP-compliant expansion of polyclonal Treg cell populations using artificial antigen-presenting cells can be used to prevent the development of GVHD in bone marrow transplant recipients.
Bluestone, J. A. et al. Type 1 diabetes immunotherapy using polyclonal regulatory T cells. Sci. Transl Med. 7, 315ra189 (2015). By giving polyclonal T reg cell infusions to patients with type 1 diabetes, the authors show that the clinical expansion process can improve the in vitro suppressive function of T reg cells and correct intrinsic patient-associated T reg cell deficits. In addition, the authors show that long-term, stable persistence of infused T reg cells can occur in vivo.
Hippen, K. L. et al. Massive ex vivo expansion of human natural regulatory T cells (T(regs)) with minimal loss of in vivo functional activity. Sci. Transl Med. 3, 83ra41 (2011).
McKenna, D. H. Jr. et al. Optimization of cGMP purification and expansion of umbilical cord blood-derived T-regulatory cells in support of first-in-human clinical trials. Cytotherapy 19, 250–262 (2017).
Tang, Q. et al. In vitro-expanded antigen-specific regulatory T cells suppress autoimmune diabetes. J. Exp. Med. 199, 1455–1465 (2004).
Moran, A. E. et al. T cell receptor signal strength in Treg and iNKT cell development demonstrated by a novel fluorescent reporter mouse. J. Exp. Med. 208, 1279–1289 (2011).
Tabares, P. et al. Human regulatory T cells are selectively activated by low-dose application of the CD28 superagonist TGN1412/TAB08. Eur. J. Immunol. 44, 1225–1236 (2014).
Setoguchi, R., Hori, S., Takahashi, T. & Sakaguchi, S. Homeostatic maintenance of natural Foxp3+ CD25+ CD4+ regulatory T cells by interleukin (IL)-2 and induction of autoimmune disease by IL-2 neutralization. J. Exp. Med. 201, 723–735 (2005).
Elinav, E., Waks, T. & Eshhar, Z. Redirection of regulatory T cells with predetermined specificity for the treatment of experimental colitis in mice. Gastroenterology 134, 2014–2024 (2008). This is an early report of CAR T reg cells, showing specificity, function, bystander suppression and trafficking.
Elinav, E., Adam, N., Waks, T. & Eshhar, Z. Amelioration of colitis by genetically engineered murine regulatory T cells redirected by antigen-specific chimeric receptor. Gastroenterology 136, 1721–1731 (2009).
Blat, D., Zigmond, E., Alteber, Z., Waks, T. & Eshhar, Z. Suppression of murine colitis and its associated cancer by carcinoembryonic antigen-specific regulatory T cells. Mol. Ther. 22, 1018–1028 (2014).
Fransson, M. et al. CAR/FoxP3-engineered T regulatory cells target the CNS and suppress EAE upon intranasal delivery. J. Neuroinflamm. 9, 112 (2012).
Morgan, R. A. et al. Case report of a serious adverse event following the administration of T cells transduced with a chimeric antigen receptor recognizing ERBB2. Mol. Ther. 18, 843–851 (2010).
Zhou, X. et al. Instability of the transcription factor Foxp3 leads to the generation of pathogenic memory T cells in vivo. Nat. Immunol. 10, 1000–1007 (2009). The authors show that T reg cells in autoimmune environments can become pathogenic ‘ex-FOXP3’ cells, highlighting a major safety concern for the use of CAR T reg cells.
Magnuson, A. M. et al. Population dynamics of islet-infiltrating cells in autoimmune diabetes. Proc. Natl Acad. Sci. USA 112, 1511–1516 (2015).
Riley, J. L., June, C. H. & Blazar, B. R. Human T regulatory cell therapy: take a billion or so and call me in the morning. Immunity 30, 656–665 (2009).
Hoffmann, P. et al. Only the CD45RA+ subpopulation of CD4+CD25high T cells gives rise to homogeneous regulatory T cell lines upon in vitro expansion. Blood 108, 4260–4267 (2006).
Fu, S. et al. CD4+ CD25+ CD62+ T-regulatory cell subset has optimal suppressive and proliferative potential. Am. J. Transplant. 4, 65–78 (2004).
Hippen, K. L. et al. Umbilical cord blood regulatory T cell expansion and functional effects of tumor necrosis factor receptor family members OX40 and 4-1BB expressed on artificial antigen-presenting cells. Blood 112, 2847–2857 (2008).
Seay, H. R. et al. Expansion of human Tregs from cryopreserved umbilical cord blood for GMP-compliant autologous adoptive cell transfer therapy. Mol. Ther. Methods Clin. Dev. 4, 178–191 (2017).
Golovina, T. N. et al. Retinoic acid and rapamycin differentially affect and synergistically promote the ex vivo expansion of natural human T regulatory cells. PLOS One 6, e15868 (2011).
Miyara, M. et al. Functional delineation and differentiation dynamics of human CD4+ T cells expressing the FoxP3 transcription factor. Immunity 30, 899–911 (2009).
Polansky, J. K. et al. DNA methylation controls Foxp3 gene expression. Eur. J. Immunol. 38, 1654–1663 (2008).
Putnam, A. L. et al. Clinical grade manufacturing of human alloantigen-reactive regulatory T cells for use in transplantation. Am. J. Transplant 13, 3010–3020 (2013).
Plesa, G. et al. TCR affinity and specificity requirements for human regulatory T cell function. Blood 119, 3420–3430 (2012).
Bonifant, C. L., Jackson, H. J., Brentjens, R. J. & Curran, K. J. Toxicity and management in CAR T cell therapy. Mol. Ther. Oncolyt. 3, 16011 (2016).
Jonuleit, H. et al. Infectious tolerance: human CD25+ regulatory T cells convey suppressor activity to conventional CD4+ T helper cells. J. Exp. Med. 196, 255–260 (2002).
Okada, M., Kanamori, M., Someya, K., Nakatsukasa, H. & Yoshimura, A. Stabilization of Foxp3 expression by CRISPR-dCas9-based epigenome editing in mouse primary T cells. Epigenetics Chromatin 10, 24 (2017).
Chai, J. G. et al. Regulatory T cells, derived from naive CD4 + CD25- T cells by in vitro Foxp3 gene transfer, can induce transplantation tolerance. Transplantation 79, 1310–1316 (2005).
Jaeckel, E., von Boehmer, H. & Manns, M. P. Antigen-specific FoxP3-transduced T cells can control established type 1 diabetes. Diabetes 54, 306–310 (2005).
Bour-Jordan, H. & Bluestone, J. A. Regulating the regulators: costimulatory signals control the homeostasis and function of regulatory T cells. Immunol. Rev. 229, 41–66 (2009).
MacDonald, K. G. et al. Alloantigen-specific regulatory T cells generated with a chimeric antigen receptor. J. Clin. Invest. 126, 1413–1424 (2016). An early paper showing how HLA-specific CARs can redirect T reg cells to promote tolerance in MHC-mismatched transplant recipients.
Boardman, D. A. et al. Expression of a chimeric antigen receptor specific for donor HLA class I enhances the potency of human regulatory T cells in preventing human skin transplant rejection. Am. J. Transplant 17, 931–943 (2017).
Noyan, F. et al. Prevention of allograft rejection by use of regulatory T cells with an MHC-specific chimeric antigen receptor. Am. J. Transplant 17, 917–930 (2017).
Yoon, J. et al. FVIII-specific human chimeric antigen receptor T-regulatory cells suppress T− and B cell responses to FVIII. Blood 129, 238–245 (2017).
Pierini, A. et al. T cells expressing chimeric antigen receptor promote immune tolerance. JCI Insight 2, e92865 (2017).
Salomon, B. et al. B7/CD28 costimulation is essential for the homeostasis of the CD4+CD25+ immunoregulatory T cells that control autoimmune diabetes. Immunity 12, 431–440 (2000).
Paulos, C. M. et al. Adoptive immunotherapy: good habits instilled at youth have long-term benefits. Immunol. Res. 42, 182–196 (2008).
Wing, K. et al. CTLA-4 control over Foxp3+ regulatory T cell function. Science 322, 271–275 (2008).
Claus, C. et al. CD27 signaling increases the frequency of regulatory T cells and promotes tumor growth. Cancer Res. 72, 3664–3676 (2012).
Akbari, O. et al. Antigen-specific regulatory T cells develop via the ICOS-ICOS-ligand pathway and inhibit allergen-induced airway hyperreactivity. Nat. Med. 8, 1024–1032 (2002).
June, C. H., Riddell, S. R. & Schumacher, T. N. Adoptive cellular therapy: a race to the finish line. Sci. Transl Med. 7, 280ps287 (2015).
Pan, J. et al. High efficacy and safety of low-dose CD19-directed CAR-T cell therapy in 51 refractory or relapsed B acute lymphoblastic leukemia patients. Leukemia 31, 2587 (2017).
Brunstein, C. G. et al. Adoptive transfer of umbilical cord blood-derived regulatory T cells and early viral reactivation. Biol. Blood Marrow Transplant 19, 1271–1273 (2013).
Riley, J. L. et al. Modulation of TCR-induced transcriptional profiles by ligation of CD28, ICOS, and CTLA-4 receptors. Proc. Natl Acad. Sci. USA 99, 11790–11795 (2002).
Lawlor, D. A., Ward, F. E., Ennis, P. D., Jackson, A. P. & Parham, P. HLA-A and B polymorphisms predate the divergence of humans and chimpanzees. Nature 335, 268–271 (1988).
Benitez, C. et al. Prospective multicenter clinical trial of immunosuppressive drug withdrawal in stable adult liver transplant recipients. Hepatology 58, 1824–1835 (2013).
Feng, S. et al. Complete immunosuppression withdrawal and subsequent allograft function among pediatric recipients of parental living donor liver transplants. JAMA 307, 283–293 (2012).
Todo, S. et al. A pilot study of operational tolerance with a regulatory T cell-based cell therapy in living donor liver transplantation. Hepatology 64, 632–643 (2016).
Acknowledgements
The authors thank members of the Riley laboratory for their thoughtful comments and support and members of the Center of Cellular Immunotherapies at the University of Pennsylvania for providing an exciting environment in which to study chimeric antigen receptor T cell therapy.
Reviewer information
Nature Reviews Immunology thanks S. Kitchen and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
All authors researched data for the article, discussed its content and wrote, reviewed and edited it before submission.
Corresponding author
Ethics declarations
Competing interests
J.L.R. holds equity in Tmunity Therapeutics. The other authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Glossary
- Chimeric antigen receptor
-
(CAR). A synthetic receptor engineered to be expressed on the surface of T cells or other immune cells to redirect cellular specificity.
- HIV reservoir
-
Persistent HIV that remains transcriptionally silent as inactive provirus within infected CD4+ T cells despite effective combination antiretroviral therapy.
- Combination antiretroviral therapy
-
(cART). Therapy that consists of two or more active drugs with different mechanisms of action that are used to subdue HIV replication.
- Exhaustion
-
A state of T cell dysfunction that develops over time with repeated exposure to cognate antigen, for example, during chronic infection with a virus such as HIV.
- Broadly neutralizing antibodies
-
(bNAbs). Antibodies that have the unique ability to neutralize and prevent infection with multiple and diverse strains of HIV.
- Homology-directed repair
-
(HDR). A mechanism in cells to repair double-stranded DNA breaks using a DNA donor template with homologous sequences flanking the break site.
- MegaTAL nuclease
-
A sequence-specific endonuclease with a DNA-binding domain that promotes efficient cleavage of genomic DNA with a high degree of fidelity.
- Good manufacturing practice
-
(GMP). A series of guidelines enforced by the Food and Drug Administration in the United States, and other similar bodies elsewhere, regarding the manufacturing of safe biological therapeutic agents.
- Tonic signalling
-
Low-level signalling caused by antigen-independent clustering of receptor molecules in the basal state of a cell.
- Latency-reversing agents
-
(LRAs). Pharmacological agents that induce HIV transcription from cells harbouring HIV provirus.
- T follicular helper cells
-
(TFH cells). A specialized CD4+ T cell subset that primarily resides in the B cell follicles of lymphoid tissue to aid the development of the humoral immune response.
- Elite controller
-
A rare population of HIV-infected individuals who can spontaneously control HIV replication in the absence of combination antiretroviral therapy.
- Cytokine storm
-
The excessive production of pro-inflammatory cytokines often induced by the over-activation of immune cells.
- Chimeric autoantibody receptors
-
(CAARs). Chimeric antigen receptor-like receptors whose extracellular domain consists of the protein target of a B cell-mediated autoimmune response.
- Pemphigus vulgaris
-
An antibody-mediated autoimmune disease that causes blistering of the skin.
- Desmogleins
-
Components of cell–cell adhesion complexes that form desmosomes under antibody-mediated attack in patients with pemphigus vulgaris.
- Bystander suppression
-
The ability of a regulatory T (Treg) cell to suppress effector T cell responses directed at an antigen distinct from the antigen that stimulated the Treg cell.
- Treg cell-specific demethylated region
-
A conserved region of intron 1 of FOXP3 that is demethylated in cells that are stably committed to the regulatory T (Treg) cell lineage.
- Suicide switches
-
Engineered logic gates used as a safety mechanism that cause cells to undergo apoptosis when certain conditions are met. Many suicide switches activate in response to exogenous drugs.
- Infectious tolerance
-
A phenomenon by which regulatory T cell activation can impart suppressive activity to effector T cells.
Rights and permissions
About this article
Cite this article
Maldini, C.R., Ellis, G. & Riley, J.L. CAR T cells for infection, autoimmunity and allotransplantation. Nat Rev Immunol 18, 605–616 (2018). https://doi.org/10.1038/s41577-018-0042-2
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41577-018-0042-2
This article is cited by
-
Brain regulatory T cells
Nature Reviews Immunology (2024)
-
Biomaterials to enhance adoptive cell therapy
Nature Reviews Bioengineering (2024)
-
Co-opting signalling molecules enables logic-gated control of CAR T cells
Nature (2023)
-
CAR T therapy beyond cancer: the evolution of a living drug
Nature (2023)
-
Post-translational covalent assembly of CAR and synNotch receptors for programmable antigen targeting
Nature Communications (2023)