Abstract
Major histocompatibility complex-I (MHC-I) presents tumour antigens to CD8+ T cells and triggers anti-tumour immunity. Humans may have 30,000–60,000 long noncoding RNAs (lncRNAs). However, it remains poorly understood whether lncRNAs affect tumour immunity. Here, we identify a lncRNA, lncRNA inducing MHC-I and immunogenicity of tumour (LIMIT), in humans and mice. We found that IFNγ stimulated LIMIT, LIMIT cis-activated the guanylate-binding protein (GBP) gene cluster and GBPs disrupted the association between HSP90 and heat shock factor-1 (HSF1), thereby resulting in HSF1 activation and transcription of MHC-I machinery, but not PD-L1. RNA-guided CRISPR activation of LIMIT boosted GBPs and MHC-I, and potentiated tumour immunogenicity and checkpoint therapy. Silencing LIMIT, GBPs and/or HSF1 diminished MHC-I, impaired antitumour immunity and blunted immunotherapy efficacy. Clinically, LIMIT, GBP- and HSF1-signalling transcripts and proteins correlated with MHC-I, tumour-infiltrating T cells and checkpoint blockade response in patients with cancer. Together, we demonstrate that LIMIT is a cancer immunogenic lncRNA and the LIMIT–GBP–HSF1 axis may be targetable for cancer immunotherapy.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The RNA-seq data (GSE99299) and processed single-cell data (GSE123814) were obtained from Gene Expression Omnibus (GEO). The MS proteomics data (PXD006003) were obtained from PRIDE repository. The TCGA cancer datasets were obtained from UCSC Xena (http://xena.ucsc.edu/). The RNA-seq data and clinical information for immune checkpoint blockade clinical trials were provided by the respective corresponding authors. All raw data supporting the findings of this study are available from the corresponding author on request. Source data are provided with this paper.
References
Zou, W., Wolchok, J. D. & Chen, L. PD-L1 (B7-H1) and PD-1 pathway blockade for cancer therapy: mechanisms, response biomarkers, and combinations. Sci. Transl. Med. 8, 328rv324 (2016).
Schumacher, T. N. & Schreiber, R. D. Neoantigens in cancer immunotherapy. Science 348, 69–74 (2015).
Garcia-Lora, A., Algarra, I. & Garrido, F. MHC class I antigens, immune surveillance, and tumor immune escape. J. Cell. Physiol. 195, 346–355 (2003).
Festenstein, H. & Garrido, F. MHC antigens and malignancy. Nature 322, 502–503 (1986).
Garrido, F., Aptsiauri, N., Doorduijn, E. M., Garcia Lora, A. M. & van Hall, T. The urgent need to recover MHC class I in cancers for effective immunotherapy. Curr. Opin. Immunol. 39, 44–51 (2016).
Hon, C. C. et al. An atlas of human long non-coding RNAs with accurate 5′ ends. Nature 543, 199–204 (2017).
Mercer, T. R., Dinger, M. E. & Mattick, J. S. Long non-coding RNAs: insights into functions. Nat. Rev. Genet. 10, 155–159 (2009).
Ponting, C. P., Oliver, P. L. & Reik, W. Evolution and functions of long noncoding RNAs. Cell 136, 629–641 (2009).
Wilusz, J. E., Sunwoo, H. & Spector, D. L. Long noncoding RNAs: functional surprises from the RNA world. Genes Dev. 23, 1494–1504 (2009).
Kung, J. T., Colognori, D. & Lee, J. T. Long noncoding RNAs: past, present, and future. Genetics 193, 651–669 (2013).
Flynn, R. A. & Chang, H. Y. Long noncoding RNAs in cell-fate programming and reprogramming. Cell Stem Cell 14, 752–761 (2014).
Huarte, M. The emerging role of lncRNAs in cancer. Nat. Med. 21, 1253–1261 (2015).
Frankish, A. et al. GENCODE reference annotation for the human and mouse genomes. Nucleic Acids Res. 47, D766–D773 (2019).
Riaz, N. et al. Tumor and microenvironment evolution during immunotherapy with nivolumab. Cell 171, 934–949 (2017).
Hugo, W. et al. Genomic and transcriptomic features of response to anti-PD-1 therapy in metastatic melanoma. Cell 168, 542 (2017).
Van Allen, E. M. et al. Genomic correlates of response to CTLA-4 blockade in metastatic melanoma. Science 350, 207–211 (2015).
Nathanson, T. et al. Somatic mutations and neoepitope homology in melanomas treated with CTLA-4 blockade. Cancer Immunol. Res 5, 84–91 (2017).
Sui, J. et al. Systematic analyses of a novel lncRNA-associated signature as the prognostic biomarker for hepatocellular carcinoma. Cancer Med. https://doi.org/10.1002/cam4.1541 (2018).
Kaplan, D. H. et al. Demonstration of an interferon γ-dependent tumor surveillance system in immunocompetent mice. Proc. Natl Acad. Sci. USA 95, 7556–7561 (1998).
Fruh, K. & Yang, Y. Antigen presentation by MHC class I and its regulation by interferon γ. Curr. Opin. Immunol. 11, 76–81 (1999).
Dong, H. et al. Tumor-associated B7-H1 promotes T-cell apoptosis: a potential mechanism of immune evasion. Nat. Med. 8, 793–800 (2002).
Perez-Pinera, P. et al. RNA-guided gene activation by CRISPR-Cas9-based transcription factors. Nat. Methods 10, 973–976 (2013).
Lin, H. et al. Host expression of PD-L1 determines efficacy of PD-L1 pathway blockade-mediated tumor regression. J. Clin. Invest. 128, 805–815 (2018).
Sun, Q., Hao, Q. & Prasanth, K. V. Nuclear long noncoding RNAs: key regulators of gene expression. Trends Genet. 34, 142–157 (2018).
Cheng, Y. S., Colonno, R. J. & Yin, F. H. Interferon induction of fibroblast proteins with guanylate binding activity. J. Biol. Chem. 258, 7746–7750 (1983).
Kim, B. H. et al. Interferon-induced guanylate-binding proteins in inflammasome activation and host defense. Nat. Immunol. 17, 481–489 (2016).
Messeguer, X. et al. PROMO: detection of known transcription regulatory elements using species-tailored searches. Bioinformatics 18, 333–334 (2002).
Consortium, E. P. An integrated encyclopedia of DNA elements in the human genome. Nature 489, 57–74 (2012).
Dai, C. & Sampson, S. B. HSF1: guardian of proteostasis in cancer. Trends Cell Biol. 26, 17–28 (2016).
West, J. D., Wang, Y. & Morano, K. A. Small molecule activators of the heat shock response: chemical properties, molecular targets, and therapeutic promise. Chem. Res. Toxicol. 25, 2036–2053 (2012).
Zou, J., Guo, Y., Guettouche, T., Smith, D. F. & Voellmy, R. Repression of heat shock transcription factor HSF1 activation by HSP90 (HSP90 complex) that forms a stress-sensitive complex with HSF1. Cell 94, 471–480 (1998).
Dayalan Naidu, S. & Dinkova-Kostova, A. T. Regulation of the mammalian heat shock factor 1. FEBS J. 284, 1606–1627 (2017).
Whitesell, L. & Lindquist, S. L. HSP90 and the chaperoning of cancer. Nat. Rev. Cancer 5, 761–772 (2005).
Yost, K. E. et al. Clonal replacement of tumor-specific T cells following PD-1 blockade. Nat. Med. 25, 1251–1259 (2019).
Harel, M. et al. Proteomics of melanoma response to immunotherapy reveals mitochondrial dependence. Cell 179, 236–250 (2019).
Heward, J. A. & Lindsay, M. A. Long non-coding RNAs in the regulation of the immune response. Trends Immunol. 35, 408–419 (2014).
Flores-Concha, M. & Onate, A. A. Long non-coding RNAs in the regulation of the immune response and trained immunity. Front. Genet. 11, 718 (2020).
Schmitt, A. M. & Chang, H. Y. Long noncoding RNAs in cancer pathways. Cancer Cell 29, 452–463 (2016).
Sun, T. T. et al. LncRNA GClnc1 promotes gastric carcinogenesis and may act as a modular scaffold of WDR5 and KAT2A complexes to specify the histone modification pattern. Cancer Discov. 6, 784–801 (2016).
Sharma, P., Hu-Lieskovan, S., Wargo, J. A. & Ribas, A. Primary, adaptive, and acquired resistance to cancer immunotherapy. Cell 168, 707–723 (2017).
Peng, D. et al. Epigenetic silencing of TH1-type chemokines shapes tumour immunity and immunotherapy. Nature 527, 249–253 (2015).
Wang, W. et al. CD8+ T cells regulate tumour ferroptosis during cancer immunotherapy. Nature 569, 270–274 (2019).
Gao, J. et al. Loss of IFN-γ pathway genes in tumor cells as a mechanism of resistance to anti-CTLA-4 therapy. Cell 167, 397–404 (2016).
Zaretsky, J. M. et al. Mutations associated with acquired resistance to PD-1 blockade in melanoma. N. Engl. J. Med. 375, 819–829 (2016).
Manguso, R. T. et al. In vivo CRISPR screening identifies Ptpn2 as a cancer immunotherapy target. Nature 547, 413–418 (2017).
Shin, D. S. et al. Primary resistance to PD-1 blockade mediated by JAK1/2 mutations. Cancer Discov. 7, 188–201 (2017).
Sucker, A. et al. Acquired IFNγ resistance impairs anti-tumor immunity and gives rise to T-cell-resistant melanoma lesions. Nat. Commun. 8, 15440 (2017).
Li, J. et al. Epigenetic driver mutations in ARID1A shape cancer immune phenotype and immunotherapy. J. Clin. Invest. https://doi.org/10.1172/JCI134402 (2020).
Benci, J. L. et al. Tumor interferon signaling regulates a multigenic resistance program to immune checkpoint blockade. Cell 167, 1540–1554 (2016).
Arun, G., Diermeier, S. D. & Spector, D. L. Therapeutic targeting of long non-coding RNAs in cancer. Trends Mol. Med. 24, 257–277 (2018).
Gil, N. & Ulitsky, I. Regulation of gene expression by cis-acting long non-coding RNAs. Nat. Rev. Genet. 21, 102–117 (2020).
Jones, A. N. & Sattler, M. Challenges and perspectives for structural biology of lncRNAs-the example of the Xist lncRNA A-repeats. J. Mol. Cell. Biol. 11, 845–859 (2019).
Shenoy, A. R. et al. GBP5 promotes NLRP3 inflammasome assembly and immunity in mammals. Science 336, 481–485 (2012).
Tretina, K., Park, E. S., Maminska, A. & MacMicking, J. D. Interferon-induced guanylate-binding proteins: guardians of host defense in health and disease. J. Exp. Med. 216, 482–500 (2019).
Yamamoto, M. et al. A cluster of interferon-γ-inducible p65 GTPases plays a critical role in host defense against Toxoplasma gondii. Immunity 37, 302–313 (2012).
Mbofung, R. M. et al. HSP90 inhibition enhances cancer immunotherapy by upregulating interferon response genes. Nat. Commun. 8, 451 (2017).
Proia, D. A. & Kaufmann, G. F. Targeting heat-shock protein 90 (HSP90) as a complementary strategy to immune checkpoint blockade for cancer therapy. Cancer Immunol. Res. 3, 583–589 (2015).
Yuno, A. et al. Clinical evaluation and biomarker profiling of Hsp90 inhibitors. Methods Mol. Biol. 1709, 423–441 (2018).
Charo, J. et al. Bcl-2 overexpression enhances tumor-specific T-cell survival. Cancer Res. 65, 2001–2008 (2005).
Owaki, H. et al. Raf-1 is required for T cell IL2 production. EMBO J. 12, 4367–4373 (1993).
Acknowledgements
We thank members of the Zou laboratory for intellectual input. This work was supported in part by the research grants from the US NIH/NCI R01 grants (CA217648, CA123088, CA099985, CA193136, CA152470, to W.Z.; and CA216919, CA213566, CA120458; to M. Cohen), and the NIH through the University of Michigan Rogel Cancer Center Grant (CA46592).
Author information
Authors and Affiliations
Contributions
G.L. and W.Z. conceived the idea, designed the experiments and composed the paper. G.L. conducted experiments. I.K. assisted in FACS analysis. J.N., S.W., S.G. and L.V. assisted in animal experiments. X.L., S.L. and J.L. assisted in bioinformatics analysis. J.Z., W.D., H.L., T.W., C.S., J.J.M., M. Cieslik and M. Cohen contributed to the interpretation of the results. W.Z. supervised the project.
Corresponding author
Ethics declarations
Competing interests
W.Z. has served as a scientific advisor or consultant for NGM, Cstone, Oncopia and Hengenix. All of the other authors declare no competing interests.
Additional information
Peer review information Nature Cell Biology thanks Weiyi Peng and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 LIMIT correlates to effector immune genes across multiple cancer types.
a-l, Correlation of LIMIT with IFNG, MHC-I, or CD8 in human patients with sarcoma (SARC) (a-c), colon cancer (COAD) (d-f), breast cancer (BRCA) (g-i), and kidney cancer (KIRC) (j-l). P value by 2 sided linear regression. Source data are provided.
Extended Data Fig. 2 Genetic loci and sequences of human LIMIT and mouse Limit.
a-b, Genetic locus and genomic sequence of human LIMIT (a) or mouse Limit (b). c, Blast alignment of human LIMIT with GBP1P1 or GBP1.
Extended Data Fig. 3 LIMIT augments MHC-I expression.
a, Schematic diagram showing the alignment among LIMIT, GBP, and shLIMIT. The shLIMIT target sequences are not present in GBP coding genes. b, A375 shFluc, shLIMIT a, and shLIMIT b cells were treated with IFNγ for 48 hours. Surface expression of PD-L1 was determined by flow cytometry (FACS). mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. c, A375 shFluc and shLIMIT cells were treated with IFNγ for 24 hours. RNA levels of indicated genes were determined. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. d, Schematic diagram of the LIMIT promoter. The locations of 5 STAT1/IRF1-binding motifs and 4 sgRNAs capable of deleting the STAT1/IRF1 binding sites are indicated. Source data are provided.
Extended Data Fig. 4 LIMIT augments MHC-I expression.
a, Schematic diagram of CRISPR activation targeting Limit. The transcriptional activator VPR was directed to the promoter of Limit by the interaction between guide RNAs and dCas9. b-c, B16 cells were transfected with dCas9-VPR alone or together with 4 sgRNAs. Subsequently, RNA levels of Limit (b) and surface expression of MHC-I (H2-Db) (c) were detected 24 and 48 hours post transfection, respectively. mean ± SD, n = 4 biological independent samples, P value by 2-sided t-test. d, B16-OVA cells stably expressing shFluc, shB2m a, and shB2m b were treated with IFNγ for 48 hours. Surface expression of OVA-H2Kb were determined by FACS. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. e, B16-OVA cells were co-cultured with OT-I cell for 48 hours. Dot plots show the CD45− tumor cells. Tumor cell death was determined by PI staining. f-g, B16-OVA cells carrying shFluc or shB2m were co-cultured with OT-I cells at a 1:4 ratio. Cell killing was determined by PI+ in CD45− tumor cells. Dot plots (f) and statistical results (g) are shown. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. h-i, Bone marrow derived dendritic cells (BMDC) (h) or macrophages (BMDM) (i) were treated with IFNγ for 24 hours. RNA levels of Limit were determined by qRT-PCR. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. j, BMDM were transfected with 5’FAM-labbled siRNA targeting Fluc or Limit. Dot plots show FSC vs. SSC and FITC vs. SSC gating. The FITC gating indicates the cells with positive siRNA transfection. 1 of 3 experiments is shown. k, BMDM were transfected with 5’FAM-labbled siRNA targeting Fluc or Limit, and treated with IFNγ for 48 hours. Surface expression of MHC-I (H2-Db) were determined by FACS. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. Source data are provided.
Extended Data Fig. 5 LIMIT augments antigen-loaded MHC-I expression in vivo.
a, YUMM1.7-OVA cells carrying shFluc or shLimit were treated with IFNγ for 48 hours. Surface expression of OVA-H2Kb were determined by FACS. mean ± SD, n = 5 biological independent samples, P value by 2-sided t-test for end point tumor volume. b, Dot plot showing the CD45− gating of YUMM1.7-OVA tumor cells. c-d, Representative histogram showing the expression of H2Db (c) or OVA-H2Kb (d) in YUMM1.7-OVA shFluc or shLimit tumor cells. e-f, Statistical results of H2Db expression (e) or OVA-H2Kb expression (f) in YUMM1.7-OVA shFluc or shLimit tumor cells. mean ± SD, n = 5 biological independent samples, P value by 2-sided t-test. Source data are provided.
Extended Data Fig. 6 LIMIT cis-activates GBPs to boost MHC-I and tumor immunity.
a-b, Fold changes of Limit expression upon IFNγ treatment in YUMM1.7 cells (a) or CT26 cells (b) stably carrying shFluc, shLimit a, or shLimit b. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. c, A375 cells were transfected with LIMIT cDNA for 24 hours. RNA levels of indicated genes were determined by qRT-PCR. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. d, RPKM of Gbp family members upon IFNγ treatment in B16 cells (GSE99299). mean ± SD, n = 3 biological independent samples. e, A375 shFluc or shLIMIT cells were overexpressed with GBP1 (GBP1OE), and treated with IFNγ for 48 hours. Surface expression of HLA-ABC or PD-L1 were determined by FACS. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. f, A375 shFluc or shLIMIT cells were overexpressed with GBP1 (GBP1OE), and treated with IFNγ for 24 hours. RNA levels of IRF1 were determined by qRT-PCR. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. g, Dot plots of intral-tumoral CD8+ T cell infiltration and activation in the YUMM1.7 tumors carrying shFluc, shLimit, shGbp2, or shLimit plus shGbp2. h-i, Correlations between GBP1-5 and LIMIT (h) or MHC-I (i) in human melanoma datasets. P value by 2 sided linear regression. j, Cancer patients having received ICB were divided into low and high GBP groups (bottom 15% vs top 15%). The response rates to ICB were calculated as the percentages of partial response (PR) plus complete response (CR). P value by Chi-square test. Patients were from 4 cohorts. k, Survival plot of patients with melanoma. Based on the expression levels of GBP1-5, patients were divided into high (top 50%) and low (bottom 50%) groups. P value by 2 sided log-rank test. Source data are provided.
Extended Data Fig. 7 GBPs activate HSF1 to stimulate MHC-I expression.
a, Prediction of potential transcription factors targeting HLA-ABC, TAP1, HSPA5 and CALR. 8 shared transcription factors were altered by IFNγ in A375 cells (GSE99299). b, ChIP-seq results of STAT1 (Hela-S3 cells treated with IFNγ) or HSF1 (HepG2 cells in basal condition) derived from ENCODE at UCSC. The enrichment of STAT1 or HSF1 in the promoters of MHC-I related genes are shown. c, A375 cells were treated with multiple proteostasis stressors and KRIBB11. Surface expression of HLA-ABC was determined 48 hours after treatment. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. d, Dot plots of IFNγ+CD8+ T cells or TNFα+CD8+ T cells in MC38 tumors carrying shFluc, shGbp2, shHsf1, and shGbp2 plus shHsf1. Source data are provided.
Extended Data Fig. 8 HSF1 drives MHC-I expression and tumor immunity.
a, B16-OVA cells were treated with IFNγ in the presence or absence of KRIBB11 for 48 hours. Cell surface expression of OVA-H2-Kb was determined by FACS. mean ± SD, n = 4 biological independent samples, P value by 2-sided t-test. b, B16-OVA cells were pretreated with IFNγ in the presence or absence of KRIBB11 for 48 hours, then cultured with OT-1 T cells. Cell death was determined by 7-AAD staining in the CD45- tumor cells. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. c, MHC-I (H2-Dd) surface staining of CT26 shFluc or shHsf1 cells treated with IFNγ for 48 hours. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. d, YUMM1.7 shFluc or shHsf1 cells were treated with IFNγ in the presence or absence of KRIBB11 for 48 hours. Surface expression of MHC-I (H2-Db) was determined by FACS. mean ± SD, n = 3 biological independent samples, P value by 2-sided t-test. e, Dot plots of CD3+, Ki67+, IFNγ+, and TNFα+ T cells in YUMM1.7 shFluc or shHsf1 tumors. f, Tumor growth curve of CT26 shFluc or shHsf1 tumors in BALB/c mice. mean ± SD, n = 6 animals, P value by 2-sided t-test for end point tumor volume. g, Percentages of CD3+, IFNγ+, TNFα+, and Ki67+ T cells in CT26 shFluc or shHsf1 tumors. mean ± SD, n = 5 biological independent samples, P value by 2-sided t-test. h, Dot plots of CD3+, Ki67+, IFNγ+, and TNFα+ T cells in CT26 shFluc or shHsf1 tumors. Source data are provided.
Extended Data Fig. 9 LIMIT-GBP-HSF1 axis drives MHC-I and tumor immunity and immunotherapy.
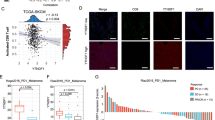
a-b, HSF1 signaling genes correlated with MHC-I expression (a) or CD8+ T cell infiltration (b) in Pan-Cancer (TCGA, PANCAN), melanoma (TCGA, SKCM) or sarcoma (TCGA, SARC). P value by 2-sided t-test. The minima, 25% percentile, median, 75% percentile, maxima for each blot are (a) (31.53, 40.0075, 42.87, 45.4925, 53.58), (32.02, 41.1175, 43.66, 46.205, 55), (31.82, 39.785, 43.16, 46.31, 50.39), (33.35, 42.215, 44.53, 47.55, 53.41), (32.9, 38.88, 41.19, 43.21, 47.55), (39.33, 44.75, 46.57, 48.4, 51.3); (b) (3.75, 15.6825, 23.6, 30.48, 49.23), (5.47, 19.5875, 24, 29.1525, 45.42), (7.711, 15.7925, 23.415, 29.7395, 39.722), (4.9254, 18.95, 27.857, 34.862, 47.79), (7.7582, 14.727, 18.553, 22.16, 36.084), (15.024, 22.149, 29.1, 35.582, 43.432). c, Survival plots of human melanoma patients (TCGA, SKCM). Based on the expression of HSF1 signaling genes, patients were divided into high (n = 150 patients) and low (n = 150 patients) groups. P value by 2-sided log-rank test. d, Single cell RNA-seq derived cell clusters pre- or post- anti-PD-1 therapy in human skin basal cell carcinoma. Two malignant clusters are denoted by color and show different sensitivities to PD-1 blockade. e, Expression of HSF1 signaling genes and MHC-I related genes in the single cell clusters prior to PD-1 blockade therapy. The therapy sensitive tumor cell cluster exhibited higher levels of HSF1 signaling genes and MHC-I related genes as compared to the therapy insensitive tumor cell cluster. f, Proteomics analysis in melanoma patients having received ICB. Protein expression of GBPs, HSF1 signaling genes, and HLA-ABC were compared in responders (R, n = 40 patients) and non-responders (NR, n = 27 patients). P value by 2-sided t-test. g, Based on the transcript levels of GBP1, human Pan-Cancers were divided into high (top 10%) and low (bottom 10%) groups. HSF1 target gene transcripts were plotted. mean ± SD, n = 1106 patients, P value by 2-sided t-test. The minima, 25% percentile, median, 75% percentile, maxima for each blot are (9.12, 12.29, 13.01, 13.8075, 18.2), (9.24, 12.73, 13.47, 14.19, 19.16), (5.32, 9.64, 10.625, 11.39, 15.74), (6.98, 10.365, 11.11, 11.78, 16.96), (10.86, 12.83, 13.59, 14.16, 16.68), (11.75, 13.77, 14.16, 14.5, 16.71), (10.57, 13.11, 13.84, 14.48, 16.33), (12.15, 13.96, 14.3, 14.71, 17.76). Source data are provided.
Extended Data Fig. 10 Scheme showing how LIMIT-GBP-HSF1 axis affects MHC-I and tumor immunity.
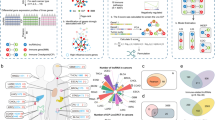
Cancer cells (or APCs) express LIMIT in response to IFNγ, thereby locally promoting the transcription of GBPs. GBPs interact with HSP90 and release HSP90-decoyed HSF1, resulting in HSF1 activation. Activated HSF1 stimulates the transcription of MHC-I and MHC-I related genes. MHC-I machinery mediates TAA-recognition and T cell activation, eliciting antitumor immune response.
Supplementary information
Supplementary Tables
Supplementary Table 1: lncRNA expression in hot versus cold melanoma. Supplementary Table 2: sequence alignment between LIMIT and GBP1P1. Supplementary Table 3: predictive targets of shLIMIT a by NCBI BLAST. Supplementary Table 4: predictive targets of shLIMIT b by NCBI BLAST. Supplementary Table 5: predictive targets of shLimit a by NCBI BLAST. Supplementary Table 6: predictive targets of shLimit b by NCBI BLAST. Supplementary Table 7: target sequences for linker DNA, sgRNA, shRNA or probes. Supplementary Table 8: primer sequences for RACE, Clone or RT–PCR
Source data
Source Data Fig. 1
Statistical source data.
Source Data Fig. 1
Unprocessed gel/blots.
Source Data Fig. 2
Statistical source data.
Source Data Fig. 2
Unprocessed gel/blots.
Source Data Fig. 3
Statistical source data.
Source Data Fig. 4
Statistical source data.
Source Data Fig. 4
Unprocessed gel/blots.
Source Data Fig. 5
Statistical source data.
Source Data Fig. 5
Unprocessed gel/blots.
Source Data Fig. 6
Statistical source data.
Source Data Fig. 6
Unprocessed gel/blots.
Source Data Extended Data Fig. 1
Statistical source data.
Source Data Extended Data Fig. 3
Statistical source data.
Source Data Extended Data Fig. 4
Statistical source data.
Source Data Extended Data Fig. 5
Statistical source data.
Source Data Extended Data Fig. 6
Statistical source data.
Source Data Extended Data Fig. 7
Statistical source data.
Source Data Extended Data Fig. 8
Statistical source data.
Source Data Extended Data Fig. 9
Statistical source data.
Rights and permissions
About this article
Cite this article
Li, G., Kryczek, I., Nam, J. et al. LIMIT is an immunogenic lncRNA in cancer immunity and immunotherapy. Nat Cell Biol 23, 526–537 (2021). https://doi.org/10.1038/s41556-021-00672-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41556-021-00672-3
This article is cited by
-
Aristolochic acids-hijacked p53 promotes liver cancer cell growth by inhibiting ferroptosis
Acta Pharmacologica Sinica (2024)
-
Long non-coding RNAs in cancer: multifaceted roles and potential targets for immunotherapy
Molecular and Cellular Biochemistry (2024)
-
The role of LncRNAs in tumor immunotherapy
Cancer Cell International (2023)
-
Bioinformatics construction and experimental validation of a cuproptosis-related lncRNA prognostic model in lung adenocarcinoma for immunotherapy response prediction
Scientific Reports (2023)
-
The complementarity of DDR, nucleic acids and anti-tumour immunity
Nature (2023)