Abstract
The genetic modification of T cells has advanced cellular immunotherapies, yet the delivery of biologics specifically to T cells remains challenging. Here we report a suite of methods for the genetic engineering of cells to produce extracellular vesicles (EVs)—which naturally encapsulate and transfer proteins and nucleic acids between cells—for the targeted delivery of biologics to T cells without the need for chemical modifications. Specifically, the engineered cells secreted EVs that actively loaded protein cargo via a protein tag and that displayed high-affinity T-cell-targeting domains and fusogenic glycoproteins. We validated the methods by engineering EVs that delivered Cas9–single-guide-RNA complexes to ablate the gene encoding the C-X-C chemokine co-receptor type 4 in primary human CD4+ T cells. The strategy is amenable to the targeted delivery of biologics to other cell types.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
All reported experimental data and plasmid maps for all plasmids generated in this study are freely available at Zenodo (https://doi.org/10.5281/zenodo.10022991). Key plasmids used in this study are distributed by Addgene, with complete and annotated GenBank files available at https://www.addgene.org/Joshua_Leonard. The raw and analysed datasets generated during the study are available for research purposes from the corresponding author on reasonable request.
Code availability
The code for analysing HTS data is available at https://github.com/leonardlab/GEMINI-HTS under an open-source license.
References
Sadelain, M., Rivière, I. & Riddell, S. Therapeutic T cell engineering. Nature 545, 423–431 (2017).
Yin, C. et al. In vivo excision of HIV-1 provirus by saCas9 and multiplex single-guide RNAs in animal models. Mol. Ther. 25, 1168–1186 (2017).
Kaminski, R. et al. Excision of HIV-1 DNA by gene editing: a proof-of-concept in vivo study. Gene Ther. 23, 690–695 (2016).
Dash, P. K. et al. Sequential LASER ART and CRISPR treatments eliminate HIV-1 in a subset of infected humanized mice. Nat. Commun. 10, 2753 (2019).
Louis Jeune, V., Joergensen, J. A., Hajjar, R. J. & Weber, T. Pre-existing anti-adeno-associated virus antibodies as a challenge in AAV gene therapy. Hum. Gene Ther. Methods 24, 59–67 (2013).
Zincarelli, C., Soltys, S., Rengo, G. & Rabinowitz, J. E. Analysis of AAV serotypes 1–9 mediated gene expression and tropism in mice after systemic injection. Mol. Ther. 16, 1073–1080 (2008).
Hamilton, J. R. et al. Targeted delivery of CRISPR–Cas9 and transgenes enables complex immune cell engineering. Cell Rep. 35, 109207 (2021).
Banskota, S. et al. Engineered virus-like particles for efficient in vivo delivery of therapeutic proteins. Cell 185, 250–265 (2022).
Segel, M. et al. Mammalian retrovirus-like protein PEG10 packages its own mRNA and can be pseudotyped for mRNA delivery. Science 373, 882–889 (2021).
Otten, G. R. et al. Potent immunogenicity of an HIV-1 gag-pol fusion DNA vaccine delivered by in vivo electroporation. Vaccine 24, 4503–4509 (2006).
Rurik, J. G. et al. CAR T cells produced in vivo to treat cardiac injury. Science 375, 91–96 (2022).
Luther, D. C., Lee, Y. W., Nagaraj, H., Scaletti, F. & Rotello, V. M. Delivery approaches for CRISPR/Cas9 therapeutics in vivo: advances and challenges. Expert Opin. Drug Deliv. 15, 905–913 (2018).
Liu, C., Zhang, L., Liu, H. & Cheng, K. Delivery strategies of the CRISPR–Cas9 gene-editing system for therapeutic applications. J. Control. Release 266, 17–26 (2017).
Dardalhon, V. et al. Lentivirus-mediated gene transfer in primary T cells is enhanced by a central DNA flap. Gene Ther. 8, 190–198 (2001).
Valadi, H. et al. Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat. Cell Biol. 9, 654–659 (2007).
Soderberg, A., Barral, A. M., Soderstrom, M., Sander, B. & Rosen, A. Redox-signaling transmitted in trans to neighboring cells by melanoma-derived TNF-containing exosomes. Free Radic. Biol. Med. 43, 90–99 (2007).
Alvarez-Erviti, L. et al. Delivery of siRNA to the mouse brain by systemic injection of targeted exosomes. Nat. Biotechnol. 29, 341–345 (2011).
Arslan, F. et al. Mesenchymal stem cell-derived exosomes increase ATP levels, decrease oxidative stress and activate PI3K/Akt pathway to enhance myocardial viability and prevent adverse remodeling after myocardial ischemia/reperfusion injury. Stem Cell Res. 10, 301–312 (2013).
Ohno, S. et al. Systemically injected exosomes targeted to EGFR deliver antitumor microRNA to breast cancer cells. Mol. Ther. 21, 185–191 (2013).
Kojima, R. et al. Designer exosomes produced by implanted cells intracerebrally deliver therapeutic cargo for Parkinson’s disease treatment. Nat. Commun. 9, 1305 (2018).
He, C. et al. Epithelial cell-derived microvesicles: a safe delivery platform of CRISPR/Cas9 conferring synergistic anti-tumor effect with sorafenib. Exp. Cell. Res. 392, 112040 (2020).
Chen, R. et al. Friend or foe? Evidence indicates endogenous exosomes can deliver functional gRNA and Cas9 protein. Small 15, e1902686 (2019).
Yao, X. et al. Engineered extracellular vesicles as versatile ribonucleoprotein delivery vehicles for efficient and safe CRISPR genome editing. J. Extracell. Vesicles 10, e12076 (2021).
McConnell, R., Y. M. & Finn, J. In International Society for Extracellular Vesicles (Taylor & Francis Online, 2022).
Kooijmans, S. A. et al. Electroporation-induced siRNA precipitation obscures the efficiency of siRNA loading into extracellular vesicles. J. Control. Release 172, 229–238 (2013).
Théry, C. et al. Minimal information for studies of extracellular vesicles 2018 (MISEV2018): a position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. J. Extracell. Vesicles 7, 1535750 (2018).
Knipping, F. et al. Disruption of HIV-1 co-receptors CCR5 and CXCR4 in primary human T cells and hematopoietic stem and progenitor cells using base editing. Mol. Ther. 30, 130–144 (2022).
Li, S., Holguin, L. & Burnett, J. C. CRISPR-Cas9-mediated gene disruption of endogenous co-receptors confers broad resistance to HIV-1 in human primary cells and humanized mice. Mol. Ther. Methods in Clin. Dev. 24, 321–331 (2022).
Stranford, D. M., Hung, M. E., Gargus, E. S., Shah, R. N. & Leonard, J. N. A systematic evaluation of factors affecting extracellular vesicle uptake by breast cancer cells. Tissue Eng. Part A 23, 1274–1282 (2017).
Longatti, A. et al. High affinity single-chain variable fragments are specific and versatile targeting motifs for extracellular vesicles. Nanoscale 10, 14230–14244 (2018).
Wang, J. H. et al. Anti-HER2 scFv-directed extracellular vesicle-mediated mRNA-based gene delivery inhibits growth of HER2-positive human breast tumor xenografts by prodrug activation. Mol. Cancer Ther. 17, 1133–1142 (2018).
Kooijmans, S. A. et al. Display of GPI-anchored anti-EGFR nanobodies on extracellular vesicles promotes tumour cell targeting. J. Extracell. Vesicles 5, 31053 (2016).
Connelly, R. J. et al. Mitogenic properties of a bispecific single-chain Fv-–Ig fusion generated from CD2-specific mAb to distinct epitopes. Int. Immunol. 10, 1863–1872 (1998).
Telerman, A. et al. Internalization of human T lymphocyte receptors. Eur. J. Immunol. 17, 991–997 (1987).
Chang, Z. L. et al. Rewiring T-cell responses to soluble factors with chimeric antigen receptors. Nat. Chem. Biol. 14, 317–324 (2018).
Thery, C., Amigorena, S., Raposo, G. & Clayton, A. Isolation and characterization of exosomes from cell culture supernatants and biological fluids. Curr. Protoc. Cell Biol. Chapter 3, Unit 3.22 (2006).
Jeppesen, D. K. et al. Comparative analysis of discrete exosome fractions obtained by differential centrifugation. J. Extracell. Vesicles 3, 25011 (2014).
Verweij, F. J. et al. The power of imaging to understand extracellular vesicle biology in vivo. Nat. Methods 18, 1013–1026 (2021).
Simonsen, J. B. Pitfalls associated with lipophilic fluorophore staining of extracellular vesicles for uptake studies. J. Extracell. Vesicles 8, 1582237 (2019).
Hung, M. E. & Leonard, J. N. A platform for actively loading cargo RNA to elucidate limiting steps in EV-mediated delivery. J. Extracell. Vesicles 5, 31027 (2016).
Bu, J. et al. An avidity-based PD-L1 antagonist using nanoparticle–antibody conjugates for enhanced immunotherapy. Nano Lett. 20, 4901–4909 (2020).
Raab, D., Graf, M., Notka, F., Schödl, T. & Wagner, R. The GeneOptimizer Algorithm: using a sliding window approach to cope with the vast sequence space in multiparameter DNA sequence optimization. Syst. Synth. Biol. 4, 215–225 (2010).
Kooijmans, S. A. A., Gitz-Francois, J., Schiffelers, R. M. & Vader, P. Recombinant phosphatidylserine-binding nanobodies for targeting of extracellular vesicles to tumor cells: a plug-and-play approach. Nanoscale 10, 2413–2426 (2018).
Yim, N. et al. Exosome engineering for efficient intracellular delivery of soluble proteins using optically reversible protein–protein interaction module. Nat. Commun. 7, 12277 (2016).
Heath, N. et al. Endosomal escape enhancing compounds facilitate functional delivery of extracellular vesicle cargo. Nanomedicine 14, 2799–2814 (2019).
Putyrski, M. & Schultz, C. Protein translocation as a tool: the current rapamycin story. FEBS Lett. 586, 2097–2105 (2012).
Gao, Y. et al. Complex transcriptional modulation with orthogonal and inducible dCas9 regulators. Nat. Methods 13, 1043–1049 (2016).
Maggio, I. et al. Integrating gene delivery and gene-editing technologies by adenoviral vector transfer of optimized CRISPR–Cas9 components. Gene Ther. 27, 209–225 (2020).
de Jong, O. G. et al. A CRISPR–Cas9-based reporter system for single-cell detection of extracellular vesicle-mediated functional transfer of RNA. Nat. Commun. 11, 1113 (2020).
Hung, M. E., Lenzini, S. B., Stranford, D. M. & Leonard, J. N. Enrichment of extracellular vesicle subpopulations via affinity chromatography. Methods Mol. Biol. 1740, 109–124 (2018).
Somiya, M. & Kuroda, S. Real-time luminescence assay for cytoplasmic cargo delivery of extracellular vesicles. Anal. Chem. 93, 5612–5620 (2021).
Mangeot, P. E. et al. Protein transfer into human cells by VSV-G-induced nanovesicles. Mol. Ther. 19, 1656–1666 (2011).
Cronin, J., Zhang, X.-Y. & Reiser, J. Altering the tropism of lentiviral vectors through pseudotyping. Curr. Gene Ther. 5, 387–398 (2005).
Frecha, C. et al. Stable transduction of quiescent T cells without induction of cycle progression by a novel lentiviral vector pseudotyped with measles virus glycoproteins. Blood 112, 4843–4852 (2008).
Frecha, C. et al. Measles virus glycoprotein-pseudotyped lentiviral vector-mediated gene transfer into quiescent lymphocytes requires binding to both SLAM and CD46 entry receptors. J. Virol. 85, 5975–5985 (2011).
Karampetsou, M. P., Comte, D., Kis-Toth, K., Kyttaris, V. C. & Tsokos, G. C. Expression patterns of signaling lymphocytic activation molecule family members in peripheral blood mononuclear cell subsets in patients with systemic lupus erythematosus. PLoS ONE 12, e0186073 (2017).
Hashiguchi, T., Maenaka, K. & Yanagi, Y. Measles virus hemagglutinin: structural insights into cell entry and measles vaccine. Front. Microbiol. 2, 247 (2011).
Gonçalves-Carneiro, D., McKeating, J. A. & Bailey, D. The measles virus receptor SLAMF1 can mediate particle endocytosis. J. Virol. 91, e02255-16 (2017).
Soares, A. R. et al. Gap junctional protein Cx43 is involved in the communication between extracellular vesicles and mammalian cells. Sci. Rep. 5, 13243 (2015).
Schumann, K. et al. Generation of knock-in primary human T cells using Cas9 ribonucleoproteins. Proc. Natl Acad. Sci. USA 112, 10437–10442 (2015).
Hultquist, J. F. et al. A Cas9 ribonucleoprotein platform for functional genetic studies of HIV–host interactions in primary human T cells. Cell Rep. 17, 1438–1452 (2016).
Liu, S. et al. HIV-1 inhibition in cells with CXCR4 mutant genome created by CRISPR–Cas9 and piggyBac recombinant technologies. Sci. Rep. 8, 8573 (2018).
Zhu, X. et al. Comprehensive toxicity and immunogenicity studies reveal minimal effects in mice following sustained dosing of extracellular vesicles derived from HEK293T cells. J. Extracell. Vesicles 6, 1324730 (2017).
Hultquist, J. F. et al. CRISPR–Cas9 genome engineering of primary CD4(+) T cells for the interrogation of HIV–host factor interactions. Nat. Protoc. 14, 1–27 (2019).
Modarai, S. R., Kanda, S., Bloh, K., Opdenaker, L. M. & Kmiec, E. B. Precise and error-prone CRISPR-directed gene editing activity in human CD34+ cells varies widely among patient samples. Gene Ther. 28, 105–113 (2021).
Breuer, C. B. et al. In vivo engineering of lymphocytes after systemic exosome-associated AAV delivery. Sci. Rep. 10, 4544 (2020).
Shrivastava, S. et al. Exosome-mediated stable epigenetic repression of HIV-1. Nat. Commun. 12, 5541 (2021).
Cheng, Q. et al. Reprogramming exosomes as nanoscale controllers of cellular immunity. J. Am. Chem. Soc. 140, 16413–16417 (2018).
Campbell, L. A. et al. Gesicle-mediated delivery of CRISPR/Cas9 ribonucleoprotein complex for inactivating the HIV provirus. Mol. Ther. 27, 151–163 (2019).
Sterzenbach, U. et al. Engineered exosomes as vehicles for biologically active proteins. Mol. Ther. 25, 1269–1278 (2017).
Dooley, K. et al. A versatile platform for generating engineered extracellular vesicles with defined therapeutic properties. Mol. Ther. 29, 1729–1743 (2021).
Levy, C. et al. Lentiviral vectors displaying modified measles virus gp overcome pre-existing immunity in in vivo-like transduction of human T and B cells. Mol. Ther. 20, 1699–1712 (2012).
Hendel, A. et al. Chemically modified guide RNAs enhance CRISPR–Cas genome editing in human primary cells. Nat. Biotechnol. 33, 985–989 (2015).
Cornu, T. I., Mussolino, C., Bloom, K. & Cathomen, T. Editing CCR5: a novel approach to HIV gene therapy. Adv. Exp. Med. Biol. 848, 117–130 (2015).
Zou, X. et al. Extracellular vesicles expressing a single-chain variable fragment of an HIV-1 specific antibody selectively target Env(+) tissues. Theranostics 9, 5657–5671 (2019).
Wang, S., Beattie, G. M., Hayek, A. & Levine, F. Development of a VSV-G protein pseudotyped retroviral vector system expressing dominant oncogenes from a lacO-modified inducible LTR promoter. Gene 182, 145–150 (1996).
Yoshida, Y., Emi, N. & Hamada, H. VSV-G-pseudotyped retroviral packaging through adenovirus-mediated inducible gene expression. Biochem. Biophys. Res. Commun. 232, 379–382 (1997).
Sanjana, N. E., Shalem, O. & Zhang, F. Improved vectors and genome-wide libraries for CRISPR screening. Nat. Methods 11, 783–784 (2014).
Ai, H. W., Shaner, N. C., Cheng, Z., Tsien, R. Y. & Campbell, R. E. Exploration of new chromophore structures leads to the identification of improved blue fluorescent proteins. Biochemistry 46, 5904–5910 (2007).
Daringer, N. M., Dudek, R. M., Schwarz, K. A. & Leonard, J. N. Modular extracellular sensor architecture for engineering mammalian cell-based devices. ACS Synth. Biol. 3, 892–902 (2014).
Atasoy, D., Aponte, Y., Su, H. H. & Sternson, S. M. A FLEX switch targets Channelrhodopsin-2 to multiple cell types for imaging and long-range circuit mapping. J. Neurosci. 28, 7025–7030 (2008).
Heredia, J. D. et al. Mapping interaction sites on human chemokine receptors by deep mutational scanning. J. Immunol. 200, 3825–3839 (2018).
Shen, Y., Rosendale, M., Campbell, R. E. & Perrais, D. pHuji, a pH-sensitive red fluorescent protein for imaging of exo- and endocytosis. J. Cell Biol. 207, 419–432 (2014).
Cong, L. et al. Multiplex genome engineering using CRISPR/Cas systems. Science 339, 819–823 (2013).
Anders, C. & Jinek, M. In vitro enzymology of Cas9. Methods Enzymol. 546, 1–20 (2014).
Acknowledgements
We thank R. D’Aquila for his support and guidance in starting this project. We thank I. Clerc for her assistance with the measles virus glycoproteins. J.N.L. discloses support for the research described in this study from Third Coast Center for AIDS Research, an NIH-funded centre (P30 AI117943), NIH grants R01AI165236 and R01AI150998 (J.F.H.), National Science Foundation (NSF) award 1844219 (J.N.L. and N. P. Kamat), Kairos Ventures (gift), and Syenex. This work was also supported by NSF Graduate Research Fellowship awards DGE-1324585 (to D.M.S.) and DGE-1842165 (to B.N.D.). Sanger sequencing was performed through the Northwestern University Sequencing Core (NUSeq) Core Facility of Northwestern’s Center for Genetic Medicine and a partnership with ACGT. NanoSight analysis was performed in the Analytical bioNanoTechnology Core Facility (ANTEC) of the Simpson Querrey Institute at Northwestern University. ANTEC is currently supported by the Soft and Hybrid Nanotechnology Experimental Resource (NSFECCS-1542205). We thank C. Wilke for her assistance with TEM. TEM was performed at the BioCryo facility of Northwestern University’s Atomic and Nanoscale Characterization Experimental (NUANCE) Center, which has received support from the Soft and Hybrid Nanotechnology Experimental Resource (NSF ECCS-1542205); the Materials Research Science and Engineering Centers (MRSEC) program (NSF DMR-1720139) at the Materials Research Center; the International Institute for Nanotechnology; and the State of Illinois, through the International Institute for Nanotechnology. It also made use of the CryoCluster equipment, which has received support from the Major Research Instrumentation (MRI) program (NSF DMR-1229693). We thank H. Edelstein for her assistance with confocal microscopy. Microscopy was performed at the Biological Imaging Facility at Northwestern University (RRID:SCR_017767), graciously supported by the Chemistry for Life Processes Institute, the Northwestern University Office for Research, and the Department of Molecular Biosciences. We thank P. Mehl for his assistance with FACS. Flow cytometry was performed at the Northwestern University Robert H. Lurie Comprehensive Cancer Center (RHLCCC) Flow Cytometry Facility, which is supported by a Cancer Center Support Grant (NCI CA060553). We thank J. Brink and S. Hockema at 496code for their assistance with HTS data analysis.
Author information
Authors and Affiliations
Contributions
D.M.S. and J.N.L. conceptualized the project and designed the experiments. D.M.S., B.N.D. and M.E.H. performed the experiments. D.M.S. and J.N.L. analysed the data. L.M.S. isolated, activated, and electroporated the primary T cells. K.E.B. and L.C. conducted the MiSeq runs. D.M.S. drafted the original manuscript and created the figures. J.N.L., J.F.H. and J.B.L. supervised the work. All authors reviewed, edited, and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
J.N.L. and D.M.S. are co-inventors on patent pending intellectual property that covers some technologies reported in this manuscript. J.N.L. and D.M.S. have financial interest in Syenex, which could potentially benefit from the outcomes of this research.
Peer review
Peer review information
Nature Biomedical Engineering thanks the anonymous reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Different scFv display techniques result in different EV targeting properties.
a, Cartoon highlighting the structures of the PDGFR transmembrane domain scFv display and lactadherin C1C2 domain anchoring to phosphatidylserine. b, Expression of scFv constructs in EV producer cell lysates. 1 µg cell lysate was loaded per lane. Expected band sizes: ∼40 kDa and ∼75 kDa (black arrows). c, Loading of scFv constructs into EVs generated from cell lines in b. 5.0×108 EVs were loaded per lane. d, Binding of targeted EVs to Jurkat T cells following a 2 h incubation. e, Representative histograms corresponding to the summary data reported in d. The subpopulation of cells showing a skewed, high degree of exosome binding is indicated by the red box. f, Recipient Jurkat T cells were incubated for 1 h in the presence or absence of anti-CD2 antibodies prior to a 2 h incubation with EVs. g, Representative histograms corresponding to the summary data reported in f. Flow cytometry experiments were performed in biological triplicate, and error bars (panels d, f) indicate standard error of the mean. EV dTomato loading evaluations are presented in Supplementary Fig. 5. Statistical tests comprise two-tailed Student’s t-tests using the Benjamini-Hochberg method to reduce the false discovery rate. (*p < 0.05, **p < 0.01, ***p < 0.001). Exact p-values are reported in Supplementary Table 1.
Extended Data Fig. 2 The ABI domain increases EV-cargo loading independently of total protein expression.
a, Expression of EYFP and EYFP-ABI in the presence of anti-CD2 targeting constructs in transiently transfected HEK293FT cells analysed by flow cytometry. A key observation is that addition of the ABI domain does not increase overall cargo protein expression in producer cells. b, Repeat of EYFP-ABI EV loading trends in the presence of an scFv shown in Fig. 3c. c, Comparison of EYFP loading into EVs with and without an NLS with ABA-binding constructs and under ABA-induced dimerization conditions. Addition of an NLS did not substantially impact EYFP loading, nor did ABA-induced dimerization substantially impact loading of nuclear-localized cargo. Experiments were performed in biological triplicate, and error bars indicate standard error of the mean. Statistical tests comprise two-tailed Student’s t-tests using the Benjamini-Hochberg method to reduce the false discovery rate. (*p < 0.05, **p < 0.01, ***p < 0.001). Exact p-values are reported in Supplementary Table 1.
Extended Data Fig. 3 The ABI domain increases Cas9 loading into EVs, and Cas9-ABI retains function.
a, Expression of Cas9 fused to either the ABI or PYL domain in transiently transfected HEK293FT cells. 2 µg cell lysate was loaded per lane. Expected band sizes: ∼160, 183, and 195 kDa (arrows). b, Cartoon illustrating the Cas9 reporter construct. Successful editing by Cas9 results in the deletion of a stop codon and (in some random fraction of cases) a repair-mediated frame shift induces express dTomato. c, Absence of an NLS or presence of the ABI domain does not meaningfully reduce Cas9 editing efficiency in transiently transfected Jurkat T cells. Cells were analysed by flow cytometry 3 d post-transfection. Experiments were performed in biological triplicate, and error bars indicate standard error of the mean. Statistical tests comprise two-tailed Student’s t-tests using the Benjamini-Hochberg method to reduce the false discovery rate. (*p < 0.05, **p < 0.01, ***p < 0.001). Exact p-values are reported in Supplementary Table 1. Samples with high cellular autofluorescence were excluded from analysis. d, Full blot of Cas9 EV active loading data presented in Fig. 3e. e, Cellular expression of Cas9 with and without the ABI domain or an NLS. 2 µg cell lysate was loaded per lane.
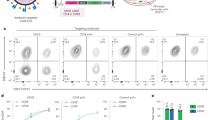
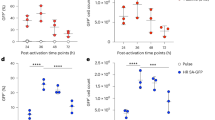
Extended Data Fig. 4 Electroporation of recombinant Cas9-sgRNA ribonucleoprotein complexes into primary T cells confers dose-dependent editing of the genomic CXCR4 target locus.
a, Analysis of actively loaded Cas9 molecules per EV in vesicles displaying an anti-CD2 scFv and VSV-G. Lanes loaded with 4.0 × 108 (‘high’) or 2.0 × 108 (‘low’) EVs were compared to samples loaded with specified numbers of recombinant Cas9 molecules quantified based upon the manufacturer’s analysis (lanes 7-13). Expected band sizes (∼160 or 195 kDa, arrows) correspond to Cas9 +/- the ABI domain. b, Quantification of Cas9 RNPs per EV. Band intensities from Cas9 standards in a were plotted against Cas9 molecules loaded (blue points), and loading of Cas9 into EVs was calculated using a line fit to the linear regime of the recombinant Cas9 standard curve (purple points; light: MV, dark: exo); this analysis indicates a loading of ∼100 Cas9 molecules per EV. c, Frequency of indels detected at the Cas9-targeted CXCR4 locus after electroporation of CD4+ T cells with different doses of CXCR4-targeted RNPs. Doses of recombinant Cas9 that correspond to equivalent Cas9 molecules per cell as EV delivery and equivalent Cas9 editing efficiencies as EVs are highlighted in light and dark grey, respectively. Background subtraction was performed using an untreated control; treatment of T cells with RNPs complexed with a non-targeted sgRNA produces similar levels of apparent CXCR4 editing as did the untreated controls, likely indicating that these conditions both represent noise associated with this assay. d, Distributions of RNP-mediated edits, by type, as described in Fig. 5. The no treatment, non-diluted CXCR4 sgRNA treatment (maximum editing), and 500x sgRNA dilution (similar editing frequency as EV-mediated delivery of Cas9-sgRNA) conditions are shown.
Supplementary information
Supplementary Information
Supplementary figures, notes and tables.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Stranford, D.M., Simons, L.M., Berman, K.E. et al. Genetically encoding multiple functionalities into extracellular vesicles for the targeted delivery of biologics to T cells. Nat. Biomed. Eng 8, 397–414 (2024). https://doi.org/10.1038/s41551-023-01142-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-023-01142-x
This article is cited by
-
Recent advances in extracellular vesicles for therapeutic cargo delivery
Experimental & Molecular Medicine (2024)