Abstract
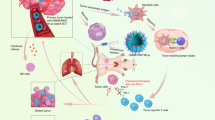
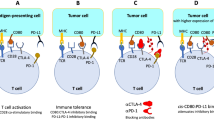
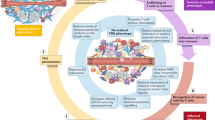
Checkpoint blockade elicits durable responses in immunogenic cancers, but it is largely ineffective in immunologically ‘cold’ tumours. Here we report the design, synthesis and performance of a bismuth-based nanoscale metal–organic framework that modulates the immunological and mechanical properties of the tumour microenvironment for enhanced radiotherapy–radiodynamic therapy. In mice with non-immunogenic prostate and pancreatic tumours irradiated with low X-ray doses, the intratumoural injection of the radiosensitizer mediated potent outcomes via the repolarization of immunosuppressive M2 macrophages into immunostimulatory M1 macrophages, the reduction of the concentration of intratumoural transforming growth factor beta (TGF-β) and of collagen density, and the inactivation of cancer-associated fibroblasts. When intravenously injected in combination with checkpoint-blockade therapy, the radiosensitizer mediated the reversal of immunosuppression in primary and distant tumours via the systemic reduction of TGF-β levels, which led to the downregulation of collagen expression, the stimulation of T-cell infiltration in the tumours and a robust abscopal effect. Nanoscale radiosensitizers that stimulate anti-tumour immunity and T-cell infiltration may enhance the therapeutic outcomes of checkpoint blockade in other tumour types.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The main data supporting the results in this study are available within the paper and its Supplementary Information. Source data for Figs. 3 and 4 are provided with this paper. The raw and analysed datasets generated during the study are too large to be publicly shared, yet they are available for research purposes from the corresponding author on reasonable request.
Change history
11 November 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41551-022-00966-3
References
Blankenstein, T., Coulie, P. G., Gilboa, E. & Jaffee, E. M. The determinants of tumour immunogenicity. Nat. Rev. Cancer 12, 307–313 (2012).
Hodi, F. S. et al. Improved survival with ipilimumab in patients with metastatic melanoma. N. Engl. J. Med. 363, 711–723 (2010).
Beer, T. M. et al. Randomized, double-blind, phase III trial of ipilimumab versus placebo in asymptomatic or minimally symptomatic patients with metastatic chemotherapy-naive castration-resistant prostate cancer. J. Clin. Oncol. 35, 40–47 (2017).
Martinez-Bosch, N., Vinaixa, J. & Navarro, P. Immune evasion in pancreatic cancer: from mechanisms to therapy. Cancers 10, 6 (2018).
Castano, A. P., Mroz, P. & Hamblin, M. R. Photodynamic therapy and anti-tumour immunity. Nat. Rev. Cancer 6, 535–545 (2006).
Weichselbaum, R. R., Liang, H., Deng, L. & Fu, Y.-X. Radiotherapy and immunotherapy: a beneficial liaison? Nat. Rev. Clin. Oncol. 14, 365–379 (2017).
Zheng, G. et al. Photodynamic molecular beacon as an activatable photosensitizer based on protease-controlled singlet oxygen quenching and activation. Proc. Natl Acad. Sci. USA 104, 8989–8994 (2007).
Zhou, Z., Song, J., Nie, L. & Chen, X. Reactive oxygen species generating systems meeting challenges of photodynamic cancer therapy. Chem. Soc. Rev. 45, 6597–6626 (2016).
Siva, S., MacManus, M. P., Martin, R. F. & Martin, O. A. Abscopal effects of radiation therapy: a clinical review for the radiobiologist. Cancer Lett. 356, 82–90 (2015).
Wan, C. et al. Irradiated tumor cell-derived microparticles mediate tumor eradication via cell killing and immune reprogramming. Sci. Adv. 6, eaay9789 (2020).
Nam, J. et al. Cancer nanomedicine for combination cancer immunotherapy. Nat. Rev. Mater. 4, 398–414 (2019).
Chen, H. et al. Nanoscintillator-mediated X-ray inducible photodynamic therapy for in vivo cancer treatment. Nano Lett. 15, 2249–2256 (2015).
Sang, W., Zhang, Z., Dai, Y. & Chen, X. Recent advances in nanomaterial-based synergistic combination cancer immunotherapy. Chem. Soc. Rev. 48, 3771–3810 (2019).
Luo, M. et al. A STING-activating nanovaccine for cancer immunotherapy. Nat. Nanotechnol. 12, 648–654 (2017).
Lu, K. et al. Low-dose X-ray radiotherapy–radiodynamic therapy via nanoscale metal–organic frameworks enhances checkpoint blockade immunotherapy. Nat. Biomed. Eng. 2, 600–610 (2018).
Lin, W., He, C. & Lu, K. Nanoparticles for photodynamic therapy, X-ray induced photodynamic therapy, radiotherapy, chemotherapy, immunotherapy, and any combination thereof. US patent US201462063770P (2014).
Furukawa, H., Cordova, K. E., O’Keeffe, M. & Yaghi, O. M. The chemistry and applications of metal-organic frameworks. Science 341, 1230444 (2013).
Cui, Y., Yue, Y., Qian, G. & Chen, B. Luminescent functional metal–organic frameworks. Chem. Rev. 112, 1126–1162 (2012).
Zhou, H.-C., Long, J. R. & Yaghi, O. M. Introduction to metal-organic frameworks. Chem. Rev. 112, 673–674 (2012).
Rabone, J. et al. An adaptable peptide-based porous material. Science 329, 1053–1057 (2010).
He, C., Liu, D. & Lin, W. Nanomedicine applications of hybrid nanomaterials built from metal–ligand coordination bonds: nanoscale metal–organic frameworks and nanoscale coordination polymers. Chem. Rev. 115, 11079–11108 (2015).
Morris, W., Briley, W. E., Auyeung, E., Cabezas, M. D. & Mirkin, C. A. Nucleic acid–metal organic framework (MOF) nanoparticle conjugates. J. Am. Chem. Soc. 136, 7261–7264 (2014).
Wang, S., McGuirk, C. M., d’Aquino, A., Mason, J. A. & Mirkin, C. A. Metal–organic framework nanoparticles. Adv. Mater. 30, 1800202 (2018).
Wang, C. et al. Synergistic assembly of heavy metal clusters and luminescent organic bridging ligands in metal–organic frameworks for highly efficient X-ray scintillation. J. Am. Chem. Soc. 136, 6171–6174 (2014).
Dougherty, T. J. et al. Photodynamic therapy. J. Natl Cancer Inst. 90, 889–905 (1998).
Garg, A. D., Nowis, D., Golab, J. & Agostinis, P. Photodynamic therapy: illuminating the road from cell death towards anti-tumour immunity. Apoptosis 15, 1050–1071 (2010).
Rabin, O., Perez, J. M., Grimm, J., Wojtkiewicz, G. & Weissleder, R. An X-ray computed tomography imaging agent based on long-circulating bismuth sulphide nanoparticles. Nat. Mater. 5, 118–122 (2006).
Mendoza-Espinosa, D. Synthesis and characterization of a Bi10O8(OAr)16 oxo-cluster supported by p-tert-butylcalix[5]arene ligands. Dalton Trans. 45, 13399–13405 (2016).
Andrews, P. C., Deacon, G. B., Junk, P. C., Kumar, I. & MacLellan, J. G. Synthesis, ethanolysis, and hydrolysis of bismuth (III) ortho-nitrobenzoate complexes en route to a pearl necklace-like polymer of Bi10 oxo-clusters. Organometallics 28, 3999–4008 (2009).
Obeid, M. et al. Calreticulin exposure is required for the immunogenicity of γ-irradiation and UVC light-induced apoptosis. Cell Death Differ. 14, 1848–1850 (2007).
Sims, G. P., Rowe, D. C., Rietdijk, S. T., Herbst, R. & Coyle, A. J. HMGB1 and RAGE in inflammation and cancer. Annu. Rev. Immunol. 28, 367–388 (2010).
Aymeric, L. et al. Tumor cell death and ATP release prime dendritic cells and efficient anticancer immunity. Cancer Res. 70, 855–858 (2010).
Gingrich, J. R. et al. Metastatic prostate cancer in a transgenic mouse. Cancer Res. 56, 4096–4102 (1996).
Tang, Y. et al. Divergent effects of castration on prostate cancer in TRAMP mice: possible implications for therapy.Clin. Cancer Res. 14, 2936–2943 (2008).
Michaelis, K. A. et al. Establishment and characterization of a novel murine model of pancreatic cancer cachexia. J. Cachexia Sarcopenia Muscle 8, 824–838 (2017).
Martin, J. D., Seano, G. & Jain, R. K. Normalizing function of tumor vessels: progress, opportunities, and challenges. Annu. Rev. Physiol. 81, 505–534 (2019).
Chauhan, V. P. et al. Reprogramming the microenvironment with tumor-selective angiotensin blockers enhances cancer immunotherapy. Proc. Natl Acad. Sci. USA 116, 10674–10680 (2019).
Tan, H.-Y. et al. The reactive oxygen species in macrophage polarization: reflecting its dual role in progression and treatment of human diseases. Oxid. Med. Cell. Longev. 2016, 2795090 (2016).
Porta, C. et al. Tolerance and M2 (alternative) macrophage polarization are related processes orchestrated by p50 nuclear factor κB. Proc. Natl Acad. Sci. USA 106, 14978–14983 (2009).
Gu, Z. et al. Mechanism of iron oxide-induced macrophage activation: the impact of composition and the underlying signaling pathway. J. Am. Chem. Soc. 141, 6122–6126 (2019).
Bosi, S., Da Ros, T., Spalluto, G. & Prato, M. Fullerene derivatives: an attractive tool for biological applications. Eur. J. Med. Chem. 38, 913–923 (2003).
Ni, K. et al. Nanoscale metal–organic framework co-delivers TLR-7 agonists and anti-CD47 antibodies to modulate macrophages and orchestrate cancer immunotherapy. J. Am. Chem. Soc. https://doi.org/10.1021/jacs.0c05039 (2020).
Martin, C. J. et al. Selective inhibition of TGFβ1 activation overcomes primary resistance to checkpoint blockade therapy by altering tumor immune landscape. Sci. Transl. Med. 12, 536 (2020).
Zinger, A. et al. Collagenase nanoparticles enhance the penetration of drugs into pancreatic tumors. ACS Nano 13, 11008–11021 (2019).
Mariathasan, S. et al. TGFβ attenuates tumour response to PD-L1 blockade by contributing to exclusion of T cells. Nature 554, 544–548 (2018).
Papageorgis, P. & Stylianopoulos, T. Role of TGFbeta in regulation of the tumor microenvironment and drug delivery (review). Int. J. Oncol. 46, 933–943 (2015).
Zhang, F. et al. TGF-β induces M2-like macrophage polarization via SNAIL-mediated suppression of a pro-inflammatory phenotype. Oncotarget 7, 52294–52306 (2016).
Akhurst, R. J. & Hata, A. Targeting the TGFβ signalling pathway in disease. Nat. Rev. Drug Discov. 11, 790–811 (2012).
Rubtsov, Y. P. & Rudensky, A. Y. TGFbeta signalling in control of T-cell-mediated self-reactivity. Nat. Rev. Immunol. 7, 443–453 (2007).
Laouar, Y., Sutterwala, F. S., Gorelik, L. & Flavell, R. A. Transforming growth factor-beta controls T helper type 1 cell development through regulation of natural killer cell interferon-gamma. Nat. Immunol. 6, 600–607 (2005).
Irvine, D. J., Hanson, M. C., Rakhra, K. & Tokatlian, T. Synthetic nanoparticles for vaccines and immunotherapy. Chem. Rev. 115, 11109–11146 (2015).
Carstens, J. L. et al. Spatial computation of intratumoral T cells correlates with survival of patients with pancreatic cancer. Nat. Commun. 8, 15095 (2017).
Stephan, M. T., Moon, J. J., Um, S. H., Bershteyn, A. & Irvine, D. J. Therapeutic cell engineering with surface-conjugated synthetic nanoparticles. Nat. Med. 16, 1035–1041 (2010).
Tang, L. et al. Enhancing T cell therapy through TCR-signaling-responsive nanoparticle drug delivery. Nat. Biotechnol. 36, 707–716 (2018).
Miller, M. A. & Weissleder, R. Imaging of anticancer drug action in single cells. Nat. Rev. Cancer 17, 399–414 (2017).
Nam, J. et al. Chemo-photothermal therapy combination elicits anti-tumor immunity against advanced metastatic cancer. Nat. Commun. 9, 1074 (2018).
Tyekucheva, S. et al. Stromal and epithelial transcriptional map of initiation progression and metastatic potential of human prostate cancer. Nat. Commun. 8, 420 (2017).
Zhou, H. et al. IGF1 receptor targeted theranostic nanoparticles for targeted and image-guided therapy of pancreatic cancer. ACS Nano 9, 7976–7991 (2015).
Gao, N. et al. Tumor penetrating theranostic nanoparticles for enhancement of targeted and image-guided drug delivery into peritoneal tumors following intraperitoneal delivery. Theranostics 7, 1689–1704 (2017).
Huang, Y. et al. Dual-mechanism based CTLs infiltration enhancement initiated by nano-sapper potentiates immunotherapy against immune-excluded tumors. Nat. Commun. 11, 622 (2020).
Chakravarthy, A., Khan, L., Bensler, N. P., Bose, P. & De Carvalho, D. D. TGF-β-associated extracellular matrix genes link cancer-associated fibroblasts to immune evasion and immunotherapy failure. Nat. Commun. 9, 4692 (2018).
Liu, M., Song, W. & Huang, L. Drug delivery systems targeting tumor-associated fibroblasts for cancer immunotherapy. Cancer Lett. 448, 31–39 (2019).
Miao, L. et al. The binding site barrier elicited by tumor-associated fibroblasts interferes disposition of nanoparticles in stroma-vessel type tumors. ACS Nano 10, 9243–9258 (2016).
Miao, L. et al. Targeting tumor-associated fibroblasts for therapeutic delivery in desmoplastic tumors. Cancer Res. 77, 719–731 (2017).
Fukumura, D., Kloepper, J., Amoozgar, Z., Duda, D. G. & Jain, R. K. Enhancing cancer immunotherapy using antiangiogenics: opportunities and challenges. Nat. Rev. Clin. Oncol. 15, 325–340 (2018).
Acknowledgements
We thank Y. Song for experimental help; the late O. Schneewind of the Department of Microbiology at the University of Chicago for help with the macrophage repolarization studies; and the National Cancer Institute (U01–CA198989 and 1R01CA253655), the Department of Defense (PC170934P2), the University of Chicago Medicine Comprehensive Cancer Center (NIH CCSG: P30 CA014599) and the Ludwig Institute for Metastasis Research for funding support.
Author information
Authors and Affiliations
Contributions
K.N. and W.L. conceived the project. K.N., Z.X., A.C. and T.L. performed the experiments and analysed the results. E.P., B.P. and P.L.R. performed the radioluminescence test, and N.G. and T.W. assisted with the qPCR analysis. M.T.S. and N.G. generated the spontaneous TRAMP model. N.G. and K.Y. performed intraprostatic injection. K.N., Z.X., A.C., R.R.W., M.T.S. and W.L. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
W.L. is founder of Coordination Pharmaceuticals, which licensed the nMOF technology from the University of Chicago. R.R.W. is a consultant to Coordination Pharmaceuticals. The other authors declare no competing interests.
Peer review
Peer review information
Nature Biomedical Engineering thanks the anonymous reviewers for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Structure of Bi10O8 SBUs.
Views of Bi10O8 SBUs in Bi-BPDC along the crystallographic a-axis or b-axis (a) and c-axis (b). Purple: bismuth; red: oxygen; blue: nitrogen; grey: carbon.
Extended Data Fig. 2 Crystal structure of Bi-DBP.
Modelled crystal structures of Bi-DBP projected along the a-axis (a), the b-axis (b), and the c-axis (c) and Bi10O8 SBU (d). Purple: bismuth; red: oxygen; blue: nitrogen; grey: carbon.
Extended Data Fig. 3 Immune profiling on bilateral TRAMP-C2 model.
Percentages of tumour-infiltrating leucocytes with respect to the total live cells from TRAMP-C2 tumour-bearing mice treated with PBS (–), PBS (+), aPD-L1 (+), Bi-DBP (+), Bi-DBP (–) + αPD-L1, or Bi-DBP (+) + αPD-L1. Data are expressed as means ± s.d., n = 5 for biological replicates. P-value by two-sided student t-test. Central lines, bounds of box and whiskers represent mean values, 25% to 75% of the range of data and 1.5-fold of interquartile range away from outliers, respectively. The result was obtained without repetition.
Supplementary information
Supplementary Information
Supplementary methods, figures and tables.
Source data
Source data for Fig. 3
Tumour-growth data in Fig. 3a,b.
Source data for Fig. 4
Tumour-growth data in Fig. 4a,b,d,e.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ni, K., Xu, Z., Culbert, A. et al. Synergistic checkpoint-blockade and radiotherapy–radiodynamic therapy via an immunomodulatory nanoscale metal–organic framework. Nat Biomed Eng 6, 144–156 (2022). https://doi.org/10.1038/s41551-022-00846-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-022-00846-w
This article is cited by
-
Radiation combined with immune checkpoint inhibitors for unresectable locally advanced non-small cell lung cancer: synergistic mechanisms, current state, challenges, and orientations
Cell Communication and Signaling (2023)
-
Radiation-induced tumor immune microenvironments and potential targets for combination therapy
Signal Transduction and Targeted Therapy (2023)
-
Engineering nanomaterial physical characteristics for cancer immunotherapy
Nature Reviews Bioengineering (2023)
-
Radiotherapy combined with immunotherapy: the dawn of cancer treatment
Signal Transduction and Targeted Therapy (2022)