Abstract
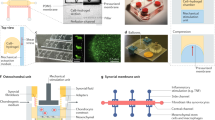
Owing to population aging, the social impact of osteoarthritis (OA)—the most common musculoskeletal disease—is expected to increase dramatically. Yet, therapy is still limited to palliative treatments or surgical intervention, and disease-modifying OA (DMOA) drugs are scarce, mainly because of the absence of relevant preclinical OA models. Therefore, in vitro models that can reliably predict the efficacy of DMOA drugs are needed. Here, we show, using a newly developed microphysiological cartilage-on-a-chip model that enables the application of strain-controlled compression to three-dimensional articular cartilage microtissue, that a 30% confined compression recapitulates the mechanical factors involved in OA pathogenesis and is sufficient to induce OA traits. Such hyperphysiological compression triggers a shift in cartilage homeostasis towards catabolism and inflammation, hypertrophy, and the acquisition of a gene expression profile akin to those seen in clinical osteoarthritic tissue. The cartilage on-a-chip model may enable the screening of DMOA candidates.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The main data supporting the findings of this study are available within the paper and its Supplementary Information. All data generated for this study are available from the corresponding author upon reasonable request.
References
Bijlsma, J. W., Berenbaum, F. & Lafeber, F. P. Osteoarthritis: an update with relevance for clinical practice. Lancet 377, 2115–2126 (2011).
Wittenauer, R., Smith, L. & Aden, K. Background Paper 6.12: Osteoarthritis (WHO, 2013).
Sanchez-Adams, J., Leddy, H. A., McNulty, A. L., O’Conor, C. J. & Guilak, F. The mechanobiology of articular cartilage: bearing the burden of osteoarthritis. Curr. Rheumatol. Rep. 16, 451 (2014).
Arden, N. & Nevitt, M. C. Osteoarthritis: epidemiology. Best. Pract. Res. Clin. Rheumatol. 20, 3–25 (2006).
Johnson, C. I., Argyle, D. J. & Clements, D. N. In vitro models for the study of osteoarthritis. Vet. J. 209, 40–49 (2016).
Esch, E. W., Bahinski, A. & Huh, D. Organs-on-chips at the frontiers of drug discovery. Nat. Rev. Drug Discov. 14, 248–260 (2015).
Kutzner, I. et al. Loading of the knee joint during activities of daily living measured in vivo in five subjects. J. Biomech. 43, 2164–2173 (2010).
Mow, V. C., Ratcliffe, A. & Robin Poole, A. Cartilage and diarthrodial joints as paradigms for hierarchical materials and structures. Biomaterials 13, 67–97 (1992).
Grodzinsky, A. J., Levenston, M. E., Jin, M. & Frank, E. H. Cartilage tissue remodelling in response to mechanical forces. Annu. Rev. Biomed. Eng. 2, 691–713 (2000).
Choi, J. B. et al. Zonal changes in the three-dimensional morphology of the chondron under compression: the relationship among cellular, pericellular, and extracellular deformation in articular cartilage. J. Biomech. 40, 2596–2603 (2007).
Lin, H., Lozito, T. P., Alexander, P. G., Gottardi, R. & Tuan, R. S. Stem cell-based microphysiological osteochondral system to model tissue response to interleukin-1β. Mol. Pharm. 11, 2203–2212 (2014).
Goldman, S. M. & Barabino, G. A. Spatial engineering of osteochondral tissue constructs through microfluidically directed differentiation of mesenchymal stem cells. Biores. Open Access 5, 109–117 (2016).
Mumme, M. et al. Nasal chondrocyte-based engineered autologous cartilage tissue for repair of articular cartilage defects: an observational first-in-human trial. Lancet 388, 1985–1994 (2016).
Kafienah, W. et al. Three-dimensional tissue engineering of hyaline cartilage: comparison of adult nasal and articular chondrocytes. Tissue Eng. 8, 817–826 (2002).
Tsimbouri, P. M. et al. Stimulation of 3D osteogenesis by mesenchymal stem cells using a nanovibrational bioreactor. Nat. Biomed. Eng. 1, 758–770 (2017).
Lee, D. A. & Bader, D. L. Compressive strains at physiological frequencies influence the metabolism of chondrocytes seeded in agarose. J. Orthop. Res. 15, 181–188 (1997).
De Croos, J. N. A., Dhaliwal, S. S., Grynpas, M. D., Pilliar, R. M. & Kandel, R. A. Cyclic compressive mechanical stimulation induces sequential catabolic and anabolic gene changes in chondrocytes resulting in increased extracellular matrix accumulation. Matrix Biol. 25, 323–331 (2006).
Khozoee, B., Mafi, P., Mafi, R. & Khan, W. Mechanical stimulation protocols of human derived cells in articular cartilage tissue engineering—a systematic review. Curr. Stem Cell Res. Ther. 12, 260–270 (2017).
Huh, D. et al. Reconstituting organ-level lung functions on a chip. Science 328, 1662–1668 (2010).
Ugolini, G. S., Visone, R., Redaelli, A., Moretti, M. & Rasponi, M. Generating multicompartmental 3D biological constructs interfaced through sequential injections in microfluidic devices. Adv. Healthc. Mater. 6, 1601170 (2017).
Occhetta, P., Visone, R. & Rasponi, M. High-throughput microfluidic platform for 3D cultures of mesenchymal stem cells. Methods Mol. Biol. 1612, 303–323 (2017).
Ng, J. M. K., Gitlin, I., Stroock, A. D. & Whitesides, G. M. Components for integrated poly(dimethylsiloxane) microfluidic systems. Electrophoresis 23, 3461–3473 (2002).
Marsano, A. et al. Beating heart on a chip: a novel microfluidic platform to generate functional 3D cardiac microtissues. Lab Chip 16, 599–610 (2016).
Visone, R. et al. A simple vacuum-based microfluidic technique to establish high-throughput organs-on-chip and 3D cell cultures at the microscale. Adv. Mater. Technol. 4, 1800319 (2019).
Ehrbar, M. et al. Biomolecular hydrogels formed and degraded via site-specific enzymatic reactions. Biomacromolecules 8, 3000–3007 (2007).
Blum, M. M. & Ovaert, T. C. Experimental and numerical tribological studies of a boundary lubricant functionalized poro-viscoelastic PVA hydrogel in normal contact and sliding. J. Mech. Behav. Biomed. Mater. 14, 248–258 (2012).
Kalyanam, S. Poro-viscoelastic behavior of gelatin hydrogels under compression—implications for bioelasticity imaging. J. Biomech. Eng. 131, 081005 (2009).
DiSilvestro, M. R., Zhu, Q., Wong, M., Jurvelin, J. S. & Suh, J.-K. F. Biphasic poroviscoelastic simulation of the unconfined compression of articular cartilage: I—simultaneous prediction of reaction force and lateral displacement. J. Biomech. Eng. 123, 191–197 (2001).
Villanueva, I., Hauschulz, D. S., Mejic, D. & Bryant, S. J. Static and dynamic compressive strains influence nitric oxide production and chondrocyte bioactivity when encapsulated in PEG hydrogels of different crosslinking densities. Osteoarthr. Cartil. 16, 909–918 (2008).
Phelps, E. A. et al. Maleimide cross-linked bioactive PEG hydrogel exhibits improved reaction kinetics and cross-linking for cell encapsulation and in situ delivery. Adv. Mater. 24, 64–70 (2012).
Wu, J. Z., Herzog, W. & Epstein, M. Evaluation of the finite element software ABAQUS for biomechanical modelling of biphasic tissues. J. Biomech. 31, 165–169 (1997).
Ray, A., Singh, P. N. P., Sohaskey, M. L., Harland, R. M. & Bandyopadhyay, A. Precise spatial restriction of BMP signaling is essential for articular cartilage differentiation. Development 142, 1169–1179 (2015).
Nishioka, T. et al. ATX–LPA1 axis contributes to proliferation of chondrocytes by regulating fibronectin assembly leading to proper cartilage formation. Sci. Rep. 6, 23433 (2016).
Leijten, J. C. H. et al. Gremlin 1, frizzled‐related protein, and Dkk‐1 are key regulators of human articular cartilage homeostasis. Arthritis Rheumatol. 64, 3302–3312 (2012).
Takaishi, H., Kimura, T., Dalal, S., Okada, Y. & D’Armiento, J. Joint diseases and matrix metalloproteinases: a role for MMP-13. Curr. Pharm. Biotechnol. 9, 47–54 (2008).
Flory, J. J. E., Fosang, A. J. & Knudson, W. The accumulation of intracellular ITEGE and DIPEN neoepitopes in bovine articular chondrocytes is mediated by CD44 internalization of hyaluronan. Arthritis Rheumatol. 54, 443–454 (2006).
Bau, B. et al. Relative messenger RNA expression profiling of collagenases and aggrecanases in human articular chondrocytes in vivo and in vitro. Arthritis Rheumatol. 46, 2648–2657 (2002).
Tsuchida, A. I. et al. Cytokine profiles in the joint depend on pathology, but are different between synovial fluid, cartilage tissue and cultured chondrocytes. Arthritis Res. Ther. 16, 441 (2014).
Kronenberg, H. M. Developmental regulation of the growth plate. Nature 423, 332–336 (2003).
Leijten, J. C. H. et al. GREM1, FRZB and DKK1 mRNA levels correlate with osteoarthritis and are regulated by osteoarthritis-associated factors. Arthritis Res. Ther. 15, R126 (2013).
Braddock, M. & Quinn, A. Targeting IL-1 in inflammatory disease: new opportunities for therapeutic intervention. Nat. Rev. Drug Discov. 3, 330–339 (2004).
Grodzinsky, A. J., Wang, Y., Kakar, S., Vrahas, M. S. & Evans, C. H. Intra‐articular dexamethasone to inhibit the development of post‐traumatic osteoarthritis. J. Orthop. Res. 35, 406–411 (2017).
Lim, H. et al. Inhibition of matrix metalloproteinase-13 expression in IL-1β-treated articular chondrocytes by a steroidal saponin, spicatoside A, and its cellular mechanisms of action. Arch. Pharm. Res. 38, 1108–1116 (2015).
Yan, B. et al. mTORC1 regulates PTHrP to coordinate chondrocyte growth, proliferation and differentiation. Nat. Commun. 7, 11151 (2016).
Pal, B., Endisha, H., Zhang, Y. & Kapoor, M. mTOR: a potential therapeutic target in osteoarthritis? Drugs R. D. 15, 27–36 (2015).
Sasaki, H. et al. Autophagy modulates osteoarthritis‐related gene expression in human chondrocytes. Arthritis Rheumatol. 64, 1920–1928 (2012).
Zweers, M. C. et al. Celecoxib: considerations regarding its potential disease-modifying properties in osteoarthritis. Arthritis Res. Ther. 13, 239 (2011).
Pavan, M., Galesso, D., Secchieri, C. & Guarise, C. Hyaluronic acid alkyl derivative: a novel inhibitor of metalloproteases and hyaluronidases. Int. J. Biol. Macromol. 84, 221–226 (2016).
Pavan, M., Galesso, D., Menon, G., Renier, D. & Guarise, C. Hyaluronan derivatives: alkyl chain length boosts viscoelastic behavior to depolymerization. Carbohydr. Polym. 97, 321–326 (2013).
Kapoor, M., Martel-Pelletier, J., Lajeunesse, D., Pelletier, J.-P. & Fahmi, H. Role of proinflammatory cytokines in the pathophysiology of osteoarthritis. Nat. Rev. Rheumatol. 7, 33–42 (2011).
Guarise, C. et al. Matrix metalloprotease 3 (MMP3) inhibition effect of a viscosupplement based on a hyaluronic acid amide derivative (HYADD4). Osteoarthr. Cartil. 26, S286–S287 (2018).
Moraes, C., Sun, Y. & Simmons, C. A. (Micro)managing the mechanical microenvironment. Integr. Biol. 3, 959–971 (2011).
Greaves, L. L., Gilbart, M. K., Yung, A. C., Kozlowski, P. & Wilson, D. R. Effect of acetabular labral tears, repair and resection on hip cartilage strain: a 7 T MR study. J. Biomech. 43, 858–863 (2010).
Wong, B. L. & Sah, R. L. Effect of a focal articular defect on cartilage deformation during patello-femoral articulation. J. Orthop. Res. 28, 1554–1561 (2010).
Lutolf, M. P. & Hubbell, J. A. Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat. Biotechnol. 23, 47–55 (2005).
Barbero, A. et al. Age related changes in human articular chondrocyte yield, proliferation and post-expansion chondrogenic capacity. Osteoarthr. Cartil. 12, 476–484 (2004).
Nam, J., Aguda, B. D., Rath, B. & Agarwal, S. Biomechanical thresholds regulate inflammation through the NF-κB pathway: experiments and modeling. PLoS ONE 4, e5262 (2009).
Hunter, C. J., Imler, S. M., Malaviya, P., Nerem, R. M. & Levenston, M. E. Mechanical compression alters gene expression and extracellular matrix synthesis by chondrocytes cultured in collagen I gels. Biomaterials 23, 1249–1259 (2002).
Dreier, R. Hypertrophic differentiation of chondrocytes in osteoarthritis: the developmental aspect of degenerative joint disorders. Arthritis Res. Ther. 12, 216 (2010).
Zhong, L. et al. Nitric oxide mediates crosstalk between interleukin 1β and WNT signaling in primary human chondrocytes by reducing DKK1 and FRZB expression. Int. J. Mol. Sci. 18, E2491 (2017).
Mobasheri, A., Bay-Jensen, A.-C., van Spil, W. E., Larkin, J. & Levesque, M. C. Osteoarthritis Year in Review 2016: biomarkers (biochemical markers). Osteoarthr. Cartil. 25, 199–208 (2017).
Goldring, S. R. & Goldring, M. B. Changes in the osteochondral unit during osteoarthritis: structure, function and cartilage–bone crosstalk. Nat. Rev. Rheumatol. 12, 632–644 (2016).
Yuan, X. L. et al. Bone–cartilage interface crosstalk in osteoarthritis: potential pathways and future therapeutic strategies. Osteoarthr. Cartil. 22, 1077–1089 (2014).
Takayama, K. et al. Local intra-articular injection of rapamycin delays articular cartilage degeneration in a murine model of osteoarthritis. Arthritis Res. Ther. 16, 482 (2014).
Matsuzaki, T. et al. Intra-articular administration of gelatin hydrogels incorporating rapamycin–micelles reduces the development of experimental osteoarthritis in a murine model. Biomaterials 35, 9904–9911 (2014).
Lienemann, P. S., Lutolf, M. P. & Ehrbar, M. Biomimetic hydrogels for controlled biomolecule delivery to augment bone regeneration. Adv. Drug Deliv. Rev. 64, 1078–1089 (2012).
DiSilvestro, M. R. & Suh, J. K. F. A cross-validation of the biphasic poroviscoelastic model of articular cartilage in unconfined compression, indentation, and confined compression. J. Biomech. 34, 519–525 (2001).
Meng, Q., Jin, Z., Fisher, J. & Wilcox, R. Comparison between FEBio and Abaqus for biphasic contact problems. Proc. Inst. Mech. Eng. H 227, 1009–1019 (2013).
Ehrbar, M. et al. Elucidating the role of matrix stiffness in 3D cell migration and remodeling. Biophys. J. 100, 284–293 (2011).
Phelps, E. A. et al. Maleimide cross-linked bioactive PEG hydrogel exhibits improved reaction kinetics and cross-linking for cell encapsulation and in-situ delivery. Adv. Mater. 24, 64–70 (2012).
Farndale, R. W., Buttle, D. J. & Barrett, A. J. Improved quantitation and discrimination of sulphated glycosaminoglycans by use of dimethylmethylene blue. Biochim. Biophys. Acta 883, 173–177 (1986).
Acknowledgements
We are grateful to G. Pagenstert for provision of the articular cartilage biopsies. We also thank Fidia Farmaceutici (Italy) for provision of the HYADD 4 and LMW-HA compounds—in particular, D. Galesso, R. Beninatto and C. Guarise for feedback on the results. Device manufacturing was partially performed at PoliFAB—the micro- and nanofabrication facility of Politecnico di Milano. This work was partially funded by the Swiss National Science Foundation (numbers 310030_149614/1 and 310030_175660/1).
Author information
Authors and Affiliations
Contributions
M.R., A.B. and P.O. conceived the project. M.R. and A.M. conceived the device. E.V. and A.M. implemented the finite element model and performed the simulations. A.M. performed the mechanical characterization of the device. A.M. and P.O. produced the devices. P.O. and A.M. performed and analysed the biological experiments. Q.V.-M. and M.E. produced the PEG gel. P.O., A.M., M.R., A.B. and I.M. wrote the manuscript. All authors discussed the results, commented on the manuscript and contributed to its final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary methods, figures, tables, references and video captions.
Supplementary Video 1
PEG hydrogel strain field on 30% compression.
Supplementary Video 2
3D reconstruction of the COC in static culture or after HPC.
Rights and permissions
About this article
Cite this article
Occhetta, P., Mainardi, A., Votta, E. et al. Hyperphysiological compression of articular cartilage induces an osteoarthritic phenotype in a cartilage-on-a-chip model. Nat Biomed Eng 3, 545–557 (2019). https://doi.org/10.1038/s41551-019-0406-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-019-0406-3
This article is cited by
-
Bone marrow lesions: plugging the holes in our knowledge using animal models
Nature Reviews Rheumatology (2023)
-
Preclinical performance testing of medical devices with antimicrobial effects
Nature Reviews Bioengineering (2023)
-
Organoids and Their Research Progress in Plastic and Reconstructive Surgery
Aesthetic Plastic Surgery (2023)
-
Modeling early changes associated with cartilage trauma using human-cell-laden hydrogel cartilage models
Stem Cell Research & Therapy (2022)
-
A role for microfluidic systems in precision medicine
Nature Communications (2022)