Abstract
REGEN-COV, a combination of the monoclonal antibodies casirivimab and imdevimab, has been approved as a treatment for high-risk patients infected with SARS-CoV-2 within five days of their diagnosis. We performed a retrospective cohort study, and used data repositories of Israel’s largest healthcare organization to determine the real-world effectiveness of REGEN-COV treatment against COVID-19-related hospitalization, severe disease, and death. We compared patients infected with Delta variant and treated with REGEN-COV (n = 289) to those infected but not-treated with REGEN-COV (n = 1,296). Demographic and clinical characteristics were used to match patients and for further adjustment as part of the C0x model. Estimated treatment effectiveness was defined as one minus the hazard ratio. Treatment effectiveness of REGEN-COV was 56.4% (95% CI: 23.7–75.1%) in preventing COVID-19 hospitalization, 59.2% (95% CI: 19.9–79.2%) in preventing severe COVID-19, and 93.5% (95% CI: 52.1–99.1%) in preventing COVID-19 death in the 28 days after treatment. In conclusion, REGEN-COV was effective in reducing the risk of severe sequelae in high-risk COVID-19 patients.
Similar content being viewed by others
Introduction
Since December 2019, SARS-CoV-2 has spread worldwide1, resulting over 310 million confirmed infections and until roughly over 5.4 million deaths up to January 20222. SARS-CoV-2 vaccines, first introduced in December 2020, have helped reduce the burden of the pandemic. Yet, there remain many people who are not vaccinated, either due to lack of vaccine access, prior medical conditions, or vaccine hesitancy3. In addition, breakthrough infections occur among vaccinated individuals4. Therefore, there is still a need for effective treatments to prevent severe COVID-19 outcomes among infected individuals.
REGEN-COV, a combination of two SARS-CoV-2 antibodies (casirivimab and imdevimab), received emergency use authorization from the U.S. Food and Drug Administration for patients aged 12 years or older in 2021. The drug is designated for patients who have been diagnosed with COVID-19 and have not deteriorated to severe illness, but are at high risk for deterioration, including immunocompromised individuals and those with high-risk medical conditions5. The efficacy of REGEN-COV has been demonstrated in clinical trials5,6,7, where it was shown to reduce symptomatic COVID-19 illness by 62% and COVID-19-related hospitalization or death by 70% in the first month after treatment5. Evidence suggests that the benefits are greater when REGEN-COV is administered within the first five days following infection8, 9.
An observational study by Razonable et al., 202210, which includes 696 patients who received REGEN-COV, was compared with propensity-matched controls of 696 non-treated patients diagnosed with mild to moderate COVID-19 at Mayo clinic sites in four US states. The results indicate that the REGEN-COV treatment significantly lowered all-cause hospitalization rates at day 14 (1.3% vs 3.3%; absolute difference[AD]: 2.0%; 95% confidence interval (CI): 0.5–3.7%) at day 21 (1.3% vs 4.2%; AD: 2.9%; 95% CI: 1.2–4.7%), and at day 28 (1.6% vs. 4.8%; AD: 3.2%; 95% CI: 1.4–5.1%). The effectiveness of REGEN-COV against all-cause ICU admission rates and all-cause mortality at three-time points were similar in both groups10. This study has specific limitations as it also presents non-COVID-19 outcomes. This might limit the ability to infer the effectiveness of REGEN-COV against hospitalizations, ICU admissions, and mortality due to COVID-19. Thus, there is a need to further explore the effectiveness of REGEN-COV in health outcomes related to COVID-19, from a massive nationwide intervention setting.
The Israeli Ministry of Health began a nationwide campaign to administer REGEN-COV at a dose of 1200 mg on September 22, 2021, during a period in which the Delta variant was the dominant variant in Israel, and Israel’s fourth wave of COVID-19 was at its peak. As part of this campaign, Clalit Health Services (CHS), Israel’s largest healthcare organization, proactively offered REGEN-COV treatment at home to eligible members who were diagnosed with COVID-19. Members were eligible if they were within 5 days of their first positive Polymerase Chain Reaction (PCR) test and were determined to be at high risk for severe illness, but had not yet developed severe COVID-19. The determination of risk was made by clinicians at the point of care, based on patient’s overall likelihood of deterioration to severe illness. The likelihood of deterioration to severe illness was evaluated using a simple score-based model that was developed by Clalit Health Services and adopted by the Israeli Ministry of Health11.
The present study aims to evaluate the real-world effectiveness of REGEN-COV treatment in preventing COVID-19-related hospitalization, severe illness, and death. A retrospective cohort study was conducted using the data repositories of Israel’s largest healthcare organization. Patients diagnosed with COVID-19 between September 19, 2021, and December 8, 2021, who were treated with REGEN-COV were matched to patients diagnosed with COVID-19 between July 1, 2021, and December 8, 2021, who were not treated with REGEN-COV. Analysis was performed using Cox regression, with estimated treatment effectiveness defined as one minus the hazard ratio. A subgroup analysis was conducted as a secondary analysis by age group (<60 or ≥60 years old).
Results
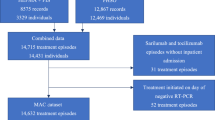
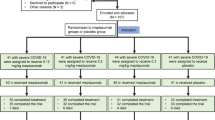
In total, 162,795 CHS members tested positive for COVID-19 between July 1 and December 8, 2021. Of this population, 306 were enrolled in our cohort and treated with REGEN-COV between September 19, 2021, and December 8, 2021, and 162,489 were non-treated with REGEN-COV. Exclusion criteria for both treated and non-treated with REGEN-COV included: participants aged <12 years old (n = 2610); participants without continuous CHS membership (n = 3562); participants who previously had the omicron variant (n = 37); participant data that had invalid information related to COVID-19 (e.g., death date, hospitalization date) (n = 514); participants hospitalized before the index date(n = 4); missing data on participant smoking status (n = 1750), and missing data on BMI (n = 18,857). 135,458 were eligible for inclusion in the study, and patients were matched on a 1:5 ratio. Of those, 149 controls were excluded before contributing follow-up time as they developed one of the outcomes before their treated match could receive the treatment. The final analysis included 289 patients treated with REGEN-COV and 1296 non-treated matched patients (Supplemental Fig. 1).
The median age of the population was 67 years (interquartile range: 58–74 years), and 48% were men. Patients treated with REGEN-COV were more likely to be smokers compared to those who were non-treated (14% vs. 11%, respectively) (Table 1). All matched variables were well-balanced after matching between the treated and non-treated groups (Supplemental Fig. 2). The difference between those who were treated with REGEN-COV to non-treated participants (potential controls) is described in Supplemental Table 1. Furthermore, Supplemental Table 1 describes the difference between those who were unmatched and non-treated individuals to matched individuals. The unmatched and non-treated individuals were younger and had fewer chronic conditions.
As compard with non-treated patients, among those treated with REGEN-COV the risk of hospitalization due to COVID-19 decreased by 56.4% (95% CI: 23.7–75.1%); the risk of severe COVID-19 illness decreased by 59.2% (95% CI: 19.9–79.2%); and the risk of COVID-19-related death decreased by 93.5% (95% CI: 52.1–99.1%) (Table 2). A full description of the Cox model, which describes this information, is presented in Supplemental Table 2−4.
The results of the secondary analysis showed that among those aged 60 years or older and treated with REGEN-COV, the risk of hospitalization due to COVID-19 decreased by 57.0% (95% CI: 16.0–75.7%); the risk of severe COVID-19 illness decreased by 61.1% (95% CI: 21.0–76.4%); and the risk of COVID-19-related death decreased by 94.4% (95% CI: 58.8–99.2%). Among those younger than 60 years old, the risk of hospitalization due to COVID-19 decreased by 91.5% (95% CI: 28.2–99.0%). However, due to the rarity of severe COVID-19 and death in this age group, the effectiveness of REGEN-COV for these outcomes could not be accurately estimated (Supplemental Table 5).
The sensitivity analysis results using propensity score matching confirm the main analysis and indicate that REGEN-COV effectively reduces the risk of severe COVID-19 hospitalization due to COVID-19 and mortality due to COVID-19 (Supplemental Table 6).
Discussion
In the current study, we estimated the effectiveness of community-based REGEN-COV treatment for patients newly infected with SARS-CoV-2 (Delta variant) who were determined to be at high risk for severe COVID-19, but who had not yet developed severe disease. Our results indicate that treatment with REGEN-COV was effective in reducing the risk of hospitalization due to COVID-19, severe COVID-19, and COVID-19-related death among patients overall and specifically for those aged 60 years or older.
The results of this real-world study are consistent with the results of the phase-III clinical trial, which showed that treatment with REGEN-COV reduced the risk of hospitalization or death by 70.4% in the 28 days following treatment initiation12. They are also consistent with the results of an observational study that showed a 70% reduction in the need for further treatment among those treated with REGEN-COV9. Importantly, the effectiveness of REGEN-COV has recently been reported to be diminished against the Omicron variant, which has become dominant in many regions worldwide.
The current study had several limitations. First, despite the careful matching of treated and non-treated individuals and the further adjustment in the Cox regression, there exists the possibility of residual confounding, specifically by behavioral factors that were not well-captured in our data. Second, the recruitment of the non-treated patients started 10-weeks earlier than the treated patients, which could result in confounding by calendar time. However, the circumstances in Israel were not different between the first 10-weeks and the remaining study period, so we do not expect this to result in substantial bias. Third, there is the possibility of selection bias among those treated with REGEN-COV compared to those who refused to be treated with REGEN-COV and were included as controls. However, only a small number of the control population is composed of individuals who refused treatment, which limits the potential bias. Fourth, REGEN-COV is less effective against the Omicron variant; the infectiousness and severity of Omicron were three times higher compared to the original Wuhan strain13. Finally, the number of treated participants is relatively small and the number of outcomes is small which lead to imprecise estimates.
This is the first study to uniquely characterize the effectiveness of REGEN-COV from real-world data that is based on a nationwide cohort enrollment from a massive treatment campaign, showing the effectiveness of a national-scale intervention using antivirals. The cohort was based on a large representative cohort that covers over half of the Israeli population, providing novel evidence regarding the effectiveness of a national treatment campaign in which treatment was offered equally to all eligible patients. The study results reveal high effectiveness of REGEN-COV in treating high-risk COVID-19 patients recently infected with the Delta variant. With many individuals remaining unvaccinated and breakthrough infections occurring among the vaccinated, effective treatment for COVID-19 remains vital.
Methods
Data sources
Data was extracted from the CHS database. CHS is the largest integrated payer-provider healthcare organization in Israel. The CHS database contains extensive medical histories of CHS’s 4.7 million members, including COVID-19 test results and outcomes. These data repositories have been previously described in detail14, 15.
Population and study design
We conducted a cohort study using CHS data to estimate the real-world effectiveness of REGEN-COV in preventing severe COVID-19-related outcomes. Eligibility criteria included: a documented first positive SARS-CoV-2 polymerase-chain-reaction (PCR) test result; a determination of being high risk for severe COVID-19 based on medical history and clinical characteristics; age 12 years-old or older; and at least one year of continuous CHS membership as of the infection date. We excluded patients who were known to be infected with the Omicron variant. We assessed Omicron infections based on sequencing of viral samples or the S-gene target failure (SGTF) technique; the prevalence of Omicron during the study period was negligible. We also excluded patients with invalid outcome data (e.g. invalid hospitalization data, etc) and those who received a positive PCR result during hospitalization for another condition.
To emulate a target trial, treated patients were individually matched with non-treated patients. Treated patients were those with a first positive PCR test result obtained between September 19, 2021 and December 8, 2021 and who received REGEN-COV treatment: Non-treated patients were those who obtained a first positive PCR test result between July 1, 2021 and December 8, 2021 and who did not receive REGEN-COV treatment. The recruitment period for the non-treated patients was a few weeks longer than for the treated patients in order to increase the sample size of the non-treated group and allow for a 1:5 matching of treated to non-treated individuals. Matching was performed using an optimal matching scheme. The Mahalanobis distance metric was used for continuous variables, and exact matching was used for categorical variables16, 17. Optimal matching minimizes the overall pairwise distances without dependency on the order of matching.
REGEN-COV was indicated but not provided to certain high-risk individuals for a range of possible reasons. These reasons included: the patient was diagnosed in the weeks before REGEN-COV was being offered by the healthcare system; logistic complexity prevented the distribution of the treatment to the patient’s home; or the patient refused to receive the treatment.
Outcomes and Follow-up
Three outcomes were examined: 1) COVID-19-related hospitalization, 2) severe COVID-19 illness, and 3) death due to COVID-19, all the outcomes were defined as per the Israeli Ministry of Health. The treated and non-treated patients were followed from the assigned index date. The index date for the treated patients was defined as the date of REGEN-COV treatment. Non-treated and matched patients were given an index date based on the relative time from infection diagnosis to treatment of the matched treated patient. For example, if the treated patient received REGEN-COV two days after their positive PCR test result, the index date for the matched non-treated patient was set to two days after their positive PCR test result. Follow-up ended with the occurrence of the outcome or at 28-days following the index date.
Covariates adjustment
Adjustments were performed in two phases. First, the treated and non-treated patients were matched on an initial set of potential confounders. Covariates included in the analysis were based on the input of domain experts and the scientific literature related to the factors associated with the COVID-19 health outcomes and the likelihood of receiving REGEN-COV18, 19.
Subjects were matched based on: age; sex; population sector (Jewish, Arab, Ultra-Orthodox); socioeconomic status (SES, based on place of residence and categorized into 20 levels); body mass index (BMI as a continuous variable); immunosuppression status; pregnancy; and calendar week of first vaccination dose.
Further adjustment was done using a Cox Proportional Hazards Regression. Confounders that were adjusted for in the model included: age; sex; population sector, SES. (as stated above); BMI (as a categorical variable: underweight, normal and obese); the number of flu vaccines received within the five years prior to COVID-19 diagnosis; smoking status; recent full vaccination status; and calendar week of first vaccination dose. We also adjusted for the chronic conditions (e.g. cardiovascular disease, diabetes, respiratory disease, are hypertension) described in Supplemental Table 7. The regression included some of the variables that were used in matching to better control possible residual confounding, for reasons further detailed under the statistical analysis section.
All variables were extracted according to the most recently documented value before the positive testing date, as recorded in the patients’ medical records. Full variable definitions are presented in Supplemental Table 7.
Matched non-treated individuals who experienced an outcome between their positive PCR test date and their assigned index date were excluded. Because the index date was only set after matching (based on the matched treated counterpart’s timing), this exclusion could only happen after matching.
Statistical analysis
Following matching, Cox proportional hazards models were fit for each outcome, adjusting for the abovementioned potential confounders. We performed a collinearity test and excluded the number of vaccination doses received due to high collinearity with a recent full vaccination.
We report one minus the hazard ratio (HR) with 95% confidence intervals as the measure of treatment effectiveness. The Cox modeling included some variables that were already used for the matching process for two reasons. First, some of the variables were continuous, and the matching was not exact. Second, not all the treated subjects had the same number of controls due to the exclusion of controls post-matching.
Missing data are rare occurrence in CHS database for the variables used; thus, we used a complete case analysis.
A subgroup analysis by age group (<60 or ≥60 year old) was conducted as a secondary analysis.
Sensitivity analysis
To assess the sensitivity of our results to the matching method, we repeated the analysis with a different matching approach - Propensity Score Matching (PSM). Multivariable logistic regression was conducted to generate propensity scores. The propensity score model included age, population sector, sex, SES, BMI, immunosuppression status, pregnancy, and first vaccination dose status as a surrogate for health-seeking behavior. For each treated subject, we matched a non-treated subject, based on propensity score similarity (1:5 matching ratio).
Ethics
This study was approved by the CHS Institutional Review Board (0052-20-COM2).
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
Due to national and organizational data privacy regulations, individual-level data such as those used for this study cannot be shared. Access to the data used for this study can be made available upon request, subject to an internal review to ensure that participant privacy is protected, and subject to completion of a data sharing agreement, approval from the institutional review board of CHS and institutional guidelines and in accordance with the current data sharing guidelines of CHS and Israeli law. Pending the aforementioned approvals, data sharing will be made in a secure setting, on a per-case-specific manner, as defined by the chief information security officer of CHS.
Code availability
The analytic code is available at https://github.com/clalitresearch/Regeneron_Effectiveness.
References
Zhu, N. et al. A Novel Coronavirus from Patients with Pneumonia in China, 2019. N. Engl. J. Med 382, 727–733 (2020).
Medicine JHU: COVID-19 DashBoard MD, USA, Johns Hopkins University & Medicine, 2022.
Denford S. et al: Exploration of attitudes regarding uptake of COVID-19 vaccines among vaccine hesitant adults in the UK: A qualitative analysis. medRxiv:2021.12.23.21268325, 2021.
Bergwerk, M. et al. Covid-19 Breakthrough Infections in Vaccinated Health Care Workers. N. Engl. J. Med. 385, 1474–1484 (2021).
FDA: FDA authorizes REGEN-COV monoclonal antibody therapy for post-exposure prophylaxis (prevention) for COVID-19, U.S. FOOD& DRUG Administration 2021.
O’Brien M. P. et al. Subcutaneous REGEN-COV Antibody Combination for Covid-19 Prevention. medRxiv:2021.06.14.21258567, 2021.
Weinreich D. M. et al. REGEN-COV Antibody Combination and Outcomes in Outpatients with Covid-19. N. Engl. J. Med. 385, e81 (2021).
Verderese J. P., et al. Neutralizing Monoclonal Antibody Treatment Reduces Hospitalization for Mild and Moderate Coronavirus Disease 2019 (COVID-19): A Real-World Experience. Clin. Infect. Dis. 74, 1063–1069 (2021).
Kakinoki Y., et al. Impact of Antibody Cocktail Therapy Combined with Casirivimab and Imdevimab on Clinical Outcome for Covid-19 patients in A Real-Life Setting: A Single Institute Analysis. medRxiv, 2021.
Razonable, R. R. et al. Casirivimab–Imdevimab treatment is associated with reduced rates of hospitalization among high-risk patients with mild to moderate coronavirus disease-19. EClinicalMedicine 40, 101102 (2021).
Dagan N., et al: A score-based risk model for predicting severe COVID-19 infection as a key component of lockdown exit strategy. medRxiv:2020.05.20.20108571, 2020.
Weinreich D. M., et al: REGEN-COV Antibody Cocktail in Outpatients with Covid-19. medRxiv, 2021.
Gao, S. J., Guo, H. & Luo, G. Omicron variant (B. 1.1. 529) of SARS‐CoV‐2, a global urgent public health alert! J. Med. Virol. 94, 1255 (2022).
Barda, N. et al. Safety of the BNT162b2 mRNA Covid-19 vaccine in a nationwide setting. N. Engl. J. Med. 385, 1078–1090 (2021).
Dagan, N. et al. BNT162b2 mRNA Covid-19 Vaccine in a Nationwide Mass Vaccination Setting. N. Engl. J. Med. 384, 1412–1423 (2021).
Ho D., Imai K., King G., Stuart E., Greifer N. Package ‘MacthIt’. Nonparametric Preprocessing for Parametric Causal Inference. 1–62 2021.
Stuart E. A., et al. MatchIt: nonparametric preprocessing for parametric causal inference. J. Stat. Software 42, 1–282011.
Barda N., et al. Performing risk stratification for COVID-19 when individual level data is not available–the experience of a large healthcare organization. medRxiv, 2020.
Gao, Y. D. et al. : Risk factors for severe and critically ill COVID‐19 patients: a review. Allergy 76, 428–455 (2021).
Acknowledgements
This study was supported by the Ivan and Francesca Berkowitz Family Living Laboratory Collaboration at Harvard Medical School and Clalit Research Institute.
Author information
Authors and Affiliations
Contributions
S.H., Y.B.S., N.D., B.Y.R., N.B., E.K., and R.D.B. conceived and designed the study. Y.B.S., N.D., E.K., N.B., participated in data extraction and analysis. S.H., Y.B.S., N.D., B.Y.R., N.B., E.K., A.L, S.S, S.Y., R.D.B, D.N., A.P. wrote the manuscript. S.S., S.Y., D.N, A.P, provided clinical guidance. All authors critically reviewed the manuscript and decided to proceed with publication. R.D.B. vouches for the data and analysis. R.D.B. D.N. A.P contributed equally as senior authors to this study.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks the anonymous reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hayek, S., Ben-shlomo, Y., Dagan, N. et al. Effectiveness of REGEN-COV antibody combination in preventing severe COVID-19 outcomes. Nat Commun 13, 4480 (2022). https://doi.org/10.1038/s41467-022-32253-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-022-32253-9
This article is cited by
-
Prospects of Innovative Therapeutics in Combating the COVID-19 Pandemic
Molecular Biotechnology (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.