Abstract
Anti tumour necrosis factor (anti-TNF) drugs increase the risk of serious respiratory infection and impair protective immunity following pneumococcal and influenza vaccination. Here we report SARS-CoV-2 vaccine-induced immune responses and breakthrough infections in patients with inflammatory bowel disease, who are treated either with the anti-TNF antibody, infliximab, or with vedolizumab targeting a gut-specific anti-integrin that does not impair systemic immunity. Geometric mean [SD] anti-S RBD antibody concentrations are lower and half-lives shorter in patients treated with infliximab than vedolizumab, following two doses of BNT162b2 (566.7 U/mL [6.2] vs 4555.3 U/mL [5.4], p <0.0001; 26.8 days [95% CI 26.2 – 27.5] vs 47.6 days [45.5 – 49.8], p <0.0001); similar results are also observed with ChAdOx1 nCoV-19 vaccination (184.7 U/mL [5.0] vs 784.0 U/mL [3.5], p <0.0001; 35.9 days [34.9 – 36.8] vs 58.0 days [55.0 – 61.3], p value < 0.0001). One fifth of patients fail to mount a T cell response in both treatment groups. Breakthrough SARS-CoV-2 infections are more frequent (5.8% (201/3441) vs 3.9% (66/1682), p = 0.0039) in patients treated with infliximab than vedolizumab, and the risk of breakthrough SARS-CoV-2 infection is predicted by peak anti-S RBD antibody concentration after two vaccine doses. Irrespective of the treatments, higher, more sustained antibody levels are observed in patients with a history of SARS-CoV-2 infection prior to vaccination. Our results thus suggest that adapted vaccination schedules may be required to induce immunity in at-risk, anti-TNF-treated patients.
Similar content being viewed by others
Introduction
Vaccination programmes have reduced SARS-CoV-2 transmission, hospitalisation and deaths1. Patients treated with immunosuppressive drugs were excluded from the original trials for COVID-19 vaccines2,3. Consequently, data relating to the magnitude and durability of immune responses and subsequent vaccine effectiveness in this population are limited4.
Drugs targeting tumour necrosis factor (TNF), such as infliximab, are the most frequently prescribed biologic therapies used in the treatment of immune-mediated inflammatory disorders (IMIDs). Observational studies indicate that most patients with inflammatory bowel disease (IBD), an archetypal IMID, mount serological responses following SARS-CoV-2 vaccines, although most were underpowered to discern the impact of specific drugs, including immunomodulators (azathioprine, mercaptopurine and methotrexate) and/or biologic therapies5,6,7,8. We reported that antibody responses following SARS-CoV-2 infection9,10 or a single dose of either the BNT162b2 or ChAdOx1 nCoV-19SARS-CoV-2 vaccines were impaired in anti-TNF treated patients when compared to vedolizumab-treated patients11. Vedolizumab, is a gut-selective anti-integrin α4β7 monoclonal antibody that, unlike anti-TNF drugs, is not associated with increased susceptibility to systemic infection or attenuated serological responses to vaccination12.
In this work, we show that anti-SARS-CoV-2 spike antibody responses are attenuated and less durable following two doses of the BNT162b2 and ChAdOx1 nCoV-19 SARS-CoV-2 vaccines in infliximab-treated compared with vedolizumab-treated patients with IBD. Irrespective of biologic drug type, one-fifth of all patients do not mount a T cell response and a minority mount neither antibody nor T cell responses. Breakthrough SARS-CoV-2 infections, which are associated with lower antibody levels after the second dose of vaccine, are more common and occur earlier in infliximab-treated patients. Higher and more sustained antibody levels are observed in patients with a history of SARS-CoV-2 infection. Further work to define immunity after third primary and booster vaccine doses is needed to inform the need for adapted vaccination schedules in at-risk anti-TNF treated patients.
Results
Patient characteristics
Between September 22, 2020 and December 23, 2020, 7226 patients were recruited to the CLARITY study from 92 UK hospitals10. In this analysis we included 2279 infliximab-treated and 1031 vedolizumab-treated participants without a history of prior SARS-CoV-2 infection, who had received uninterrupted biologic therapy since recruitment and had an antibody test between 14 and 70 days after the second dose of either the BNT162b2 and ChAdOx1 nCoV-19 SARS-CoV-2 vaccines. Participant characteristics are shown in Table 1.
Additional analyses are presented for a subset of 211 infliximab-treated and 71 vedolizumab-treated patients included in our T cell experiments (Supplementary Table 1), and a further 530 infliximab-treated and 224 vedolizumab-treated participants who had a history of SARS-CoV-2 infection before vaccination (Supplementary Table 2).
Anti-SARS-CoV-2-spike (S) antibody level following two doses of SARS-CoV-2 vaccine
Overall, the geometric mean [geometric SD] of anti-S receptor-binding domain (RBD) antibody concentration was higher in recipients of two doses of the BNT162b2 than ChAdOx1 nCoV-19 vaccines (1084.1 U/mL [7.6] vs 289.9 U/mL[5.2], p < 0.0001). Anti-S RBD antibody concentrations were lower in patients treated with infliximab than in those treated with vedolizumab, following a second dose of BNT162b2 (566.7 U/mL [6.2] vs 4555.3 U/mL [5.4], p < 0.0001) and ChAdOx1 nCoV-19 (184.7 U/mL [5.0] vs 784.0 U/mL [3.5], p < 0.0001) vaccines (Fig. 1).
The wider bar represents the geometric mean, while the narrower bars are drawn one geometric standard deviation on either side of the geometric mean. Based on published data using neutralisation assays threshold shown of 15 U/mL was used to determine seroconversion11. The biologic treatment infliximab is shown in green and vedolizumab in orange. The number of individuals tested for each group are shown in black at the top of each panel. Source data are provided as a Source Data file.
Crude sensitivity analyses, excluding patients treated with a concomitant immunomodulator, confirmed lower anti-S RBD antibody concentrations in patients treated with infliximab alone versus vedolizumab alone (BNT162b2 809.1 U/mL [4.9] vs 4691.5 U/mL [5.9], p < 0.0001, ChAdOx1 nCoV-19 178.5 U/mL [4.6] vs 778.0 U/mL [3.5], p < 0.0001).
After propensity matching for immunomodulator use and the other factors associated with choice of biologic, we confirmed lower anti-S RBD antibody concentrations in infliximab-treated compared to vedolizumab-treated patients (BNT162b2 600.1 U/mL [6.0] vs 4674.1 U/mL [4.7], p < 0.0001, ChAdOx1 nCoV-19 195.2 U/mL [4.5] vs 779.2 U/mL [3.6], p < 0.0001) (Supplementary Table 3).
Multivariable linear regression analyses in patients without prior SARS-CoV-2 infection confirmed that antibody concentrations were reduced six and four-fold in infliximab-treated compared with vedolizumab-treated participants who received the BNT162b2 (fold change [FC] 0.15 [95% CI 0.12, 0.19], p < 0.0001) and ChAdOx1 nCoV-19 ([FC] 0.24 [95% CI 0.21, 0.28], p < 0.0001) vaccines (Fig. 2a, b respectively). Age ≥60 years and Crohn’s disease were also independently associated with lower anti-S RBD antibody concentrations in vaccinated participants. Thiopurine or methotrexate use was independently associated with lower anti-S RBD antibody concentrations in participants who received the BNT162b2, but not the ChAdOx1 nCoV-19, vaccine. Current smoking, non-white ethnicity and steroid use were associated with lower anti-S RBD antibody concentrations in participants who received the ChAdOx1 nCoV-19 but not the BNT162b2 vaccine. To assess the effect of vaccine type on antibody responses, we combined our response data in a model that included vaccine type in addition to the significant factors above. Vaccination with the BNT162b2 vaccine compared to the ChAdOx1 nCoV-19 was independently associated with a 3.7 fold [95% CI 3.29–4.12] higher anti-S RBD antibody concentration (p < 0.0001) (Fig. 2c).
Exponentiated coefficients of the linear regression model of log anti-S RBD antibody concentration in participants who received a BNT162b2 vaccine. b ChAdOx1 nCoV-19 vaccine. c either the BNT162b2 or ChAdOx1 nCoV-19 vaccine. The resultant values represent the fold change of antibody concentration associated with each variable (black square). The horizontal solid line through each square represents the 95% confidence interval. Each vaccine was modelled separately, and then a further model was created using all available data. The vertical dotted line represents a fold change of 1. Tests were two-tailed. p values were derived from linear regression using the t-test statistic and reported without correction for multiple testing. Source data are provided as a Source Data file. UC ulcerative colitis, IBDU IBD unclassified.
Seroconversion rates after the first vaccine dose were lower in infliximab-treated compared to vedolizumab-treated participants (Fig. 1). However, administration of a second vaccine dose resulted in a >100-fold and >25-fold increase in antibody concentrations in recipients of the BNT162b2 and ChAdOx1 nCoV-19 vaccines, respectively (Fig. 1). Overall, more infliximab-treated than vedolizumab-treated patients failed to seroconvert after their second vaccine dose (5.9% vs 1.3%, p < 0.0001). Seroconversion rates stratified by biologic therapy and vaccine type are reported in Supplementary Table 4.
Anti-spike T cell responses following two doses of BNT162b2 and ChAdOx1 nCoV-19 SARS-CoV-2 vaccines
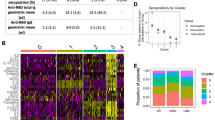
There were no significant differences in the magnitude of anti-spike T cell responses observed in infliximab-treated compared with vedolizumab-treated patients after one or two doses of either vaccine (Fig. 3a). The proportion of patients failing to mount detectable T cell responses were similar in both groups (infliximab 19.6% vs. vedolizumab 19.2%). For recipients of one and two doses of the BNT162b2 vaccine, there was a modest positive correlation between T cell responses and antibody concentration. This association was not observed in recipients following either dose of the ChAdOx1 nCoV-19 vaccine (Fig. 3b). When T cell responses were ranked by magnitude of antibody responses, most patients who did not mount an antibody response after the first vaccine dose (indicated by the dark grey bar) had a detectable T cell response (Fig. 4). In addition to the uncoupling of the T cell and antibody responses demonstrated, this analysis emphasised that about one-fifth of participants made no T cell responses irrespective of vaccine used (indicated by the light grey bars). Moreover, a minority of individuals (3/67) 4.5% for BNT162b2 and (1/56) 1.8% for ChAdOx1 nCoV-19 vaccines carry neither detectable antibody nor T cell responses after two doses of vaccine (Figs. 3b, 4).
a Spike MEP T cell responses SFC per 106 PBMC stratified by vaccine platform, biologic therapy (infliximab vs vedolizumab) and the number of vaccine doses. The horizontal bar represents the geometric mean and the narrow bars represent one geometric standard deviation on either side of the geometric mean. The number of T cell responders / total number of individuals tested are shown in black at the top of each panel. b Scatterplot demonstrating the correlation between T cell responses against spike MEP pool (SFC per 106 PBMC) and anti-SARS-CoV-2 spike antibody concentration after the first (LHS) and second (RHS) dose of BNT162B2 (top) and ChAdOx1 nCoV-19 (bottom) vaccine. The number of non-T cell responders/total number of individuals tested is shown in blue on the bottom RHS of each panel. The shaded grey band represents the 95% confidence interval. The horizontal dotted line in b represents a threshold of 15 U/mL of anti-S1 SARS-CoV-2 antibody. The tests were two-tailed and p values were reported without correction for multiple testing. The biologic infliximab is shown in green and vedolizumab is shown in orange. Source data are provided as a Source Data file. MEP mapped epitope peptide, SFC spot forming cells, PBMC peripheral blood mononuclear cell, LHS left-hand side, RHS right-hand side, R Spearman’s rank correlation.
Top panel shows T cell responses to spike, and the bottom panel shows anti-S RBD responses plotted for individual study participants ordered by increasing magnitude of anti-S RBD antibody concentration (U/mL). The vertical dark grey bars at the LHS of the panels indicate individuals with no anti-S RBD response. The vertical light grey bars in the panels indicate individuals with no T cell response. The horizontal dotted line represents a threshold shown of 15 U/mL of anti-S RBD. Source data are provided as a Source Data file. LHS left-hand side, MEP mapped epitope peptide, SFC spot forming cells.
Durability of antibody responses following two doses of BNT162b2 and ChAdOx1 nCoV-19 SARS-CoV-2 vaccines
The estimated half-life of anti-S RBD antibodies was shorter in participants receiving the BNT162b2 compared to the ChAdOx1 nCoV-19 vaccines (30.8 days [95% CI 30.3–31.5] vs 40.5 days [95% CI 39.2–41.6], p value <0.0001). When stratified by biologic, half-life estimates were shorter in infliximab-treated than vedolizumab-treated patients following two doses of BNT162b2 (26.8 days [95% CI 26.2–27.5] vs 47.6 [95% CI 45.5–49.8], p value <0.0001) and ChAdOx1 nCoV-19 (35.9 days [95% CI 34.9–36.8] vs 58.0 days [95% CI 55.0–61.3], p value <0.0001) (Supplementary Fig. 1 and Supplementary Table 5).
Overall, following two doses of either vaccine, anti-S RBD antibodies showed minimal decay to the last follow-up in patients treated with vedolizumab (Fig. 5 and Supplementary Fig. 2) and were similar to those observed in participants in the Virus Watch community cohort (Supplementary Fig. 3). However, in infliximab-treated participants, the geometric mean concentrations dropped to the seroconversion threshold by about 25 weeks after the second dose irrespective of the vaccine administered (Fig. 5). Infliximab compared to vedolizumab treatment, current smoking and white ethnicity were associated with a faster fall in anti-S RBD antibody concentration below the seroconversion threshold. (Supplementary Figs. 4, 5).
Geometric means are calculated using a rolling 15-day window (i.e. 7 days on either side of the day indicated). The shaded areas represent the 95% confidence intervals of the geometric means. The horizontal blue line represents the seroconversion threshold (15 U/mL). The number of participants included at each time point is presented in Supplementary Fig. 2. Overall, data from 4474 participants with no history of prior infection (3029 on infliximab and 1445 on vedolizumab) and 1179 participants with a history of prior infection (833 on infliximab and 346 on vedolizumab) were included in this graph between 22 weeks before and 29 weeks after the second vaccine dose. The biologic treatment infliximab is shown in green and vedolizumab is shown in orange. Source data are provided as a Source Data file.
Breakthrough SARS-CoV-2 infections following two doses of vaccine
Of 5123 participants without polymerase chain reaction (PCR)-positive or serological evidence of prior SARS-CoV-2 infection, 267 had a first positive SARS-CoV-2 PCR test 2 or more weeks after the second vaccine dose. Overall, 89.2% patients were symptomatic: the most commonly reported symptoms were fatigue (73.7%), anosmia/ageusia (71.4%), fever (57.1%), cough (54.9%), myalgia (45.9%), hoarse voice (30.8%), confusion (27.8%) and chest pains (23.3%). Overall, 1.2% (3/253) of participants with PCR-confirmed infection were hospitalised because of COVID-19.
Breakthrough SARS-CoV-2 infections were more frequent (5.8% (201/3441) vs 3.9% (66/1682), p = 0.0039) and the time to breakthrough shorter in patients treated with infliximab than vedolizumab (p = 0.0027) (Fig. 6b). In contrast biologic class did not impact on time to PCR-confirmed infection prior to vaccination (p = 0.63) (Fig. 6a). In a model that included biologic and vaccine type, shorter time to breakthrough infection was associated with infliximab (Hazard Ratio (HR) 1.52 [95% CI 1.15–2.01], p = 0.003) and having received the ChAdOx1 nCoV-19 (HR 1.49 [95% CI 1.15–1.92], p = 0.0023) vaccine. Geometric mean [geometric SD] anti-S RBD antibody concentrations measured 2 to 10 weeks after a second vaccine dose were significantly lower in participants who subsequently had a PCR-confirmed breakthrough SARS-CoV-2 infection: for every tenfold rise in anti-S RBD antibody concentration we observed a 0.8-fold reduction in odds of breakthrough infection ([95% CI 0.70–0.99], p = 0.03).
a The time to PCR-confirmed SARS-CoV-2 infection in participants who have not received any dose of either vaccine stratified by biologic therapy (infliximab vs vedolizumab). b The time to a PCR-confirmed SARS-CoV-2 breakthrough infection in participants following two doses of either vaccine stratified by biologic therapy. The biologic treatment infliximab is shown in green and vedolizumab in orange. The number of participants at each time point are displayed in black at the bottom of each figure. P values are calculated using the log-rank test. Source data are provided as a Source Data file.
Antibody responses in patients with prior SARS-CoV-2 infection
Amongst patients with a history of SARS-CoV-2 infection before vaccination, geometric mean [SD] anti-S RBD antibody concentrations were lower in infliximab-treated compared with vedolizumab-treated patients after a second dose of BNT162b2 (1330.0 U/mL [5.3] vs 7169.5 U/mL [4.6], p < 0.0001) and ChAdOx1 nCoV-19 (399.7 U/mL [5.4] vs 2077.3 [4.6] p < 0.0001) vaccines. In all patients, antibody concentrations following vaccination were higher in patients without a history of SARS-CoV-2 infection (Fig. 1). Irrespective of vaccine or biologic type, minimal decay of anti-S RBD antibodies were observed up to a follow-up of 21 weeks.
Discussion
We have shown that in infliximab-treated patients, anti-SARS-CoV-2 spike antibody responses are attenuated following two doses of the BNT162b2 and ChAdOx1 nCoV-19SARS-CoV-2 vaccines. One-fifth of both infliximab-treated and vedolizumab-treated patients did not mount a T cell response and a small subset of patients had neither antibody nor T cell responses. Antibody half-lives were shorter in infliximab-treated patients. Breakthrough SARS-CoV-2 infections were more common and occurred earlier in infliximab-treated patients who received the ChAdOx1 nCoV-19 vaccine. The risk of breakthrough infection was predicted by lower antibody levels after the second dose of the vaccine. Irrespective of biologic treatment, higher and more sustained antibody levels were observed in patients with a history of SARS-CoV-2 infection.
Sustained antibody responses observed in vaccinated patients with a history of prior SARS-CoV-2 infection indicate that third antigen exposure enhances the serological response. This supports the rationale for prioritising a third dose of vaccine to clinically vulnerable patient populations13,14,15,16, who otherwise may face further periods of social distancing or hospitalisation following infection. Whilst drawing direct comparisons between IBD patients and patients treated with more potent chemotherapies is limited by the degree to which patients are immunosuppressed, data from solid organ transplant recipients shows that a third dose of vaccine also leads to sustained immune responses17.
Irrespective of biologic or immunosuppressant use, and in keeping with the original trials2,18, the highest antibody responses were seen in recipients of the BNT162b2 vaccine. Like in the general population, these responses waned more quickly than in the recipients of the ChAdOx1 nCoV-19 vaccine19. Unlike the general population20, but similar to renal transplant recipients4, we did not observe differences in T cell ELISpot responses between recipients of the BNT162b2 and ChAdOx1 nCoV-19 vaccines. The differences observed in breakthrough infection by vaccine type reported here are consistent with the differences in efficacy reported in the respective clinical trials2,3,21. The higher peak antibody levels and the lower rate of SARS-CoV-2 breakthrough infections suggest that the BNT162b2 rather than the ChAdOx1 nCoV-19 vaccine should be used for primary vaccination in infliximab-treated patients and, although untested, supports the use of BNT162b2 for third doses in all patients treated with an anti-TNF regardless of the primary vaccine type.
All patients treated with anti-TNF therapy should receive a third primary dose of the SARS-CoV-2 vaccine and our data support recent recommendations that this should occur about 4–8 weeks after the second dose13,14,16 during periods of high transmission in the population. Our data demonstrate that patients treated with vedolizumab and infliximab-treated patients with prior SARS-CoV-2 infection have sustained antibody levels beyond 6 months.
When starting a biologic, it would be reasonable to consider differences in SARS-CoV-2 vaccine response as one of the factors when determining which drug to use. For patients who need to start anti-TNF therapy, the benefits of combination immunomodulator therapy should be weighed against the risk of attenuated vaccine response, and whenever feasible, patients should first receive a SARS-CoV-2 vaccine dose. Further research to determine whether timing third vaccine doses towards the end of anti-TNF treatment cycles when drug levels are lowest leads to greater immunogenicity9 is needed. Other strategies including the temporary discontinuation of immunomodulators22, the use of heterologous vaccines23 and adjuvants including the influenza vaccines (ComFluCOV)24 need to be studied in immunosuppressed patient groups.
The biology underpinning loss of durable antibody responses and uncoupling of the B cell and T cell responses merit further research. TNF is a pleiotropic cytokine and its activities include maturation of antigen-presenting cells, modulation of T cell responses and stimulation of immunoglobulin synthesis25,26,27. TNF neutralisation, or genetic ablation, results in substantial loss of B-cells in primary follicles in germinal centres, reduced numbers of memory B-cells in the periphery but preserved numbers of T cells25. Uncoupling of humoral and T cell immunity to SARS-CoV-2 has been observed in healthy individuals28, and although the relative contributions of memory B cell and T cell responses have yet to be fully defined in SARS-CoV-2 immunity, the preservation of T cell immunity reported here should provide some reassurance for anti-TNF treated patients. However, it is noteworthy that one-fifth made no anti-spike T cell response following two doses of either vaccine. Chronic TNF exposure, a feature of many IMIDs, can render T cells anergic and can be reversed by anti-TNF treatment29. This may in part explain why the magnitude of T cell responses observed in anti-TNF-treated patients in this study did not differ significantly from patients treated with vedolizumab.
Although our data show major differences in the magnitude and durability of antibody responses, we have not assessed the impact of biologic therapy on specific immunoglobulin classes, antibody neutralisation or mucosal immune responses, which may be impaired, in particular, with anti-a4b7 therapy30,31. However, previous studies have demonstrated that anti-RBD antibody levels such as the ones measured in this study, strongly correlate with Wuhan Hu-1 live virus and variant S RBD neutralisation assays32,33, and we have demonstrated here that early antibody responses to vaccination correlates with the subsequent risk of breakthrough infection in immunosuppressed patients.
Infliximab was associated with attenuated, less durable vaccine-induced anti-SARS-CoV-2 spike antibody responses and a 50% increase in subsequent breakthrough SARS-CoV-2 infection. Further work to define immunity after third primary and booster vaccine doses is needed to inform the need for adapted vaccination schedules in at-risk anti-TNF treated patients.
Methods
Patient and settings
impaCt of bioLogic therApy on saRs-cov-2 Infection and immuniTY (CLARITY) IBD is a UK-wide, multicentre, prospective observational cohort study investigating the impact of infliximab and vedolizumab and/or concomitant immunomodulators (azathioprine, mercaptopurine and methotrexate) on SARS-CoV-2 acquisition, illness and immunity in patients with IBD.
Study methods have been previously described10,11. Consecutive patients were recruited at the time of attendance at infusion units between 22 September 2020 and 23 December 2020 (Supplementary Table 1). Patients aged 5 years and over, with a diagnosis of IBD, treated with infliximab or vedolizumab were eligible for inclusion. Follow-up visits coincided with biologic infusions and occurred eight-weekly. Here, we report vaccine-induced antibody responses after the second dose of either the BNT162b2 or ChAdOx1 nCoV-19 vaccines. Participants were eligible for our primary immunogenicity analysis, if they had had an anti-S RBD antibody test between 14 and 70 days after a second-dose vaccine, defined as the second dose of any of the licenced COVID-19 vaccines, 10-14 weeks after the first dose. Anti-S RBD antibody levels were compared with samples from 605 fully vaccinated adult participants from the Virus Watch study, a household community cohort of 10,000 individuals representative of the UK population of England and Wales recruited between 1 June 2020 to 31 August 202119. Peripheral blood mononuclear cells (PBMC) for T cell experiments were collected from patients 4 to 6 weeks after the first and second dose of vaccine at the time of biologic infusions, at selected sites which could facilitate PBMC extraction within 12 h of venepuncture.
Outcome measures
Our primary outcome was anti-S RBD antibodies 2 to 10 weeks after the second dose of the BNT162b2 or ChAdOx1 nCoV-19 vaccines.
Secondary outcomes were:
-
(i)
the proportion of participants who seroconverted
-
(ii)
anti-spike T cell responses in patients following the first and second dose of vaccines
-
(iii)
the durability of vaccine responses
-
(iv)
risk of breakthrough infections two or more weeks after two doses of vaccine
-
(v)
antibody concentrations and seroconversion rates in patients with PCR or serological evidence of past SARS-CoV-2 infection at, or prior, to the post-vaccination serum sample
Variables
Variables recorded by participants were demographics (age, sex, ethnicity, comorbidities, height and weight, smoking status, and postcode), IBD disease activity (PRO2), SARS-CoV-2 symptoms aligned to the COVID-19 symptoms study (symptoms, previous testing, and hospital admissions for COVID-19) and vaccine uptake (type and date of primary vaccination). Study sites completed data relating to IBD history (age at diagnosis, disease duration, and phenotype according to the Montreal classifications, previous surgeries, and duration of current biologic and immunomodulator therapy)10. We linked our data by NHS number or Community Health Index to Public Health England, Scotland, and Wales archive dates and results of all SARS-CoV-2 PCR tests undertaken and vaccines administered. Data were entered electronically into a purpose-designed REDCap database hosted at the Royal Devon and Exeter NHS Foundation Trust34. Participants without access to the internet or electronic device completed their questionnaires on paper case record forms that were subsequently entered by local research teams.
Laboratory methods
To determine antibody responses specific to vaccination we used the Roche Elecsys Anti-SARS-CoV-2 spike (S) immunoassay35 alongside the nucleocapsid (N) immunoassay36. This double sandwich electrochemiluminescence immunoassay uses a recombinant protein of the receptor-binding domain on the spike protein as an antigen for the determination of antibodies against SARS-CoV-2. Sample electrochemiluminescence signals are compared to an internal calibration curve and quantitative values are reported as units (U)/mL. In-house assay validation experiments on the Roche Elecsys Anti-SARS-CoV-2 spike (S) immunoassay were performed on 20 samples from healthy individuals who have been vaccinated. This demonstrated:
-
i.
The intra-assay and inter-assay coefficient of variation were 1.3% and 5.6%, respectively
-
ii.
Anti-SARS-CoV-2 (S) antibodies were stable in uncentrifuged blood and serum at ambient temperature for up to seven days permitting postal transport
-
iii.
No effect was observed on recovery of anti-SARS-CoV-2 (S) antibodies following four freeze/thaw cycles
-
iv.
No analytical interference was observed for the detection of anti-SARS-CoV-2 (S) with infliximab or vedolizumab up to 10,000 and 60,000 mg/L, respectively, or with anti-drug antibodies to infliximab or vedolizumab up to 400 and 38 AU/mL, respectively (data not shown).
Seroconversion was defined at a threshold of 15 U/mL. ElecSys Anti-SARS-CoV-2 spike (S) RBD concentrations of greater than or equal to 15 U/ml are associated with neutralisation of ≥20% with a positive predictive value of 99.10% (95% CI: 97.74–99.64)11.
At the entry to CLARITY IBD and at follow-up visits, all patients were tested for previous SARS-CoV-2 infection using the Roche Elecsys anti-SARS-CoV-2 (N) immunoassay. We have previously reported that anti-N antibody responses following SARS-CoV-2 natural infection are impaired in patients treated with infliximab or vedolizumab11. As such, a threshold 0.12 times above the cut-off index was set, using receiver operator characteristic curve and area under the curve analysis of anti-N antibody results from participants two weeks following a PCR-confirmed infection to maximise specificity, beyond which patients were deemed to have had prior SARS-CoV-2 infection (Supplementary Fig. 6). Patients with a PCR test confirming SARS-CoV-2 infection at any time prior to vaccination were deemed to have evidence of past infection irrespective of any antibody test result. Breakthrough infections were defined by a positive SARS-CoV-2 PCR test 2 or more weeks after the second vaccine dose.
Peripheral blood mononuclear cell isolation
Whole blood was collected in lithium heparin tubes and PBMCs were isolated by density-gradient centrifugation using LymphoprepTM (Stem Cell Technologies) layered onto SepMateTM (Stem Cell Technologies) tubes. PBMC isolation was performed within 12 h of venepuncture. Purified PBMCs were cryopreserved in 10% DMSO/50% FBS and stored in liquid nitrogen pending batch analysis.
Spike-peptide specific T cell responses
IFN-γ T cell ELISpot assays were performed using pre-coated plates (Mabtech 3420-2APT) and using the protocol described previously28,32. Two-hundred thousand cells were seeded per well and cells were stimulated with a peptide pool, containing 18 peptides derived from SARS-CoV-2 spike protein37 at a concentration of 10 μg/ml/peptide; the peptide pool utilises a mapped epitope pool (MEP) or 12–20mer peptides, mapped as eliciting high-prevalence CD4 responses covering diverse HLA-II haplotypes28,32. Use of this spike MEP in otherwise healthy SARS-CoV-2 seropositive individuals elicits a T cell response in 83% of individuals at 16–18 weeks after natural SARS-CoV-2 infection and 91% of healthy individuals 2–3 weeks after two-dose vaccination with seronegative individuals showing a level of response indistinguishable from pre-pandemic controls28,32. Plates were cultured for 18–20 h before development and data were collected using an AID classic ELISpot plate reader (Autoimmun Diagnostika GMBH). Results are expressed as differences in (delta) spot forming cells (SFC) per 106 PBMC between peptide stimulation and a media-only control. A response below 2 standard deviations of the media-only control wells was deemed to be a null response. Data were excluded if the response to the positive control anti-CD3 stimulation was <200 SFC per 106 PBMCs.
Sample size
The sample size for CLARITY IBD was based on the number of participants required to demonstrate a difference in the impact of infliximab and vedolizumab on seroprevalence and seroconversion following SARS-CoV-2 infection, with an estimated background seroprevalence of 0.05. We calculated that a sample of 6970 patients would provide 80% power to detect differences in the seroprevalence of SARS-CoV-2 antibodies in infliximab-treated compared with vedolizumab-treated patients, whilst controlling for immunomodulator status at the 0.05 significance level.
Statistical analyses
Analyses were undertaken using R 4.1.2 (R Foundation for Statistical Computing, Vienna, Austria). All tests were two-tailed and p values were reported without correction for multiple testing. P values <0.05 were considered significant. We included patients with missing clinical data in analyses for which they had data and have specified the denominator for each variable. Anti-S RBD antibody concentrations are reported as geometric means and standard deviations. Other continuous data are reported as a median and interquartile range, and discrete data as numbers and percentages, unless otherwise stated.
Univariable analyses, using Spearman’s rank correlation coefficients, and t-tests of log-transformed anti-S RBD antibody concentration were used to identify demographic, disease, vaccine and treatment-related factors associated with the concentration of anti-S RBD antibodies across the cohort. Crude sensitivity analyses excluding patients treated without a concomitant immunomodulator were undertaken to control for the effect of immunomodulator use on anti-S RBD antibody concentrations. Propensity matching was used to account for the other significant differences in baseline variables between infliximab-treated and vedolizumab-treated patients using the MatchIt package38. A priori, patients were matched exactly on diagnosis, immunomodulator use, and then using optimal matching, on age, the number of comorbidities, ethnicity, and presence of active disease. Multivariable linear regression models were used to identify factors independently associated with log anti-S RBD concentration. A priori, we included age, ethnicity, biologic medication and immunomodulator use. Results are presented after exponentiation so that the coefficients of the model correspond to the fold change (FC) associated with each binary covariate. For age, a cut-off was chosen based on a graphical inspection of the relationship between age and anti-S RBD antibody concentrations.
Mann–Whitney U-test was used to compare the magnitude of T cell response (SFC/106 PBMCs) stratified by treatment and vaccine received, and Spearman’s rank correlation coefficient was calculated to determine the correlation between antibody and T cell responses.
Anti-S RBD antibody half-lives were estimated using an exponential model of decay. Linear mixed models were fit using the lme4 and lmerTest package, with biologic treatment and vaccine type as fixed effects and each subject as a random effect. Each of these effects were estimated independently for gradient and intercept. 95% confidence intervals of fixed effects were calculated using likelihood ratios. P values for comparison of half-lives were estimated from the full linear mixed-effects model that incorporated vaccine, biologic drug and prior SARS-CoV-2 infection status.
We visualised the durability of antibody responses by calculating 15-day rolling geometric mean anti-S RBD antibody concentrations. For this analysis we included participants who had an antibody test carried out between 1 and 70 days after the second vaccine dose. Cox proportional hazard regression models were used to identify the demographic, disease and treatment-related factors associated with the time to fall in anti-S RBD antibody concentration below the seroconversion threshold.
Kaplan–Meier curves and Cox proportional hazard regression model was used to identify treatment-related factors associated with time to breakthrough infection. A linear regression model of log-transformed geometric mean anti-S RBD antibody concentration was used to determine the risk of breakthrough infections.
Where appropriate the same analyses were used to compare antibody responses in participants with PCR evidence of SARS-CoV-2 infection at any time prior to vaccination.
Ethical consideration
Patients were included after providing informed, written consent and compensation for participation was not provided. The sponsor was the Royal Devon and Exeter NHS Foundation Trust. The Surrey Borders Research Ethics committee approved the study (REC reference: REC 20/HRA/3114) in September 2020. The protocol is available online at https://www.clarityibd.org. The study was registered with the ISRCTN registry (https://doi.org/10.1186/ISRCTN45176516).
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
The study protocol including the statistical analysis plan is available at https://www.clarityibd.org/. Individual participant de-identified data that underlie the results reported in this article will be available immediately after publication for a period of 5 years. Due to the sensitive nature of the data, this will be made available to investigators whose proposed use of the data has been approved by an independent review committee. Analyses will be restricted to the aims in the approved proposal. Proposals should be directed to tariq.ahmad1@nhs.net. To gain access data requestors will need to sign a data access agreement. Data from the Virus Watch study is currently being archived on the Office of National Statistics Secure Research Service and will be available shortly. Source data are provided with this paper in the Source Data file. Source data are provided with this paper.
Code availability
Statistical analyses were undertaken in R 4.1.2 (R Foundation for Statistical Computing, Vienna, Austria. Code has been made available at: https://github.com/exeteribd/clarityibd-public.
References
Bernal, J. L. et al. Effectiveness of the Pfizer-BioNTech and Oxford-AstraZeneca vaccines on covid-19 related symptoms, hospital admissions, and mortality in older adults in England: test negative case-control study. BMJ 373, n1088 (2021).
Voysey, M. et al. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: an interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. 397, 99–111 (2021).
Polack, F. P. et al. Safety and efficacy of the BNT162b2 mRNA covid-19 vaccine. N. Engl. J. Med. 383, 2603–2615 (2020).
Prendecki, M. et al. Immunological responses to SARS-CoV-2 vaccines in kidney transplant recipients. Lancet. 398, 1482–1484 (2021).
Wong, S.-Y. et al. Serologic response to messenger RNA coronavirus disease 2019 vaccines in inflammatory bowel bisease patients receiving biologic therapies. Gastroenterology 161, 715–718 (2021).
Kappelman, M. D. et al. Humoral immune response to mRNA COVID-19 vaccines among patients with IBD. Gastroenterology 161, 1340–1343 (2021).
Kearns, P. et al. Examining the immunological effects of COVID-19 vaccination in patients with conditions potentially leading to diminished immune response capacity – The OCTAVE Trial. SSRN Electron. J. https://doi.org/10.2139/SSRN.3910058 (2021).
Sakuraba, A., Luna, A. & Micic, D. Serologic response to coronavirus disease 2019 (COVID-19) vaccination in patients with immune-mediated inflammatory diseases: a systematic review and meta-analysis. Gastroenterology 162, 88–108.e9 (2021).
Chanchlani, N. et al. Adalimumab and infliximab impair SARS-CoV-2 antibody responses: results from a therapeutic drug monitoring study in 11422 biologic-treated patients. J. Crohn’s Colitis https://doi.org/10.1093/ECCO-JCC/JJAB153 (2021).
Kennedy, N. A. et al. Inflammatory bowel disease anti-SARS-CoV-2 antibody responses are attenuated in patients with IBD treated with infliximab. Gut 70, 865–875 (2021).
Kennedy, N. A. et al. Infliximab is associated with attenuated immunogenicity to BNT162b2 and ChAdOx1 nCoV-19SARS-CoV-2 vaccines in patients with IBD. Gut 70, 1884–1893 (2021).
Harrington, J. E., Hamilton, R. E., Ganley-Leal, L., Farraye, F. A. & Wasan, S. K. The immunogenicity of the influenza, pneumococcal, and hepatitis B vaccines in patients with inflammatory bowel disease treated With vedolizumab. Crohn’s Colitis 360, 2 (2020).
Joint Committee on Vaccination and Immunisation. Joint Committee on Vaccination and Immunisation (JCVI) advice on third primary dose vaccination. https://www.gov.uk/government/publications/third-primary-covid-19-vaccine-dose-for-people-who-are-immunosuppressed-jcvi-advice/joint-committee-on-vaccination-and-immunisation-jcvi-advice-on-third-primary-dose-vaccination (2021).
Centre for Disease Control and Prevention. COVID-19 vaccines for moderately to severely immunocompromised people. https://www.cdc.gov/coronavirus/2019-ncov/vaccines/recommendations/immuno.html (2021).
European Medicines Agency. ECDC and EMA highlight considerations for additional and booster doses of COVID-19 vaccines. https://www.ema.europa.eu/en/news/ecdc-ema-highlight-considerations-additional-booster-doses-covid-19-vaccines (2021).
National Advisory Committee on Immunization (NACI). Summary of National Advisory Committee on Immunization (NACI) rapid response: additional dose of COVID-19 vaccine in immunocompromised individuals following a 1- or 2-dose primary series. https://www.canada.ca/en/public-health/services/immunization/national-advisory-committee-on-immunization-naci/summary-september-10-2021-additional-dose-covid-19-vaccine-immunocompromised-following-1-2-dose-series.html?utm_campaign=hc-sc-covidvaccine-21-22 (2021).
Hall, V. G. et al. Randomized trial of a third dose of mRNA-1273 vaccine in transplant recipients. N. Engl. J. Med. 385, 1244–1246 (2021).
EE, W. et al. Safety and immunogenicity of two RNA-based covid-19 vaccine candidates. N. Engl. J. Med. 383, 2439–2450 (2020).
Shrotri, M. et al. Spike-antibody waning after second dose of BNT162b2 or ChAdOx1. Lancet 398, 385–387 (2021).
McDonald, I., Murray, S. M., Reynolds, C. J., Altmann, D. M. & Boyton, R. J. Comparative systematic review and meta-analysis of reactogenicity, immunogenicity and efficacy of vaccines against SARS-CoV-2. npj Vaccines 6, 1–14 (2021).
Thomas, S. J. et al. Safety and efficacy of the BNT162b2 mRNA covid-19 vaccine through 6 Months. N. Engl. J. Med. 385, 1761–1773 (2021).
Park, J. K. et al. Effect of methotrexate discontinuation on efficacy of seasonal influenza vaccination in patients with rheumatoid arthritis: a randomised clinical trial. Ann. Rheum. Dis. 76, 1559–1565 (2017).
Barros-Martins, J. et al. Immune responses against SARS-CoV-2 variants after heterologous and homologous ChAdOx1 nCoV-19/BNT162b2 vaccination. Nat. Med. 27, 1525–1529 https://doi.org/10.1038/s41591-021-01449-9 (2021).
Lazarus, R. et al. Safety and immunogenicity of concomitant administration of COVID-19 vaccines (ChAdOx1 or BNT162b2) with seasonal influenza vaccines in adults in the UK (ComFluCOV): a multicentre, randomised, controlled, phase 4 trial. Lancet 398, 2277–2287 (2021).
Pasparakis, M., Alexopoulou, L., Episkopou, V. & Kollias, G. Immune and inflammatory responses in TNFα-deficient mice: a critical requirement for TNFα in the formation of primary B cell follicles, follicular dendritic cell networks and germinal centers, and in the maturation of the humoral immune response. J. Exp. Med. 184, 1397–1411 (1996).
Ritter, U., Meissner, A., Ott, J. & Körner, H. Analysis of the maturation process of dendritic cells deficient for TNF and lymphotoxin-α reveals an essential role for TNF. J. Leukoc. Biol. 74, 216–222 (2003).
Salinas, G. F. et al. Anti-TNF treatment blocks the induction of T cell-dependent humoral responses. Ann. Rheum. Dis. 72, 1037–1043 (2013).
Reynolds, C. J. et al. Discordant neutralizing antibody and T cell responses in asymptomatic and mild SARS-CoV-2 infection. Sci. Immunol. 5, eabf3698 (2020).
Cope, A. P. et al. Chronic exposure to tumor necrosis factor (TNF) in vitro impairs the activation of T cells through the T cell receptor/CD3 complex; reversal in vivo by anti-TNF antibodies in patients with rheumatoid arthritis. J. Clin. Invest. 94, 749–760 (1994).
Sandborn, W. J. et al. Vedolizumab as induction and maintenance therapy for Crohn’s disease. N. Engl. J. Med. 369, 711–721 (2013).
Bourges, D. et al. Differential expression of adhesion molecules and chemokines between nasal and small intestinal mucosae: implications for T- and sIgA+ B-lymphocyte recruitment. Immunology 122, 551–561 (2007).
Reynolds, C. J. et al. Prior SARS-CoV-2 infection rescues B and T cell responses to variants after first vaccine dose. Science 372, 1418–1423 (2021).
Dailey, J. et al. Antibody responses to SARS-CoV-2 after infection or vaccination in children and young adults with inflammatory bowel disease. Inflamm. Bowel Dis. https://doi.org/10.1093/IBD/IZAB207 (2021)
Harris, P. A. et al. The REDCap consortium: Building an international community of software platform partners. J. Biomed. Inform. 95, 103208 (2019).
Roche Diagnostics GmbH. Elecsys® Anti-SARS-CoV-2 S assay method sheet. https://diagnostics.roche.com/gb/en/products/params/elecsys-anti-sars-cov-2-s.html (2020).
Muench, P. et al. Development and validation of the elecsys anti-SARS-CoV-2 immunoassay as a highly specific tool for determining past exposure to SARS-CoV-2. J. Clin. Microbiol. 58, 1694–1714 (2020).
Peng, Y. et al. Broad and strong memory CD4+ and CD8+ T cells induced by SARS-CoV-2 in UK convalescent individuals following COVID-19. Nat. Immunol. 21, 1336 (2020).
Ho, D. E., Imai, K., King, G. & Stuart, E. A. MatchIt: nonparametric preprocessing for parametric causal inference. J. Stat. Softw. 42, 1–28 (2011).
Acknowledgements
CLARITY IBD is an investigator-led, UK National Institute for Health Research COVID-19 urgent public health study, funded by the Royal Devon and Exeter NHS Foundation Trust, NIHR Imperial Biomedical Research Centre, Hull University Teaching Hospital NHS Trust, UKRI (MR/V036939/1) and by unrestricted educational grants from F. Hoffmann-La Roche AG (Switzerland), Biogen GmbH (Switzerland), Celltrion Healthcare (South Korea), Takeda (UK) and Galapagos NV (Belgium). None of our funding bodies had any role in study design, data collection or analysis, writing, or decision to submit for publication. The NIHR Clinical Research Network supported study set-up, site identification and delivery of this study. This was facilitated by Professor Mark Hull, the National Speciality Lead for Gastroenterology. We acknowledge the contribution of our Patient Advisory Group who helped shape the trial design around patient priorities. Our partners, Crohn’s and Colitis UK (CCUK), continue to support this group and participate in Study Management Team meetings. We thank Professor Graham Cooke and Dr Katrina Pollock for their helpful discussions and review of the data. Laboratory tests were undertaken by the Exeter Blood Sciences Laboratory at the Royal Devon and Exeter NHS Foundation Trust. The Exeter NIHR Clinical Research Facility coordinated sample storage and management. This research used data assets made available by National Safe Haven as part of the Data and Connectivity National Core Study, led by Health Data Research UK in partnership with the Office for National Statistics and funded by UK Research and Innovation (research which commenced between 1 October 2020–31 March 2021 grant ref MC_PC_20029; 1 April 2021–30 September 2022 grant ref MC_PC_20058). Tariq Malik and James Thomas from Public Health England, Guy Stevens, Katie Donelon, Elen de Lacy from Public Health Wales and Johanna Bruce from Public Health Scotland supported linkage of central SARS-CoV-2 PCR test results with study data. Roche Diagnostics Limited provided the Elecsys Anti-SARS-CoV-2 immunoassay for the study. Faculty of Medicine at Imperial College London, Exeter NIHR Clinical Research Facility, Jeffrey Cheah Biomedical Centre at the University of Cambridge, Newcastle University Medical School and The Queen’s Medical Research Institute at the University of Edinburgh facilitated PBMC extractions for the T cell experiments. We thank Professor Robert Aldridge for access to data from the Virus Watch Collaborative. S.L. is supported by a Wellcome GW4-CAT fellowship (222850/Z/21/Z). N.C. acknowledges support from CCUK. J.C.L. is a Lister Prize Fellow and acknowledges support from the Cambridge NIHR Biomedical Research Centre and the Francis Crick Institute which receives core funding from Cancer Research UK (FC001169), the UK Medical Research Council (FC001169) and the Wellcome Trust (FC001169). G.-R.J. is supported by a Wellcome Trust Clinical Research Career Development Fellowship (220725/Z/20/Z). C.A.L. acknowledges support from the NIHR Newcastle Biomedical Research Centre and the support of the Programmed Investigation Unit at Royal Victoria Infirmary, Newcastle upon Tyne. C.W.L. is funded by a UKRI Future Leaders Fellowship. R.J.B. and D.M.A. are supported by MRC (MR/W020610/1, MR/S019553/1, MR/R02622X/1 and MR/V036939/1), NCSi4P, NIHR EME NIHR134607 and NIHR COV-LT2-0027, Innovate UK SBRI894, NIHR Imperial Biomedical Research Centre (BRC):ITMAT, Cystic Fibrosis Trust SRC (2019SRC015) and Horizon 2020 Marie Skłodowska-Curie Innovative Training Network (ITN) European Training Network (No 860325). N.P. is supported by the NIHR Imperial Biomedical Research Center (BRC). We acknowledge the study co-ordinators of the Exeter Inflammatory Bowel Disease Research Group: Marian Parkinson and Helen Gardner-Thorpe for their ongoing administrative support to the study. The sponsor of the study was the Royal Devon and Exeter NHS Foundation Trust.
Author information
Authors and Affiliations
Consortia
Contributions
N.A.K., J.R.G., C.B., S.S., N.P. and T.A. participated in the conception and design of this study. C.B. was the project manager and coordinated patient recruitment. R.N. and T.J.M. coordinated all biochemical analyses and central laboratory aspects of the project. S.L., N.A.K., A.S., D.M.S., C.J.R., R.C.S., S.H.K., F.P.P., K.-M.L., D.K.B., N.C., D.C., C.B., M.J., S.S., J.L.A., L.C., J.C.L., C.D.M., A.L.H., P.M.I., G.-R.J., K.B.K., C.A.L., C.W.L., D.M.A., R.J.B., J.R.G., N.P. and T.A. were involved in the acquisition, analysis or interpretation of data. D.M.S., C.J.R., K.-M.L., D.K.B. and F.F.P. performed, analysed and interpreted T cell experiments. T cell experiments were supervised, designed, analysed and interpreted by R.J.B. and D.M.A. Data analysis was done by N.A.K., D.M.S. and R.J.B. Drafting of the manuscript was done by S.L., N.A.K., N.C., S.S., C.W.L., D.M.A., R.J.B., J.R.G., N.P. and T.A. R.J.B., N.P. and T.A. obtained the funding for the study. All the authors contributed to the critical review and final approval of the manuscript. N.A.K., N.P. and T.A. have verified the underlying data.
Corresponding author
Ethics declarations
Competing interests
Dr. S Lin reports non-financial support from Pfizer, non-financial support from Ferring, outside the submitted work. Dr. Kennedy reports grants from F. Hoffmann-La Roche AG, grants from Biogen Inc, grants from Celltrion Healthcare, grants from Galapagos NV, non-financial support from Immundiagnostik, during the conduct of the study; grants and non-financial support from AbbVie, grants and personal fees from Celltrion, personal fees and non-financial support from Janssen, personal fees from Takeda, personal fees and non-financial support from Dr. Falk, outside the submitted work. Dr. Saifuddin has received travel expense support from Dr. Falk Pharma. Dr. Chee reports non-financial support from Ferring, personal fees and non-financial support from Pfizer, outside the submitted work. Prof. Sebastian reports grants from Takeda, Abbvie, AMGEN, Tillots Pharma, personal fees from Jaansen, Takeda, Galapagos, Celltrion, Falk Pharma, Tillots pharma, Cellgene, Pfizer, Pharmacocosmos, outside the submitted work. Dr. Alexander reports sponsorship from Vifor Pharma for accommodation/travel to BSG 2019, outside the submitted work. Dr. Lee reports personal fees from Abbvie, personal fees from C4X Discovery, personal fees from PredictImmune and personal fees from AG pus diagnostics. Dr. Hart reports personal fees from Abbvie, personal fees from Allergan, personal fees from BMS, personal fees from Celltrion, personal fees from Falk, personal fees from GSK, personal fees from Takeda, personal fees from Pfizer, personal fees from Janssen, personal fees from Galapogos, personal fees from AstraZeneca, outside the submitted work. Dr. Irving reports grants and personal fees from Takeda, grants from MSD, grants and personal fees from Pfizer, personal fees from Galapagos, personal fees from Gilead, personal fees from Abbvie, personal fees from Janssen, personal fees from Boehringer Ingelheim, personal fees from Topivert, personal fees from VH2, personal fees from Celgene, personal fees from Arena, personal fees from Samsung Bioepis, personal fees from Sandoz, personal fees from Procise, personal fees from Prometheus, outside the submitted work. Dr. Jones has received speaker fees from Takeda, Ferring and Janssen. Dr. Kok reports personal fees from Janssen, personal fees from Takeda, personal fees from PredictImmune, personal fees from Amgen, outside the submitted work. Dr. Lamb reports grants from Genentech, grants and personal fees from Janssen, grants and personal fees from Takeda, grants from AbbVie, personal fees from Ferring, grants from Eli Lilly, grants from Pfizer, grants from Roche, grants from UCB Biopharma, grants from Sanofi Aventis, grants from Biogen IDEC, grants from Orion OYJ, personal fees from Dr. Falk Pharma, grants from Astra Zeneca, outside the submitted work. Prof. Lees reports personal fees from Abbvie, personal fees from Janssen, personal fees from Pfizer, personal fees from Takeda, grants from Gilead, personal fees from Gilead, personal fees from Galapagos, personal fees from Iterative Scopes, personal fees from Trellus Health, personal fees from Celltion, personal fees from Ferring, personal fees from BMS, during the conduct of the study. Prof Boyton and Prof Altmann are members of the Global T cell Expert Consortium and have consulted for Oxford Immunotec outside the submitted work. Dr. Goodhand reports grants from F. Hoffmann-La Roche AG, grants from Biogen Inc, grants from Celltrion Healthcare, grants from Galapagos NV, non-financial support from Immundiagnostik, during the conduct of the study. Dr. Powell reports personal fees from Takeda, personal fees from Janssen, personal fees from Pfizer, personal fees from Bristol-Myers Squibb, personal fees from Abbvie, personal fees from Roche, personal fees from Lilly, personal fees from Allergan, personal fees from Celgene, outside the submitted work; and Dr. Powell has served as a speaker/advisory board member for Abbvie, Allergan, Bristol-Myers Squibb, Celgene, Falk, Ferring, Janssen, Pfizer, Tillotts, Takeda and Vifor Pharma. Prof. Ahmad reports grants and non-financial support from F. Hoffmann-La Roche AG, grants from Biogen Inc, grants from Celltrion Healthcare, grants from Galapagos NV, non-financial support from Immundiagnostik, during the conduct of the study; personal fees from Biogen inc, grants and personal fees from Celltrion Healthcare, personal fees and non-financial support from Immundiagnostik, personal fees from Takeda, personal fees from ARENA, personal fees from Gilead, personal fees from Adcock Ingram Healthcare, personal fees from Pfizer, personal fees from Genentech, non-financial support from Tillotts, outside the submitted work. The following authors have nothing to declare: Diana Muñoz Sandoval, Catherine Reynolds, Rocio Castro Seoane, Sherine H Kottoor, Franziska Pieper, Kai-Min Lin, David Butler, Neil Chanchlani, Claire Bewshea, Rachel Nice, Laura Constable, Charles D Murray, Timothy J McDonald.
Peer review
Peer review information
Nature Communications thanks Eloisa Bonfa, and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lin, S., Kennedy, N.A., Saifuddin, A. et al. Antibody decay, T cell immunity and breakthrough infections following two SARS-CoV-2 vaccine doses in inflammatory bowel disease patients treated with infliximab and vedolizumab. Nat Commun 13, 1379 (2022). https://doi.org/10.1038/s41467-022-28517-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-022-28517-z
This article is cited by
-
Cytokine signature in convalescent SARS-CoV-2 patients with inflammatory bowel disease receiving vedolizumab
Scientific Reports (2024)
-
Effect of DMARDs on the immunogenicity of vaccines
Nature Reviews Rheumatology (2023)
-
Trajectory analyses to identify persistently low responders to COVID-19 vaccination in patients with inflammatory bowel disease: a prospective multicentre controlled study, J-COMBAT
Journal of Gastroenterology (2023)
-
SARS-CoV-2-specific immune responses and clinical outcomes after COVID-19 vaccination in patients with immune-suppressive disease
Nature Medicine (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.