Abstract
Spinal cord injury leads to a massive response of innate immune cells in non-regenerating mammals, but also in successfully regenerating zebrafish. However, the role of the immune response in successful regeneration is poorly defined. Here we show that inhibiting inflammation reduces and promoting it accelerates axonal regeneration in spinal-lesioned zebrafish larvae. Mutant analyses show that peripheral macrophages, but not neutrophils or microglia, are necessary for repair. Macrophage-less irf8 mutants show prolonged inflammation with elevated levels of Tnf-α and Il-1β. Inhibiting Tnf-α does not rescue axonal growth in irf8 mutants, but impairs it in wildtype animals, indicating a pro-regenerative role of Tnf-α. In contrast, decreasing Il-1β levels or number of Il-1β+ neutrophils rescue functional regeneration in irf8 mutants. However, during early regeneration, interference with Il-1β function impairs regeneration in irf8 and wildtype animals. Hence, inflammation is dynamically controlled by macrophages to promote functional spinal cord regeneration in zebrafish.
Similar content being viewed by others
Introduction
Zebrafish, in contrast to mammals, are capable of functional spinal cord regeneration after injury. Recovery of swimming function critically depends on regeneration of axonal connections across the complex non-neural injury site1,2. It is therefore important to determine the factors that allow axons to cross the lesion site in zebrafish.
In mammals, a prolonged immune response, consisting of pro-inflammatory macrophages3, microglia cells4 and neutrophils5 together with cytokines released from other cell types, such as endothelial cells, oligodendrocytes, or fibroblasts6 contribute to an inhibitory environment for axonal regeneration. However, activated macrophages can also promote axonal regeneration7,8,9, suggesting complex roles of the immune response after spinal injury.
In zebrafish, we can dissect the roles of these cell types in successful functional spinal cord repair10. Zebrafish possess an innate immune system from early larval stages and develop an adaptive immune system at juvenile stages, similar to those in mammals11. Indeed, microglia is activated after spinal cord injury in adult12,13 and larval zebrafish14, suggesting functions of innate immune cells in repair. Adaptive immunity is also important for spinal cord regeneration15.
Larval zebrafish regenerate more rapidly than adults. Axonal and functional regeneration is observed within 48 h after spinal cord injury in 3 day-old larvae1,2. At the same time, the larval system presents complex tissue interactions that allow us to analyse how axons cross a non-neural lesion environment. For example, axons encounter Pdgfrb+ fibroblast-like cells that deposit regeneration-promoting Col XII in the lesion site in a Wnt-signalling dependent manner1. These cells and molecules are present also in the injury sites of adult zebrafish and mammals1,6. How immune cells contribute to this growth-conducive lesion site environment in zebrafish is unclear.
Here we show that peripheral macrophages control axonal regeneration by producing pro-regenerative tumour necrosis factor alpha (Tnf-α) and by reducing levels of interleukin-1 β (Il-1β). While early expression of il-1β promotes axonal regeneration, prolonged high levels of Il-1β in the macrophage-less irf8 mutant are detrimental. Preventing formation of Il-1β producing neutrophils or inhibiting excess il-1β directly, largely restored repair in irf8 mutants. This indicates that regulation of a single immune system-derived factor, Il-1β, is a major determinant of successful spinal cord regeneration.
Results
The immune response coincides with axonal regeneration
We analysed axonal regrowth in larval zebrafish that underwent complete spinal cord transection at 3 days post-fertilisation (dpf) in relation to invasion of the injury site by different cell types. Axons were present in the injury site by 1 day post-lesion (dpl). The thickness of the axonal bundle that connects the injured spinal cord increased up to 2 dpl and thereafter plateaued for up to at least 4 dpl (Supplementary Fig. 1A). The thickness of the connecting axon bundle positively correlated with the recovery of touch-evoked swimming distance for individual animals at 2 dpl (Supplementary Fig. 2A–C). This is consistent with previous results showing continuous axon labelling over the lesion site (axon bridging) in 80% of animals by 2 dpl, which then plateaued. Presence of an axon bridge correlates with functional recovery, as animals without axon bridge showed worse recovery of touch-evoked swimming distance1 and re-lesioning abolished functional recovery14. Hence, a percent score of larvae with bridged injury sites is a quick and reliable measure for anatomical repair1,14.
After injury, we observed a rapid and massive influx of immune cells, with neutrophils (Mpx+) peaking at 2 h post-lesion (hpl) and macrophages (mpeg1:GFP+; 4C4-) and microglia (mpeg1:GFP+; 4C4+) accumulating in the lesion site a few hours later and peaking at 2 dpl (Fig. 1a, Supplementary Movie 1). Myelinating cells (cldnK:GFP+) and endothelial cells (fli1:GFP+) were not abundant in the lesion site during axonal regrowth (Supplementary Fig. 1C, D), in contrast to functionally important pdgfrb:GFP+ fibroblasts1 that were present in the lesion site at 1 dpl, peaking at 2 dpl (Supplementary Fig. 1B). This suggests that myelinating cells and endothelial cells are not essential for axon bridging. However, at later time points after injury, axons were clearly associated with processes of myelinating cells (Supplementary Fig. 1C), which may impact functional repair. In contrast, the spatio-temporal pattern of immune cell invasion of the injury site suggests an early role for the immune system in orchestrating axon growth over the lesion site.
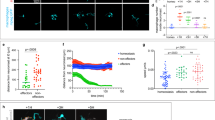
Spinal injury leads to an inflammatory response that promotes axonal regeneration. a Neutrophils, macrophages, and microglial cells show different dynamics after injury. Neutrophils (Mpx+) accumulate in the injury site very early, peaking at 2 hpl. Macrophages (mpeg1:GFP+/4C4−) and microglial cell (mpeg1:GFP+/4C4+) numbers peak at 48 hpl. Fluorescence images were projected onto transmitted light images. b–e Incubation with dexamethasone (timeline in b) reduces neutrophil and macrophage numbers (c, d; Mann–Whitney U-test: **P < 0.01, ***P < 0.001), as well as the proportion of animals with axonal bridging (e; Fisher’s exact test: ***P < 0.001). f–i, Incubation of animals with LPS during early regeneration (timeline in f) increased numbers of neutrophils and macrophages (g, h; t-test: **P < 0.01, ***P < 0.001), as well as the proportion of animals with axonal bridging at 24 hpl (i Fisher’s exact test: *P < 0.05). Lateral views of the injury site are shown; rostral is left. Rectangles indicate region of quantification; arrows indicate axonal bridging. Scale bars: 50 μm; Error bars indicate SEM
Immune system activation promotes axonal regeneration
To determine the importance of the immune reaction, we inhibited it using the anti-inflammatory synthetic corticosteroid dexamethasone14. This reduced the number of microglia14, macrophages and neutrophils in the injury site (Fig. 1b–d) and the proportion of larvae exhibiting axon bridging (control: 78% of examined animals, dexamethasone: 30%; Fig. 1e). The average thickness of axon bridges was also reduced by dexamethasone treatment and correlated with impaired recovery of touch-evoked swimming distance. (Supplementary Fig. 2A–C). gfap:GFP+ astroglia-like processes that cross the injury site slightly later than axons1 also showed reduced bridging, from 77.6% of examined animals to 48.3% (Supplementary Fig. 2D) under dexamethasone treatment. In addition, depleting the number of immune cells with a well-established morpholino combination against pu.1 and gcsfr16 reduced the proportion of larvae with axonal bridges from 81% of examined animals to 57% (Supplementary Fig. 3A, B).
For a gain-of-function approach, we used incubation with bacterial lipopolysaccharides (LPS)17. This increased the number of neutrophils and macrophages in the lesion site (Fig. 1f–h). To detect a potential accelerating effect on axonal regrowth, we analysed larvae at 18 hpl, when axonal regeneration was incomplete in untreated animals. This showed an increase in the proportion of larvae with axonal bridges from 41% of examined animals in wildtype to 60% in LPS-treated animals (Fig. 1i). Hence, immune system activity is necessary for and promotes axonal regeneration across a spinal lesion site.
Macrophages determine regenerative success
To analyse the role of different immune cell types in repair, we used mutants. In mutants for the macrophage-lineage determining transcription factor irf8, macrophages and microglial cells, but not neutrophils are missing during early development18. Homozygous mutants are adult viable and show no overt developmental aberrations, except for an increased number of neutrophils18. In situ hybridisation for the macrophage and microglia marker mpeg1 confirmed expression in the ventral trunk of unlesioned larvae and in a spinal lesion site at 2 dpl in wildtype larvae, but complete absence of signal in unlesioned and lesioned irf8 larvae (Fig. 2a).
In the irf8 mutant, axonal regeneration and functional recovery after injury show long-term impairment. a In situ hybridisation for mpeg1 confirms the absence of macrophages and microglial cells before and after injury in the irf8 mutant compared to controls. Arrows indicate labelling around the injury site and brackets indicate the ventral area of the larvae where the macrophages can be found in the circulation. Note that blackish colour is due to melanocytes. b Quantification of the proportion of larvae with axonal bridging (anti-acetylated Tubulin) shows that at 1 dpl, axonal bridging is unimpaired in irf8 mutants, whereas at 2 dpl, irf8 mutants fail to show full regrowth and even by 5 dpl, the proportion of irf8 larvae with a bridged lesion site is still lower than in wildtype controls (Fisher’s exact test: ***P < 0.001, n.s. indicated no significance). c Irf8 mutants never fully recover touch-evoked swimming distance in the observation period, whereas wildtype control animals do. Representative swim tracks are displayed. Note that unlesioned irf8 larvae show swimming distances that are comparable to those in wildtype controls (Two-way ANOVA: F15,1372 = 11.42, P < 0.001; unles. = unlesioned, les. = lesioned). All lesions are done at 3 dpf. Lateral views of the injury site are shown; rostral is left. Arrows indicate axonal bridging. Scale bars: 200 μm in a and 50 μm in c. Error bars indicate SEM
Next, we determined axonal regrowth and recovery of parameters of swimming capacity in irf8 mutants compared to wildtype animals. Wildtype and mutants showed comparable proportions of animals with axon bridges at 1 dpl (wildtype: 44% of examined animals; irf8 mutant: 43%). At 2 dpl, however, axonal continuity was observed in 80% of wildtype animals but only in 41% of irf8 mutants (Fig. 2b). At 5 dpl–2.5 times as long as wildtype animals need for maximal axon bridging—the proportion of mutant larvae with bridged lesion sites was increased compared to 2 dpl (55% of examined animals vs. 41%), but regenerative success was still strongly reduced compared to wildtype controls (55% of examined animals vs. 87%; Fig. 2c).
Analysing touch-evoked swimming, we found that wildtype animals swam comparable distances to unlesioned controls at 2 dpl, as previously described1. In contrast, recovery of touch-evoked swimming distance in irf8 larvae plateaued at 2 dpl and did not reach levels of unlesioned animals to at least 5 dpl (Fig. 2c). This indicates that in the absence of macrophages and microglia in irf8 mutants, initial axonal regeneration is unaffected, but axonal regrowth and functional recovery after spinal cord injury are impaired long-term.
To determine the importance of microglia for regeneration, we analysed csf1ra/b double-mutants (see Methods) in which the function of colony-stimulating factor 1 receptor (Csf1r) is compromised. Csf1r is selectively needed for microglia differentiation19. After injury in csf1ra/b mutants, we observed a strong reduction in the number of microglial cells (to 17% of wildtype), but an increase in macrophage numbers (by 55% compared to wildtype) in the injury site (Fig. 3a, c). Interestingly, neutrophil numbers were also strongly reduced (to 64.1% of wildtype at 2 hpl and 16% at 1 dpl) (Fig. 3b), perhaps due to feedback regulation from increased macrophage numbers. Whereas microglia cells were reduced in number in the entire fish, neutrophils were still present in the ventral trunk area. In these mutants, axon bridging was unimpaired (Fig. 3d). Hence, microglia are not necessary for axonal regeneration and reduced numbers of neutrophils do not negatively affect axonal regrowth. Combined with results from the irf8 mutant, this indicates that recruitment of peripheral macrophages is critical for successful spinal cord regeneration.
Absence of microglial cells and reduced neutrophil numbers do not affect axon bridging. a Numbers of microglial cells (4C4+; arrows) in the injury site of the csf1ra/b mutants are much lower than in wildtype animals (t-test: ***P < 0.001). b Fewer neutrophils (Mpx+) are found in the injury site (arrows) of csf1ra/b mutants than in wildtype animals (t-test: *P < 0.05, ***P < 0.001). Note neutrophils ventral to the injury site (brackets). c The number of macrophages (Mfap4+) is increased in the injury site in the mutants at 1 dpl, but not at 2 dpl (t-test: ***P < 0.001, ns indicates no significance). d Immunostaining against acetylated tubulin shows that axon bridging (arrows) is not affected in the mutants compared to wildtype animals at 2 dpl (Fisher’s exact test: ns indicates no significance). Lateral views of the injury site are shown; rostral is left. Wt = wildtype; Scale bars: 50 µm in a, b, d; 25 µm in b. Error bars indicate SEM
Macrophages are not necessary for Col XII deposition
Next, we asked whether macrophages act via a previously reported regeneration-promoting mechanism, comprising Wnt-dependent deposition of Col XII in the lesion site by pdgfrb:GFP+ fibroblast-like cells1. Inhibition of the immune response with dexamethasone did not inhibit appearance of pdgfrb:GFP+ fibroblast-like cells in the lesion site (Supplementary Fig. 4A). By crossing a reporter line for Wnt pathway activity (6xTCF:dGFP)1 into the irf8 mutant, we found that activation of the pathway was unaltered in the mutant (Supplementary Fig. 4E). Similarly, expression of col12a1a and col12a1b mRNA in irf8 mutants was indistinguishable from that in wildtype animals (Supplementary Fig. 4B). Deposition of Col I protein and mRNA expression of 11 other ECM components were also not altered in the irf8 mutant at 1 and 2 dpl (Supplementary Fig. 4B, C). Moreover, immunolabelling against Tp63 showed that by 2 dpl, the injury site in the irf8 mutants was completely covered by basal keratinocytes, an additional source of Col XII1, as in wildtype animals (Supplementary Fig. 4D). In contrast, a PCR screen of 21 potentially macrophage-derived ECM-modifying matrix metalloproteinases20 (mmps) indicated lower mRNA levels for mmp11a, mmp16a/b, mmp24, and mmp28 in the injury site of irf8 mutants compared to wildtype animals (Supplementary Fig. 5A, B). This suggests a potential for macrophages to alter the lesion site ECM with Mmps. Overall, macrophages do not overtly regulate Wnt-signalling, deposition of some crucial ECM components or basal keratinocyte coverage of the injury site during regeneration.
Cellular debris is not a major impediment to regeneration
Macrophages could serve as a substrate for axon growth or promote regeneration by removing debris by phagocytosis—a major function of macrophages in peripheral nerve regeneration in zebrafish21,22. In time-lapse movies of double transgenic animals in which neurons (Xla.Tubb:DsRed) and macrophages (mpeg1:GFP) were labelled (Supplementary Fig. 6B and Supplementary Movie 2) we observed axons crossing the spinal lesion site at the same time macrophages migrated in and out of the injury site. However, no obvious physical interactions between these cell types were observed, making it unlikely that macrophages acted as an axon growth substrate.
We frequently observed macrophages ingesting neuronal material and transporting that away from the injury site in time-lapse movies (Supplementary Fig. 6B and Supplementary Movie 2). In agreement with this observation, TUNEL labelling indicated strongly increased levels of dead or dying cells in the late (48 hpl), but not the early (24 hpl) phase of axonal regeneration in the injury site of irf8 mutants (Supplementary Fig. 6A).
To determine the impact of debris on regeneration, we prevented cell death and consequently debris accumulation in irf8 larvae using the pan-caspase inhibitor QVD23, that is functional in zebrafish24. This treatment led to lower debris levels that were comparable to those seen in wildtype larvae at 2 dpl (Supplementary Fig. 6C), but failed to increase regenerative success in irf8 mutants (control, 38% of examined larvae with axon bridges; QVD, 40%. Thickness of axon bridge: control 19.03+/−2.14 µm; QVD: 18.32+/−2.53 µm; t-test: P > 0.05. Supplementary Fig. 6E). Conversely, inhibiting debris phagocytosis with the pharmacological inhibitor O-phospho-l-serine (L-SOP)25 in wildtype animals increased levels of debris in the injury site, but did not impair axonal bridging (Supplementary Fig. 7A–C). This suggests no obvious connection between debris levels and/or phagocytosis and regenerative success.
Pro-and anti-inflammatory phases are altered in irf8 mutants
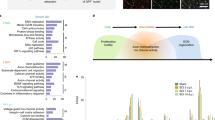
To determine a possible role of cytokines in the regenerative failure of irf8 mutants, we analysed relative levels of pro-and anti-inflammatory cytokines in the lesion site during regeneration in wildtype animals and irf8 mutants by qRT-PCR. In wildtype animals, expression levels of pro-inflammatory cytokines il-1β and tnf-α were high during initial regeneration (>25-fold for il-1β; >12-fold for tnf-α for approximately to 12 hpl) and reduced again during late regeneration (12–48 hpl), although still elevated compared to unlesioned controls (Fig. 4a, b). Anti-inflammatory cytokines, such as tgf-β1a and tgf-β3 were expressed at low levels during initial regeneration, and upregulated during late regeneration (approximately 3-fold for tgf-β1a and 2-fold for tgf-β3), indicating a bi-phasic immune response within the 48-h time frame of analysis (Fig. 4c, d).
Inflammation is bi-phasic and dysregulated in irf8 mutants. a, b Absence of macrophages in the irf8 mutant fish leads to increased il-1β and tnf-α mRNA levels during the late stage of inflammation (>12 hpl). An early peak in tnf-α expression is missing in irf8 mutants. c, d Expression of anti-inflammatory cytokines, tgf-β1a and tgf-β3, which peak during late regenerative phases in wildtype animals, is strongly reduced in irf8 mutants (t-tests: *P < 0.05, **P < 0.01, ***P < 0.001; wt = wildtype animals). # indicates statistical significance when compared to unlesioned animals. Error bars indicate SEM
In irf8 mutants, levels of pro-inflammatory cytokines remained high during the late phase of regeneration (Fig. 4a, b) and anti-inflammatory cytokines were not upregulated (Fig. 4c, d), resulting in a sustained pro-inflammatory environment in irf8 mutants.
The lack of anti-inflammatory cytokines correlated with the lack of macrophages and microglia in irf8 mutants. We performed qRT-PCR in fluorescence activated flow sorted mpeg1:GFP cells in wildtype animals to determine whether macrophages and microglial cells expressed tgf-β1a and tgf-β3. mpeg1:GFP+ cells, but also mpeg1:GFP– cells expressed these cytokines (Supplementary Fig. 8A). In situ hybridisation showed wide-spread labelling with some more strongly labelled cells around the injury site in wildtype, but not irf8 mutants (Supplementary Fig. 8B). This is consistent with expression of tgf-β1a and tgf-β3 in microglia/macrophages and other cell types26. Hence, the immune response is bi-phasic with an initial pro-inflammatory phase, followed by an anti-inflammatory phase in wildtype animals. In the absence of macrophages in irf8 mutants, animals fail to switch to an anti-inflammatory state.
Tnf-α promotes axonal regeneration
To determine whether increased levels of pro-inflammatory cytokines contributed to impaired axon growth in irf8 mutants, we first inhibited Tnf-α signalling. Pomalidomide, a pharmacological inhibitor of Tnf-α release27, had no effect on axonal regrowth in irf8 mutants. In contrast, in wildtype animals Pomalidomide strongly inhibited axon bridging at 1 dpl (control: 62% of examined animals showed an axonal bridge; Pomalidomide: 36%) and 2 dpl (control: 75% of examined animals; Pomalidomide: 45%) (Fig. 5a).
Tnf-α is essential for axonal regeneration. a Tnf-α inhibition by Pomalidomide reduces the proportion of wildtype animals with axon bridging at 1 and 2 dpl. No effect is observed in irf8 mutants (Two-way ANOVA followed by Bonferroni post-test: F3,16 = 12.16, **P < 0.01, n.s indicates no significance). b CRISPR/Cas9-mediated disruption of tnf-α is effective as shown by RFLP analysis. This reveals efficient somatic mutation in the gRNA target site, indicated by resistance to restriction endonuclease digestion (arrow). c Axonal bridging (arrow; Xla.Tubb:DsRed+) is strongly impaired after disruption of the tnf-α gene. (Fisher’s exact test: ***P < 0.001) and the impairment persists at 5 dpl. Lateral views of the injury site are shown; rostral is left. Scale bar: 50 μm. Error bars indicate SEM
To confirm pharmacological results, we targeted tnf-α by using CRISPR manipulation with a gene-specific guideRNA (gRNA). Injection of the gRNA into the zygote efficiently mutated the gene as shown by restriction fragment length polymorphism (RFLP) analysis (Fig. 5b) and produced function-disrupting insertion-deletion mutations in a highly conserved domain28 (Supplementary Table 1). Western blots of 4-day old larvae and immunohistochemistry in the injury site showed robustly reduced Tnf-α protein levels (Supplementary Fig. 9A, B).
Axon bridging was inhibited in wildtype animals by tnf-α gRNA injection in a way that was comparable to drug treatment (1 dpl: control: 51% of examined animals showed bridging; gRNA: 27%; 2 dpl: control: 88% of examined animals showed bridging; gRNA: 40%). At 5 dpl, axon bridging was still strongly impaired (control: 84.1% of examined animals showed bridging; gRNA: 38.3%; Fig. 5c), indicating long-term impairment of regeneration. Hence, tnf-α dysregulation is not a major cause of regenerative failure in irf8 mutants, but tnf-α is necessary for axonal regeneration in wildtype animals.
To determine which cells expressed tnf-α in wildtype animals, we used immunohistochemistry for L-Plastin, labelling all immune cells, in tnf-α:GFP transgenic fish (Fig. 6d). Nearly all tnf-α:GFP+ cells co-labelled with L-Plastin (96%) at 12 hpl. Thus, expression of tnf-α occurred mainly in immune cells (Fig. 6a). Double-labelling tnf-α:GFP reporter fish with neutrophil (Mpx), microglia (4C4) and macrophage (Mfap4) markers at 24 hpl, when axons were actively growing, indicated that >95% of tnf-α:GFP+ cells in the injury were peripheral macrophages. However other cell types, such as neurons29, may also express tnf-α. More than 72% of macrophages were tnf-α:GFP+, whereas for microglia (<6.5%) and neutrophils (<0.7%) the proportion was much smaller. Over time, the proportion of tnf-α:GFP+ macrophages was reduced (from 72.5% at 1 dpl to 59% at 2 dpl) (Fig. 6b). Our observations suggest that macrophages promote regeneration by expressing tnf-α.
Tnf-α is expressed by macrophages and regulates the immune response. a Top row: tnf-α:GFP labelling occurs almost exclusively in L-plastin+ immune cells (L-plastin in green; tnf-α:GFP in magenta; yellow arrow indicates a rare tnf- α:GFP+ microglial cell; 12 hpl) b In the injury site, the number and proportion of macrophages (Mfap4+) that are tnf-α:GFP+ are much higher than numbers and proportions of microglia (4C4+) and neutrophils (Mpx+), indicating that the main source of Tnf-α is the macrophages. Arrows indicate double-labelled cells and arrowheads indicate immune cells that are tnf-α:GFP-. Single optical sections are shown; the proportion of macrophages that are tnf-α:GFP+ decreases over time, whereas the proportion of tnf-α:GFP+ microglial cells slightly increases (One-way ANOVA followed by Bonferroni post-test: F4,195 = 376.3, **P < 0.01, *P < 0.05). c Quantification of the immune cells after tnf-α gRNA injection shows that Tnf-α disruption leads to increased numbers of neutrophils (Mpx+) at 1 dpl but not at 2 dpl, whereas the numbers of macrophages/microglia (mpeg1:GFP+) remains unchanged (Mann–Whitney U-test: *P < 0.05, ns indicates no significance). d qRT-PCR indicates that tnf-α disruption leads to increased levels of il-1β mRNA at 2 dpl (t-tests: *P < 0.05). Lateral views of the injury site are shown; rostral is left. Scale bars: 50 μm. Error bars indicate SEM
To elucidate effects of tnf-α inhibition, we determined numbers of neutrophils and macrophages/microglia at 24 and 48 hpl in tnf-α gRNA injected animals. This showed no changes in macrophages, but a 49.7% increase in the number of neutrophils at 1 dpl (Fig. 6c). qRT-PCR indicated that il-1β mRNA levels were increased by 108%, whereas tnf-α, tgf-β1a and tgf-β3 mRNA levels remained unchanged at 2 dpl (Fig. 6d). This suggests a moderate enhancement of the pro-inflammatory response when Tnf-α is inhibited.
Il-1β inhibits regeneration in irf8 mutants
To test whether sustained high levels of Il-1β were responsible for regenerative failure in irf8 mutants, we interfered with il-1β function in three different ways. Firstly, we inhibited caspase-1, which is necessary for activation of Il-1β, using the pharmacological inhibitor YVAD that is functional in zebrafish30 (Fig.7a–e). Secondly, we disrupted il-1β RNA splicing with an established morpholino (Supplementary Fig. 10A–D)31. Finally, we targeted il-1β in a CRISPR approach (Supplementary Fig. 10E–H).
Inhibition of Il-1β function rescues axonal regeneration in irf8 mutants. Lateral views of the injury site are shown; rostral is left. a YVAD reduces expression levels of il-1β and tnf-α in irf8 mutants (two-sample t-test: *P < 0.05) at 2 dpl. b YVAD impairs migration of peripheral macrophages (Mfap4+) and neutrophils (Mpx+) in wildtype animals and irf8 mutants (only neutrophils quantified, due to absence of macrophages) (t-tests: ***P < 0.001). c YVAD moderately reduces the number of TUNEL+ cells in the irf8 mutants at 2 dpl. (Two-Way ANOVA followed by Bonferroni multiple comparisons: F3,121 = 112.5, ***P < 0.001). d YVAD does not influence axonal regeneration in wildtype animals but rescues axonal bridging (arrows) in irf8 mutants (Fisher’s exact test: **P < 0.01, ns indicates no significance) at 2 dpl. e Impaired touch-evoked swimming distance in irf8 mutants is rescued by YVAD treatment, to levels that are no longer different from lesioned and unlesioned wildtype animals at 2 dpl. YVAD has no influence on swimming distance in lesioned or unlesioned wildtype animals (Two-way ANOVA followed by Bonferroni multiple comparisons: F1,309 = 35.229, ***P < 0.0001, ns indicates no significance). Rectangle in b denotes quantification area. Scale bar: 50 μm for b, d. Error bars indicate SEM
To determine whether interfering with Il-1β function mitigated inflammation in irf8 mutants, we quantified immune cells, expression of il-1β, tnf-α, and dead cells. Indeed, after YVAD treatment we observed a reduction of neutrophil peak numbers (by 38% at 2 hpl; Fig. 7b), as well as strongly reduced levels of il-1β and tnf-α mRNA expression (at 2 dpl; Fig. 7a) in irf8 mutants. Moreover, the number of TUNEL+ cells was reduced at 2 dpl in the irf8 mutant, but not to wildtype levels (Fig. 7c). In lesioned wildtype animals, YVAD reduced peak numbers of neutrophils (by 40% at 2 hpl) and macrophages (by 28% at 48 hpl), but no influence on low numbers of TUNEL+ cells at 2 dpl was observed. Hence, interfering with Il-1β function reduces inflammation in irf8 mutants and wildtype animals.
Axon bridging in wildtype animals was not affected by YVAD treatment at 2 dpl (control: 79% of examined animals showed bridging; YVAD: 78%) (Fig. 7d), indicating that high levels of Il-1β were not necessary for axonal regeneration. In contrast, in YVAD-treated irf8 mutants, we observed a remarkable rescue of axon bridging at 2 dpl (control: 38% of examined animals showed bridging; YVAD: 69%) (Fig. 7d).
Injecting a well-established31 morpholino targeting il-1β into irf8 mutants at the one-cell-stage inhibited il-1β splicing (Supplementary Fig. 10A, D). Morpholino-injected animals showed a rescue of axon bridging at 2 dpl (control: 40% of examined animals showed bridging; YVAD: 60%) (Supplementary Fig. 10B, C).
Finally, injecting a gRNA targeting il-1β at the one-cell stage led to somatic mutation in the target site of il-1β, indicated by RFLP analysis (Supplementary Fig. 10E, H). This strongly rescued axonal bridging in lesioned irf8 mutants (control: 40% of examined animals showed bridging; acute il-1β gRNA: 70%) (Supplementary Fig. 10F, G). Hence, three independent manipulations show that excessive il-1β levels in irf8 mutants are a key reason for impaired axonal regeneration.
Il-1β promotes axonal regeneration during the early regeneration
To determine whether roles of Il-1β and general inflammation differed for different phases of the inflammation, we separately analysed early (0–1 dpl; Supplementary Fig. 11A) and late (1–2 dpl; Supplementary Fig. 11B) regeneration by drug incubation. During the early phase, YVAD treatment led to a weak inhibition of axonal regeneration in both wildtype (control: 58% of examined animals showed bridging; YVAD: 41%) and irf8 mutants (control: 41% of examined animals showed bridging; YVAD: 36%). Similarly, dexamethasone treatment inhibited axonal regeneration in both wildtype (control: 57.5% of examined animals showed bridging; dexamethasone: 36.6%) and irf8 (control: 44.6% of examined animals showed bridging; dexamethasone: 34%). Interestingly, while LPS promoted regeneration in the early phase in wildtype animals (control: 53.2% of examined animals showed bridging; LPS: 68.7%), it was detrimental in irf8 mutants (control: 39% of examined animals showed bridging; LPS: 25.5%), perhaps because baseline inflammation was already high in the mutant.
During late regeneration, only dexamethasone had an inhibitory effect in wildtype animals (from 82.1% of examined animals that showed bridging to 64.4%). YVAD had no effect in wildtype animals during late regeneration, when il-1β was already down-regulated (control: 81% crossing; YVAD: 78% crossing), but a strong rescue effect of YVAD was observed in the irf8 mutant (control: 37% of examined animals showed bridging; YVAD: 68%). This rescue effect was comparable to that observed when Il-1β was suppressed for the entire 48 h (cf. Fig. 7d). LPS had no effect in wildtype or mutants during late regeneration. Hence, early inflammation and il-1β upregulation promote regeneration, but il-1β must be down-regulated at later phases of axonal regeneration.
Reduction of Il-1β levels rescues swimming in irf8 mutants
To determine whether ll-1β inhibition also rescued recovery of swimming function in irf8 mutants, we analysed touch-evoked swimming distances. YVAD had no effect in unlesioned mutant or wildtype animals and did not affect recovery in lesioned wildtype animals (Fig. 7e). In contrast, YVAD-treatment rescued the touch-evoked swimming distance in irf8 mutants to levels that were indistinguishable from wildtype lesioned or unlesioned animals (Fig. 7e). Mean velocity and path shape (meandering) were also rescued (Supplementary Fig. 10I, J). These observations indicate that inhibition of Il-1β alone restores most axonal regeneration and recovery of touch-evoked swimming parameters in the absence of macrophages.
Neutrophils are a major source of il-1β
To understand il-1β regulation, we determined the source of Il-1β in wildtype and irf8 mutants. Using Il-1β immunohistochemistry and a transgenic reporter line (il-1β:GFP), we found expression in microglia, macrophages, neutrophils and basal keratinocytes in the injury site (Fig. 8c, d; Supplementary 12A). Neuronal labelling (HuC/D+) did not overlap with il-1β:GFP labelling (Supplementary Fig. 12B). While numbers of il-1β:GFP+ immune cells did not change significantly between 1 and 2 dpl, the percentage of macrophages (from 50.6 to 34.3%) and neutrophils that were labelled for the il-1β:GFP transgene were reduced (from 53.3 to 23.7%), likely reflecting resolution of inflammation (Supplementary Fig. 12A).
Levels of il-1β expression are increased in the injury site of irf8 mutants. a At 1 dpl, expression levels of il-1β are comparable between irf8 mutants and wildtype (Wt) animals but are higher in the mutant at 2 dpl in qRT-PCR (t-test: **P < 0.01, ns indicates no significance). b In situ hybridisation confirms increased expression of il-1β mRNA at 2 dpl. c In the injury site, the number and proportion of neutrophils (Mpx+) that are Il-1β immuno-positive (arrows) are increased in irf8 mutants at 1 dpl compared to wildtype animals. d The number of basal keratinocytes (Tp63+) that are Il-1β immuno-positive is increased in irf8 mutants. Single optical sections are shown; boxed areas are shown in higher magnifications (t-test: *P < 0.05, **P < 0.01). Lateral views of the injury site are shown; rostral is left. Scale bars: 100 μm in b, c, d and 50 µm for higher magnification areas. Error bars indicate SEM
In irf8 mutants, detection of il-1β mRNA by qRT-PCR and in situ hybridisation confirmed increased levels at 2 dpl, but not 1 dpl (Fig. 8a, b), despite lack of il-1β expressing microglia and macrophages. Instead, we observed increased numbers of Il-1β+ neutrophils (by 97%) and basal keratinocytes (by 58%) compared to wildtype animals at 1 dpl (Fig. 8c, d). Importantly, the proportion of neutrophils that were Il-1β+ was also increased from 33.6% in wildtype animals to 49% in the irf8 mutant at 1 dpl. This demonstrates that neutrophils are more likely to express il-1β in the absence of macrophages.
Increased numbers of Il-1β+ neutrophils in irf8 mutants could, at least in part, be due to higher overall numbers of neutrophils in the injury site. We found a peak of neutrophil numbers in the lesion site of irf8 mutants at 2 hpl, as in wildtype animals (Fig. 9a). However, the number of neutrophils was 27% higher than in wildtype, potentially due to the higher abundance of this cell type in the irf8 mutant18. While neutrophil numbers declined over time in wildtype and irf8 mutants, they did so more slowly in irf8 mutants. At 24 hpl, twice, and at 48 hpl, three times the number of neutrophils as in wildtype animals remained in the mutant. Hence, macrophages control number of and cytokine expression by neutrophils32, leading to prolonged presence of Il-1β+ neutrophils in the injury site of irf8 mutants.
Preventing neutrophil formation partially rescues functional spinal cord regeneration in the irf8 mutant. a In irf8 mutants, higher peak numbers of neutrophils (Mpx+) at 2 hpl and slower clearance over the course of regeneration are observed (Two-Way ANOVA followed by Bonferroni multiple comparisons: F8,427 = 13.19 *P < 0.05, **P < 0.01, ***P < 0.001). Note that wildtype data are the same as shown in Fig. 1a, as counts in irf8 mutants and wildtype animals were done in the same experiments. b Combination treatment with pu.1 and gcsfr morpholinos efficiently prevents neutrophil accumulation in the lesion site (Mann–Whitney U-test: ***P < 0.001). c In pu.1/gcsfr morpholino injected irf8 mutant fish, levels of il-1β and tnf-α mRNA expression are reduced at 2 dpl, as shown by qRT-PCR (t-test: ***P < 0.001). d, e In pu.1/gcsfr morpholino injected irf8 mutant fish, axonal bridging (arrows, d Fisher’s exact test: **P < 0.01) and behavioural recovery (e One-Way ANOVA followed by Bonferroni multiple comparisons: F5,142 = 23.21, **P < 0.01, ns indicates no significance) are partially rescued. Lateral views of the injury site are shown; rostral is left. Scale bars: 100 μm. Error bars indicate SEM
Neutrophils inhibit regeneration in irf8 mutants
To determine the relative importance of the neutrophils for regenerative failure in irf8 mutants, we reduced their numbers using pu.1/gcsfr morpholino treatment. This strongly reduced numbers of neutrophils by 84.6% in the injury site at 2 hpl, when the neutrophil reaction peaked in untreated irf8 mutants (Fig. 9b). pu.1/gcsfr morpholino treatment also reduced il-1β mRNA levels by 54% and tnf-α mRNA levels by 70% at 2 dpl (Fig. 9c). Remarkably, axon bridging (control: 43% of examined animals showed bridging; pu.1/gcsfr morpholino: 60%; Fig. 9d) and recovery of touch-evoked swimming distance were partially rescued in these neutrophil-depleted mutants at 2 dpl (Fig. 9e). This shows that in the absence of macrophages, the prolonged presence of Il-1β+ neutrophils is detrimental to regeneration.
Discussion
We identify a biphasic role of the innate immune response for axonal bridging of the non-neural lesion site in larval zebrafish. Initial inflammation and Il-1β presence promote axon bridging, whereas later, Il-1β levels need to be tightly controlled by peripheral macrophages. Inhibiting Il-1β largely compensated for the absence of macrophages, underscoring the central role of this cytokine. Macrophage-derived Tnf-α promotes regeneration, partially by reducing neutrophil number and il-1β levels (summarised in Supplementary Fig. 13). This indicates important and highly dynamic functions of the immune system for successful spinal cord regeneration.
The function of the immune system changes dramatically over time. Within the first hours after injury, neutrophils and the pro-inflammatory cytokines il-1β and tnf-α dominate the injury site. Initially, inflammation promotes axonal growth. This is indicated by reducing effects on axon bridging of early Il-1β inhibition and the promoting effect of LPS in wildtype animals. Indeed, it has been reported that Il-1β can promote neurite growth33,34. However, from about 12 hpl, macrophages and anti-inflammatory cytokines are in the lesion site and during this late phase of regeneration, Il-1β mediated inflammation in macrophage-less mutants strongly inhibits regeneration.
How does Il-1β inhibit spinal cord regeneration? High Il-1β levels may condition the environment to be inhibitory to axonal regrowth. Blocking excessive Il-1β signalling in irf8 mutants revealed that Il-1β increases numbers of neutrophils, levels of il-1β and tnf-α expression, as well as cell death in the lesion environment. Morevover, reduced expression of some metalloproteinases in the irf8 mutant suggest that the lesion site ECM may be altered. However, several ECM components, including functionally important Col XII1, were unaltered in expression in the irf8 mutant. Similar to our observations, an Il-1β deficient mouse showed slightly increased axonal regrowth after spinal injury35.
Axonal regeneration is promoted by Tnf-α. Even though il-1β and tnf-α were similarly upregulated in the irf8 mutant, only reducing Il-1β levels rescued the mutant. Conversely, in wildtype animals, Il-1β had only a relatively small promoting effect on early regeneration, whereas Tnf-α was indispensable for axonal regrowth. Different functions for the two pro-inflammatory cytokines have been reported36. They also differ in cell type of origin. Whereas Il-1β is expressed by a substantial proportion of neutrophils, microglia and macrophages, Tnf-α is mainly expressed by macrophages in the injury site. This indicates a clear difference between tissue-resident microglia and peripheral macrophages. In mammals, tnf-α is produced by both microglia and macrophages37.
Tnf-α may exert its positive role for regeneration at least in part by controlling neutrophil numbers and Il-1β levels. Both of these parameters are increased when Tnf-α is inhibited and are inhibitory to regeneration. Anti-inflammatory actions of Tnf-α have been described in the context of auto-immunity38, but whether this interaction between Tnf-α and Il-1β is direct or indirect, needs to be elucidated. For example, Tnf-α can be neuroprotective after CNS injury36,39 and thus indirectly reduce inflammation. In the regenerating fin, Tnf-α has an important promoting function for blastema formation40. This suggests that Tnf-α may be involved in remodelling repair cells in the lesion site after spinal injury, which then creates an axon growth-promoting environment.
The role of Tnf-α for axonal regeneration in mammals is not clear. Some reports indicate axon growth promoting properties of Tnf-α41,42, whereas others show inhibition of axon growth43. Negative effects of Tnf-α on lesion-induced cell death44 and functional recovery37,45 have also been reported. However, knock out of Tnf-α had no reported effect after spinal injury46.
Preventing neutrophil formation in irf8 mutants, indicates that il-1β expressing neutrophils are major mediators of the inhibitory immune response in the absence of microglia and macrophages. However, the rescue of axon regrowth and swimming function was only partial. This could be explained by the absence of the early regeneration-promoting influence of the inflammation or basal keratinocytes still expressing il-1β in neutrophil-depleted irf8 mutants. In mammals, neutrophils cause secondary cell death47,48 and depleting neutrophils leads to favourable injury outcomes5, similar to our observations.
Macrophages control inflammation, as their absence in irf8 mutants leads to abnormally high expression levels of pro-inflammatory cytokines il-1β and tnf-α. This is similar to observations in fin regeneration49. In the absence of macrophages, positive feedback regulation of il-1β takes place, as indicated by more il-1β positive neutrophils and basal keratinocytes in the irf8 mutants and reduced il-1β mRNA levels when Il-1β function was inhibited. Moreover, a higher proportion of neutrophils were Il-1β+ in irf8 mutants, showing that without macrophages, neutrophils have a more pro-inflammatory phenotype. We show that macrophages/microglia, together with other tissues, express anti-inflammatory cytokines tgf-β1a and tgf-β3 and could thus be partly responsible for reducing pro-inflammatory phenotypes in wildtype animals.
Macrophages do not promote regeneration primarily by preventing cell death or removing debris. We observed phagocytosing macrophages by time-lapse imaging and debris levels were clearly increased it the absence of macrophages in irf8 mutants. However, when axon regrowth was rescued in the mutant by Il-1β inhibition, debris levels were still higher than in controls. Preventing cell death did not rescue axon growth and inhibition phagocytosis in wildtype animals did not impair regeneration. Hence, regenerative success does not correlate with debris abundance. Interestingly, in fin regeneration, lack of macrophages also leads to increased cell death. As this leads to death of tissue progenitor cells, fin regeneration is inhibited49. In mammalian spinal injury, debris, especially myelin debris, is inhibitory to regeneration50.
Are macrophages the most important immune cell type for axonal regrowth? Unimpaired axonal regrowth in the csfr1a/b mutant, in which microglial cells are absent and neutrophils are strongly reduced in number, indicates that these cells may be dispensable for regeneration. However, the increase in peripheral macrophages in this mutant could have compensated for a possible regeneration-promoting role of microglia. Since some neutrophils are still present in the injury site in csfr1a/b mutants, these might contribute to promoting axonal regrowth.
Endothelial cells and myelinating cells are unlikely to be major mediators of early regeneration in larval spinal cord regeneration. Endothelial cells from injured blood vessels were slow to reform blood vessels and were rarely invading the lesion site. In contrast, in mammals endothelial cells accumulate in the injury site, where they may have anti-inflammatory functions51. Myelinating cells bridged the lesion site, but were not abundant and only did so, when axons had already crossed the lesion site. Although relatively late, axons become remyelinated, which may contribute to recovery of some swimming parameters after injury. In mammals, transplanted myelinating cells, such as olfactory ensheathing cells and Schwann cells have been shown to improve recovery after spinal injury52,53.
Astroglia-like processes cross the injury site and this depends on the immune response, as we show here. While these processes cross the injury site independently of and slightly later than axons and axons still cross when these cells are ablated1, astroglia-like processes produce growth factors that support axonal regeneration54,55.
Timing of the immune response is crucial for regenerative success after spinal lesion. Macrophages in mammals3,37 and zebrafish56 display pro-inflammatory and anti-inflammatory phenotypes and the anti-inflammatory phenotypes are seen as beneficial for regeneration7,8,9. We show that inflammation is rapidly downregulated in zebrafish concurrent with the upregulation of anti-inflammatory cytokines, which does not readily occur in mammals3.
In summary, we have established an accessible in vivo system to study complex interactions of immune cells and a spinal injury site in successful regeneration. This allows fundamental insight into the role of immune cells that may ultimately inform non-regenerating systems. Here, we demonstrate a pivotal role of macrophages in promoting functional spinal cord regeneration, by producing Tnf-α and controlling Il-1β-mediated inflammation.
Methods
Animals
All zebrafish lines were kept and raised under standard conditions57 and all experiments were approved by the British Home Office (project license no.: 70/8805). Regeneration proceeds within 48 h of the lesion, therefore most analyses of axonal regrowth, cellular repair, and behavioural recovery can be performed before the fish are protected under the A(SP)A 1986, reducing the number of animals used in regeneration studies following the principles of the 3 rs. Approximately 11,000 larvae of either sex were used for this study, of which 8% were over 5 dpf.
The following lines were used: WIK wild type zebrafish, Tg(Xla.Tubb:DsRed)zf14826, abbreviated as Xla.Tubb:DsRed58; Tg(mpeg1:EGFP)gl22, abbreviated as mpeg1:GFP59, and Tg(mpx:GFP)uwm1, abbreviated as mpx:GFP60, Tg(fli1:EGFP)y1, abbreviated as fli1:GFP61; irf8st95/st95, abbreviated as irf8 mutants18; csf1raj4e1/j4e1 × csf1rb+/re01 incrosses, phenotypically sorted for absence of 4C4+ cells in the head, abbreviated as csfr1a/b mutants19; TgBAC(pdgfrb:Gal4FF)ncv24; Tg(UAS:GFP), abbreviated as pdgfrb:GFP62,Tg(6xTCF/LefminiP:2dGFP), abbreviated as 6xTCF:dGFP63, Tg(claudin k:Gal4)ue101; Tg(14xUAS:GFP) abbreviated as cldnK:GFP64, Tg(tnfa:eGFP-F)sa43296, abbreviated as tnf-α:GFP56 and Tg(il-1β:eGFP)sh445, abbreviated as il-1β:GFP65.
Drug treatment
Dexamethasone (Dex) (Sigma, Gillingham, UK) was dissolved in DMSO to a stock concentration of 5 mM. The working concentration was 10 μM prepared by dilution from stock solution in fish water. Ac-YVAD-cmk (YVAD) (Sigma) was dissolved in DMSO to a stock concentration of 10 mM. The working concentration was 50 μM prepared by dilution from the stock solution in fish water. Q-VD-OPh (Sigma), abbreviated as QVD in the manuscript, was dissolved in DMSO to a stock concentration of 10 mM. The working concentration was 50 μM. O-Phospho-l-serine (L-SOP) (Sigma) was dissolved in PBS to a stock concentration of 10 mM. The working concentration was 10 μM prepared by dilution from stock solution. Lipopolysaccharides from Escherichia coli O55:B5 (LPS, Sigma) were dissolved in PBS to a stock concentration of 1 mg/ml. The working dilution was 50 μg/ml. Pomalidomide (Cayman Chemicals, Michigan, USA) was diluted in DMSO at a stock concentration of 10 mg/ml. For the treatments, 6.9 μl of the stock where diluted in 1.5 ml of fish water. Larvae were pre-treated for 2 h before the injury and were incubated for 24 and 48 hpl. Larvae were collected from the breeding tanks and were randomly divided into Petri dishes at a density of maximally 30 larvae per dish, but no formal randomisation method was used. For most drug treatments, larvae were incubated with the drug from 3 dpl until 5 dpl, if not indicated differently.
Spinal cord lesions
Zebrafish larvae at 3 dpf were anaesthetised in PBS containing 0.02% aminobenzoic-acid-ethyl methyl-ester (MS222, Sigma), as described1. Larvae were transferred to an agarose-coated petri dish. Following removal of excess water, the larvae were placed in a lateral position, and the tip of a sharp 30 ½ G syringe needle was used to inflict a stab injury or a dorsal incision on the dorsal part of the trunk at the level of the 15th myotome.
Behavioural analysis
Behavioural analysis was performed as previously described14. Briefly, lesioned and unlesioned larvae were touched caudal to the lesion site using a glass capillary. The swim distance of their escape response, the mean velocity and the meandering were recorded for 15 s after touch and analyzed using a Noldus behaviour analysis setup (EthoVision version 7). Data given is averaged from triplicate measures per fish. Between repeated measures, the larvae were left to recover for 1 min. The observer was blinded to the treatment during the behavioural assay. The assay was performed on five independent clutches in order to assess the behavioural recovery in the irf8 mutants and three independent clutches after the YVAD treatment.
Fluorescence-activated cell sorting
Macrophages and microglia were isolated from 4 dpf transgenic mpeg1:eGFP embryos by FACS. For this purpose, about 500 fish were lesioned by transecting the spinal cord. Trunk-containing lesion site were dissected and collected at 24 hpl and used for cell dissociation66. Cells purified after FACS were used for qRT-PCR.
Quantitative RT-PCR
RNA was isolated from the injury sites of the larvae using the RNeasy Mini Kit (Qiagen, Hilden, Germany). Forty larvae were used for each condition. cDNA used as template was created using the iScript™ cDNA Synthesis Kit (Bio-Rad, Munich, Germany). Standard RT-PCR was performed using SYBR Green Master Mix (Bio-Rad). qRT-PCR was performed at 58 °C using Roche Light Cycler 96 (Roche Diagnostics, West Sussex, UK) and relative mRNA levels determined using the Roche Light Cycler 96 SW1 software. Samples were run in duplicates and expression levels were normalised to β-actin control. Primers were designed to span an exon-exon junction using Primer-BLAST. Sequences are given in supplementary Table 2. All experiments were carried out at least as biological triplicates.
In situ hybridisation
For whole mount in situ hybridisation1, after fixation in 4% PFA, larvae were digested with 40 μg/ml Proteinase K (Invitrogen, Carlsbad, USA). Thereafter, larvae were washed briefly in PBT and were re-fixed for 20 min in 4% PFA followed by washes in PBT. After washes, larvae were incubated at 67 °C for 2 h in pre-warmed hybridisation buffer. Hybridisation buffer was replaced with digoxigenin (DIG) labelled ISH probes diluted in hybridisation buffer and incubated at 67 °C overnight. The next day, larvae were washed thoroughly at 67 °C with hybridisation buffer, 50% 2× SSCT/50% deionized formamide, 2x SSCT and 0.2x SSCT. Larvae were then washed in PBT and incubated for 1 h in blocking buffer under slow agitation. Thereafter, larvae were incubated overnight at 4 °C in blocking buffer containing pre-absorbed anti-DIG antibody. The next day, larvae were washed in PBT, followed by washes in staining buffer. Colour reaction was performed by incubating larvae in staining buffer supplemented with NBT/BCIP (Sigma-Aldrich) substrate. The staining reaction was terminated by washing larvae in PBT.
Immunofluorescence
All incubations were performed at room temperature unless stated otherwise. Antibodies used are listed in supplementary Table 3. For most immunolabelling experiments, the larvae were fixed in 4% PFA-PBS containing 1% DMSO at 4 °C overnight. After washes in PBS, larvae were washed in PBTx. After permeabilization by incubation in PBS containing 2 mg/ml Collagenase (Sigma) for 25 min larvae were washed in PBTx. They were then incubated in blocking buffer for 2 h and incubated with primary antibody (1:50–1:500) diluted in blocking buffer at 4 °C overnight. On the following day, larvae were washed times in PBTx, followed by incubation with secondary antibody diluted in blocking buffer (1:300) at 4 °C overnight. The next day, larvae were washed three times in PBTx and once in PBS for 15 min each, before mounting in glycerol.
For whole mount immunostaining using primary antibodies from the same host species (rabbit anti-Il-1β, rabbit anti-Mpx, rabbit anti-Tp63) the samples were initially incubated with the first primary antibody at 4 °C overnight. After washes with PBTx the samples were incubated with the conjugated first secondary antibody overnight at 4 °C. Subsequently, samples were incubated with blocking buffer for 1 h at RT in order to saturate open binding sites of the first primary antibody. Next, the samples were incubated with unconjugated Fab antibody against the host species of the primary antibody in order to cover the IgG sites of the first primary antibody, so that the second secondary antibody will not bind to it. After this, samples were incubated with the second primary antibody overnight at 4 °C and subsequently with the second conjugated secondary antibody overnight at 4 °C before mounting in glycerol. No signal was detected when the second primary antibody was omitted, indicating specificity of the consecutive immunolabeling protocol.
For whole mount immunostaining of acetylated tubulin1, larvae were fixed in 4% PFA for 1 h and then were dehydrated and transferred to 100% MeOH and then stored at −20 °C overnight. The next day, head and tail were removed, and the samples were incubated in pre-chilled Acetone. Thereafter, larvae were washed and digested with Proteinase K and re-fixed in 4% PFA. After washes the larvae were incubated with BSA in PBTx for 1 h. Subsequently the larvae were incubated for 2 overnights with primary antibody (acetylated tubulin). After washes and incubation with the secondary antibody the samples were washed in PBS for 15 min each, before mounting in glycerol.
Evaluation of cell death using acridine orange
In order to assess the levels of cell death after injury we used the acridine orange live staining as described by others67. Briefly, at 1 and 2 dpl the larvae were incubated in 2.5 μg/ml solution of dye diluted into conditioned water for 20 min. After the staining, the larvae were washed by changing the water and larvae were live-mounted for imaging.
Identification of dying cells after injury
In order to assess the levels of cell death after injury cross sections of larvae were used. Larvae were fixed in 4% PFA overnight at 4 °C. After washes with 0.5% PBSTx, the larvae were transferred to 100% methanol and incubated for 10 min at room temperature. After rehydration, the larvae were washed with PBSTx 0.5%. Following this, larvae were mounted in 4% agarose and 50 μm sections were performed using a vibratome (MICROM HM 650 V, VWR, Leicestershire, UK). The sections were then permeabilized using 14 μg/ml diluted in 0.5% PBSTx. After brief wash with PBSTx the sections were postfixed in 4% PFA for 20 min. Excess PFA was washed out and the samples were incubated with the TUNEL reaction mix according to the In-situ Cell Death Detection Kit TMR red protocol (Roche).
Western blotting
Zebrafish larvae were sacrificed by an overdose of MS-222 at 4 dpf and used for protein extraction. Around 60 fish per condition were homogenised in 250 µl of 1x PBS/1% Triton X-100 (containing protease inhibitor cocktail complete, Roche Diagnostics), using a tissue grinder. After 1 h incubation at 4 degrees, lysates were centrifuged at 12,000 rpm for 20 mins to remove Triton-X-100-insoluble debris. Protein concentrations were quantified using a BCA assay following manufacturer’s instruction and the same amount of protein for each sample was loaded on a denaturating 12% acrylamide gel. After the electrophoretic run, the proteins were transferred on a nitrocellulose membrane (BioRad, Germany) and, after 1 h blocking in PBS/5% non-fat dry milk/0.1% Tween-20, probed with either rabbit anti-TNFα (1:2000, Anaspec; Fremont, CA), rabbit anti IL-1 (1:200, Proteintech, Manchester, UK) or mouse anti-α Tubulin (1:2000, DSHB) O/N at 4 degrees. Goat anti-rabbit (IRdye680LT, LI-COR, Lincoln, Nebraska, USA) and goat anti-mouse (IRdye800CW, LI-COR) secondary antibodies were used and the signal was detected by an Odyssey (LI-COR) imaging system and analysed with the Image Studio Lite software version 5.2.
Morpholino injection
All morpholinos were injected into single cell stage larvae in total volume of 2 nl. Knockdown of il-1β was carried out using the antisense morpholino against il-1β (5ʹ-CCCACAAACTGCAAAATATCAGCTT-3ʹ), targeting the splice site between intron 2 and exon 3 according to31. In order to block neutrophil development, we used the previously described MO combination of pu.1 (5′-GATATACTGATACTCCATTGGTGGT-3′) which targets the translational start (ATG) of the pu.1 and the splice blocking MO against gcsfr (5′- TTTGTCTTTACAGATCCGCCAGTTC-3′)16. All morpholinos and standard control (5′-CCTCTTACCTCAGTTACAATTTATA-3′) were obtained from Gene Tools, LLC, Oregon, USA.
CRISPR-mediated genome editing
CRISPR gRNA for il-1β was designed using CRISPR Design (http://crispr.mit.edu) and ZiFit (http://zifit.partners.org/ZiFiT) webtools. Vectors were generated by ligating the annealed oligonucleotides into the pT7-gRNA expression vector1. The gRNA was transcribed using the mMESSAGE mMACHINE T7 kit (Ambion, ThermoFisher SCIENTIFIC, Loughborough, UK) and assessed for size and quality on an electrophoresis gel. The injection mix consisted of 75 pg il-1β gRNA (target sequence: 5′-TGTGGAGCGGAGCCTTCGGCGGG-3′) and 150 pg Cas9 RNA and was injected into single cell stage larvae. The CrRNA for tnf-α (target sequence: 5′-CCCGATGATGGCATTTATTTTGT-3′) and the tracrRNA were ordered from Merck KGaA (Germany, Darmstadt). The injection mix included 1 μl Tracer 250 ng/μl, 1 μl gRNA, 1 μl Cas9 protein, 1 μl RNAse free H20, 1 μl fluorescent dextran. Larvae injected with GFP gRNA (target sequence: 5′GGCGAGGGCGATGCCACCTA-3) and uninjected larvae were used as controls. The efficiency of the mutagenesis was assessed by RFLP analysis.
Live imaging of zebrafish larvae and time-lapse imaging
For the acquisition of all fluorescent images, LSM 710 and LSM 880 confocal microscopes were used. For live confocal imaging, zebrafish larvae were anesthetized in PBS containing 0.02% MS222 and mounted in 1.5% low melting point agarose (Ultra-PureTM, Invitrogen). During imaging, the larvae were covered with 0.01% MS222-containing fish water to keep preparations from drying out. For time-lapse imaging, agarose covering the lesion site was gently removed after gelation. Time-lapse imaging was performed for 19 h starting at 6 hpl. Acquired time-lapse images were denoised using the ImageJ plugin CANDLE-J algorithm. Comparison of raw movies with CANDLE-J-processed movies showed that edges of features remained conserved after denoising.
Scoring and measurement of spinal cord bridging
Axonal and astroglial bridging was scored in fixed and live mounted samples using fluorescence-equipped stereomicroscope (Leica MDG41) and confocal microscopes (LSM 710, LSM 880) at time points of interest as previously described1. Any continuity of labelling between the two spinal cord stumps was scored as “bridged”. In some cases, the thickness of the axonal bridge was measured in collapsed confocal image stacks, by determining the length of (a) vertical line(s) that covers the width of crossing fascicles at the centre of the injury site. The observer was blinded to the experimental condition before scoring or measuring and experiments were performed blinded to the experimental condition on at least three independent clutches of larvae.
Cell counting in whole-mounted larvae
A volume of interest was defined centred on the lesion site from confocal images. The dimensions were: width = 200 μm, height = 75 μm (above the notochord), depth = 50 μm. Images were analysed using the Imaris (Bitplane, Belfast, UK) or ImageJ software. The number of cells was quantified manually in 3D view, blinded to the experimental condition on at least three independent clutches of larvae.
Quantification of diffuse signals in whole-mount larvae
For most quantifications of diffuse signal, e.g., acridine orange, image stacks, centred in the lesion site (height: 50 µm) were collapsed and an area of interest defined: width = 100 μm, height = 50 μm (above the notochord). The image was thresholded and the ‘’Analyze Particles” tool in Fiji with default settings was used to calculate the percentage of area taken up by signal.
To quantify Col I and Tnf-α in the injury site (Supplementary Figs 4C and 9A) we used a previously published protocol1. Briefly, image stacks were collapsed, thresholded and the area of the signal was measured.
All analyses were performed blinded to the experimental condition on at least three independent clutches of larvae.
Statistical analysis
Power analysis using G*Power68, was used to calculate power (aim > 0.8) for the experiments and determine the group sizes accordingly. Statistical power was >0.8 for all experiments. All quantitative data were tested for normality and analyzed with parametric and non-parametric tests as appropriate. The statistical analysis was performed using IBM SPSS Statistics 23.0. Shapiro-Wilk’s W-test was used in order to assess the normality of the data. Quantitative RT-PCR data were analyzed as previously described69,70. Kruskal–Wallis test followed by Dunn’s multiple comparisons, One-way ANOVA followed by Bonferroni multiple comparisons test, two-way ANOVA, followed by Bonferroni multiple comparisons, t-test, Mann–Whitney U-test or Fischer’s exact test were used, as indicated in the figure legends. *P < 0.05, **P < 0.01, ***P < 0.001, n.s. indicates no significance. Error bars indicate the standard error of the mean (SEM). The Figures were prepared with Adobe Photoshop CC and Adobe Illustrator CC. Graphs were generated using GraphPad Prism 7.
Data availability
The authors declare that all data supporting the findings of this study are available within the article and its supplementary information files, or from the corresponding authors on reasonable request.
References
Wehner, D. et al. Wnt signaling controls pro-regenerative Collagen XII in functional spinal cord regeneration in zebrafish. Nat. Commun. 8, 126 (2017).
Becker, T., Wullimann, M. F., Becker, C. G., Bernhardt, R. R. & Schachner, M. Axonal regrowth after spinal cord transection in adult zebrafish. J. Comp. Neurol. 377, 577–595 (1997).
Kigerl, K. A. et al. Identification of two distinct macrophage subsets with divergent effects causing either neurotoxicity or regeneration in the injured mouse spinal cord. J. Neurosci. 29, 13435–13444 (2009).
Norden, D. M., Muccigrosso, M. M. & Godbout, J. P. Microglial priming and enhanced reactivity to secondary insult in aging, and traumatic CNS injury, and neurodegenerative disease. Neuropharmacology 96, 29–41 (2015).
Taoka, Y. et al. Role of neutrophils in spinal cord injury in the rat. Neuroscience 79, 1177–1182 (1997).
Tran, A. P., Warren, P. M. & Silver, J. The biology of regeneration failure and success after spinal cord injury. Physiol. Rev. 98, 881–917 (2018).
Gensel, J. C. et al. Macrophages promote axon regeneration with concurrent neurotoxicity. J. Neurosci. 29, 3956–3968 (2009).
David, S., Bouchard, C., Tsatas, O. & Giftochristos, N. Macrophages can modify the nonpermissive nature of the adult mammalian central nervous system. Neuron 5, 463–469 (1990).
Yin, Y. et al. Oncomodulin is a macrophage-derived signal for axon regeneration in retinal ganglion cells. Nat. Neurosci. 9, 843–852 (2006).
Becker, T. & Becker, C. G. Axonal regeneration in zebrafish. Curr. Opin. Neurobiol. 27C, 186–191 (2014).
Renshaw, S. A. & Trede, N. S. A model 450 million years in the making: zebrafish and vertebrate immunity. Dis. Model Mech. 5, 38–47 (2012).
Becker, T. & Becker, C. G. Regenerating descending axons preferentially reroute to the gray matter in the presence of a general macrophage/microglial reaction caudal to a spinal transection in adult zebrafish. J. Comp. Neurol. 433, 131–147 (2001).
Hui, S. P., Dutta, A. & Ghosh, S. Cellular response after crush injury in adult zebrafish spinal cord. Dev. Dyn. 239, 2962–2979 (2010).
Ohnmacht, J. et al. Spinal motor neurons are regenerated after mechanical lesion and genetic ablation in larval zebrafish. Development 143, 1464–1474 (2016).
Hui, S. P. et al. Zebrafish regulatory T cells mediate organ-specific regenerative programs. Dev. Cell 43, 659–672 e655 (2017).
Feng, Y., Renshaw, S. & Martin, P. Live imaging of tumor initiation in zebrafish larvae reveals a trophic role for leukocyte-derived PGE(2). Curr. Biol. 22, 1253–1259 (2012).
Novoa, B., Bowman, T. V., Zon, L. & Figueras, A. LPS response and tolerance in the zebrafish (Danio rerio). Fish. Shellfish. Immunol. 26, 326–331 (2009).
Shiau, C. E., Kaufman, Z., Meireles, A. M. & Talbot, W. S. Differential requirement for irf8 in formation of embryonic and Adult macrophages in zebrafish. PLoS One 10, e0117513 (2015).
Oosterhof, N. et al. Colony-stimulating factor 1 receptor (CSF1R) regulates microglia density and distribution, but not microglia differentiation in vivo. Cell Rep. 24, 1203–1217.e1206 (2018).
Newby, A. C. Metalloproteinase expression in monocytes and macrophages and its relationship to atherosclerotic plaque instability. Arterioscler. Thromb. Vasc. Biol. 28, 2108–2114 (2008).
Rosenberg, A. F., Wolman, M. A., Franzini-Armstrong, C. & Granato, M. In vivo nerve-macrophage interactions following peripheral nerve injury. J. Neurosci. 32, 3898–3909 (2012).
Villegas, R. et al. Dynamics of degeneration and regeneration in developing zebrafish peripheral axons reveals a requirement for extrinsic cell types. Neural Dev. 7, 19 (2012).
Keoni, C. L. & Brown, T. L. Inhibition of apoptosis and efficacy of pan caspase iInhibitor, Q-VD-OPh, in models of human disease. J. Cell Death 8, 1–7 (2015).
Ogryzko, N. V. et al. Zebrafish tissue injury causes upregulation of interleukin-1 and caspase-dependent amplification of the inflammatory response. Dis. Model Mech. 7, 259–264 (2014).
Witting, A., Muller, P., Herrmann, A., Kettenmann, H. & Nolte, C. Phagocytic clearance of apoptotic neurons by Microglia/Brain macrophages in vitro: involvement of lectin-, integrin-, and phosphatidylserine-mediated recognition. J. Neurochem. 75, 1060–1070 (2000).
Finnson, K. W., McLean, S., Di Guglielmo, G. M. & Philip, A. Dynamics of transforming growth factor beta signaling in wound healing and scarring. Adv. Wound Care 2, 195–214 (2013).
Muller, G. W. et al. Amino-substituted thalidomide analogs: potent inhibitors of TNF-alpha production. ACS Med. Chem. Lett. 9, 1625–1630 (1999).
Savan, R., Kono, T., Igawa, D. & Sakai, M. A novel tumor necrosis factor (TNF) gene present in tandem with theTNF-alpha gene on the same chromosome in teleosts. Immunogenetics 57, 140–150 (2005).
Kisiswa, L. et al. TNFalpha reverse signaling promotes sympathetic axon growth and target innervation. Nat. Neurosci. 16, 865–873 (2013).
Vojtech, L. N., Scharping, N., Woodson, J. C. & Hansen, J. D. Roles of inflammatory caspases during processing of zebrafish interleukin-1beta in Francisella noatunensis infection. Infect. Immun. 80, 2878–2885 (2012).
Nguyen-Chi, M. et al. Transient infection of the zebrafish notochord with E. coli induces chronic inflammation. Dis. Model Mech. 7, 871–882 (2014).
Tauzin, S., Starnes, T. W., Becker, F. B., Lam, P. Y. & Huttenlocher, A. Redox and Src family kinase signaling control leukocyte wound attraction and neutrophil reverse migration. J. Cell. Biol. 207, 589–598 (2014).
Boato, F. et al. Interleukin-1 beta and neurotrophin-3 synergistically promote neurite growth in vitro. J. Neuroinflamm. 8, 183 (2011).
Temporin, K. et al. IL-1beta promotes neurite outgrowth by deactivating RhoA via p38 MAPK pathway. Biochem. Biophys. Res. Commun. 365, 375–380 (2008).
Boato, F. et al. Absence of IL-1beta positively affects neurological outcome, lesion development and axonal plasticity after spinal cord injury. J. Neuroinflamm. 10, 6 (2013).
Turrin, N. P. & Rivest, S. Tumor necrosis factor alpha but not interleukin 1 beta mediates neuroprotection in response to acute nitric oxide excitotoxicity. J. Neurosci. 26, 143–151 (2006).
Kroner, A. et al. TNF and increased intracellular iron alter macrophage polarization to a detrimental M1 phenotype in the injured spinal cord. Neuron 83, 1098–1116 (2014).
Liu, J. et al. TNF is a potent anti-inflammatory cytokine in autoimmune-mediated demyelination. Nat. Med. 4, 78–83 (1998).
Bruce, A. J. et al. Altered neuronal and microglial responses to excitotoxic and ischemic brain injury in mice lacking TNF receptors. Nat. Med. 2, 788–794 (1996).
Nguyen-Chi, M. et al. TNF signaling and macrophages govern fin regeneration in zebrafish larvae. Cell Death Dis. 8, e2979 (2017).
Schwartz, M. et al. Tumor necrosis factor facilitates regeneration of injured central nervous system axons. Brain Res. 545, 334–338 (1991).
Saleh, A. et al. Tumor necrosis factor-alpha elevates neurite outgrowth through an NF-kappaB-dependent pathway in cultured adult sensory neurons: diminished expression in diabetes may contribute to sensory neuropathy. Brain Res. 1423, 87–95 (2011).
Kato, K., Liu, H., Kikuchi, S., Myers, R. R. & Shubayev, V. I. Immediate anti-tumor necrosis factor-alpha (etanercept) therapy enhances axonal regeneration after sciatic nerve crush. J. Neurosci. Res. 88, 360–368 (2010).
Ferguson, A. R. et al. Cell death after spinal cord injury is exacerbated by rapid TNF alpha-induced trafficking of GluR2-lacking AMPARs to the plasma membrane. J. Neurosci. 28, 11391–11400 (2008).
Genovese, T. et al. TNF-alpha blockage in a mouse model of SCI: evidence for improved outcome. Shock 29, 32–41 (2008).
Farooque, M., Isaksson, J. & Olsson, Y. Improved recovery after spinal cord injury in neuronal nitric oxide synthase-deficient mice but not in TNF-alpha-deficient mice. J. Neurotrauma 18, 105–114 (2001).
Saiwai, H. et al. The LTB4-BLT1 axis mediates neutrophil infiltration and secondary injury in experimental spinal cord injury. Am. J. Pathol. 176, 2352–2366 (2010).
Kubota, K. et al. Myeloperoxidase exacerbates secondary injury by generating highly reactive oxygen species and mediating neutrophil recruitment in experimental spinal cord injury. Spine 37, 1363–1369 (2012).
Hasegawa, T. et al. Transient inflammatory response mediated by interleukin-1beta is required for proper regeneration in zebrafish fin fold. eLife 6, e22716 (2017).
Church, J. S., Milich, L. M., Lerch, J. K., Popovich, P. G. & McTigue, D. M. E6020, a synthetic TLR4 agonist, accelerates myelin debris clearance, Schwann cell infiltration, and remyelination in the rat spinal cord. Glia 65, 883–899 (2017).
Cohen, M. et al. Newly formed endothelial cells regulate myeloid cell activity following spinal cord injury via expression of CD200 ligand. J. Neurosci. 37, 972–985 (2017).
Nakhjavan-Shahraki, B. et al. Transplantation of olfactory ensheathing cells on functional recovery and neuropathic pain after spinal cord injury; systematic review and meta-analysis. Sci. Rep. 8, 325 (2018).
Bunge, M. B. Efficacy of Schwann cell transplantation for spinal cord repair is improved with combinatorial strategies. J. Physiol. 594, 3533–3538 (2016).
Mokalled, M. H. et al. Injury-induced ctgfa directs glial bridging and spinal cord regeneration in zebrafish. Science 354, 630–634 (2016).
Goldshmit, Y. et al. Fgf-dependent glial cell bridges facilitate spinal cord regeneration in zebrafish. J. Neurosci. 32, 7477–7492 (2012).
Nguyen-Chi, M. et al. Identification of polarized macrophage subsets in zebrafish. eLife 4, e07288 (2015).
Westerfield, M. The Zebrafish Book: A Guide for the Laboratory use of Zebrafish (Danio rerio). 4th edn. (University of Oregon Press, 2000).
Peri, F. & Nusslein-Volhard, C. Live imaging of neuronal degradation by microglia reveals a role for v0-ATPase a1 in phagosomal fusion in vivo. Cell 133, 916–927 (2008).
Ellett, F., Pase, L., Hayman, J. W., Andrianopoulos, A. & Lieschke, G. J. mpeg1 promoter transgenes direct macrophage-lineage expression in zebrafish. Blood 117, e49–e56 (2011).
Renshaw, S. A. et al. A transgenic zebrafish model of neutrophilic inflammation. Blood 108, 3976–3978 (2006).
Lawson, N. D. & Weinstein, B. M. In vivo imaging of embryonic vascular development using transgenic xebrafish. Dev. Biol. 248, 307–318 (2002).
Ando, K. et al. Clarification of mural cell coverage of vascular endothelial cells by live imaging of zebrafish. Development 143, 1328–1339 (2016).
Shimizu, N., Kawakami, K. & Ishitani, T. Visualization and exploration of Tcf/Lef function using a highly responsive Wnt/beta-catenin signaling-reporter transgenic zebrafish. Dev. Biol. 370, 71–85 (2012).
Münzel, E. J. et al. Claudin k is specifically expressed in cells that form myelin during development of the nervous system and regeneration of the optic nerve in adult zebrafish. Glia 60, 253–270 (2012).
Ogryzko, N. V. et al. Macrophage Il-1beta protects against mycobacterial infection downstream of Hif-1alpha in zebrafish. bioRxiv 306506, https://doi.org/10.1101/306506 (2018).
Reimer, M. M. et al. Dopamine from the brain promotes spinal motor neuron generation during development and adult regeneration. Dev. Cell 25, 478–491 (2013).
Tucker, B. & Lardelli, M. A rapid apoptosis assay measuring relative acridine orange fluorescence in zebrafish embryos. Zebrafish 4, 113–116 (2007).
Faul, F., Erdfelder, E., Buchner, A. & Lang, A. G. Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav. Res. Methods 41, 1149–1160 (2009).
Ganger, M. T., Dietz, G. D. & Ewing, S. J. A common base method for analysis of qPCR data and the application of simple blocking in qPCR experiments. BMC Bioinform. 18, 534 (2017).
Livak, K. J. & Schmittgen, T. D. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25, 402–408 (2001).
Acknowledgements
We thank Dr. William Talbot and Dr. Stephen Renshaw for sharing mutants before publication, Dr. Bertrand Vernay for expert advice on microscopy and Joly Ghanawi for excellent fish facility management. Supported by the BBSRC to C.G.B. and T.B., NC3Rs PhD studentship to C.G.B./T.B. for T.M.T., DFG to D.W., Summer research studentships to T.M. (Carnegie Trust) and EK (Anatomical Society). N.O. was funded by Biotechnology and Biological Sciences Research Council (BBSRC) project grant (BB/L000830/1). T.M.T. and M.K. are currently being paid by Biogen who did not have any influence on this study.
Author information
Authors and Affiliations
Contributions
Conceptualisation–T.M.T., T.Be. and C.G.B.; Investigation–T.M.T., D.W., L.C., T.M., M.K., M.L., A.U., T.Ba. and E.K.; Resources–N.O., S.A.R., Y.F. and T.J.H.; Supervision–D.W., N.O., Y.F., T.Be. and C.G.B.; Writing–T.M.T., T.Be. and C.G.B.; Funding acquisition–T.Be. and C.G.B.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tsarouchas, T.M., Wehner, D., Cavone, L. et al. Dynamic control of proinflammatory cytokines Il-1β and Tnf-α by macrophages in zebrafish spinal cord regeneration. Nat Commun 9, 4670 (2018). https://doi.org/10.1038/s41467-018-07036-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-018-07036-w
This article is cited by
-
Genes in Axonal Regeneration
Molecular Neurobiology (2024)
-
Ligament injury in adult zebrafish triggers ECM remodeling and cell dedifferentiation for scar-free regeneration
npj Regenerative Medicine (2023)
-
Glia instruct axon regeneration via a ternary modulation of neuronal calcium channels in Drosophila
Nature Communications (2023)
-
Impact of Copper Nanoparticles and Copper Ions on Transcripts Involved in Neural Repair Mechanisms in Rainbow Trout Olfactory Mucosa
Archives of Environmental Contamination and Toxicology (2023)
-
Sphk1 deficiency induces apoptosis and developmental defects and premature death in zebrafish
Fish Physiology and Biochemistry (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.