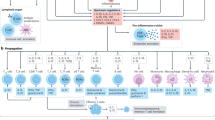
Abstract
Dendritic cells (DCs) play an important role in T cell alterations in primary hypertension (PH). We determined the numbers and maturation markers of peripheral blood total DCs (tDCs), myeloid cells (mDCs), and plasmacytoid cells (pDCs) and their association with hypertension-mediated organ damage (HMOD) markers and selected immune parameters in 30 adolescents with white coat hypertension (WCH), 25 adolescents with PH and a group of 35 age- and sex-matched children with normotension. Using multicolor flow cytometry, expression of maturation markers (CD86 and CD83) in tDCs (Lin1−/HLA-DR+), myeloid DCs (Lin1−/HLA-DR+/CD11c+) (mDCs), and plasmacytoid DCs (Lin1−/HLA-DR+/CD123+) (pDCs) and the distribution of peripheral Th17-bearing and T-reg cells were defined. In subjects with hypertension, carotid intima-media thickness (cIMT), left ventricular mass index (LVMI), and pulse wave velocity (PWV) were assessed. Compared with WCH and subjects with normotension, subjects with hypertension had reduced tDC and pDC numbers, an increased percentage of mDC subsets, an elevated mDC/pDC ratio, an increased population of mature mDC and pDC subsets bearing CD83 of high density, a decreased subset of CD86-bearing pDCs, and increased expression of DC activation markers (HLA-DR, CD86), as well as CD11c (mDCs) and CD123 (pDCs). PWV, LVMI, and cIMT values correlated negatively with tDCs and pDCs and positively with mDC numbers. Expression of DC maturation/activation markers (CD83, CD86, HLA-DR, CD11c, and CD123) correlated positively with PWV. Certain DC characteristics of WCH subjects resembled those of PH subjects (decreased tDC frequency and upregulation of activation marker expression). These changes correlated with HMOD. WCH subjects presented a DC phenotype that was intermediate between the normotensive and hypertensive phenotypes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Guzik TJ, Hoch NE, Brown KA, McCann LA, Rahman A, Sergey Dikalov, et al. Role of the T cell in the genesis of angiotensin II induced hypertension and vascular dysfunction. J Exp Med. 2007;204:2449–60.
Youn JC, You HT, Lim BJ, Koch MJ, Lee J, Chang DY, et al. Immunosenescent CD8+ T cells and C-X-C chemokine receptor type 3 are increased in human hypertension. Hypertension. 2013;32:126–33.
Gackowska L, Michalkiewicz J, Niemirska A, Helmin Basa A, Kłosowski M, Kubiszewska I, et al. Loss of CD31 receptor in CD4+ and CD8+ T cell subsets in children with primary hypertension is associated with hypertension severity and hypertensive target organ damage. J Hypertension. 2018;36:2148–56.
Kirabo A, Fontana V, de Faria AP, Loperena R, Galindoc L, Wu J, et al. DC isoketal-modified proteins activate T cells and promote hypertension. J Clin Invest. 2014;124:4642–56.
Dixon KB, Davies SS, Kirabo A. Dendritic cells and isolevuglandins in immunity, inflammation, and hypertension. Am J Physiol Heart Circ Physiol. 2017;312:H368–H374.
Vinh A, Chen W, Blinder Y, Weiss D, Tylor WR, Geronzy JJ, et al. Inhibition and genetic ablation of the B7/CD28 T cell costimulation axis prevents experimental hypertension. Circulation. 2010;122:2529–37.
O’Keeffe M, Mok WH, Radford KJ. Human dendritic cell subsets and function in health and disease. Cell Mol Life Sci. 2015;72:1–17.
Merad M, Sathe P, Helft J, Miller J, Mortha A. The dendritic cells lineage: ontogeny and function of dendritic cells and their subsets in the steady state and in the inflamed setting. Ann Rev Immunol. 2013;31:563–604.
Swiecki M, Colonna M. The multifaceted biology of plasmacytoid dendritic cells. Nat Rev Immunol. 2015;15:471–85.
Chen K, Wang JM, Yuan R, Yi X, Li L, Gong W, et al. Tissue resident dentridic cells and diseases involving dendritic cells malfunction. Int Immunopharmacol. 2016;34:1–15.
Litwin M, Michalkiewicz J, Gackowska L. Primary hypertension in children and adolescents is an immuno-metabolic disease with hemodynamic consequences. Curr Hypertens Rep. 2013;15:331–9.
Gackowska L, Michalkiewicz J, Helmin-Basa A, Klosowski M, Niemirska A, Obrycki L, et al. Regulatory T-cell subset distribution in children with primary hypertension is associated with hypertension severity and hypertensive target organ damage. J Hypertension. 2020;38:692–700.
Trojanek JB, Niemirska A, Grzywa R, Wierzbicka A, Obrycki Ł, Kułaga Z, et al. Leukocyte matrix metalloproteinase and tissue inhibitor gene expression patterns in children with primary hypertension. J Hum Hypertens. 2020;34:355–63.
Flynn JT, Daniels SR, Hayman LL, Maahs DM, McCrindle BW, Mitsnefes M, et al. American Heart Association Atherosclerosis, Hypertension and Obesity in Youth Committee of the Council on Cardiovascular Disease in the Young. Update: ambulatory blood pressure monitoring in children and adolescents: a scientific statement from the American Heart Association. Hypertension 2014;63:1116–35.
Doyon A, Kracht D, Bayazit AK, Deveci M, Duzova A, Krmar RT, et al. Carotid artery intima-media thickness and distensibility in children and adolescents: reference values and role of body dimensions. Hypertension 2013;62:550–6.
de Simone G, Daniels SR, Devereux RB, Meyer RA, Roman MJ, de Divitiis O, et al. Left ventricular mass and body size in normotensive children and adults: assessment of allometric relation of height for weight. J Am Coll Cardiol. 1992;20:1251–60.
Van Bortel LM, Laurent S, Boutouyrie P, Chowienczyk P, Cruickshank JK, De Backer T, et al. Artery Society; European Society of Hypertension Working Group on Vascular Structure and Function; European Network for Noninvasive Investigation of Large Arteries. Expert consensus document on the measurement of aortic stiffness in daily practice using carotid-femoral pulse wave velocity. J Hypertens. 2012;30:445–8.
Canonico B, Zamai L, Burattini S, Granger V, Mannello F, Gobbi P, et al. Evaluation of leukocyte stabilisation in TransFix-treated blood Samales by flow cytometry and transmission electron microscopy. J Immunol Methods. 2004;295:67–78.
Kulaga Z, Litwin M, Tkaczyk M, Rózdzyńska A, Barwicka K, Grajda A, et al. The height-, weight-, and BMI-for-age of Polish school-aged children and adolescents relative to international and local growth references. BMC Public Health. 2010;10:109.
Nguyen H, Chiasson VL, Chatterjee P, Kopriva SE, Young KJ, Mitchell BM. IL-17 causes Rho-kinase-mediated endothelial dysfunction and hypertension. Cardiovascular Res. 2013;97:696–704.
Kim MK, Kim J. Properties of mature and immature dendritic cells: phenotype, morphology, phagocytosis, and migration. R Soc Chem Adv. 2019;9:11230–8.
Curtsinger M, Mescher MF. Inflammatory cytokines as a third signal for T cell activation. Curr Opin Immunol. 2010;22:333–40.
Itani HA, Xiao L, Saleh MA, Wu J, Pilkinton MA, Dale BL, et al. CD70 exacerbates blood pressure elevation and renal damage in response to repeated hypertensive stimuli. Circ Res. 2016;118:1233–43.
Christ A, Temmerman L, Legein B, Daemen MJAP, Biessen EAL. : Dendritic cells in cardiovascular diseases. Circulation. 2013;128:2603–13.
Van Vre EA, Van Brussel I, Bosmans JM, Vrints CJ, Bult H. Dendritic cells in human atherosclerosis: from circulation to atherosclerotic plaques. Mediators Inflamm. 2011;2011:941396.
Gill MA, Blanco P, Arce E, Pascual V, Bancherau J, Pałucka AK. Blood dendritic cells and DC-poietins in systemic lupus erythematossus. Hum Immunol. 2002;63:1172–80.
Yilmaz A, Fuchs T, Dietel B, Altendorf R, Cicha I, Sumpf C, et al. Transient decrease in circulating dendritic cell precursors after acute stroke: potential recruitment into the brain. Clin Sci. 2010;118:147–57.
Sugi Y, Yasukawa H, Kai H, Fukui D, Futamata N, Mawatari K, et al. Reduction and activation of circulating dendritic cells in patients with decompensated heart failure. Int J Cardiol. 2011;147:258–64.
Yilmaz A, Weber J, Cicha I, Stumpf C, Klein M, Raithel D, et al. Decrease in circulating myeloid myeloid dendritic cell precursors in coronary artery disease. J Am Cell Cardiol. 2006;48:70–80.
VaN Brussel I, Van Vre EA, De Mayer GR, Vrints CJ, Bosman JM, Bult H. Decreased numbers of peripheral blood dendritic cells in patients with coronary artery disease are associated with diminished plasma Flt3 ligand levels and impaired plasmacytoid dendritic cell functions. Clin Sci. 2011;120:415–26.
Lu X, Rudemiller NP, Privratsky JR, Ren J, Wen Y, Griffiths R, et al. Classical dendritic cells mediate hypertension by promoting renal oxidative stress and fluid retention. Hypertension. 2020;75:131–8.
Litwin M, Feber J. Origins of primary hypertension in children: early vascular or biological aging? Hypertension 2020;76:1400–9.
Funding
The work was supported by research grant No. 2013/11/B/NZ4/03832 awarded by the National Research Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Kubiszewska, I., Gackowska, L., Obrycki, Ł. et al. Distribution and maturation state of peripheral blood dendritic cells in children with primary hypertension. Hypertens Res 45, 401–413 (2022). https://doi.org/10.1038/s41440-021-00809-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-021-00809-9
Keywords:
This article is cited by
-
Optimizing the generation of mature bone marrow-derived dendritic cells in vitro: a factorial study design
Journal of Genetic Engineering and Biotechnology (2023)
-
A new face among our Associate Editors
Hypertension Research (2023)
-
Pathophysiology of primary hypertension in children and adolescents
Pediatric Nephrology (2023)
-
Dendritic cells as potential initiators of immune-mediated hypertensive disorders
Hypertension Research (2022)