Abstract
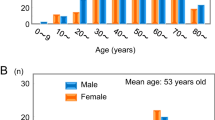
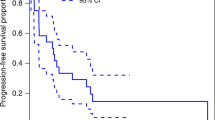
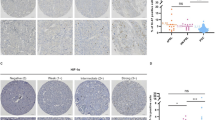
The available data on the natural history of pheochromocytomas and paragangliomas after radical surgery are heterogeneous and discordant. The aim of our retrospective multicenter study was to find predictors of recurrence in patients with pheochromocytomas and sympathetic paragangliomas submitted to radical surgery in Piedmont (a region in northwest Italy). We collected data from 242 patients diagnosed between 1990 and 2016. Forty-two patients (17.4%) had disease recurrence. Multivariate analysis showed that genetic mutation (HR = 3.62; 95% CI 1.44−9.13; p = 0.006), younger age (HR = 0.97; 95% CI 0.95−0.99; p = 0.031) and larger tumor size (HR = 1.01; 95% CI 1.00−1.02; p = 0.015) were independently associated with a higher recurrence risk of pheochromocytoma and paraganglioma; in pheochromocytomas, genetic mutation (HR = 3.4; 95% CI 1.00−11.48; p = 0.049), younger age (HR = 0.97; 95% CI 0.94−0.99; p = 0.02), higher tumor size (HR = 1.01; 95% CI 1.00−1.03; p = 0.043) and PASS value (HR = 1.16; 95% CI 1.03−1.3; p = 0.011) were associated with recurrence. Moreover, tumor size was the only predictor of metastatic pheochromocytoma and paraganglioma (HR = 4.6; 95% CI 1.4−15.0; p = 0.012); tumor size (HR = 3.93; 95% CI 1.2−16.4; p = 0.026) and PASS value (HR = 1.27; 95% CI 1.06−1.53; p = 0.007) were predictors of metastatic pheochromocytoma. In conclusion, our findings suggest that the recurrence of pheochromocytoma and sympathetic paraganglioma develops more frequently in younger subjects, patients with a family history of chromaffin tissue neoplasms, mutations in susceptibility genes, larger tumors and higher values of PASS. We recommend genetic testing in all patients with PPGL and strict follow-up at least on an annual basis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Lenders JWM, Duh Q-Y, Eisenhofer G, Gimenez-Roqueplo A-P, Grebe SKG, Murad MH, et al. Pheochromocytoma and paraganglioma: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2014;99:1915–42.
Ohno Y, Sone M, Taura D, Yamasaki T, Kojima K, Honda-Kohmo K. et al. Evaluation of quantitative parameters for distinguishing pheochromocytoma from other adrenal tumors. Hypertens Res. 2018;41:165–75.
Bravo EL, Gifford RW. Pheochromocytoma: diagnosis, localization and management. N Engl J Med. 1984;311:1298–303.
Thompson LDR. Pheochromocytoma of the adrenal gland scaled score (PASS) to separate benign from malignant neoplasms: a clinicopathologic and immunophenotypic study of 100 cases. Am J Surg Pathol. 2002;26:551–66.
Kimura N, Takayanagi R, Takizawa N, Itagaki E, Katabami T, Kakoi N, et al. Pathological grading for predicting metastasis in phaeochromocytoma and paraganglioma. Endocr Relat Cancer. 2014;21:405–14.
Koh JM, Ahn SH, Kim H, Kim BJ, Sung TY, Kim YH, et al. Validation of pathological grading systems for predicting metastatic potential in pheochromocytoma and paraganglioma. PLoS ONE. 2017;12:1–14.
Plouin PF, Amar L, Dekkers OM, Fassnach M, Gimenez-Roqueplo AP, Lenders JWM, et al. European Society of Endocrinology Clinical Practice Guideline for long-term follow-up of patients operated on for a phaeochromocytoma or a paraganglioma. Eur J Endocrinol. 2016;174:1–10.
Dahia PLM. Pheochromocytoma and paraganglioma pathogenesis: learning from genetic heterogeneity. Nat Rev Cancer. 2014;14:108–19.
Amar L, Lussey-Lepoutre C, Lenders JWM, Djadi-Prat J, Plouin PF, Steichen O. Recurrence or new tumors after complete resection of pheochromocytomas and paragangliomas: a systematic review and meta-analysis. Eur J Endocrinol. 2016;175:135–45.
Lam AK. Update on adrenal tumours in 2017 World Health Organization (WHO) of endocrine tumours. Endocr Pathol. 2017;28:213–27.
Korevaar TIM, Grossman AB. Pheochromocytomas and paragangliomas: assessment of malignant potential. Endocrine. 2011;40:354–65.
Ayala-Ramirez M, Feng L, Johnson MM, Ejaz S, Habra MA, Rich T, et al. Clinical risk factors for malignancy and overall survival in patients with pheochromocytomas and sympathetic paragangliomas: primary tumor size and primary tumor location as prognostic indicators. J Clin Endocrinol Metab. 2011;96:717–25.
Eisenhofer G, Goldstein DS, Sullivan P, Csako G, Brouwers FM, Lai EW, et al. Biochemical and clinical manifestations of dopamine-producing paragangliomas: Utility of plasma methoxytyramine. J Clin Endocrinol Metab. 2005;90:2068–75.
Eisenhofer G, Lenders JWM, Timmers H, Mannelli M, Grebe SK, Hofbauer LC, et al. Measurements of plasma methoxytyramine, normetanephrine, and metanephrine as discriminators of different hereditary forms of pheochromocytoma. Clin Chem. 2011;57:411–20.
Eisenhofer G, Tischler AS, De Krijger RR. Diagnostic tests and biomarkers for pheochromocytoma and extra-adrenal paraganglioma: from routine laboratory methods to disease stratification. Endocr Pathol. 2012;23:4–14.
Rao D, Peitzsch M, Prejbisz A, Hanus K, Fassnacht M, Beuschlein F, et al. Plasma methoxytyramine: clinical utility with metanephrines for diagnosis of pheochromocytoma and paraganglioma. Eur J Endocrinol. 2017;177:103–13.
Eisenhofer G, Lenders JWM, Siegert G, Bornstein SR, Friberg P, Milosevic D, et al. Plasma methoxytyramine: a novel biomarker of metastatic pheochromocytoma and paraganglioma in relation to established risk factors of tumour size, location and SDHB mutation status. Eur J Cancer. 2012;48:1739–49.
Rao F, Keiser HR, O’Connor DT. Malignant pheochromocytoma: chromaffin granule transmitters and response to treatment. Hypertension. 2000;36:1045–52.
Cotesta D, Caliumi C, Alò P, Petramala L, Reale MG, Masciangelo R, et al. High plasma levels of human chromogranin A and adrenomedullin in patients with pheochromocytoma. Tumori. 2005;91:53–8.
Amar L, Servais A, Gimenez-Roqueplo AP, Zinzindohoue F, Chatellier G, Plouin PF. Year of diagnosis, features at presentation, and risk of recurrence in patients with pheochromocytoma or secreting paraganglioma. J Clin Endocrinol Metab. 2005;90:2110–6.
Park J, Song C, Park M, Yoo S, Park SJ, Hong S. et al. Predictive characteristics of malignant pheochromocytoma. Korean J Urol. 2011;52:241–6.
Press D, Akyuz M, Dural C, Aliyev S, Monteiro R, Mino J, et al. Predictors of recurrence in pheochromocytoma. Surgery. 2014;156:1523–7.
John H, Ziegler WH, Hauri D, Jaeger P. Pheochromocytomas: can malignant potential be predicted? Urology. 1999;53:679–83.
Feng F, Zhu Y, Wang X, Wu Y, Zhou W, Jin X, et al. Predictive factors for malignant pheochromocytoma: analysis of 136 patients. J Urol. 2011;185:1583–9.
Cho YY, Kwak MK, Lee SE, Ahn SH, Kim H, Suh S, et al. A clinical prediction model to estimate the metastatic potential of pheochromocytoma/paraganglioma: ASES score. Surgery. 2018;0:1–7.
Goffredo P, Sosa JA, Roman SA. Malignant pheochromocytoma and paraganglioma: a population level analysis of long-term survival over two decades. J Surg Oncol. 2013;107:659–64.
Wiseman GA, Pacak K, O’Dorisio MS, Neumann DR, Waxman AD, Mankoff DA, et al. Usefulness of 123I-MIBG scintigraphy in the evaluation of patients with known or suspected primary or metastatic pheochromocytoma or paraganglioma: results from a prospective multicenter trial. J Nucl Med. 2009;50:1448–54.
Lenders JWM, Eisenhofer G. Update on modern management of pheochromocytoma and paraganglioma. Endocrinol Metab. 2017;32:152
Pasini B, Stratakis CA. SDH mutations in tumorigenesis and inherited endocrine tumours: lesson from the phaeochromocytoma-paraganglioma syndromes. J Intern Med. 2009;266:19–42.
Corssmit EP, Romijn JA. Management of endocrine disease: clinical management of paragangliomas. Eur J Endocrinol. 2014;171:231–43.
Kimura N, Watanabe T, Noshiro T, Shizawa S, Miura Y. Histological grading of adrenal and extra-adrenal pheochromocytomas and relationship to prognosis: a clinicopathological analysis of 116 adrenal pheochromocytomas and 30 extra-adrenal sympathetic paragangliomas including 38 malignant tumors. Endocr Pathol. 2005;16:23–32.
Strong VE, Kennedy T, Al-Ahmadie H, Tang L, Coleman J, Fong Y, et al. Prognostic indicators of malignancy in adrenal pheochromocytomas: clinical, histopathologic, and cell cycle/apoptosis gene expression analysis. Surgery. 2008;143:759–68.
Agarwal A, Mehrotra PK, Jain M, Gupta SK, Mishra A, Chand G, et al. Size of the tumor and pheochromocytoma of the adrenal gland scaled score (PASS): can they predict malignancy? World J Surg. 2010;34:3022–8.
Wu D, Tischler AS, Lloyd RV, DeLellis RA, De Krijger R, Van Nederveen F, et al. Observer variation in the application of the pheochromocytoma of the adrenal gland scaled score. Am J Surg Pathol. 2009;33:599–608.
Hamidi O, Young WF, Iñiguez-Ariza NM, Kittah NE, Gruber L, Bancos C, et al. Malignant pheochromocytoma and paraganglioma: 272 patients over 55 years. J Clin Endocrinol Metab. 2017;102:3296–305.
Hamidi O, Young WF, Gruber L, Smestad J, Yan Q, Ponce OJ, et al. Outcomes of patients with metastatic phaeochromocytoma and paraganglioma: a systematic review and meta-analysis. Clin Endocrinol (Oxf). 2017;87:440–50.
Opocher G, Schiavi F. Genetics of pheochromocytomas and paragangliomas. Best Pract Res Clin Endocrinol Metab. 2010;24:943–56.
Acknowledgements
For their contributions to the present study, we would like to thank Chiara Bima, Alessia Pozzato, Elena Capello, Erika Rainero and Elena Nasari.
Funding
This study was supported by a grant from the University of Turin. The work of P.M., M.P., B.P., F.V., E.G., E.A. and M.M. has been supported by the “Dipartimenti di Eccellenza 2018–2022” program (project no D15D18000410001). The funding sources had no role in the study design, data collection and analysis, manuscript preparation, or decision to submit the paper for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Parasiliti-Caprino, M., Lucatello, B., Lopez, C. et al. Predictors of recurrence of pheochromocytoma and paraganglioma: a multicenter study in Piedmont, Italy. Hypertens Res 43, 500–510 (2020). https://doi.org/10.1038/s41440-019-0339-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-019-0339-y
Keywords
This article is cited by
-
Pediatric malignant pheochromocytoma with atypical presentation as vision changes, lung metastasis, and recurrence: a case report
Journal of Medical Case Reports (2024)
-
A retrospective study on the association between urine metanephrines and cardiometabolic risk in patients with nonfunctioning adrenal incidentaloma
Scientific Reports (2022)
-
Minimally invasive adrenalectomy for large pheochromocytoma: not recommendable yet? Results from a single institution case series
Langenbeck's Archives of Surgery (2022)
-
Surgical outcomes in the pheochromocytoma surgery. Results from the PHEO-RISK STUDY
Endocrine (2021)
-
Recent advances in the management of pheochromocytoma and paraganglioma
Hypertension Research (2020)