Abstract
Objective
To evaluate the efficacy of immunomodulatory therapy (IMT) in paediatric anterior uveitis.
Methods
Chart review of all patients ≤ 18 years treated for anterior uveitis using a stepladder approach during a 10-year period. The type and duration of IMT were noted. The data were analysed depending on chronicity, aetiology, and type of IMT using appropriate statistical tests. The outcome measures included ocular complications, the need for surgical intervention, and visual outcomes.
Results
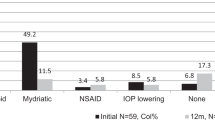
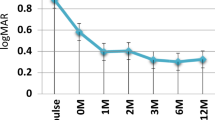
One hundred and thirty-four patients (191 eyes) were analyzed. The median age at diagnosis was 7 years (interquartile range (IQR): 7.5 years). The median follow-up was 4 years (IQR: 6 years). The most common causes of anterior uveitis were Juvenile idiopathic arthritis (64 patients, 47.8%) and undifferentiated (33 patients, 24.6%). All patients were started on topical steroids and cycloplegics. 94 (70%) patients required IMT. 92 (68.6%) were started on Methotrexate as the first agent, of which 21 (22%) were switched to a different agent owing to side effects. Biologic agent was added in 55 (41%) patients. 21 (16%) required switch to a second biologic agent, 5 (3.7%) to third, and 1 (0.8%) to fourth biologic agent. At the last exam, 11 (8%) had persistent inflammation. 55 (41%) had ocular complications, and 113 (84%) had a best corrected visual acuity ≥ 20/40.
Conclusion
Early introduction of IMT and switch to different agents may be required to control anterior uveitis and reduce the complications in children. IMT is safe and effective in treating paediatric anterior uveitis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Kump LI, Cervantes-Castañeda RA, Androudi SN, Foster CS. Analysis of pediatric uveitis cases at a tertiary referral center. Ophthalmology. 2005;112:1287–92.
Rosenberg KD, Feuer WJ, Davis JL. Ocular complications of pediatric uveitis. Ophthalmology. 2004;111:2299–306.
Thorne JE, Suhler E, Skup M, Tari S, Macaulay D, Chao J, et al. Prevalence of noninfectious uveitis in the united states: A claims-based analysis. JAMA Ophthalmol. 2016;134:1237–45.
Smith JA, Mackensen F, Sen HN, Leigh JF, Watkins AS, Pyatetsky D, et al. Epidemiology and course of disease in childhood uveitis. Ophthalmology. 2009;116:1544–51. 1551.e1541
de Boer J, Wulffraat N, Rothova A. Visual loss in uveitis of childhood. Br J Ophthalmol. 2003;87:879–84.
Cunningham ET Jr. Uveitis in children. Ocul Immunol Inflamm. 2000;8:251–61.
Nagpal A, Leigh JF, Acharya NR. Epidemiology of uveitis in children. Int Ophthalmol Clin. 2008;48:1–7.
Kadayifçilar S, Eldem B, Tumer B. Uveitis in childhood. J Pediatr Ophthalmol Strabismus. 2003;40:335–40.
Tugal-Tutkun I. Pediatric uveitis. J Ophthalmic Vis Res. 2011;6:259–69.
Cann M, Ramanan AV, Crawford A, Dick AD, Clarke SLN, Rashed F, et al. Outcomes of non-infectious paediatric uveitis in the era of biologic therapy. Pediatr Rheumatol Online J. 2018;16:51.
Wentworth BA, Freitas-Neto CA, Foster CS. Management of pediatric uveitis. F1000Prime Rep. 2014;6:41.
Curragh DS, O’Neill M, McAvoy CE, Rooney M, McLoone E. Pediatric uveitis in a well-defined population: Improved outcomes with immunosuppressive therapy. Ocul Immunol Inflamm. 2018;26:978–85.
Angeles-Han ST, Ringold S, Beukelman T, Lovell D, Cuello CA, Becker ML, et al. 2019 American College of Rheumatology/arthritis foundation guideline for the screening, monitoring, and treatment of juvenile idiopathic arthritis-associated uveitis. Arthritis Care Res. 2019;71:703–16.
Miraldi Utz V, Bulas S, Lopper S, Fenchel M, Sa T, Mehta M, et al. Effectiveness of long-term infliximab use and impact of treatment adherence on disease control in refractory, non-infectious pediatric uveitis. Pediatr Rheumatol Online J. 2019;17:79.
Jabs DA, Nussenblatt RB, Rosenbaum JT. Standardization of uveitis nomenclature for reporting clinical data. Results of the first international workshop. Am J Ophthalmol. 2005;140:509–16.
Ferrara M, Eggenschwiler L, Stephenson A, Montieth A, Nakhoul N, Araùjo-Miranda R, et al. The challenge of pediatric uveitis: Tertiary referral center experience in the united states. Ocul Immunol Inflamm. 2019;27:410–7.
Couto C, Frick MM, LaMattina K, Schlaen A, Khoury M, Lopez MM, et al. Chronic anterior uveitis in children. Ocul Immunol Inflamm. 2016;24:392–6.
Clarke LA, Guex-Crosier Y, Hofer M. Epidemiology of uveitis in children over a 10-year period. Clin Exp Rheumatol. 2013;31:633–7.
Zulian F, Martini G, Falcini F, Gerloni V, Zannin ME, Pinello L, et al. Early predictors of severe course of uveitis in oligoarticular juvenile idiopathic arthritis. J Rheumatol. 2002;29:2446–53.
Kotaniemi K, Kautiainen H, Karma A, Aho K. Occurrence of uveitis in recently diagnosed juvenile chronic arthritis: a prospective study. Ophthalmology. 2001;108:2071–5.
Gregory AC 2nd, Kempen JH, Daniel E, Kaçmaz RO, Foster CS, Jabs DA, et al. Risk factors for loss of visual acuity among patients with uveitis associated with juvenile idiopathic arthritis: the systemic immunosuppressive therapy for eye diseases study. Ophthalmology. 2013;120:186–92.
Woreta F, Thorne JE, Jabs DA, Kedhar SR, Dunn JP. Risk factors for ocular complications and poor visual acuity at presentation among patients with uveitis associated with juvenile idiopathic arthritis. Am J Ophthalmol. 2007;143:647–55.
Thorne JE, Woreta F, Kedhar SR, Dunn JP, Jabs DA. Juvenile idiopathic arthritis-associated uveitis: Incidence of ocular complications and visual acuity loss. Am J Ophthalmol. 2007;143:840–6.
Funding
This study is funded by Children’s Hospital Ophthalmology Foundation.
Author information
Authors and Affiliations
Contributions
All the authors were responsible for designing the review protocol, writing the protocol and manuscript, conducting the search, extracting and analyzing data, interpreting results, updating reference lists and creating’Summary of findings’ tables.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Huynh, E., Elhusseiny, A.M. & Nihalani, B.R. Paediatric anterior uveitis management in the USA: a single-centre, 10-year retrospective chart review exploring the efficacy and safety of systemic immunomodulatory therapy. Eye 37, 1325–1330 (2023). https://doi.org/10.1038/s41433-022-02121-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02121-3
This article is cited by
-
Encouraging visual outcomes in children with idiopathic and JIA associated uveitis: a population-based study
Pediatric Rheumatology (2023)