Abstract
5-aminosalicylate (5-ASA) is widely prescribed for the treatment of inflammatory bowel disease (IBD) and prevention of inflammation-associated colorectal cancer (CRC). Its clinical effect is widely attributed to modulation of host inflammatory responses. However, the recent association of intestinal dysbiosis and selective enrichment in Escherichia coli in patients with IBD and CRC raises the possibility that 5-ASA might also affect the enteric microflora. The aim of this study was to investigate the effect of 5-ASA on the growth and virulence of E. coli associated with IBD and CRC, and its impact on host cell inflammatory responses. Our results show that 5-ASA inhibited E. coli growth in a dose-dependent manner and downregulated the expression of bacterial virulence genes associated with IBD (fliC, fimH, ompC, yfgL, nlpL, lpfA, htrA, dsbA, fyuA, and chuA) and CRC (pks). 5-ASA inhibited E. coli motility (30–70%), epithelial adherence and invasion, and IL-8 secretion (p < 0.05). 5-ASA reduced E. coli survival in J774A.1 macrophages by 20 to 50% (p < 0.01) and TNF-α secretion by infected macrophages up to 30% (p < 0.05). In addition, 5-ASA reduced DNA damage in epithelial cells (Caco-2) induced by pks-positive E. coli. Our results reveal a multifaceted and previously unrecognized effect of 5-ASA on the growth and virulence of IBD- and CRC-associated E. coli, in addition to its inhibitory effect on host cell inflammatory responses. These results suggest that 5-ASA may abrogate the proinflammatory and oncogenic effects of E. coli in patients with IBD and CRC.
Similar content being viewed by others
Introduction
5-aminosalicylic acid (5-ASA, also known as mesalamine) has been used for several decades as a primary treatment for IBD [1]. It remains the cornerstone of therapy to induce and maintain remission in patients with mild to moderate ulcerative colitis (UC) [2]. Recent studies have demonstrated that 5-ASA prevents the development of colorectal cancer (CRC) in patients with long-standing colitis [3], and inhibits tumor growth in colon cancer patients [4]. The clinical effects of 5-ASA are widely attributed to pleiotropic modulation of host inflammatory responses, including inhibition of lipoxygenase and cyclooxygenase [5], interleukin-1 (IL-1) [6], tumor necrosis factor-alpha (TNF-α) [7], nuclear factor NF-ĸB [8, 9], and induction of peroxisome proliferator-activated receptor-gamma (PPARγ) [10, 11].
However, our understanding of the mechanisms of action of 5-ASA precedes the discovery of abnormalities in the resident intestinal microflora, termed “dysbiosis”, in patients with IBD and CRC. Mounting evidence implicates resident enteric bacteria in the pathogenesis of inflammatory bowel disease [12,13,14] and colorectal cancer [15, 16]. Resident E. coli, particularly the adherent and invasive E. coli (AIEC) pathotype, has been consistently linked to ileal Crohn’s disease (CD) and intestinal inflammation across species [17,18,19]. Furthermore, AIEC are frequently isolated from the colonic mucosa of patients with CRC [20], suggesting a possible link between E. coli and CRC development [21, 22]. CRC-associated E. coli frequently harbor the pks pathogenicity island that encodes multi-enzymatic machinery for synthesizing a peptide-polyketide hybrid genotoxin, colibactin. Colibactin can induce double-strand DNA breakage and, consequently, chromosomal instability involved in CRC [23]. While the effects of 5-ASA on host inflammatory responses are well recognized, it has emerged that 5-ASA can also modulate the expression of genes involved in metabolism and invasiveness of Salmonella [24], and the growth of Mycobacterium avium [25]. Treatment with 5-ASA has also been related to reduced transcription of 16S rRNA in resident enteric bacteria [26]. These observations raise the possibility that the beneficial effects of 5-ASA observed in IBD and CRC could be mediated, in part, by modulating intestinal bacteria.
It is against this background that we sought to examine the effects of 5-ASA on the growth and virulence of E. coli strains associated with IBD and CRC, and on the inflammatory responses of intestinal epithelial cells and macrophages. We also investigated the effect of 5-ASA on DNA damage induced by pks-positive E. coli. We found that 5-ASA abrogates the virulence of IBD- and CRC-associated E. coli in a multifaceted fashion, including growth, gene expression, motility, adhesion and invasion of epithelial cells, survival in macrophages, and induction of host inflammatory responses. In addition, 5-ASA inhibits DNA damage induced by pks-positive E. coli in intestinal epithelial cells. Our findings reveal previously unrecognized antimicrobial activity of 5-ASA against IBD- and CRC-associated E. coli and suggest that the beneficial effects of 5-ASA observed in patients with IBD and CRC may be due to a dual effect on host and enteric bacteria.
Materials and methods
Bacterial strains
Fifteen well characterized E. coli strains cultured from the intestinal mucosa of patients with IBD [17, 27] (7 strains) and CRC [20] (8 strains) were evaluated. The seven IBD associated strains (T75, 524–2, 541–1, 541–15, 578–1, 24LW-1, and LF82) were isolated from the ileums of patients with CD (Table 1). All of these strains except T75 have an AIEC pathotype. T75 is a non-pathogenic strain from a CD patient, and was used as a non-AIEC control in this study. Prototypical AIEC LF82 (kindly provided by Arlette Darfeuille-Michaud) was used as a positive control for AIEC. Of the 8 CRC-associated E. coli strains (Table 1), 7 were isolated from colonic mucosa of patients with non-IBD associated CRC (HM44, HM194, HM213, HM229, HM288, HM334, and HM354), and kindly provided by Dr. Jon Rhodes [20]. Strain NC101 was isolated from the feces of a healthy mouse, and induces CRC in IL10−/− AOM treated and monocolonized mice [22, 28]. All E. coli strains were stored at −70°C. Experimental cultures were derived from frozen stocks without subculture and grown in LB broth at 37oC ± treatments as described below.
Chemicals
5-ASA was purchased from Sigma-Aldrich (St. Louis, MO). Due to its strong hydrophobicity and sensitivity to oxidation, stock solutions were freshly made in DMSO (Fisher Scientific, Waltham, MA), and dilutions were made immediately before each experiment.
Standardized growth analysis
E. coli was grown in LB broth overnight at 37°C with shaking. Overnight cultures were diluted 1:100 into fresh LB broth containing either DMSO (Control) or 5-ASA at specified concentrations. Growth of E. coli was monitored for 12–24 h at 37 °C with shaking. At each time point, the turbidity of three samples from the same treatment was measured at OD600. Growth curves were plotted with OD600 as the function of time. For easier comparison between 5-ASA-treated and untreated control samples, the area under each growth curve (AUC) was calculated with Graphpad Prism7.03.
Transcriptional analysis of virulence genes
E. coli was grown in media with or without 5-ASA (1.5 mg ml−1) to mid log phase. RNA was extracted using the Qiagen RNAProtect-RNeasy Kit per manufacturer’s protocol. Total RNA was treated with TURBO DNA-Free Kit (Ambion), followed by a two-step qRT-PCR reaction, using Qiagen’s QuantiTect Reverse Transcription Kit and QuantiNova SYBR Green PCR Kit. Twelve genes associated with virulence of IBD- and CRC-associated E. coli [29,30,31,32,33,34,35,36] (see Table 2) were selected for transcriptional analysis in response to 5-ASA. E. coli uidA (Table 2) was used as the reference/house-keeping gene. Each qPCR reaction contained 1 μl of cDNA, 1.4 μl of each forward and reverse primers (10 μM), 10 µL of 2 × SYBR Green Master Mix, 2 μl of QN ROX Reference Dye, and 5.2 μl of nuclease-free water to make the total volume of 20 µl. The reaction was run with ABI7000 (Applied Biosystems). The comparative quantification (ΔCt) method was used to determine the up- or downregulated genes. The relative change of a targeted gene expression was calculated by using the equation RQ = 2−ΔΔCT.
Motility assay
E. coli was grown overnight at 37 °C in LB broth. Soft agar plates (1% tryptone, 0.5% NaCl, 0.25% agar) were prepared the day before assay. DMSO or 5-ASA was added into the agar to make final concentrations of 0, 1, and 1.5 mg ml−1. After transferring 2 μl of the overnight culture on to the center of each plate, high-motility E. coli strains were allowed to grow at 37 °C for 8 h; low motility strains grew for 18 h. Motility was quantified by measuring the diameter of the circular swarming area formed by the growing motile bacteria. E.coli T75, HM334, and HM358, were found to be non-motile and excluded from 5-ASA testing.
Cell lines and culture conditions
Human colonic epithelial cell line Caco-2 (ATCC HTB-37) and murine macrophage cell line J774A.1 (ATCC TIB-67) were obtained from the American Type Culture Collection. The HEK-Blue KD-TLR5 cell line was purchased from InvivoGen (San Diego, CA, USA). Caco-2 and J774A.1 cells were grown and maintained in media as described by Baumgart et al [17]. HEK-Blue KD-TLR5 cells were grown in DMEM (Gibco, Rockville, MD, USA) supplemented with 10% FBS. Monolayers of all cell lines were maintained at 37 °C with 5% CO2.
Adhesion and invasion of cultured epithelial cells
E. coli was cultured overnight in LB broth ± 5-ASA (1 mg ml−1) or DMSO (1%, Control) at 37 °C with shaking. Bacterial pellets were resuspended in PBS before dilution in cell culture media ± 5-ASA (1 mg ml−1) to an m.o.i (multiplicity of infection) of 10. Caco-2 cells were grown and infected with bacteria by the same procedure as described by Baumgart et al [17]. At 3 h post infection, the cells were washed 3× with PBS and lysed with 1% Triton X-100. Serial dilutions of the lysates were made in PBS and plated on LB agar. The total number of colonies recovered was used to calculate the number of adherent bacteria. For invasion assays, the cells were treated with gentamicin (100 µg ml−1) for one hour after initial infection and 3× wash with PBS to kill extracellular bacteria. Cells were then washed 3× after gentamicin treatment, lysed, and plated as described above.
E. coli survival in macrophages
Murine macrophage J774A.1 cells were seeded in 24-well plates (1 × 105 cells/well) and grown for two days at 37 °C with 5% CO2. E. coli was grown in LB broth with either 5-ASA (1 mg ml−1) or DMSO (1%) overnight at 37 ℃. E. coli was diluted in cell culture media at an m.o.i of 20. J774A.1 cells were infected with E. coli for 1 h at 37°C, washed 3 × with PBS, and treated with gentamicin (100 µg ml−1) for 1 h to kill extracellular bacteria. For E. coli uptake assays, J774A.1 cells were washed 3× with PBS, lysed in 1% Triton X-100, and enumerated by quantitative plating as described above. For intracellular survival assays, after the initial gentamycin treatment (100 µg ml−1), the cells were kept in medium containing 25 µg ml−1 gentamycin overnight at 37 °C. At 24 h post infection, the cells were washed 3× with PBS, and lysed with 1% Triton X-100. The number of E. coli survived was determined by quantitative plating. The bacterial survival rate was calculated as R = (# survived/# uptaken) × 100.
Proinflammatory cytokine secretion
Supernatants of Caco-2 (at 3 h post infection) and J774A.1 (at 24 h post infection) cell cultures were collected and centrifuged to remove any cells or cell debris. The concentrations of IL-8 secreted by Caco-2 cells, and TNF-α by J774A.1 cells were analyzed by ELISA methods, using Human IL-8 Antibody Pair Kit (Invitrogen), and mouse TNF-α Antibody Pair Kit (Invitrogen) per manufacturer’s instructions.
NF-ĸB activation assay
HEK-Blue KD-TLR5 cells were used to detect the induction of NF-ĸB by E. coli infection. The cells were seeded in 96-well plates at a density of 5 × 104 cells per well. E. coli, grown overnight in LB containing either 5-ASA (1 mg ml−1) or DMSO (1%), was diluted into the HEK-Blue KD-TLR5 medium at an m.o.i of 200 as 10 × inocula; 10 μl of this inoculum was added into each well containing 100 μl of medium for a final m.o.i of 20. Three replicates were performed for each strain and treatment. After 3 h of infection at 37 °C, the medium was removed gently from each well, and replaced with 100 µl of fresh medium containing gentamycin (200 μg ml−1). At 24 h post infection, the spent medium was collected, and centrifuged at 12,000 r.p.m. for 5 min to remove any particulate matter. Five microliters of the supernatant were used to quantify the production of SEAP (secreted alkaline phosphatase), an indicator of NF-ĸB promotor activity, with the QUANTI-Blue Kit (InvivoGen, San Diego, CA, USA) following the manufacturer’s instructions. The SEAP activities were detected as optical density at 620 nm.
PPARγ and TNF-α gene expression
Caco-2 cells at density of 1 × 106 cells/well in 12-well plates were treated with either DMSO (0.75%) or 5-ASA (0.75 mg ml−1) for 16 h at 37°C (low concentration of 5-ASA was used here because at higher concentrations, ≥1%, DMSO decreased cell viability in our preliminary tests). The cells were washed once with PBS, and infected with overnight cultures of LF82 pretreated with either DMSO (1%) or 5-ASA (1 mg ml−1) for 16 h at 37°C. After 3 h of incubation at 37°C, the cell medium was removed, and the cell surface was rinsed once with PBS, then detached with a rubber placeman and centrifuged at 10,000 r.p.m. for 3 min at 4 °C. The cell pellet was used to extract total RNA with Qiagen’s RNeasy Kit as per manufacturer’s instructions. PPARγ mRNA was analyzed by qRT-PCR with the same procedure as described above for bacterial virulence genes. The primers for PPARγ [10] included: Forward primer (F-primer) 5′-CCTGATAGGCCCCACTGTGT-3′ and Reverse primer (R-primer) 5′-CAGGTGGGAGTGGAACAAT-3′. The primers for the human house-keeping gene β-actin are 5′-TCACCCACACTGTGCCCATCTACG-3′ (F-primer) and 5′-CAGCGGAACCGCTCATTGCCAATG-3′ (R-primer).
Mouse macrophage cell line J774A.1 was used for examining TNF-α gene expression. J774A.1 cells in 12-well plates were pretreated as described for Caco-2 cells and infected with LF82 (see above) for 60 min at 37 °C. The cells were washed, harvested, and processed for total RNA isolation by the same procedure as for Caco-2 cells. The qPCR primers [10] for mouse TNF-α are 5′-TGGGAGTAGACAAGGTACAACCC-3′ (F-primer), and 5′-CATCTTCTCAAAATTCGAGTGACAA-3′ (R-primer). The mouse β-actin was used as the house-keeping gene, and its qPCR primers are 5′-GGGTCAGAAGGATTCCTATG-3′ (F-primer), and 5′-GGTCTCAAACATGATCTGGG-3′ (R-primer). Quantitative RT-PCR was carried out with the same procedure as described above.
Comet assay
The impact of 5-ASA on the genotoxicity of pks-positive E. coli was evaluated using single cell electrophoresis (comet assay). Three CRC-E. coli strains were evaluated: two pks-positive (NC101 and HM334), and one pks-negative (HM288). The comet assay was performed in dim light to reduce background DNA damage. For sample preparation, Caco-2 cells in 12-well plates were infected with E. coli with or without 5-ASA pretreatment as described above at an m.o.i of 20. After 3 h incubation at 37 °C, the cells were washed once with Ca+2- and Mg+2-free PBS, and lifted with 200 μl of pre-warmed trypsin-EDTA (Invitrogen) for 2 min at room temperature, and followed by addition of 500 μl of fresh cell medium to stop trypsin reaction. The cell suspension was centrifuged for 5 min at 3000 r.p.m. at 4 °C, and the cell pellet was resuspended in cold PBS (Ca+2- and Mg+2-free) to achieve a density of 1 × 105 cells ml−1. Trevigen’s Comet Assay Kit was used for the downstream process of comet assay, and the manufacture’s instruction was followed for all steps.
Statistical analysis
Differences in growth, gene expression, motility, adhesion, invasion, cytokine production, and NF-ĸB activation between control and 5-ASA -treated samples were analyzed by 2-way ANOVA with Dunnett’s test for multiple comparisons. All statistical analyses were performed with GraphPad Prism 7.03 software and p < 0.05 was considered significant.
Results
5-ASA downregulates E. coli activity in free culture
Inhibition of growth
The hydrophobicity and low solubility of 5-ASA in DMSO (maximum 5-ASA concentration = 100 mg ml−1) in concert with the adverse effects of DMSO on bacterial growth at concentrations > 2% (see Supplementary Data Figures S1A-G), restricted experiments to 5-ASA concentrations of ≤ 2 mg ml−1. In preliminary experiments we observed that 5-ASA at 1.5 mg ml−1 inhibited the growth of 15/15 E. coli strains (Table 1) after 24 h (data not shown). On this basis, we performed a series of titration experiments with 7 representative strains (Control: T75; AIEC: LF82, 541–1, 541–15, and NC101; and CRC: HM334 and HM288), at 5-ASA concentrations of 1, 1.5, and 2 mg ml−1 (@ 6.5 to 13 mM), which spans the clinically relevant range of 1–100 mM [24, 37], to identify minimal inhibitory concentrations of 5-ASA. Our results show that 5-ASA inhibited E. coli growth in a dose-dependent manner: 2 > 1.5 > 1 mg ml−1 (Fig. 1). For 6 out of 7 strains growth was inhibited (p < 0.05) by 5-ASA at the lowest concentration (1 mg ml−1). At lower concentrations (<1 mg ml−1), 5-ASA had no effect on E. coli growth (data not shown).
5-ASA inhibits growth of E. coli. E. coli was grown in LB broth containing either DMSO (Control) or 5-ASA at 1, 1.5, and 2 mg ml−1. Data were from one of three separate experiments, each with three replicates. AUC = area under the curve. The error bars show standard deviation (SD). *p < 0.05; **p < 0.01; ns, not significant
Inhibition of virulence gene transcription
Quantitative RT-PCR (qRT-PCR) was used to examine the effects of 5-ASA on the expression of a panel of 11 genes involved in the virulence of E. coli associated with IBD and CRC [29,30,31,32,33,34,35,36] (Table 2). This panel spans motility (fliC), epithelial cell adhesion and invasion (fimH, ompC, yfgL, nlpL, and lpfA), stress (htrA and dsbA), siderophores (chuA, and fyuA), and genotoxin (pks). As shown in Table 3, 5-ASA (1.5 mg ml−1) uniformly downregulated 10 representative virulence genes in CD-associated E. coli. The two stress-related genes, htrA or dsbA, involved in macrophage survival of E. coli [31, 32], were downregulated 2 to 5 folds in 5 of the 7 CD strains. Similar results were also observed with CRC-E. coli (Table 3). The transcription levels of the 11 virulence genes were broadly downregulated by 5-ASA treatment, especially in the 6 pks-positive strains (Table 3). In contrast, the two pks-negative strains (HM358 and HM288) responded differently to 5-ASA, with majority of the genes upregulated.
Inhibition of motility
E. coli motility impacts mucosal colonization [29, 38]. 5-ASA inhibited the transcription of the motility-related gene (fliC) in 5/7 CD-associated E. coli strains, and 5/6 fliC-positive CRC strains (Table 3). 5-ASA inhibited swarming of all motile CD- and CRC-E. coli (p < 0.05, Fig. 2a, b). The degree of inhibition was dose-dependent, e.g., the motility of strain 541–15 was 75 and 37% of the DMSO control at 1 and 1.5 mg ml−1 of 5-ASA (Fig. 2a), respectively. Strains T75, HM334, and HM358 were non-motile and excluded from this analysis.
5-ASA inhibits E. coli motility. Overnight cultures in LB broth were applied to the soft agar plates containing DMSO (Control), or 5-ASA at different concentrations (see Methods). Average diameters of the radial growth were used to calculate the relative motility. a Relative motility of different E. coli strains. The error bars (SD) and significance were derived from 4 replicates. **p < 0.01. b E. coli swarming images in the soft agar plates
5-ASA downregulates E. coli infectivity and proinflammatory responses of intestinal epithelial cells
Inhibition of E. coli infectivity
Due to its impact on virulence gene expression and motility, we hypothesized that 5-ASA might also impair the ability of E. coli to adhere to and invade intestinal epithelial cells. Four of the 6 pks-positive strains (HM44, HM164, HM313, and HM229) were excluded from these experiments because of their cytotoxic effect on host cells (data not shown). To some extent, 5-ASA reduced the ability of all E. coli strains to adhere to or invade Caco-2 cells (8 out of 11, p < 0.05) (Fig. 3a). The magnitude of the effect of 5-ASA on adhesion and invasion varied by strain and the impact on adhesion was independent of the impact on invasion, e.g., for CD-E. coli, the average inhibition of adhesion and invasion was 58 and 40%, respectively, whereas for CRC-E. coli, the average inhibition of adhesion and invasion was 55 and 62%, respectively.
5-ASA inhibits E. coli infectivity and host cell inflammatory responses. Overnight cultures grown in LB broth containing either DMSO or 5-ASA (1 mg ml−1) were used for infection. a Relative adhesion and invasion (three replicates); b IL-8 production (four replicates); c NF-ĸB activation (3 replicates); d Relative PPARγ gene expression (three replicates). In (d), the lowercase letters (above each column) represent the significance between treatments: same letters indicate no difference (p > 0.05), whereas different letters indicate significant difference (p < 0.01; see the Supplementary Data Table S1 for complete p values). The pre-treatments are shown in the parentheses along the x-axis. Error bars = SD. *p < 0.05, **p < 0.01
Reduction of IL-8 secretion by caco-2 cells
Bacterial infection induces the secretion of proinflammatory cytokines (e.g., IL-8) by intestinal epithelial cells [39]. Pre-treating CD-E. coli (5 of 7 strains) with 5-ASA reduced IL-8 production by Caco-2 cells in a strain-dependent fashion (p < 0.05; Fig. 3b). In addition, CD-associated E. coli induced more IL-8 secretion (p < 0.05) than CRC strains (Fig. 3b), and they also displayed greater inhibition (40–60%) of IL-8 production by 5-ASA than CRC-associated E. coli (10–20%). The basal secretion of IL-8 by Caco-2 cells without bacterial infection was 7.90 ± 1.23 pg ml−1.
Suppression of NF-κB activation
The nuclear factor, NF-κB, and its signal transduction pathway can be activated by bacterial infection [40], and is involved in IL-8 production [41] and colon cancer [42]. Treatment of E. coli with 5-ASA inhibited the activation of NF-κB (p < 0.05) in HEK-Blue KD-TLR5 cells by all but 2 strains—the pks-negative cancer strains, HM288 and HM358 (Fig. 3c). For 9/11 strains, 5-ASA treatment inhibited NF-κB activation by 35–75% relative to untreated controls (− 5-ASA). Activation of NF-ĸB was undetectable in the absence of bacteria.
Promotion of PPARγ gene expression
PPARγ is a transcriptional factor that promotes anti-inflammatory responses of intestinal epithelial cells and macrophages. Gene expression of PPARγ was upregulated by 5-ASA treatment of Caco-2 cells (p < 0.01, Fig. 3d and Supplementary Data Table S1). In contrast, LF82 infection inhibited PPARγ gene expression in Caco-2 cells more than 2 fold (p < 0.01). However, pretreatment of LF82, Caco-2, or both with 5-ASA before infection reduced the suppression of PPARγ expression by LF82 (p < 0.01, Supplementary Data Table S1).
5-ASA inhibits intracellular survival and proinflammatory responses of E. coli-infected macrophages
Inhibition of E. coli survival in macrophages
Granuloma formation is considered a hallmark of CD, and E. coli DNA has been identified in resected granulomas [43]. The ability of CD-associated E. coli, mainly AIEC, to replicate in macrophages implicates them in the inflammatory response and elaboration of TNF-α. Therefore, we examined the effect of 5-ASA on E. coli survival in J774 A.1 macrophages. As expected, the non-AIEC control E. coli T75 (see Table 1) survived poorly (<50%) in J774 A.1 in the absence of 5-ASA treatment (Fig. 4a). In contrast, the other 10 E. coli strains had survival rates greater than 100% (indicating replication within J774A.1 cells) without 5-ASA treatment (Fig. 4a). Nevertheless, 5-ASA reduced the intracellular survival (p < 0.01) of 5/6 CD-associated AIEC and 1/4 CRC-E. coli in macrophages (Fig. 4a).
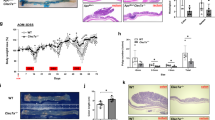
5-ASA reduces E. coli survival and alters TNF-α production in infected J774A.1 cells. J774A.1 macrophages were infected with E. coli grown in LB broth with either DMSO or 5-ASA (1 mg ml−1) overnight at 37 °C. Intracellular bacteria were determined at 1 and 24 h post infection. Spent media at 24 h post infection was used for TNF-α quantification. *p < 0.05; **p < 0.01. Error bar = SD. a Relative E. coli survival in J774A.1 macrophages (three replicates); b TNF-α secretion (four replicates); c Relative TNF-α expression (three replicates). In (c), the lowercase letters (above each column) represent the significance between treatments: same letters indicate no difference (p > 0.05); different letters indicate significant difference (p < 0.01; see Supplementary Data Table S1); “J774A.1 control” column shows the relative expression level of TNF-α in the absence of 5-ASA and bacterial infection; the pre-treatments are shown in the parentheses along the x-axis
Reduction of TNF-α secretion and transcription
TNF-α is the prototypical cytokine of CD and antibody blockade can induce remission [44]. 5-ASA treatment of E. coli reduced TNF-α production by J774A.1 cells by 20–30% when infected with 5/6 CD-associated AIEC and one (HM288) of the two pks-negative CRC-associated E. coli strains at 24 h post infection (p < 0.05; Fig. 4b). In contrast, 5-ASA stimulated TNF-α production (by 30%; p < 0.01,) by J774A.1 cells infected with the two pks-positive CRC-associated E. coli strains, NC101 and HM334, under the same conditions (Fig. 4b). The basal secretion of TNF-α was 0.041 ± 0.013 ng ml−1 in the absence of bacterial infection. The transcriptional level of TNF-α in J774A.1 cells decreased more than 2 fold after 5-ASA treatment (p < 0.01; Fig. 4c), but increased ~30-fold after LF82 infection (p < 0.01). Pretreatment of LF82, J774A.1, or both, with 5-ASA before infection dramatically reduced TNF-α gene expression (>100-fold; p < 0.01) (Fig. 4c and Supplementary Data Table S1).
5-ASA inhibits genotoxicity of CRC-E. coli
Treatment of E. coli with 5-ASA downregulated pks gene transcription in all pks-positive CRC-associated E. coli strains (Table 3). Colibactin, a product of the pks island, plays a crucial role in the genotoxicity of E. coli [45]. We therefore employed the comet assay to investigate the effect of 5-ASA treatment of pks-positive E. coli on DNA breakage in the colonic epithelial Caco-2 cells (Fig. 5a). E. coli treated with 5-ASA caused less DNA damage in the infected Caco-2 cells than untreated controls, e.g., 14% (at 2 mg ml−1 5-ASA) vs 34% (Control) for NC101 (p < 0.01), 38 (at 2 mg ml−1 5-ASA) vs 50% (Control) for HM334 (p < 0.01; Fig. 5b). As a control strain, HM288 (pks-negative) did not cause any DNA damage (data not shown).
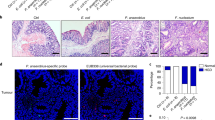
5-ASA inhibits E. coli-induced DNA damage in Caco-2 cells. The pks-positive strains NC101 and HM334 were treated with either DMSO or 5-ASA at concentrations of 1.5 or 2 mg ml−1 for 17 h before infection of Caco-2 cells at an m. o. i. of 20. At 3 h post infection (see Methods), about 500 Caco-2 cells (infected and un-infected) were mixed with low-melting agarose pre-warmed at 40 °C, and transferred on to a Comet slide. After electrophoresis, the genomic DNA was stained with SYBR green, visualized and quantified under UV light. The data were from one of three independent experiments. a Comet cell images (arrow showing one of the comets). b Comet formation, which is expressed as a percentage of total cells counted (200–250 cells). **p < 0.01, ns not significant, Error bar = SD
Discussion
5-ASA has been used as a primary treatment of IBD [1] for over 60 years and is the mainstay of therapy to induce and maintain remission in patients with mild to moderate UC [2]. 5-ASA can also prevent or inhibit the development of colorectal cancer in patients with UC [3, 4]. The mechanisms behind the beneficial effects of 5-ASA are poorly understood, and precede the implication of intestinal dysbiosis and pathosymbiont E.coli in the etiopathogenesis of IBD and CRC. To explore the possibility that the clinical benefits of 5-ASA may due to its action on both E.coli and the host, we examined the effect of 5-ASA on the growth and virulence of E. coli associated with IBD and non-IBD CRC, and its impact on host cell inflammatory responses. Our findings reveal substantial and pleiotropic antimicrobial activity of 5-ASA against IBD- and CRC-associated E. coli.
At concentrations (≥1 mg ml−1 = ≥ 6.5 mM) that parallel the intraluminal concentrations of 5-ASA in IBD patients (1 to 100 mM) [24, 37], 5-ASA consistently inhibited the growth of CD- and CRC-associated E. coli in vitro. These findings support the possibility that 5-ASA could inhibit E. coli proliferation and consequently abrogate dysbiosis in patients with IBD and non-IBD CRC. Concomitantly, 5-ASA reduced the growth of non-AIEC T75. Although this could hamper the beneficial effects of symbiont E.coli, the ability of 5-ASA to temper the proinflammatory and pro-oncogenic effects of dysbiotic opportunistic pathosymbiotic AIEC likely outweighs any negative impact on commensal E. coli.
We demonstrated that 5-ASA downregulated the transcription of a broad range of virulence genes in 80% of E. coli strains evaluated. Reduced transcription correlated with reduced virulence in functional assays. For example, reduced transcription of fliC by 5-ASA was associated with decreased E. coli motility. Similarly, downregulation of fimH, yfgL, ompC, and nlpL in E. coli treated with 5-ASA was associated with reduced adhesion and invasion of intestinal epithelial cells, and IL-8 secretion. In addition, 5-ASA also downregulated stress-related genes (dsbA and htrA) and the secretion of TNF-α induced by the persistence of E. coli in macrophages [46]. As bacterial motility, adhesion, invasion, intracellular survival, and cytokine elaboration are central to the virulence of CD- and CRC-associated E. coli, our findings raise the possibility that the ability of 5-ASA to impact these traits of E. coli may be related to its clinical effects in patients with IBD, and could be beneficial for treating non-IBD CRC.
Colibactin induces inflammation-associated CRC in mice [22] and in sporadic CRC [47]. In this report we show for the first time that 5-ASA treatment reduced the expression of the pks gene, and inhibits DNA damage caused by pks-positive CRC-E. coli in colonic epithelial cells (Caco-2). How these 5-ASA-associated changes impact the expression or effects of colibactin, or whether the protective effect of 5-ASA is reproduced in vivo remains to be determined.
IL-8 and TNF-α are proinflammatory cytokines that are upregulated in IBD and CRC [48, 49], and in part by the NF-ĸB pathway [50]. Our observations that 5-ASA decreases CD- and CRC-E. coli-induced-activation of NF-ĸB, the secretion of IL-8 by Caco-2 epithelial cells, and TNF-α by J774A.1 support the concept that 5-ASA may inhibit proinflammatory host-bacterial interactions implicated in the pathogenesis of IBD and CRC in vivo.
In contrast to other E. coli strains, the two pks-positive CRC-associated E. coli strains (NC101 and HM334) increased TNF-α production after 5-ASA treatment. Kaiser et al. [51] reported that at low concentrations (0.006–0.06 nM), TNF-α promotes intestinal epithelial cell growth, while at high concentrations (6–60 nM) it inhibits epithelial cell growth through different receptor activation. Thus 5-ASA treatment of pks-positive E. coli might exert a dual chemo-protective function, reducing pks gene expression and genotoxicity, while inhibiting epithelial cell growth by stimulating TNF-α production.
PPARγ belongs to a family of nuclear receptors. Studies have shown that PPARγ functions as an endogenous regulator of anti-inflammation in murine intestine [52, 53]. Rousseaux et al. [10] speculated that PPARγ mediates the therapeutic action of 5-ASA. Our finding of increased PPARγ gene transcription in 5-ASA-treated Caco-2 cells supports this concept. Moreover, pretreatment of E. coli LF82 with 5-ASA partially neutralized the depression of PPAR-γ gene expression in Caco-2 cells induced by LF82 infection. This suggests a dual activity of 5-ASA to up-regulate host anti-inflammatory responses to infection while down-regulating E. coli virulence.
In conclusion, our data reveal multifaceted and previously unrecognized effects of 5-ASA on growth and virulence of CD- and CRC-associated E. coli and their interactions with cultured host cells in vitro. We hope these findings will inform future studies directed at further elucidating the anti-inflammatory and antibacterial activity of 5-ASA in patients with IBD and CRC.
References
Abdu-Allah HH, El Shorbagi A-NA, Abdel-Moty SG, El-Awady R, M Abdel-Alim A-A., 5-Aminosalyclic Acid (5-ASA): a unique anti-inflammatory salicylate. Med Chem. 2016;6:306–15.
Nielsen OH, Munck LK. Drug insight: aminosalicylates for the treatment of IBD. Nat Clin Pract Gastroenterol Hepatol. 2007;4:160–70.
Rubin DT, et al. Colorectal cancer prevention in inflammatory bowel disease and the role of 5-aminosalicylic acid: a clinical review and update. Inflamm Bowel Dis. 2008;14:265–74.
Ikeda I, et al. 5-Aminosalicylic acid given in the remission stage of colitis suppresses colitis-associated cancer in a mouse colitis model. Clin Cancer Res. 2007;13:6527–31.
Punchard NA, Greenfield SM, Thompson RP. Mechanism of action of 5-arninosalicylic acid. Mediat Inflamm. 1992;1:151–65.
Rachmilewitz D, Karmeli F, Schwartz LW, Simon PL. Effect of aminophenols (5-ASA and 4-ASA) on colonic interleukin-1 generation. Gut. 1992;33:929–32.
Kaiser GC, Yan F, Polk DB. Mesalamine blocks tumor necrosis factor growth inhibition and nuclear factor kappaB activation in mouse colonocytes. Gastroenterol . 1999;116:602–9.
Egan LJ, et al. Inhibition of interleukin-1-stimulated NF-ĸb RelA/p65 phosphorylation by mesalamine is accompanied by decreased transcriptional activity. J Biol Chem. 1999;274:26448–53.
Dammann K, et al. PAK1 modulates a PPARγ/NF-ĸB cascade in intestinal inflammation. Biochim Biophys Acta. 2015;1853:2349–60.
Rousseaux C, et al. Intestinal antiinflammatory effect of 5-aminosalicylic acid is dependent on peroxisome proliferator-activated receptor-gamma. J Exp Med. 2005;201:1205–15.
Annese V, Rogai F, Settesoldi A, Bagnoli S. PPARγ in inflammatory bowel disease. PPAR Res. 2012;620839:9.
Vindigni SM, Zisman TL, Suskind DL, Damman CJ. The intestinal microbiome, barrier function, and immune system in inflammatory bowel disease: a tripartite pathophysiological circuit with implications for new therapeutic directions. Ther Adv Gastroenterol. 2016;9:606–25.
Chu H, et al. Gene-microbiota interactions contribute to the pathogenesis of inflammatory bowel disease. Sci. 2016;352:1116–20.
Sartor RB, Mazmanian SK. Intestinal microbes in inflammatory bowel diseases. Am J Gastroenterol Suppl. 2012;1:15–21.
Gagnière J, et al. Gut microbiota imbalance and colorectal cancer. World J Gastroenterol. 2016;22:501–18.
Arthur JC, et al. Microbial genomic analysis reveals the essential role of inflammation in bacteria-induced colorectal cancer. Nat Commun. 2014;5:4724.
Baumgart M, et al. Culture independent analysis of ileal mucosa reveals a selective increase in invasive Escherichia coli of novel phylogeny relative to depletion of Clostridiales in Crohn’s disease involving the ileum. ISME J. 2007;1:403–18.
Darfeuille-Michaud A, et al. High prevalence of adherent-invasive Escherichia coli associated with ileal mucosa in Crohn’s disease. Gastroenterol. 2004;127:412–21.
Simpson KW, et al. Adherent and invasive Escherichia coli is associated with granulomatous colitis in Boxer dogs. Infect Immun. 2006;74:4778–92.
Martin HM, et al. Enhanced Escherichia coli adherence and invasion in Crohn’s disease and colon cancer. Gastroenterol. 2004;127:80–93.
Khan AA, et al. Colorectal cancer-inflammatory bowel disease nexus and felony of Escherichia coli. Life Sci. 2017;180:60–7.
Arthur JC, et al. Intestinal inflammation targets cancer-inducing activity of the microbiota. Sci . 2012;338:120–3.
Cuevas-Ramos G, et al. Escherichia coli induces DNA damage in vivo and triggers genomic instability in mammalian cells. Proc Natl Acad Sci USA. 2010;107:11537–42.
Kaufman J, Griffiths TA, Surette MG, Ness S, Rioux KP. Effects of mesalamine (5-Aminosalicylic Acid) on bacterial gene expression. Inflamm Bowel Dis. 2009;15:985–96.
Greenstein RJ, Su L, Shahidi A, Brown ST. On the Action of 5-Amino-Salicylic Acid and Sulfapyridine on M. avium including Subspecies paratuberculosis. PLoS ONE. 2007;2:e516.
Swidsinski A, Weber J, Loening-baucke V, Hale LP, Lochs H. Spatial organization and composition of the mucosal flora in patients with inflammatory bowel disease. J Clin Microbiol. 2005;43:3380–9.
Kothary V, et al. Rifaximin resistance in Escherichia coli associated with inflammatory bowel disease correlates with prior rifaximin use, mutations in rpoB, and activity of Phe-Arg-β-Naphthylamide-inhibitable efflux pumps. Antimicrob Agents Chemother. 2013;57:811–7.
Kim SC, et al. Variable phenotypes of enterocolitis in interleukin 10-deficient mice monoassociated with two different commensal bacteria. Gastroenterol . 2005;128:891–906.
He Y, Xu T, Fossheim LE, Zhang XH. FliC, a Flagellin protein, is essential for the growth and virulence of fish pathogen Edwardsiella tarda. PLoS ONE. 2012;7:1–7.
Dogan B, et al. Inflammation-associated adherent-invasive Escherichia coli are enriched in pathways for use of propanediol and iron and M-cell translocation. Inflamm Bowel Dis. 2014;20:1919–32.
Bringer M-AA, Rolhion N, Glasser A-LL, Darfeuille-Michaud A. The oxidoreductase DsbA plays a key role in the ability of the Crohn’s disease-associated adherent-invasive Escherichia coli strain LF82 to resist macrophage killing. J Bacteriol. 2007;189:4860–71.
Bringer MA, Barnich N, Glasser AL, Bardot O, Darfeuille-Michaud A. HtrA stress protein is involved in intramacrophagic replication of adherent and invasive Escherichia coli strain LF82 isolated from a patient with Crohn’s disease. Infect Immun. 2005;73:712–21.
Rolhion N, Carvalho FA, Darfeuille-Michaud A. OmpC and the sigma(E) regulatory pathway are involved in adhesion and invasion of the Crohn’s disease-associated Escherichia coli strain LF82. Mol Microbiol. 2007;63:1684–700.
Barnich N, Bringer MA, Claret L, Daffeuille-Michaud A. Involvement of Lipoprotein NlpI in the virulence of adherent invasive Escherichia coli strain LF82 isolated from a patient with Crohn’s disease. Infect Immun. 2004;72:2484–93.
Barnich N, Boudeau J, Claret L, Darfeuille-Michaud A. Regulatory and functional co-operation of flagella and type 1 pill in adhesive and invasive abilities of AIEC strain LF82 isolated from a patient with Crohn’s disease. Mol Microbiol. 2003;48:781–94.
Prorok-Hamon M, et al. Colonic mucosa-associated diffusely adherent afaC + Escherichia coli expressing lpfA and pks are increased in inflammatory bowel disease and colon cancer. Gut. 2014;63:761–70.
Frieri G, et al. Mucosal 5-aminosalicylic acid concentration inversely correlates with severity of colonic inflammation in patients with ulcerative colitis. Gut. 2000;47:410–4.
Lane MC, et al. Role of motility in the colonization of uropathogenic Escherichia coli in the urinary tract. Infect Immun. 2005;73:7644–56.
Jung HC, et al. A distinct array of proinflammatory cytokines is expressed in human colon epithelial cells in response to bacterial invasion. J Clin Invest. 1995;95:55–65.
Lawrence T. The nuclear factor NF-kappaB pathway in inflammation. Cold Spring Harb Perspect Biol. 2009;1:a001651.
Khanjani S, Terzidou V, Johnson MR, Bennett PR. NF-ĸB and AP-1 drive human myometrial IL8 expression. Mediat Inflamm. 2012;2012:504952.
Wang S, Liu Z, Wang L, Zhang X. NF-kappaB signaling pathway, inflammation and colorectal cancer. Cell Mol Immunol. 2009;6:327–34.
Ryan P, et al. Bacterial DNA within granulomas of patients with Crohn’s disease–detection by laser capture microdissection and PCR. Am J Gastroenterol. 2004;99:1539–43.
Deventer SJHVAN. Immunotherapy of Crohn’ s Disease. Scand J Immunol. 2000;51:18–22.
Healy AR, Nikolayevskiy H, Patel JR, Crawford JM, Herzon SB. A mechanistic model for colibactin-induced genotoxicity. J Am Chem Soc. 2016;138:15563–70.
Rahman K, Sasaki M, Nusrat A, Klapproth JMA. Crohn’s disease-associated Escherichia coli survive in macrophages by suppressing NFκB signaling. Inflamm Bowel Dis. 2014;20:1419–25.
Buc E, et al. High prevalence of mucosa-associated E. coli producing cyclomodulin and genotoxin in colon cancer. PLoS ONE. 2013;8:e56964.
Subramanian S, et al. Characterization of epithelial IL-8 response to inflammatory bowel disease mucosal E. coli and its inhibition by mesalamine. Inflamm Bowel Dis. 2008;14:162–75.
Sethi G, Sung B, Aggarwal BB. TNF: a master switch for inflammation to cancer. Front Biosci. 2008;13:5094–107.
Tak PP, Firestein GS, Tak PP, Firestein GS. NF-kappaB: a key role in inflammatory diseases. J Clin Invest. 2001;107:7–11.
Kaiser GC, Polk DB. Tumor necrosis factor alpha regulates proliferation in a mouse intestinal cell line. Gastroenterol. 1997;112:1231–40.
Nakajima A, et al. Endogenous PPAR gamma mediates anti-inflammatory activity in murine ischemia-reperfusion injury. Gastroenterol. 2001;120:460–9.
Straus DS, Glass CK. Anti-inflammatory actions of PPAR ligands: new insights on cellular and molecular mechanisms. Trends Immun. 2007;28:551–8.
Acknowledgements
We are grateful for the support of Jill Roberts and Jill Roberts Center for IBD, Weill Cornell Medicine, New York, NY 10021, USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Zhang, S., Fu, J., Dogan, B. et al. 5-Aminosalicylic acid downregulates the growth and virulence of Escherichia coli associated with IBD and colorectal cancer, and upregulates host anti-inflammatory activity. J Antibiot 71, 950–961 (2018). https://doi.org/10.1038/s41429-018-0081-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41429-018-0081-8
This article is cited by
-
Anticolitic activity of prodigiosin loaded with selenium nanoparticles on acetic acid–induced colitis in rats
Environmental Science and Pollution Research (2022)
-
Ostarine attenuates pyocyanin in Pseudomonas aeruginosa by interfering with quorum sensing systems
The Journal of Antibiotics (2021)
-
Integrating omics for a better understanding of Inflammatory Bowel Disease: a step towards personalized medicine
Journal of Translational Medicine (2019)