Abstract
Acute lymphoblastic leukemia (ALL) is a cancer-specific lymphoid cell. Induction and consolidation chemotherapy alone or in combination with different therapeutic approaches remain the main treatment. Although complete or partial remission of the disease can be achieved, the risk of relapse or refractory leukemia is still high. More effective and safe therapy options are yet unmet needs. In recent years’ new therapeutic approaches have been widely used. Hematopoietic Stem Cell Transplantation (HSCT) presents significant limitations and the outcome of the consolidation treatment is patient dependent. Side effects such as Graft versus Host Disease (GvHD) in allogeneic hematopoietic stem cell transplantation are extremely common, therefore, using alternative methods to address these challenges for treatment seems crucial. In the last decade, T cells genetically engineered with Chimeric Antigen Receptor (CAR) treatment for the ALL are largely studied and represent the new era of strategy. According to the Phase I/II clinical trials, this technology results seem very promising and can be used in the next future as an effective and safe treatment for ALL treatment. In this review different generations, challenges, and clinical studies related to chimeric antigen receptor (CAR) T-cells for ALL treatment are discussed.
Similar content being viewed by others
Introduction
Acute lymphoblastic leukemia (ALL) or lymphocytic leukemia, is progressive cancer in children and adults. Lymphoid progenitor cells in the bone marrow, blood, and extra-medullary sites undergo malignant transformation and proliferation. The majority of ALL cases are classified as precursor B-cell type, but the T-cell neoplasm is a rare and extremely aggressive phenotype and is slightly more common in adults than in children [1]. According to the American Cancer Society, the estimated number of new cases in the United States (USA) in 2021 is 5,690 including both children and adults. Among all cases, 80% occurs in children and young adults [2].
The treatment for ALL consists of three phases: remission induction, consolidation, and long-term maintenance, with central nervous system (CNS) prophylaxis given at intervals throughout treatment. The frontline of treatment for induction therapy is the standard chemotherapy. Targeted drug therapy can be used alone or in combination with chemotherapy for all three phases [3].
Induction therapy aims to destroy the leukemia cells (blast). Complete remission is achieved when there is no sign of leukemia cells in the blood and the bone marrow after the treatment and normal hematopoiesis is restored. In the consolidation phase, the treatment is intensified and lasts for several months to reduce the number of leukemia cells still in the body and to avert the relapse of the disease [3, 4].
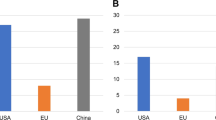
Several chemo-drugs developed over the past 40 years are combined to prevent the resistance, indeed the 5-year survival rates in children and adolescents up to 19 years was only 10% in the 1960s, but increased to 80–90% at present. Approximately 2–3% of patients are refractory to induction chemotherapy, and 10–15% experience relapse [1, 5, 6]. In contrast, the 5 years survival rate in adult ALL in the United States is 68.6 percent, reports the NCI (National Cancer Institute), and about 40% in Europe. Despite 80–90% of the adult patients’ response to induction chemotherapy, only 30–40% of adult patients will achieve long-term remission [3, 4, 7].
ALL is a highly heterogeneous disease, although cases can be stratified into a favorable, intermediate, and adverse-risk group based on the genetic profile that encompasses recurrent chromosomal aberrations as well as a mutation in the genes involved in hematopoietic proliferation and differentiation. Cytogenetics at the time of diagnosis is the single most important prognostic factor for patients treated upfront with chemotherapy regimens alone, and to make decisions regarding the use of allogeneic hematopoietic stem cell transplantation (HSCT) as consolidation therapy [8,9,10]. HSCT may provide some major complications such as complexity and graft versus host disease (GVHD) [11].
One of the significant obstacles to the cure of acute leukemia is its propensity to relapse after chemotherapy or hematopoietic stem-cell transplantation (HSCT). As a result, scientists pursued novel efficient treatments free of these issues. Many of the approaches are currently being evaluated for ALL salvage and improvements in the therapy of adult ALL are highly encouraging. Targeted agents, such as Imatinib mesylate, a specific tyrosine kinase inhibitor of BCR-ABL, in children with Philadelphia chromosome-positive ALL, have been shown to improve survival when they are combined with conventional chemotherapy in a consolidation phase [12, 13].
In the past decade, immunotherapies involving endogenous T cells have emerged as a new strategy to treat r/r ALL and avoid chemotherapy resistance [14]. The rationale for immunotherapy in ALL is supported by evidence for immune surveillance in the development of leukemia [15].
Chimeric antigen receptor (CAR) T-cells are genetically modified polyclonal T or natural killer (NK) cells with fusion proteins to guide them toward a given molecule in the tumor cell surface. CAR T-cell components include an extracellular antigen recognition domain of the single-chain Fragment variant (scFv) derived from an antibody, a transmembrane domain, and an intracellular signaling domain. Targeting moiety is presented in native form without the need for additional processing within the groove MHC molecules. So, CAR T-cells identify target tumor cells regardless of a patient’s MHC haplotype.
The use of ligand or peptide to target the CAR-T is an area of development. The roles of monoclonal antibodies, chimeric CAR‐T‐cell therapies, and other novel targeted approaches in adult ALL continue to be defined [3]. Their incorporation into frontline adult ALL therapy, in concomitant or sequential strategies, may increase the cure rates to levels achieved in pediatric ALL and may reduce the need for prolonged intensive and maintenance chemotherapy.
In this review article, we discuss CAR T-cell therapies against ALL, focusing on the target antigens used for CAR design, the difference in CAR generations, CAR T-cell clinical trials and FDA-approved, challenges in CAR T-cell therapies, and the latest overcoming strategies.
CAR T-cell generations
Adoptive cell therapies (ACTs) have been used to treat cancer for over 30 years. The rationale that led to the chimeric antigen receptor-modified T (CAR T)-cells was to overcome the HLA restriction, the effective presentation of target epitopes, and the lack of a broad TCR gene repertoire [16].
CAR T-cells have been investigated in preclinical and clinical studies. In hematological malignancies, the efficacy in targeting cancer encompasses also the complete and long-lasting durable clinical response observed in late-stage chemotherapy-resistant leukemias and lymphomas. Conversely, in solid tumors treatment, the efficacy is yet unmet, and further study is still needed [17,18,19,20].
Chimeric antigen receptors (CARs) have a modular design consisting of an ectodomain, a hinge, a transmembrane domain (TDM), and an intracellular signaling domain. The ectodomain is a signal peptide, an extracellular MHC-independent antigen-binding domain derived from a monoclonal antibody, a single-chain Fragment variant (scFv) formed by the variable portions of heavy and light chains of an immunoglobulin. A spacer lends flexibility and connects the ectodomain to the transmembrane domain (Figs. 1, 2A) [21, 22].
A CAR molecule comprises an extracellular MHC-independent antigen-binding ectodomain derived from a monoclonal antibody, including a single-chain variable fragment (scFV), a linker, and a spacer/hinge region, a transmembrane domain, and an intracellular T cell signaling endodomain counting CD3ζ and costimulatory domains.
CAR T cells can be categorized into four generations, based on domains used in their designs and the CAR structures. (A) In the first generation of CARs, there was only one intracellular signal component CD3ζ. (B & C) The second generation and third generation added costimulatory molecules, one and more than one respectively. (D) In the fourth-generation CAR T cells, the recognition of target antigens leads to the induction of cytokine production through the activation of downstream factors.
The majority of CAR T cells are designed with immunoglobulin (Ig)-like domain hinges derived from IgG. Long spacers provide extra flexibility to the CAR and allow for better access to membrane-proximal epitopes or complex glycosylated antigens. By contrast, CARs with shorter hinges, including an IgG-derived hinge lacking the CH2-CH3 regions, or hinges derived from native CD28 and CD8 hinges, can be used to target membrane-distal epitopes [23,24,25,26,27,28,29].
The transmembrane domain consists of a hydrophobic α-helix that spans the cell membrane mainly derived from CD4, CD8α, or CD28 which confer the stability of the receptor. Further studies have been demonstrated that linking the proximal domain to its corresponding transmembrane domain may enable proper CAR T cell signaling [21, 23]. The intracellular domain of the TCR-CD3 complex transduces the signal in the activation cascade.
According to the structure of the endodomain, based on the number of the costimulatory domain used, CAR T generation passed through four different generations. The first generation used CD3 ζ alone but the administration of cytokines such as interleukin-2 was necessary to increase in vivo tumor rejection. [30, 31].
Afterward, an effort has been invested in understanding the effects of CAR co-stimulation. Additional signals to the engineering T cell can provide the improvement in T-cell effector function and reduce T cell exhaustion.
Studies in mouse tumor models showed that the incorporation of the CD28 or CD137 (4–1BB) signaling domains enhances the antitumor activity and in vivo persistence of chimeric antigen receptors as compared with the inclusion of the CD3 zeta chain alone. These findings are relevant in the context of poorly immunogenic tumors [32]. T cells expressing CARs with CD28/CD3ζ or 4–1BB/CD3ζ signaling domains exhibit differences in effector function, clinical efficacy, and toxicity that are assumed to result from the activation of divergent signaling cascades [33]. Milone et al. demonstrated that CD137 has superior antileukemic efficacy and improved persistence in a primary human acute lymphoblastic leukemia xenograft model and the activity appears to be antigen-independent [34].
In the second generation, an intracellular domain such as CD28 or (CD137) 4–1BB and (CD134) OX40 was added to the cytoplasmic tail of first-generation CARs to overcome the weakening of the T cell proliferation in vitro and its long-term survival after reinfusion (Fig. 2B) [35]. 4–1BB-based CARs have resulted in greater long-term persistence whereas CD28 costimulatory domains resulted in proliferation, survival, and establishment of effector and memory cells and showed faster and higher intensities of phosphorylation, indicating higher signal strengths [27].
CD134 and CD137 elicit T cell proliferation and can play a key role in IL-2 production, survival of T cells, and their perseverance [36].
Most CARs derived from second-generation constructs were used in clinical trials of T cells genetically engineered to express CD19 for patients with B-ALL. Successful second-generation CARs for B-ALL treatment were designed by the University of Pennsylvania (UPenn), the Memorial Sloan Kettering Cancer Center (MSKCC), and National Cancer Institute (NCI) containing scFv, transmembrane, either CD28 or 4–1BB and CD3ζ (Fig. 3) [37,38,39,40,41,42,43,44,45,46,47].
A At Memorial Sloan KetteringCancer Center and B National Cancer Institute, patients have been treated with a CD28ζ second-generation CAR. Respectively, A 19–28ζ and B FMC63–28ζ constructs were introduced into T cells by retroviral transduction. C Instead, at the University of Pennsylvania, a 4–1BBζ containing a second-generation CD19-targeted CAR T, was introduced by a lentiviral vector. Moreover, the single-chain variable fragment (scFv) was the difference between the A (SJ scFv) group and the B and C groups (FMC63 scFv).
The third generation of CARs was designed to imitate the natural physiology condition and activation of these immune cells by the integration of multiple costimulatory signaling domains, such as CD28, CD137 (4–1BB), ICOS, or CD134 (OX40), into the CD3 zeta domain (Fig. 2C).
At last, CAR T-cells redirected for universal cytokine killing (TRUCKs) are known as the fourth generation of CARs (Fig. 2D). This generation produces IL-12 or IFN-γ and some other cytokines; this strategy could overcome any antigen loss within the cancer cells as a result could induce the immune system to encounter the cancer cells [48]. It is noteworthy that the third and fourth-generation CARs are still in development and not yet approved along with the allogeneic CAR-T [49].
CAR-T cell manufacturing
The workflow of the CAR-T cells manufacturing includes isolation of donor T cells, followed by efficient activation, gene transfer of the CAR construct, CAR-T cells expansion, phenotyping, and quality check analysis. (Fig. 4). Leukocytes are taken from patients (autologous) or healthy donor (allogeneic) peripheral blood mononuclear cells (PBMCs). Although most clinical studies use autologous CAR T-cells for B-ALL treatment, the administration of allogeneic CAR T-cells has been also reported in a small and limited numbers clinical study [50]. Several different subsets of leukocytes are used in clinical trials such as CD3 + T cells, central memory cells, naïve cells, and memory stem cells. T cells subsets are separated using specific antibodies followed by the activation process by purifying autologous antigen-presenting cells (APCs) from the patients or donors, or beads coated with anti-CD3/anti-CD28 monoclonal antibodies, or anti-CD3 antibodies alone or in combination with feeder cells and growth factors, such as IL-2.
A After extracting autologous T cells from the peripheral blood of the patient, CAR genes are introduced into T cells to manufacture CAR T cells, which are then widely extended in vitro and infused into the patient. B After extracting allogeneic T cells from the peripheral blood of a healthy donor, CAR genes are introduced into T cells to manufacture Universal CAR (UCAR) T cells, which are then widely extended in vitro and administered to the patients.
Lentiviral and retroviral vectors have been widely used in basic research due to the high transfer efficiency and afterward applied for the design and construction of CARs to treat ALL cancers. Because of their safer integration site profile and the ability to infect non-dividing and quiescent cells, lentiviral vectors are more commonly used than γ-retroviral vectors in clinical trials. Lentiviral integration patterns occur far away from the transcriptional sites resulting in a lower risk of mutagenesis [51, 52]. At multiple stages throughout the vector manufacturing process to be used in the clinic, the product is narrowly tested for the presence of replication-competent retrovirus/lentivirus (RCRs/RCLs) to ward off the possibility to be oncogenic as per FDA 2006 guidance. FDA also mandated a long follow-up for RCLs up to 15 years in patients treated for monitoring any potential delayed adverse event using integrating vectors [51, 52].
As we previously described, in the CAR T cell studies, various domains have been used within each of the segments. The antigen-binding domain and the costimulatory domain have been manipulated more than other segments resulting in more variations across the various construct used in the clinic. CAR T-cell therapy constructs against B-cell acute lymphoblastic leukemia include 19–28Z (CD3ζ chain and CD28 co-signaling domain), 19-BBZ (costimulatory 4–1BB and CD3ζ domains and anti-CD19 scFv), TSLPR-BBZ or TSLPR-Z (CD3 zeta intracellular domain, a 4–1BB co-signaling domain, a CD8 TMD, and the scFvs for TSLPR targeting), M971-BBZ or M971–28Z (m971 anti-CD22 monoclonal antibody) [37, 38, 47, 50, 53,54,55,56,57,58,59,60,61]. Other methods include Sleeping Beauty transposon system and mRNA transfection. The general scheme in clinical trials is similar, however, the methods used are various. The validation requirements are in terms of T cell expansion, T cell transduction, biological activity, quality control testing, and release criteria [21].
Three clinical trials designed to assess the safety and feasibility of CTL019 T cell therapy in relapsed/refractory CD19 + malignancies were conducted at the Children’s Hospital of Philadelphia (CHOP) (Pediatric cohort, Clinicaltrials.gov: NCT01626495) and the Hospital of the University of Pennsylvania (PENN) (Adult cohort, NCT02030847, and NCT01029366).
A phase I/IIa clinical trial performed at the UPenn and children’s hospital of Philadelphia (CHOP) employed a lentiviral engineered autologous T-cell construct expressing a second-generation CAR composed of anti-CD19 scFv, CD3ζ as a signaling domain, and 4–1BB as the costimulatory domain [34]. Indeed, the efficacy in re-inducing remission in patients with multiply relapsed B-ALL is remarkable, demonstrating that the second costimulatory signals have been necessary to achieve relevant T-cell expansion and longer-term persistence in vivo [38, 62, 63].
At Memorial Sloan Kettering Cancer Center [37], and at National Cancer Institute [46] instead, patients received CD28ζ second-generation CAR T cells genetically modified with a replication-defective gammaretroviral vector derived from the Moloney murine leukemia virus. The differences between these cancer centers relied also on the single-chain variable fragment (scFv) as depicted in Fig. 3.
Target antigens
Several target antigens have been investigated for CAR T-cell therapy in both preclinical and clinical trials. Ideal target antigens for CAR-T cells are homogeneously expressed within tumors, but not on normal tissues, which could cause toxicity by CAR-T cells. Those biomarkers are expressed at different levels on the surface of ALL cells that include the thymic stromal lymphopoietin receptor (TSLPR), CD19, CD22, CD20.
In the case of B-cell malignancies, CD19 expressed throughout B-cell development, was chosen as an acceptable target even if it’s not a tumor-specific antigen, due to its high expression on most malignant B cells, while at the same time lacking expression on hematopoietic stem cells, limiting the risk of aplastic anemia [47].
B-cell aplasia is an on-target/off-tumor effect associated with hypogammaglobulinemia a defect in humoral immunity that can last months to years after treatment, experience recurrent upper and lowers respiratory infections, and result in immunoglobulin G replacement [35, 50, 64,65,66,67].
The combination of multi-antigen targeting may increase the effectiveness of this therapeutic approach. The different therapies at the present encompass pooled CAR-T cells, dual CAR-T cells, tandem CAR-T cells, and trivalent CAR T-cells. To prevent tumor antigen escape and to alleviate on-target, off-tumor toxicities, the Boolean logic gates of “AND”, “OR”, and “NOT” have been applied to gate the activity of multi-antigen targeted CAR-T cells. In detail: “AND” logic-gated can be activated in the presence of both antigens simultaneously, “OR” logic gate in the presence of either targeted antigen, finally “NOT” logic gate to avoid the off-target effect [68].
CD20 is expressed on a variety of lymphoid malignancies as a B-cell-specific antigen. CD20-based CAR T-cell cancer therapy has shown high efficacy alone or in combination with CD19 in vitro and in vivo animal models of ALL and CLL [69, 70].
Thymic stromal lymphopoietin (TSLP) is a biological agent similar to IL-7, which could play an important role in hematopoietic cell maturation and pediatric acute lymphoblastic leukemia stimulation [71, 72]. The cognate receptor TSLPR is encoded by cytokine receptor-like factor 2 (CRLF2) gene in a B-ALL cell with a CRLF2 rearrangement. Overexpression of TSLPR is reported in 15% of patients without typical chromosomal rearrangements [73] and is associated with a higher risk for disease relapse. This observation suggests that TSLPR is a novel and attractive candidate for CAR T-cell therapy in some B-ALL cases. Qin et al. indicated that CAR T-cells targeted against TSLPR oncoprotein with 3G11-derived scFv could proficiently eradicate TSLPR expressing cells. TSLPR-based CAR T-cells also have shown therapeutic potential in mice models of B-ALL [74, 75].
CD7 is another transmembrane protein that is typically expressed in T-ALL, not in B-ALL except in rare cases of antigen aberrancy. CD7-based CAR T-cell cancer therapy has been generated and used against malignant T cell lines and primary tumors in a xenograft model of T-AL. Gomes-Silva et al. examined in vitro and in vivo efficacy of CD7-specific CARs for T malignancies. They concluded that CD7-based CAR T-cells have robust antitumor activity in T-cell malignancies [76]. A recent ongoing clinical trial assesses the safety, feasibility, and efficacy of CAR T cell therapy against CD7-positive hematological malignancies in child, adult, and older adult patients [77].
CD38, which is a transmembrane glycoprotein expressed on B- and T-cells, is a candidate therapeutic target for T-cell acute lymphoblastic leukemia whose function is as an adhesion protein related to CD31 or functions as multifunctional ectoenzyme associated with the NAD + and NADP catabolism [78]. Anti-CD38 CAR T-cell demonstrated efficient removal of HTLV-1 + T-cell leukemia [79]. Hofmann et al. recently performed a study for evaluation of efficiency and safety of anti-CD38 CAR T-cells in a 24-year-old female patient with refractory/relapsed B-ALL. They reported a potent and specific antitumor activity of CAR T-38 cells [80]. An ongoing clinical trial is designed for the evaluation of efficiency and side effects of anti-CD38 CAR T-cells in relapsed B- ALL after CD19/CD22 CAR T-cell therapy [81]. In addition, anti-CD38 CAR-T is also being explored in myeloma [78].
Clinical trials
Clinical trials of CAR T-cells in the treatment of multiple hematologic malignancies, including ALL [38, 39, 46], chronic lymphocytic leukemia (CLL) [16, 82], and non-Hodgkin lymphoma (NHL) [54, 83] has significantly improved the perspective of children with recurrent/resistant disease. The evidence of principle was given in the initial studies of a small group of patients with chemotherapy-resistant disease that showed remarkable responses. The successful treatment of patients via CD19-directed CAR T-cells was the basis for further research on the potential of CAR T-cells targeted immunotherapy of ALL.
A case study has been conducted on two children who experienced chemotherapy-refractory/relapsed in 2013 (ClinicalTrials.gov number, NCT01626495) [16] to answer the question of the capability of chimeric antigen receptor T cells would expand in vivo and have clinical activity. CTL019 as chimeric antigen receptor included a CD137 (4–1BB) signaling domain; infusion of such engineering T-cell was previously reported as promising in the treatment of chronic lymphocytic leukemia (CLL) [55]. Although the cytokine-release syndrome and the development of B-cell aplasia were severe, complete remission was observed in both patients, but one of them had a relapse and loss of the CD19-leukemia expressing cells 2 months later.
Maude et al. extended the investigation to better understand the rate of complete and durability of remission, long-term persistence of chimeric antigen receptor-modified T cells CTL019, to a large cohort of a total of 30 children and adults (ClinicalTrials.gov number NCT01029366). Two blinatumomab-resistance patients and 15 patients who had undergone allogeneic hematopoietic cell transplantation were evaluated in such phase I/IIA Study. A durable remission was achieved in 24 months with overall survival (OS) rate of 78% (95% CI, 65 to 95) and a 6-month event-free survival (EFS) rate of 68% (95% CI, 50 to 92) [38].
At Memorial Sloan Kettering Cancer Center (MSKCC) early studies were conducted by Sadeilan’s group in 2011 [84]. 10 adult patients with chemotherapy-refractory chronic lymphocytic leukemia (CLL) or relapsed B-cell acute lymphoblastic leukemia (ALL) have been enrolled for treatment with autologous T cells modified to express 19–28z, a second-generation chimeric antigen (Ag) receptor specific to the B-cell lineage Ag CD19. The inert CD8 transmembrane domain replaced with the transmembrane and cytoplasmic signaling domains of the T-cell costimulatory CD28 receptor aimed to overcome the lack in most B leukemia cells to express a ligand for activating costimulatory receptors. [Clinicaltrial.gov numbers #NCT00466531 (CLL protocol) and #NCT01044069 (B-ALL protocol)]. The primary point was to assess the safety of infusing 19–28z + T cells, whereas the secondary endpoint was to assess the in vivo function of CAR-modified T cells evaluating the clinical response. The clinical benefit was achieved in the setting of prior cyclophosphamide-conditioning chemotherapy and low tumor burden or minimal residual disease. In the follow-up studies [51] they report the dramatic ability of autologous 19–28z CAR-modified T cells to induce MRD − CRs in five patients with relapsed and/or chemotherapy-refractory B-ALL. Those studies are a breakthrough in the efficacy of the CAR-T therapy approach in patients with an aggressive disease that allowed the transition to a standard-of-care allogeneic hematopoietic stem cells transplant (allo-SCT). In adults relapsed B-ALL has a markedly poor prognosis with an expected median survival of fewer than 6 months. A Phase I protocol in 2014 (ClinicalTrials.gov #NCT01044069) states the complete remission (CR) of 88% in an additional cohort of 16 adult patients with relapsed/refractory B-ALL [37].
In a phase I study by Lee et al. at the Pediatric Oncology Branch of the National Cancer Institute (NCI) at the Clinical Center of the US National Institutes of Health on 20 children and young adults with relapsed/refractory B-ALL a CR of 70% was achieved with the TCR ζ (zeta)/CD28 CAR T [ClinicalTrials.gov, number NCT01593696] [46]. The strength of the study is to provide an accurate response rate in a homogenously treated patient population with a standardized treatment protocol as the authors remarked the differences with the previous report of Davila and colleagues [37].
According to the results and former studies, they corroborate that long-term persistence is not necessary to induce antitumor effects and shorter persistence could have potential benefits because patients treated with this approach do not have severe prolonged B-cell aplasia. Additionally, they showed the correlation of CAR T-cell expansion with both anti-leukemia efficacy and cytokine release syndrome severity and therefore the development of neurotoxicity because of CSF penetration of CAR-T cells.
Park et al. (2018) (ClinicalTrials.gov #NCT01044069) reported data from long-term follow-up in early 2018. CR of 83% with the utilization of 19–28z CAR T cells on 53 adults patients with ALL at a median follow-up of 29 months and a median OS of 12.9 months [85].
Interestingly, this group at the MSKCC found that the best predictor of short-term response and toxic effects was the peak CAR T-cell expansion. In contrast, in the long-term outcomes, the disease burden at the time of the treatment impacts significantly the long event-free survival and overall survival. In this case, the authors didn’t find a significant correlation between the persistence of CAR T cells and survival altogether in the subgroups of patients, which indicates that 19–28z CAR T-cell persistence is not requisite for durable remissions. The lack of correlation with T-cell persistence has been demonstrated in preclinical studies where was shown the high effector function and self-limited expansion of CD28-based CARs [56, 57].
The rationale for the dual antigen targeted CAR T cells is due to the common mechanism of target antigen loss and/or mutation underlying the relapse. Dual-targeted CAR T cells can be generated either with bicistronic CARs that express two different targets ScFv simultaneously in every cell or with mono-CARs.
In a Phase I/II clinical trial, bispecific CAR T-cell therapy called AUTO3 designed to target CD19 and CD22 simultaneously was considered (R/R) B-cell ALL pediatric patients, [58]. OX40 costimulatory domain for the CD19 and a 4–1BB for the CD22 were incorporated for the second-generation CARs. The end-point of the study was the safety and efficacy evaluations. Three dose levels were explored (1 × 106, 3 × 106, and 5 × 106 transduced CAR + T cells/kg) and CAR T cells were infused as a single (for <25% blasts) or split (for >25% blasts) dose based on leukemia burden. 4/4 of patients achieved MRD complete remission with no antigen-negative escape at this early stage.
Yang et al. (2019) enrolled for a phase I study (US NIH Clinical#: NCT03825731) 17 patients with relapsed/refractory B-ALL including 4 pts previously treated with CD19 CAR-T cells. Four were adults, 13 pediatrics (age 1–45). CD19 CD22 bispecific scFv contained a 4–1BB costimulatory signal domain. All pts received a conditioning regimen of fludarabine and cyclophosphamide intravenously before a single infusion of CAR-T cells. The primary endpoints were to gauge feasibility and toxicity, and therefore the secondary endpoints included disease response and engraftment/persistence of infused CD19/CD22 dual CAR-T cells. The study showed safety, and clinical efficiency of CD19/CD22 dual CAR T, noteworthy low toxicity with dose-dependent high CR rate was reported. Nobody relapsed with a median observation time of 60 (7–139) days [86].
Gu et al. (2020) at the Institute of Hematology & Blood Diseases Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College supported their preclinical results proposed a search of CD19 CAR T with scFvs capable of binding to different CD19 epitopes as a choice for patients with mutations in CD19. Despite many efforts that are made to enhance the planning of the CAR, loss of the epitope results in non-responding patients and relapse.
The single-arm pilot study reported the security, and clinical efficiency of CD19 CAR T constructed with a replacement anti-CD19 chimeric antigen receptor (HI19α-4–1BB-ζ CAR T, or CNCT19) in treating 20 pediatric and adult patients with R/R B-ALL. A high CR/CRi rate (90%) was reported after a follow-up of 28 days, median overall survival of 12.9 months, and relapse-free survival of 6.93 months (NCT02975687) [87].
As the authors stated and that we are agreed thereupon, so far a long-term follow-up has revealed a significant proportion of patients relapse after treatment, this suggests that more efforts are needed to spot biomarkers. The exhaustion of CAR-T cells and therefore the subsequent inability to maintain the CAR-T cell-killing effect were major underlying factors for relapse. It is not yet clear whether the expansion kinetics of various T cell subsets are related to differential responses observed concerning long-term patient responses to therapy. Moreover, the antitumor capabilities of some T cell subsets, like CD8 + central memory T cells (TCM), remain controversial and have not been subjected to adequate study. They proposed as a potential biomarker the percentage of CD8 + naïve T cells (TN) based on the results that CAR T cells generated from less differentiated T cell subsets exhibited more proliferative potential and antitumor activity than did those derived from differentiated cell subsets.
In ongoing clinical trials, NCT03984968 at the Hospital of Soochow University as consolidation therapy, T cells expressing CD19 antigen (feeding T cell) were constructed, expanded in vitro, and infused back along with CD19 CAR-T cells into patients to continuously stimulate the therapeutic effect and reduce the relapse rate.
Annesley et al. (2019) showed the effectiveness of CAR T cell product in infant patients. Safety and MRD-CR were similar to those of non-infant ALL patients. However, patients’ number during this study was not enough to form a definitive decision in this regard [88].
Tables 1 and 2 show the list of clinical trials assessing CAR T-cell therapy for pediatric and adult ALL patients that are performed in different centers.
CAR-T toxicity
The two major toxicities associated with CAR-T therapy are cytokine release syndrome (CRS) and the Immune effector cell-associated neurotoxicity syndrome (ICANS) in ALL patients compared to other B-cell malignancies, particularly in adults. The long-term efficiency and safety of this promising approach are not yet available and remain a challenge [59, 60, 89]. The foremost common side effects (incidence greater than 20%) were hypogammaglobulinemia, pyrexia, infections-pathogen unspecified, encephalopathy, headache, decreased appetite, bleeding episodes, coagulopathy, hypotension, nausea, tachycardia, diarrhea, vomiting, viral infectious disorders, fatigue, hypoxia, even poor concentration, and delirium. Additionally, two clinical trials (NCT01626495 and NCT02906371) in ALL pediatric patients reported an acute kidney injury (AKI) and electrolyte abnormalities as a serious complication following the CAR-T treatment [37, 38, 47, 50, 53, 58, 61, 84,85,86,87, 90, 91]. Cytokine-associated toxicity, also referred to as cytokine release syndrome (CRS), occurs as an immediate consequence of the activation of macrophages related to inflammatory cytokines triggered by large amounts of IFN-γ released by activated T cells [92, 93]. Across the clinical trials presented in this review, CRS has been reported to occur in any grade in the range of 56–100% including severe CRS (grade ≥) for 3–71% sometimes with a fatal outcome [16, 37,38,39, 47, 54, 83, 92, 94, 95]. Of note, CRS grading systems differ across clinical trials. Since the beginning of the description of several circulating cytokines elevation leading to the overwhelming majority of symptoms, CRS grading was not clear and lack of consensus available among the institutions made the comparisons between products and trials difficult. CRS must be recognized and treated promptly to preserve life-threatening consequences and to don’t impair the efficacy [96]. The driving cytokine underlying CRS is assumed to be IL-6 [97, 98] indeed, immunosuppression using tocilizumab, an anti-IL-6 receptor antibody, with or without corticosteroids, can reverse the syndrome but could limit the efficacy of the immunotherapy [93].
The first effort to realize a far better refinement of the clinical sign based on the Common Terminology Criteria for Adverse Events (CTC AE v4.03) was achieved by sharing the expertize and experiences of a multi-institutional group of pediatric oncologists in the USA in 2014. Their work has been referred to Lee criteria and has been widely adopted [92]. The algorithm takes patients' response to intravenous fluids (IVFs) and vasopressors, oxygen requirement, and organ toxicities under consideration. Although other different criteria systems wont to grade CRS has been followed, a consensus scale has recently been published by the American Society for Transplantation and Cellular Therapy (16).
Identify biomarkers that allow stratifying the high-risk patients before therapy to intervene preventively could potentially reduce the prospect of developing severe CRS (sCRS) after the infusion.
The approach of Davila et al. in 2015 at MSKCC was to identify a set of criteria for the diagnosis of an sCRS based on the presence of fevers start about 24 h after the infusion with 19–28z CAR T cells, the elevation of specific cytokines, and clinical toxicities as hypotension. Commonly elevated serum proteins during CRS are IL-6, TNF-a, IL-10, INF-g, IL-15, IL-2, IL-10, C-reactive protein (CRP), ferritin, and IL-8 (8, 19–21). Elevation of seven cytokines of 39 measured correlated (r = 0.43 to 0.88) to pretreatment tumor burden and also to an sCRS in the cohort of 16 adult R/R B-ALL. Application of those criteria allowed the stratification of the patients into different groups: sCRS will likely require therapeutic intervention with corticosteroids or interleukin-6 receptor blockade and nCRS will experience mild symptoms that would require routine management [37]. Additionally, they found the serum C-reactive protein CRP elevation as a reliable biomarker.
Hay et al. in 2017 in a clinical report of a large cohort of 133 adult patients with CD19 + relapsed/refractory B-ALL, CLL, or NHL reported CRS developed in 70% of patients 62.5% with grade 1 to 3 CRS (grade 1, 26%; grade 2, 32%; grade 3, 4.5%), 3.8% with grade 4, and 3.8% with grade 5. Life-threatening CRS mainly occurred during the CAR T-cell dose-escalation phase of their study. As previously demonstrated CAR-T cell dose was related to the risk of severe CRS in patients with a high tumor burden and an early intervention approach won’t impair the efficacy [39, 95]. In their study MCP-1 evaluation was superior to CRP testing, serum Willebrand factor VWF and the serum angiopoietin Ang-2:Ang-1 ratio were higher before starting CAR T-cell immunotherapy in patients who subsequently developed more severe CRS, suggesting that preexisting endothelial activation might be a previously unrecognized risk factor for severe CRS. The authors remarked the thrombocytopenia before lymphodepletion chemotherapy was also associated with subsequent severe CRS.
Macrophage activation syndrome (MAS) or Secondary haemophagocytic lymphohistiocytosis (sHLH) has been recognized as the causative agent of severe immunological disorders characterized by pro-inflammatory cytokine production, immune-induced multiorgan failure, and lymphohistiocytic tissue infiltration. In rare cases, CRS can evolve into fulminant and refractory HLH/MAS-like toxicities resulting in death [99,100,101,102]. One among the foremost important challenges of those severe immunological disorders is that the inability to distinguish MAS/ sHLH within the context of CRS. CAR-T-cell therapy-associated TOXicity Working Group (CARTOX) expanding the Lee et al. criteria developed a consistent approach for monitoring, grading, and management of those toxicities [99, 103]. MAS/sHLH observed at the MD Anderson Cancer Center was reporting in ~1% of all patients [103]. The diagnosis has been made at ferritin levels of >10,0000 ng/ml during the CRS phase within the primary 5 days after cell infusion. Additional therapy with etoposide was given as previously reported [104,105,106]. Shah et al. 2020 applied such criteria in the Phase I Anti-CD22 CAR-T cell dose-escalation trial using anakinra for treatment of HLH-like manifestations [102].
In association with or following CRS, another common toxicity observed after CAR T cell therapy is neurotoxicity, whose consensus grading scale has also been published by The American Society for Transplantation and Cellular Therapy defined as ICANS. Peculiar symptoms that may occur during or more commonly after CRS, (in a rare case before), vary among patients and encompass, delirium, encephalopathy, aphasia, lethargy, difficulty concentrating, agitation, tremor, seizures, and, rarely, cerebral edema [93, 107]. Neurotoxicity is now considered to be treated separately. Macrophage activation, endothelial activation, and the enrichment of pro-inflammatory cytokines in the CNS have all been proposed as potential mechanisms for CAR T cell-related ICANS [59]. Neurologic symptoms might be observed in association with pathological processes including hepatic failure, severe hypertension, eclampsia, infection, electrolyte abnormalities, and immunosuppressive and cytotoxic drug therapies. The pathogenesis of Neurologic Adverse events (AE) is still unknown, in 2017, Gust et al. reported in 133 adults with refractory B-ALL, NHL, or CLL that followed by the endothelial activation the blood-brain barrier might be disrupted allowing high circulating cytokines to access the cerebrospinal fluid. The presence of fever, high serum IL-6, and MCP-1 concentrations within the first 36 h are predictive of severe neurotoxicity, and early intervention is needed [108]. Tocilizumab has no beneficial effect on ICANS and should even worsen it in some cases highlighting the need for the development of preemptive therapies instead of tocilizumab for management of neurotoxicity [109]. Although it has been proposed that siltuximab with a higher affinity for IL-6 might be preferred over tocilizumab, can’t be considered in the frontline therapy approach as it’s not yet FDA-approved for now.
CAR T-cell FDA-approved
There are currently five FDA-approved CAR T-cell therapies, including Lisocabtagene Maraleucel (Breyanzi), Axicabtagene Ciloleucel (Yescarta), Brexucabtagene Autoleucel (Tecartus) [110], Idecabtagene Vicleucel (Abecma), and Tisagenlecleucel (Kymriah) [111, 112]. Among them, only Tisagenlecleucel (Trade name of Kymriah™) is indicated for the treatment of pediatric and young adults patients with (R/R) B-cell ALL [113]. Tisagenlecleucel, an autologous CD19-targeted CAR T-cell, recently was approved by Food and Drug Administration (FDA), European Union (EU), and Japan as a cell-based therapy product for use in pediatric patients with refractory or relapsed (R/R) B-cell precursor ALL [114,115,116,117,118]. Based on clinical data, 83% of patients have attained a partial or complete response to a single injection of tisagenlecleucel in a short period [89]. Besides, time left after primary treatment without certain complications, and overall survival was higher for tisagenlecleucel treated patients than other cancer treatment approaches [119]. It is essential to understand that the approved CAR-T therapies all target CD19.
Advantage of CAR T treatment
There are many benefits for CAR T-cell therapies over conventional treatments. CAR T-cell therapy can help patients who’s their cancer recurs after several treatments to achieve complete remissions for years. Some patients live for long periods without their cancer progress. Major advantages of CAR T-cell therapies are the low number of infusions needed, short treatment period, and rapid recovery than traditional treatments. CAR T-cell therapies also benefit from living cells, which can amplify in patients’ body to provide memory for many years. Therefore, existing long-lived CAR T-cells can recognize and kill cancer cells when there is a relapse. Available data shows a complete remission for a long time in relapse/refectory patients after receiving a single infusion of CAR T-cell therapies. In addition to treating local cancers, this treatment modality can also be successful in eradicating metastatic cells [120].
CAR-T cell therapy is a targeted therapy with high specificity which can remove cancer cells expressing the corresponding tumor-associated antigens, unlike the usual adaptive immune cells. So, to a great extent, this treatment method will avoid unnecessary eliminating of healthy normal cells. Interestingly, CAR-T cells can identify cell surface antigens without the help of major histocompatibility complex (MHC) genes expression. So, cancer cells cannot escape from the immune system (T cell immune surveillance) by hiding MHC or surface molecules contributed to antigen processing and presentation [121,122,123]. It should be noted that CAR-T cells are almost potentially able to detect different forms of potential antigens including lipids, carbohydrates, and proteins [124]. Furthermore, chimeric antigen receptors have a flexible intracellular signaling domain that allows the cell to prevent the downregulation of costimulatory molecules induced directly or indirectly by tumor cells [125].
Challenges of CAR-T cell therapy
Although the rate of the primary response to CAR T-cell therapy in B-cell malignancies for relapsed or refractory disease is remarkably effective and is related to a CRi/CR (74–90%) in some clinical trials [37, 38, 47, 50, 58, 84,85,86,87] still many patients fail to respond or relapse after the initial treatment. A global study has demonstrated that the relapse rate of CD19-targeted CAR-T cell therapy is ~30%.
This is the results of two important factors: short-term sustainment of CAR T-cells in the bodies of patients with CD19 + cells and therefore the absence of surface antigen CD19 (CD19- variants) and/or surface antigen CD20 (CD20- variants) in patients due to the presence of mutations or deletions in the respective the CD19 or CD20 genes.
In patients with acute leukemia, the downregulation or even loss of antigenic epitope on CD19 appears to be a dominant mechanism of tumor escape. Frameshift code insertion, deletion in CD19 exons 2–5 that encode for the extracellular domain or loss of heterozygosity (LOH) results in epitope loss in 10 to 20% of pediatric B-ALL treated with CD19-directed immunotherapy as detected by clinical flow cytometry [53, 126].
The loss of CD19 targeted epitope followed by the CAR T therapy was reported for the first time on B-ALL patients relapsed 2 months after the success of the treatment. Deep sequencing data showed malignant CD19- clones in the bone marrow and peripheral blood at day 23 [16]. The phenomenon can be explained with the induction of the subclonal selection with a different phenotype due to the result of the therapy suppressing and/or eradicating the leukemic clone identified at the time of diagnosis. Multiple mechanisms have been uncovered that are responsible for the antigen loss considering the main impediment of the promising treatment.
Sotillo et al. reported preexisting alternatively spliced at exon 2 lacking the CTL019 epitope binding site as previously believed and acquired mutations in the malignant B cells of relapsed pediatric patients. The authors highlighted the possibility of targeting alternative CD19 ectodomain based on the evidence that the entire protein is not discarded. In following studies aimed to explore the mechanism associated with the CD19-/r B-ALL, in a cohort study of 12 patients with B-ALL, antigen loss was originated from alterations in CD19 exons 2–5 lead to a truncated protein with a nonfunctional or absent transmembrane domain, whereas alternatively spliced variants were found only with low frequency [40]. These findings were not in support of the splicing hypothesis and suggested an alternative targeting or combination CAR approach. Bagashev et al. reported the presence of mutated and misfolded CD19 in the endoplasmic reticulum of the malignant B cells [127]. Another mechanism of antigen loss is the cell lineage switch. The first case regarding cell lineage switch was reported in 2015. A CLL patient with Richter transformation relapsed after CAR T-cell therapy with a CD19- plasmablastic lymphoma [128].
Afterward, another report showed 2 of 7 patients with mixed lineage leukemia (MLL)-rearranged B-ALL and in a case report of a pediatric B-ALL, relapsing with CD19-negative AML after CD19 CAR T-cell therapy [129, 130]. Ruella et al., reported a novel intriguing not previously described mechanism where CAR T-cell on the leukemia surfaces bound in cis to CD19, covering it from recognizing by the CAR [131].
Partial antigen loss is caused by antigen downregulation and is considered as another mechanism of immune escape to the treatment [132,133,134,135]. Watanabe et al. using a CD20 CAR have been the first to set the threshold level of antigen molecules per target cells required to induce lytic function. It has been concluded that CAR-T cells can recognize and lyse cells expressing considerably low levels of the target Ag and were activated and expanded upon such stimulation. This finding suggested that CAR-T therapy might show a better effect in the case of only a limited number of target Ags on the tumor cells [133]. Another research stated that a CD30 CAR could specifically kill lymphoma cells while “ignoring” healthy CD30 + cells due to differential expression of antigen molecules on the cell surface [136]. Walker et al. documented that CAR T-cell function is also influenced by CAR numbers per engineered T cells [134]. Recently, this finding was confirmed in relapsed patients with decreased levels of CD22 on the B-ALL cell surfaces [132].
R/R ALL patients who relapsed after allo-HSCT usually have a poor prognosis, and donor lymphocyte infusion (DLI) can only save a few numbers of patients. The efficacy and safety of donor-derived CARs targeted against CD19 for relapsed B-ALL patients after allo-HSCT administration is studied [137]. Also, it has been reported that the CD123 antigen is overexpressed in ALL patients with relapsed disease. Dual-targeted CAR T-cells against CD19/CD123 were an effective manner for diminishing CD19 antigen loss in animal studies [131]. GVHD rate in Donor-derived allogeneic CAR T treatments remains very low because of low-dose cell infusions [89, 138].
To make sure better expansion, persistence, and safety of CAR-T cells, patients usually receive cyclophosphamide and fludarabine before CAR-T infusion to scale back the occurrence of lymphocytes and lower the burden of leukemia [139]. A phase I clinical trial showed that 22 of 53 adult patients with B-ALL (41.5%) received lymphodepleting chemotherapy followed by 19–29z CAR T-cells expanded severe (grade 3–4) neurologic side effects characterized predominantly by aphasia, encephalopathy, depressed consciousness, myoclonus, and seizure [81]. As a result, this modern treatment should be employed along with specialized medical care by a medical group with different expertise and all the required facilities to certify optimal consequences for patients [60]. So, children with relapsed or refractory ALL, which receiving chimeric antigen receptor (CAR) T‐cell therapy, even need Psychosocial care [140]. Additionally, the cost of this treatment is very high for patients; ~282,000 euros per patient [141].
A CD22 CAR T-cell clinical study also reported that CAR T-cell administration could provide a suitable complete remission (CR) or CR with incomplete count recovery (CRi) (80%) evaluated after 30 days in this study. Most patients only experienced mild cytokine-release syndrome and neurotoxicity [142].
It was shown that preconditioning chemotherapy and reducing disease burden positively affect treatment response without any increase in toxicity [143]. Also, it had been demonstrated that Allogeneic HCT might improve event-free survival following CD19 CAR T-cell therapy [144]. Tocilizumab, an IL-6R antagonistic monoclonal antibody, has been extensively wont to reduce CRS [145].
However, even with the considerable CR rate, ~50% of CD19-targeted CAR T-cell therapies relapsed within a year after treatment. These patients are mostly resistant to secondary treatment with CD22 targeted CAR T-cell therapy. In some cases, relapse happened because of loss of the CD19 antigen. However, CD19 antigen expression remains in the relapsed tumor cells of most patients, and the underlying mechanisms are unknown.
It is offered that CAR molecules can lead to host immune responses because they are immunogenic. This immune response can eliminate infused CAR T-cells. In some patients, anti-CAR immune responses are produced by CD8 T cells. Humanized ScFv has higher CAR T-cell persistency and lowers relapse rate. Vaccination also improves CAR T-cell persistency. Furthermore, 4–1BB CAR T-cell clinical trials have described higher persistency compared with CD28. However, a recent study reported better efficacy for CD28 CAR T-cells [139]. So, the choice between 4–1BB and CD28 targeted CAR T-cells remains controversial. We can bring into account target-mediated toxicity, which results when CAR-T cells damage the healthy cells that express the target, as a challenge in the development of CAR T-cell products. Although this problem can resolve via knocking out the targeting antigen in CAR T-cells by using CRISPR/Cas9 as a new gene-editing technology [146].
Another problem for the development of CAR T-cell therapy is an economical challenge. Currently, the costs of CAR T-cell products and their related costs are also an essential concern for health policymakers, especially in developing countries. However, it seems that by advancement in the field of CAR T-cell therapy overtime work, it can be possible to make its production more cost-effective [147].
Access can be considered as another limiting factor in the term of CAR T-cell therapy. FDA-approved drugs or enrollment in clinical trials are two the crucial access patients. So, challenges with patient recruitment, enrollment, and retention can limit patients’ access to CAR T-cell therapy. Relatively high cost, inclusion criteria limitations, and the uncertain time interval between leukapheresis and infusion can be other limiting factors for access [148].
Strategies to overcome challenges
One clear way to overcome the antigen loss challenge after CAR T-cell therapy is using more than one target. This strategy is implemented using four different methods: (a) Making different cell populations express various CARs and fusing them sequentially using coadministration; (b) Designing bicistronic or tricistronic vector by expressing two or three different CARs on one cell; (c) Engineering T cells with two different CAR vector (cotransduction), or (d) Encoding bispecific tandem CARs on one chimeric protein by a single vector [135, 149,150,151]. Transplantation of allogeneic stem cells (allo-SCT) is another potent approach to overcome a patient’s relapse. To decrease the antigen loss and relapse rate, dual-targeted (CD19/CD22) and donor-derived CAR T-cells have entered clinical trial phases. Dual-targeted CARs can be produced as bicistronic or mono-CARs. In the first approach, Engineered T cells are known to express both ScFv simultaneously. As per the latter strategy, all T cells may not be able to express both CD19 and CD22 as the cell population has three different CARs of CD19−, CD22−, or CD19/22-targeted T cells. In CD19/22-targeted cells, the ratio of CD19/CD22 CARs may not be the same. Also, mixed or sequential administration of CAR19 and CAR22 T cells could be used for ALL treatments [152]. A new strategy uses one tricistronic transgene vector that simultaneously expresses three CARs (CD19/CD20/CD22 CARs) on a single T-cell [153]. This approach demonstrates that coexpressing CD19/CD20/CD22 CAR T-cell is regarded as an excellent solution for treatment in ALL, due to simultaneous targeting of CD19, CD20, and CD22. For this reason, increasing the rate of CAR T-cell success and decreasing the relapse rate of ALL due to targeting CD19 − helps escape B-ALL while maintaining their upfront efficacy [150].
As mentioned above, the differentiation of MAS/sHLH from CRS is a crucial challenge in treatment with CAR T-cell therapy. Therefore, efforts are underway to expand the implementation of strategies known to treat/prevent this complication. Predictive biomarkers, including Ferritin and cytokine profiling, were applied to distinguish MAS/sHLH from CRS. Another strategy to treat/prevent this complication is the use of steroids and/or anakinra without affecting CAR T cell efficacy [101, 154].
Checkpoint inhibitors
Programmed death-ligand 1 (PD-L1) and programmed death-ligand 2 (PD-L2) genes expression, due to the inhibition of CAR T-cell antitumor activity (T cell exhaustion), is one of the most critical challenges for effective use of CAR T-cell in solid tumors and hematological malignancies [155, 156]. Utilizing checkpoint blockade in combination with CARs is one of the strategies to overcome this issue. Additionally, it was reported that checkpoint inhibitors administration could provide an effective and safe improvement in CD19-targeted CAR T-cell therapy in relapsed B-cell ALL [157]. This improvement is due to the release of the immune blockade on the T cell, removing the restriction that’s holding it in check and, in turn, following checkpoint inhibitors, which provide a more significant activity in T cells [158].
In a clinical study performed on 13 children (ranging in age from 4 to 17 years) with relapsed or refractory B-cell ALL treated with CD19-directed CAR T-cell therapy, it was observed that PD-1 checkpoint blockade may improve the CAR T-cell persistence; thus amplifying the rate of CAR T-cell success and reducing the relapse rate of B-cell ALL [159]. Furthermore, mutation design on CD28 costimulatory domain of second-generation CAR T-cells is another strategy that not only improved CAR T-cell durability and decreased exhaustion, but also may be reduced expression of programmed cell death protein 1 (PD-1) in B-cell acute lymphoblastic leukemia (B-ALL) mice [160].
Another strategy for improved CAR T-cell function is these cells engineered to co-express other molecular, including costimulatory molecules, checkpoint blockade, and cytokines which are referred to as armored’ CAR-T. The co-express checkpoint blockade and cytokinesis are thus able to improve the antitumor efficacy of the CAR-T cells, stimulating their pro-inflammatory impact due to their effect on tumor-related dendritic cells (DCs), macrophages, tumor-infiltrating lymphocytes (TILs), and natural killer (NK) cells [161, 162].
Conclusion
Currently, chemotherapy is considered, as the first line to confront ALL. Stem cells are non-specialized cells that are found in many adults and embryonic tissues. Hematopoietic stem cells have multipotent characteristics, reproducibility, and plasticity. They also have high anticancer potential as a promising approach for the treatment of ALL. For this reason, the transplantation of hematopoietic stem cells has been regarded as a secondary line in human ALL therapy. Although chemotherapy and transplantation of hematopoietic stem cells [Allogeneic stem cells transplantation] remain the gold standard for ALL therapy, the significant complications such as graft versus host disease (GvHD) of these approaches are among their limitations. Due to these issues, novel strategies can be used for ALL treatment. With the advent of knowledge of immunotherapy and its associated methods, increased efficacy in the treatment of cancer was created. Especially, CAR T cell technology as an Immunotherapy-based strategy is suggested as an ideal candidate for ALL treatment. So, this technology could provide great potential in the treatment of cancer. Although it has serious challenges such as cytotoxicity, cytokine release syndrome, neurotoxicity, and ICANS. Development in the production of different generations of CAR technology and their combined use in other ways, such as hematopoietic stem cell transplantation, can be used as an efficient method of ALL treatment after failure of chemotherapy methods. This technology can be used in the future as an effective and safe treatment for ALL treatment.
Future Perspectives
The central portion of current researches and most likely future investigations are focused on the identification of new target antigens and novel combinations of currently available targets. One principal challenge is to select better preclinical studies to recognize potential combinations. Also, exploration of antigen loss mechanisms and identification of overcoming strategies is essential to the research purpose. Overcoming T-cell function inhibitors in the tumor microenvironment can accelerate the development and advancement of CAR T-cell products. Currently, there are ~470 clinical trials in the field of CAR T-cell therapy and possibly thousands of combinations to study.
References
Hunger SP, Mullighan CG. Acute lymphoblastic leukemia in children. N. Engl J Med. 2015;373:1541–52.
Siegel RL, Miller KD, Fuchs H, Jemal A. Cancer statistics, 2021. CA Cancer J Clin. 2021;71:7–33.
Jabbour E, O’Brien S, Konopleva M, Kantarjian HJC. New insights into the pathophysiology and therapy of adult acute lymphoblastic leukemia. Cancer. 2015;121:2517–28.
Terwilliger T, Abdul-Hay M. Acute lymphoblastic leukemia: a comprehensive review and 2017 update. Blood Cancer J. 2017;7:e577.
Hunger SP, Lu X, Devidas M, Camitta BM, Gaynon PS, Winick NJ, et al. Improved survival for children and adolescents with acute lymphoblastic leukemia between 1990 and 2005: a report from the children’s oncology group. J Clin Oncol. 2012;30:1663.
Sun W, Malvar J, Sposto R, Verma A, Wilkes JJ, Dennis R, et al. Outcome of children with multiply relapsed B-cell acute lymphoblastic leukemia: a therapeutic advance in childhood leukemia & lymphoma study. Leukemia. 2018;32:2316–25.
De Angelis R, Sant M, Coleman MP, Francisci S, Baili P, Pierannunzio D, et al. Cancer survival in Europe 1999–2007 by country and age: results of EUROCARE-5—a population-based study. Lancet Oncol. 2014;15:23–34.
Pullarkat V, Slovak ML, Kopecky KJ, Forman SJ. Appelbaum FRJB, The Journal of the American Society of Hematology. Impact of cytogenetics on the outcome of adult acute lymphoblastic leukemia: results of Southwest Oncology Group 9400 study. Blood. 2008;111:2563–72.
Moorman AV, Harrison CJ, Buck GA, Richards SM, Secker-Walker LM, Martineau M, et al. Karyotype is an independent prognostic factor in adult acute lymphoblastic leukemia (ALL): analysis of cytogenetic data from patients treated on the Medical Research Council (MRC) UKALLXII/Eastern Cooperative Oncology Group (ECOG) 2993 trial. Blood. 2007;109:3189–97.
Henig I, Zuckerman T. Hematopoietic stem cell transplantation-50 years of evolution and future perspectives. Rambam Maimonides Med J. 2014;5:e0028.
Sung AD, Chao NJ. Concise review: acute graft-versus-host disease: immunobiology, prevention, and treatment. Stem cells Transl Med. 2013;2:25–32.
Eryılmaz E, Canpolat C. Novel agents for the treatment of childhood leukemia: an update. OncoTargets Ther. 2017;10:3299–306.
Ohno R. Treatment of Philadelphia-chromosome-positive acute lymphoblastic leukemia with imatinib in combination with chemotherapy. Curr Hematol Malig Rep. 2006;1:180–7.
Hucks G. The journey to CAR T cell therapy: the pediatric and young adult experience with relapsed or refractory B-ALL. Blood Cancer J. 2019;9:1–9.
Ishii K. Novel immunotherapeutic approaches for the treatment of acute leukemia (myeloid and lymphoblastic). Ther Adv Hematol. 2016;7:17–39.
Grupp SA, Kalos M, Barrett D, Aplenc R, Porter DL, Rheingold SR, et al. Chimeric antigen receptor–modified T cells for acute lymphoid leukemia. N. Engl J Med. 2013;368:1509–18.
Waldman AD, Fritz JM, Lenardo MJ. A guide to cancer immunotherapy: from T cell basic science to clinical practice. Nat Rev Immunol. 2020;20:651–68.
Kershaw MH, Westwood JA, Parker LL, Wang G, Eshhar Z, Mavroukakis SA, et al. A phase I study on adoptive immunotherapy using gene-modified T cells for ovarian cancer. Clin Cancer Res. 2006;12:6106–15.
Lamers CH, Sleijfer S, Vulto AG, Kruit WH, Kliffen M, Debets R, et al. Treatment of metastatic renal cell carcinoma with autologous T-lymphocytes genetically retargeted against carbonic anhydrase IX: first clinical experience. J Clin Oncol. 2016;24:e20–2.
Brown CE, Alizadeh D, Starr R, Weng L, Wagner JR, Naranjo A, et al. Regression of glioblastoma after chimeric antigen receptor T-cell therapy. N. Engl J Med. 2016;375:2561–9.
Zhang C, Liu J, Zhong JF, Zhang X. Engineering car-t cells. Biomark Res. 2017;5:22.
Abate-Daga D, MLJMT-O Davila. CAR models: next-generation CAR modifications for enhanced T-cell function. Mol Ther Oncolytics. 2016;3:16014.
Guedan S, Calderon H, Posey AD, Maus MV. Engineering and design of chimeric antigen receptors. Mol Ther Methods Clin Dev. 2019;12:145–56.
Guest D, Hawkins RE, Kirillova N, Cheadle EJ, Arnold J, O’Neill, J A, et al. The role of extracellular spacer regions in the optimal design of chimeric immune receptors: evaluation of four different scFvs and antigens. J Immunother. 2005;28:203–11.
James SE, Greenberg PD, Jensen MC, Lin Y, Wang J, Till BG, et al. Press antigen sensitivity of CD22-specific chimeric TCR is modulated by target epitope distance from the cell membrane J Immunol. 2008;180:7028–38.
Wilkie S, Picco G, Foster J, Davies DM, Julien S, Cooper L, et al. Retargeting of human T cells to tumor-associated MUC1: the evolution of a chimeric antigen receptor J Immunol. 2008;180:4901–9.
Jayaraman J, Mellody MP, Hou AJ, Desai RP, Fung AW, Pham AHT, et al. CAR-T design: elements and their synergistic function. EBioMedicine. 2020;58:102931.
Hudecek M, Lupo-Stanghellini MT, Kosasih PL, Sommermeyer D, Jensen MC, Rader C, et al. Receptor affinity and extracellular domain modifications affect tumor recognition by ROR1-specific chimeric antigen receptor T cells. Clin Cancer Res. 2013;19:3153–64.
Hudecek M, Sommermeyer D, Kosasih PL, Silva-Benedict A, Liu L, Rader C, et al. The nonsignaling extracellular space domain of chimeric antigen receptors is decisive vivo antitumor activity. Cancer Immunol Res. 2015;3:125–35.
Brocker TJB. Chimeric Fv-ζ or Fv-ε receptors are not sufficient to induce activation or cytokine production in peripheral T cells. Blood. 2000;96:1999–2001.
Weinkove R, George P, Dasyam N. Selecting costimulatory domains for chimeric antigen receptors: functional and clinical considerations. Clin Transl Immunol 2019;8:e1049.
Carpenito C, Milone MC, Hassan R, Simonet JC, Lakhal M, Suhoski MM, et al. Control of large, established tumor xenografts with genetically retargeted human T cells containing CD28 and CD137 domains. Proc Natl Acad Sci USA. 2009;106:3360–5.
Salter AI, Ivey RG, Kennedy JJ, Voillet V, Rajan A, Alderman EJ, et al. Phosphoproteomic analysis of chimeric antigen receptor signaling reveals kinetic and quantitative differences that affect cell function. Sci Signal. 2018;11:eaat6753.
Milone MC, Fish JD, Carpenito C, Carroll RG, Binder GK, Teachey D, et al. Chimeric receptors containing CD137 signal transduction domains mediate enhanced survival of T cells and increased antileukemic efficacy in vivo. Mol Ther. 2009;17:1453–64.
Finney HM, Lawson AD, Bebbington CR. Chimeric receptors providing both primary and costimulatory signaling in T cells from a single gene product. J Immunol. 1998;161:2791–7.
Finney HM, Akbar AN. Activation of resting human primary T cells with chimeric receptors: costimulation from CD28, inducible costimulator, CD134, and CD137 in series with signals from the TCRζ chain. J Immunol. 2004;172:104–13.
Davila ML, Riviere I, Wang X, Bartido S, Park J, Curran K, et al. Efficacy and toxicity management of 19-28z CAR T cell therapy in B cell acute lymphoblastic leukemia. Sci Transl Med. 2014;6:224ra25–ra25.
Maude SL, Frey N, Shaw PA, Aplenc R, Barrett DM, Bunin NJ, et al. Chimeric antigen receptor T cells for sustained remissions in leukemia. N Engl J Med. 2014;371:1507–17.
Turtle CJ, Hanafi L-A, Berger C, Gooley TA, Cherian S, Hudecek M, et al. CD19 CAR–T cells of defined CD4+: CD8+ composition in adult B cell ALL patients. J Clin Invest. 2016;126:2123–38.
Gardner RA, Finney O, Annesley C, Brakke H, Summers C, Leger K, et al. Intent-to-treat leukemia remission by CD19 CAR T cells of defined formulation and dose in children and young adults. Blood 2017;129:3322–31.
Shah BD, Stock W, Wierda WG, Oluwole O, Holmes H, Schiller GJ, et al. Phase 1 results of ZUMA-3: KTE-C19, an anti-CD19 chimeric antigen receptor (CAR) T cell therapy, in Adult patients with relapsed/refractory acute lymphoblastic leukemia (R/R ALL). Blood 2017;130:888.
Maude SL, Teachey DT, Rheingold SR, Shaw PA, Aplenc R, Barrett DM, et al. Sustained remissions with CD19-specific chimeric antigen receptor (CAR)-modified T cells in children with relapsed/refractory ALL. J Clin Oncol. 2016;34:3011.
Grupp SA, Maude SL, Shaw PA, Aplenc R, Barrett DM, Callahan C, et al. Durable remissions in children with relapsed/refractory ALL treated with T cells engineered with a CD19-targeted chimeric antigen receptor (CTL019). Blood. 2015;126:681.
Maude SL, Barrett DM, Rheingold SR, Aplenc R, Teachey DT, Callahan C, et al. Efficacy of humanized CD19-targeted chimeric antigen receptor (CAR)-modified T cells in children and young adults with relapsed/refractory acute lymphoblastic leukemia. Blood. 2016;128:217.
Maude SL, Shah DT, Porter DL, Grupp SAJB. CD19-targeted chimeric antigen receptor T-cell therapy for acute lymphoblastic leukemia. Blood. 2015;125:4017–23.
Lee DW, Kochenderfer JN, Stetler-Stevenson M, Cui YK, Delbrook C, Feldman SA, et al. T cells expressing CD19 chimeric antigen receptors for acute lymphoblastic leukaemia in children and young adults: a phase 1 dose-escalation trial. Lancet. 2015;385:517–28.
Forsberg MH, Das A, Saha K. The potential of CAR T therapy for relapsed or refractory pediatric and young adult B-cell ALL. Ther Clin Risk Manag. 2018;14:1573.
Li J, Li W, Huang K, Zhang Y, Kupfer G. Chimeric antigen receptor T cell (CAR-T) immunotherapy for solid tumors: lessons learned and strategies for moving forward. J Hematol Oncol. 2018;11:22.
Zhang J-P, Zhang R, Tsao S-T, Liu Y-C, Chen X, Lu D-P, et al. Sequential allogeneic and autologous CAR-T–cell therapy to treat an immune-compromised leukemic patient. Blood Adv. 2018;2:1691.
Bonifant CL, Jackson HJ, Brentjens RJ, Curran KJ. Toxicity and management in CAR T-cell therapy. Mol Ther Oncolytics. 2016;3:16011.
Levine BL, Miskin J, Wonnacott K, Keir C. Global manufacturing of CAR T cell therapy. Mol Ther Methods Clin Dev. 2017;4:92–101.
Scholler J, Brady TL, Binder-Scholl G, Hwang WT, Plesa G, Hege KM, et al. Decade-long safety and function of retroviral-modified chimeric antigen receptor T cells. Sci Transl Med. 2012;4:132ra53.
Maude SL, Laetsch TW, Buechner J, Rives S, Boyer M, Bittencourt H, et al. Tisagenlecleucel in children and young adults with B-cell lymphoblastic leukemia. N Engl J Med. 2018;378:439–48.
Turtle CJ, Hanafi L-A, Berger C, Hudecek M, Pender B, Robinson E, et al. Immunotherapy of non-Hodgkin’s lymphoma with a defined ratio of CD8+and CD4+CD19-specific chimeric antigen receptor–modified T cells. Sci Transl Med. 2016;8:355ra116–355ra116.
Porter DL, Levine BL, Kalos M, Bagg A. Chimeric antigen receptor–modified T cells in chronic lymphoid leukemia. N Engl J Med. 2011;365:725–33.
Van Der Stegen SJ, Hamieh M. The pharmacology of second-generation chimeric antigen receptors. Nat Rev Drug Disco. 2015;14:499–509.
Zhao Z, Condomines M, van der Stegen SJ, Perna F, Kloss CC, Gunset G, et al. Structural design of engineered costimulation determines tumor rejection kinetics and persistence of CAR T cells. Cancer Cell. 2015;28:415–28.
Amrolia PJ, Wynn R, Hough R, Vora A, Bonney D, Veys P, et al. Simultaneous trgeting of CD19 and CD22: phase I study of AUTO3, a bicistronic chimeric antigen receptor (CAR) T-cell therapy, in pediatric patients with relapsed/refractory B-cell acute lymphoblastic leukemia (r/r B-ALL): Amelia study. Blood. 2018;132(Supplement 1):279.
Wang Z, Han W. Biomarkers of cytokine release syndrome and neurotoxicity related to CAR-T cell therapy. Biomark Res. 2018;6:4.
Mahadeo KM, Khazal SJ, Abdel-Azim H, Fitzgerald JC, Taraseviciute A, Bollard CM, et al. Management guidelines for paediatric patients receiving chimeric antigen receptor T cell therapy. Nat Rev Clin Oncol. 2019;16:45–63.
Vora SB, Waghmare A, Englund JA, Qu P, Gardner RA, Hill JA. Infectious complications following CD19 chimeric antigen receptor T-cell therapy for children, adolescents and young adults. Open Forum Infect. Dis. 2020;7:ofaa121.
Fitzgerald JC, Weiss SL, Maude SL, Barrett DM, Lacey SF, Melenhorst JJ, et al. Cytokine release syndrome after chimeric antigen receptor T cell therapy for acute lymphoblastic leukemia. Crit Care Med. 2017;45:e124.
Frey NV, Shaw PA, Hexner EO, Pequignot E, Gill S, Luger SM, et al. Optimizing chimeric antigen receptor T-cell therapy for adults with acute lymphoblastic leukemia. J Clin Oncol. 2020;38:415–22.
Cordeiro A, Bezerra ED, Hill JA, Turtle CJ, Maloney DG, Bar M. Late effects of CD19-targeted CAR-T cell therapy. Blood. 2018;132:223.
Brentjens RJ, Davila ML, Riviere I, Park J, Wang X, Cowell LG, et al. CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci Transl Med. 2013;5:177ra38.
Kochenderfer JN, Dudley ME, Feldman SA, Wilson WH, Spaner DE, Maric I, et al. B-cell depletion and remissions of malignancy along with cytokine-associated toxicity in a clinical trial of anti-CD19 chimeric-antigen-receptor-transduced T cells. Blood. 2012;119 12:2709–20.
Brudno JN, Kochenderfer JN. Toxicities of chimeric antigen receptor T cells: recognition and management. Blood. 2016;127:3321–30.
Han X, Wang Y, Wei J. oncology. Multi-antigen-targeted chimeric antigen receptor T cells for cancer therapy. J Hematol Oncol. 2019;12:1–10.
Riaz IB, Zahid U, Kamal MU, Husnain M, McBride A, Hua A, et al. Anti-CD 19 and anti-CD 20 CAR-modified T cells for B-cell malignancies: a systematic review and meta-analysis. Immunotherapy. 2017;9:979–93.
Zah E, Lin MY, Silva-Benedict A, Jensen MC, Chen YYT. Cells Expressing CD19/CD20 bispecific chimeric antigen receptors prevent antigen escape by malignant B cells. Cancer. Immunol Res. 2016;4:498–508.
Cianferoni A, JJEroci Spergel. The importance of TSLP in allergic disease and its role as a potential therapeutic target. Expert Rev Clin Immunol. 2014;10:1463–74.
Tasian SK, Doral MY, Wood BL, Borowitz MJ, Collins-Underwood JR, Harvey RC, et al. Thymic stromal lymphopoietin stimulation of pediatric acute lymphoblastic leukemias with CRLF2 alterations induces JAK/STAT and PI3K phosphosignaling. Blood. 2010;116:410.
Shaltiel IA, Aprelia M, Saurin AT, Chowdhury D, Kops GJ, Voest EE, et al. Distinct phosphatases antagonize the p53 response in different phases of the cell cycle. Proc Natl Acad Sci USA. 2014;111:7313–8.
Qin H, Cho M, Haso W, Zhang L, Tasian SK, Oo HZ, et al. Eradication of B-ALL using chimeric antigen receptor–expressing T cells targeting the TSLPR oncoprotein. Blood. 2015;126:629–39.
Davies DM, Maher J. TLSPR: a new CAR in the showroom for B-ALL. Blood. 2015;126:567–9.
Gomes-Silva D, Srinivasan M, Sharma S, Lee CM, Wagner DL, Davis TH, et al. CD7-edited T cells expressing a CD7-specific CAR for the therapy of T-cell malignancies. Blood. 2017;130:285–96.
Fleischer LC, Spencer HT, Raikar SS. Targeting T cell malignancies using CAR-based immunotherapy: challenges and potential solutions. J Hematol Oncol. 2019;12:1–21.
Naik J, Themeli M, de Jong-Korlaar R, Ruiter RW, Poddighe PJ, Yuan H, et al. CD38 as a therapeutic target for adult acute myeloid leukemia and T-cell acute lymphoblastic leukemia. Haematologica. 2019;104:e100.
Mihara K, Yoshida T, Ishida S, Takei Y, Kitanaka A, Shimoda K, et al. All-trans retinoic acid and interferon-α increase CD38 expression on adult T-cell leukemia cells and sensitize them to T cells bearing anti-CD38 chimeric antigen receptors. Blood Cancer J. 2016;6:e421–e.
Hofmann S, Schubert M-L, Wang L, He B, Neuber B, Dreger P, et al. Chimeric antigen receptor (CAR) T cell therapy in acute myeloid leukemia (AML). J Clin Med. 2019;8:200.
Smith AJ, Oertle J, Warren D.PratoD. Chimeric antigen receptor (CAR) T cell therapy for malignant cancers: Summary and perspective. J Cell Immunother. 2016;2:59–68.
Turtle CJ, Hay KA, Hanafi L-A, Li D, Cherian S, Chen X, et al. Durable molecular remissions in chronic lymphocytic leukemia treated with CD19-specific chimeric antigen receptor–modified T cells after failure of ibrutinib. J Clin Oncol. 2017;35:3010.
Kochenderfer JN, Dudley ME, Kassim SH, Somerville RP, Carpenter RO, Stetler-Stevenson M, et al. Chemotherapy-refractory diffuse large B-cell lymphoma and indolent B-cell malignancies can be effectively treated with autologous T cells expressing an anti-CD19 chimeric antigen receptor. J Clin Oncol. 2015;33:540.
Brentjens RJ, Riviere I, Park JH, Davila ML, Wang X, Stefanski J, et al. Safety and persistence of adoptively transferred autologous CD19-targeted T cells in patients with relapsed or chemotherapy refractory B-cell leukemias. Blood. 2011;118:4817–28.
Park JH, Rivière I, Gonen M, Wang X, Sénéchal B, Curran KJ, et al. Long-term follow-up of CD19 CAR therapy in acute lymphoblastic leukemia. N Engl J Med. 2018;378:449–59.
Yang J, Jiang P, Zhang X, Zhu X, Dong Q, He J, et al. Anti-CD19/CD22 dual CAR-T therapy for refractory and relapsed B-cell acute lymphoblastic leukemia. Blood. 2019;134:284.
Gu R, Liu F, Zou D, Xu Y, Lu Y, Liu B, et al. Efficacy and safety of CD19 CAR T constructed with a new anti-CD19 chimeric antigen receptor in relapsed or refractory acute lymphoblastic leukemia. J Hematol Oncol. 2020;13:1–13.
Annesley C, Summers C, Pulsipher MA, Wayne AS, Rivers J, Lamble AJ, et al. Clinical experience of CAR T cell immunotherapy for relapsed and refractory infant ALL demonstrates feasibility and favorable responses. Blood. 2019;134:3869.
Zheng PP, Kros JM, Li J. Approved CAR T cell therapies: ice bucket challenges on glaring safety risks and long-term impacts. Drug Discov Today. 2018;23:1175–82.
Gupta S, Seethapathy H, Strohbehn IA, Frigault MJ, O’Donnell EK, Jacobson CA, et al. Acute kidney injury and electrolyte abnormalities after chimeric antigen receptor T-cell (CAR-T) therapy for diffuse large B-cell lymphoma. Am J Kidney Dis. 2020;76:63–71.
Li D, Li X, Zhou W-L, Huang Y, Liang X, Jiang L, et al. Genetically engineered T cells for cancer immunotherapy. Signal Transduct Target Ther. 2019;4:1–17.
Lee DW, Gardner R, Porter DL, Louis CU, Ahmed N, Jensen M, et al. Current concepts in the diagnosis and management of cytokine release syndrome. Blood 2014;124:188–95.
Lee D, Santomasso B, Locke F, Ghobadi A, Turtle CJ, Brudno JN, et al. ASTCT consensus grading for cytokine release syndrome and neurologic toxicity associated with immune effector cells. Biol Blood Marrow Transpl. 2019;25:625–38.
Locke FL, Neelapu SS, Bartlett NL, Siddiqi T, Chavez JC, Hosing CM, et al. Phase 1 results of ZUMA-1: a multicenter study of KTE-C19 anti-CD19 CAR T cell therapy in refractory aggressive lymphoma. Mol Ther. 2017;25:285–95.
Hay KA, Hanafi L-A, Li D, Gust J, Liles CW, Wurfel MM, et al. Kinetics and biomarkers of severe cytokine release syndrome after CD19 chimeric antigen receptor–modified T-cell therapy. Blood. 2017;130:2295–306.
Shimabukuro-Vornhagen A, Gödel P, Subklewe M, Stemmler HJ, Schlößer HA, Schlaak M, et al. Cytokine release syndrome. J Immunother Cancer. 2018;6:56.
Hunter CA, Jones SA. IL-6 as a keystone cytokine in health and disease. Nat Immunol. 2015;16:448–57.
Teachey DT, Lacey SF, Shaw PA, Melenhorst JJ, Maude SL, Frey N, et al. Identification of predictive biomarkers for cytokine release syndrome after chimeric antigen receptor T-cell therapy for acute lymphoblastic leukemia. Cancer Disco. 2016;6:664–79.
Sandler RD, Tattersall RS, Schoemans H, Greco R, Badoglio M, Labopin M, et al. Diagnosis and management of secondary HLH/MAS following HSCT and CAR-T cell therapy in adults; a review of the literature and a survey of practice within EBMT centres on behalf of the autoimmune diseases working party (ADWP) and transplant complications working party (TCWP). Front Immunol. 2020;11:524.
Ishii K, Shalabi H, Yates B, Delbrook C, Mackall CL, Fry TJ, et al. Tocilizumab-refractory cytokine release syndrome (CRS) triggered by chimeric antigen receptor (CAR)-transduced T cells may have distinct cytokine profiles compared to typical CRS. Blood. 2016;128:3358.
Major A, Collins J, Craney C, Heitman AK, Bauer E, Zerante E, et al. Management of hemophagocytic lymphohistiocytosis (HLH) associated with chimeric antigen receptor T-cell (CAR-T) therapy using anti-cytokine therapy: an illustrative case and review of the literature. Leuk Lymphoma. 2021;62:1765–9.
Shah NN, Highfill SL, Shalabi H, Yates B, Jin J, Wolters PL, et al. CD4/CD8 T-cell selection affects chimeric antigen receptor (CAR) T-cell potency and toxicity: updated results from a phase I anti-CD22 CAR T-cell trial. J Clin Oncol. 2020;38:1938–50.
Neelapu SS, Tummala S, Kebriaei P, Wierda W, Gutierrez C, Locke FL, et al. Chimeric antigen receptor T-cell therapy - assessment and management of toxicities. Nat Rev Clin Oncol. 2018;15:47–62.
Henter JI, Horne A, Aricó M, Egeler RM, Filipovich AH, Imashuku S, et al. HLH-2004: diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer. 2007;48:124–31.
Jordan MB, Allen CE, Weitzman S, Filipovich AH, McClain KL. How I treat hemophagocytic lymphohistiocytosis. Blood. 2011;118:4041–52.
Schram AM, Berliner N. How I treat hemophagocytic lymphohistiocytosis in the adult patient. Blood. 2015;125:2908–14.
Karschnia P, Jordan JT, Forst DA, Arrillaga-Romany IC, Batchelor TT, Baehring JM, et al. Clinical presentation, management, and biomarkers of neurotoxicity after adoptive immunotherapy with CAR T cells. Blood. 2019;133:2212–21.
Gust J, Hay KA, Hanafi L-A, Li D, Myerson D, Gonzalez-Cuyar LF, et al. Endothelial activation and blood-brain barrier disruption in neurotoxicity after adoptive immunother- apy with CD19 CAR-T cells. Cancer Disco. 2017;7:1404–19.
Locke FL, Neelapu SS, Bartlett NL, Lekakis LJ, Jacobson CA, Braunschweig I, et al. Preliminary results of prophylactic tocilizumab after axicabtageneciloleucel (axi-cel; KTE-C19) treatment for patients with refractory, aggressive non-Hodgkin lymphoma (NHL). Blood 2017;130:1547.
Mian A, Hill BT. Brexucabtagene autoleucel for the treatment of relapsed/refractory mantle cell lymphoma. Expert Opinion on Biological Therapy. 2021;21:435–41.
CRS CRS, NT NT, Lymphohistiocytosis H. US Food and Drug Administration approves Bristol Myers Squibb’s and bluebird bio’s Abecma (idecabtagene vicleucel), the first anti-BCMA CAR T cell therapy for relapsed or refractory multiple myeloma. Abecma is a first-in-class BCMA-directed personalized immune cell therapy delivered as a one-time infusion for triple-class exposed patients with multiple survival. 2021;5:11-2.
Albinger N, Hartmann J, Ullrich E. Current status and perspective of CAR-T and CAR-NK cell therapy trials in Germany. Gene Ther. 2021;28:513–27.
Zheng P-P, Kros JM, Li J. Approved CAR T cell therapies: ice bucket challenges on glaring safety risks and long-term impacts. Drug Discov Today. 2018;23:1175–82.
Prasad V. Immunotherapy: Tisagenlecleucel—the first approved CAR-T-cell therapy: implications for payers and policy makers. Nat Rev Clin Oncol. 2018;15:11.
Xu D, Jin G, Chai D, Zhou X, Gu W, Chong Y, et al. The development of CAR design for tumor CAR-T cell therapy. Oncotarget. 2018;9:13991.
Boyer MW. Chimeric antigen receptor T-cell therapy hits the market. Immunotherapy. 2018;10:911–2. https://doi.org/10.2217/imt-2018-0075
Braendstrup P, Levine BL, Ruella MJC. The long road to the first FDA-approved gene therapy: chimeric antigen receptor T cells targeting CD19. Cytotherapy 2020;22:57–69.
Akhoundi M, Mohammadi M, Sahraei SS, Sheykhhasan M, Fayazi N. CAR T cell therapy as a promising approach in cancer immunotherapy: challenges and opportunities. Cell Oncol. 2021;44:495–53.
Whittington MD, McQueen R, Ollendorf DA, Kumar VM, Chapman RH, Tice JA, et al. Long-term survival and value of chimeric antigen receptor t-cell therapy for pediatric patients with relapsed or refractory leukemia. JAMA Pediatrics. 2018;172:1161–68.
Zhao Z, Chen Y, Francisco NM, Zhang Y, Wu M. The application of CAR-T cell therapy in hematological malignancies: advantages and challenges. Acta Pharmaceutica Sin B 2018;8:539–51.
Ramos CA, Heslop HE, Brenner MK. CAR-T cell therapy for lymphoma. Annu Rev Med. 2016;67:165–83.
Bonini C, Mondino A. Adoptive T‐cell therapy for cancer: the era of engineered T cells. Eur J Immunol. 2015;45:2457–69.
Catalán E, Charni S, Jaime P, Aguiló JI, Enríquez JA, Naval J, et al. MHC-I modulation due to changes in tumor cell metabolism regulates tumor sensitivity to CTL and NK cells. Oncoimmunology. 2015;4:e985924.
Hillerdal V, Essand M. Chimeric antigen receptor-engineered T cells for the treatment of metastatic prostate cancer. BioDrugs. 2015;29:75–89.
Duong CP, Yong CS, Kershaw MH, Slaney CY, Darcy PK. Cancer immunotherapy utilizing gene-modified T cells: from the bench to the clinic. Mol Immunol. 2015;67:46–57.
Xu X, Sun Q, Liang X, Chen Z, Zhang X, Zhou X, et al. Mechanisms of relapse after CD19 CAR T-cell therapy for acute lymphoblastic leukemia and its prevention and treatment strategies. Front Immunol. 2019;10:2664.
Bagashev A, Sotillo E, Tang C-HA, Black KL, Perazzelli J, Seeholzer SH, et al. CD19 alterations emerging after CD19-directed immunotherapy cause retention of the misfolded protein in the endoplasmic reticulum. Mol Cell Biol. 2018;38:e00383–18.
Evans AG, Rothberg PG, Burack WR, Huntington SF, Porter DL, Friedberg JW, et al. Evolution to plasmablastic lymphoma evades CD19‐directed chimeric antigen receptor T cells. Br J Haematol. 2015;171:205–9.
Gardner R, Wu D, Cherian S, Fang M, Hanafi L-A, Finney O, et al. Acquisition of a CD19-negative myeloid phenotype allows immune escape of MLL-rearranged B-ALL from CD19 CAR-T-cell therapy. Blood. 2016;127:2406–10.
Oberley MJ, Gaynon PS, Bhojwani D, Pulsipher MA, Gardner RA, Hiemenz MC, et al. Myeloid lineage switch following chimeric antigen receptor T‐cell therapy in a patient with TCF3‐ZNF384 fusion‐positive B‐lymphoblastic leukemia. Pediatr Blood Cancer. 2018;65:e27265.
Ruella M, Xu J, Barrett DM, Fraietta JA, Reich TJ, Ambrose DE, et al. Induction of resistance to chimeric antigen receptor T cell therapy by transduction of a single leukemic B cell. Nat Med. 2018;24:1499–503.
Fry TJ, Shah NN, Orentas RJ, Stetler-Stevenson M, Yuan CM, Ramakrishna S, et al. CD22-CAR T cells induce remissions in CD19-CAR naïve and resistant B-ALL. Nat Med. 2018;24:20.
Watanabe K, Terakura S, Martens AC, Van Meerten T, Uchiyama S, Imai M, et al. Target antigen density governs the efficacy of anti–CD20-CD28-CD3 ζ chimeric antigen receptor–modified effector CD8+ T cells. J Immunol. 2015;194:911–20.
Walker AJ, Majzner RG, Zhang L, Wanhainen K, Long AH, Nguyen SM, et al. Tumor antigen and receptor densities regulate efficacy of a chimeric antigen receptor targeting anaplastic lymphoma kinase. Mol Ther. 2017;25:2189–201.
Majzner RG, Mackall CL. Tumor antigen escape from CAR T-cell therapy. Cancer Disco. 2018;8:1219–26.
Hombach AA, Görgens A, Chmielewski M, Murke F, Kimpel J, Giebel B, et al. Superior therapeutic index in lymphoma therapy: CD30+ CD34+hematopoietic stem cells resist a chimeric antigen receptor T-cell attack. Mol Ther. 2016;24:1423–34.
Sun K, Zhang X, Wang Z, Chen Y, Zhang L, Cheng W, et al. Allogeneic CAR-T cell therapy for treatment of relapse after Allo-HSCT in patients with refractory CML lymphoid blast crisis: significance of HLA matched donor/patient pair in the safety/efficacy of CAR-T cell therapy. Blood. 2018;132:4275.
Zhao J, Song Y, Liu D. Clinical trials of dual-target CAR T cells, donor-derived CAR T cells, and universal CAR T cells for acute lymphoid leukemia. J Hematol Oncol. 2019;12:17.
Xu J, Wang X, Chen J, Chen S, Li Z, Liu H, et al.Embryonic stem cell-derived mesenchymal stem cells promote colon epithelial integrity and regeneration by elevating circulating IGF-1 colitis mice. 2020;10:12204.
Steineck A, Wiener L, Mack JW, Shah NN, Summers C, Rosenberg AR. Psychosocial care for children receiving chimeric antigen receptor (CAR) T‐cell therapy. Pediatr Blood Cancer. 2020;67:e28249
England SS. NHS England to fund CAR-T for childhood leukaemia. PharmacoEconomics Outcomes News. 2018;812:37–22.
Pan J, Niu Q, Deng B, Liu S, Wu T, Gao Z, et al. CD22 CAR T-cell therapy in refractory or relapsed B acute lymphoblastic leukemia. Leukemia. 2019;33:2854–66.
Curran KJ, Margossian S, Kernan NA, Silverman LB, Williams DA, Shukla NN, et al. Toxicity and response following CD19-specific CAR T cells in pediatric/young adult relapsed/refractory B-ALL. Blood. 2019;134:2361–8.
Hay KA, Gauthier J, Hirayama AV, Voutsinas JM, Wu Q, Li D, et al. Factors associated with durable EFS in adult B-cell ALL patients achieving MRD-negative CR after CD19 CAR T-cell therapy. Blood. 2019;133:1652–63.
Zhao R, Cui Y, Li S, Qin L, Li P. Current status and hurdles for CAR-T cell immune therapy. Blood Sci. 2019;1:148–55.
Guo Y, Feng K, Tong C, Jia H, Liu Y, Wang Y, et al. Efficiency and side effects of anti-CD38 CAR T cells in an adult patient with relapsed B-ALL after failure of bi-specific CD19/CD22 CAR T cell treatment. Cell Mol Immunol. 2020;17:430–2.
Rajkumar SV. Value and cost of myeloma therapy. Am Soc Clin Oncol Educ Book. 2018;38:662–6.
Xu X, Huang S, Xiao X, Sun Q, Liang X, Chen S, et al. Challenges and clinical strategies of CAR T-cell therapy for acute lymphoblastic leukemia: overview and developments. Front Immunol. 2020;11:569117.
Shah NN, Maatman T, Hari P, Johnson B. Multi targeted CAR-T cell therapies for B-cell malignancies. Front Oncol. 2019;9:146.
Fousek K, Watanabe J, Joseph SK, George A, An X, Byrd TT, et al. CAR T-cells that target acute B-lineage leukemia irrespective of CD19 expression. Leukemia. 2021;35:75–89.
Dai H, Wu Z, Jia H, Tong C, Guo Y, Ti D, et al. Bispecific CAR-T cells targeting both CD19 and CD22 for therapy of adults with relapsed or refractory B cell acute lymphoblastic leukemia. J Hematol Oncol. 2020;13:30.
Hua J, Qian W, Wu X, Zhou L, Yu L, Chen S, et al. Sequential infusion of anti-CD22 and anti-CD19 chimeric antigen receptor T cells for a pediatric Ph-like B-ALL patient that relapsed after CART-cell and Haplo-HSCT therapy: a case report and review of literature. Onco Targets Ther. 2020;13:2311–7.
Liu J, Zhong JF, Zhang X, Zhang C. Allogeneic CD19-CAR-T cell Infus allogeneic hematopoietic stem cell transplant B cell malignancies. J Hematol Oncol. 2017;10:35.
Ombrello A, Yates B, Shalabi H, Fry T, Shah N. Experience with and management of HLH-like toxicities following chimeric antigen receptor T-cell therapy for treatment of relapsed/refractory pre-B ALL. Arthritis Rheumatol. 2020;72:16–7.
Morgan MA, Schambach A. Engineering CAR-T cells for improved function against solid tumors. Front Immunol. 2018;9:2493.
Knaus HA, Kanakry CG, Luznik L, Gojo I. Immunomodulatory drugs: immune checkpoint agents in acute leukemia. Curr. Drug Targets. 2017;18:315–31.
Liu X, Ranganathan R, Jiang S, Fang C, Sun J, Kim S, et al. A chimeric switch-receptor targeting PD1 augments the efficacy of second-generation CAR T cells in advanced solid tumors. Cancer Res. 2016;76:1578–90.
Yoon DH, Osborn MJ, Tolar J, Kim CJ. Incorporation of immune checkpoint blockade into chimeric antigen receptor T cells (CAR-Ts): combination or built-in CAR-T. Int J Mol Sci. 2018;19:340.
Savojipour S, Assari Arani A, Agheli L, Hassanzadeh A. The determinants of urban families’ health expenditure. J Economic Policy. 2018;10:25–52.
Boucher JC, Li G, Shrestha B, Zhang Y, Vishwasrao P, Cabral ML, et al. Mutation of the CD28 costimulatory domain confers increased CAR T cell persistence and decreased exhaustion. Am Assoc Immnol. 2018;200.
Yeku OO, Purdon TJ, Koneru M, Spriggs D, Brentjens RJ. Armored CAR T cells enhance antitumor efficacy and overcome the tumor microenvironment. Sci Rep. 2017;7:10541
Jaspers JE, Brentjens RJ. Development of CAR T cells designed to improve antitumor efficacy and safety. Pharm Ther. 2017;178:83–91.
Ghorashian S, Kramer AM, Onuoha S, Wright G, Bartram J, Richardson R, et al. Enhanced CAR T cell expansion and prolonged persistence in pediatric patients with ALL treated with a low-affinity CD19 CAR. Nat Med. 2019;25:1408–14.
Ghorashian S, Kramer AM, Onuoha S, Wright G, Bartram JL, Richardson R, et al. Therapy of paediatric B-ALL with a fast off rate CD19 CAR leads to enhanced expansion and prolonged CAR T cell persistence in patients with low bone marrow tumour burden, and is associated with a favourable toxicity profile. Blood. 2019;134:225
Acknowledgements
We express my deepest gratitude to Mrs. Farzaneh Chitsaz for her help in figure preparation.
Author information
Authors and Affiliations
Contributions
MS and PD designed the concept. MS, HM, and PD searched the literature. MS, HM, and PD wrote the manuscript. MS created the figures. PD revised the manuscript. The authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sheykhhasan, M., Manoochehri, H. & Dama, P. Use of CAR T-cell for acute lymphoblastic leukemia (ALL) treatment: a review study. Cancer Gene Ther 29, 1080–1096 (2022). https://doi.org/10.1038/s41417-021-00418-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41417-021-00418-1
This article is cited by
-
CAR T therapies in multiple myeloma: unleashing the future
Cancer Gene Therapy (2024)
-
Harnessing the potential of CAR-T cell therapy: progress, challenges, and future directions in hematological and solid tumor treatments
Journal of Translational Medicine (2023)
-
Intestinal barrier functions in hematologic and oncologic diseases
Journal of Translational Medicine (2023)
-
Modern treatment strategies in pediatric oncology and hematology
Discover Oncology (2023)
-
Boric Acid Affects Cell Proliferation, Apoptosis, and Oxidative Stress in ALL Cells
Biological Trace Element Research (2023)