Abstract
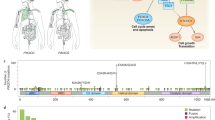
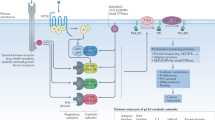
Phosphoinositide 3-kinases (PI3Ks) play a central role in tumourigenesis with recurrent activating mutations of its p110α subunit (PIK3CA) identified in several tumours. Although several PI3K inhibitors are approved for haematological malignancies, only alpelisib was approved in solid tumours and for the treatment of PIK3CA-related overgrowth spectrum (PROS) syndrome. Traditional PI3K inhibitors inhibit both wild-type and mutant PI3K with almost equal potency, thus limiting their efficacy due to on-target toxicity. Since the initiation of phase I clinical trials investigating next generation allosteric mutant and isoform selective PIK3CA inhibitors, there has been a surge in interest in PIK3CA targeting in solid tumours. Preclinical characterisation of these compounds showed that maximal mutant protein inhibition fails to elicit metabolic and glucose homoeostasis dysregulation, one of the dose limiting toxicities of both selective and pan PI3K inhibitors. While extreme selectivity can be hypothesised to grant activity and safety advantage to these novel agents, on the other hand reduced benefit can be speculated for patients harbouring multiple or rare PIK3CA mutations. This review summarises the current understanding of PI3K alterations and the state-of-the-art treatment strategies in PI3K driven solid tumours, while also exploring the potential intrinsic and acquired resistance mechanisms to these agents, and the emerging role of mutant selective PIK3CA inhibitors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Not applicable.
References
Samuels Y, Wang Z, Bardelli A, Silliman N, Ptak J, Szabo S, et al. High frequency of mutations of the PIK3CA gene in human cancers. Science. 2004;304:554. https://doi.org/10.1126/science.1096502
Zhang Y, Kwok-Shing Ng P, Kucherlapati M, Chen F, Liu Y, Tsang YH, et al. A pan-cancer proteogenomic atlas of PI3K/AKT/mTOR pathway alterations. Cancer Cell. 2017;31:820.e3–32.e3. https://doi.org/10.1016/j.ccell.2017.04.013
Zehir A, Benayed R, Shah RH, Syed A, Middha S, Kim HR, et al. Mutational landscape of metastatic cancer revealed from prospective clinical sequencing of 10,000 patients. Nat Med. 2017;23:703–13. https://doi.org/10.1038/nm.4333
Janku F, Yap TA, Meric-Bernstam F. Targeting the PI3K pathway in cancer: are we making headway. Nat Rev Clin Oncol. 2018;15:273–91. https://doi.org/10.1038/nrclinonc.2018.28
Petroni G, Buque A, Zitvogel L, Kroemer G, Galluzzi L. Immunomodulation by targeted anticancer agents. Cancer Cell. 2021;39:310–45. https://doi.org/10.1016/j.ccell.2020.11.009
Andre F, Ciruelos E, Rubovszky G, Campone M, Loibl S, Rugo HS, et al. Alpelisib for PIK3CA-mutated, hormone receptor-positive advanced breast cancer. N Engl J Med. 2019;380:1929–40. https://doi.org/10.1056/NEJMoa1813904
Keppler-Noreuil KM, Sapp JC, Lindhurst MJ, Parker VE, Blumhorst C, Darling T, et al. Clinical delineation and natural history of the PIK3CA-related overgrowth spectrum. Am J Med Genet A. 2014;164A:1713–33. https://doi.org/10.1002/ajmg.a.36552
McGranahan N, Swanton C. Clonal heterogeneity and tumor evolution: past, present, and the future. Cell. 2017;168:613–28. https://doi.org/10.1016/j.cell.2017.01.018
Jaiswal BS, Janakiraman V, Kljavin NM, Chaudhuri S, Stern HM, Wang W, et al. Somatic mutations in p85alpha promote tumorigenesis through class IA PI3K activation. Cancer Cell. 2009;16:463–74. https://doi.org/10.1016/j.ccr.2009.10.016
Gerstung M, Jolly C, Leshchiner I, Dentro SC, Gonzalez S, Rosebrock D, et al. The evolutionary history of 2,658 cancers. Nature. 2020;578:122–8. https://doi.org/10.1038/s41586-019-1907-7
Andre F, Ciruelos EM, Juric D, Loibl S, Campone M, Mayer IA, et al. Alpelisib plus fulvestrant for PIK3CA-mutated, hormone receptor-positive, human epidermal growth factor receptor-2-negative advanced breast cancer: final overall survival results from SOLAR-1. Ann Oncol. 2021;32:208–17. https://doi.org/10.1016/j.annonc.2020.11.011
Andre F, Hurvitz S, Fasolo A, Tseng LM, Jerusalem G, Wilks S, et al. Molecular alterations and everolimus efficacy in human epidermal growth factor receptor 2-overexpressing metastatic breast cancers: combined exploratory biomarker analysis from BOLERO-1 and BOLERO-3. J Clin Oncol. 2016;34:2115–24. https://doi.org/10.1200/JCO.2015.63.9161
Mosele F, Stefanovska B, Lusque A, Tran Dien A, Garberis I, Droin N, et al. Outcome and molecular landscape of patients with PIK3CA-mutated metastatic breast cancer. Ann Oncol. 2020;31:377–86. https://doi.org/10.1016/j.annonc.2019.11.006
Baselga J, Cortes J, Kim SB, Im SA, Hegg R, Im YH, et al. Pertuzumab plus trastuzumab plus docetaxel for metastatic breast cancer. N Engl J Med. 2012;366:109–19. https://doi.org/10.1056/NEJMoa1113216
Baselga J, Campone M, Piccart M, Burris HA 3rd, Rugo HS, Sahmoud T, et al. Everolimus in postmenopausal hormone-receptor-positive advanced breast cancer. N Engl J Med. 2012;366:520–9. https://doi.org/10.1056/NEJMoa1109653
Ogino S, Nosho K, Kirkner GJ, Shima K, Irahara N, Kure S, et al. PIK3CA mutation is associated with poor prognosis among patients with curatively resected colon cancer. J Clin Oncol. 2009;27:1477–84. https://doi.org/10.1200/JCO.2008.18.6544
De Roock W, Claes B, Bernasconi D, De Schutter J, Biesmans B, Fountzilas G, et al. Effects of KRAS, BRAF, NRAS, and PIK3CA mutations on the efficacy of cetuximab plus chemotherapy in chemotherapy-refractory metastatic colorectal cancer: a retrospective consortium analysis. Lancet Oncol. 2010;11:753–62. https://doi.org/10.1016/S1470-2045(10)70130-3
Mao C, Yang ZY, Hu XF, Chen Q, Tang JL. PIK3CA exon 20 mutations as a potential biomarker for resistance to anti-EGFR monoclonal antibodies in KRAS wild-type metastatic colorectal cancer: a systematic review and meta-analysis. Ann Oncol. 2012;23:1518–25. https://doi.org/10.1093/annonc/mdr464
Huang L, Liu Z, Deng D, Tan A, Liao M, Mo Z, et al. Anti-epidermal growth factor receptor monoclonal antibody-based therapy for metastatic colorectal cancer: a meta-analysis of the effect of PIK3CA mutations in KRAS wild-type patients. Arch Med Sci. 2014;10:1–9. https://doi.org/10.5114/aoms.2014.40728
Liu P, Cheng H, Roberts TM, Zhao JJ. Targeting the phosphoinositide 3-kinase pathway in cancer. Nat Rev Drug Discov. 2009;8:627–44. https://doi.org/10.1038/nrd2926
Stransky N, Cerami E, Schalm S, Kim JL, Lengauer C. The landscape of kinase fusions in cancer. Nat Commun. 2014;5:4846. https://doi.org/10.1038/ncomms5846
Croessmann S, Sheehan JH, Lee KM, Sliwoski G, He J, Nagy R, et al. PIK3CA C2 domain deletions hyperactivate phosphoinositide 3-kinase (PI3K), generate oncogene dependence, and are exquisitely sensitive to PI3Kalpha inhibitors. Clin Cancer Res. 2018;24:1426–35. https://doi.org/10.1158/1078-0432.CCR-17-2141
Krop IE, Mayer IA, Ganju V, Dickler M, Johnston S, Morales S, et al. Pictilisib for oestrogen receptor-positive, aromatase inhibitor-resistant, advanced or metastatic breast cancer (FERGI): a randomised, double-blind, placebo-controlled, phase 2 trial. Lancet Oncol. 2016;17:811–21. https://doi.org/10.1016/S1470-2045(16)00106-6
Vuylsteke P, Huizing M, Petrakova K, Roylance R, Laing R, Chan S, et al. Pictilisib PI3Kinase inhibitor (a phosphatidylinositol 3-kinase [PI3K] inhibitor) plus paclitaxel for the treatment of hormone receptor-positive, HER2-negative, locally recurrent, or metastatic breast cancer: interim analysis of the multicentre, placebo-controlled, phase II randomised PEGGY study. Ann Oncol. 2016;27:2059–66. https://doi.org/10.1093/annonc/mdw320
Matulonis U, Vergote I, Backes F, Martin LP, McMeekin S, Birrer M, et al. Phase II study of the PI3K inhibitor pilaralisib (SAR245408; XL147) in patients with advanced or recurrent endometrial carcinoma. Gynecol Oncol. 2015;136:246–53. https://doi.org/10.1016/j.ygyno.2014.12.019
Levy B, Spira A, Becker D, Evans T, Schnadig I, Camidge DR, et al. A randomized, phase 2 trial of Docetaxel with or without PX-866, an irreversible oral phosphatidylinositol 3-kinase inhibitor, in patients with relapsed or metastatic non-small-cell lung cancer. J Thorac Oncol. 2014;9:1031–5. https://doi.org/10.1097/JTO.0000000000000183
Jimeno A, Bauman JE, Weissman C, Adkins D, Schnadig I, Beauregard P, et al. A randomized, phase 2 trial of docetaxel with or without PX-866, an irreversible oral phosphatidylinositol 3-kinase inhibitor, in patients with relapsed or metastatic head and neck squamous cell cancer. Oral Oncol. 2015;51:383–8. https://doi.org/10.1016/j.oraloncology.2014.12.013
Di Leo A, Johnston S, Lee KS, Ciruelos E, Lonning PE, Janni W, et al. Buparlisib plus fulvestrant in postmenopausal women with hormone-receptor-positive, HER2-negative, advanced breast cancer progressing on or after mTOR inhibition (BELLE-3): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2018;19:87–100. https://doi.org/10.1016/S1470-2045(17)30688-5
Baselga J, Im SA, Iwata H, Cortes J, De Laurentiis M, Jiang Z, et al. Buparlisib plus fulvestrant versus placebo plus fulvestrant in postmenopausal, hormone receptor-positive, HER2-negative, advanced breast cancer (BELLE-2): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2017;18:904–16. https://doi.org/10.1016/S1470-2045(17)30376-5
Martin M, Chan A, Dirix L, O’Shaughnessy J, Hegg R, Manikhas A, et al. A randomized adaptive phase II/III study of buparlisib, a pan-class I PI3K inhibitor, combined with paclitaxel for the treatment of HER2- advanced breast cancer (BELLE-4). Ann Oncol. 2017;28:313–20. https://doi.org/10.1093/annonc/mdw562
Soulieres D, Faivre S, Mesia R, Remenar E, Li SH, Karpenko A, et al. Buparlisib and paclitaxel in patients with platinum-pretreated recurrent or metastatic squamous cell carcinoma of the head and neck (BERIL-1): a randomised, double-blind, placebo-controlled phase 2 trial. Lancet Oncol. 2017;18:323–35. https://doi.org/10.1016/S1470-2045(17)30064-5
Damodaran S, Zhao F, Deming DA, Mitchell EP, Wright JJ, Gray RJ, et al. Phase II study of copanlisib in patients with tumors with PIK3CA mutations: results from the NCI-MATCH ECOG-ACRIN Trial (EAY131) Subprotocol Z1F. J Clin Oncol. 2022:40:1552–61. https://doi.org/10.1200/JCO.21.01648
Narayan P, Prowell TM, Gao JJ, Fernandes LL, Li E, Jiang X, et al. FDA approval summary: alpelisib plus fulvestrant for patients with HR-positive, HER2-negative, PIK3CA-mutated, advanced or metastatic breast cancer. Clin Cancer Res. 2021;27:1842–9. https://doi.org/10.1158/1078-0432.CCR-20-3652
Toska E, Castel P, Chhangawala S, Arruabarrena-Aristorena A, Chan C, Hristidis VC, et al. PI3K inhibition activates SGK1 via a feedback loop to promote chromatin-based regulation of ER-dependent gene expression. Cell Rep. 2019;27:294.e5–306.e5. https://doi.org/10.1016/j.celrep.2019.02.111
Toska E, Osmanbeyoglu HU, Castel P, Chan C, Hendrickson RC, Elkabets M, et al. PI3K pathway regulates ER-dependent transcription in breast cancer through the epigenetic regulator KMT2D. Science. 2017;355:1324–30. https://doi.org/10.1126/science.aah6893
Bosch A, Li Z, Bergamaschi A, Ellis H, Toska E, Prat A, et al. PI3K inhibition results in enhanced estrogen receptor function and dependence in hormone receptor-positive breast cancer. Sci Transl Med. 2015;7:283ra51. https://doi.org/10.1126/scitranslmed.aaa4442
Rugo HS, Lerebours F, Ciruelos E, Drullinsky P, Ruiz-Borrego M, Neven P, et al. Alpelisib plus fulvestrant in PIK3CA-mutated, hormone receptor-positive advanced breast cancer after a CDK4/6 inhibitor (BYLieve): one cohort of a phase 2, multicentre, open-label, non-comparative study. Lancet Oncol. 2021;22:489–98. https://doi.org/10.1016/S1470-2045(21)00034-6
Wei X, Liu J, Zhao H, Zhang Y, Liu Q, Zou B, et al. 33O A phase I study to evaluate safety, pharmacokinetics (PK), and preliminary efficacy of CYH33, a phosphatidylinositol 3-kinase α (PI3Kα) inhibitor, in patients (pts) with advanced solid tumours. Ann Oncol. 2021;32:S14.
Herrera-Abreu MT, Palafox M, Asghar U, Rivas MA, Cutts RJ, Garcia-Murillas I, et al. Early adaptation and acquired resistance to CDK4/6 inhibition in estrogen receptor-positive breast cancer. Cancer Res. 2016;76:2301–13. https://doi.org/10.1158/0008-5472.CAN-15-0728
Bedard PL, Davies MA, Kopetz S, Juric D, Shapiro GI, Luke JJ, et al. First-in-human trial of the PI3Kbeta-selective inhibitor SAR260301 in patients with advanced solid tumors. Cancer. 2018;124:315–24. https://doi.org/10.1002/cncr.31044
Jung M, Kim C, Kim H, Lee C, Lee H, Bae W, et al. SO-10 An open-label, multi-centre, phase Ib/II study of PI3Kβ selective inhibitor GSK2636771 administered in combination with paclitaxel in patients with advanced gastric cancer having alterations in PI3K/Akt pathway. Ann Oncol. 2021;32:S206 https://doi.org/10.1016/j.annonc.2021.05.034
Vanhaesebroeck B, Guillermet-Guibert J, Graupera M, Bilanges B. The emerging mechanisms of isoform-specific PI3K signalling. Nat Rev Mol Cell Biol. 2010;11:329–41. https://doi.org/10.1038/nrm2882
Hamilton E, Lee A, Swart R, Newton G, O’Connell B, Roberts J, et al. Abstract PS11-32: Mario-3 phase II study safety run-in evaluating a novel triplet combination of eganelisib (formerly IPI-549), atezolizumab (atezo), and nab-paclitaxel (nab-pac) as first-line (1L) therapy for locally advanced or metastatic triple-negative breast cancer (TNBC). Cancer Res. 2021;81:PS11-32–PS11-32. https://doi.org/10.1158/1538-7445.Sabcs20-ps11-32
Furman RR, Sharman JP, Coutre SE, Cheson BD, Pagel JM, Hillmen P, et al. Idelalisib and rituximab in relapsed chronic lymphocytic leukemia. N Engl J Med. 2014;370:997–1007. https://doi.org/10.1056/NEJMoa1315226
Juric D, Krop I, Ramanathan RK, Wilson TR, Ware JA, Sanabria Bohorquez SM, et al. Phase I dose-escalation study of taselisib, an oral PI3K inhibitor, in patients with advanced solid tumors. Cancer Discov. 2017;7:704–15. https://doi.org/10.1158/2159-8290.CD-16-1080
Dent S, Cortes J, Im YH, Dieras V, Harbeck N, Krop IE, et al. Phase III randomized study of taselisib or placebo with fulvestrant in estrogen receptor-positive, PIK3CA-mutant, HER2-negative, advanced breast cancer: the SANDPIPER trial. Ann Oncol. 2021;32:197–207. https://doi.org/10.1016/j.annonc.2020.10.596
Vasan N, Razavi P, Johnson JL, Shao H, Reznik E, Smith ML, et al. Double PIK3CA mutations in cis enhance PI3Kα oncogene activation and sensitivity to PI3Kα inhibitors in breast cancer. Ann Oncol. 2019;30:iii1 https://doi.org/10.1093/annonc/mdz095
Buckbinder L, St. Jean DJ, Tieu T, Wang W, Kryukov G, Jonsson P, et al. Abstract LB194: discovery and characterization of a mutant selective PI3Kα H1047X inhibitor with a best-in-class profile. Cancer Res. 2022;82:LB194. https://doi.org/10.1158/1538-7445.Am2022-lb194
Hudes G, Carducci M, Tomczak P, Dutcher J, Figlin R, Kapoor A, et al. Temsirolimus, interferon alfa, or both for advanced renal-cell carcinoma. N Engl J Med. 2007;356:2271–81. https://doi.org/10.1056/NEJMoa066838
Motzer RJ, Escudier B, Oudard S, Hutson TE, Porta C, Bracarda S, et al. Efficacy of everolimus in advanced renal cell carcinoma: a double-blind, randomised, placebo-controlled phase III trial. Lancet. 2008;372:449–56. https://doi.org/10.1016/S0140-6736(08)61039-9
Yao JC, Shah MH, Ito T, Bohas CL, Wolin EM, Van Cutsem E, et al. Everolimus for advanced pancreatic neuroendocrine tumors. N Engl J Med. 2011;364:514–23. https://doi.org/10.1056/NEJMoa1009290
Yao JC, Fazio N, Singh S, Buzzoni R, Carnaghi C, Wolin E, et al. Everolimus for the treatment of advanced, non-functional neuroendocrine tumours of the lung or gastrointestinal tract (RADIANT-4): a randomised, placebo-controlled, phase 3 study. Lancet. 2016;387:968–77. https://doi.org/10.1016/S0140-6736(15)00817-X
Schmid P, Abraham J, Chan S, Wheatley D, Brunt AM, Nemsadze G, et al. Capivasertib plus paclitaxel versus placebo plus paclitaxel as first-line therapy for metastatic triple-negative breast cancer: the PAKT trial. J Clin Oncol. 2020;38:423–33. https://doi.org/10.1200/JCO.19.00368
Sweeney C, Bracarda S, Sternberg CN, Chi KN, Olmos D, Sandhu S, et al. Ipatasertib plus abiraterone and prednisolone in metastatic castration-resistant prostate cancer (IPATential150): a multicentre, randomised, double-blind, phase 3 trial. Lancet. 2021;398:131–42. https://doi.org/10.1016/S0140-6736(21)00580-8
Razavi P, Dickler MN, Shah PD, Toy W, Brown DN, Won HH, et al. Alterations in PTEN and ESR1 promote clinical resistance to alpelisib plus aromatase inhibitors. Nat Cancer. 2020;1:382–93. https://doi.org/10.1038/s43018-020-0047-1
Juric D, Castel P, Griffith M, Griffith OL, Won HH, Ellis H, et al. Convergent loss of PTEN leads to clinical resistance to a PI(3)Kalpha inhibitor. Nature. 2015;518:240–4. https://doi.org/10.1038/nature13948
Curigliano G, Martin M, Jhaveri K, Beck JT, Tortora G, Fazio N, et al. Alpelisib in combination with everolimus +/− exemestane in solid tumours: phase Ib randomised, open-label, multicentre study. Eur J Cancer. 2021;151:49–62. https://doi.org/10.1016/j.ejca.2021.03.042
Hyman DM, Tran B, Paz-Ares L, Machiels JP, Schellens JH, Bedard PL, et al. Combined PIK3CA and FGFR inhibition with alpelisib and infigratinib in patients with PIK3CA-mutant solid tumors, with or without FGFR alterations. JCO Precis Oncol. 2019;3:1–13. https://doi.org/10.1200/PO.19.00221
Hopkins BD, Pauli C, Du X, Wang DG, Li X, Wu D, et al. Suppression of insulin feedback enhances the efficacy of PI3K inhibitors. Nature. 2018;560:499–503. https://doi.org/10.1038/s41586-018-0343-4
Zhang M, Jang H, Nussinov R. PI3K inhibitors: review and new strategies. Chem Sci. 2020;11:5855–65. https://doi.org/10.1039/d0sc01676d
Folgiero V, Di Carlo SE, Bon G, Spugnini EP, Di Benedetto A, Germoni S, et al. Inhibition of p85, the non-catalytic subunit of phosphatidylinositol 3-kinase, exerts potent antitumor activity in human breast cancer cells. Cell Death Dis. 2012;3:e440. https://doi.org/10.1038/cddis.2012.179
Sasso JM, Tenchov R, Wang D, Johnson LS, Wang X, Zhou QA. Molecular glues: the adhesive connecting targeted protein degradation to the clinic. Biochemistry. 2022. https://doi.org/10.1021/acs.biochem.2c00245
Thorpe LM, Yuzugullu H, Zhao JJ. PI3K in cancer: divergent roles of isoforms, modes of activation and therapeutic targeting. Nat Rev Cancer. 2015;15:7–24. https://doi.org/10.1038/nrc3860
Author information
Authors and Affiliations
Contributions
CB conceptualised and supervised the study. All authors were involved in data curation, investigation, methodology, writing, reviewing, and editing. The final version was approved by all authors.
Corresponding author
Ethics declarations
Competing interests
MR reports travelling funding for Sanofi. CP remunerated Consultant and/or Speaker for: Angelini Pharma, AstraZeneca, BMS, Eisai, General Electric, Ipsen, MSD; Protocol Steering Committee Member for: BMS, Eisai and MSD. VS reports research grants from Eli Lilly/Loxo Oncology, Blueprint Medicines Corporation, Turning Point Therapeutics, Boston Pharmaceuticals, and Helsinn Pharmaceuticals, and a grant and an advisory board/consultant positions with Eli Lilly/Loxo Oncology during the conduct of the study, as well as research grants from Roche/Genentech, Bayer, GlaxoSmithKline, Nanocarrier, Vegenics, Celgene, Northwest Biotherapeutics, Berg Health, Incyte, Fujifilm, D3, Pfizer, Multivir, Amgen, AbbVie, Alfasigma, Agensys, Boston Biomedical, IderaPharma, Inhibrx, Exelixis, Blueprint Medicines, Altum, Dragonfly Therapeutics, Takeda, National Comprehensive Cancer Network, NCI-Cancer Therapy Evaluation Program, The University of Texas MD Anderson Cancer Center, Turning Point Therapeutics, Boston Pharmaceuticals, Novartis, PharmaMar, Medimmune, advisory board/consultant positions with Helsinn, Incyte, QED Pharma, Daiichi Sankyo, Signant Health, Novartis, Relay Therapeutics, Pfizer, Roche, and Medimmune, travel funds from PharmaMar, Incyte, ASCO, and ESMO, and other support from Medscape outside the submitted work. GC received honoraria for speaker’s engagement: Roche, Seattle Genetics, Novartis, Lilly, Pfizer, Foundation Medicine, NanoString, Samsung, Celltrion, BMS, MSD; honoraria for providing consultancy: Roche, Seattle Genetics, NanoString; honoraria for participating in Advisory Board: Roche, Lilly, Pfizer, Foundation Medicine, Samsung, Celltrion, Mylan; honoraria for writing engagement: Novartis, BMS; honoraria for participation in Ellipsis Scientific Affairs Group; Institutional research funding for conducting phase I and II clinical trials: Pfizer, Roche, Novartis, Sanofi, Celgene, Servier, Orion, AstraZeneca, Seattle Genetics, AbbVie, Tesaro, BMS, Merck Serono, Merck Sharp Dome, Janssen-Cilag, Philogen, Bayer, Medivation, Medimmune. All remaining authors have declared no conflict of interest.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Belli, C., Repetto, M., Anand, S. et al. The emerging role of PI3K inhibitors for solid tumour treatment and beyond. Br J Cancer 128, 2150–2162 (2023). https://doi.org/10.1038/s41416-023-02221-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-023-02221-1
This article is cited by
-
A deep learning-based theoretical protocol to identify potentially isoform-selective PI3Kα inhibitors
Molecular Diversity (2024)
-
PI3K/AKT/mTOR signaling transduction pathway and targeted therapies in cancer
Molecular Cancer (2023)