Abstract
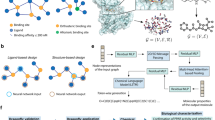
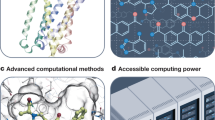
Hepatocellular carcinoma (HCC) is one of the most common and deadly cancers in the world. The therapeutic outlook for HCC patients has significantly improved with the advent and development of systematic and targeted therapies such as sorafenib and lenvatinib; however, the rise of drug resistance and the high mortality rate necessitate the continuous discovery of effective targeting agents. To discover novel anti-HCC compounds, we first constructed a deep learning-based chemical representation model to screen more than 6 million compounds in the ZINC15 drug-like library. We successfully identified LGOd1 as a novel anticancer agent with a characteristic levoglucosenone (LGO) scaffold. The mechanistic studies revealed that LGOd1 treatment leads to HCC cell death by interfering with cellular copper homeostasis, which is similar to a recently reported copper-dependent cell death named cuproptosis. While the prototypical cuproptosis is brought on by copper ionophore-induced copper overload, mechanistic studies indicated that LGOd1 does not act as a copper ionophore, but most likely by interacting with the copper chaperone protein CCS, thus LGOd1 represents a potentially new class of compounds with unique cuproptosis-inducing property. In summary, our findings highlight the critical role of bioavailable copper in the regulation of cell death and represent a novel route of cuproptosis induction.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 Countries. CA Cancer J Clin. 2021;71:209–49.
Llovet JM, Zucman-Rossi J, Pikarsky E, Sangro B, Schwartz M, Sherman M, et al. Hepatocellular carcinoma. Nat Rev Dis Prim. 2016;2:16018.
Jin H, Shi Y, Lv Y, Yuan S, Ramirez CFA, Lieftink C, et al. EGFR activation limits the response of liver cancer to lenvatinib. Nature. 2021;595:730–4.
Gao Q, Zhu H, Dong L, Shi W, Chen R, Song Z, et al. Integrated proteogenomic characterization of HBV-Related hepatocellular carcinoma. Cell. 2019;179:561–77.e22
Jiang Y, Sun A, Zhao Y, Ying W, Sun H, Yang X, et al. Proteomics identifies new therapeutic targets of early-stage hepatocellular carcinoma. Nature. 2019;567:257–61.
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144:646–74.
Galluzzi L, Vitale I, Aaronson SA, Abrams JM, Adam D, Agostinis P, et al. Molecular mechanisms of cell death: recommendations of the nomenclature committee on cell death 2018. Cell Death Differ. 2018;25:486–541.
Green DR. A Matter of Life and Death. Cold Spring Harb Perspect Biol. 2022;14:a041004.
Bedoui S, Herold MJ, Strasser A. Emerging connectivity of programmed cell death pathways and its physiological implications. Nat Rev Mol Cell Biol. 2020;21:678–95.
Kahlson MA, Dixon SJ. Copper-induced cell death. Science. 2022;375:1231–2.
Koren E, Fuchs Y. Modes of regulated cell death in cancer. Cancer Discov. 2021;11:245–65.
Peng F, Liao M, Qin R, Zhu S, Peng C, Fu L, et al. Regulated cell death (RCD) in cancer: key pathways and targeted therapies. Signal Transduct Target Ther. 2022;7:286.
Tong X, Tang R, Xiao M, Xu J, Wang W, Zhang B, et al. Targeting cell death pathways for cancer therapy: recent developments in necroptosis, pyroptosis, ferroptosis, and cuproptosis research. J Hematol Oncol. 2022;15:174.
Li H, Wei W, Xu H. Drug discovery is an eternal challenge for the biomedical sciences. Acta Mater Med. 2022;1:1–3.
Eder J, Sedrani R, Wiesmann C. The discovery of first-in-class drugs: origins and evolution. Nat Rev Drug Discov. 2014;13:577–87.
Issa NT, Stathias V, Schurer S, Dakshanamurthy S. Machine and deep learning approaches for cancer drug repurposing. Semin Cancer Biol. 2021;68:132–42.
Kuenzi BM, Park J, Fong SH, Sanchez KS, Lee J, Kreisberg JF, et al. Predicting drug response and synergy using a deep learning model of human cancer cells. Cancer Cell. 2020;38:672–84.e6.
Chandak T, Mayginnes JP, Mayes H, Wong CF. Using machine learning to improve ensemble docking for drug discovery. Proteins. 2020;88:1263–70.
Zhang R, Li X, Zhang X, Qin H, Xiao W. Machine learning approaches for elucidating the biological effects of natural products. Nat Prod Rep. 2021;38:346–61.
Zhu J, Wang J, Wang X, Gao M, Guo B, Gao M, et al. Prediction of drug efficacy from transcriptional profiles with deep learning. Nat Biotechnol. 2021;39:1444–52.
Stokes JM, Yang K, Swanson K, Jin W, Cubillos-Ruiz A, Donghia NM, et al. A deep learning approach to antibiotic discovery. Cell. 2020;180:688–702.e13.
Tsvetkov P, Coy S, Petrova B, Dreishpoon M, Verma A, Abdusamad M, et al. Copper induces cell death by targeting lipoylated TCA cycle proteins. Science. 2022;375:1254–61.
Corsello SM, Nagari RT, Spangler RD, Rossen J, Kocak M, Bryan JG, et al. Discovering the anti-cancer potential of non-oncology drugs by systematic viability profiling. Nat Cancer. 2020;1:235–48.
Tai Y, Gao JH, Zhao C, Tong H, Zheng SP, Huang ZY, et al. SK-Hep1: not hepatocellular carcinoma cells but a cell model for liver sinusoidal endothelial cells. Int J Clin Exp Pathol. 2018;11:2931–8.
Yang K, Swanson K, Jin W, Coley C, Eiden P, Gao H, et al. Analyzing learned molecular representations for property prediction. J Chem Inf Model. 2019;59:3370–88.
Wu Z, Ramsundar B, Feinberg EN, Gomes J, Geniesse C, Pappu AS, et al. MoleculeNet: a benchmark for molecular machine learning. Chem Sci. 2018;9:513–30.
Sterling T, Irwin JJ. ZINC 15–ligand discovery for everyone. J Chem Inf Model. 2015;55:2324–37.
Mendez D, Gaulton A, Bento AP, Chambers J, De Veij M, Felix E, et al. ChEMBL: towards direct deposition of bioassay data. Nucleic Acids Res. 2019;47:D930–40.
Yang T, Li Z, Chen Y, Feng D, Wang G, Fu Z, et al. DrugSpaceX: a large screenable and synthetically tractable database extending drug space. Nucleic Acids Res. 2021;49:D1170–8.
Demichev V, Messner CB, Vernardis SI, Lilley KS, Ralser M. DIA-NN: neural networks and interference correction enable deep proteome coverage in high throughput. Nat Methods. 2020;17:41–4.
Subramanian A, Tamayo P, Mootha VK, Mukherjee S, Ebert BL, Gillette MA, et al. Gene set enrichment analysis: a knowledge-based approach for interpreting genome-wide expression profiles. Proc Natl Acad Sci USA. 2005;102:15545–50.
Jumper J, Evans R, Pritzel A, Green T, Figurnov M, Ronneberger O, et al. Highly accurate protein structure prediction with AlphaFold. Nature. 2021;596:583–9.
Morris GM, Huey R, Lindstrom W, Sanner MF, Belew RK, Goodsell DS, et al. AutoDock4 and AutoDockTools4: automated docking with selective receptor flexibility. J Comput Chem. 2009;30:2785–91.
Volkamer A, Griewel A, Grombacher T, Rarey M. Analyzing the topology of active sites: on the prediction of pockets and subpockets. J Chem Inf Model. 2010;50:2041–52.
O’Boyle NM, Banck M, James CA, Morley C, Vandermeersch T, Hutchison GR. Open Babel: an open chemical toolbox. J Cheminform. 2011;3:33.
Eberhardt J, Santos-Martins D, Tillack AF, Forli S. AutoDock Vina 1.2.0: new docking methods, expanded force field, and python bindings. J Chem Inf Model. 2021;61:3891–8.
Adasme MF, Linnemann KL, Bolz SN, Kaiser F, Salentin S, Haupt VJ, et al. PLIP 2021: expanding the scope of the protein-ligand interaction profiler to DNA and RNA. Nucleic Acids Res. 2021;49:W530–4.
Jafari R, Almqvist H, Axelsson H, Ignatushchenko M, Lundback T, Nordlund P, et al. The cellular thermal shift assay for evaluating drug target interactions in cells. Nat Protoc. 2014;9:2100–22.
Dai L, Zhao T, Bisteau X, Sun W, Prabhu N, Lim YT, et al. Modulation of protein-interaction states through the cell cycle. Cell. 2018;173:1481–94.e13.
Hayes JD, Dinkova-Kostova AT, Tew KD. Oxidative stress in cancer. Cancer Cell. 2020;38:167–97.
Chen L, Min J, Wang F. Copper homeostasis and cuproptosis in health and disease. Signal Transduct Target Ther. 2022;7:378.
Perelman A, Wachtel C, Cohen M, Haupt S, Shapiro H, Tzur A. JC-1: alternative excitation wavelengths facilitate mitochondrial membrane potential cytometry. Cell Death Dis. 2012;3:e430.
Huang KF, Ma KH, Hung YC, Lo LC, Lin KC, Liu PS, et al. A new copper ionophore DPMQ protects cells against ultraviolet B irradiation by inhibiting the TRPV1 channel. J Cell Physiol. 2018;233:9594–610.
Donnelly PS, Liddell JR, Lim S, Paterson BM, Cater MA, Savva MS, et al. An impaired mitochondrial electron transport chain increases retention of the hypoxia imaging agent diacetylbis(4-methylthiosemicarbazonato)copperII. Proc Natl Acad Sci USA. 2012;109:47–52.
Zhang B, Georgiev O, Hagmann M, Gunes C, Cramer M, Faller P, et al. Activity of metal-responsive transcription factor 1 by toxic heavy metals and H2O2 in vitro is modulated by metallothionein. Mol Cell Biol. 2003;23:8471–85.
Aubert L, Nandagopal N, Steinhart Z, Lavoie G, Nourreddine S, Berman J, et al. Copper bioavailability is a KRAS-specific vulnerability in colorectal cancer. Nat Commun. 2020;11:3701.
Camacho DM, Collins KM, Powers RK, Costello JC, Collins JJ. Next-generation machine learning for biological networks. Cell. 2018;173:1581–92.
Liu X, Carr P, Gardiner MG, Banwell MG, Elbanna AH, Khalil ZG, et al. Levoglucosenone and its pseudoenantiomer iso-levoglucosenone as scaffolds for drug discovery and development. ACS Omega. 2020;5:13926–39.
Tsai YH, Borini Etichetti CM, Cicetti S, Girardini JE, Spanevello RA, Suarez AG, et al. Design, synthesis and evaluation of novel levoglucosenone derivatives as promising anticancer agents. Bioorg Med Chem Lett. 2020;30:127247.
Camp JE, Greatrex BW. Levoglucosenone: bio-based platform for drug discovery. Front Chem. 2022;10:902239.
Giri GF, Danielli M, Marinelli RA, Spanevello RA. Cytotoxic effect of levoglucosenone and related derivatives against human hepatocarcinoma cell lines. Bioorg Med Chem Lett. 2016;26:3955–7.
Westman J, Wiman K, Mohell N. Levoglucosenone derivatives for the treatment of disorders such as cancer, autoimmune diseases and heart diseases. WIPO pantent WO2007/139497 A1. 2007.
Kirshner JR, He S, Balasubramanyam V, Kepros J, Yang CY, Zhang M, et al. Elesclomol induces cancer cell apoptosis through oxidative stress. Mol Cancer Ther. 2008;7:2319–27.
Ren X, Li Y, Zhou Y, Hu W, Yang C, Jing Q, et al. Overcoming the compensatory elevation of NRF2 renders hepatocellular carcinoma cells more vulnerable to disulfiram/copper-induced ferroptosis. Redox Biol. 2021;46:102122.
Xiao Y, Chen DI, Zhang X, Cui Q, Fan Y, Bi C, et al. Molecular study on copper-mediated tumor proteasome inhibition and cell death. Int J Oncol. 2010;37:81–7.
Dai L, Prabhu N, Yu LY, Bacanu S, Ramos AD, Nordlund P. Horizontal cell biology: monitoring global changes of protein interaction states with the proteome-wide Cellular Thermal Shift Assay (CETSA). Annu Rev Biochem. 2019;88:383–408.
Prabhu N, Dai L, Nordlund P. CETSA in integrated proteomics studies of cellular processes. Curr Opin Chem Biol. 2020;54:54–62.
Skopp A, Boyd SD, Ullrich MS, Liu L, Winkler DD. Copper-zinc superoxide dismutase (Sod1) activation terminates interaction between its copper chaperone (Ccs) and the cytosolic metal-binding domain of the copper importer Ctr1. Biometals. 2019;32:695–705.
Pope CR, De Feo CJ, Unger VM. Cellular distribution of copper to superoxide dismutase involves scaffolding by membranes. Proc Natl Acad Sci USA. 2013;110:20491–6.
Wong PC, Waggoner D, Subramaniam JR, Tessarollo L, Bartnikas TB, Culotta VC, et al. Copper chaperone for superoxide dismutase is essential to activate mammalian Cu/Zn superoxide dismutase. Proc Natl Acad Sci USA. 2000;97:2886–91.
Wang J, Luo C, Shan C, You Q, Lu J, Elf S, et al. Inhibition of human copper trafficking by a small molecule significantly attenuates cancer cell proliferation. Nat Chem. 2015;7:968–79.
Sun J, Prabhu N, Tang J, Yang F, Jia L, Guo J, et al. Recent advances in proteome-wide label-free target deconvolution for bioactive small molecules. Med Res Rev. 2021;41:2893–926.
Stockwell BR. Ferroptosis turns 10: emerging mechanisms, physiological functions, and therapeutic applications. Cell. 2022;185:2401–21.
Lei G, Zhuang L, Gan B. Targeting ferroptosis as a vulnerability in cancer. Nat Rev Cancer. 2022;22:381–96.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (32070748, 81902787); Excellent Scientific and Technological Innovation Training Program of Shenzhen (RCYX20210706092040048); Natural Science Foundation of Top Talent of SZTU (Grant No. GDRC202125); Singapore’s National Research Foundation (NRF‐CRP22‐2019‐0003).
Author information
Authors and Affiliations
Contributions
Conceptualization: LYD; Methodology: LYD, JGW, PN, FY, NP; Investigation: FY, LJ, HCZ, JNH, MYH, ZJL, CZ, FTL; Visualization: FY, CBY; Supervision: LYD, JGW, PN; Writing—original draft: FY, LYD; Writing—review & editing: FY, LJ, JGW, LYD.
Corresponding authors
Ethics declarations
Competing interests
PN is the inventor of patents related to the CETSA method and is a cofounder and board member of Pelago Biosciences AB. LYD, JGW, FY, LJ, CBY, HCZ and MYH have a patent pending for compound LGOd1. The remaining authors declare they have no competing interests.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, F., Jia, L., Zhou, Hc. et al. Deep learning enables the discovery of a novel cuproptosis-inducing molecule for the inhibition of hepatocellular carcinoma. Acta Pharmacol Sin 45, 391–404 (2024). https://doi.org/10.1038/s41401-023-01167-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-023-01167-7