Abstract
Study design
Cross-sectional construct validation study.
Objectives
To test the construct validity of the Leisure Time Physical Activity Questionnaire for People with Spinal Cord Injury (LTPAQ-SCI) by examining associations between the scale responses and cardiorespiratory fitness (CRF) in a sample of adults living with spinal cord injury (SCI).
Setting
Three university-based laboratories in Canada.
Methods
Participants were 39 adults (74% male; M age: 42 ± 11 years) with SCI who completed the LTPAQ-SCI and a graded exercise test to volitional exhaustion using an arm-crank ergometer. One-tailed Pearson’s correlation coefficients were computed to examine the association between the LTPAQ-SCI measures of mild-, moderate-, heavy-intensity and total minutes per week of LTPA and CRF (peak volume of oxygen consumption [V̇O2peak] and peak power output [POpeak]).
Results
Minutes per week of mild-, moderate- and heavy-intensity LTPA and total LTPA were all positively correlated with V̇O2peak. The correlation between minutes per week of mild intensity LTPA and V̇O2peak was small-medium (r = 0.231, p = 0.079) while all other correlations were medium-large (rs ranged from 0.276 to 0.443, ps < 0.05). Correlations between the LTPAQ-SCI variables and POpeak were also positive but small (rs ranged from 0.087 to 0.193, ps > 0.05), except for a medium-sized correlation between heavy-intensity LTPA and POpeak (r = 0.294, p = 0.035).
Conclusions
People with SCI who report higher levels of LTPA on the LTPAQ-SCI also demonstrate greater levels of CRF, with stronger associations between moderate- and heavy-intensity LTPA and CRF than between mild-intensity LTPA and CRF. These results provide further support for the construct validity of the LTPAQ-SCI as a measure of LTPA among people with SCI.
Similar content being viewed by others
Introduction
Participation in exercise, sports and other forms of leisure-time physical activity (LTPA) has significant positive effects on the fitness, health and well-being of people living with spinal cord injury (SCI) [1,2,3]. However, the vast majority of people with SCI are insufficiently active to derive these benefits [4] because they face so many barriers to participation [5]. Consequently, there is a need to develop, test and implement strategies to increase LTPA participation in people living with SCI.
Reliable and valid measures of LTPA are required to assess the effectiveness of LTPA-enhancing interventions. Review articles [6,7,8] have catalogued the measurement properties of wearable and self-report physical activity measures that have been used in SCI research. Although the reliability and validity of wearable measures are improving, a significant limitation of these devices is that they cannot distinguish between LTPA and other types of physical activity (e.g., household, transportation, occupational activity) [7]. Because LTPA is the only form of physical activity that has been shown to significantly improve fitness in people with SCI [1], it is crucial that scientists have valid and reliable methods to measure it. Another limitation of some wearable devices (e.g., wrist-worn accelerometers), is that they underestimate the intensity of wheeled activity on slopes and rough, uneven surfaces [9,10,11]. The SCI exercise guidelines [12] stipulate that exercise must be done at a moderate- to heavy-intensity in order to achieve significant health and fitness benefits. Systems that track SCI exercise guideline adherence require valid and reliable measures of the amount of activity performed at moderate- and heavy-intensities. Given the limitations of wearable devices, self-report measures are considered superior for feasibly collecting data on the types and amounts of LTPA performed by people with SCI [7].
Compared to all other measures of PA used in SCI research, the Physical Activity Recall Assessment for People with SCI (PARA-SCI) [13] has yielded the strongest evidence of reliability and validity [7, 8, 14]. Using a structured, standardized interview format, respondents are cued to recall and rate the intensity of all LTPA and activities of daily living that they have performed over the previous 3 days [15]. The PARA-SCI has demonstrated positive evidence of criterion validity (using both indirect calorimetry and doubly-labelled water as criteria), construct validity and test-retest reliability [13, 14, 16]. However, because the PARA-SCI was designed to capture the types, frequencies, intensities and durations of all physical activities, it can create unnecessary participant and clinician/researcher burden in situations where investigators are interested only in measuring LTPA [7]. In response to these concerns, the Leisure Time Physical Activity Questionnaire for People with SCI (LTPAQ-SCI) was developed [17].
The LTPAQ-SCI is an SCI-specific, self-report assessment of LTPA that measures the number of minutes of mild, moderate, and heavy intensity LTPA that a person performed over the previous 7 days [17]. It can be self- or interviewer-administered in less than 5 min. The reporting format used in the LTPAQ-SCI parallels the reporting structure of one of the most widely used self-report measures of PA in the general population--the International Physical Activity Questionnaire-Short Form [18].
Research has produced positive evidence of the LTPAQ-SCI’s test-retest reliability. Intraclass correlation coefficients were significant for LTPAQ-SCI measures of mild, moderate, heavy and total LTPA over a one-week test-retest period [17]. A recent study of the test-retest reliability of a Canadian-French version of the questionnaire produced similarly strong ICCs [19]. Evidence of the measure’s criterion validity was shown by significant correlations between LTPAQ-SCI measures of mild, moderate, heavy and total LTPA minutes per week and PARA-SCI measures (i.e., the criterion) of LTPA minutes per day at these same intensities [17].
Support for the LTPAQ-SCI’s construct validity has been generated in hypothesis-testing studies [20]. For example, LTPAQ-SCI measures of LTPA have been shown to increase significantly in response to LTPA-enhancing interventions delivered to adults with SCI [21] and multiple sclerosis [22]. LTPAQ-SCI measures of LTPA have also been shown to differ in predicted directions between adults with SCI with low versus high depressive symptomatology [23], and between athletes with disabilities who participate in sport at lower (recreational, developmental) versus higher (provincial, state, national) competitive levels [24]. It is important to note, however, that construct validation is an ongoing process, and no one single experiment can ‘prove’ construct validity [20]. Rather, each supportive study serves to strengthen the construct’s nomological network [25], by demonstrating that the construct operates predictably within a system of key concepts.
Cardiorespiratory fitness (CRF) is a key concept in relation to LTPA. It is well-established that participation in moderate- to heavy-intensity exercise (a specific type of LTPA) imparts significant improvements in the CRF of adults with SCI [1, 26]. If the LTPAQ-SCI is to be used as a measure of LTPA, then its construct validation should include tests of its associations with CRF (these types of tests are sometimes referred to as tests of ‘convergent validity’ [20]). Therefore, the purpose of the present study was to examine the association between the number of minutes per week of mild, moderate, heavy and total LTPA reported by adults with SCI who completed the LTPAQ-SCI, and their CRF. It was hypothesized that number of minutes per week of LTPA would be positively correlated with participants’ CRF.
Method
Participants
Participants were 51 individuals who completed the LTPAQ-SCI and CRF assessment during baseline testing for CHOICES (NCT01718977), a multicentre, randomized controlled clinical trial assessing the effects of two different exercise interventions on cardiovascular health outcomes in adults with SCI [27]. This construct validation study was planned a priori, as a secondary analysis of data that were being collected as part of the CHOICES protocol. CHOICES study inclusion criteria were: male or female; 18–60 years of age; chronic (>1 year since injury), traumatic, motor-complete SCI [American Spinal Injury Association Impairment Scale (AIS) A and B]; and neurological level of injuries (NLI) between the cervical fourth and thoracic sixth vertebrae (C4-T6). AIS and NLI were determined using the International Standards for neurological Classification of SCI [28]. Participants were excluded if they had: any medical history of symptoms of cardiovascular disease; major trauma or surgery in the last six months; fracture within the previous 12 months; or any psychological or cognitive dysfunction that prevented understanding English instructions. All study procedures were approved by the research ethics board at each trial site and all participants provided written informed consent prior to any of the study procedures.
Measures
LTPAQ-SCI
The LTPAQ-SCI was administered during an interview conducted by a research assistant (face-to-face interview at two sites and telephone interview at one site). Consistent with the LTPAQ-SCI administration instructions [17], participants were first presented with a standardized definition of LTPA: “physical activity that you choose to do during your free time, such as exercising, playing sports, gardening, and taking the dog for a walk (necessary physical activities such as physiotherapy, grocery shopping, pushing/wheeling for transportation are not considered LTPA)”. Next, participants were given a validated [13], SCI-specific definition of mild-intensity LTPA and were asked to recall (a) the number of days, over the past 7 days, that they did mild-intensity LTPA and (b) on those days, how many minutes they usually spent doing mild-intensity LTPA. These steps were repeated for moderate-intensity and heavy-intensity LTPA. Mild-intensity activities were defined as “activities that require you to do very light work. You should feel like you are working a little bit but overall you should not find yourself working too hard”. Moderate-intensity activities were defined as “activities that require some physical effort. You should feel like you are working somewhat hard but you should feel like you can keep going for a long time”. Finally, heavy-intensity activities were defined as “activities that require a lot of physical effort. You should feel like you are working really hard (almost at your maximum) and can only do the activity for a short time before getting tired. These activities can be exhausting”. The number of minutes per week of LTPA performed at each intensity (mild, moderate and heavy) was calculated by multiplying the days of activity by the minutes of activity. Total LTPA was calculated as a sum of LTPA at each intensity, thus yielding the total number of minutes of LTPA undertaken in the past week.
Cardiorespiratory fitness (CRF)
All participants underwent an incremental exercise test using an electronically braked arm-crank ergometer (Lode BV, Groningen, The Netherlands; Vancouver site. Monark 881E, Monark Exercise AB, Vansbro, Sweden; Toronto and Hamilton sites.) until the point of volitional exhaustion. Heart rate was recorded continuously using a chest strap HR monitor (T31; Polar Electro Inc., Woodbury, NY, USA). Respiratory gases were collected using a metabolic cart that was calibrated, prior to each use, according to the manufacturer’s instructions (Parvomedics Truemax 2400, Sandy, Utah, USA; Vancouver site. Vmax Encore, SensorMedics, California, USA; Toronto site. Moxus Metabolic System, AEI Technologies, Illinois, USA; Hamilton site).
Participants were asked to empty their bladders prior to the test to minimize the influence of autonomic dysreflexia. The test protocol began with a warm-up of arm cranking at 0 Watts for two minutes. Afterwards, the protocol continued with 1-minute stages, with a resistance increment of 5–10 Watts per stage depending on the participant’s neurological level of injury [29]. Participants were instructed to maintain a cycling cadence of 50 revolutions per minute (rpm) throughout the duration of the test with continuous motivation delivered by the assessor. The test continued to the point of volitional exhaustion or when the cadence dropped below 30 rpm. Borg’s rating of perceived exertion 6–20 was administered at the end of every stage [30]. The highest volume of oxygen consumption (V̇O2) of 20-second averaging during the test was recorded as peak volume of oxygen consumption (V̇O2peak). Peak power output (POpeak) was defined as the highest PO achieved, unless volitional exhaustion occurred within 20-s of the beginning of the stage, in which case POpeak was recorded as the PO at the second-last completed stage of the test.
Procedure
At two sites (Hamilton and Vancouver), the LTPAQ-SCI was administered during the baseline testing session, prior to the CRF test. At one site (Toronto), the LTPAQ-SCI was administered 8 days after the fitness test but before starting exercise in the CHOICES trial. This timing was deliberate to avoid participants reporting any LTPA that was performed as part of the CHOICES baseline testing or training protocols.
Data management and analyses
The respiratory exchange ratio (RER) was used to corroborate attainment of V̇O2peak during the fitness test. Analyses were conducted only on participants who exhibited an RER ≥1.00, representing a conservative yet reliable lower-range of expected peak RER responses in SCI and healthy adults [29, 31]. People with tetraplegia cannot achieve the same V̇O2peak and POpeak as people with paraplegia due to more severe autonomic and upper-body motor impairments [32]. Consequently, the distributions of these values differ for people with tetraplegia versus paraplegia [32]. Therefore, the measures of CRF (i.e., V̇O2peak and POpeak) were standardized for lesion level (i.e., paraplegia or tetraplegia) through transformations to z-scores prior to analysis.
Descriptive statistics were calculated as means, standard deviations, medians and minimum-maximum for continuous variables, and as percentages for the categorical variables. Shapiro Wilk tests were used to check the normality assumption. Because the LTPAQ-SCI variables presented significant deviations from the normal distribution, a square root transformation was carried out on these variables. Using the transformed variables, one-tailed Pearson correlation coefficients were calculated between the LTPAQ-SCI measures of mild, moderate, heavy and total LTPA and the measures of CRF (i.e., V̇O2peak and POpeak). Since the hypotheses were directional (i.e., all the correlations were expected to be positive), one-tailed tests were used. All analyses were conducted using IBM SPSS Statistics v. 26. Alpha was set at 0.05 for all analyses and was not adjusted for multiplicity given that all hypotheses were specified a priori (cf. [33]). Cohen’s conventions were used to interpret the magnitude of the correlations (i.e., rs of 0.10, 0.30, 0.50 constitute small, medium and large correlations, respectively) [34].
Results
Preliminary analyses
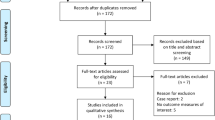
After excluding data from 12 participants who did not achieve RER ≥1.00, 39 participants remained for the main analyses. Excluded participants presented significantly lower POpeak and VO2peak values than the included ones. In addition, all excluded participants had tetraplegia. No significant differences were found between excluded and included participants regarding sex, age, age at injury, time since injury, body mass or height, or LTPAQ-SCI values. Exploratory analyses indicated neither age nor years since injury were significant bivariate correlates of POpeak or VO2peak. In exploratory regression analyses, neither age nor years since injury were significant predictors of any LTPAQ-SCI variable. Therefore, for parsimony, these variables were not included in subsequent analyses. Subsequent analyses were conducted with data from the remaining 39 participants. Table 1 shows the demographic data for both the full sample and the final sample, as well as the p values of the tests performed to detect potential differences between included and excluded participants
Correlations between the LTPAQ-SCI measures of LTPA and aerobic fitness
Table 2 presents the full correlation matrix. Minutes per week of mild-, moderate- and heavy-intensity LTPA and total LTPA were all positively correlated with V̇O2peak. The correlation between V̇O2peak and mild-intensity LTPA was small-medium (r = 0.231, p = 0.079), while the correlations of V̇O2peak with moderate-intensity LTPA (r = 0.276, p = 0.045) and heavy-intensity LTPA (r = 0.443, p = 0.002) were medium-large.
Correlations between the LTPAQ-SCI variables and POpeak were also positive. However, the correlations of POpeak with mild-intensity LTPA (r = 0.087, p = 0.300) and moderate-intensity LTPA (r = 0.193, p = 0.119) were trivial to small, while the correlation between heavy-intensity LTPA and POpeak (r = 0.294, p = 0.035) was medium-sized.
Discussion
The purpose of this study was to conduct a test of the construct validity of the LTPAQ-SCI. As hypothesized, minutes per week of LTPA reported on the LTPAQ-SCI were positively correlated with participants’ CRF. Correlations tended to be stronger for heavy versus mild-intensity LTPA and for V̇O2peak than for POpeak.
Overall, the pattern and size of the correlations were similar to correlations reported between CRF and other self-report measures of PA for people with and without SCI. For instance, in prior tests of the PARA-SCI’s construct validity [16], correlations between CRF and moderate- and heavy-intensity LTPA were medium-sized, while the correlation between CRF and mild-intensity LTPA was small. These findings align with research demonstrating that in order to produce significant CRF benefits, adults with SCI must exercise at a moderate- to heavy-intensity [1]. Exercise of a mild intensity is insufficient [35]. Our results show that the LTPAQ-SCI does indeed capture CRF-enhancing LTPA in adults with SCI.
Our results are also similar to the medium-sized correlations reported in validation studies of the IPAQ-SF, one of the most widely-used self-report measures of PA for the general population. For instance, across three studies that reported correlations between the IPAQ-SF measure of total minutes per week of PA and V̇O2max, the median correlation was r = 0.30 [36]. We found a correlation of r = 0.33 between LTPAQ-SCI total LTPA and V̇O2peak. It is worth noting that only ~50% of the variance in CRF can be explained by environmental factors, such as physical activity, with the rest attributed to hereditary/genetic factors [37]. Furthermore, additional variance in CRF within the SCI population can be attributed to the severity and exact level of neurological injury sustained, contributing to the degree of autonomic and functional impairment [38]. Thus, it is encouraging to observe similar, associations between LTPA and V̇O2peak in individuals with high-level SCI, supporting the construct validity of the LTPAQ-SCI in the context of other well-used self-report measures of PA.
Our analyses suggested that LTPA was more strongly correlated with V̇O2peak than POpeak. This finding differs from results from the PARA-SCI validation studies in which CRF tended to be more strongly correlated with POpeak than V̇O2peak [16]. These discrepancies are likely a statistical artefact. There was greater variability in POpeak values in the PARA-SCI validation study than in the present study. When data variability is reduced, correlations may be lower than expected [39]. Nevertheless, as the correlations with POpeak were all positive, and stronger for moderate- and heavy-intensity LTPA than mild-intensity LTPA, we take this as further support for the construct validation of the LTPAQ-SCI as a measure of CRF-enhancing LTPA.
Importantly, scale validation studies do not confirm that the scale itself is valid. No study can ‘validate’ a scale. Rather, validation studies substantiate the inferences that can be made about people based on their scale scores (e.g., the amount of LTPA they do each week) [20] and that the scale is valid for use with a particular group of people in a particular context [20]. The present study was conducted with a sample of men and women with chronic, motor complete cervical or high thoracic injuries. Although we would expect the results to generalize to individuals with incomplete, lower-level injuries[16], this hypothesis should be tested in heterogenous samples.
There is also a need to conduct LTPAQ-SCI validation studies in countries other than Canada, because definitions of LTPA may differ across cultural contexts [40]. For instance, the instructions for completing the LTPAQ-SCI stipulate that physiotherapy should not be counted. This stipulation is included because during development of the PARA-SCI and LTPAQ-SCI, many of the physiotherapy activities reported by Canadians with SCI, were neither leisure-time nor fitness-enhancing activities (e.g., passive stretching, practicing transfers, practicing using mobility equipment) [15]. However, in other countries or contexts, physiotherapy may routinely include exercise or sport activities and may therefore be counted as LTPA. In a similar vein, active transportation is uncommon among Canadians with SCI [41] because climate, terrain and long distances are significant barriers. In some countries, however, it may be more common for people with SCI to use active forms of transportation (e.g., handcycling in European countries [42]) in order to get exercise. In these circumstances, it may make sense to report such activities on the LTPAQ-SCI. By testing the relationships between CRF and LTPAQ-SCI scores, including and excluding physiotherapy and active transportation activities, users of the LTPAQ-SCI can better define and measure LTPA in their contexts.
Strengths of this study include standardized administrations of the LTPAQ-SCI and the CRF test. While multi-site data collection was a strength insofar as it facilitated participant enrolment and statistical power, it may also be considered a limitation that introduced variability through different CRF testing equipment and testers at each site. A further limitation is that only one aspect of physical fitness was measured. Muscular strength and endurance are two additional physical fitness aspects that should correlate positively with LTPAQ-SCI scores [16] and should be examined in future construct validation studies. Furthermore, if study participants engaged primarily in strength-training LTPA (e.g., lifting weights), the correlation between their LTPAQ-SCI measure of minutes per week of LTPA and their CRF may have been attenuated relative to individuals who engaged primarily in CRF-enhancing LTPA (e.g., arm cycling).
Another study limitation is that data collected from nearly half of the tetraplegic participants (12 out of 27) could not be used because they terminated the CRF test before achieving criteria indicative of a peak exercise test (i.e., RER ≥ 1.00). Because of arm fatigue during exercise testing, peripheral ratings of perceived exertion increase much faster in those with tetraplegia than paraplegia [43] prompting participants to terminate the test before achieving peak. Given this challenge, researchers should consider other feasible, valid measures of CRF that could be used in LTPAQ-SCI construct validation studies involving participants with tetraplegia, for example, individualized ramp tests, submaximal aerobic endurance, or submaximal predictive equations such as the 6-minute arm test validated for individuals with SCI [44]. An alternative construct validation approach may be to assess associations between LTPAQ-SCI scores and 7-day overall physical activity levels measured via wearable devices. While limitations of accelerometers attached to a single anatomical location or wheelchair have been noted in people with SCI [7, 9], the estimation of physical activity intensity can be improved by utilising multi-sensor devices that incorporate physiological signals (such as galvanic skin responses or heart rate) and utilising complex or individualised modelling approaches [45, 46]. Combined with the use of diaries or logs to distinguish periods of LTPA from other physical activity types, assessing the associations between outputs from multi-sensor wearable devices and the LTPAQ-SCI may be a way to test the validity of this measure while overcoming some of the challenges noted with assessing CRF in individuals with tetraplegia.
In conclusion, the results of the present study demonstrate that self-reported LTPA, as measured by the LTPAQ-SCI, is positively correlated with CRF in adults with chronic, motor complete cervical or high thoracic SCI, being the associations stronger for moderate- and heavy-intensity LTPA. When considered with previous research showing that LTPAQ-SCI scores vary in predictable ways across meaningful groups and in response to behavioural interventions [17, 19,20,21,22,23,24], these results provide further support for the construct validity of the LTPAQ-SCI as a measure of LTPA for adults with SCI. Further construct validation studies are needed to demonstrate the validity of the LTPAQ-SCI for use as a measure of LTPA in more heterogeneous samples of people with SCI and in other countries and contexts.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
van der Scheer JW, Martin Ginis KA, Ditor DS, Goosey-Tolfrey V, Hicks AL, West CR, et al. Effects of exercise on fitness and health of adults with spinal cord injury: a systematic review. Neurology. 2017;89:736–45.
Martin Ginis KA, Jetha A, Mack DE, Hetz S. Physical activity and subjective well-being among people with spinal cord injury: a meta-analysis. Spinal Cord. 2010;48:65–72.
Farrow M, Nightingale T, Maher J, McKay C, Thompson D, J B. The effect of exercise on cardiometabolic risk factors in adults with chronic spinal cord injury: a systematic review: exercise and CMS risk in SCI. Arch Phys Med Rehabilit 2020. https://doi.org/10.1016/j.apmr.2020.04.020.
Martin Ginis KA, Latimer AE, Arbour-Nicitopoulos KP, Buchholz AC, Bray SR, Craven BC, et al. Leisure time physical activity in a population-based sample of people with spinal cord injury Part I: demographic and injury-related correlates. Arch Phys Med Rehabilit. 2010;91:722–8.
Williams TL, Smith B, Papathomas A. The barriers, benefits and facilitators of leisure time physical activity among people with spinal cord injury: a meta-synthesis of qualitative findings. Health Psychol Rev. 2014;8:404–25.
Tsang K, Hiremath SV, Crytzer TM, Dicianno BE, Ding D. Validity of activity monitors in wheelchair users: a systematic review. J Rehabil Res Dev. 2016;53:641–58.
Nightingale TE, Rouse PC, Thompson D, Bilzon JLJ. Measurement of physical activity and energy expenditure in wheelchair users: methods, considerations and future directions. Sports Med - open. 2017;3:10.
Lankhorst K, Oerbekke M, van den Berg-Emons R, Takken T, de Groot J. Instruments measuring physical activity in individuals who use a wheelchair: a systematic review of measurement properties. Arch Phys Med Rehabilitation. 2020;101:535–52.
Ma JK, McCracken LA, Voss C, Chan FHN, West CR, Martin Ginis KA. Physical activity measurement in people with spinal cord injury: comparison of accelerometry and self-report (the Physical Activity Recall Assessment for People with Spinal Cord Injury). Disabil Rehabilit. 2020;42:240–6.
Conger SA, Scott SN, Fitzhugh EC, Thompson DL, Bassett DR. Validity of physical activity monitors for estimating energy expenditure during wheelchair propulsion. J Phys Act Health. 2015;12:1520–6.
Collins EG, Gater D, Kiratli J, Butler J, Hanson K, Langbein WE. Energy cost of physical activities in persons with spinal cord injury. Med Sci Sports Exerc. 2010;42:691–700.
Martin Ginis KA, van der Scheer JW, Latimer-Cheung AE, Barrow A, Bourne C, Carruthers P, et al. Evidence-based scientific exercise guidelines for adults with spinal cord injury: An update and a new guideline. Spinal Cord. 2018;56:308–21.
Martin Ginis KA, Latimer AE, Craven BC, Hicks AL. Development and evaluation of an activity measure for people with spinal cord injury. Med Sci Sports Exerc. 2005;37:1099–111.
Tanhoffer RA, Tanhoffer AI, Raymond J, Hills AP, Davis GM. Comparison of methods to assess energy expenditure and physical activity in people with spinal cord injury. J Spinal Cord Med. 2012;35:35–45.
Martin Ginis KA, Latimer-Cheung AE Physical Activity Recall Assessment for People with Spinal Cord Injury (PARA-SCI): https://sciactioncanada.ok.ubc.ca/resources/para-sci-manual/. Accessed May 2020.
Latimer AE, Martin Ginis KA, Craven BC, Hicks AL. The physical activity recall assessment for people with spinal cord injury: validity. Med Sci Sports Exerc. 2006;38:208–16.
Martin Ginis KA, Phang SH, Latimer AE, Arbour-Nicitopoulos KP. Reliability and validity tests of the leisure time physical activity questionnaire for people with spinal cord injury. Arch Phys Med Rehabilit. 2012;93:677–82.
Craig CL, Marshall AL, Sjostrom M, Bauman AE, Booth ML, Ainsworth BE, et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc. 2003;35:1381–95.
Cummings I, Lamontagne M-E, Sweet SN, Spivock M, Batcho CS. Canadian-French adaptation and test-retest reliability of the leisure time physical activity questionnaire for people with disabilities. Ann Phys Rehabilitation Med. 2019;62:161–7.
Streiner DL, Norman GR, Cairney J Health Measurement ScalesA practical guide to their development and use, Oxford University Press, New York; 2015.
Ma JK, West CR, Martin, Ginis KA. The effects of a patient and provider co-developed, behavioral physical activity intervention on physical activity, psychosocial predictors, and fitness in individuals with spinal cord injury: a randomized controlled trial. Sports Med. 2019;49:1117–31.
Lithopoulos A, Bassett-Gunter RL, Martin Ginis KA, Latimer-Cheung AE. The effects of gain- versus loss-framed messages following health risk information on physical activity in individuals with multiple sclerosis. J Health Commun. 2017;22:523–31.
Barbonetti A, Cavallo F, D’Andrea S, Muselli M, Felzani G, Francavilla S, et al. Lower vitamin D levels are associated with depression in people with chronic spinal cord injury. Arch Phys Med Rehabil. 2017;98:940–6.
Stapleton JN, Perrier M-J, Campbell DS, Tawse HL, Martin, Ginis KA. Social cognitive predictors of competitive level among athletes with physical disabilities. Psychol Sport Exerc. 2016;22:46–52.
Cronbach LJ, Meehl PE. Construct validity in psychological tests. Psychological Bull. 1955;52:281–302.
Hicks AL, Martin Ginis KA, Pelletier CA, Ditor DS, Foulon B, Wolfe DL. The effects of exercise training on physical capacity, strength, body composition and functional performance among adults with spinal cord injury: a systematic review. Spinal Cord. 2011;49:1103–27.
Krassioukov AV, Currie KD, Hubli M, Nightingale TE, Alrashidi AA, Ramer L, et al. Effects of exercise interventions on cardiovascular health in individuals with chronic, motor complete spinal cord injury: protocol for a randomised controlled trial [Cardiovascular Health/Outcomes: improvements created by exercise and education in SCI (CHOICES) Study]. BMJ Open. 2019;9:e023540.
Kirshblum SC, Burns SP, Biering-Sorensen F, Donovan W, Graves DE, Jha A, et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med. 2011;34:535–46.
Eerden S, Dekker R, Hettinga FJ. Maximal and submaximal aerobic tests for wheelchair-dependent persons with spinal cord injury: a systematic review to summarize and identify useful applications for clinical rehabilitation. Disabil Rehabil. 2018;40:497–521.
Scherr J, Wolfarth B, Christle JW, Pressler A, Wagenpfeil S, Halle M. Associations between Borg’s rating of perceived exertion and physiological measures of exercise intensity. Eur J Appl Physiol. 2013;113:147–55.
Edvardsen E, Hem E, Anderssen SA. End criteria for reaching maximal oxygen uptake must be strict and adjusted to sex and age: a cross-sectional study. PLoS One. 2014;9:e85276.
Simmons OL, Kressler J, Nash MS. Reference fitness values in the untrained spinal cord injury population. Arch Phys Med Rehabil. 2014;95:2272–8.
Streiner DL. Best (but oft-forgotten) practices: the multiple problems of multiplicity—whether and how to correct for many statistical tests. Am J Clin Nutr. 2015;102:721–8.
Cohen J. A power primer. Psychological Bull. 1992;112:155–9.
van der Scheer JW, de Groot S, Tepper M, Faber W, Veeger DH, van der Woude LH. Low-intensity wheelchair training in inactive people with long-term spinal cord injury: a randomized controlled trial on fitness, wheelchair skill performance and physical activity levels. J Rehabil Med. 2016;48:33–42.
Lee PH, Macfarlane DJ, Lam TH, Stewart SM. Validity of the international physical activity questionnaire short form (IPAQ-SF): a systematic review. Int J Behav Nutr Phys Act. 2011;8:115.
Bouchard C, An P, Rice T, Skinner JS, Wilmore JH, Gagnon J, et al. Familial aggregation ofV˙o 2 max response to exercise training: results from the HERITAGE family study. J Appl Physiol. 1999;87:1003–8.
West CR, Gee CM, Voss C, Hubli M, Currie KD, Schmid J, et al. Cardiovascular control, autonomic function, and elite endurance performance in spinal cord injury. Scand J Med Sci Sports. 2015;25:476–85.
Goodwin LD, Leech NL. Understanding correlation: factors that affect the size of r. J Exp Educ. 2006;74:249–66.
Booth M. Assessment of physical activity: an international perspective. Res Q Exerc Sport. 2000;71:114–20.
Perrier MJ, Stork MJ, Martin Ginis KA. Type, intensity and duration of daily physical activities performed by adults with spinal cord injury. Spinal Cord. 2017;55:64–70.
Hettinga FJ, Valent L, Groen W, van Drongelen S, de Groot S, van der Woude LHV. Hand-cycling: an active form of wheeled mobility, recreation, and sports. Phys Med rehabilitation Clin North Am. 2010;21:127–40.
Au JS, Totosy De Zepetnek JO, Macdonald MJ. Modeling perceived exertion during graded arm cycling exercise in spinal cord injury. Med Sci Sports Exerc. 2017;49:1190–6.
Totosy de Zepetnek JO, Au JS, Hol AT, Eng JJ, MacDonald MJ. Predicting peak oxygen uptake from submaximal exercise after spinal cord injury. Appl Physiol Nutr Metab. 2016;41:775–81.
Hiremath SV, Ding D, Farringdon J, Vyas N, Cooper RA. Physical activity classification utilizing SenseWear activity monitor in manual wheelchair users with spinal cord injury. Spinal Cord. 2013;51:705–9.
Nightingale TE, Walhin JP, Thompson D, Bilzon JLJ Predicting physical activity energy expenditure in wheelchair users with a multisensor device. BMJ Open Sport Exercise Med. 2015; 1: bmjsem-2015-000008. https://doi.org/10.1136/bmjsem-2015-000008.
Acknowledgements
We thank Adrienne Sinden for her assistance with manuscript preparation.
Funding
This study was funded by a project grant from the Canadian Institutes of Health Research (CIHR) with the funding reference number (TCA 118348). The first author holds the Reichwald Family Southern Medical Program Chair in Chronic Disease Prevention.
Author information
Authors and Affiliations
Contributions
KAMG was responsible for conceptualizing and designing the study, interpreting results and writing the report. JU-C was responsible for analyzing the data, writing the results, creating tables and providing feedback on the report. AAA was responsible for collecting and cleaning the data, drafting the methods section and providing feedback on the report. TEN was responsible for assisting during data collection, drafting the methods section, assisting with data interpretation, and providing feedback on the report. JSA was responsible for assisting in the design of the study protocol, drafting the methods section, assisting with data interpretation, and providing feedback on the report. KDC was responsible for assisting during data collection and providing feedback on the report. MH was responsible for assisting during data collection and providing feedback on the report. AK is the Principal Investigator for the CHOICES study and was responsible for designing and overseeing implementation of all aspects of the CHOICES protocol and providing feedback on the report.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics
Ethics approval was obtained from the University of British Columbia (H12-02945-11), McMaster University (12–672) and Toronto Rehabilitation Institute – University Health Network (12–5797).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Martin Ginis, K.A., Úbeda-Colomer, J., Alrashidi, A.A. et al. Construct validation of the leisure time physical activity questionnaire for people with SCI (LTPAQ-SCI). Spinal Cord 59, 311–318 (2021). https://doi.org/10.1038/s41393-020-00562-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41393-020-00562-9
This article is cited by
-
A Comparison of Neuropathic Pain Experiences Among Paralympic Versus Recreational Athletes with Spinal Cord Injury
Sports Medicine - Open (2023)
-
The effects of active upper-limb versus passive lower-limb exercise on quality of life among individuals with motor-complete spinal cord injury
Spinal Cord (2022)
-
Implementation of the spinal cord injury exercise guidelines in the hospital and community settings: Protocol for a type II hybrid trial
Spinal Cord (2022)
-
Associations between left ventricular structure and function with cardiorespiratory fitness and body composition in individuals with cervical and upper thoracic spinal cord injury
Spinal Cord (2021)