Abstract
Purpose
Accurate prediction of competing risks of mortality remains a key component of prostate cancer treatment decision-making. We sought to validate the Prostate Cancer Comorbidity Index (PCCI) score for predicting other-cause mortality (OCM) and cancer outcomes in men undergoing radical prostatectomy (RP).
Materials and methods
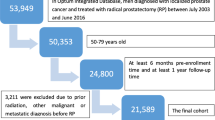
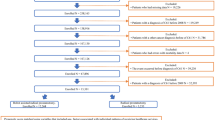
We sampled 4857 men with prostate cancer treated with RP in the VA from 2000–2018. Risks of OCM, 90-day all-cause mortality (ACM), prostate cancer-specific mortality, metastasis, and biochemical recurrence by PCCI score were assessed using Cox proportional hazards and logistic regression. We compared prediction of 90-day ACM between PCCI and the American Society of Anesthesiology (ASA) score, a validated predictor of short-term mortality.
Results
Over median follow-up of 6.7 years (IQR 3.7–10.3), there was a stepwise increase in risk of OCM with higher PCCI score, with hazards (95%CI) of 1.53 (1.14–2.04), 2.11 (1.55–2.88), 2.36 (1.68–3.31), 3.61 (2.61–4.98), and 4.99 (3.58–6.96) for PCCI 1-2, 3-4, 5-6, 7-9, and 10 + (vs. 0), respectively. Projected 10-year cumulative incidence of OCM was 8%, 12%, 16%, 19%, 26%, and 32% for scores of 0, 1-2, 3-4, 5-6, 7-9, and 10+ , respectively. Men with PCCI 7+ had greater odds of 90-day ACM (OR 3.48, 95%CI 1.26–9.63) while men with higher ASA did not. Higher PCCI score was associated with worse cancer outcomes, with the highest categories driving the associations.
Conclusions
The PCCI is a robust measure of short- and long-term OCM after RP, validated for use in clinical care and health services research focusing on surgical patient populations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Daskivich TJ, Kwan L, Dash A, Greenfield S, Litwin MS. Weighted versus unweighted Charlson score to predict long-term other-cause mortality in men with early-stage prostate cancer. Eur Urol. 2014;66(6):1002–9.
Daskivich TJ, Thomas IC, Luu M, Shelton JB, Makarov DV, Skolarus TA, et al. External validation of the prostate cancer specific comorbidity index: A claims based tool for the prediction of life expectancy in men with prostate cancer. J Urol. 2019;202(3):518–24.
Frendl DM, FitzGerald G, Epstein MM, Allison JJ, Sokoloff MH, Ware JE. Predicting the 10-year risk of death from other causes in men with localized prostate cancer using patient-reported factors: Development of a tool. PLoS One. 2020;15(12):e0240039.
Albertsen PC, Moore DF, Shih W, Lin Y, Li H, Lu-Yao GL. Impact of comorbidity on survival among men with localized prostate cancer. J Clin Oncol. 2011;29(10):1335–41.
Sohlberg EM, Thomas IC, Yang J, Kapphahn K, Daskivich TJ, Skolarus TA, et al. Life expectancy estimates for patients diagnosed with prostate cancer in the Veterans Health Administration. Urol Oncol. 2020;38(9):734 e731–4.
Tewari A, Johnson CC, Divine G, CRAWFORD ED, GAMITO EJ, DEMERS R, et al. Long-term survival probability in men with clinically localized prostate cancer: a case-control, propensity modeling study stratified by race, age, treatment, and comorbidities. J Urol. 2004;171(4):1513–9.
Walz J, Gallina A, Saad F, Montorsi F, Perrotte P, Shariat SF, et al. A nomogram predicting 10-year life expectancy in candidates for radical prostatectomy or radiotherapy for prostate cancer. J Clin Oncol. 2007;25(24):3576–81.
Froehner M, Koch R, Hubler M, Wirth MP. Validation of an age-adjusted prostate cancer-specific comorbidity index. Eur Urol. 2016;69(5):764–6.
Daskivich TJ, Kwan L, Dash A, Saigal C, Litwin MS. An age adjusted comorbidity index to predict long-term, other cause mortality in men with prostate cancer. J Urol. 2015;194(1):73–8.
Daskivich TJ, Chamie K, Kwan L, Labo J, Dash A, Greenfield S, et al. Improved prediction of long-term, other cause mortality in men with prostate cancer. J Urol. 2011;186(5):1868–73.
Daskivich TJ, Thomas IC, Luu M, Shelton JB, Makarov DV, Skolarus TA, et al. Reply by authors. J Urol. 2020;203(2):421.
Daskivich TJ, Fan KH, Koyama T, Albertsen PC, Goodman M, Hamilton AS, et al. Effect of age, tumor risk, and comorbidity on competing risks for survival in a U.S. population-based cohort of men with prostate cancer. Ann Intern Med. 2013;158(10):709–17.
Fitz-Henry J. The ASA classification and peri-operative risk. Ann R Coll Surg Engl. 2011;93(3):185–7.
Hackett NJ, De Oliveira GS, Jain UK, Kim JY. ASA class is a reliable independent predictor of medical complications and mortality following surgery. Int J Surg. 2015;18:184–90.
Freedland SJ, Humphreys EB, Mangold LA, Eisenberger M, Dorey FJ, Walsh PC, et al. Risk of prostate cancer-specific mortality following biochemical recurrence after radical prostatectomy. JAMA 2005;294(4):433–9.
Froehner M, Kellner AE, Koch R, Baretton GB, Hakenberg OW, Wirth MP. A combined index to classify prognostic comorbidity in candidates for radical prostatectomy. BMC Urol. 2014;14:28.
Daskivich TJ, Litwin MS, Penson DF. Effect of age, tumor risk, and comorbidity in a u.s. Population-based cohort of men with prostate cancer. Ann Intern Med. 2013;159(5):370.
Bechis SK, Carroll PR, Cooperberg MR. Impact of age at diagnosis on prostate cancer treatment and survival. J Clin Oncol. 2011;29(2):235–41.
Huynh-Le MP, Myklebust TÅ, Feng CH, Karunamuni R, Johannesen TB, Dale AM, et al. Age dependence of modern clinical risk groups for localized prostate cancer-A population-based study. Cancer 2020;126(8):1691–9.
Daskivich TJ, Dru CJ, Skarecky D, Ahlering T, Freedland SJ. Association of comorbid disease burden at diagnosis with higher tumor grade in men with non-metastatic prostate cancer. Prostate Cancer Prostatic Dis. 2017;20(3):343–7.
Maurice MJ, Zhu H, Kiechle JE, Kim SP, Abouassaly R. Comorbid disease burden is independently associated with higher risk disease at prostatectomy in patients eligible for active surveillance. J Urol. 2015;195:919–24.
Panigrahi G, Ambs S. How comorbidities shape cancer biology and survival. Trends Cancer 2021;7(6):488–95.
Filson CP, Shelton JB, Tan HJ, Kwan L, Skolarus TA, Saigal CS, et al. Expectant management of veterans with early-stage prostate cancer. Cancer 2016;122(4):626–33.
Daskivich TJ, Chamie K, Kwan L, Labo J, Dash A, Greenfield S, et al. Comorbidity and competing risks for mortality in men with prostate cancer. Cancer 2011;117(20):4642–50.
Daskivich TJ, Fan KH, Koyama T, Albertsen PC, Goodman M, Hamilton AS, et al. Prediction of long-term other-cause mortality in men with early-stage prostate cancer: results from the Prostate Cancer Outcomes Study. Urology 2015;85(1):92–100.
Moghanaki D, Howard LE, De Hoedt A, Aronson WJ, Kane CJ, Amling CL, et al. Validity of the National Death Index to ascertain the date and cause of death in men having undergone prostatectomy for prostate cancer. Prostate Cancer Prostatic Dis. 2019;22(4):633– 5.
Author information
Authors and Affiliations
Contributions
MSC. study concept and design, acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. LEH: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, statistical analysis. SS: analysis and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, statistical analysis. AD: study concept and design, acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. SJF: study concept and design, acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. WA: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. MT: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. ZK: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. CK: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. CA: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. MC: acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support. TJD: study concept and design, acquisition of data, analysis, and interpretation of data, drafting of the manuscript, critical revision of the manuscript for important intellectual content, technical or material support.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Chen, M.S., Howard, L.E., Stock, S. et al. Validation of the prostate cancer comorbidity index in predicting cause-specific mortality in men undergoing radical prostatectomy. Prostate Cancer Prostatic Dis 26, 715–721 (2023). https://doi.org/10.1038/s41391-022-00550-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-022-00550-5
This article is cited by
-
Relative impact of lymph-node metastasis and seminal vesical invasion on oncologic outcomes following radical prostatectomy
Prostate Cancer and Prostatic Diseases (2023)