Abstract
Background
Shiga toxin-producing Escherichia coli is responsible for post-diarrheal (D+) hemolytic uremic syndrome (HUS), which is a cause of acute renal failure in children. The glycolipid globotriaosylceramide (Gb3) is the main receptor for Shiga toxin (Stx) in kidney target cells. Eliglustat (EG) is a specific and potent inhibitor of glucosylceramide synthase, first step of glycosphingolipid biosynthesis, actually used for the treatment of Gaucher’s disease. The aim of the present work was to evaluate the efficiency of EG in preventing the damage caused by Stx2 in human renal epithelial cells.
Methods
Human renal tubular epithelial cell (HRTEC) primary cultures were pre-treated with different dilutions of EG followed by co-incubation with EG and Stx2 at different times, and cell viability, proliferation, apoptosis, tubulogenesis, and Gb3 expression were assessed.
Results
In HRTEC, pre-treatments with 50 nmol/L EG for 24 h, or 500 nmol/L EG for 6 h, reduced Gb3 expression and totally prevented the effects of Stx2 on cell viability, proliferation, and apoptosis. EG treatment also allowed the development of tubulogenesis in 3D-HRTEC exposed to Stx2.
Conclusions
EG could be a potential therapeutic drug for the prevention of acute kidney injury caused by Stx2.
Impact
-
For the first time, we have demonstrated that Eliglustat prevents Shiga toxin 2 cytotoxic effects on human renal epithelia, by reducing the expression of the toxin receptor globotriaosylceramide.
-
The present work also shows that Eliglustat prevents Shiga toxin 2 effects on tubulogenesis of renal epithelial cells.
-
Eliglustat, actually used for the treatment of patients with Gaucher’s disease, could be a therapeutic strategy to prevent the renal damage caused by Shiga toxin.
Similar content being viewed by others
Introduction
Infection with Shiga toxin (Stx)-producing Escherichia coli (STEC) is the main etiology of post-diarrheal (D+) hemolytic uremic syndrome (HUS), also called typical HUS1. HUS is characterized by hemolytic anemia, thrombocytopenia, and acute kidney injury (AKI)2. In Argentina, diarrhea-associated HUS is endemic, being the country with the highest incidence rate in the world, with 10–17 cases per 100,000 children aged <5 years, and a case mortality rate <4%3. Children with AKI due to HUS can result in chronic renal failure and long-term renal sequels in about 30% of cases4 and kidney transplants in about 9% of children and adolescents5. The acute stage of the disease is marked by hematological alterations, oligoanuria/anuria, hypertension, and edema4,6. STEC not only affects children in many parts of the world but also adults, as occurred in Germany during the outbreak of STEC-HUS7.
There is no specific therapy presently available to protect people from the damage caused by Stx, and supportive care is applied to reduce mortality in patients with HUS4. This involves intravenous volume expansion especially in the early phases of the illness, fluid and electrolyte management, packed red blood cell transfusion, and dialysis8.
Cattle have been identified as the main reservoir for STEC. Humans can be contaminated by eating undercooked beef products and by other sources including other domestic animals, fresh fruits and vegetables and products that have been contaminated with manure3,9,10. Drinking or swimming in contaminated water, person-to-person transmission, and contact with infected animals have been described as other infection sources11,12.
Shiga toxin type 1 and 2 (Stx1 and Stx2, respectively) and their variants are the main virulence factors produced by STEC strains, such as O157:H713. However, epidemiological data show that Stx2a-producing STEC strains are more likely to cause HUS than those strains that produce only Stx13,14.
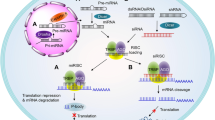
Stx contains a single A subunit bound to a monopentamer of B subunits15,16. The initial step in the renal pathogenesis of STEC-HUS starts with the binding of the B pentamer to the glycolipid globotriaosylceramide (Gb3) located on the cell membrane. Subsequently, Stx is endocytosed and retrograde transported to the endoplasmic reticulum17,18. The A subunit exerts RNA N-glycohydrolase activity on the 28S ribosomal subunit, leading to halt the protein synthesis causing ribotoxic stress and finally apoptosis19,20. Gb3 is the main receptor for Stx, which is highly expressed on the plasma membrane of human kidney cells, such as glomerular endothelial cells, podocytes, mesangial cells, and tubular epithelial cells21,22,23, as well as in other target organs, such as the brain24.
Previous works, carried out in primary cultures of human renal tubular epithelial cells (HRTECs), showed that Stx2 inhibited protein synthesis, decreased cell viability and cell proliferation, and induced apoptosis25,26,27,28. We demonstrated that the compound C-9 (Genzyme, Cambridge, MA), an inhibitor of glucosylceramide (GL) synthase, reduced Gb3 expression and therefore prevented the decrease of cell viability caused by Stx2 in HRTEC primary cultures29 and also in human glomerular endothelial cells (HGECs)30. In addition, in rats intraperitoneally injected with Stx2, treatment with C-9 reduced the animal mortality and the renal injury in the surviving animals31.
Eliglustat (EG), another potent and selective GL synthase inhibitor, has been approved by the US Food and Drug Administration and recently by the National Administration of Drugs, Foods and Medical Devices (ANMAT) in Argentina to be used for the oral treatment of adults with Gaucher’s disease32. Therefore, the aim of the present work was to evaluate the efficiency of EG in preventing the damage caused by Stx2 in HRTEC primary cultures, which are a main target of Stx2 action. Results in the present work show that EG could be used to prevent the human renal damage caused by Stx2.
Materials and methods
Reagents
Stx2a was purchased at Phoenix Lab, Tuft Medical Center, Boston, MA.
EG, also known as Genz-112638, was purchased at MedKoo Biosciences, Inc., Morrisville, NC33.
Cell cultures
Primary cultures of HRTEC were developed from kidneys removed from pediatric patients undergoing nephrectomies, indicated for the correction of urological conditions or tumor resections, at the Hospital General de Pediatría Pedro de Elizalde, Buenos Aires, Argentina. Cortical renal fragments were dissected and processed as described previously28,34. HRTEC primary cultures were grown in RPMI 1640 medium supplemented with 5% fetal bovine serum (FBS), L-glutamine (2 mmol/L), penicillin/streptomycin (100 U/mL), and endothelial cell growth supplement (ECGS) (Merck-Sigma, St. Louis, MO). HRTECs were used between 1 and 5 passages to guarantee the morphogenetic stability of the cells. HRTEC showed a similar morphology observed under light microscopy. Cells were characterized by immunofluorescence, using an antibody against aquaporin 1 (AQP1) (Alpha Diagnostic, San Antonio, TX). More than 90% of the cells were positive for AQP1, indicating their origin in the renal proximal tubule. None of the cells were stained with the endothelial antibody PECAM CD31 (DAKO, Tecnolab, Buenos Aires, Argentina).
In selected experiments, the HK-2 cell line was used. Cells were grown in Dulbecco’s Modified Eagle Medium-F12 medium containing 10% FBS, L-glutamine, and penicillin/streptomycin. All cell cultures were incubated in 5% CO2 and a humidified atmosphere at 37 °C.
Neutral red cytotoxicity assay
Neutral red uptake was performed to evaluate cell viability as was described previously29. For this purpose, HRTEC and HK-2 were seeded in 96-well plates and grown to confluence in culture medium. Cells were then incubated with serial dilutions of Stx2 (0.001–1000 ng/mL) for 24 and 72 h. The concentration of Stx2 able to cause the death of 50% of the cells (CD50) after 72 h of the toxin exposure was established and used for the rest of the experiments.
Next, HRTEC and HK-2 were pre-treated with or without EG (1–500 nmol/L) for 6 and 24 h, followed by co-treatment with same concentration of EG with or without Stx2 (1 or 10 ng/mL), for 24 or 72 h. Control cells were incubated under the same medium conditions but without EG and Stx2 treatments. HRTEC cultures were also co-treated with EG (500 or 5000 nmol/L) and Stx2 (1 ng/mL) during 24 and 72 h. For another set of experiments, HRTEC were pre-incubated with lipopolysaccharide (LPS, 1 μg/mL) (Sigma-Aldrich, St. Louis, MO) with or without 50 nmol/L EG, during 24 h, followed by the addition of Stx2 (1 ng/mL) for 72 h. All treatments were performed under arrest growth conditions without FBS and ECGS.
At the end of the treatments, cells were incubated with a solution of 50 μg/mL neutral red in RPMI medium for 2 h at 37 °C. Cells were then fixed in a solution of CaCl2 (1%) and formaldehyde (4%), solubilized in acetic acid (1%) and ethanol (50%), and absorption was read in an automated plate spectrophotometer at 540 nm29. Cell viability is expressed as neutral red uptake percent with respect to control cells incubated without EG and Stx2.
Cell proliferation assay
Cell proliferation was evaluated by the incorporation of 5-bromo-2-deoxyuridine (BrdU) into cell nuclei during DNA replication, as previously described28. HRTECs were grown to 50–70% confluence on coverslips inserted in a 24-well plate, and all treatments were performed in triplicate. HRTECs were pre-incubated with EG (1–500 nmol/L) for 6 or 24 h, followed by co-incubation with the same dilution of EG with or without Stx2 (1 ng/mL) for 24 h, under arrest growth conditions. Prior to finishing the treatments, all cells received a 2-h pulse of BrdU (10 µmol/L) (Sigma-Aldrich, St. Louis, MO). BrdU uptake into the cell nuclei was detected using a primary antibody anti-BrdU (1:100) (Sigma-Aldrich, St. Louis, MO) and an anti-mouse IgG secondary antibody conjugated with Alexa fluor 488 (1:200) (Invitrogen, Waltham, MA). To count the total number of cells, nuclei were stained with Hoechst (1 µg/mL). Micrographs were taken with a digital camera (Nikon E4300) under a fluorescence microscope (Nikon Eclipse E-2000) and processed using the Image J (NIH) analysis software.
Apoptosis and necrosis
Apoptosis and necrosis were analyzed on HRTEC primary cultures grown on coverslips, as previously described28. Cells grown on coverslips were treated with or without EG and Stx2 as described above for BrdU assay. Each experiment was performed in duplicate. After treatments, cells were incubated with Annexin V–fluorescein isothiocyanate (FITC)–Propidium Iodide (AV-PI) according to manufacturer’s proceedings (BD Biosciences, San Jose, CA). Staining for AV (green) and PI (red) was immediately observed under a fluorescence microscope, and micrographs of each well were taken as described above.
Negative cells for both AV and PI (AV−/PI−) staining were considered live cells; AV-positive and PI-negative (AV+/PI−) stained cells were considered in primary apoptosis; both AV- and PI-positive (AV+/PI+) and AV-negative and PI-positive (AV−/PI+) stained cells were considered necrotic cells.
For some assays, after treatments, cells were treated with trypsin to detach from the coverslips and the number of cells was counted in a Neubauer chamber.
Tubulogenesis assay
Confluent HRTECs were pre-treated with or without 50 nmol/L EG for 24 h, followed by co-treatment with EG and 1 ng/mL Stx2 for 24 h. Some cells were treated with EG without Stx2, and control cells were incubated without Stx2 and EG. All treatments were performed under arrest growth conditions. After treatments, cells were detached and washed, and three-dimensional (3D) cultures of HRTECs (3D-HRTEC) were developed34. For this purpose, 4 × 104 treated cells were seeded per well on matrigel (Sigma-Merck, St. Louis, MO) and incubated in culture medium containing the same supplements used for HRTEC primary cultures34. Cell aggregation and formation of tubular shape structures was observed under an inverted optical microscope (Nikon Eclipse TS100), and micrographs of two different assays were taken with a digital camera (Nikon Coolpix S10).
Glycolipid extraction and thin layer chromatography (TLC)
Expression of Gb3 receptor was analyzed in HRTECs by TLC as described previously30,35. Cells were grown in culture flasks at 37 °C in an atmosphere of 5% CO2 to almost confluence and incubated then with or without 50 nmol/L EG for 24, 48, and 96 h, or 500 nmol/L EG for 6 h, in arrest growth conditions. Some cells were treated with EG (50 nmol/L) for 24 h followed by co-treatment with EG and Stx2 (1 ng/mL) for another 24 h. Control cells were incubated in arrest growth conditions without treatment. After treatments, total glycolipids were extracted from HRTECs, following a modified protocol of Bligh and Dyer method36. Briefly, 4 mL of chloroform:methanol:water (1:2:1 v/v) were added to 2.5 × 106 cells and incubated on ice for 15 min. Subsequently, 2.5 mL of chloroform:methanol:water (1:1:0.5) were added to the tube and the mixture was centrifuged to separate phases. The lower phase was dried, and submitted to alkaline hydrolysis in 1 mL of methanol and 0.1 mL of NaOH (1.0 N) during 16 h at 37 °C. To separate phases, 2 mL chloroform and 0.5 mL water were added, and the chloroform phase with neutral glycolipids was dried and used for the determination of Gb3 expression. Aliquots of glycolipids extracts were dissolved in chloroform–methanol (2:1) and separated by TLC in a mix of chloroform, methanol, and water (65:35:8). Samples were compared to a purified Gb3 standard (0.5–2.0–μg; Matreya, State College, PA). The glycolipids bands were revealed after treating the TLC plate with a solution of orcinol (Acros Organics, Belgium). The densitometric analysis of Gb3 bands was performed by the Image J software.
Statistical analysis
Results are reported as mean ± standard error of the mean (SEM). Student’s t test was used for individual comparisons. One-way analysis of variance followed by Tukey post hoc test was used for comparison of three or more groups. A p value < 0.05 was considered significant. The statistical analysis was performed using the GraphPad software.
Results
EG prevents the cytotoxic effects of Stx2 on HRTEC and HK-2 cell viability
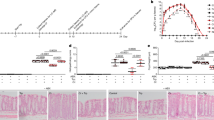
Confluent HRTEC primary cultures and HK-2 cell line were incubated with different Stx2 concentrations for 24 and 72 h. Cell viability was then evaluated by neutral red uptake. The CD50 of Stx2, estimated from the dose–response curves of cell viability, was 1 ng/mL at 72 h for HRTEC (Fig. 1a) and 10 ng/mL at 72 h for HK-2 (Fig. 1b).
HRTEC (a) and HK-2 (b) cultures were treated with serial dilutions of Stx2 for 24 and 72 h, and cell viability was measured by neutral red uptake assay. Results represent cell viability percent with respect to control untreated cells (100%). Dotted lines indicate the CD50 of Stx2 in HRTEC (a) and HK-2 (b). Results are expressed as mean ± SEM of a representative experiment of three assays realized in triplicate. Student’s t test indicates significant differences *p < 0.05, **p < 0.01, and ***p < 0.001 for Stx2 vs. non-treated cells.
To evaluate whether EG protects renal epithelial cells from Stx2 cytotoxic effect, cell viability was assessed in HRTEC and HK-2 monolayers pre-incubated with different concentrations of EG for 6 h or 24 h, followed by the addition of 1 and 10 ng/mL Stx2, respectively, for 24 or 72 h. The treatment of either HRTEC or HK-2 with EG significantly prevented the cytotoxic effect of Stx2 in a dose- and time-dependent manner (Fig. 2a, b).
HRTEC (a) and HK-2 (b) cultures were incubated with or without Stx2 (1 and 10 ng/mL, respectively) for 24 or 72 h or were pre-incubated with different concentrations of Eliglustat (EG) for 6 and 24 h, followed by the addition of Stx2 for 24 or 72 h. c shows results of HRTECs pre-incubated with or without lipopolysaccharide (LPS, 1 μg/mL) and/or EG (500 nmol/L) for 24 h, followed by the addition of Stx2 for 72 h. All graphics express the cell viability percent with respect to control non-treated cells representing 100%. Results are expressed as mean ± SEM of representative experiments performed in triplicates or quadruplicates. ANOVA followed by Tukey post hoc test indicate significant differences: *p < 0.05, **p < 0.01, and ***p < 0.001 for Stx2 or EG + Stx2 vs. non-treated cells and vs. cells treated with same dilution of EG and without Stx2; #p < 0.05 for LPS + Stx2 vs. Stx2.
Pre-incubation of HRTEC with 50 nmol/L EG for 24 h completely prevented the decrease of cell viability caused by 1 ng/mL Stx2 at 24 h and also at 72 h (Fig. 2a). Moreover, the pre-incubation with 500 nmol/L EG for 6 h was enough to totally prevent the reduction of cell viability caused by Stx2 at 24 h (Fig. 2a).
In addition, pre-incubation of HK-2 with 1 nmol/L EG for 24 h or 10 nmol/L EG for 6 h totally prevented the reduction of cell viability caused by 10 ng/mL Stx2 at 24 h (Fig. 2b). Furthermore, pre-incubation of HK-2 with 10 nmol/L EG, for 24 h, totally prevented the Stx2 cytotoxicity at 72 h.
The incubation of HRTEC and HK-2 with EG alone did not modify cell viability at any dose and time tested compared to untreated control cells, considered as 100% cell viability (Fig. 2a, b).
Co-incubation of HRTEC with EG (500 nmol/L) and Stx2 (1 ng/mL), for 24 and 72 h, did not protect the cells from the cytotoxic effect of Stx2 (data not shown). HRTEC co-incubated with a higher concentration of EG (5 μmol/L) and Stx2 partially protected the cells from Stx2 effect at 72 h, but not at 24 h (data not shown).
Furthermore, the pre-incubation of HRTEC with LPS (1 μg/mL), followed with the addition of Stx2 (1 ng/mL) for 72 h, significantly increased the effect of Stx2 on cell viability (Fig. 2c). Nevertheless, the pre-incubation of HRTEC with EG (50 nmol/L) for 24 h protected the cells from the combined effect of LPS and Stx2 at 72 h of exposure (Fig. 2c). Cells incubated with EG or LPS alone, or with both EG and LPS, showed no significant differences compared to control non-treated cells.
EG prevents the inhibitory effects of Stx2 on cell proliferation
Cell proliferation was evaluated by BrdU uptake in HRTEC primary cultures grown on coverslips. Representative microphotographs in Fig. 3a show that the incubation of HRTECs with 1 ng/mL Stx2, for 24 h, significantly reduced the number of cell nuclei that incorporated BrdU, and the number of cells attached, with respect to non-treated control cells. The percentage of BrdU uptake was 23.1 ± 6.7% in control cells and 7.6 ± 0.2% in HRTECs exposed to Stx2 (Fig. 3b), which demonstrates that Stx2 significantly decreased the cell proliferation rate in HRTEC cultures.
a Representative microphotographs show BrdU uptake in HRTEC treated with: Stx2: 1 ng/mL, for 24 h; EG + Stx2: 50 nmol/L EG for 24 h, followed by EG + Stx2 for 24 h; and Control: non-treated HRTEC cultures. Scale bars = 50 μm. BrdU uptake was calculated by counting BrdU-positive cells (green nuclei) per total number of cells (blue nuclei) stained with Hoechst. Graphics show BrdU uptake percent in cells pre-incubated with or without different dilutions of EG for 24 h (b) or 6 h (c) followed by incubation with the same dilution of EG in the presence or absence of Stx2 (1 ng/mL) for another 24 h. Results are expressed as mean ± SEM for n = 3 of a representative experiment of three assays. ANOVA followed by Tukey post hoc test indicate significant differences: *p < 0.05, **p < 0.01, and ***p < 0.001 for Stx2 or EG + Stx2 vs. untreated cells and vs. cells treated with the same dilution of EG and without Stx2.
Cell proliferation was also evaluated in HRTEC cultures pre-treated with different concentrations of EG during 6 or 24 h, followed by co-incubation with the same EG concentrations with or without Stx2 (1 ng/mL) for 24 h. Pre-treatment of HRTEC with 50 nmol/L EG for 24 h (Fig. 3b) or 500 nmol/L EG for 6 h (Fig. 3c), followed by the addition of Stx2 for 24 h significantly prevented, at about 100%, the inhibition of BrdU uptake caused by Stx2. The treatment of HRTEC with EG in the absence of Stx2 did not alter significantly the BrdU uptake compared to untreated control cells (Fig. 3b, c)
EG prevents the induction of apoptosis and necrosis caused by Stx2
Apoptosis and necrosis were assessed by the incorporation of AV-FITC/PI into HRTEC primary cultures. As shown in representative micrographs in Fig. 4a, the significant increase of primary apoptotic cells (AV+) caused by Stx2 was prevented by EG treatment. Incubation of HRTECs with Stx2 (1 ng/mL, 24 h) enhanced the percentage of primary (AV+/PI−) apoptotic cells (15 ± 1.3%) to about double compared to non-treated control cells (7.9 ± 0.9%) (Fig. 4b, c). Pre-treatment of HRTEC with 50 nmol/L EG for 24 h (Fig. 4b) or 500 nmol/L EG for 6 h (Fig. 4c) followed by co-treatment with EG and Stx2 for another 24 h completely prevented the apoptotic stimuli of Stx2.
AV/PI incorporation was used to evaluate cell death in HRTEC. a Representative microphotographs show merge images of apoptotic cells that incorporated AV (green) with or without PI (red), and their corresponding white and black images with total cells, in HRTECs treated with: Stx2: 1 ng/mL, for 24 h; EG + Stx2: 50 nmol/L EG for 24 h, followed by EG + Stx2 for 24 h; and Control: non-treated HRTEC cultures. Inset in the image of cells treated with Stx2 shows a detail of a cell stained with both AV/PI (yellow-green). Scale bar = 100 μm. Primary apoptosis (AV+/PI−) was quantified in HRTECs pre-treated with different concentrations of EG for 24 h (b) or 6 h (c), followed by the addition of Stx2 (1 ng/mL) for 24 h. d, e show the percentage of AV+/PI+ and AV−/PI+ cells in HRTEC cultures pre-treated with EG for 24 and 6 h, respectively. Results are expressed as mean ± SEM of three independent experiments. ANOVA followed by Tukey post hoc test indicate significant differences; *p < 0.05, and **p < 0.01, for Stx2 or EG + Stx2 vs. untreated Control cells and vs. cells treated with the same dilution of EG and without Stx2.
Moreover, Fig. 4d, e show that Stx2 also induced a significant rise in the percentage of AV−/PI+ and AV+/PI+ (7.0 ± 2.0%) necrotic cells, compared to control (4.5 ± 1.1%) cultures. Furthermore, the toxin induced the percentage of dead cells (25–30%) detached from the coverslips, which could have undergone apoptosis and/or necrosis. These Stx2 effects were completely prevented by the same EG treatments used for studies shown above, corroborating doses and treatment times. EG alone did not induce significant apoptosis or necrosis in any of the studies performed in HRTECs.
EG prevents the effect of Stx2 on 3D-HRTEC cultures
To investigate the ability of EG to prevent the effect of Stx2 in 3D-HRTEC cultures, primary cultures were pre-incubated with or without 50 nmol/L EG, followed by the addition of 1 ng/mL Stx2 for 24 h. Cells were then seeded on matrigel to develop 3D-HRTEC (Fig. 5). Control cells migrated, formed multicellular cords (5 h), and cellular aggregates (day 1) emerged and evolved into structures with tubular appearance at day 4 on matrigel. The exposure to 1 ng/mL Stx2 completely inhibited cell migration and aggregation showing cell debris and dead cells trapped in the matrix on the fourth day, compared to the appearance of tubular structures in control HRTEC at this time. Pre-treatment with 50 nmol/L EG for 24 h allowed HRTEC to migrate and aggregate despite having been exposed to the toxin and to develop tubular structures like in control HRTEC (Fig. 5).
HRTEC cultures were treated or not with Stx2 (1 ng/mL, 24 h). Some of them were pre-treated with EG (50 nmol/L) for 24 h followed by co-treatment with the same concentration of EG and Stx2 for 24 h. After treatments, cells were seeded on matrigel to develop 3D-HRTEC cultures. Representative micrographs show that non-treated control cells aggregated (5 h–1 day) and developed tubular structures (4 days). Cells incubated with Stx2 remained scattered (5 h-4 days). Cells treated with EG prevented the effect of Stx2 showing the development of 3D-HRTEC cultures similar to controls. Scale bars = 100 μm.
EG decreases Gb3 expression in HRTEC primary cultures
The effect of EG on Gb3 expression was evaluated in HRTEC primary cultures by TLC assay. Figure 6a shows that the treatment of HRTEC with 50 nmol/L EG, for 24 h, significantly decreased the expression levels of Gb3 receptor, which remained low until 96 h of incubation. Similarly, the incubation of HRTEC with 500 nmol/L EG, for only 6 h, significantly decreased Gb3 expression. The decrease in Gb3 expression due to EG treatment may explain the effect of EG in preventing the Stx2 activity in human kidney epithelial cells.
HRTEC were treated with: a 500 nmol/L EG for 6 h; 50 nmol/L EG for 24–96 h; b 1 ng/mL Stx2 for 24 h; or pre-treated with or without 50 nmol/L EG followed by addition of Stx2 for 24 h. Glycolipids extracted from control non-treated or treated HRTECs (2.5 × 106) were separated by TLC and detected with orcinol (a, b). Graphics show the densitometric analysis of Gb3 bands. Data are expressed as mean ± SD of two independent experiments.
As shown in Fig. 6b, co-incubation of HRTEC with Stx2 and 50 nmol/L EG, for 48 h, also produced a significant reduction in Gb3 expression. Moreover, Gb3 expression in HRTEC treated with Stx2 alone was comparable to that of untreated control cells.
Discussion
The present work demonstrates that EG prevents Stx2 cytotoxic effects on HRTECs, one of the main targets of the toxin. A strategy is proposed based on short-term inhibition of GL synthase, first step in the glycosphingolipid biosynthesis, to inhibit Gb3 expression and therefore avoid the binding and action of Stx2 in renal cells expressing Gb3.
The exposure of HRTEC to Stx2 inhibited cell viability and stimulated the percentage of apoptosis, which corroborates previous results of our group and others25,26,27,28. Although 24 h after incubation with Stx2 most of the cells still survived, a significant inhibition in cell proliferation and an increase in apoptosis and necrosis were observed in the remaining cells. Therefore, cell proliferation and apoptosis mechanisms were observed at 24 h, before most of the cells were detached due to Stx2.
The treatment with EG prevented Stx2 effect on cell viability in a dose- and time-dependent manner in HRTEC primary cultures. These results were also obtained in the human proximal tubule cell line HK-2. Furthermore, EG protection against Stx2 was also observed on cell proliferation, and apoptosis/necrosis mechanisms in HRTEC primary cultures.
We have previously shown that 3D-HRTEC cultures developed tubulogenesis resembling the original tissue characteristics, which was inhibited by pre-exposure to Stx234. Herein the treatment with EG allowed HRTECs to develop tubular structures as in control cultures and prevented Stx2 effect on tubulogenesis.
Our group has been studying the effect of different GL synthase inhibitors on renal cells. In the present work, EG was more effective in a time and dose manner, comparing with our previous results using the compound C-9, another GL synthase inhibitor, in HRTEC primary cultures. While the treatment of HRTEC with EG in the nanomolar range (50 nmol/L) significantly reduced Gb3 expression and completely protected from Stx2 effects, higher concentrations of C-9 (1–5 μmol/L) in the order of micromolar, with a minimal pre-incubation time of 24 h, were necessary in the primary cultures29. The effect of EG to prevent the toxin action was maintained up to 72 h in HRTEC as well as in HK-2 exposed to both Stx2 and EG. Moreover, a shorter pre-incubation time with EG (500 nmol/L), for only 6 h, was enough to inhibit Gb3 expression and produce a total protective effect from Stx2 in HRTEC primary cultures. These results demonstrate that EG protects HRTEC cultures from Stx2 action by reducing the expression of Gb3 receptor.
Moreover, the treatment of HRTECs with EG followed by the addition of Stx2 also reduced Gb3 expression to the same level as with the treatment with EG alone, indicating that Stx2 does not interfere with EG mechanism of action.
Co-treatment of HRTEC with 500 nmol/L EG and Stx2 did not protect the cells from Stx2 activity. Although a higher concentration of EG (5 µmol/L) protected HRTEC cultures from Stx2 cytotoxic effect at 72 h without a pre-incubation period, this protective effect did not occur at 24 h. These results demonstrate that a minimum period of time is necessary for EG to inhibit the expression of the Stx2 receptor and therefore exert a protective effect.
The treatment with EG also avoided the Stx2-mediated cytotoxic effect enhanced by LPS. We have previously shown that the sensitivity of HRTEC cultures to Stx2-mediated cytotoxic effect was increased by LPS and others pro-inflammatory factors26. Besides, it was demonstrated that both Stx and LPS are required to elicit the triad of HUS symptoms37. The toxin may be absorbed from the inflamed gastrointestinal tract together with LPS, a major product of Gram-negative bacteria as STEC, and induce synergistic effect during Stx-induced HUS, which could be due to an increase in the expression of the Gb3 receptor produced by LPS38.
We have previously shown that the treatment with C-9 for 48 h significantly reduced the expression of both GL synthase and Gb3 receptor in HRTEC primary cultures. The inhibition of GL synthase and Gb3 was also observed in the kidney of rats orally treated with C-929,31. Moreover, the treatment of HK-2 and HGEC primary cultures with Miglustat (750 μmol/L for 48 h), another GL synthase inhibitor, also reduced significantly the Gb3 expression and only partially prevented the effect of Stx235. Other studies showed that the incubation of HGEC with the ceramide analogous D-PDMP, another inhibitor of glycosphingolipid synthesis, with a concentration in the order of micromolar (5 µM) for 72 h, reduced Gb3Cer and Gb4 content23.
Hence, both HRTEC and HK-2 cultures express Gb3 and are sensitive to Stx2. Herein dose–response curves show that HRTECs are more sensitive to Stx2 than HK-2. These results may be due to the differences between established cell lines and primary cultures. Established cell lines often differ from original cells. However, the activity of Stx2 in this work was comparable to that observed in previous studies with C-9 in primary cultures29.
The GL synthesis is the first step in the biosynthesis of Gb3 and other glycosphingolipids39. This reaction is catalyzed by GL synthase, which glycosylates the ceramide using uridine diphospho-glucose40. Galactose is then added to GL-producing lactosylceramide, followed by the addition of another galactose to produce Gb341. Different inhibitors of GL synthase have been synthesized and tested for treating several glycosphingolipidoses diseases33,41,42. Studies in cell cultures demonstrated that these compounds inhibit glycosphingolipid synthesis but do not alter cell growth or increase intracellular ceramide levels39. Herein the treatment of HRTEC and HK-2 with EG alone did not produce any significant effect compared to non-treated control cells in any of the times and doses assayed, as well as in all the mechanisms studied, indicating that this compound does not interfere with tubular epithelial growth and morphology.
GL synthase inhibitors have been evolved, changing the chemical conformation of the compounds, for better efficiency and specificity41. These modifications resulted in a compound with an improved action such as EG. EG (also known as Genz-112638) and C-9 (also known as Genz-123346) were reported to have comparable effects in rodents. However, EG was demonstrated to have a better pharmacokinetic and pharmacodynamic profile for the use in humans and contains a natural ceramide structure, compared to C-943. Therefore, it was of our interest to evaluate EG, now used for the treatment of Gaucher’s disease, in renal human epithelial cells for the prevention of Stx2 activity.
For several years, different ways of preventing the binding of Stx to target organs have been studied44,45,46,47,48,49. However, at present, there is no effective therapy available for human use to prevent infection with STEC or to protect from Stx2 effects and development of HUS. Taking into account that in patients HUS development occurs between several days after bloody diarrhea appears, it would be relevant to find an efficient treatment that could be administrated during this period to avoid the action of Stx2 in the target organs and the development of the disease. In this sense, our studies demonstrate that EG was effective in preventing the action of Stx2 in the human tubular renal epithelia at shorter treatment times and at lower concentrations than other GL synthase inhibitors previously studied. Further studies in experimental animal models will be developed to corroborate the action of EG in vivo. The treatment with EG could be a therapeutic strategy to prevent the action of Stx2 in target tissues and the development of AKI in diarrhea-associated HUS patients.
References
Karmali, M. A. et al. The association between hemolytic uremic syndrome and infection by verotoxin-producing Escherichia coli. J. Infect. Dis. 151, 775–782 (1985).
Gianantonio, C., Vitacco, M., Mendiaharzu, F. & Rutty, A. The hemolytic-uremic syndrome. J. Pediatr. 64, 478–491 (1964).
Rivas, M., Chinen, I., Miliwebsky, E. & Masana, M. Risk factors for Shiga toxin-producing Escherichia coli-associated human diseases. Microbiol. Spectr. https://doi.org/10.1128/microbiolspec.EHEC-0002-2013 (2014).
Balestracci, A., Battaglia, L. M., Toledo, I., Martin, S. M. & Alvarado, C. Prodromal phase of hemolytic uremic syndrome related to shiga toxin-producing Escherichia coli: the wasted time. Pediatr. Emerg. Care https://doi.org/10.1097/PEC.0000000000001850 (2019).
National System of Procurement and Transplant Information of the Argentine Republic. Report of patients registered on the waiting list. http://www.sintra.incucai.gov.ar (2020).
Repetto, H. A. Epidemic hemolytic-uremic syndrome in children. Kidney Int. 52, 1708–1719 (1997).
Frank, C. H. et al. Epidemic profile of Shiga-toxin-producing Escherichia coli O104:H4 outbreak in Germany. N. Engl. J. Med. 365, 1771–1780 (2011).
Cody, E. M. & Dixon, B. P. Hemolytic uremic syndrome. Pediatr. Clin. North Am. 66, 235–246 (2019).
Hussein, H. S. & Bollinger, L. M. Prevalence of Shiga toxin-producing Escherichia coli in beef cattle. J. Food Prot. 68, 2224–2241 (2005).
Meichtri, L. et al. Shiga toxin-producing Escherichia coli in healthy young beef steers from Argentina: prevalence and virulence properties. Int. J. Food Microbiol. 96, 189–198 (2004).
Ludwig, K. et al. Shiga toxin-producing Escherichia coli infection and antibodies against Stx2 and Stx1 in household contacts of children with enteropathic hemolytic-uremic syndrome. J. Clin. Microbiol. 40, 1773–1782 (2002).
Rivas, M., Miliwebsky, E., Chinen, I., Deza, N. & Leotta, G. The epidemiology of hemolytic uremic syndrome in Argentina. Diagnosis of the etiologic agent, reservoirs and routes of transmission. Medicine 66, 27–32 (2006).
Kaper, J. B., Nataro, J. P. & Mobley, H. L. Pathogenic Escherichia coli. Nat. Rev. Microbiol. 2, 123–140 (2004).
Basu, D. & Tumer, N. E. Do the A subunits contribute to the differences in the toxicity of Shiga toxin 1 and Shiga toxin 2? Toxins 7, 1467–1485 (2015).
O’Brien, A. D. & Holmes, R. K. Shiga and Shiga-like toxins. Microbiol. Rev. 51, 206–220 (1987).
Lingwood, C. A. Role of verotoxin receptors in pathogenesis. Trends Microbiol. 4, 147–153 (1996).
Sandvig, K. et al. Retrograde transport of endocytosed Shiga toxin to the endoplasmic reticulum. Nature 358, 510–512 (1992).
Johannes, L. & Römer, W. Shiga toxins – from cell biology to biomedical applications. Nat. Rev. Microbiol. 8, 105–116 (2010).
Endo, Y. et al. Site of action of a Vero toxin (VT2) from E. coli O157:H7 and of Shiga toxin on eukaryotic ribosomes. RNA N-glycosidase activity of the toxins. Eur. J. Biochem. 171, 45–50 (1988).
Tesh, V. L. Activation of cell stress response pathways by Shiga toxins. Cell. Microbiol. 14, 1–9 (2012).
Psotka, M. A. et al. Shiga toxin 2 targets the murine renal collecting duct epithelium. Infect. Immun. 77, 959–969 (2009).
Obrig, T. G. & Karpman, D. Shiga toxin pathogenesis: kidney complications and renal failure. Curr. Top. Microbiol. Immunol. 357, 105–136 (2012).
Legros, N. et al. Colocalization of receptors for Shiga toxins with lipid rafts in primary human renal glomerular endothelial cells and influence of D-PDMP on synthesis and distribution of glycosphingolipid receptors. Glycobiology 27, 947–965 (2017).
Legros, N. et al. Shiga toxin glycosphingolipid receptors and their lipid membrane ensemble in primary human blood-brain barrier endothelial cells. Glycobiology 27, 99–109 (2017).
Karpman, D. et al. Apoptosis of renal cortical cells in the hemolytic-uremic-syndrome: in vivo and in vitro studies. Infect. Immun. 66, 636–644 (1998).
Pistone Creydt, V., Silberstein, C., Zotta, E. & Ibarra, C. Cytotoxic effect of Shiga toxin-2 holotoxin and its B subunit on human renal tubular epithelial cells. Microbes Infect. 8, 410–419 (2006).
Silberstein, C., Pistone Creydt, V., Gerhardt, E., Nuñez, P. & Ibarra, C. Inhibition of water absorption in human proximal tubular epithelial cells in response to Shiga toxin-2. Pediatr. Nephrol. 23, 1981–1990 (2008).
Márquez, L. B. et al. Effects of Escherichia coli subtilase cytotoxin and shiga toxin 2 on primary cultures of human renal tubular epithelial cells. PLoS ONE 9, e87022 (2014).
Silberstein, C., Copeland, D. P., Chiang, W. L., Repetto, H. A. & Ibarra, C. A glucosylceramide synthase inhibitor prevents the cytotoxic effects of Shiga toxin-2 on human renal tubular epithelial cells. J. Epith. Biol. Pharmacol. 1, 71–75 (2008).
Amaral, M. M. et al. Action of Shiga toxin type-2 and subtilase cytotoxin on human microvascular endothelial cells. PLoS ONE 8, e70431 (2013).
Silberstein, C. et al. A glucosylceramide synthase inhibitor protects rats against the cytotoxic effects of Shiga toxin-2. Pediatr. Res. 69, 390–394 (2011).
Cox, T. M. et al. Eliglustat compared with imiglucerase in patients with Gaucher’s disease type 1 stabilised on enzyme replacement therapy: a phase 3, randomised, open-label, non-inferiority trial. Lancet 385, 2355–2362 (2015).
McEachern, K. A., Fung, J. & Komarnitsky, S. A specific and potent inhibitor of glucosylceramide synthase for substrate inhibition therapy of Gaucher disease. Mol. Genet. Metab. 91, 259–267 (2007).
Márquez, L. B., Araoz, A., Repetto, H. A., Ibarra, F. R. & Silberstein, C. Effects of Shiga toxin 2 on cellular regeneration mechanisms in primary and three-dimensional cultures of human renal tubular epithelial cells. Microb. Pathog. 99, 87–94 (2016).
Girard, M. C. et al. Prevention of renal damage caused by Shiga toxin type 2: action of Miglustat on human endothelial and epithelial cells. Toxicon 105, 27–33 (2015).
Bligh, E. G. & Dyer, W. J. A rapid method of total lipid extraction and purification. Can. J. Biochem. Physiol. 37, 911–917 (1959).
Keepers, T. R., Psotka, M. A., Gross, L. K. & Obrig, T. G. A murine model of HUS: Shiga toxin with lipopolysaccharide mimics the renal damage and physiologic response of human disease. J. Am. Soc. Nephrol. 17, 3404–3414 (2006).
Clayton, F. et al. Lipopolysaccharide upregulates renal Shiga toxin receptors in a primate model of hemolytic uremic syndrome. Am. J. Nephrol. 25, 536–540 (2005).
Lee, L., Abe, A. & Shayman, J. A. Improved inhibitors of glucosylceramide synthase. J. Biol. Chem. 274, 14662–14669 (1999).
Kolter, T., Proia, R. L. & Sandhoff, K. Combinatorial ganglioside biosynthesis. J. Biol. Chem. 277, 25859–25862 (2002).
Shayman, J. A. & Larsen, S. D. The development and use of small molecule inhibitors of glycosphingolipid metabolism for lysosomal storage diseases. J. Lipid Res. 55, 1215–1225 (2014).
Abe, A. et al. Reduction of globotriaosylceramide in Fabry disease mice by substrate deprivation. J. Clin. Invest. 105, 1563–1571 (2000).
Yew, N. S. et al. Increased hepatic insulin action in diet-induced obese mice following inhibition of glucosylceramide synthase. PLoS ONE 5, e11239 (2010).
Trachtman, H. et al. Effect of an oral Shiga toxin-binding agent on diarrhea-associated hemolytic uremic syndrome in children: a randomized controlled trial. JAMA 290, 1337–1344 (2003).
Okuda, T. et al. Targeted disruption of Gb3/CD77 synthase gene resulted in the complete deletion of globo-series glycosphingolipids and loss of sensitivity to verotoxins. J. Biol. Chem. 281, 10230–10235 (2006).
Hanashima, T. et al. Effect of Gb3 in lipid rafts in resistance to Shiga-like toxin of mutant Vero cells. Microb. Pathog. 45, 124–133 (2008).
Rogers, T. J. & Paton, J. C. Therapeutic strategies for Shiga toxin-producing Escherichia coli infections. Expert Rev. Anti Infect. Ther. 7, 683–686 (2009).
Russo, L. M., Melton-Celsa, A. R., Smith, M. A., Smith, M. J. & O’Brien, A. D. Oral intoxication of mice with Shiga toxin type 2a (Stx2a) and protection by anti-Stx2a monoclonal antibody 11E10. Infect. Immun. 82, 1213–1221 (2014).
Torres, A. G. et al. Recent advances in Shiga toxin-producing Escherichia coli research in Latin America. Microorganisms 6, 100 (2018).
Acknowledgements
We are grateful to the Pediatric Surgery team at the “Sección de Cirugía Pediátrica, Hospital General de Pediatría Pedro de Elizalde”, Buenos Aires, Argentina for providing kidney samples. We thank Natalia Beltramone, Flavia Sacerdoti, and Juan José Casal (IFIBIO-Houssay) for the technical assistance. This work was supported by grants to C.S. from the University of Buenos Aires (UBACYT20020160100078BA) and to C.I., M.M.A., and C.S. from the National Scientific and Technical Research Council (CONICET: PUE 0041).
Author information
Authors and Affiliations
Contributions
Each author has met the Pediatric Research authorship requirements. D.S.S., L.K.F.S., and C.S.: substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; A.B., C.I., M.M.A., and C.S.: drafting the article or revising it critically for important intellectual content; all authors approved the final manuscript version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Informed consent
Written informed consent from the next of kin or guardians on behalf of the children was obtained for use of kidney samples for research. The Ethics Committee of the Hospital General de Niños Pedro de Elizalde approved the use of human renal tissues for the development of primary cell cultures for research purposes.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sánchez, D.S., Fischer Sigel, L.K., Balestracci, A. et al. Eliglustat prevents Shiga toxin 2 cytotoxic effects in human renal tubular epithelial cells. Pediatr Res 91, 1121–1129 (2022). https://doi.org/10.1038/s41390-021-01622-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-021-01622-3