Abstract
Serum amyloid P component (SAP) is a universal constituent of human amyloid deposits including those in Alzheimer’s disease. SAP has been observed to be elevated in patients with depression, and higher SAP levels are associated with better response to the antidepressant escitalopram. The mechanisms underlying these clinical observations remain unclear. We examined the effect of SAP on serotonin transporter (SERT) expression and localization using Western blot, confocal microscopy, and positron emission tomography with the radioligand [11C]DASB. We also investigated the effect of SAP on treatment response to escitalopram in mice with the forced swim test (FST), a classical behaviour paradigm to assess antidepressant effects. SAP reduced [11C]DASB binding as an index of SERT levels, consistent with Western blots showing decreased total SAP protein because of increased protein degradation. In conjunction with the global decrease in SERT levels, SAP also promotes VAMP-2 mediated SERT membrane insertion. SAP levels are correlated with behavioural despair and SSRI treatment response in mice with FST. In MDD patients, the SAP and membrane SERT levels are correlated with response to SSRI treatment. SAP has complex effects on SERT levels and localization, thereby modulating the effect of SSRIs, which could partially explain clinical variability in antidepressant treatment response. These results add to our understanding of the mechanism for antidepressant drug action, and with further work could be of clinical utility.
Similar content being viewed by others
Introduction
Major depressive disorder (MDD), or simply depression, is a leading cause of disability worldwide, and is characterized by episodes of low mood, neurovegetative disturbances, and suicidality [1]. Many antidepressant medications are used, but efficacy is modest [2] and treatment response is often unpredictable [3], necessitating repeated trials of different medications. The most common class of antidepressants is the selective serotonin reuptake inhibitors (SSRIs), which target the serotonin transporter (SERT) to increase synaptic serotonin levels. However, the molecular mechanisms by which this proximal action leads to antidepressant effects remains an active area of research [4].
Serum amyloid P component (SAP) is a glycoprotein that forms a dual pentamer structure capable of binding amyloid protein deposits such as those characteristic of Alzheimer’s disease [5]. SAP is also one of the acute phase proteins induced in the liver by infection or injury, under the regulation of CD14 and toll-like receptor 4 (Tlr4) [6]. There is evidence that inflammation in MDD can reduce the effect of antidepressant medications and psychotherapy [7]. Inflammatory markers such as IL-6, TNFα, and CRP have been associated with antidepressant treatment resistance [7, 8], but the neurobiological mechanisms underlying the association between inflammation and mood symptoms remain obscure [9].
Serotonin uptake from the synaptic space into cells is the function of the SERT, which is encoded by the SLC64A gene (solute carrier family 6, member A4). The SERT contains 12 transmembrane domains and relies on the Na+ gradient to drive active 5-HT transport across the cell membrane [10]. The SERT has been studied extensively because it is targeted by the SSRIs, and may affect susceptibility to depression. For example, a polymorphic repeat in the 5-HTT gene promotor region (5-HTTPR) has short (14 repeats) or long alleles (16 repeats) [11]. The short 5-HTTPR allele is associated with lower 5-HTT expression and increased susceptibility to depression with childhood or adult stressors [12].
Aside from inflammation, another possible relationship between SAP and depression could be mediated by SERT. Recently, we found that peripheral blood plasma SAP levels were higher at baseline in patients with depression than unaffected controls [13]. Our study also reported that SAP levels are reduced by antidepressant treatment, yet paradoxically, higher SAP levels are associated with better response to SSRI treatment. A greater reduction in SAP levels with antidepressant treatment was associated with better clinical response.
In this paper, we investigate a potential mechanism that may explain our earlier clinical observations. We hypothesize that SAP regulates both SERT levels and membrane localization, thereby modulating response to antidepressants. Our proposed model is that SAP reduces total SERT levels while simultaneously increasing membrane localization of SERT. Thus, a higher baseline SAP level is difficult to interpret clinically without knowing the proportion of SERT in the membrane, which is the fraction targeted by SSRI antidepressants. Understanding more about these molecular mechanisms may help to design clinical predictors of antidepressant response that could assist in the selection of treatments that are more likely to be effective.
Materials and methods
PET imaging
Mouse imaging studies were approved by the animal care committee at the Center for Addiction and Mental Health (CAMH protocol #831). Two groups of four healthy adult male mice (DBA/2J) underwent 90-minute dynamic PET imaging following bolus injection of [11C]DASB through a catheter (Anicath™ Non-Wing IV Cannula) in the lateral tail vein. The patency of the catheter was maintained by flushing with heparinized saline (30 IU/ml). Temperature and respiration were monitored closely during the scan and under anesthesia (isoflurane: 1.5–2%; O2 rate: 1 L/min). One hour after the baseline scan, SAP (50 μg) or saline were injected i.p. before a second [11C]DASB PET scan. The SAP and saline group of mice were not significantly different in weight (29 ± 1 vs. 31 ± 1 g), injected activity at baseline (7.03 ± 0.38 vs. 6.84 ± 0.44 MBq, respectively) or after treatment (6.92 ± 0.58 vs. 6.93 ± 0.47 MBq, respectively), or injected mass before (3.0 ± 1.1 vs. 3.2 ± 1.0 nmol/kg, respectively) or after treatment (1.7 ± 0.3 vs. 1.8 ± 0.2 nmol/kg, respectively). PET images were acquired using a nanoScan PET/CT scanner (Mediso, Budapest, Hungary).
The acquired list mode data were sorted into 39, 3D (3 × 5 s, 3 × 15 s, 3 × 20 s, 7 × 60 s, 17 × 180 s and 6 x 300s) true sinograms (ring difference 84). The 3D sinograms were converted to 2D sinograms using Fourier-rebinning [14], during which corrections were included for detector geometry and efficiencies, attenuation, and scatter using a CT-based body-air map, prior to image reconstruction using a 2D–filtered back projection (FBKP) with a Hann filter at a cutoff of 0.50 cm−1. A static image of the complete emission acquisition was reconstructed with the manufacturer’s proprietary iterative 3D algorithm (6 subsets, 4 iterations). All image data were corrected for dead-time and decay corrected to the start of acquisition. The dynamic FBKP images were used for the extraction of time-activity curves (TACs) and kinetic modelling. The static iterative image was used for PET and CT co-registration and for co-registration with a standard mouse brain MR template and atlas [15]. Image analyses including CT to MR brain template co-registration, extraction of regional brain TACs, kinetic modelling, and BPND map construction were performed using PMOD (version 4.203, Zürich, Switzerland). Modified cerebellar cortex with voxels close to the brainstem removed was used as the reference region for modelling with a simplified reference tissue model [16, 17].
Animal experiments
All non-PET scan animal procedures were approved by the Institutional Animal Care and Use Committee of Capital Medical University (the ethics protocol number is AEEI-2020-150). All animal experiments were conducted in accordance with the procedures approved in the protocols. Male DBA/2N mice at the age of 7 weeks were purchased from Vital River Laboratories and acclimatized to the animal facility for one week. Tail blood samples were collected 2 days before behavioural testing. Mice were randomly divided into two groups: 8 animals were injected with saline, and 20 animals were injected with escitalopram oxalate (SSRI) (i.p. 5 mg/kg) 1 h before the start of testing. The forced swim test was conducted as previously described [18]. For tissue analysis, mice were sacrificed by cervical dislocation, and specific brain regions were dissected according to mouse brain atlas landmarks [19].
SERT internalization assay
Cortical neurons were plated on coverslips and incubated with or without SAP (100 nM) for 1 h, and then escitalopram (10 μM) was added and incubated for another 1 h. Neurons were “live”-labeled in culture medium with antibodies recognizing extracellular epitopes of SERT (1.6 μg/ml) for 15 min at 37 °C. After washing twice with PBS, antibodies localized to the cell surface were immediately removed with a 0.5 M glycine (pH2.2) wash. Cells were fixed in 4% paraformaldehyde for 20 min at room temperature. The secondary antibody was added to permeabilized cells. A control with no primary antibody added was included for each experiment to ensure that antibody internalization was specific. Cells were viewed using confocal microscopy (Olympus FluoView FV1200, 60× oil-immersion lens). The mean intensity of SERT signal in each cell was quantified using ImageJ. An alternative protocol for internalization was described in supplementary materials.
SERT membrane insertion
Existing cell surface SERT in WT or VAMP2-KD cortical neurons was pre-blocked with antibody recognizing extracellular epitopes of SERT and non-fluorescent secondary antibody for 45 min at 4 °C, respectively. For insertion, cortical neurons were treated with or without SAP (100 nM) for 10 min at 37 °C. Newly inserted SERT on the plasma membrane was stained first with SERT primary antibody and then the secondary antibody for 45 min at 4 °C. Cells were fixed in 4% paraformaldehyde for 20 min at room temperature. For SERT internalization and membrane insertion, cortical neurons were imaged by confocal microscopy (Olympus FluoView FV1200, 60× oil-immersion lens). The mean fluorescence intensity of the SERT signal in cells was analyzed using ImageJ (NIH).
The nucleotide sequence CATGAGGGTGAACGTGGACAA (Sigma-Aldrich, catalog TRCN0000236330,) was used to silence the expression of VAMP2.
Protein extraction and Western blot
Total protein extraction and Western blot analyses were performed as previously described [20,21,22]. Membrane protein extraction was conducted using the membrane, nuclear, and cytosol protein extraction kit (KeyGEN BioTECH, Jiangsu, China, Cat # KGBSP002; BioBasic, Canada, Cat # BPS002). More details are described in the supplementary information.
Pulse-chase experiments
HEK293T cells were transiently transfected with Halo-SERT plasmids using lipofectamine3000 transfection reagent (ThermoFisher Scientific, Cat # L3000015). As previously described [23], 11 h after transfection, cells were treated with vehicle or SAP (100 nM, 1 h), then the cells were labeled with 2 µM HaloTag®TMR (Promega, Cat # G8251; 12 h after transfection) and were harvested at 0, 4, 8, and 12 h after labeling. Total protein was extracted with lysis buffer, subjected to SDS-PAGE, and then Western blot. The blots were analyzed by TMR fluorescence followed by immunoblotting. Fluorescent bands were quantified using ImageLab (Bio-Rad). More details are described in the supplementary information.
5-HT reuptake assay
5-HT reuptake assays were conducted in HEK293T cells transiently transfected with SERT plasmid using the Neurotransmitter transporter uptake assay kit (Molecular Devices, Cat # R8173) according to the manufacturer’s instruction. More details are described in the supplementary information.
Human clinical studies
This study was approved by the Human Research and Ethics Committee of Beijing Anding Hospital, Capital Medical University (Chinese Clinical Trial Registry Identifier: ChiCTR-OOC-17012566). Patients with major depressive disorder (MDD) were recruited via referral from healthcare professionals. All subjects provided written informed consent and capacity to consent was assessed by a trained research assistant. There were 61 patients with MDD and clinical assessments were described previously [13].
Inclusion criteria for MDD patients were: (i) outpatients between 18 and 65 years of age, (ii) met DSM-IV criteria for either single episode or recurrent MDD according to the Chinese version of the Mini International Neuropsychiatric Interview (MINI) administered by experienced research psychiatrists, (iii) a QIDS-SR16 score of ≥11, and (iv) HAMD-17 (Hamilton Depression Rating Scale) score of ≥14. Exclusion criteria were: (i) >7 days antidepressant medication in the past 14 days of MDD episode, (ii) lifetime history of bipolar, schizophrenia, or other Axis I psychiatric disorders, (iii) drug or alcohol dependence, (iv) pregnancy or breastfeeding, (v) lack of response or intolerance to escitalopram; (vi) serious suicide risk as defined by a score of ≥3 based on the item 3 in HAMD-17, and (vii) medical contraindications to antidepressant medications.
Inclusion criteria for the unaffected controls were: (i) no lifetime DSM-IV Axis I psychiatric disorder, (ii) no significant medical illness, and (iii) pregnancy. All participants were required to have the ability to communicate and provide written informed consent. All patients were treated with escitalopram, starting at 5 mg/day to 10–20 mg/day within 7 days, and the dose remained unchanged until the patients completed the 12-week study. Peripheral blood samples were collected and leukocytes isolated as previously described [24].
Statistical analyses
Data were analyzed by t-test, one-way analysis of variance (ANOVA) followed by Tukey’s test, or two-way ANOVA followed by Bonferroni post hoc test (GraphPad Prism 6.0, GraphPad Software, CA, USA). All data were expressed as mean ± standard error of mean (S.E.M.). The significance levels of p < 0.05, p < 0.01, or p < 0.001 were used for all analyses.
To see if SAP levels predicted the effect of SSRI treatment on learned behavioural despair in the forced swim test (FST), we fitted a moderated regression model with SAP levels as a continuous independent variable and SSRI treatment as a dichotomous moderator on immobility time in the FST. Pearson’s correlation was calculated to examine the relationships between SAP levels, SERT membrane expression, HAMD-17 score before and after escitalopram, and percentage reduction in the HAMD-17 after treatment. More details are described in the supplementary information.
Results
SAP decreases in vivo [11C]DASB binding in mouse brain
We quantified the amount of SERT using PET imaging with [11C]DASB. At baseline, [11C]DASB binding in DBA/2J mice showed the expected anatomical distribution, with strong binding in midbrain and thalamus, moderate levels in striatum, and relatively lower levels in hippocampus, cortex, and cerebellum. [11C]DASB binding was markedly decreased throughout the brain one hour after treatment with SAP (i.p. 50 μg), but not saline (Fig. 1A, B). BPND values after SAP administration in thalamus, midbrain, striatum, hippocampus, frontal cortex and whole brain without cerebellum were 1.58 ± 0.17, 1.55 ± 0.14, 1.22 ± 0.18, 1.03 ± 0.11, 0.61 ± 0.14, 0.76 ± 0.11, respectively. In comparison, baseline values were 2.00 ± 0.12, 1.96 ± 0.08, 1.63 ± 0.13, 1.28 ± 0.08, 0.89 ± 0.13, 1.03 ± 0.07, respectively. Thus, SAP induced a significant decrease in SERT binding of 26% in whole brain (p < 0.05). For the saline-treated mice, BPND values in above brain regions were 2.12 ± 0.18 vs. 2.09 ± 0.11, 1.92 ± 0.18 vs. 1.90 ± 0.14, 1.80 ± 0.14 vs. 1.74 ± 0.08, 1.30 ± 0.14 vs. 1.25 ± 0.11, 1.18 ± 0.09 vs. 1.16 ± 0.05, 1.14 ± 0.10 vs. 1.12 ± 0.06, respectively, before and after injection of the saline (p > 0.05).
A Average binding potential (BPND) map in coronal, sagittal, and transverse planes of four mice at baseline and after SAP treatment (left panel) as compared to another four mice before and after saline injection (right panel), superimposed with the MR template of Dorr [15]. B BPND in frontal cortex, hippocampus, striatum, thalamus, midbrain, and whole brain without cerebellum (WB). *p < 0.05 (paired t-test, SAP versus baseline1).
SAP reduces total SERT levels by promoting degradation
To confirm the PET data, we used Western blots as an alternate method to quantify SERT levels in response to SAP treatment. We first determined the dose of SAP needed by measuring SERT-mediated 5-HT reuptake in SERT plasmid-transfected HEK293T cells treated with various concentrations of SAP. As shown in Fig. S1A, 5-HT reuptake was significantly inhibited by 100 nM SAP, so this dose was chosen for the following experiments. Consistent with the results from PET data, mouse brain slices treated with SAP had lower total levels of SERT as measured by Western blot (Fig. 2A, B, t4 = 5.297, p < 0.01). Testing in HEK293T cells transfected with SERT plasmid showed similar results (Fig. S1B, C, t4 = 5.983, p < 0.01). This decrease in SERT induced by SAP could be due to decreased protein synthesis or increased degradation. To determine which of these possibilities was more likely, we used pulse-chase studies to examine SERT protein half-life in transfected HEK293T cells in the presence or absence of SAP. The amount of fluorescent halo-tagged SERT is significantly lower 8 and 12 h after adding SAP, suggesting that SAP facilitates SERT degradation (Fig. 2C, D).
A Representative Western blot images of total SERT in mouse brain tissue in the presence of SAP (50 μg, 1 h). β-actin was used as a loading control. B Densitometric analysis of total SERT levels, normalized to β-actin, shown as a percentage of the saline group on the same blots: mean ± S.E.M. N = 3 independent repeats. Data were analyzed by t-test, *p < 0.05 as compared to the saline group. Pulse-chase labelling of SERT protein in HEK293T cells transiently transfected with Halo-SERT plasmid treated with either vehicle or SAP (100 nM, 1 h). The amount of fluorescent Halo-tagged SERT was plotted over time (C) and quantified (D). β-actin was used as a loading control. The level of Halo-SERT was normalized to β-actin, and shown as the percentage of the levels of Halo-SERT at 0 h. N = 3 independent repeats. Data are shown as mean ± S.E.M., and analyzed by two-way ANOVA followed by Sidak’s post hoc test. **p < 0.01, and ****p < 0.0001 as compared to vehicle. E Representative Western blot images of SERT on cell surface membrane in mouse brain tissue in the presence of SAP (50 μg, 1 h). TfR was used as a loading control. F Densitometric analysis of SERT levels on the cell surface, normalized to the level of TfR, presented as a percentage of the saline group on the same blots. G Densitometric analysis of TfR levels on the cell surface presented as a percentage of the saline group on the same blots. Data shown as mean ± S.E.M. N = 3 independent repeats; t-test, *p < 0.05 as compared to saline group.
SAP increases SERT levels at the cell membrane
The SERT must be on the cell membrane to transport serotonin from the synapse into the cell. Thus, we examined the localization of SERT in mouse brain tissue with and without SAP. We found that membrane levels of SERT are significantly increased after SAP administration, despite a reduction of total SERT levels (Fig. 2E–G, t4 = 4.254, p < 0.05; Figure S2A, B detecting on the same blots as Fig. 2E, t4 = 2.937, p < 0.05). This suggests that SAP may have two effects on SERT: simultaneously decreasing total levels by increasing degradation while increasing membrane levels.
SAP enhances VAMP-2 mediated SERT membrane insertion
To investigate the mechanism by which SAP increases membrane levels of SERT, we examined the effect of SAP on the membrane insertion of SERT in cortical neurons using confocal microscopy. As shown in Fig. 3A, B, SAP-treated neurons have a significantly higher newly inserted SERT levels on the membrane than control neurons (n = 36 cells per group from 2 independent experiments. Unpaired t-test, t70 = 5.629, ****p < 0.0001 compared to Ctr.) These results confirm that SAP enhances membrane insertion of the SERT.
A After preblocking existing cell surface SERT with antibodies recognizing extracellular epitopes of SERT and nonfluorescent secondary antibody, we incubated cells (cortical neurons) with or without SAP for 10 min at 37 °C. Neurons were stained for SERT (green) to detect newly inserted SERT on the plasma membrane. B Quantification shows the normalized percentage in the mean intensity of SERT. N = 36 cells per group from 2 independent experiments. ****p < 0.0001, unpaired t-test. C, D Confocal images and quantification of immunostaining for SERT insertion in Ctr or VAMP2-KD cells (cortical neurons) with or without SAP treatment for 10 min at 37 °C. Neurons were stained for SERT (green) to detect newly inserted SERT on the plasma membrane under nonpermeabilized conditions. N = 17/14 cells per group. p = 0.5144, unpaired t-test. Scale bars: 10 μm.
Previous studies have reported that SERT interacts with VAMP-2 (vesicle-associated membrane protein 2) [25], suggesting that SERT cell membrane insertion could occur through a membrane fusion-dependent exocytotic process that relies on VAMP2. To further delineate the mechanism by which SAP increased membrane SERT, we repeated the previous experiment after knocking down VAMP-2 with shRNA in cortical neurons. As shown in Fig. S3A, B, the expression levels of VAMP-2 were significantly decreased with transfection of VAMP-2 shRNA (n = 4, t6 = 8.247, p < 0.001). We found that VAMP-2 shRNA blocked the effect of SAP on increasing membrane SERT levels (Fig. 3C, D: n = 17/14 cells per group, unpaired t-test, t29 = 0.6601, p = 0.5831). These data suggest that VAMP-2 is necessary for SAP to enhance membrane SERT levels.
SAP blocks SSRI-induced SERT internalization
One potential mechanism by which SSRI antidepressants function to inhibit SERT function is by increasing SERT internalization, thereby reducing the membrane levels of SERT that can function to reuptake serotonin. Because we found that SAP increases SERT insertion into the membrane, we sought to investigate whether SAP affects SSRI-induced SERT internalization. We used a modified version of an internalization assay that has been described previously [26]. SSRI treatment significantly increased the amount of internalized SERT in cortical neurons, consistent with previous reports [27]. SAP diminished the effect of SSRI treatment on increasing internalized SERT, while SAP alone did not alter the amount of internalized SERT vs. control (Fig. 4A, B: *p < 0.05 compared to Ctr, #p < 0.05 compared to SSRI, one-way ANOVA, F3,94 = 1.149, n = 23/33/22/20 cells per group; Fig. S4A, B (used an alternative protocol): ****p < 0.0001 compared to Ctr, ####p < 0.0001 compared to SSRI, one-way ANOVA, F3,54 = 1.548, n = 16/17/13/12 cells per group; Fig. 4C, D and Fig. S4C, D with no primary antibody added during staining). Western blots produced similar results in mouse brain tissues (Fig. 4E–G and Fig. S5A, B) and transfected HEK293T cells (Fig. S5C, D): the membrane levels of SERT were significantly decreased by SSRI treatment, and this effect was blocked by co-treatment with SAP (Fig. 4E–G, F2,6 = 0.6141, p < 0.05; Figure S5A, B (detected on the same blots as Fig. 4E), F2,6 = 0.3900, p < 0.01; Fig. S5C, D, n = 4, F2,9 = 1.722, p < 0.001).
A-D SERT staining in neurons treated with SSRI and SAP, including a 0.5 M glycine wash. A, B Quantification shows the mean intensity of SERT (n = 23, 33, 22, 20 cells per group, respectively). *p = 0.0438 relative to Ctr group, #p = 0.0268 relative to SSRI group, 1-way ANOVA. C, D Quantification shows the mean intensity of signal with no primary antibody added (n = 16, 14, 14, 12 cells per group, respectively). Scale bars, 10 μm. E Representative Western blots showing SERT on the cell membrane in mouse brain tissue in the presence of SAP (50 μg, 1 h) and/or SSRI (5 mg/kg, 1 h). TfR was used as a loading control. F Densitometric analysis of SERT levels on cell surface membrane, normalized to the level of TfR, shown as a percentage of the saline group from the same blots. G Densitometric analysis of TfR levels on the cell membrane shown as a percentage of the saline group from the same blots. Data were shown as mean ± S.E.M. N = 3 independent repeats. Data were analyzed by one-way ANOVA followed by Tukey’s post hoc test, *p < 0.05 as compared to saline group, #p < 0.05 as compared to SSRI group.
SAP levels are correlated with depression-like behaviour and SSRI treatment response in mice
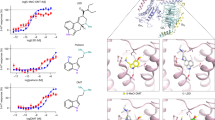
To examine the relationship between SAP levels and depression-like behaviour in mice, we examined mice either treated with the SSRI escitalopram or vehicle in the forced swim test (FST). Immobility time during the last 4 min of the FST is thought to be a measure of behavioural despair, and has been used as a screening test for antidepressant action [28]. There was a significant correlation between SAP levels and immobility time that interacted with SSRI treatment (R2adj = 0.46, F3,24 = 8.57, p = 0.00048) (Fig. 5A). As expected, escitalopram treatment significantly lowered immobility time in the FST (t = −3.98, p = 0.00055). SAP levels were significantly correlated with immobility time (t = 3.12, p = 0.0046) and there was a significant interaction between SAP and escitalopram on immobility time (t = −3.32, p = 0.0029). This suggests that escitalopram treatment changed the relationship between SAP levels and behavioural despair in mice. Simple slopes analysis revealed that SAP was positively correlated with immobility time in untreated mice (β = 1.16 [0.34–2.0], p = 0.0096) but there was a trend towards a negative correlation in mice treated with escitalopram (β = −0.76 [−1.54–0.022], p = 0.062).
A Immobility time in the FST plotted against SAP levels in mice treated with the SSRI escitalopram (red) or saline (blue). B Mean immobility time in the FST for the 50th and 100th percentile of SAP levels in mice treated with the SSRI [escitalopram oxalate] or saline-treated controls. C Representative Western blot images of SERT on the cell surface of PBMCs from patients with MDD. TfR was used as the loading control. D Densitometric analysis of the levels of SERT on the cell surface, normalized to the level of TfR and presented as a percentage of the control group from the same blot. Data are shown as mean ± S.E.M. N = 11 non-responders, 7 controls, and 8 responders. Data were analyzed by one-way ANOVA followed by Tukey’s post hoc test. **p < 0.01 as compared to controls, and ###p < 0.001 as compared to responders. E SAP levels in plasma from patients with MDD and healthy controls were measured with an ELISA. Results are shown as the Log of SAP concentration. N = 21 controls, 22 non-responders and 18 responders. Data were analyzed by one-way ANOVA followed by Tukey’s post hoc test. *p < 0.05 as compared to control group, and ###p < 0.001 as compared to those of responders group. F Correlation table showing the Pearson’s r comparing SAP levels (SAP), SERT membrane expression (SERT), HAMD-17 score before treatment with SSRI’s (Pre), and the % improvement in HAMD-17 score after treatment (% improvement). Correlations passing the significance threshold (p < 0.05) are shown in colour. G SAP levels plotted against SERT membrane expression. H SAP levels plotted against the % improvement in HAMD-17 score after SSRI treatment. I SERT membrane expression plotted against the % improvement in HAMD-17 score after SSRI treatment. J SAP levels plotted against pre-treatment [HAMD-17 score].
In essence, mice with higher SAP levels demonstrated greater behavioural despair in the FST, but mice with higher SAP levels also had greater reductions in behavioural despair when treated with escitalopram. SSRI treatment was effective at lowering immobility time overall (F1,24 = 12.66, p = 0.0016), but the main effect of SSRI treatment on behavioural despair occurs in the mice with the highest SAP levels (p = 0.0011). In contrast, there is little effect of SSRI treatment for mice with lower SAP (p = 0.91) (Fig. 5B).
SAP levels and SERT expression in MDD patients
We previously reported that SAP is higher in patients with MDD, and is associated with clinical response to SSRI treatment [13]. Thus, we hypothesized that SAP and SERT membrane levels may affect the efficacy of SSRI treatment for depression. To test this hypothesis, we measured SERT membrane levels in peripheral blood mononuclear cells (PBMCs) from depressed patients who were SSRI responders or non-responders. As predicted, SSRI-responsive depressed patients had significantly higher SERT membrane levels than non-responders or healthy controls (Fig. 5C, D, F2,23 = 5.261, p < 0.001; Fig. S6A–C (detected on the same blots as Fig. 5C). Figure S6B, C: F2,23 = 2.934, p < 0.0001). Similarly, SAP levels in depressed patients who responded to SSRI treatment was higher than in unaffected controls or SSRI non-responders (Fig. 5E, F2,58 = 0.5347, p < 0.001). The demographic and clinical information for patients with MDD and control subjects was shown in Table S1.
SAP levels are correlated with SSRI treatment response and SERT membrane expression but not initial depression symptoms in humans
To examine the relationship between SAP levels and SSRI treatment in MDD, SAP levels were measured in 40 MDD patients, and HAMD-17 (Hamilton Depression Rating Scale-17) scores were measured before and after SSRI (escitalopram) treatment. SERT membrane expression levels were obtained from 18 of the 40 patients. SAP levels significantly positively correlated with SERT membrane expression (r (16) = 0.75 [0.43–0.90], t = 4.52, p = 0.0021) (Fig. 5F, G) and reduction in HAMD-17 score after SSRI treatment (r(38) = 0.49 [0.22–0.70], t = 3.50, p = 0.0048) (Fig. 5F, H). SERT membrane expression was also significantly correlated with reduction in HAMD-17 score (r(16) = 0.72 [0.38–0.90], t = 4.17, p = 0.0036) (Fig. 5F, I). In contrast to the mouse data, SAP levels were not significantly correlated with pre-treatment HAMD-17 score (r(38) = 0.13 [−0.19–0.42], t = 0.80, p = 0.43) (Fig. 5F, J).
Discussion
Our results indicate that SAP has complex effects on SERT levels, SERT localization, and response to SSRI treatment. SAP reduces SERT levels in vivo as measured by PET scans with the radiotracer [11C]DASB in mouse brain, and this is confirmed by Western blots with mouse brain protein. SAP reduces total SERT levels by promoting degradation instead of reducing synthesis, while also enhancing VAMP-2 mediated SERT membrane insertion. The SSRI antidepressant escitalopram induces SERT internalization that is blocked by SAP. In human subjects, higher SAP and SERT membrane levels are associated with better response to SSRI treatment. In the mouse, SAP levels are correlated with depression-like behaviour and response to SSRI treatment. The data presented here add to our previously published results that higher SAP levels are associated with both depression and better response to the SSRI antidepressant escitalopram [13].
These results support our hypothetical model in which the higher SAP levels in depression leads to both a reduction in total SERT and increased membrane insertion of SERT. Since SERT must be on the cell membrane to be targeted by SSRIs, it is logical that higher SAP and greater SERT at the cell membrane would also be correlated with better response to SSRI treatment. Thus, measurement of SAP levels in patients with depression could be useful as a clinical indicator of the potential efficacy of SSRI treatment, and with further work, could potentially be used to guide the selection of antidepressant medication.
Future work could explore this idea further by testing whether SAP levels predict response to other types of antidepressant medications that act primarily at the norepinephrine transporter like the tricyclic antidepressants despimpramine, nortryptiline and clomipramine, the dopamine transporter inhibitor buproprion, or the monoamine oxidase inhibitors. We predict that higher SAP levels would not affect treatment response to these other non-SSRI antidepressant medications.
Interestingly, the PET data suggest a rapid decrease in [11C]DASB binding one hour after SAP administration (Fig. 1). This could imply that SAP modifies SERT binding affinity for [11C]DASB; however, we also detected decreased SERT levels in mice 1 h after SAP treatment, with the pulse-chase data suggesting SAP increased SERT degradation. The typical half-life of SERT is several days at baseline [29], so SAP may interact with SERT to engage rapid degradation. There is currently little research of SAP in the context of protein degradation pathways; however, disruption of the ubiquitin proteasome system (UPS) has been implicated in Alzheimer’s [30]. SERT degradation by the UPS has been demonstrated [31], so future experiments could explore whether SAP affects SERT ubiquitination.
An important question that is not addressed by our experiments is whether increased SAP levels are a consequence of depression or instead, that SAP elevation is part of the pathophysiology of depression. Prospective clinical studies of patients with recurrent episodes of depression could provide a platform to better understand the timing of events in this relationship by measuring SAP levels during both episodes of depression and when symptoms are in remission. Ascertaining when SAP levels are altered relative to symptom could suggest directionality. Another approach to attempt to disentangle the causality of this relationship could be to measure SAP levels in mice undergoing chronic mild stress, social defeat, or other environmental paradigms designed to induce a depression-like state. If SAP increase is necessary for the behavioural manifestations of depression, then one would expect to see higher levels of SAP early in the course of these depression induction procedures. If elevated SAP is observed only after the behavioural correlates of depression are observed in the mouse, this would suggest that SAP elevation is a consequence of the depressed state.
Although both the mouse and human data are consistent with our proposed model, in the current study we did not observe significantly higher SAP levels in patients with depression, which we reported previously [13]. The simplest interpretation of this lack of replication is that we had a smaller number of patients with depression in the current study (n = 40) compared to our previous work (n = 85), so we were underpowered to detect the previous findings. We also observed that SAP levels in mice were positively correlated with both immobility time in the FST (a behaviour related to depression in humans), and with response to escitalopram treatment. FST is established in the literature to predict SSRI treatment response [32]; however, this behaviour alone may not be reflective of MDD as a complete syndrome. It would be interesting to explore the relationship between SAP, SERT, and treatment in more valid mouse models for depression involving chronic and psychosocial stress.
In humans, the combination of SAP levels and membrane SERT provides the best prediction of reductions in depressive symptoms, although adding SERT expression alone explains most of the variance in antidepressant response. This suggests that SERT membrane expression is more explanatory than SAP levels in this data, which could indicate that most of the relationship between SAP levels and antidepressant response was mediated through the relationship between SAP levels and SERT expression.
Another approach to determining whether SAP elevation is causal in the pathogenesis of depression is to use the SAP knock out mouse mutant (Apcs−/−) [33]. We would predict that the loss of function of SAP in the homozygous Apcs−/− mouse or heterozygous Apcs−/+ mouse should protect against the depressive phenotype in mice exposed to chronic mild stress or other depression-inducing paradigms. If SAP elevation is but one of many consequences of depression, then the Apcs−/− mice would show the same depression-related behaviours as wild type Apcs+/+ mice when subject to chronic mild stress or social defeat.
Another potential clinical application of our findings is the possibility that SAP or a small molecule analog could be used to augment SSRI treatment. The idea would be to pharmacologically enhance SERT membrane levels to improve SSRI efficacy. Related to this idea is the observation that both antidepressant medications and electroconvulsive therapy for depression increase VAMP-2 levels [34]. VAMP-2 is required for SAP to increase membrane SERT, and it is possible that increased VAMP-2 and SERT membrane insertion are important for the treatment of depression in general, not only with SSRI medications.
Because SAP is an important component of the amyloid plaques in Alzheimer’s disease, it is possible that SAP could play a role in the very high prevalence of depression in Alzheimer’s, which has been reported to be as high as 50% [35]. The accumulation of amyloid plaques could contribute to the emergence of depression, in addition to the psychological effects of progressive dementia and disability in Alzheimer’s. There are of course many other features of Alzheimer’s disease that could increase susceptibility to depression, such as the loss of noradrenergic neurons in the locus ceruleus and cholinergic neurons in the basal nucleus of Meynert [36].
A final point of discussion is to reflect on our incomplete knowledge of antidepressant medication action and the difficulty in interpreting the data presented here. Our results show that SAP has two different effects on SERT: decreasing the total amount of SERT while simultaneously increasing membrane levels. These dual effects prevent a simple model to explain the relationships between depression, SSRI treatment response, and the levels of SERT and SAP. It remains a challenge to experimentally dissect these relationships because of the limitations of clinical research with human subjects and the limited validity of animal models for psychiatric disorders [37, 38]. Similarly, the increased susceptibility to depression associated with lower SERT expression from the 5-HTTPR short allele seems to be incompatible with the action of SSRI antidepressants, which would further decrease SERT activity [12]. While we cannot completely explain our experimental observations, we argue that our data provide new insights into the complex regulation of SERT in the context of depression and antidepressant treatment.
In summary, we have identified a novel molecular biomarker associated with both depression and with response to SSRI treatment that could be useful to guide the clinical selection of antidepressant medication treatment. The modulation of SERT degradation and membrane insertion by SAP is also of interest in unravelling the neurobiological origin and pathobiology of depression, as well as being relevant to antidepressant mechanisms of action. Future studies could expand on our results by studying additional antidepressant medications and SAP knock-out mice, with the potential for short term and long-term clinical applications in the treatment of depression.
References
Disease GBD, Injury I, Prevalence C. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392(10159):1789–858. https://doi.org/10.1016/S0140-6736(18)32279-7.
Cipriani A, Furukawa TA, Salanti G, Chaimani A, Atkinson LZ, Ogawa Y, et al. Comparative efficacy and acceptability of 21 antidepressant drugs for the acute treatment of adults with major depressive disorder: a systematic review and network meta-analysis. Lancet 2018;391:1357–66.
Gaynes BN, Rush AJ, Trivedi MH, Wisniewski SR, Spencer D, Fava M. The STAR*D study: treating depression in the real world. Cleve Clin J Med. 2008;75:57–66.
Nestler EJ, Barrot M, DiLeone RJ, Eisch AJ, Gold SJ, Monteggia LM. Neurobiology of depression. Neuron 2002;34:13–25.
Emsley J, White HE, O’Hara BP, Oliva G, Srinivasan N, Tickle IJ, et al. Structure of pentameric human serum amyloid P component. Nature. 1994;367:338–45.
Cho K, Pham TN, Crivello SD, Jeong J, Green TL, Greenhalgh DG. Involvement of CD14 and toll-like receptor 4 in the acute phase response of serum amyloid A proteins and serum amyloid P component in the liver after burn injury. Shock. 2004;21:144–50.
Strawbridge R, Arnone D, Danese A, Papadopoulos A, Herane Vives A, Cleare AJ. Inflammation and clinical response to treatment in depression: A meta-analysis. Eur Neuropsychopharmacol. 2015;25:1532–43.
Jha MK, Minhajuddin A, Gadad BS, Greer T, Grannemann B, Soyombo A, et al. Can C-reactive protein inform antidepressant medication selection in depressed outpatients? Findings from the CO-MED trial. Psychoneuroendocrinology. 2017;78:105–13.
Jones BDM, Daskalakis ZJ, Carvalho AF, Strawbridge R, Young AH, Mulsant BH, et al. Inflammation as a treatment target in mood disorders: review. BJPsych Open. 2020;6:e60.
Baudry A, Pietri M, Launay J-M, Kellermann O, Schneider B. Multifaceted regulations of the serotonin transporter: impact on antidepressant response. Front Neurosci. 2019;13. https://doi.org/10.3389/fnins.2019.00091.
Hariri AR, Holmes A. Genetics of emotional regulation: the role of the serotonin transporter in neural function. Trends Cogn Sci. 2006;10:182–91.
Caspi A, Sugden K, Moffitt TE, Taylor A, Craig IW, Harrington H, et al. Influence of life stress on depression: moderation by a polymorphism in the 5-HTT gene. Science 2003;301:386–9.
Yang J, Zhou J, Zhou J, Wang H, Sun Z, Zhu X, et al. Serum amyloid P component level is associated with clinical response to escitalopram treatment in patients with major depressive disorder. J Psychiatr Res. 2022;146:172–8.
Defrise M, Kinahan PE, Townsend DW, Michel C, Sibomana M, Newport DF. Exact and approximate rebinning algorithms for 3-D PET data. IEEE Trans Med Imaging. 1997;16:145–58.
Dorr AE, Lerch JP, Spring S, Kabani N, Henkelman RM. High-resolution three-dimensional brain atlas using an average magnetic resonance image of 40 adult C57Bl/6J mice. Neuroimage. 2008;42:60–9.
Lammertsma AA, Hume SP. Simplified reference tissue model for PET receptor studies. Neuroimage. 1996;41:153–8.
Gunn RN, Lammertsma AA, Hume SP, Cunningham VJ. Parametric imaging of ligand-receptor binding in PET using a simplified reference region model. Neuroimage. 1997;6:279–87.
Can A, Dao DT, Arad M, Terrillion CE, Piantadosi SC, Gould TD. The mouse forced swim test. J visualized experiments: JoVE. 2012;59:e3638.
Paxinos G, Watson C. The mouse brain in stereotaxic coordinates. 3rd ed. San Diego, CA: Academic Press Inc.; 2012.
Su P, Li S, Chen S, Lipina TV, Wang M, Lai TK, et al. A dopamine D2 receptor-DISC1 protein complex may contribute to antipsychotic-like effects. Neuron. 2014;84:1302–16.
Lee FJ, Pei L, Moszczynska A, Vukusic B, Fletcher PJ, Liu F. Dopamine transporter cell surface localization facilitated by a direct interaction with the dopamine D2 receptor. Embo J. 2007;26:2127–36.
Pei L, Li S, Wang M, Diwan M, Anisman H, Fletcher PJ, et al. Uncoupling the dopamine D1-D2 receptor complex exerts antidepressant-like effects. Nat Med. 2010;16:1393–5.
Oeding SJ, Majstrowicz K, Hu XP, Schwarz V, Freitag A, Honnert U, et al. Identification of Miro1 and Miro2 as mitochondrial receptors for myosin XIX. J Cell Sci. 2018;131. https://doi.org/10.1242/jcs.219469.
Li H, Su P, Lai TK, Jiang A, Liu J, Zhai D, et al. The glucocorticoid receptor-FKBP51 complex contributes to fear conditioning and posttraumatic stress disorder. J Clin Investig. 2020;130:877–89.
Muller HK, Kragballe M, Fjorback AW, Wiborg O. Differential regulation of the serotonin transporter by vesicle-associated membrane protein 2 in cells of neuronal versus non-neuronal origin. PloS One. 2014;9:e97540.
Man HY, Wang Q, Lu WY, Ju W, Ahmadian G, Liu L, et al. Activation of PI3-kinase is required for AMPA receptor insertion during LTP of mEPSCs in cultured hippocampal neurons. Neuron. 2003;38:611–24.
Lau T, Horschitz S, Berger S, Bartsch D, Schloss P. Antidepressant-induced internalization of the serotonin transporter in serotonergic neurons. FASEB J: Off Publ Fed Am Soc Exp Biol. 2008;22:1702–14.
Yankelevitch-Yahav R, Franko M, Huly A, Doron R. The forced swim test as a model of depressive-like behavior. J Vis Exp: JoVE. 2015. https://doi.org/10.3791/52587.
Vicentic A, Battaglia G, Carroll FI, Kuhar MJ. Serotonin transporter production and degradation rates: studies with RTI-76. Brain Res. 1999;841:1–10.
Gong B, Radulovic M, Figueiredo-Pereira ME, Cardozo C. The ubiquitin-proteasome system: potential therapeutic targets for Alzheimer’s disease and spinal cord injury. Front Mol Neurosci. 2016;9:4.
Lu Q, Murakami C, Hoshino F, Murakami Y, Sakane F. Diacylglycerol kinase delta destabilizes serotonin transporter protein through the ubiquitin-proteasome system. Biochimica et biophysica acta. Mol Cell Biol lipids. 2020;1865:158608.
Kara NZ, Stukalin Y, Einat H. Revisiting the validity of the mouse forced swim test: Systematic review and meta-analysis of the effects of prototypic antidepressants. Neurosci Biobehav Rev. 2018;84:1–11.
Pilling D, Gomer RH. Persistent lung inflammation and fibrosis in serum Amyloid P component (Apcs−/−) knockout mice. PloS one. 2014;9:e93730.
Yamada M, Takahashi K, Tsunoda M, Nishioka G, Kudo K, Ohata H, et al. Differential expression of VAMP2/synaptobrevin-2 after antidepressant and electroconvulsive treatment in rat frontal cortex. Pharmacogenomics J. 2002;2:377–82.
Lyketsos CG, Olin J. Depression in Alzheimer’s disease: overview and treatment. Biol Psychiatry. 2002;52:243–52.
Förstl H, Burns A, Luthert P, Cairns N, Lantos P, Levy R. Clinical and neuropathological correlates of depression in Alzheimer’s disease. Psychol Med. 1992;22:877–84.
Wong AH, Josselyn SA. Caution when diagnosing your mouse with schizophrenia: the use and misuse of model animals for understanding psychiatric disorders. Biol Psychiatry. 2016;79:32–8.
Nestler EJ, Hyman SE. Animal models of neuropsychiatric disorders. Nat Neurosci. 2010;13:1161–9.
Funding
This work was supported by Advanced Innovation Center for Human Brain Protection, Capital Medical University, and Center for Addiction and Mental Health.
Author information
Authors and Affiliations
Contributions
FL oversaw and supervised the overall project. PS conducted the Western blot analysis of both mouse brain tissues, HEK293T cells, and human samples as well as measurement of SAP in human samples with help from QC and FJSL. SY carried out the experiments using confocal microscope. JY, ZS, JZ, and ML recruited the patients with MDD and collected the blood samples. JT, AJ, and DZ conducted the PET scanning with support from NV. FY JC, and YL performed the mouse FST experiments with help from ZX, and YL measured the mouse SAP levels. JS and PS analyzed the human data with help from XW. FL, AHCW, PS, SY, JT, and JS wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Su, P., Yan, S., Yang, J. et al. Serum amyloid P component (SAP) modulates antidepressant effects through promoting membrane insertion of the serotonin transporter. Neuropsychopharmacol. 48, 508–517 (2023). https://doi.org/10.1038/s41386-022-01449-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-022-01449-4