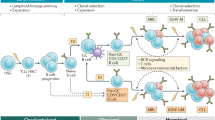
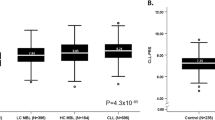
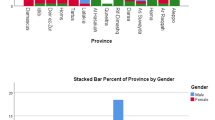
Abstract
East Asians, Asian Indians and Amerindians have a five to ten-fold lower age-adjusted incidence rate (AAIR) of chronic lymphocytic leukaemia (CLL) compared with persons of predominately European descent. The data we review suggest a genetic rather than environmental basis for this discordance. All these populations arose from a common African Black ancestor but different clades have different admixture with archaic hominins including Neanderthals, Denisovans and Homo erectus, which may explain different CLL incidences. There are also some differences in clinical laboratory and molecular co-variates of CLL between these populations. Because the true age-adjusted incidence rate in African Blacks is unknown it is not possible to determine whether modern Europeans acquired susceptibility to CLL or the other populations lost susceptibility and/or developed resistance to developing CLL. We also found other B-cell lymphomas and T- and NK-cell cancers had different incidences in the populations we studied. These data provide clues to determining the cause(s) of CLL.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Surveillance, Epidemiology, and End Results (SEER) Program (www.seer.cancer.gov) SEER*Stat Database: Incidence - SEER 9 Regs Research Data, Nov 2018 Sub (1975-2016).
Chihara D, Ito H, Matsuda T, Shibata A, Katsumi A, Nakamura S, et al. Differences in incidence and trends of haematological malignancies in Japan and the United States. Br J Haematol. 2014;164:536–45.
Lee SJ, Tien HF, Park HJ, Kim JA, Lee DS. Gradual increase of chronic lymphocytic leukemia incidence in Korea, 1999-2010: comparison to plasma cell myeloma. Leuk Lymphoma. 2016;57:585–9.
Miranda-Filho A, Pineros M, Ferlay J, Soerjomataram I, Monnereau A, Bray F. Epidemiological patterns of leukaemia in 184 countries: a population-based study. Lancet Haematol. 2018;5:e14–24.
Yang SM, Li JY, Gale RP, Huang XJ. The mystery of chronic lymphocytic leukemia (CLL): why is it absent in Asians and what does this tell us about etiology, pathogenesis and biology? Blood Rev. 2015;29:205–13.
Shirley MH, Barnes I, Sayeed S, Finlayson A, Ali R. Incidence of breast and gynaecological cancers by ethnic group in England, 2001–2007: a descriptive study. BMC Cancer. 2014;14:979.
APA, Chicago, Harvard, MLA & Bluebook.
http://statisticstimes.com/demographics/countries-by-sex-ratio.php.
Gale RP, Cozen W, Goodman MT, Wang FF, Bernstein L. Decreased chronic lymphocytic leukemia incidence in Asians in Los Angeles County. Leuk Res. 2000;24:665–9.
Mak V, Ip D, Mang O, Dalal C, Huang S, Gerrie A, et al. Preservation of lower incidence of chronic lymphocytic leukemia in Chinese residents in British Columbia: a 26-year survey from 1983 to 2008. Leuk Lymphoma. 2014;55:824–7.
Abnet CC, Arnold M, Wei WQ. Epidemiology of esophageal squamous cell carcinoma. Gastroenterology. 2018;154:360–73.
Lin Y, Totsuka Y, Shan B, Wang C, Wei W, Qiao Y, et al. Esophageal cancer in high-risk areas of China: research progress and challenges. Ann Epidemiol. 2017;27:215–21.
Bassig BA, Au WY, Mang O, Ngan R, Morton LM, Ip DK, et al. Subtype-specific incidence rates of lymphoid malignancies in Hong Kong compared to the United States, 2001–2010. Cancer Epidemiol. 2016;42:15–23.
Zhang YL, Yuan JQ, Wang KF, Fu XH, Han XR, Threapleton D, et al. The prevalence of EGFR mutation in patients with non-small cell lung cancer: a systematic review and meta-analysis. Oncotarget. 2016;7:78985–93.
Rawstron AC, Ssemaganda A, de Tute R, Doughty C, Newton D, Vardi A, et al. Monoclonal B-cell lymphocytosis in a hospital-based UK population and a rural Ugandan population: a cross-sectional study. Lancet Haematol. 2017;4:e334–40.
Furtwangler A, Rohrlach AB, Lamnidis TC, Papac L, Neumann GU, Siebke I, et al. Ancient genomes reveal social and genetic structure of Late Neolithic Switzerland. Nat Commun. 2020;11:1915.
Marcus JH, Posth C, Ringbauer H, Lai L, Skeates R, Sidore C, et al. Genetic history from the Middle Neolithic to present on the Mediterranean island of Sardinia. Nat Commun. 2020;11:939.
Oversti S, Majander K, Salmela E, Salo K, Arppe L, Belskiy S, et al. Human mitochondrial DNA lineages in Iron-Age Fennoscandia suggest incipient admixture and eastern introduction of farming-related maternal ancestry. Sci Rep. 2019;9:16883.
Jeong C, Balanovsky O, Lukianova E, Kahbatkyzy N, Flegontov P, Zaporozhchenko V, et al. The genetic history of admixture across inner Eurasia. Nat Ecol Evol. 2019;3:966–76.
Wall JD, Yang MA, Jay F, Kim SK, Durand EY, Stevison LS, et al. Higher levels of neanderthal ancestry in East Asians than in Europeans. Genetics. 2013;194:199–209.
Laurini JA, Perry AM, Boilesen E, Diebold J, Maclennan KA, Muller-Hermelink HK, et al. Classification of non-Hodgkin lymphoma in Central and South America: a review of 1028 cases. Blood. 2012;120:4795–801.
Arnaiz-Villena A, Parga-Lozano C, Moreno E, Areces C, Rey D, Gomez-Prieto P. The origin of amerindians and the peopling of the Americas according to HLA genes: admixture with Asian and pacific people. Curr Genom. 2010;11:103–14.
Moorjani P, Thangaraj K, Patterson N, Lipson M, Loh PR, Govindaraj P, et al. Genetic evidence for recent population mixture in India. Am J Hum Genet. 2013;93:422–38.
Sud A, Chattopadhyay S, Thomsen H, Sundquist K, Sundquist J, Houlston RS, et al. Analysis of 153 115 patients with hematological malignancies refines the spectrum of familial risk. Blood. 2019;134:960–9.
Speedy HE, Kinnersley B, Chubb D, Broderick P, Law PJ, Litchfield K, et al. Germ line mutations in shelterin complex genes are associated with familial chronic lymphocytic leukemia. Blood. 2016;128:2319–26.
Dameshek W, SH, Arbor B. Chronic lymphatic leukemia in twin brothers aged fifty-six. JAMA. 1929;92:1348–9.
Brok-Simoni F, Rechavi G, Katzir N, Ben-Bassat I. Chronic lymphocytic leukaemia in twin sisters: monozygous but not identical. Lancet. 1987;1:329–30.
Speedy HE, Di Bernardo MC, Sava GP, Dyer MJ, Holroyd A, Wang Y, et al. A genome-wide association study identifies multiple susceptibility loci for chronic lymphocytic leukemia. Nat Genet. 2014;46:56–60.
Berndt SI, Skibola CF, Joseph V, Camp NJ, Nieters A, Wang Z, et al. Genome-wide association study identifies multiple risk loci for chronic lymphocytic leukemia. Nat Genet. 2013;45:868–76.
Law PJ, Sud A, Mitchell JS, Henrion M, Orlando G, Lenive O, et al. Genome-wide association analysis of chronic lymphocytic leukaemia, Hodgkin lymphoma and multiple myeloma identifies pleiotropic risk loci. Sci Rep. 2017;7:41071.
Coombs CC, Rassenti LZ, Falchi L, Slager SL, Strom SS, Ferrajoli A, et al. Single nucleotide polymorphisms and inherited risk of chronic lymphocytic leukemia among African Americans. Blood. 2012;120:1687–90.
Wu SJ, Huang SY, Lin CT, Lin YJ, Chang CJ, Tien HF. The incidence of chronic lymphocytic leukemia in Taiwan, 1986-2005: a distinct increasing trend with birth-cohort effect. Blood. 2010;116:4430–5.
Marinelli M, Ilari C, Xia Y, Del Giudice I, Cafforio L, Della Starza I, et al. Immunoglobulin gene rearrangements in Chinese and Italian patients with chronic lymphocytic leukemia. Oncotarget. 2016;7:20520–31.
Xia Y, Fan L, Wang L, Gale RP, Wang M, Tian T, et al. Frequencies of SF3B1, NOTCH1, MYD88, BIRC3 and IGHV mutations and TP53 disruptions in Chinese with chronic lymphocytic leukemia: disparities with Europeans. Oncotarget. 2015;6:5426–34.
Yi SH, Yan YT, Jin MT, Xiong WJ, Li ZJ, Yu Y, et al. High frequency mutations of MYD88 and KMT2D in Chinese chronic lymphocytic leukemia. Blood. 2019;134:2761.
https://www.mycancergenome.org/content/disease/chronic-lymphocytic-leukemia/#ref-2.
Consortium APG. AACR project GENIE: powering precision medicine through an international consortium. Cancer Discov. 2017;7:818–31.
Jeromin S, Weissmann S, Haferlach C, Dicker F, Bayer K, Grossmann V, et al. SF3B1 mutations correlated to cytogenetics and mutations in NOTCH1, FBXW7, MYD88, XPO1 and TP53 in 1160 untreated CLL patients. Leukemia. 2014;28:108–17.
Beekman R, Campo E. Shelterins, a genetic crossroad in CLL. Blood. 2016;128:2279–80.
https://en.wikipedia.org/wiki/List_of_countries_by_total_health_expenditure_per_capita.
https://www.worldometers.info/demographics/us-demographics/.
www.statista.com › Society › Demographics.
Ko BS, Chen LJ, Huang HH, Wen YC, Liao CY, Chen HM, et al. Subtype-specific epidemiology of lymphoid malignancies in Taiwan compared to Japan and the United States, 2002–2012. Cancer Med. 2018;7:5820–31.
Smith A, Crouch S, Lax S, Li J, Painter D, Howell D, et al. Lymphoma incidence, survival and prevalence 2004–2014: sub-type analyses from the UK’s Haematological Malignancy Research Network. Br J Cancer. 2015;112:1575–84.
Shirley MH, Sayeed S, Barnes I, Finlayson A, Ali R. Incidence of haematological malignancies by ethnic group in England, 2001–2007. Br J Haematol. 2013;163:465–77.
https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type.
Sall A, Toure AO, Sall FB, Ndour M, Fall S, Sene A, et al. Characteristics of chronic lymphocytic leukemia in Senegal. BMC Hematol. 2016;16:10.
Mulwa-Babu E, Paresh D, Riyat M. Chronic lymphocytic leukemia in Kenya: an immunophenotypic and clinicopathologic study. J Afr Cancer. 2013;5:192–7.
Omoti CE, Awodu OA, Bazuaye GN. Chronic lymphoid leukaemia: clinico-haematological correlation and outcome in a single institution in Niger Delta region of Nigeria. Int J Lab Hematol. 2007;29:426–32.
Yang S, Gale RP, Shi H, Liu Y, Lai Y, Lu J, et al. Is there an epidemic of chronic lymphocytic leukaemia (CLL) in China? Leuk Res. 2018;73:16–20.
Qiu HX, Xu W, Cao XS, Zhou M, Shen YF, Xu YL, et al. Cytogenetic characterisation in Chinese patients with chronic lymphocytic leukemia: a prospective, multicenter study on 143 cases analysed with interphase fluorescence in situ hybridisation. Leuk Lymphoma. 2008;49:1887–92.
Li H, Yi SH, Xiong WJ, Liu HM, Lyu R, Wang TY, et al. Chronic lymphocytic leukemia prognostic index: a new integrated scoring system to predict the time to first treatment in chinese patients with chronic lymphocytic leukemia. Chin Med J. 2017;130:135–42.
Choi Y, Lee JH, Jung CW, Jo JC, Kim JS, Kim I, et al. Treatment outcome and prognostic factors of Korean patients with chronic lymphocytic leukemia: a multicenter retrospective study. Korean J Intern Med. 2020; https://doi.org/10.3904/kjim.2019.210.
Rani L, Mathur N, Gogia A, Vishnubhatla S, Kumar L, Sharma A, et al. Immunoglobulin heavy chain variable region gene repertoire and B-cell receptor stereotypes in Indian patients with chronic lymphocytic leukemia. Leuk Lymphoma. 2016;57:2389–400.
Geographic Diversity and Management of CLL in Indian Patients, iwCLL 2019.
Tejaswi V, Lad DP, Jindal N, Prakash G, Malhotra P, Khadwal A, et al. Chronic lymphocytic leukemia: real-world data from India. JCO Glob Oncol. 2020;6:866–72.
Stanganelli C, Torres DC, Ortega C, Sotelo N, Marquez ME, Segges P, et al. Distinctive IGHV gene usage and stereotyped receptors in South American patients with chronic lymphocytic leukemia. Hematol Oncol. 2019;37:644–8.
Cruz-Mora A, Murrieta-Alvarez I, Olivares-Gazca JC, Leon-Pena A, Cantero-Fortiz Y, Garcia-Navarrete YI, et al. Up to half of patients diagnosed with chronic lymphocytic leukemia in Mexico may not require treatment. Hematology. 2020;25:156–9.
Strati P, Parikh SA, Chaffee KG, Kay NE, Call TG, Achenbach SJ, et al. Relationship between co-morbidities at diagnosis, survival and ultimate cause of death in patients with chronic lymphocytic leukaemia (CLL): a prospective cohort study. Br J Haematol. 2017;178:394–402.
Gentile M, Shanafelt TD, Rossi D, Laurenti L, Mauro FR, Molica S, et al. Validation of the CLL-IPI and comparison with the MDACC prognostic index in newly diagnosed patients. Blood. 2016;128:2093–5.
Acknowledgements
Profs. Robin Foa’ (Universita “La Sapienza” di Roma), Kanti Rai (Northwell Health), Daniel Catovsky, Gerald Marti (National Institutes of Health) and Marc Goodman (Cedars-Sinai Medical Centre) kindly reviewed the typescript. RPG acknowledges support from the National Institute of Health Research (NIHR) Biomedical Research Centre funding scheme.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, S., Varghese, A.M., Sood, N. et al. Ethnic and geographic diversity of chronic lymphocytic leukaemia. Leukemia 35, 433–439 (2021). https://doi.org/10.1038/s41375-020-01057-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41375-020-01057-5
This article is cited by
-
Unexpected chronic lymphocytic leukemia B cell activation by bisphosphonates
Cancer Immunology, Immunotherapy (2024)
-
Ibrutinib versus bendamustine plus rituximab for first-line treatment of 65 or older patients with untreated chronic lymphocytic leukemia without del(17p)/TP53 mutation in China: a lifetime economic research study
BMC Health Services Research (2023)