Abstract
Introduction
To evaluate the effect of antenatal magnesium sulfate (MgSO4) on mortality and morbidity outcomes related to the gastrointestinal system (GI) in preterm infants.
Methods
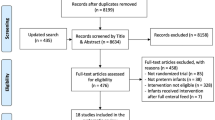
Data sources: A systematic literature search was conducted in November 2022. PubMed, CINAHL Plus with Full Text (EBSCOhost), Embase (Elsevier), and CENTRAL (Ovid) were searched. There were 6695 references. After deduplication, 4332 remained. Ninety-nine full-text articles were assessed and forty four articles were included in the final analysis.
Study eligibility criteria
Randomized or quasi-randomized clinical trials and observational studies that evaluated at least one of the pre-specified outcomes were included. Preterm infants whose mothers were given antenatal MgSO4 were included and whose mothers did not receive antenatal MgSO4 were the comparators. The main outcomes and measures were: Necrotizing enterocolitis (NEC) (stage ≥ 2), surgical NEC, spontaneous intestinal perforation (SIP), feeding intolerance, time to reach full feeds, and GI-associated mortality.
Study appraisal and synthesis methods
A random-effects model meta-analysis was performed to yield pooled OR and its 95% CI for each outcome due to expected heterogeneity in the studies. The analysis for each predefined outcome was performed separately for adjusted and unadjusted comparisons. All included studies were assessed for methodological quality. The risk of bias was assessed using elements of the Cochrane Collaboration’s tool 2.0 and the Newcastle–Ottawa Scale for randomized controlled trials (RCTs) and non-randomized studies (NRS), respectively. The study findings were reported as per PRISMA guidelines.
Results
A total of thirty-eight NRS and six RCTs involving 51,466 preterm infants were included in the final analysis. There were no increased odds of stage ≥2 NEC, (NRS : n = 45,524, OR: 0.95; 95% CI: 0.84–1.08, I2- 5% & RCT’s: n = 5205 OR: 1.00; 95% CI: 0.89–1.12, I2- 0%), SIP (n = 34,186, OR: 1.22, 95% CI: 0.94–1.58, I2–30%), feeding intolerance (n = 414, OR: 1.06, 95% CI: 0.64–1.76, I2–12%) in infants exposed to antenatal MgSO4. On the contrary, the incidence of surgical NEC was significantly lower in MgSO4 exposure infants (n = 29,506 OR:0.74; 95% CI: 0.62–0.90, ARR: 0.47%). Studies assessing the effect on GI-related mortality were limited to make any conceivable conclusion. The certainty of evidence (CoE) for all outcomes was adjudged as ‘very low’ as per GRADE.
Conclusion
Antenatal magnesium sulfate did not increase the incidence of gastrointestinal-related morbidities or mortality in preterm infants. With the current evidence concerns, regarding the adverse effects of MgSO4 administration leading to NEC/SIP or GI-related mortality in preterm infants should not be a hurdle in its routine use in antenatal mothers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
All data included in the analysis are available in public domain. The details including search strategy, list of excluded studies with reason for exclusion, risk of bias assessment and quality assessment of included studies are all available in the online supplementary file.
References
Mittendorf R. Magnesium sulfate tocolysis: time to quit. Obstet Gynecol. 2007;109:1204–5.
Nelson KB, Grether JK. Can magnesium sulfate reduce the risk of cerebral palsy in very low birthweight infants? Pediatrics. 1995;95:263–9.
Costantine MM, Weiner SJ, Eunice Kennedy Shriver National Institute of Child H, Human Development Maternal-Fetal Medicine Units N. Effects of antenatal exposure to magnesium sulfate on neuroprotection and mortality in preterm infants: a meta-analysis. Obstet Gynecol. 2009;114:354–64.
Zeng X, Xue Y, Tian Q, Sun R, An R. Effects and safety of magnesium sulfate on neuroprotection: a meta-analysis based on PRISMA guidelines. Medicine (Baltimore). 2016;95:e2451.
Committee Opinion No. 455. Magnesium sulfate before anticipated preterm birth for neuroprotection. Obstet Gynecol. 2010;115:669–71.
WHO recommendations on interventions to improve preterm birth outcomes. Geneva, Switzerland: World Health Organization; 2015.
Crowther CA, Middleton PF, Voysey M, Askie L, Duley L, Pryde PG, et al. Assessing the neuroprotective benefits for babies of antenatal magnesium sulphate: an individual participant data meta-analysis. PLoS Med. 2017;14:e1002398.
Wilson A, Hodgetts-Morton VA, Marson EJ, Markland AD, Larkai E, Papadopoulou A, et al. Tocolytics for delaying preterm birth: a network meta-analysis (0924). Cochrane Database Syst Rev. 2022;8:CD014978.
Duley L, Gulmezoglu AM, Henderson-Smart DJ, Chou D. Magnesium sulphate and other anticonvulsants for women with pre-eclampsia. Cochrane Database Syst Rev. 2010;2010:CD000025.
Cruikshank DP, Pitkin RM, Reynolds WA, Williams GA, Hargis GK. Effects of magnesium sulfate treatment on perinatal calcium metabolism. I. Maternal and fetal responses. Am J Obstet Gynecol. 1979;134:243–9.
Lu JF, Nightingale CH. Magnesium sulfate in eclampsia and pre-eclampsia: pharmacokinetic principles. Clin Pharmacokinet. 2000;38:305–14.
Santafe MM, Garcia N, Lanuza MA, Tomas M, Besalduch N, Tomas J. Presynaptic muscarinic receptors, calcium channels, and protein kinase C modulate the functional disconnection of weak inputs at polyinnervated neonatal neuromuscular synapses. J Neurosci Res. 2009;87:1195–206.
Riaz M, Porat R, Brodsky NL, Hurt H. The effects of maternal magnesium sulfate treatment on newborns: a prospective controlled study. J Perinatol. 1998;18:449–54.
Rantonen T, Kaapa P, Jalonen J, Ekblad U, Peltola O, Valimaki I, et al. Antenatal magnesium sulphate exposure is associated with prolonged parathyroid hormone suppression in preterm neonates. Acta Paediatr. 2001;90:278–81.
Malaeb SN, Rassi AI, Haddad MC, Seoud MA, Yunis KA. Bone mineralization in newborns whose mothers received magnesium sulphate for tocolysis of premature labour. Pediatr Radio. 2004;34:384–6.
Mehta R, Petrova A. Intrapartum magnesium sulfate exposure attenuates neutrophil function in preterm neonates. Biol Neonate. 2006;89:99–103.
Gordon PV, Price WA, Stiles AD, Rutledge JC. Early postnatal dexamethasone diminishes transforming growth factor alpha localization within the ileal muscularis propria of newborn mice and extremely low-birth-weight infants. Pediatr Dev Pathol. 2001;4:532–7.
Gordon PV, Paxton JB, Herman AC, Carlisle EM, Fox NS. Igf-I accelerates ileal epithelial cell migration in culture and newborn mice and may be a mediator of steroid-induced maturation. Pediatr Res. 2004;55:34–41.
Iams J. CR, In: Creasy RK RR, Iams J, Lockwood, C MTe. Preterm labor and delivery. Maternal-Fetal Medicine: Principles and Practice. 2004. pp 623–61.
Havranek T, Ashmeade TL, Afanador M, Carver JD. Effects of maternal magnesium sulfate administration on intestinal blood flow velocity in preterm neonates. Neonatology. 2011;100:44–9.
Gursoy T, Imamoglu EY, Ovali F, Karatekin G. Effects of antenatal magnesium exposure on intestinal blood flow and outcome in preterm neonates. Am J Perinatol. 2015;32:1064–9.
Fang S, Kempley ST, Gamsu HR. Prediction of early tolerance to enteral feeding in preterm infants by measurement of superior mesenteric artery blood flow velocity. Arch Dis Child Fetal Neonatal Ed. 2001;85:F42–5.
Robel-Tillig E, Knupfer M, Pulzer F, Vogtmann C. Blood flow parameters of the superior mesenteric artery as an early predictor of intestinal dysmotility in preterm infants. Pediatr Radio. 2004;34:958–62.
Maruyama K, Koizumi T, Tomomasa T, Morikawa A. Intestinal blood-flow velocity in uncomplicated preterm infants during the early neonatal period. Pediatr Radio. 1999;29:472–7.
Coombs RC, Morgan ME, Durbin GM, Booth IW, McNeish AS. Abnormal gut blood flow velocities in neonates at risk of necrotising enterocolitis. J Pediatr Gastroenterol Nutr. 1992;15:13–9.
Kempley ST, Gamsu HR. Superior mesenteric artery blood flow velocity in necrotising enterocolitis. Arch Dis Child. 1992;67:793–6.
Rattray BN, Kraus DM, Drinker LR, Goldberg RN, Tanaka DT, Cotten CM. Antenatal magnesium sulfate and spontaneous intestinal perforation in infants less than 25 weeks gestation. J Perinatol. 2014;34:819–22.
Kamyar M, Clark EA, Yoder BA, Varner MW, Manuck TA. Antenatal magnesium sulfate, necrotizing enterocolitis, and death among neonates <28 weeks gestation. AJP Rep. 2016;6:e148–54.
Shalabi M, Mohamed A, Lemyre B, Aziz K, Faucher D, Shah PS, et al. Antenatal exposure to magnesium sulfate and spontaneous intestinal perforation and necrotizing enterocolitis in extremely preterm neonates. Am J Perinatol. 2017;34:1227–33.
Wiswell TE, Caddell JL, Graziani LJ, Kornhauser MS, Spitzer AR. Maternally-administered magne- sium sulfate (MgSO4) decreases the incidence of severe necrotizing enterocolitis (NEC) in preterm infants: a prospective study. Pediatr Res. 1996;39:1501.
Mikhael M, Bronson C, Zhang L, Curran M, Rodriguez H, Bhakta KY. Lack of evidence for time or dose relationship between antenatal magnesium sulfate and intestinal injury in extremely preterm neonates. Neonatology. 2019;115:371–8.
Shepherd E, Salam RA, Manhas D, Synnes A, Middleton P, Makrides M, et al. Antenatal magnesium sulphate and adverse neonatal outcomes: a systematic review and meta-analysis. PLoS Med. 2019;16:e1002988.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Walsh MC, Kliegman RM. Necrotizing enterocolitis: treatment based on staging criteria. Pediatr Clin North Am. 1986;33:179–201.
Meyer CL, Payne NR, Roback SA. Spontaneous, isolated intestinal perforations in neonates with birth weight less than 1000 g not associated with necrotizing enterocolitis. J Pediatr Surg. 1991;26:714–7.
Cumpston M, Li T, Page MJ, Chandler J, Welch VA, Higgins J, et al. Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev. 2019;10:ED000142.
Wells G, Shea B, O’Connell D, Peterson J, Welch v, Losos M, et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2012.
Schunemann HJ. GRADE: from grading the evidence to developing recommendations. A description of the system and a proposal regarding the transferability of the results of clinical research to clinical practice. Z Evid Fortbild Qual Gesundh. 2009;103:391–400.
Wan X, Wang W, Liu J, Tong T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol. 2014;14:135.
Crowther CA, Hiller JE, Doyle LW, Haslam RR. Effect of magnesium sulfate given for neuroprotection before preterm birth: a randomized controlled trial. Jama. 2003;290:2669–76.
Gupta NGR, Gupta A, Garg R, Mishra S. Magnesium sulfate for fetal neuroprotection in women at risk of preterm birth: analysis of its effect on cerebral palsy. J South Asian Feder Obst Gynae. 2021;13:90–3.
Marret S, Marpeau L, Zupan-Simunek V, Eurin D, Leveque C, Hellot M-F, et al. Magnesium sulphate given before very-preterm birth to protect infant brain: the randomised controlled PREMAG trial*. Bjog. 2007;114:310–8.
Paradisis M, Osborn DA, Evans N, Kluckow M. Randomized controlled trial of magnesium sulfate in women at risk of preterm delivery-neonatal cardiovascular effects. J Perinatol. 2012;32:665–70.
Rouse DJ, Hirtz DG, Thom E, Varner MW, Spong CY, Mercer BM, et al. A randomized, controlled trial of magnesium sulfate for the prevention of cerebral palsy. N Engl J Med. 2008;359:895–905.
Wolf HT, Brok J, Henriksen TB, Greisen G, Salvig JD, Pryds O, et al. Antenatal magnesium sulphate for the prevention of cerebral palsy in infants born preterm: a double-blind, randomised, placebo-controlled, multi-centre trial. BJOG. 2020;127:1217–25.
de Veciana M, Porto M, Major CA, Barke JI. Tocolysis in advanced preterm labor: impact on neonatal outcome. Am J Perinatol. 1995;12:294–8.
Schanler RJ, Smith LG Jr, Burns PA. Effects of long-term maternal intravenous magnesium sulfate therapy on neonatal calcium metabolism and bone mineral content. Gynecol Obstet Invest. 1997;43:236–41.
Kimberlin DF, Hauth JC, Goldenberg RL, Bottoms SF, Iams JD, Mercer B, et al. The effect of maternal magnesium sulfate treatment on neonatal morbidity in < or = 1000-gram infants. Am J Perinatol. 1998;15:635–41.
Elimian A, Verma R, Ogburn P, Wiencek V, Spitzer A, Quirk JG. Magnesium sulfate and neonatal outcomes of preterm neonates. J Matern Fetal Neonatal Med. 2002;12:118–22.
Jazayeri A, Jazayeri MK, Sutkin G. Tocolysis does not improve neonatal outcome in patients with preterm rupture of membranes. Am J Perinatol. 2003;20:189–93.
Yokoyama K, Takahashi N, Yada Y, Koike Y, Kawamata R, Uehara R, et al. Prolonged maternal magnesium administration and bone metabolism in neonates. Early Hum Dev. 2010;86:187–91.
Basu SK, Chickajajur V, Lopez V, Bhutada A, Pagala M, Rastogi S. Immediate clinical outcomes in preterm neonates receiving antenatal magnesium for neuroprotection. J Perinat Med. 2011;40:185–9.
Lee NY, Cho SJ, Park EA. Influence of antenatal magnesium sulfate exposure on perinatal outcomes in VLBW infants with maternal preeclampsia. Neonatal Med. 2013;20:28–34.
Weisz DE, Shivananda S, Asztalos E, Yee W, Synnes A, Lee SK, et al. Intrapartum magnesium sulfate and need for intensive delivery room resuscitation. Arch Dis Child Fetal Neonatal Ed. 2015;100:F59–65.
James AT, Corcoran JD, Hayes B, Franklin O, El-Khuffash A. The effect of antenatal magnesium sulfate on left ventricular afterload and myocardial function measured using deformation and rotational mechanics imaging. J Perinatol. 2015;35:913–8.
Suh BS, Ko KH, Bang JS, Joung Y, Lee YJ, Lee JW, et al. Neonatal outcomes of premature infants who were delivered from mother with hypertensive disorders of pregnancy and effects of antihypertensive drugs and MgSO4. kjp. 2015;26:190–9.
Bouet PE, Brun S, Madar H, Baisson AL, Courtay V, Gascoin-Lachambre G, et al. Implementation of an antenatal magnesium sulfate protocol for fetal neuroprotection in preterm infants. Sci Rep. 2015;5:14732.
Bozkurt O, Eras Z, Canpolat FE, Oguz SS, Uras N, Dilmen U. Antenatal magnesium sulfate and neurodevelopmental outcome of preterm infants born to preeclamptic mothers. J Matern Fetal Neonatal Med. 2016;29:1101–4.
De Jesus LC, Sood BG, Shankaran S, Kendrick D, Das A, Bell EF, et al. Antenatal magnesium sulfate exposure and acute cardiorespiratory events in preterm infants. Am J Obstet Gynecol. 2015;212:94.e91–7.
Morag I, Okrent AL, Strauss T, Staretz-Chacham O, Kuint J, Simchen MJ, et al. Early neonatal morbidities and associated modifiable and non-modifiable risk factors in a cohort of infants born at 34-35 weeks of gestation. J Matern Fetal Neonatal Med. 2015;28:876–82.
Garcia Alonso L, Pumarada Prieto M, Gonzalez Colmenero E, Concheiro Guisan A, Suarez Albo A, Duran Fernandez-Feijoo C, et al. Prenatal therapy with magnesium sulfate and its correlation with neonatal serum magnesium concentration. Am J Perinatol. 2018;35:170–6.
Lloreda-Garcia JM, Lorente-Nicolás A, Bermejo-Costa F, Martínez-Uriarte J, López-Pérez R. Necesidad de reanimación en prematuros menores de 32 semanas expuestos a sulfato de magnesio para neuroprotección fetal. Rev Chil de Pediatría. 2016;87:261–7.
Downey LC, Cotten CM, Hornik CP, Laughon MM, Toila VN, Clark RH, et al. Association of in utero magnesium exposure and spontaneous intestinal perforations in extremely low birth weight infants. J Perinatol. 2017;37:641–4.
Jung EJ, Byun JM, Kim YN, Lee KB, Sung MS, Kim KT, et al. Antenatal magnesium sulfate for both tocolysis and fetal neuroprotection in premature rupture of the membranes before 32 weeks’ gestation. J Matern Fetal Neonatal Med. 2018;31:1431–41.
Narasimhulu D, Brown A, Egbert NM, Rojas M, Haberman S, Bhutada A, et al. Maternal magnesium therapy, neonatal serum magnesium concentration and immediate neonatal outcomes. J Perinatol. 2017;37:1297–303.
Stockley EL, Ting JY, Kingdom JC, McDonald SD, Barrett JF, Synnes AR, et al. Intrapartum magnesium sulfate is associated with neuroprotection in growth-restricted fetuses. Am J Obstet Gynecol. 2018;219:606.e601–606.e608.
Qasim A, Jain SK, Aly AM. Antenatal magnesium sulfate exposure and hemodynamically significant patent ductus arteriosus in premature infants. AJP Rep. 2019;9:e353–6.
Özlü F, Hacıoğlu C, Büyükkurt S, Yapıcıoğlu H, Satar M. Changes on preterm morbidities with antenatal magnesium. Cukurova Med J. 2019;44:502–8.
Gochi Valdovinos A, Arriaga-Redondo M, Dejuan Bitriá E, Pérez Rodríguez I, Márquez Isidro E, Blanco Bravo D. Terapia prenatal con sulfato de magnesio y obstrucción intestinal por meconio en recién nacidos pretérmino. An de Pediatría. 2022;96:138–44.
Hong JY, Hong JY, Choi YS, Kim YM, Sung JH, Choi SJ, et al. Antenatal magnesium sulfate treatment and risk of necrotizing enterocolitis in preterm infants born at less than 32 weeks of gestation. Sci Rep. 2020;10:12826.
Kim SH, Kim YJ, Shin SH, Cho H, Shin SH, Kim EK, et al. Antenatal magnesium sulfate and intestinal morbidities in preterm infants with extremely low gestational age. Pediatr Neonatol. 2021;62:202–7.
Üstün N, Hocaoğlu M, Turgut A, Ovalı F. Effects of antenatal magnesium sulfate use for neuroprotection on cardiorespiratory complications during the early neonatal period in preterm infants. J Surg Med [Internet]. 2021;5:843–7.
Chandran S, Tergestina M, Ross B, Joshi A, Rebekah G, Kumar M. Effects of antenatal magnesium sulfate on the gut function of preterm (<32 weeks) very low birth weight neonates: experience from a Tertiary Institute in South India. J Trop Pediatr. 2021;67:1–9.
Ayed M, Ahmed J, More K, Ayed A, Husain H, AlQurashi A, et al. Antenatal magnesium sulfate for preterm neuroprotection: a single-center experience from Kuwait Tertiary NICU. Biomed Hub. 2022;7:80–7.
Sung SI, Ahn SY, Choi SJ, Oh SY, Roh CR, Yang M, et al. Increased risk of meconium-related ileus in extremely premature infants exposed to antenatal magnesium sulfate. Neonatology. 2022;119:68–76.
Bansal V, Desai A. Efficacy of antenatal magnesium sulfate for neuroprotection in extreme prematurity: a comparative observational study. J Obstet Gynaecol India. 2022;72:36–47.
Özlü F, Hacıoğlu C, Büyükkurt S, Yapıcıoğlu H, Satar M. Changes on preterm morbidities with antenatal magnesium. Cukurova Med J. 2019;44:502–8.
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928.
Krinsky DL. Natural products: show me the data. Am J Health Syst Pharm. 1998;55:125.
Ghidini A, Espada RA, Spong CY. Does exposure to magnesium sulfate in utero decrease the risk of necrotizing enterocolitis in premature infants? Acta Obstet Gynecol Scand. 2001;80:126–9.
Author information
Authors and Affiliations
Contributions
AP: conceptualized, formulated the research methodology, performed formal analysis, curated data, and wrote the original draft, reviewed and edited the manuscript. Nell Aronoff participated in formulating the research methodology and provided resources for the literature search. She also contributed to writing, reviewing, and editing the manuscript. PC: administered the project and also contributed to manuscript writing, reviewing and editing. SD: conceptualized, formulated the research methodology, performed formal analysis, curated data, wrote the original draft, reviewed, edited the manuscript, supervised/administered the whole project and guarantor for the project. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
AP, NA, and SD: have no relevant conflicts to disclose. PC: was supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD; grant number: R01HD104909 and the National Institutes of Health (NIH)/National Heart Lung and Blood Institute (NHLBI; grant no.: K12 HL138052). The results of this manuscript are not supported or endorsed by any of the funding institutions.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Prasath, A., Aronoff, N., Chandrasekharan, P. et al. Antenatal Magnesium Sulfate and adverse gastrointestinal outcomes in Preterm infants—a systematic review and meta-analysis. J Perinatol 43, 1087–1100 (2023). https://doi.org/10.1038/s41372-023-01710-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01710-8