Abstract
Objective
Our aim was to examine the frequency and type of placental abnormalities in neonates with LSV.
Study design
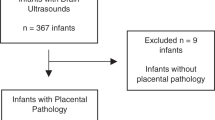
We prospectively reviewed cranial ultrasounds (cUS) from neonates born at ≤32 weeks of gestation at Parkland Hospital between 2012 and 2014. Our cohort included neonates with LSV and gestational age and sex matched controls with normal cUS. We retrieved placental pathology reports retrospectively and compared placental abnormalities in both groups.
Results
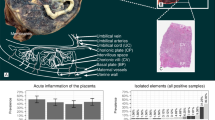
We reviewed 1351 cUS from a total of 407 neonates. Placental pathology evaluations were complete for 64/65 (98%) neonates with LSV and 68/70 (97%) matched controls. There were no significant differences for any type of placental abnormities between LSV and control groups. However, infants with highest stage LSV were more likely to have large for gestational age (LGA) placentas (p = 0.01).
Conclusion
The association between LSV and LGA placenta may indicate a shared vascular response to an adverse prenatal environment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request and may require institutional data agreements.
References
Teele RL, Hernanz-Schulman M, Sotrel A. Echogenic vasculature in the basal ganglia of neonates: a sonographic sign of vasculopathy. Radiology 1988;169:423–7.
Ben-Ami T, Yousefzadeh D, Backus M, Reichman B, Kessler A, Hammerman-Rozenberg C. Lenticulostriate vasculopathy in infants with infections of the central nervous system sonographic and Doppler findings. Pediatr Radio. 1990;20:575–9.
Cantey JB, Sisman J. The etiology of lenticulostriate vasculopathy and the role of congenital infections. Early Hum Dev. 2015;91:427–30.
Sisman J, Chalak L, Heyne R, Pritchard M, Weakley D, Brown LS, et al. Lenticulostriate vasculopathy in preterm infants: a new classification, clinical associations and neurodevelopmental outcome. J Perinatol. 2018;38:1370–8.
Redline RW. Placental pathology: a systematic approach with clinical correlations. Placenta. 2008;29:S86–91.
Khong TY, Mooney EE, Ariel I, Balmus NC, Boyd TK, Brundler MA, et al. Sampling and definitions of placental lesions: Amsterdam Placental Workshop Group Consensus Statement. Arch Pathol Lab Med. 2016;140:698–713.
Mittendorf R, Covert R, Pryde PG, Lee KS, Ben-Ami T, Yousefzadeh D. Association between lenticulostriate vasculopathy (LSV) and neonatal intraventricular hemorrhage (IVH). J Perinatol. 2004;24:700–5.
Hemachandra AH, Oravec D, Collin M, Tafari N, Mhanna MJ. Early and late postnatal identification of isolated lenticulostriate vasculopathy in preterm infants: associated findings. J Perinatol. 2003;23:20–3.
Strand C, Laptook AR, Dowling S, Campbell N, Lasky RE, Wallin LA, et al. Neonatal intracranial hemorrhage: I. Changing pattern in inborn low-birth-weight infants. Early Hum Dev. 1990;23:117–28.
Greer LG, Ziadie MS, Casey BM, Rogers BB, McIntire DD, Leveno KJ. An immunologic basis for placental insufficiency in fetal growth restriction. Am J Perinatol. 2012;29:533–8.
Mir IN, Johnson-Welch SF, Nelson DB, Brown LS, Rosenfeld CR, Chalak LF. Placental pathology is associated with severity of neonatal encephalopathy and adverse developmental outcomes following hypothermia. Am J Obstet Gynecol. 2015;213:849 e1–7.
Pinar H, Sung CJ, Oyer CE, Singer DB. Reference values for singleton and twin placental weights. Pediatr Pathol Lab Med. 1996;16:901–7.
Chalak L, Redline RW, Goodman AM, Juul SE, Chang T, Yanowitz TD, et al. Acute and chronic placental abnormalities in a multicenter cohort of newborn infants with hypoxic-ischemic encephalopathy. J Pediatr. 2021;237:190–6.
Zhou YY, Ravishankar S, Luo G, Redline RW. Predictors of high grade and other clinically significant placental findings by indication for submission in singleton placentas from term births. Pediatr Dev Pathol. 2020;23:274–84.
Mir IN, Chalak LF, Brown LS, Johnson-Welch S, Heyne R, Rosenfeld CR, et al. Impact of multiple placental pathologies on neonatal death, bronchopulmonary dysplasia, and neurodevelopmental impairment in preterm infants. Pediatr Res. 2020;87:885–91.
Khalife N, Glover V, Hartikainen AL, Taanila A, Ebeling H, Jarvelin MR, et al. Placental size is associated with mental health in children and adolescents. PLoS One. 2012;7:e40534.
Tegethoff M, Greene N, Olsen J, Meyer AH, Meinlschmidt G. Maternal psychosocial stress during pregnancy and placenta weight: evidence from a national cohort study. PLoS One. 2010;5:e14478.
Barker DJ. Maternal nutrition and cardiovascular disease. Nutr Health. 1993;9:99–106.
Barker DJ, Gluckman PD, Godfrey KM, Harding JE, Owens JA, Robinson JS. Fetal nutrition and cardiovascular disease in adult life. Lancet 1993;341:938–41.
Sun C, Groom KM, Oyston C, Chamley LW, Clark AR, James JL. The placenta in fetal growth restriction: What is going wrong? Placenta 2020;96:10–8.
Gagnon R. Placental insufficiency and its consequences. Eur J Obstet Gynecol Reprod Biol. 2003;110:S99–107.
Lumey LH. Compensatory placental growth after restricted maternal nutrition in early pregnancy. Placenta 1998;19:105–11.
Lawrence JB, Oxvig C, Overgaard MT, Sottrup-Jensen L, Gleich GJ, Hays LG, et al. The insulin-like growth factor (IGF)-dependent IGF binding protein-4 protease secreted by human fibroblasts is pregnancy-associated plasma protein-A. Proc Natl Acad Sci USA 1999;96:3149–53.
Barker DJ, Bull AR, Osmond C, Simmonds SJ. Fetal and placental size and risk of hypertension in adult life. BMJ 1990;301:259–62.
Xu F, Yang S, Liu Y, Zheng X, Yang H, Zhang J, et al. Placental pathology and neonatal outcomes in pre-eclampsia with gestational diabetes mellitus. J Matern Fetal Neonatal Med. 2021;34:1149–54.
Fatayerji N, Engelmann GL, Myers T, Handa RJ. In utero exposure to ethanol alters mRNA for insulin-like growth factors and insulin-like growth factor-binding proteins in placenta and lung of fetal rats. Alcohol Clin Exp Res. 1996;20:94–100.
Mittal P, Espinoza J, Hassan S, Kusanovic JP, Edwin SS, Nien JK, et al. Placental growth hormone is increased in the maternal and fetal serum of patients with preeclampsia. J Matern Fetal Neonatal Med. 2007;20:651–9.
Macdonald EM, Natale R, Regnault TR, Koval JJ, Campbell MK. Obstetric conditions and the placental weight ratio. Placenta 2014;35:582–6.
Andescavage N, Yarish A, Donofrio M, Bulas D, Evangelou I, Vezina G, et al. 3-D volumetric MRI evaluation of the placenta in fetuses with complex congenital heart disease. Placenta 2015;36:1024–30.
Rosier-van Dunne FM, van Wezel-Meijler G, Kaschula RO, Wranz PA, Odendaal HJ, de Vries JI. Placental histology related to fetal brain sonography. Arch Dis Child Fetal Neonatal Ed 2011;96:F53–8.
Mittendorf R, Kuban K, Pryde PG, Gianopoulos JG, Yousefzadeh D. Antenatal risk factors associated with the development of lenticulostriate vasculopathy (LSV) in neonates. J Perinatol. 2005;25:101–7.
Author information
Authors and Affiliations
Contributions
Dr. Sisman, conceptualized and designed the study, drafted the initial manuscript, reviewed and revised the manuscript. Dr. Leon, BP, NNP and SB, MS collected data, carried out analysis, reviewed and revised the manuscript. Dr. Mir conceptualized and design the study, coordinated and supervised data collection, and critically reviewed the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sisman, J., Leon, R.L., Payton, B.W. et al. Placental pathology associated with lenticulostriate vasculopathy (LSV) in preterm infants. J Perinatol 43, 568–572 (2023). https://doi.org/10.1038/s41372-022-01557-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01557-5