Abstract
Objective
To evaluate how neonatologists and NICU parents perceive communication in the NICU.
Study Design
A mixed-methods approach using an online survey and three focus groups with NICU parents and neonatologists, utilizing videos of simulated conversations between a neonatologist and mother.
Results
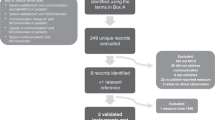
A total of 72 participants responded to the online survey. Parents ranked the invasiveness of common NICU clinical procedures differently than the neonatologist standard but assessed the quality of the simulated conversation similarly. A total of 13 parents and 6 physicians participated in the focus groups. Major themes from both neonatologist and parent focus groups were the impact of making a connection with the parents, the importance of making decisions yet not making assumptions based on the divergent use of language by neonatologists and parents, and providing hope.
Conclusions
Parents and neonatologists differ in their perception of key aspects of NICU language use and communication but also agree on many aspects.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Ely DM, Driscoll AK. Infant mortality in the United States, 2017: data from the period linked birth/infant death file. Natl Vital- Stat Rep. 2019;68:1–20.
Harrison W, Goodman D. Epidemiologic trends in neonatal intensive care, 2007–2012 | JAMA Pediatrics. JAMA Network. 2015;169:855–62.
Del Fabbro A, Cain K. Infant mental health and family mental health issues. Newborn Infant Nurs Rev. 2016;16:281–4. https://doi.org/10.1053/j.nainr.2016.09.020.
Alkozei A, McMahon E, Lahav A. Stress levels and depressive symptoms in NICU mothers in the early postpartum period. J Matern Fetal Neonatal Med. 2014;27:1738–43.
Aftyka A, Rybojad B, Rozalska I, Rzonca P, Humeniuk E. Post-traumatic stress disorder in parents of children hospitalized in the neonatal intensive care unit (NICU): Medical and demographic risk factors. Psychiatr Danubina. 2014;26:347–52.
Gonya J, Nelin LD. Factors associated with maternal visitation and participation in skin-to-skin care in an all referral level IIIc NICU. Acta Paediatr. 2013;102:e53–56.
Williams KG, Patel KT, Stausmire JM, Bridges C, Mathis MW, Barkin JL. The neonatal intensive care unit: environmental stressors and supports. Int J Environ Res Public Health. 2018;15:60.
Enke C, Oliva y Hausmann A, Miedaner F, Roth B, Woopen C. Communicating with parents in neonatal intensive care units: the impact on parental stress. Patient Educ Counseling. 2017;100:710–9.
Heydarpour S, Keshavarz Z, Bakhtiari M. Factors affecting adaptation to the role of motherhood in mothers of preterm infants admitted to the neonatal intensive care unit: a qualitative study. J Adv Nurs. 2017;73:138–48.
Labrie NHM, van Veenendaal NR, Ludolph RA, Ket JCF, van der Schoor SRD, van Kempen AAMW. Effects of parent-provider communication during infant hospitalization in the NICU on parents: a systematic review with meta-synthesis and narrative synthesis. Patient Educ Couns 2021;104:1526–52.
Slomian J, Honvo G, Emonts P, Reginster JY, Bruyère O. Consequences of maternal postpartum depression: A systematic review of maternal and infant outcomes. Women’s Health (Lond). 2019;15:1–55.
Fallon V, Groves R, Halford JC, Bennett KM, Harrold JA. Postpartum anxiety and infant-feeding outcomes. J Hum Lact. 2016;32:740–58.
O’Brien K, Bracht M, Macdonell K, McBride T, Robson K, O’Leary L, et al. A pilot cohort analytic study of Family Integrated Care in a Canadian neonatal intensive care unit. BMC Pregnancy Childbirth. 2013;13:1–8.
Weiss S, Goldlust E, Vaucher YE. Improving parent satisfaction: an intervention to increase neonatal parent-physician communication. J Perinatol. 2010;30:425–30.
Berman L, Raval MV, Ottosen M, Mackow AK, Cho M, Goldin AB. Parent perspectives on readiness for discharge home after neonatal intensive care unit admission. J Pediatr. 2019;205:98–104.
Lorié ES, Wreesmann WW, van Veenendaal NR, van Kempen AAMW, Labrie NHM. Parents’ needs and perceived gaps in communication with healthcare professionals in the neonatal (intensive) care unit: a qualitative interview study. Patient Educ Counseling. 2021;104:1518–25.
Wigert H, Dellenmark Blom M, Bry K. Parents’ experiences of communication with neonatal intensive-care unit staff: an interview study. BMC Pediatr. 2014;14:304.
Guttmann KF, Orfali K, Kelley AS. Measuring communication quality in the Neonatal Intensive Care Unit. Pediatr Res. 2021. https://doi.org/10.1038/s41390-021-01522-6. Online ahead of print.
Lacey J, Corbett J, Forni L, Hooper L, Hughes F, Minto G, et al. A multidisciplinary consensus on dehydration: definitions, diagnostic methods and clinical implications. Ann Med. 2019;51:232–51.
Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Res Psychol. 2006;3:77–101.
Immy H. Qualitative research in health care. McGraw-Hill Educ (UK). 2005;p90-102:147–65.
Umberger E, Canvasser J, Hall SL. Enhancing NICU parent engagement and empowerment. Semin Pediatr Surg. 2018;27:19–24.
Gale G, Franck LS, Kools S, Lynch M. Parents’ perceptions of their infant’s pain experience in the NICU. Int J Nurs Stud. 2004;41:51–8.
Clark OE, Fortney CA, Dunnells ZDO, Gerhardt CA, Baughcum AE. Parent perceptions of infant symptoms and suffering and associations with distress among bereaved parents in the NICU. J Pain Symptom Manag. 2021;S0885-3924:00209–8.
Wreesmann WW, Lorié ES, van Veenendaal NR, van Kempen AAMW, Ket JCF, Labrie NHM. The functions of adequate communication in the neonatal care unit: A systematic review and meta-synthesis of qualitative research. Patient Educ Counseling. 2020;104:1505–17.
Drago M, Lorenz JM, Hammond J, Hardart GE, Morris MC. How to hold an effective NICU family meeting: capturing parent perspectives to build a more robust framework. J Perinatol. 2021;41:2217–24. https://doi.org/10.1038/s41372-021-01051-4. Epub 2021 Apr 21.
Boss RD, Urban A, Barnett MD, Arnold RM. Neonatal critical care communication (NC3): training NICU physicians and nurse practitioners. J Perinatol. 2013;33:642–6.
Grobman WA, Kavanaugh K, Moro T, DeRegnier R-A, Savage T. Providing advice to parents for women at acutely high risk of periviable delivery. Obstet Gynecol. 2010;115:904–9.
Guillén Ú, Mackley A, Laventhal N, Kukora S, Christ L, Derrick M, et al. Evaluating the use of a decision aid for parents facing extremely premature delivery: a randomized trial. J Pediatr. 2019;209:52–60.e1.
Muthusamy AD, Leuthner S, Gaebler-Uhing C, Hoffmann RG, Li S-H, Basir MA. Supplemental written information improves prenatal counseling: a randomized trial. Pediatrics 2012;129:e1269–74.
Arnolds M, Laventhal N. Perinatal counseling at the margin of gestational viability: where we’ve been, where we’re going, and how to navigate a path forward. J Pediatr. 2021;233:255–62.
Drach LL. Communication between neonatologists and parents when prognosis is uncertain. J Perinatol. 2020;40:1412–22.
Gaucher N, Payot A. From powerlessness to empowerment: Mothers expect more than information from the prenatal consultation for preterm labour. Paediatr Child Health. 2011;16:638–42.
Jager S, Kavanaugh K, Hoffman S, Laitano T, Jeffries E, Tucker Edmonds B. Parents’ descriptions of neonatal palliation as a treatment option prior to periviable delivery. J Perinat Neonatal Nurs. 2020;34:178–85.
Madrigal VN, Carroll KW, Hexem KR, Faerber JA, Morrison WE, Feudtner C. Parental decision-making preferences in the pediatric intensive care unit. Crit Care Med. 2012;40:2876–82.
Feudtner C, Morrison W. The darkening veil of “do everything. Arch Pediatr Adolesc Med. 2012;166:694.
Quill TE, Arnold R, Back AL. Discussing treatment preferences with patients who want “everything”. Ann Intern Med. 2009;151:345–9.
French KB. Care of extremely small premature infants in the neonatal intensive care unit: a parent’s perspective. Clin Perinatol. 2017;44:275–82.
Boss RD, Hutton N, Sulpar LJ, West AM, Donohue PK. Values parents apply to decision-making regarding delivery room resuscitation for high-risk newborns. Pediatrics 2008;122:583–9.
Kaemingk BD, Carroll K, Thorvilson MJ, Schaepe KS, Collura CA. Uncertainty at the limits of viability: a qualitative study of antenatal consultations. Pediatrics. 2021;147:e20201865. https://doi.org/10.1542/peds.2020-1865. Epub 2021 Mar 3.
Funding
Supported by Brown Summer Assistantship Funding.
Author information
Authors and Affiliations
Contributions
RW designed the qualitative study, conducted all focus groups, administered survey, wrote manuscript, and approved final manuscript. CH contributed to study, designed quantitative survey and approved final manuscript. RT conducted statistical analysis and approved final manuscript. KH edited manuscript, performed thematic analysis, and approved final manuscript. BEL substantially contributed to study design, data acquisition, data analysis, edited and approved the final manuscript as submitted.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The study was conducted with the approval of the Women and Infants hospital Internal Review Board and was given exempt status. Informed consent was obtained from all participants in the study. The study was performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Winters, R., Hennigan, C.M., Tucker, R. et al. Words matter: exploring communication between parents and neonatologists. J Perinatol 42, 745–751 (2022). https://doi.org/10.1038/s41372-021-01293-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01293-2
This article is cited by
-
Narrative neonatology: integrating narrative medicine into the neonatal intensive care unit
Journal of Perinatology (2023)
-
Prenatally-diagnosed renal failure: an ethical framework for decision-making
Journal of Perinatology (2023)