Abstract
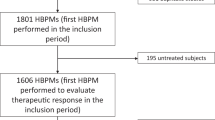
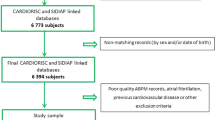
Ambulatory blood pressure monitoring (ABPM) is now considered the gold standard to evaluate BP, and predicts related cardiovascular risk. However, no study has reported the association of long-term changes in ABPM with the incidence of cardiovascular events, therefore the objective of this work. We included patients from the Bordeaux cohort of hypertensive patients, who had undergone at least two ABPM; the first was performed before or after antihypertensive treatment was started, and the second was the last recording available before any cardiovascular event. We included 591 patients (mean age, 54 years) with a 7-year average interval between the first and last ABPM, a 10-year average follow-up, and a total of 111 cardiovascular events. The patients were divided into four groups: G0, first and last 24 h systolic blood pressure (SBP) < 130; G1, first 24 h SBP ≥ 130, last 24 h SBP < 130; G2, first 24 h SBP < 130, last 24 h SBP ≥ 130; and G3, first 24 h SBP ≥ 130, last 24 h SBP ≥ 130 mmHg. Baseline ABPM better predicted future events than the last ABPM. G0 and G2 had similar survival. G1 and G3 had a worse prognosis than G0 and G2, while G1 had an intermediate risk between G0 and G3, indicating some benefit of treatment. In conclusion, our study showed the prognostic value of the first ABPM recorded in hypertensive patients and the persistence of risk when 24 h BP is controlled by antihypertensive treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Kannel WB. Blood pressure as a cardiovascular risk factor: prevention and treatment. JAMA. 1996;275:1571–6.
Andersson OK, Almgren T, Persson B, Samuelsson O, Hedner T, Wilhelmsen L. Survival in treated hypertension: follow up study after two decades. BMJ. 1998;317:167–71.
Muntner P, Shimbo D, Carey RM, Charleston JB, Gaillard T, Misra S, et al. Measurement of blood pressure in humans: a scientific statement from The American Heart Association. Hypertension. 2019;73:e35–e66.
Clement DL, De Buyzere ML, De Bacquer DA, de Leeuw PW, Duprez DA, Fagard RH, et al. Prognostic value of ambulatory blood-pressure recordings in patients with treated hypertension. N Engl J Med. 2003;348:2407–15.
Gosse P, Cremer A, Papaioannou G, Yeim S. Arterial stiffness from monitoring of timing of korotkoff sounds predicts the occurrence of cardiovascular events independently of left ventricular mass in hypertensive patients. Hypertension. 2013;62:161–7.
Cremer A, Boulestreau R, Gaillard P, Laine M, Papaioannou G, Gosse P. Twenty-four-hour central pulse pressure for cardiovascular events prediction in a low-cardiovascular-risk population: results from the Bordeaux cohort. J Am Heart Assoc. 2018;7:1–7.
O’Brien E, Parati G, Stergiou G, Asmar R, Beilin L, Bilo G, et al. European Society of Hypertension position paper on ambulatory blood pressure monitoring. J Hypertens. 2013;31:1731–68.
Pfeffer MA, McMurray JJ. Lessons in uncertainty and humility—clinical trials involving hypertension. N Engl J Med. 2016;375:1756–66.
Conen D, Ridker PM, Buring JE, Glynn RJ. Risk of cardiovascular events among women with high normal blood pressure or blood pressure progression: prospective cohort study. BMJ. 2007;335:432.
Ference BA, Bhatt DL, Catapano AL, Packard CJ, Graham I, Kaptoge S, et al. Association of genetic variants related to combined exposure to lower low-density lipoproteins and lower systolic blood pressure with lifetime risk of cardiovascular disease. JAMA. 2019.
Luo D, Cheng Y, Zhang H, Ba M, Chen P, Li H, et al. Association between high blood pressure and long term cardiovascular events in young adults: systematic review and meta-analysis. BMJ. 2020;370:m3222.
Sheppard JP, Stevens S, Stevens R, Martin U, Mant J, Hobbs FDR, et al. Benefits and harms of antihypertensive treatment in low-risk patients with mild hypertension. JAMA Intern Med. 2018;178:1626–34.
Gosse P, Promax H, Durandet P, Clementy J. ‘White coat’ hypertension. No harm for the heart. Hypertension. 1993;22:766–70.
Gosse P, Dauphinot V, Roche F, Pichot V, Celle S, Barthelemy JC. Prevalence of clinical and ambulatory hypertension in a population of 65-year-olds: the PROOF study. J Clin Hypertens. 2010;12:160–5.
Thomopoulos C, Parati G, Zanchetti A. Effects of blood pressure lowering on outcome incidence in hypertension: 3. Effects in patients at different levels of cardiovascular risk-overview and meta-analyses of randomized trials. J Hypertens. 2014;32:2305–14.
Zanchetti A. Bottom blood pressure or bottom cardiovascular risk? How far can cardiovascular risk be reduced? J Hypertens. 2009;27:1509–20.
Asayama K, Satoh M, Murakami Y, Ohkubo T, Nagasawa SY, Tsuji I, et al. Cardiovascular risk with and without antihypertensive drug treatment in the Japanese general population: participant-level meta-analysis. Hypertension. 2014;63:1189–97.
Chowdhury EK, Nelson MR, Wing LMH, Jennings GLR, Beilin LJ, Reid CM, et al. Change in blood pressure variability among treated elderly hypertensive patients and its association with mortality. J Am Heart Assoc. 2019;8:e012630.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Gosse, P., Doublet, J., Gaudissard, J. et al. Long-term evolution of ambulatory blood pressure and cardiovascular events in hypertensive patients. J Hum Hypertens 36, 517–523 (2022). https://doi.org/10.1038/s41371-021-00538-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-021-00538-z
This article is cited by
-
Non-dipping blood pressure pattern is associated with cardiovascular events in a 21-year follow-up study
Journal of Human Hypertension (2024)