Abstract
The field of regenerative medicine continues to make substantial advancements in therapeutic strategies addressing urologic diseases. Tissue engineering borrows principles from the fields of cell biology, materials science, transplantation and engineering in an effort to repair or replace damaged tissues. This review is intended to provide a current overview of the use of stem cells and tissue engineering technologies specifically in the treatment of genitourinary diseases. Current themes in the field include the use of adult stem cells seeded onto biocompatible resorbable matrices for implantation as tissue substitutes, which is conducive to host tissue in-growth. Injection therapy of adult stem cells for organ rehabilitation is also making strong headway toward the restoration of organ structure and function. With new data describing the molecular mechanisms for differentiation, work has begun on targeting tissues for regeneration by genetic modification methods. Promising laboratory discoveries portend the emergence of a new class of clinical therapies for regenerative medicine applications in the genitourinary tract.
Similar content being viewed by others
Main
The field of tissue engineering (TE) has evolved substantially over the past four decades into an international area of science that is being investigated in virtually every country in the world. Early advances in the field were the result of groundbreaking discoveries of the pioneers in the regenerative medicine field including Joseph and Charles Vacanti, Robert Langer, and Eugene Bell. In fact, it was Joseph and Charles Vacanti who first used the term “Tissue Engineering” (1). They eloquently described the interplay required by cells, scaffolds, and added growth factors in the microenvironment of mechanotransducing bioreactors to develop cellular constructs that could ultimately serve as functional tissues suitable for transplantation. The field of TE has exponentially grown in size such that it now claims its own international academic society, Tissue Engineering Regenerative Medicine International Society, which the expanding community of scientists and physicians in the field have steadfastly supported (1–4). As of today, the principles of TE are being applied widely to create new tissue constructs in virtually every organ system.
In general, the field of TE combines the principles of cell biology, materials science, and engineering to devise therapeutic strategies in various acquired and congenital diseases (5–7). From a clinical perspective, the goal of regenerative medicine efforts is to restore end organ function, either by native tissue rehabilitation, or by development of functional reproducible tissue substitutes with minimal immunogenicity and which resemble native tissues in biologic and mechanical properties.
When autologous tissue is lacking, other possible sources of tissue include homologous tissues from cadavers or donors, heterologous tissues from animals (bovine), and synthetic materials (silicone, polyurethane, Teflon, poly(lactic acid), poly(glycolic acid), and poly(lactic-co-glycolic acid)), which are often referred to as alloplastic materials. The use of allogeneic tissues, such as with organ transplantation, can be limited by the need for tissue matching, donor organ availability, and lifelong immunosuppression. On the other hand, biocompatible and structurally similar alloplastic materials can be used for prosthetics and other clinical devices. However, functional recovery to the caliber of the original tissue is seldom achieved. TE offers the potential to circumvent many of these difficulties.
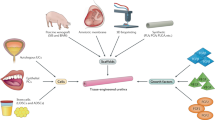
TE approaches can be classified into two categories: acellular and cellular techniques. Acellular techniques entail the use of acellular matrices as a scaffold for organ regeneration, requiring the host organ to incorporate new tissue onto the scaffold with proper layering and orientation. Collagen-rich matrices can be completely synthesized in the laboratory for subsequent cellular in-growth. These matrices slowly degrade and eventually are replaced by host extracellular matrix invested with in-growing cells. Scaffolds can also be harvested from other autologous, allogeneic, or xenogenic tissues, and then processed by chemical and mechanical means to remove cellular components for eventual implantation (8–10).
Common cellular techniques employ the use of donor cells, which are processed before implantation. These cells can be directly injected into the host, or expanded and processed in culture, seeded onto a support matrix or scaffold, and then implanted into the recipient. Tissue or cell sources can vary from autologous, allogenic (same species, different individual), or heterologous (such as bovine), with the most preferred source being autologous so as to eliminate the risk of rejection and associated complications of immunosuppression. For autologous sources, a tissue sample can be obtained from the patient by biopsy (10–15). Improvements in culture techniques have enabled the isolation of individual cell types from these tissue biopsies, which are then selectively expanded to amounts sufficient for implantation (6,9,16,17). Similar to acellular techniques, the scaffold material must be biocompatible, bioresorbable, and illicit minimal immunogenicity while expanded cellular components integrate into the local environment. These scaffold structures may be seeded or impregnated with growth factors and other cell signaling peptides to regulate cell activity and mimic the microenvironment provided by the extracellular matrix. Ideal scaffolds should also provide the appropriate three-dimensional lattice where cell-adhesion may occur while performing the mechanical functions of the damaged tissues. Thus, the final steps of the regenerative process occur in vivo (18–20).
Over the past two decades, research in TE techniques and stem cell tissue sources has led to potentially viable replacements for a variety of genitourinary tissues including ureter, bladder, prostate, urethra, external urinary sphinctor, and penile structures.
STEM CELLS
Many current strategies for TE rely on the presence of autologous tissue samples from which specific cells types can be isolated, expanded, and seeded onto a matrix for subsequent reimplantation. However, in instances of severe end organ failure or neoplasia, retrieval of normal cells is often problematic. The ability of stem cells to expand and differentiate into desired tissue types makes them an attractive alternative cell source for regenerative medicine applications. Novel therapeutic strategies are emerging and utilize stem cells as the primary cellular component of various TE constructs.
Stem cells are defined by their ability to self-renew and differentiate into a variety of cellular types. They are further classified by the breadth of cell lineages to which they may potentially differentiate (21). Summarization of the established classification of stem cells and their corresponding lineage potential has been well described. Briefly, cells derived from the zygote have the greatest differentiation potential and are classified as totipotent, capable of forming cells of ectoderm, mesoderm, endoderm, and gonadal ridge lineage. Embryonic stem cells and embryonic germ cells are isolated from the inner cell mass of the blastocyst and primordial germ cells respectively, and they give rise to all three germ layers and cells of the gonadal ridge, respectively. However, they do not give rise to extraembryonic tissues and thus are termed pluripotent. Multipotent stem cells are harvested from developing germ layers or their respective adult organs and are capable of self-renewal and differentiation into organ-specific cell types. Unipotent cells are progenitor cells with limited or no capacity for self-renewal (22).
Human embryonic stem cells (hESC) isolated by immunosurgery from the inner cell mass of a developing embryo can be maintained in cell culture in an undifferentiated state for a prolonged period of time using various published protocols (23,24). Their pluripotency is highlighted by their ability to form embryoid bodies in vitro, which are cell aggregations that contain all three germ layers. Clinical applications using these cells is challenging due to their propensity to form teratomas in vivo (24,25).
The harvest of hESC requires the destruction of human embryos and has raised significant ethical and political concerns. In August 2001, the United States federal government ordered that only previously generated human embryonic stem cell lines could be used in research supported by federal funding. Although over 70 existing cell lines met this criteria, the National Institutes of Health reported that only 11 were available, most of which were grown on mouse feeder cells and were at one point in time potentially exposed to murine viruses or proteins (26). These barriers to the development of hESC technologies have prompted the search for alternative stem cell sources including fetal tissues, parthenogenesis, amniotic fluid-derived stem cells, somatic cell nuclear transfer, and adult multipotent stem cells. These are briefly mentioned below, and extensive discussion on these topics can be found elsewhere (27–35).
Multipotent stem cells are harvested from adult organs or developing tissues, thus avoiding any controversy surrounding hESC. They can be extracted from many different tissues including bone marrow, striated muscle, fat, skin, testicle, and synovial membrane. Adult-derived stem cells are gaining popularity as researchers are finding a more extensive differentiation potential than previously thought and were frequently used in the studies below (29–31).
In addition, several multipotent or pluripotent stem cell populations derived from fetal tissues have been shown to produce a number of lineages including bone marrow, hepatic, and neural tissues. Fetal mesenchymal stem cells do not express human leukocyte antigen class II antigens and are thought to exist in a preimmune state. Both differentiated and undifferentiated fetal mesenchymal stem cells do not illicit reactive lymphocyte proliferation, making them ideal for allogeneic transplant or mismatch situations (32). In addition, stem cells isolated from amniotic fluid have exhibited pluripotency to all three germ layers and possess the ability to self-replicate despite a large number of passages (33). Procurement of these cells is through amniocentesis and obviates the need for destruction of human embryos. With the ease of procurement and published protocols for maintenance and directed differentiation, amniotic fluid stem cells have the potential to become a major source of stem cells for therapeutic applications (34,35).
GENITOURINARY APPLICATIONS OF STEM CELLS AND TE
Ureter.
Multiple conditions can affect the tenuous blood supply of the ureter or otherwise damage the delicate structure leading to significant stricture disease. These include penetrating trauma, impacted ureteral stones, retroperitoneal fibrosis, and iatrogenic injury. Surgical replacement of long segments of ureter (>2 cm) requires complex reconstructive procedures sometimes requiring intestinal interposition. A number of researchers have attempted to treat these conditions using engineering scaffolds to allow the expansion of local progenitor populations. Smith et al. (36) engineered allogeneic grafts using porcine small intestine submucosa (SIS) and applied these in an onlay manner to 2 cm porcine ureter defects comprising half of the circumference of the ureter. Renal function was grossly preserved as seen on i.v. urography, and histologic analysis showed reconstitution of normal ureteral architecture including muscle layers. In another animal study, Dahms et al. (37) performed a segmental replacement (<1 cm) of rat ureter using acellular matrix of tubularized collagen. Although these studies have produced promising results, there have been no successful reports of complete replacement of larger ureteral segments with engineered grafts. Canine experiments by Osman et al. (38) proved unsuccessful in the application of allogeneic acellular tube grafts to 3 cm complete ureteral defects. El-Hakim et al. attempted ureteral segment substitution using bladder urothelial cells expanded in culture and seeded onto three different types of matrices: autologous SIS, harvested xenogenic ureteral acellular matrix, and autologous deepithelialized small bowel reimplanted in a retubularized (4 cm Monti) configuration. These efforts proved unsatisfactory except in the last group which demonstrated preserved renal function without evidence of obstruction; however, histologic examination revealed regeneration of small bowel mucosa rather than seeded urothelial cells (39). Other studies have shown successful seeding of acellular xenogenic and allogeneic tubular scaffolds with stratified urothelium (40), but successful reimplantation and reestablishment of structure and native peristaltic function have yet to be achieved.
Bladder.
High pressure neurogenic bladders as seen in association with myelomeningocele or spinal cord injury may require bladder augmentation using intestinal segments to achieve adequate capacity and low pressure storage. Use of intestinal segments can lead to complications of urolithiasis, metabolic disturbances, excessive mucous production, and malignant disease. Much work has been done in creating tissue engineered bladder substitutes to potentially avoid the metabolic and neoplastic complications. A variety of regenerative medicine techniques to create bladder wall substitutes have been examined. Acellular substitutes from decellularized scaffolds have been obtained from a variety of tissue sources including xenogenic and allogeneic SIS and bladder (41–43). One study showed successful regeneration of mouse bladder by implanting decellularized bladder matrix scaffold impregnated with fibroblast growth factor (44). The most noteworthy study to date used tissue engineered bladder wall substitutes in seven patients with neurogenic bladder. Autologous urothelial and smooth muscle cells were obtained through open biopsy, expanded in vitro and then seeded onto artificial matrices before implantation (45). Although the authors noted changes in technique over the course of the study, four patients showed improved compliance and increased capacity. This study demonstrated the feasibility of using engineered tissue substitutes for partial hollow organ replacement in humans, obviating the need for intestinal substitution. A multi-institutional Food and Drug Administration-approved Phase 2 clinical trial is currently underway.
Stem cell research has also played a major role in developing bladder substitutes. With muscle invasive transitional cell carcinoma or severe persistent hemorrhagic cystitis, where cystectomy and urinary diversion are indicated, tissue biopsy for in vitro expansion may not be indicated, feasible, or of low yield. The use of stem cells as a primary nonimmunogenic tissue source for seeding of decellularized scaffolds is being heavily investigated. Successful directed differentiation of human embryoid body-derived stem cells into bladder urothelium has been reported, using coculture of stem cells with bladder mesenchyme to provide the adequate stimulatory effects of mesenchymal inductive cofactors (42). Co-culture of these stem cells with mesenchymal tissue and subsequent seeding on decellularized xenogenic SIS has been described to successfully form composite grafts. Although the function of these grafts was not tested in vivo, these studies demonstrate the feasibility of generating stem cell-derived bladder substitutes (41).
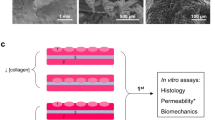
Korossis et al. (46) further addressed functionality in engineered bladder substitutes and intuitively suggested in vitro exposure of tissue constructs to mechanical transduction that mimic in vivo conditions. They noted the addition of mechanical dimensions to culture conditions enhanced micro- and macroscopic structural development and overall mechanical properties of engineered non-bladder tissues. These findings are extrapolated as beneficial to in vitro development of bladder substitutes. Incorporation of mechanical transduction in bioreactors has been described for other engineered tissues; however, these principles have yet to be applied to stem cell tissue sources for the purposes of creating bladder substitutes (47,48).
Prostate.
Replacement of diseased prostatic tissue may not be a clinically relevant topic, though the prevalence of prostatic disease and paucity of animal models has sparked an interest in alternative research techniques. A recent study described in vivo directed differentiation of hESC into prostatic tissue using tissue recombination techniques. They created heterospecific tissue recombinants with hESC and rat and murine urogenital sinus mesenchyme, and then reimplanted these into the renal cortex of immunodeficient mice. They were able to achieve glandular differentiation, verified with production of prostate specific antigen. Controls grown without mesenchyme produced teratomas (49). Aboseif et al. (50) performed similar studies using tissue recombinants from rat seminal vesical mesencyhme and adult human bladder epithelium. These chimeric constructs were also implanted into the subcapsular space of immunodeficient mice kidneys. They demonstrated the development of glandular structures in the epithelium, exhibiting the inductive effects of mesenchyme on epithelial tissues (50). A large body of work for TE of the prostate has grown from the need for animal models to test novel cancer and surgical therapies (51,52). Other stem cell studies in the prostate focus on discerning the biologic characteristics of prostate cancer.
Urethra.
Hypospadias, traumatic urethral defects, and stricture disease are traditionally addressed by means of local or distant epithelial flaps and grafts. Various genital and extragenital tissues have been used for urethral reconstruction, including foreskin, tunica vaginalis, buccal and bladder mucosa, and peritoneum (53,54). These techniques have not always produced satisfactory functional and structural replacement of urothelium, and they rely on the availability of healthy donor tissues. TE techniques are used to provide a plentiful source of healthy tissue for reconstructive purposes. Using similar techniques as those developed for ureters, acellular collagen-based matrices have been applied successfully as onlay patch grafts (10). Multiple investigators have described the use of acellular matrices for reconstruction, but this technique has only shown success when used as patch or onlay grafts, since acellular matrices fashioned into tubularized constructs led to recurrent stricture formation. However, tubularized acellular collagen matrices seeded with cells expanded in culture have repeatedly been successful in animal studies. These studies describe decellularized porcine or rabbit bladder submucosa seeded with xenogenic transitional cells or autologous skin cells expanded in vitro (54,55). Bach proposed an elegant variation in scaffold technique, where an autologous scaffold was created by implanting silicone tubing into rat subcutaneous tissue, and then harvested the fibrous capsule that developed around the tubing. This scaffold was seeded with cultured urothelial cells suspended in fibrin glue, which they have reported to be a reliable vehicle for transplantation of cultured cells (56).
El-Kassaby et al. (57) describe the use of an allogeneic collagen-based matrix derived from cadaver bladder submucosa during urethroplasty for stricture disease. The matrix was applied in an onlay fashion to the urethral plate and resulted in successful urethral reconstruction in 24 of 28 patients. All 24 had improved uroflowmetry and urethral caliber at a mean follow-up of 37 months and did not require any additional procedures. These investigators reported a similar technique several years prior with successful outcome in 3 of 4 patients, though with limited follow-up (58).
Incontinence.
The prevalence of urinary incontinence has been estimated at 13–20% in men and 5–60% in women (59,60).
Surgical procedures for stress urinary incontinence (SUI) seek to improve the coaptation pressure of the urethra-sphincter complex by means of injectable bulking agents (e.g., collagen), mechanical sphincters, urethral slings, and more recently with cell injection therapy. There is an increasing body of work investigating the potential for autologous myoblast and stem cell therapies for rhabdosphincter regeneration. The most impressive study to date was published by Strasser et al. (61), who conducted a randomized controlled trial comparing ultrasound-guided transurethral rhabdosphincter injection of autologous myo-and fibroblasts vs. transurethral collagen injection for SUI in women. They reported an incontinence cure rate of 90% in their cell injection group, compared with only 10% of the collagen treated group. They showed improvement in urinary incontinence, rhabdosphincter thickness and contractility (assessed by ultrasound), and quality of life scores on a prevalidated questionnaire instrument. The same investigators achieved near identical treatment results in a later group of 20 female patients accrued after the original trial (62). Another group of patients that included 42 women and 21 men with SUI also underwent autologous myoblasts injections, which included men who previously underwent radical prostatectomy or brachytherapy for prostate cancer. They reported a successful cure rate in 39 of 42 women (92.9%) and 11 of 21 men (52.4%) treated with injected myo- and fibroblasts at a follow-up of 12 mo. This study demonstrates the feasibility of this endoscopic injection therapy for men with SUI after local therapy for prostate cancer (63). The authors noted the importance of endoscopic ultrasound as a reliable method to guide precise delivery of injection therapy and subsequent objective evaluation of the rhabdosphincter. In addition, the clinical efficacy demonstrated through a randomized control trial represents an appropriate level of sophistication that should be applied to clinical trials whenever possible in evaluating stem cell and TE technology.
Lecoeur et al. (64) attempted de novo porcine sphincter generation via implantation of labeled autologous myofibers containing muscle precursor cells obtained from neck muscle biopsy. Rhabdosphincter injury was induced by endoscopic electrocautery, followed by implantation of myofibers both longitudinally along the urethra, and focally away from the native sphincter applied in a circumferential orientation, functionally generating a new sphincter in vivo. This cluster of circularly oriented muscle fibers exhibited reproducible contractions adequate to establish recordable urethral peak pressure on urodynamic evaluation 30 d after implantation. Suppression of tonic activity by curare suggests neural innervation of this sphincter complex. Histologic evaluation verified resulting nerve fiber development in the vicinity of the implanted myotubules, and neural tissue was present in greater density than surrounding tissue. Both these points suggest concomitant neuronal development and innervation of the transplanted myofibers.
Autograft, allograft, xenograft, and synthetic materials are all options for suburethral slings. Like any tissue substitute, each has its own inherent advantages and disadvantages. Tissue-engineered slings have been successfully created and implanted into rats with sciatic nerve injury. They were shown to maintain measurable leak point pressures in contrast to controls that were also denervated but did not undergo a sling procedure. The tissue-engineered slings were composed of SIS seeded with muscle-derived cells, and this construct did not show any significant difference in leak point pressure compared with sling material made of SIS alone. Despite this, the study showed the feasibility of applying slings to a reproducible sciatic nerve injury rat model and demonstration of leak point pressure measurements (65).
Penis.
Disease processes of the penis include ambiguous genitalia requiring penile reconstruction, trauma, erectile dysfunction, and Peyronie's disease. The field of TE is making significant strides in the development of potential treatments for these various structural disorders of the phallus, many of which have inadequate current therapies. Peyronie's disease is a condition of the penis that results in plastic induration and marked curvature with erections. It is usually associated with the presence of an inflammatory reaction and fibrotic plaque in the tunica albuginea. The prevelance is estimated at 0.4–23% of men (66). There are several published reports describing use of fascial, venous, and synthetic grafts to repair defects in tunica albuginea in the setting of penile trauma or treatment of Peyronie's disease (67–70). In clinical studies, Breyer et al. (71) reported a complication rate higher than expected in patients who underwent tunica grafting with SIS (Surgisis®) after plaque incision or excision for Peyronie's disease. At a mean follow-up of 15 months in 19 patients, complications included penile shortening (63%), pain (26%), infection (5%), and hematoma formation (26%) at the graft site that required ultrasound guided aspiration. There were no significant differences regarding erectile dysfunction pre- and postoperatively as determined on a previously published erectile dysfunction diagnostic questionnaire tool (72). More recent animal studies describe the successful creation of tissue-engineered corporal grafts paving the way for future replacement strategies. Joo et al. (70) reported successful grafting of decellularized porcine bladder submucosa onto rabbit corpora. Histologic analysis verified tissue integration without excessive scarring or contracture 2 month following surgery.
Of particular interest are descriptions of engineered replacements for damaged erectile tissues within the corporal bodies. Falke et al. describe a novel technique to generate human cavernosal muscle and endothelial cells in vivo. Processed acellular rabbit corpora seeded with human corpus cavernosa muscle and endothelial cells were implanted in mice and subsequently generated well vascularized corporal tissues (73). Although functional studies have not been performed, the preliminary studies appear promising.
Multiple investigators have attempted interposition of autologous nerve grafts during radical prostatectomy for cancer in an attempt at preservation of erectile function. Clinical trials using sural nerve interposition have shown only limited success (74–76). More recently, May et al. published an extensive review examining the use of neurotrophic bioartificial scaffolds for regeneration of cavernous nerves following local injury from trauma or radical prostatectomy. These collagen based nerve scaffolds were seeded with autologous Schwann cells and interposed in large nerve defects. These authors included their own animal studies, which showed the return of erectile function in rats grafted with bioartificial nerve scaffolds after cavernous nerve ablation. These seeded scaffolds were shown to be superior to both interposed autologous nerve graft interposition and unseeded silicone nerve conduits (77).
Additional studies in erectile dysfunction have examined gene therapy applications to enhance endothelial vasodilatation of the corporal bodies, ultimately upregulating erectile response. Induced mutation in several target genes has been described to upregulate the production of nitric oxide and other vasodilatory proteins (78). Deng et al. has reported successful animal studies in intracavernosal injection therapy of genetically engineered stem cells for the treatment of erectile dysfunction. In a series of experiments, this group demonstrated in vivo directed protein upregulation using intracavernosal injection of viral vehicles carrying selected mutant genes for transfection. They suggested in vitro transfection of mesenchymal stem cells with subsequent cell injection as therapy for corporal dysfunction. Histologic evaluation verified the increased tissue concentration of targeted proteins and the morphologic verification of incorporated stem cells, which remained within the corpora up to 3 week postinjection. Another recent report using stem cell injection therapy of corpora cavernosa has also demonstrated in vivo differentiation of these cells into corporal tissue (79).
CONCLUSION
The fields of TE and stem cell research continue to search for novel techniques of tissue replacement and rehabilitation in the genitourinary tract. In identifying possible replacements for current treatment strategies, recent studies have included randomized controlled trials for cell injection therapy, and animal studies utilizing genetically enhanced stem cells that render metabolically programmed tissue substitutes. The latter shows great promise for attaining directed cellular function and protein upregulation, and is a new application of stem cell gene therapy.
The use of adult stem cells, specifically autologous progenitor cells obtained from biopsy, appears to have sufficient clinical utility for in vitro expansion and autologous tissue generation, thus avoiding the controversies surrounding the use of hESCs.
Abbreviations
- hESC:
-
human embryonic stem cells
- NIH:
-
National Institutes of Health
- SIS:
-
small intestine submucosa
- SUI:
-
stress urinary incontinence
- TE:
-
tissue engineering
References
Langer R, Vacanti JP 1993 Tissue engineering. Science 260: 920–926
Vacanti CA 2006 The history of tissue engineering. J Cell Mol Med 10: 569–576
Vacanti JP 2007 Tissue engineering: a 20 year personal perspective [editorial]. Tissue Eng 13: 231–232
Atala A, Nyberg LM 2000 Tissue engineering. World J Urol 18: 1
Mikos AG, Herring SW, Ochareon P, Elisseeff J, Lu HH, Kandel R, Schoen FJ, Toner M, Mooney D, Atala A, Van Dyke ME, Kaplan D, Vunjak-Novakovic G 2006 Engineering complex tissues. Tissue Eng 12: 3307–3339
Atala A 2006 Recent developments in tissue engineering and regenerative medicine. Curr Opin Pediatr 18: 167–171
Park H, Cannizzaro C, Vunjak-Navokavic G, Langer R, Vacanti CA, Farokhzad OC 2007 Nanofabrication and microfabrication of functional materials for tissue engineering. Tissue Eng 13: 1867–1877
Brehmer B, Rohrmann D, Becker C, Rau G, Jakse G 2007 Different types of scaffolds for reconstruction of the urinary tract by tissue engineering. Urol Int 78: 23–29
Sievert KD, Amend B, Stenzl A 2007 Tissue engineering for the lower urinary tract: a review of a state of the art approach. Eur Urol 52: 1580–1589
Chen F, Yoo JJ, Atala A 1999 Acellular collagen matrix as a possible “off the shelf” biomaterial for urethral repair. Urology 54: 407–410
Atala A 1999 Future perspective in reconstructive surgery using tissue engineering. Urol Clin North Am 26: 157–165
Atala A, Freeman MR, Vacanti JP, Shepard J, Retik AB 1993 Implantation in vivo and retrieval of artificial structures consisting of rabbit and human urothelium and human bladder muscle. J Urol 150: 608–612
Godbey WT, Atala A 2002 In vitro systems for tissue engineering. Ann N Y Acad Sci 961: 10–26
Dahms SE, Piechota HJ, Dahiya R, Lue TF, Tanagho EA 1998 Composition and biomechanical properties of the bladder acellular matrix graft: comparative analysis in rat, pig and human. Br J Urol 82: 411–419
Piechota HJ, Dahms SE, Nunes LS, Dahiya R, Lue TF, Tanagho EA 1998 In vitro functional properties of the rat bladder regenerated by the bladder acellular matrix graft. J Urol 159: 1717–1724
Atala A 2004 Tissue engineering for the replacement of organ function in the genitourinary system. Am J Transplant 4: 58–73
David R, Groebner M, Franz WM 2005 Magnetic cell sorting purification of differentiated embryonic stem cells stably expressing truncated human CD4 as surface marker. Stem Cells 23: 477–482
Hynes RO 1992 Integrins: versatility, modulation, and signaling in cell adhesion. Cell 69: 11–25
Deuel TF 1997 Growth factors. In: Lanza RP, Langer R, Chick WL (eds) Principles of Tissue Engineering. Academic Press, New York, pp 133–149
Kim BS, Mooney DJ 1998 Development of biocompatible synthetic extracellular matrices for tissue engineering. Trends Biotechnol 16: 224–230
Keller G 2005 Embryonic stem cell differentiation: emergence of a new era in biology and medicine. Genes Dev 19: 1129–1155
Becker C, Gerhard J 2007 Stem cells for regeneration of urological structures. Eur Urol 51: 1217–1228
Thomson JA, Itskovitz-Eldor J, Shapiro SS, Waknitz MA, Swiergiel JJ, Marshall VS, Jones JM 1998 Embryonic stem cell lines derived from human blastocysts. Science 282: 1145–1147
Reubinoff BE, Pera MF, Fong CY, Trounson A, Bongso A 2000 Embryonic stem cell lines from human blastocysts: somatic differentiation in vitro. Nat Biotechnol 18: 399–404
Itskovitz-Eldor J, Schuldiner M, Karsenti D, Eden A, Yanuka O, Amit M, Soreq H, Benvenisty N 2000 Differentiation of human embryonic stem cells into embryoid bodies comprising the three embryonic germ layers. Mol Med 6: 88–95
Kennedy D 2003 Stem cells: still here, still waiting. Science 300: 865
Marchant J 2006 Human eggs supply ‘ethical' stem cells. Nature 441: 1038
Atala A, Koh CJ 2004 Tissue engineering applications of therapeutic cloning. Annu Rev Biomed Eng 6: 27–40
Vrana KE, Hipp JD, Goss AM, McCool BA, Riddle DR, Walker SJ, Wettstein PJ, Studer LP, Tabar V, Cunnuff K, Chapman K, Vilner L, West MD, Grant KA, Cibelli JB 2003 Nonhuman primate parthenogenetic stem cells. Proc Natl Acad Sci USA 100: 11911–11916
Peterson BE, Bowen WC, Patrene Mars WM, Sullivan AK, Murase N, Boggs SS, Greenberger JS, Goff JP 1999 Bone marrow as a potential source of hepatic oval cells. Science 284: 1168–1170
Fierabracci A, Caione P, Di Giovine M, Zavaglia D, Bottazzo GF 2007 Identification and characterization of adult stem/progenitor cells in the human bladder (bladder spheroids): perspectives in application in pediatric surgery. Pediatr Surg Int 23: 837–839
Chung SY, Koh CJ 2007 Fetal tissues. In: Atala A, Lanza R, Nerem R, Thomson JA (eds) Principles of Regenerative Medicine. Academic Press, Burlington, MA, pp 968–977
De Coppi P, Bartsch G Jr, Siddiqui MM, Xu T, Santos CC, Perin L, Mostoslavsky G, Serre AC, Snyder EY, Yoo JJ, Furth ME, Soker S, Atala A 2007 Isolation of amniotic stem cells lines with potential for therapy. Nat Biotechnol 25: 100–106
In't Anker PS, Scherjon SA, Kleijburg-van der Keur C, Noort WA, Claas FH, Willemze R, Fibbe WE, Kanhai HH 2003 Amniotic fluid as a novel source of mesenchymal stem cells for therapeutic transplantation. Blood 102: 1548–1549
Tsai MS, Hwang SM, Tsai YL, Cheng FC, Lee JL, Chang YJ 2006 Clonal amniotic fluid-derived stem cells express characteristics of both mesenchymal and neural stem cells. Biol Reprod 74: 545–551
Smith TG III, Gettman M, Lindberg G, Napper C, Pearle MS, Cadeddu JA 2002 Ureteral replacement using porcine small intestine submucosa in a porcine model. Urology 60: 931–934
Dahms SE, Piechota HJ, Nunes L, Dahiya R, Lue TF, Tanagho EA 1997 Free ureteral replacement in rats: regeneration of ureteral wall components in the acellular matrix graft. Urology 50: 818–825
Osman Y, Shokeir A, Gabr M, El-Tabey N, Mohsen T, El-Baz M 2004 Canine ureteral replacement with long acellular matrix tube: is it clinically applicable?. J Urol 172: 1151–1154
El-Hakim A, Marcovish R, Chiu K-Y, Lee BR, Smith AD 2005 Ureteral segmental replacement revisited. J Endourol 19: 1069–1074
Matsunuma H, Kagami H, Narita Y, Hata K-I, Ono Y, Ohshima S, Ueda M 2006 Constructing a tissue engineered ureter using decellularized matrix with cultured uroepithelial cells and bone marrow-derived mononuclear cells. Tissue Eng 12: 509–518
Lakshmanan Y, Fromberger D, Hearhart JD, Gearhart JP 2005 Human embryoid body-derived stem cells in co-culture with bladder smooth muscle and urothelium. Urology 65: 821–826
Frimberger D, Morales N, Shamblott M, Gearhart JD, Gearhart JP, Lakshmanan Y 2005 Human embryoid body-derived stem cells in bladder regeneration using rodent model. Urology 65: 827–832
Obara T, Matsura S, Narita S, Satoh S, Tsuchiya N, Habuchi T 2006 Bladder acellular matrix grafting regenerates urinary bladder in the spinal cord injury rat. Urology 68: 892–897
Kanematsu A, Yamamoto S, Noguchi T, Ozeki M, Tabata Y, Ogawa O 2003 Bladder regeneration by bladder acellular matrix combined with sustained release of exogenous growth factor. J Urol 170: 1633–1638
Atala A, Bauer SB, Soker S, Yoo JJ, Retik AB 2006 Tissue-engineered autologous bladders for patients needing cystoplasty. Lancet 367: 1241–1246
Korossis S, Bolland F, Ingham E, Fisher J, Kearney J, Southgate J 2006 Tissue engineering of the urinary bladder: considering structure-function relationships and the role of mechanotransduction. Tissue Eng 12: 635–644
Sodian R, Lemke T, Fritsche C, Hoerstrup SP, Fu P, Potapov EV, Hausmann H, Hetzer R 2002 Tissue-engineering bioreactors: a new combined cell seeding and perfusion system for vascular tissue engineering. Tissue Eng 8: 863–870
Kim B-S, Nikolovski J, Bonadio J, Mooney DJ 1999 Cyclic mechanical strain regulates development of engineered smooth muscle tissue. Nat Biotechnol 17: 979–983
Taylor RA, Cowin PA, Cunha GR, Pera M, Trounson AO, Pederson J, Risbridger GP 2006 Formation of human prostate tissue from embryonic stem cells. Nat Methods 3: 179–181
Aboseif S, El-Sakka A, Young P, Cunha G 1999 Mesenchymal reprogramming of adult human epithelial differentiation. Differentiation 65: 113–118
O'connor KC 1999 Three-dimensional cultures of prostatic cells: tissue models for the development of novel anti-cancer therapies. Pharm Res 16: 486–493
Han B, Grassl ED, Barocas VH, Coad JE, Bischof JC 2005 A cryoinjury model using engineered tissue equivalents for cryosurgical applications. Ann Biomed Eng 33: 972–982
Fu Q, Deng C-L 2006 Ten year experience with composite bladder mucosa-skin grafts in hypospadias repair. Urology 67: 1274–1277
De Filippo RE, Yoo JJ, Atala A 2002 Urethral replacement using cell seeded tubularized collagen matrices. J Urol 168: 1789–1792; discussion 1792–1793.
Fu Q, Deng CL, Liu W, Cao YL 2007 Urethral replacement using epidermal cell-seeded tubular acellular bladder collagen matrix. BJU Int 99: 1162–1165
Bach AD, Bannasch H, Galla TJ, Bittner KM, Stark GB 2001 Fibrin glue as matrix for cultured autologous urothelial cells in urethral reconstruction. Tissue Eng 7: 45–54
El-Kassaby AW, Retik AB, You JJ, Atala A 2003 Urethral stricture repair with an off-the-shelf collagen matrix. J Urol 169: 170–173
Atala A, Guzman L, Retik AB 1999 A novel inert collagen matrix for hypospadias repair. J Urol 162: 1148–1151
Nygaard I, Thom DH, Calhoun E 2007 Urinary incontinence in women. In: Litwin MS, Saigal CS (eds) Urologic Diseases in America. NIH/NIDDK Publication No. 07-5512, Bethesda, MD, pp 157–191.
Stothers L, Thom DH, Calhoun E 2007 Urinary incontinence in men. In: Litwin MS, Saigal CS (eds) Urologic Diseases in America. NIH/NIDDK Publication No. 07-5512, Bethesda, MD, pp 193–222
Strasser H, Marksteiner R, Margreiter E, Pinggera GM, Mitterberger M, Frauscher F, Ulmer H, Fussenegger M, Kofler K, Bartsch G 2007 Autologous myoblasts and fibroblasts versus collagen for treatment of stress urinary incontinence in women: a randomized controlled trial. Lancet 369: 2179–2186
Mitterberger M, Pinggera GM, Marksteiner R, Margreiter E, Fussenegger M, Frauscher F, Ulmer H, Hering S, Bartsch G, Strasser H 2008 Adult stem cell therapy of female stress urinary incontinence. Eur Urol 53: 169–175
Strasser H, Marksteiner R, Margreiter E, Mitterberger M, Pinggera GM, Frauscher F, Fussenegger M, Kofler K, Bartsch G 2007 Transurethral ultrasonography-guided injection of adult autologous stem cell versus transurethral endoscopic injection of collagen in treatment of urinary incontinence. World J Urol 25: 385–392
Lecoeur C, Swieb S, Zini L, Riviere C, Combrisson H, Gherardi R, Abbou C, Yiou R 2007 Intraurethral transfer of satellite cells by myofiber implants results in the formation of innervated myotubes exerting tonic contractions. J Urol 178: 332–337
Cannon TW, Sweeney DD, Conway DA, Kamo I, Yoshimura N, Sacks M, Chancellor MB 2005 A tissue-engineered suburethral sling in an animal model of stress urinary incontinence. BJU Int 96: 664–669
Wessells H, Joyce GF, Wise M, Wilt TJ 2007 Erectile dysfunction and Peyronie's disease. In: Litwin MS, Saigal CS (eds) Urologic Diseases in America. Bethesda, MD, NIH/NIDDK Publication No. 07-5512, pp 483–530.
Gelbard MK, Hayden B 1991 Expanding contractures of the tunica albuginea due to Peyronies's disease with temporalis fascia free grafts. J Urol 145: 772–776
Leungwattanakij S, Tiewthanom V, Hellstrom WJ 2003 Evaluation of corporal fibrosis in cadaveric pericardium and vein grafts for tunica albuginea substitution in rats. Asian J Androl 5: 295–299
Seftel AD, Oates RD, Goldstein I 1992 Use of polytetraflouroethylene tube graft as a circumferential neotunica during replacement of a penile prosthesis. J Urol 148: 1531–1533
Joo KJ, Kim B-S, Han J-H, Kim C-J, Kwon C-H, Park H-J 2006 Porcine vesical acellular matrix graft of tunica albuginea for penile reconstruction. Asian J Androl 8: 543–548
Breyer BN, Brant WO, Garcia MM, Bella AJ, Lue TF 2007 Complications of porcine small intestine submucosa graft for Peyronie's Disease. J Urol 177: 589–591
Rosen RC, Cappelleri JC, Smith MD, Lipsky J, Pena BM 1999 Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Int J Impot Res 11: 319–326
Falke G, Yoo JJ, Kwon TG, Moreland R, Atala A 2003 Formation of corporal tissue architecture in vivo using human cavernosal muscle and endothelial cells seeded on collagen matrices. Tissue Eng 9: 871–879
Walsh PC 2001 Nerve grafts are rarely necessary and unlikely to improve sexual function in men undergoing anatomic radical prostatectomy. Urology 57: 1020–1024
Kim ED, Nath R, Slawin KM, Kadmin D, Miles BJ, Scardino TS 2001 Bilateral nerve grafting during radical retropubic prostatectomy; extended follow-up. Urology 58: 983–987
Scardino PT, Kim ED 2001 Rationale for and results of nerve grafting during radical prostatectomy. Urology 57: 1016–1019
May F, Vroemen M, Matiasek K, Henke J, Brill T, Lehmer A, Apprich M, Erhardt W, Schoeler S, Paul R, Blesch A, Hartung R, Gansbacher B, Weidner N 2005 Nerve replacement strategies for cavernous nerves. Eur Urol 48: 372–378
Deng W, Bivalacqua TJ, Hellstrom WJ, Kadowitz PJ 2005 Gene and stem cell therapy for erectile dysfunction. Int J Impot Res 17: S57–S63
Song YS, Lee HJ, Park IH, Kim WK, Ku JH, Kim SU 2007 Potential differentiation of human mesenchymal stem cell transplanted in rat corpus cavernosum toward endothelial or smooth muscle cells. Int J Impot Res 19: 378–385
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yamzon, J., Kokorowski, P. & Koh, C. Stem Cells and Tissue Engineering Applications of the Genitourinary Tract. Pediatr Res 63, 472–477 (2008). https://doi.org/10.1203/PDR.0b013e31816a704a
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31816a704a
This article is cited by
-
Novel therapeutic approaches of tissue engineering in male infertility
Cell and Tissue Research (2020)
-
A novel kartogenin-platelet-rich plasma gel enhances chondrogenesis of bone marrow mesenchymal stem cells in vitro and promotes wounded meniscus healing in vivo
Stem Cell Research & Therapy (2019)
-
Biomaterial Scaffolds for Reproductive Tissue Engineering
Annals of Biomedical Engineering (2017)
-
Stem cells: novel players in the treatment of erectile dysfunction
Asian Journal of Andrology (2012)