Abstract
Heterozygous SFTPC mutations have been associated with adult and pediatric interstitial lung disease (pILD). Inheritance is autosomal dominant, but de novo mutations may cause sporadic disease. SFTPC mutations have been associated with variable onset of symptoms, ranging from early infancy to late adulthood. The underlying mechanisms for this variability are unknown. Recently, mutations in ABCA3 (encoding member A3 of the adenosine triphosphate–binding cassette family of transporters) were identified as a cause of pILD. To test the hypothesis that ABCA3 mutations modify the severity of lung disease in individuals with SFTPC mutations, we sequenced ABCA3 from four symptomatic infants with the same SFTPC mutation, a substitution of isoleucine by threonine in codon 73 (I73T). Each infant developed respiratory symptoms by 2 mo of age and inherited the mutation from an asymptomatic parent. Three of the four infants were also heterozygous for an ABCA3 mutation, which was inherited from the parent without SFTPC I73T. The finding of heterozygosity for ABCA3 mutations in severely affected infants with SFTPC I73T, and independent inheritance from disease-free parents supports that ABCA3 acts as a modifier gene for the phenotype associated with an SFTPC mutation.
Similar content being viewed by others
Main
Pulmonary surfactant is a mixture of lipids and specific proteins that reduces surface tension at the air-liquid interface and prevents end-expiratory atelectasis. Lack of surfactant is the primary cause of respiratory distress syndrome (RDS) in infants born prematurely. Although surfactant phospholipids are primarily responsible for lowering surface tension, two small hydrophobic proteins, surfactant proteins B and C (SP-B and SP-C), have key roles in regulating surfactant function and metabolism (1). SP-C deficiency and mutations in the SP-C gene (SFTPC) have been associated with both sporadic interstitial lung disease (ILD) due to de novo mutations and familial ILD inherited as autosomal dominant (2–10). One particular SFTPC mutation, a substitution of threonine (T) for isoleucine (I) in codon 73 (I73T) has been identified in multiple unrelated families (9–11). The age at onset and severity of lung disease due to SFTPC I73T as well as other SFTPC mutations is highly variable, ranging from death in early infancy to development of pulmonary fibrosis in the fifth or sixth decade (7, 9–12). SP-C deficiency in knockout mouse models results in lung disease depending on genetic background (13,14). The variability in mouse and human lung disease suggests that SFTPC-associated lung disease may be influenced by environmental factors and/or modifier genes.
A candidate gene that may modify SFTPC-related lung disease is the ATP-binding cassette A3 (ABCA3) gene. ABCA3 encodes a 1704-amino acid protein that is highly expressed in the lung and has been localized to the limiting membrane of lamellar bodies in alveolar type II cells (15–18). Recent studies support that ABCA3 transports lipids into lamellar bodies, the storage organelle for surfactant within alveolar type II cells and is required for the formation of normal lamellar bodies (19–21). Autosomal recessive ABCA3 deficiency results in fatal neonatal RDS (22), whereas some ABCA3 mutations, also inherited in autosomal recessive fashion, are associated with ILD and prolonged survival (23). The lung histopathology in children with the milder phenotype is similar to that observed in children with SFTPC mutations. We hypothesized that ABCA3 genetic variants modify the pulmonary phenotype of some SFTPC mutations.
METHODS
Patients.
From June 1993 through December 2005, DNA samples were obtained from 325 children with chronic lung disease of unknown etiology as part of a study to identify genetic defects in surfactant metabolism. The entry criteria included the following: (1) gestational age of 36 wk or older and age 30 d or older or discharged from the neonatal intensive care unit or gestational age younger than 36 wk and age older than 3 mo or discharge from the neonatal intensive care unit and (2) indications of parenchymal lung disease as manifested by two of three of the following factors: need for supplemental oxygen; clinical signs of lung disease, including cough, tachypnea, retractions, or rales; and abnormal chest radiograph. Infants younger than 30 d were eligible for enrollment if there was a family history of lung disease. A history of neonatal lung disease was not a requirement for inclusion. The children were referred by their primary providers. The review boards of the participating institutions approved the protocols for these evaluations, and written consent for genetic testing was obtained from the families. Patients were not excluded based on sex or race/ethnicity. Fifty-six percent was male, 43% female, and 1% unknown. The distribution of samples by racial/ethnic background was 218 (67%) white (non-Hispanic), 23 (7%) African American, 41 (12.5%) Hispanic, 15 (4.5%) Asian, 6 (1.8%) other, and 17 (5.2%) unknown.
DNA preparation and mutational analysis.
Genomic DNA was prepared from blood leukocytes with use of a commercially available kit (Gentra Systems, Minneapolis, MN). Polymerase chain reaction (PCR) products spanning exons 1 and 2 (genomic positions, –143 to 996) and exons 3 to 6 (genomic positions, 1212 to 2522) of the SFTPC gene were generated from genomic DNA by PCR and analyzed by direct sequencing of the PCR products with the use of previously described conditions (24). The 30 coding exons of the ABCA3 gene and their respective splice junction sites were amplified by previously published conditions and primer sets (23). Automated DNA sequencing was performed through the Johns Hopkins School of Medicine's genetic resources core DNA sequencing facility using Applied Biosystems 3730 DNA Analyzer (Applied Biosystems). DNA sequencing chromatograms were analyzed with the aid of Sequencher 4.2 software (Gene Codes Corporation, Ann Arbor, MI). The resulting ABCA3 and SFTPC sequences were compared with reference sequences (15,25).
Restriction digest analysis.
The restriction endonuclease BsrGI was purchased from New England Biolabs (Beverly, MA) and used according to manufacturer's specifications for analysis of ABCA3 E292V, as reported previously (23).
RESULTS
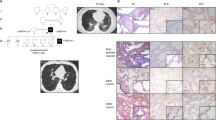
Of the 325 children enrolled in the study, 55 (17%) were found to have an SFTPC mutation identified as the probable cause of their lung disease. SFTPC I73T was the most commonly identified mutation, found in 19 children, which comprised 35% of the mutant SFTPC alleles. Seven of the 19 children were the subject of an earlier report, including one who was a compound heterozygote for SFTPC I73T and SFTPC L110R (10). ABCA3 E292V was assayed for in the 19 children because of its association with multiple unrelated children and lung disease (23). Two infants were identified with ABCA3 E292V and had the onset of their symptoms at younger than 2 mo of age. Each parent did not have any respiratory symptoms, and DNA samples were available from both parents for analysis (Fig. 1). Two additional infants were discordant in their respiratory symptoms from their parents and also had available DNA from the both of their parents (Table 1). The 30 coding exons of ABCA3 were sequenced from these four children. Sequencing confirmed that patients 1 and 2 had the ABCA3 E292V mutation and no other mutation. Patient 3 was heterozygous for a missense mutation in exon 8, a substitution of methionine for leucine at codon 212, L212M. Patient 4 did not have any mutations identified. Analysis of parental DNA of three children who were heterozygous for both SFTPC I73T, and an ABCA3 mutation demonstrated that the ABCA3 mutation was inherited from the opposite parent who had SFTPC I73T (Fig. 2).
Pedigrees of patients with SFTPC I73T evaluated for ABCA3 mutations. Index cases identified by arrows with age at enrollment and onset of symptoms noted below symbol. Age of parents and symptomatic family members are noted below symbol. Circle, female; square, male; shaded quarter symbol, SFTPC I73T; solid quarter symbol, ABCA3 E292V; checkered quarter symbol, ABCA3 L212M; slash through symbol, deceased; IPF, idiopathic pulmonary fibrosis; RSV, respiratory syncytial virus.
DISCUSSION
There are many examples of monogenic disorders whose phenotype is influenced by modifier genes, such as polymorphisms that affect the expression of fetal Hb in sickle cell disease (26). We chose ABCA3 as a candidate modifier gene for the lung disease due to SFTPC mutations because of its involvement in surfactant metabolism and the similarities in the lung pathology findings in children with ABCA3 mutations to those with SFTPC-related lung disease. To test this hypothesis, we selected families with the most severe pulmonary phenotypic discordance, each with an affected infant whose respiratory symptoms began at younger than 2 mo of age and an asymptomatic parent with SFTPC I73T. We focused on families with SFTPC I73T, as it is the most frequently reported SFTPC mutation associated with lung disease, (9–12) and to minimize effects on disease severity due to different SFTPC mutations. Three of four infants were also heterozygous for an ABCA3 mutation, supporting a role for ABCA3 in modifying lung disease due to SFTPC mutations.
Two of the four infants had ABCA3 E292V, a mutation that has been associated with pILD (23). The population frequency of ABCA3 E292V is low, approximately one in 275 individuals (personal communication, T. Garmany and A. Hamvas). Thus, the finding of ABCA3 E292V in two of the 19 patients with SFTPC I73T seems unlikely to have occurred by chance. The third infant had a different missense mutation, ABCA3 L212M, which results in a conservative neutral substitution. It is possible that L212M represents a rare but benign polymorphism. However, two siblings with significant respiratory symptoms and who had lung histopathology findings consistent with surfactant dysfunction were compound heterozygotes for a previously identified ABCA3 nonsense mutation (R106X) and L212M, suggesting that L212M is a disease-causing mutation (L.M. Nogee, unpublished data). No ABCA3 mutation was identified in the fourth infant. Other genetic modifiers or other critical environmental exposures may have contributed to the severity of lung disease, in particular a respiratory syncytial virus infection at 2 mo of age. A history of viral infections was noted in symptomatic young infants in a large kindred with familial ILD due to SFTPC L188Q (7). In addition, RSV infection of cells in culture that expressed a low level of a SFTPC mutation identified in patients with ILD that skips exon 4 (SFTPC Δexon4) resulted in cell death, indicating a possible interaction of low levels of expression of abnormal SP-C with viral infections (27).
The pathophysiology of SFTPC-related lung disease is complex, and the mechanisms whereby ABCA3 mutations modify the lung disease due to SFTPC mutations are unknown. SFTPC mutations may cause SP-C deficiency by a dominant negative mechanism. Mature SP-C is derived from a larger proprotein (proSP-C) that self-associates in the secretory pathway (28). ProSP-C containing mutations may be targeted for degradation (29). Thus, abnormal SP-C may also cause wild-type SP-C to be degraded, leading to SP-C deficiency. Decreased or absent SP-C has been observed in some patients with SFTPC mutations (3,24,30). As ABCA3 deficiency alters surfactant homeostasis, including abnormal processing and routing of SP-C (31) and hindering lamellar body biogenesis (19), decreased functional ABCA3 activity in patients with SFTPC mutations may result in more severe symptoms of surfactant deficiency. We did not perform expression studies to directly assess the effects of the ABCA3 mutations observed in these patients.
Lung disease due to SFTPC mutations may result from a toxic gain-of-function mechanism of abnormal proSP-C. Increased proSP-C expression may overwhelm the protein degradation pathway leading to abnormal accumulations of proSP-C containing mutations. Perinuclear accumulations of mutated proSP-C have been observed in vitro (32,33) and in explanted lung tissue from a patient with an SFTPC mutation (6). These accumulations of abnormal protein may result in the unfolded protein response, cytotoxicity, and eventual apoptotic death (5,34). Expression of SFTPC Δexon4 in transgenic mice disrupted lung development that correlated with the degree of transgene expression, further supporting the potential toxicity of abnormal proSP-C (29). Altered surfactant homeostasis with abnormal processing and routing of SP-C due to decreased ABCA3 function (31) may thus exacerbate the accumulation of inappropriately processed SP-C, leading to more cell injury and death. Both loss-of-function and toxic gain-of-function mechanisms may be involved in the development of SFTPC-related lung disease at different points in time.
The relative contribution of ABCA3 to SFTPC-related lung disease is unknown. Our study was not population based with enrolled infants identified by their primary physicians based on the unusual nature of their lung disease, and we selected those infants for whom we had parental DNA and whom knew had variable severity of lung disease. There is thus a significant ascertainment bias that limits interpretation of the frequency of ABCA3 as a gene that modifies some SFTPC mutations.
In summary, the finding that three infants with severe lung disease and SFTPC I73T were also heterozygous for ABCA3 mutations, in contrast to their asymptomatic parents from whom they inherited the SFTPC mutation, supports the hypothesis that ABCA3 mutations modify the severity of lung disease associated with SFTPC mutations. Studies of the effects of SFTPC mutations in combination with ABCA3 mutations both in vitro and ultimately in animal models will be needed to confirm this hypothesis. We speculate that ABCA3 genetic variants may also contribute to the development and progression of other common diseases in the general population, such as asthma or bronchopulmonary dysplasia.
Abbreviations
- ABCA3:
-
adenosine triphosphate–binding cassette protein group A3 gene
- pILD:
-
pediatric interstitial lung disease
- SFTPC:
-
surfactant protein C gene
References
Weaver TE, Conkright JJ 2001 Function of surfactant proteins B and C. Annu Rev Physiol 63: 555–578
Tredano M, Griese M, Brasch F, Schumacher S, de Blic J, Marque S, Houdayer C, Elion J, Couderc R, Bahuau M 2004 Mutation of SFTPC in infantile pulmonary alveolar proteinosis with or without fibrosing lung disease. Am J Med Genet A 126: 18–26
Nogee LM, Dunbar AE 3rd, Wert SE, Askin F, Hamvas A, Whitsett JA 2001 A mutation in the surfactant protein C gene associated with familial interstitial lung disease. N Engl J Med 344: 573–579
Amin RS, Wert SE, Baughman RP, Tomashefski JF Jr, Nogee LM, Brody AS, Hull WM, Whitsett JA 2001 Surfactant protein deficiency in familial interstitial lung disease. J Pediatr 139: 85–92
Beers MF, Mulugeta S 2005 Surfactant protein C biosynthesis and its emerging role in conformational lung disease. Annu Rev Physiol 67: 663–696
Hamvas A, Nogee LM, White FV, Schuler P, Hackett BP, Huddleston CB, Mendeloff EN, Hsu FF, Wert SE, Gonzales LW, Beers MF, Ballard PL 2004 Progressive lung disease and surfactant dysfunction with a deletion in surfactant protein C gene. Am J Respir Cell Mol Biol 30: 771–776
Thomas AQ, Lane K, Phillips J 3rd, Prince M, Markin C, Speer M, Schwartz DA, Gaddipati R, Marney A, Johnson J, Roberts R, Haines J, Stahlman M, Loyd JE 2002 Heterozygosity for a surfactant protein C gene mutation associated with usual interstitial pneumonitis and cellular nonspecific interstitial pneumonitis in one kindred. Am J Respir Crit Care Med 165: 1322–1328
Stevens PA, Pettenazzo A, Brasch F, Mulugeta S, Baritussio A, Ochs M, Morrison L, Russo SJ, Beers MF 2005 Nonspecific interstitial pneumonia, alveolar proteinosis, and abnormal proprotein trafficking resulting from a spontaneous mutation in the surfactant protein C gene. Pediatr Res 57: 89–98
Lawson WE, Grant SW, Ambrosini V, Womble KE, Dawson EP, Lane KB, Markin C, Renzoni E, Lympany P, Thomas AQ, Roldan J, Scott TA, Blackwell TS, Phillips JA 3rd, Loyd JE, du Bois RM 2004 Genetic mutations in surfactant protein C are a rare cause of sporadic cases of IPF. Thorax 59: 977–980
Cameron HS, Somaschini M, Carrera P, Hamvas A, Whitsett JA, Wert SE, Deutsch G, Nogee LM 2005 A common mutation in the surfactant protein C gene associated with lung disease. J Pediatr 146: 370–375
Brasch F, Griese M, Tredano M, Johnen G, Ochs M, Rieger C, Mulugeta S, Muller KM, Bahuau M, Beers MF 2004 Interstitial lung disease in a baby with a de novo mutation in the SFTPC gene. Eur Respir J 24: 30–39
Percopo S, Cameron HS, Nogee LM, Pettinato G, Montella S, Santamaria F 2004 Variable phenotype associated with SP-C gene mutations: fatal case with the I73T mutation. Eur Respir J 24: 1072–1073
Glasser SW, Burhans MS, Korfhagen TR, Na CL, Sly PD, Ross GF, Ikegami M, Whitsett JA 2001 Altered stability of pulmonary surfactant in SP-C-deficient mice. Proc Natl Acad Sci U S A 98: 6366–6371
Glasser SW, Detmer EA, Ikegami M, Na CL, Stahlman MT, Whitsett JA 2003 Pneumonitis and emphysema in sp-C gene targeted mice. J Biol Chem 278: 14291–14298
Connors TD, Van Raay TJ, Petry LR, Klinger KW, Landes GM, Burn TC 1997 The cloning of a human ABC gene (ABC3) mapping to chromosome 16p13.3. Genomics 39: 231–234
Yamano G, Funahashi H, Kawanami O, Zhao LX, Ban N, Uchida Y, Morohoshi T, Ogawa J, Shioda S, Inagaki N 2001 ABCA3 is a lamellar body membrane protein in human lung alveolar type II cells. FEBS Lett 508: 221–225
Mulugeta S, Gray JM, Notarfrancesco KL, Gonzales LW, Koval M, Feinstein SI, Ballard PL, Fisher AB, Shuman H 2002 Identification of LBM180, a lamellar body limiting membrane protein of alveolar type II cells, as the ABC transporter protein ABCA3. J Biol Chem 277: 22147–22155
Zen K, Notarfrancesco K, Oorschot V, Slot JW, Fisher AB, Shuman H 1998 Generation and characterization of monoclonal antibodies to alveolar type II cell lamellar body membrane. Am J Physiol 275: L172–L183
Cheong N, Madesh M, Gonzales LW, Zhao M, Yu K, Ballard PL, Shuman H 2006 Functional and trafficking defects in ATP binding cassette A3 mutants associated with respiratory distress syndrome. J Biol Chem 281: 9791–9800
Nagata K, Yamamoto A, Ban N, Tanaka AR, Matsuo M, Kioka N, Inagaki N, Ueda K 2004 Human ABCA3, a product of a responsible gene for abca3 for fatal surfactant deficiency in newborns, exhibits unique ATP hydrolysis activity and generates intracellular multilamellar vesicles. Biochem Biophys Res Commun 324: 262–268
Garmany TH, Moxley MA, White FV, Dean M, Hull WM, Whitsett JA, Nogee LM, Hamvas A 2006 Surfactant composition and function in patients with ABCA3 mutations. Pediatr Res 59: 801–805
Shulenin S, Nogee LM, Annilo T, Wert SE, Whitsett JA, Dean M 2004 ABCA3 gene mutations in newborns with fatal surfactant deficiency. N Engl J Med 350: 1296–1303
Bullard JE, Wert SE, Whitsett JA, Dean M, Nogee LM 2005 ABCA3 mutations associated with pediatric interstitial lung disease. Am J Respir Crit Care Med 172: 1026–1031
Nogee LM, Dunbar AE 3rd, Wert S, Askin F, Hamvas A, Whitsett JA 2002 Mutations in the surfactant protein C gene associated with interstitial lung disease. Chest 121: 20S–21S
Warr RG, Hawgood S, Buckley DI, Crisp TM, Schilling J, Benson BJ, Ballard PL, Clements JA, White RT 1987 Low molecular weight human pulmonary surfactant protein (SP5): isolation, characterization, and cDNA and amino acid sequences. Proc Natl Acad Sci U S A 84: 7915–7919
Chui DH, Dover GJ 2001 Sickle cell disease: no longer a single gene disorder. Curr Opin Pediatr 13: 22–27
Bridges JP, Xu Y, Na CL, Wong HR, Weaver TE 2006 Adaptation and increased susceptibility to infection associated with constitutive expression of misfolded SP-C. J Cell Biol 172: 395–407
Conkright JJ, Bridges JP, Na CL, Voorhout WF, Trapnell B, Glasser SW, Weaver TE 2001 Secretion of surfactant protein C, an integral membrane protein, requires the N-terminal propeptide. J Biol Chem 276: 14658–14664
Bridges JP, Wert SE, Nogee LM, Weaver TE 2003 Expression of a human surfactant protein C mutation associated with interstitial lung disease disrupts lung development in transgenic mice. J Biol Chem 278: 52739–52746
Nogee LM 2002 Abnormal expression of surfactant protein C and lung disease. Am J Respir Cell Mol Biol 26: 641–644
Brasch F, Schimanski S, Muhlfeld C, Barlage S, Langmann T, Aslanidis C, Boettcher A, Dada A, Schroten H, Mildenberger E, Prueter E, Ballmann M, Ochs M, Johnen G, Griese M, Schmitz G 2006 Alteration of the pulmonary surfactant system in full-term infants with hereditary ABCA3 deficiency. Am J Respir Crit Care Med 174: 571–580
Beers MF, Lomax CA, Russo SJ 1998 Synthetic processing of surfactant protein C by alveolar epithelial cells. The COOH terminus of proSP-C is required for post-translational targeting and proteolysis. J Biol Chem 273: 15287–15293
Kabore AF, Wang WJ, Russo SJ, Beers MF 2001 Biosynthesis of surfactant protein C: characterization of aggresome formation by EGFP chimeras containing propeptide mutants lacking conserved cysteine residues. J Cell Sci 114: 293–302
Mulugeta S, Nguyen V, Russo SJ, Muniswamy M, Beers MF 2005 A surfactant protein C precursor protein BRICHOS domain mutation causes endoplasmic reticulum stress, proteasome dysfunction, and caspase 3 activation. Am J Respir Cell Mol Biol 32: 521–530
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the National Institutes of Health (HL-54703 to L.M.N.) and the Eudowood Foundation.
Rights and permissions
About this article
Cite this article
Bullard, J., Nogee, L. Heterozygosity for ABCA3 Mutations Modifies the Severity of Lung Disease Associated with a Surfactant Protein C Gene (SFTPC) Mutation. Pediatr Res 62, 176–179 (2007). https://doi.org/10.1203/PDR.0b013e3180a72588
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3180a72588
This article is cited by
-
Correlating SFTPC gene variants to interstitial lung disease in Egyptian children
Journal of Genetic Engineering and Biotechnology (2022)
-
Child Interstitial Lung Disease in an Infant with Surfactant Protein C Dysfunction due to c.202G>T Variant (p.V68F)
Lung (2022)
-
Surfactant protein disorders in childhood interstitial lung disease
European Journal of Pediatrics (2021)
-
Clinical and genetic spectrum of interstitial lung disease in Chinese children associated with surfactant protein C mutations
Italian Journal of Pediatrics (2019)
-
The biology of the ABCA3 lipid transporter in lung health and disease
Cell and Tissue Research (2017)