Abstract
Brain slices from 7-d-old Wistar rats were exposed to oxygen-glucose deprivation (OGD) for 30 min. OGD slices were incubated with vehicle or with the CB1/CB2 cannabinoid agonist WIN55212 (50 μM), the CB1 agonist arachidonyl-2-chloroethylamide (ACEA) (50 μM), or the CB2 agonist JW133 (50 μM), alone or combined with the CB1 and CB2 receptor antagonist SR 141716 (50 μM) or SR 144528 (50 μM), respectively. Neuronal damage was assessed by histologic analysis and spectrophotometric determination of lactate dehydrogenase (LDH) efflux into the incubation medium. Additionally, medium glutamate levels were determined by high-performance liquid chromatography (HPLC) and those of tumor necrosis factor α (TNF-α) by enzyme-linked immunosorbent assay. Finally, inducible nitric oxide synthase (iNOS) and CB1/CB2 receptor expression were determined in slices homogenate by Western blot. Both CB1 and CB2 receptors were expressed in slices. OGD increased CB1 expression, cellular damage, LDH efflux, glutamate and TNF-α release, and inducible nitric oxide synthase (iNOS) expression; WIN55212 inhibited all these actions. SR141716 and SR144528 inhibited the effect of R(+)-WIN-55212-2 (WIN), as well as the reduction of LDH efflux by ACEA and JW133, respectively. In conclusion, WIN55212 afforded robust neuroprotection in the forebrain slices exposed to OGD, by acting on glutamatergic excitotoxicity, TNF-α release, and iNOS expression; this neuroprotective effect seemed to be mediated by CB1 and CB2 receptors.
Similar content being viewed by others
Main
Perinatal hypoxia-ischemia remains the single most important cause of brain injury in the newborn, leading to death or lifelong sequelae (1,2). The complexities of neonatal hypoxic-ischemic encephalopathy (NHIE) pathophysiology suggest that successful neuroprotection could be achieved only with a multitherapeutic approach (2). In recent years, interest in the neuroprotective possibilities of cannabinoids has grown (3–5). Endocannabinoids emerge as natural brain protective substances in different damaging situations (3,4); in newborn rats, enhanced levels of cannabinoids have been observed in the brain after acute excitotoxic insult (6). Exogenous cannabinoid agonists are neuroprotective in different paradigms of brain injury (7,8); they inhibit intracellular calcium influx, reduce glutamate and TNF-α release, decrease stimulated iNOS expression, induce hypothermia, and exert immunomodulatory and antioxidant actions (3–5,9,10). Some of these effects are dependent on the activation of the principal brain cannabinoid receptors, the CB1 receptors, and others are dependent on the molecular properties of the cannabinoid or the activation of non-CB1 receptors (3). There are few studies regarding the possible neuroprotective effect of cannabinoids in newborns. Early studies describe that the administration of anandamide (11) or the cannabinoid agonist Δ (9)-tetrahydrocannabinol (12) affords neuroprotection in a newborn rat model with excitotoxic neuronal injury. It has also been demonstrated that the cannabinoid agonist WIN, prevents early neuronal death by CB1-independent mechanisms, and prevents late neuronal death by CB1-dependent mechanisms in a model of acute asphyxia in newborn rats (13).
In our study, we investigated the mechanisms involved in the prevention of early hypoxic-ischemic neuronal death in the newborn rat brain using WIN. This involved an in vitro model using the exposure of newborn rat brain slices to OGD. This reproduces most the mechanisms of hypoxic-ischemic damage in the newborn brain, as glutamatergic excitotoxicity, cytokine release, or NO toxicity, with characteristics different from those of adult rat brain slice OGD; it is therefore considered an in vitro model of NHIE (14).
METHODS
Preparation and incubation of slices.
The experimental protocol has been described elsewhere (14). Briefly, newborn Wistar rats (7–10 d old) were killed by decapitation (according to the Committee of Animal Care at the Universidad Complutense of Madrid), the forebrain was removed and coronally cut (1 mm anterior and 3 mm posterior to the bregma), and the central portion was sliced (0.5 mm slice thickness) using a Vibroslice (WPI, Stevenage, UK) into cold (12–14°C) modified Krebs-Henseleit solution (preincubation solution) containing (mM): NaCl (120), KCl (2), CaCl2 (0.5), NaHCO3 (26), MgSO4 (10), KH2PO4 (1.18), glucose (11), and sucrose (200). Slices were incubated in sucrose-free preincubation solution for 45 min and later in a modified Krebs-Henseleit solution (incubation solution) containing (mM): NaCl (120), KCl (2), CaCl2 (2), NaHCO3 (26), MgSO4 (1.19), KH2PO4 (1.18), glucose (11) and 5,6,7,8-tetrahydrobiopterin (BH4, 10 mM), bubbled with 95% O2/5% CO2 in a shaking water bath at 37°C.
The slices of the control group (CG, n = 28) were then incubated 30 min further in the same conditions, and slices of the “ischemic” experimental group (OGD, n = 30) were incubated for 30 min in incubation solution without glucose and equilibrated with 95% N2/5% CO2. In all groups, the end of the period of 30 min was considered as time 0 (t0). After these periods of 30 min, the medium was replaced with fresh incubation solution equilibrated with 95% O2/5% CO2 (“reperfusion” phase). Thereafter, the incubation solution was renewed every 30 min, up to and including 150 min (t150). Samples were taken each time the incubation solution was replaced, except the sample to determine TNF-α levels, which was collected once only at t150. At t150, slices were taken out and frozen immediately with liquid nitrogen.
Before starting to study the neuroprotective effect of WIN, tests were run using a concentration of WIN from 0.5 to 100 μM, to obtain the optimal drug concentration. Next, at this optimal concentration, WIN alone (WIN, n = 14), or with the CB1 receptor antagonist SR141716 (50 μM; SR1, n = 7), or the CB2 receptor antagonist SR144528 (50 μM, n = 8) was added to the preincubation solution, remaining present until the end of the experiment. In another set of experiments, the CB1-specific agonist arachidonyl-2-chloroethylamide (ACEA) (50 μM, n = 10), alone or with SR1 (50 μM, n = 8), or the CB2-specific agonist 1,1-dimethylbutyl-1-deoxy-Δ (9)-tetrahydrocannabinol (JWH133) (50 μM; JW, n = 10), alone or with SR2 (50 μM, n = 8) was added.
Histologic study.
At the end of the experiment, the brain slices were fixed overnight in 4% paraformaldehyde. They were then embedded in paraffin and cut into 3-μm sections using a microtome. Each section was stained using Nissl's technique and observed with a Nikon Eclipse 90i microscope with a Nikon Digital Camera DXM 1200F, coupled to computerized image-processing software (Metamorph 6.3r1, Molecular Devices Corp.). Digital microphotographs (×400) were taken from three different 500-μm2 areas of striatum using slices from at least three different specimens to count viable neurons with their nuclei present in the focal plane. Cell counting was performed by an investigator blinded to the experimental protocol.
LDH activity assay.
As a marker of necrotic tissue damage, LDH released from damaged cells in the slices was determined in the incubation solution, as previously described (14). LDH activity was measured spectrophotometrically at 340 nm by following the oxidation of NADH (decrease in absorbance) in the presence of pyruvate using a Thermomax microplate reader (Molecular Devices, Sunnyvale, CA). LDH efflux was expressed as the LDH activity present in the incubation solution. Data are expressed as mOD/min and reflect the total LDH release.
HPLC determination of glutamate concentration.
Samples of the incubation solution were collected at t0. Analysis of glutamate in each sample was performed by HPLC with fluorimetric detection (Perkin Elmer Binary LC Pump 250 and Fluorescence Detector LC 240) following precolumn derivatization with the o-phtalaldialdehyde procedure, as previously described (14). Glutamate derivatives were separated isocratically on a reverse phase column (4.6 × 150 mm, 5-mm particle diameter, Nucleosil 100-C18) using a mobile phase consisting of sodium acetate buffer (0.05 M, pH 6.5), 20% methanol and 2% tetrahydrofuran. The area of each peak was determined with a Perkin Elmer Nelson Model 1020 integrator (Phoenix 8088 ROM BIOS Version 2.52 software) and compared with the peak area of the corresponding external standard. The limit of detection in these conditions was 10 ng/mL.
Western blot analyses.
For analysis of iNOS, CB1, and CB2 expression, slices were homogenized in lysis buffer (10 mM Tris, pH 8.0; 0.2% Nonidet P-40;1 mM dithioerythritol); after centrifugation for 15 min, the proteins present in the supernatant were loaded (10 μg) and size-separated in 10% SDS-polyacrylamide gel electrophoresis (50 mA), as previously described (14). The gels were blotted onto a PVDF membrane (Millipore, Bedford, MA), incubated with specific polyclonal antibodies against iNOS (Santa Cruz Biotechnology, Santa Cruz, CA; 1:1000 dilution), CB1 and CB2 (Chemicon International Inc; both at a 1:300 dilution), and processed as recommended by the supplier. Proteins recognized by the antibodies were revealed by an ECL kit following the manufacturer's instructions (Amersham Iberica, Madrid, Spain). INOS, CB1, and CB2 expression was quantified by densitometric analysis of bands. Commercial markers (Bio-Rad prestained) were used as molecular weight standards, and β-actin was used to normalize the protein lane charge of the blot.
TNF-α determination.
Soluble TNF-α released from cells into the incubation solution was determined by a rat TNF-α immunoassay (Rat TNF-α UltraSensitive, Biosource International Inc., Camarillo, CA.
Chemicals and statistical analyses.
SR141716 and SR144528 were a generous gift from Sanofi-Synthelabo (Paris, France). BH4 was obtained from RBI, and, unless otherwise stated, the other chemicals were from Sigma Chemical Co. (Madrid, Spain).
Results are expressed as mean ± SEM of the indicated number of experiments. Statistical comparisons were made using analysis of variance (ANOVA), with the Newman-Keuls test for multiple comparisons. A p value <0.05 was considered as statistically significant. Statistical analysis was performed using the 11.0.0 version of SPSS software (SPSS Inc.).
RESULTS
Expression of the cannabinoid receptors CB1 and CB2.
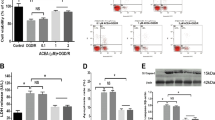
Western blot analysis at t150 demonstrated the presence of the CB1 and CB2 receptors in the CG. OGD induced a significant increase in CB1 expression but not an increase in CB2 expression (Fig. 1).
Determination of CB1 and CB2 expression in homogenates of the brain slices from 7-d-old rats, maintained in physiologic solution (CG), or after OGD. (A) Representative Western blot. (B) Quantification of CB1 (left columns) and CB2 (right columns) expression by densitometric analysis, expressed as a percentage of the optic density of the protein band in CG. Commercial markers (Bio-Rad prestained) were used as molecular weight standards. β-Actin was used to normalize the protein lane charge of the blot. Bars represent the mean ± SEM of five to seven experiments. *ANOVA, p < 0.05 vs CG.
Characterization of the effect of WIN on brain injury after OGD.
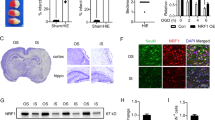
As observed after Nissl staining, OGD led to severe tissue damage, with a large reduction in the number of viable neurons (Fig. 2). Viable striatal neuron density was 348.4 ± 14.6 versus. 33.3 ± 2.8 per mm2 for CG and OGD, respectively. In CG, LDH efflux was minimal and remained stable throughout the 150-min experimental period; by contrast, OGD induced a significant increase in LDH efflux during the entire experimental period, as we have described previously (14) (Fig. 3). Prior incubation of OGD slices with WIN reduced LDH efflux in a dose-dependent manner (Fig. 3). A concentration of 50 μM was the most effective dose, reducing LDH efflux to levels similar to those in CG (Fig. 3). Higher concentration, however, further increased LDH efflux, suggesting some toxic effect (Fig. 3). Thus, a concentration of 50 μM was selected as the optimal WIN concentration for experiments. Based on its Ki values, similar concentration of ACEA and JW were selected after testing showed a higher concentration was not more effective.
Light micrographs of striatum neurons from coronal brain slices from 7-d-old rats after Nissl staining (original magnification, ×400), showing examples of a brain slice maintained in physiologic solution (CG) (A); a brain slice after OGD (B); a brain slice after OGD incubated with WIN55212 (50 μM) (C); a brain slice after OGD co-incubated with WIN + SR141716 (50 μM) (D); and a brain slice after OGD co-incubated with WIN + SR144528 (50 μM) (E). Scale bar: 100 μm.
Time profile of LDH efflux in brain slices from 7-d-old rats maintained in physiologic solution (CG, open circles), or after OGD without treatment (filled circles) or with WIN55212 (0.5 μM, filled triangles; 1 μM, open diamonds; 10 μM, filled diamonds; 50 μM, open squares; or 100 μM, filled squares). LDH efflux was quantified as LDH activity measured spectrophotometrically and expressed in mOD/min. Points represent the mean ± SEM of six to 10 experiments. *p < 0.05 vs control; †p < 0.05 vs OGD.
In addition to reducing LDH efflux, WIN increased the number of viable neurons observed under the microscope (264.1 ± 10.9 per mm2, p < 0.05 versus OGD) (Fig. 2). Co-incubation with either SR1 or SR2 inhibited both protective effects of WIN (Figs. 2 and 4A); neuronal density was 50.1 ± 2.3 and 59.5 ± 3.1 per mm2 for SR1 and SR2, respectively (p < 0.05 versus CG and WIN). Co-incubation of WIN with SR1 and SR2 together had no additional inhibiting effect (data not shown).
Time profile of LDH efflux in brain slices from 7-d-old rats, maintained in physiologic solution (CG, open circles) or after OGD without treatment (filled circles) or incubated with WIN55212 (50 μM; filled triangles), WIN + SR141716 (50 μM; filled diamonds), or WIN + SR144528 (50 μM; open squares) (A) or with WIN55212 (50 μM; filled triangles), ACEA (50 μM; open squares), or JW133 (50 μM; filled diamonds) (B). LDH efflux was quantified as LDH activity measured spectrophotometrically and expressed in mOD/min. Points represent the mean ± SEM of 12 to 30 experiments. *p < 0.05 vs control; †p < 0.05 vs OGD.
Incubation with ACEA or JW reduced LDH efflux, but to a lesser extent than with WIN (Fig. 4B). The effect was receptor specific, as SR1 reversed the effect of ACEA as did SR2 with JW (data not shown).
Effect of WIN on glutamate and TNF-α concentration and iNOS expression.
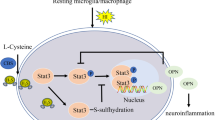
OGD induced a significant increase in glutamate concentration in the incubation medium (Fig. 5A). This increase was reduced by WIN to <50% of the OGD values (Fig. 5A). Co-incubation with SR1 or SR2 eliminated the WIN-induced reduction of glutamate concentration.
Measurements in the incubating medium of brain slices from 7-d-old rats maintained in physiologic solution (CG, n = 30) or after OGD without treatment (OGD) or with WIN55212 (50 μM; WIN), WIN + SR141716 (50 μM; W+SR1), or WIN + SR144528 (50 μM; W+SR2) of glutamate concentration, by HPLC at the end of OGD (A). TNF-α concentration, by enzyme-linked immunosorbent assay at the end of the experiment (B). Bars represent the mean ± SEM of seven to 30 experiments. *ANOVA, p < 0.05 vs CG; †ANOVA, p < 0.05 vs OGD; ‡ANOVA, p < 0.05 vs WIN.
When compared with CG, exposure to OGD caused a twofold increase in TNF-α concentration (Fig. 5B). WIN inhibited this increase in TNF-α, with concentrations lower than those found in CG. Co-incubation with SR1 or SR2 inhibited the TNF-α reduction by WIN.
In CG slice homogenate, a small expression of iNOS was detected by Western blot analysis (Fig. 6). In contrast, OGD caused a strong overexpression of iNOS (Fig. 4). This overexpression was attenuated by WIN (Fig. 6). This effect of WIN was counteracted by SR1 or SR2 co-incubation (Fig. 6).
Determination of iNOS expression in homogenates of brain slices from 7-d-old rats, maintained in physiologic solution (CG), or after OGD without treatment (OGD) or with WIN55212 (50 μM; WIN), WIN + SR141716 (50 μM; W+SR1), or WIN + SR144528 (50 μM; W+SR2). (A) Representative Western-Blot. (B) Quantification of iNOS expression by densitometric analysis, expressed as percentage of the optic density of the iNOS protein band in CG. Bars represent the mean ± SEM of five to seven experiments. *ANOVA, p < 0.05 vs CG.
DISCUSSION
We have demonstrated for the first time that (1) a cannabinoid agonist induced a robust neuroprotective effect in an in vitro model of NHIE; (2) this neuroprotective effect is related to the modulation of some relevant factors involved in hypoxic-ischemic brain damage; (3) CB2 receptors play a relevant role, offering interesting therapeutic options; and (4) the simultaneous activation of both CB1 and CB2 receptors offers more benefits than CB1 or CB2 activation alone.
The neuroprotective effects shown confirm those previously observed by us in an in vivo model of NHIE in rats (13) and offer cannabinoids as a promising strategy against acute neurodegeneration (3,4,7,8). The 50-μM dose of WIN used is higher than that commonly used in cell cultures (7) due to the thickness of the forebrain slices (500 μm). These required greater drug concentrations to achieve appropriate WIN concentration in the deepest layers of the slice. LDH efflux in brain slices incubated with 50 μM of WIN remained stable throughout the experiment and at levels similar to those of the CG, supporting the neuroprotective effect of WIN and also its lack of toxic effects. Our experiments have analyzed for the first time the effects of a cannabinoid on the activation of some critical factors that determine neuronal death in NHIE. These factors include glutamatergic excitotoxicity, TNF-α release, and iNOS expression (1,2). The immature brain is selectively vulnerable to glutamatergic excitotoxicity (1,14–16). WIN reduced glutamate concentration in the incubation medium when compared with untreated OGD brain slices alone. Drugs reducing glutamate release are of particular value in neuroprotection in NHIE, as glutamate receptor blockers are neurotoxic in immature brains (2). Cannabinoids are known to inhibit glutamate release by presynaptic G protein-coupled receptor activation (17–22).
WIN led to a decrease in TNF-α release. Great attention is paid to the role of TNF-α in NHIE because it is particularly harmful to the immature brain. It is involved in apoptotic and oxidative injury processes using different mechanisms, including iNOS induction (1,14,23,24). Cannabinoids inhibit the increase in TNF-α production after immunologic stimuli, both in vivo and in vitro (10) by modulating different transcriptional factors (25) and enhancing the release of the endogenous interleukin-1 receptor antagonist (IL-1ra) (26). In addition to this, cannabinoids reduce the release of glutamate, which in turn enhances TNF-α release by activation of its secretase, TNF-α convertase (TACE/ADAM17) (27). Interestingly, WIN reduced TNF-α concentrations to an even lower level than those of the CG, suggesting that some stimulation of TNF-α release derived from brain slice manipulation occurs, thus emphasizing the anti-inflammatory effect of cannabinoids (5,10,26).
Expression of iNOS was increased by OGD, as reported (14,28). Different mechanisms participate in iNOS induction during hypoxia, including TNF-α (23) or glutamate (28) release; massive production of NO after induction of iNOS plays a major role in hypoxic brain injury (1,16,29). The induction of iNOS after OGD was counteracted by WIN. Cannabinoids inhibit iNOS expression in glial cells after different stimuli (9,26,30) by enhancing IL-1ra release (26) and inhibiting the transcriptional activity of the nuclear factor-κB (NF-κB) (9,31). This effect on NF-κB activity is of particular importance because this is the mechanism by which glutamate induces the expression of iNOS (28).
Western blot revealed the presence of CB1 receptors in newborn rat brain slices and, for the first time, CB2 receptors. The neuroprotective effect of WIN was eliminated by SR1 and SR2, suggesting the participation of both CB1 and CB2 receptors in this effect. CB1 receptors are found in the brain during the early prenatal developmental stages, increasing in density soon after birth (32). CB1 was overexpressed 150 min after OGD, as observed 2 h after focal ischemia in the rat brain (33). This agrees with the suggested role of endocannabinoids as natural neuroprotectors after brain injuries (4,6). Our results suggesting the participation of CB1 receptors in WIN-induced neuroprotection are supported by LDH efflux reduction by ACEA and confirm previous results from ischemic brain injury experiments in mice (34). SR1 reversed the WIN-induced reduction of glutamate release. Although the role of CB1 in cannabinoid reduction of glutamate release in adult brain remains controversial (17–22), our results support a role for these receptors in cannabinoid prevention of excitotoxic damage in newborn brain, as reported (11,12). SR1 not only reversed the WIN-induced reduction of glutamate release, but increased OGD-induced glutamate release. Similar results were observed in cultured cerebellar neurons and have been interpreted as inverse agonism of SR1 or the block in activity of endogenous ligands at cannabinoid receptors (17). We also confirmed the involvement of CB1 receptors in WIN modulation of TNF-α release and iNOS expression enhancement, an effect thought to be exerted on glial cells (9,10).
Recently, CB2 receptors have been discovered in brain neurons (35) and microglial cells (36), both being present in the forebrain slices that we used. A striking result of our study was the elimination of WIN neuroprotection by SR2. JW, a selective CB2 agonist, was also equally capable of reducing LDH efflux. This is, to our knowledge, the first report of CB2 intermediation of cannabinoid neuroprotection in models of brain ischemia. CB2 receptors are overexpressed in glial cells in different paradigms of inflammatory brain insult (37,38); although inflammation plays a pivotal role in ischemic brain damage (24), we did not observe an increase in CB2 expression in OGD brain slices. It has been reported that in cultured cells, CB2 receptors participate in the reduction by cannabinoids, of lipolysaccharide-induced TNF-α release (10) and iNOS expression increase (26,30); ours is the first evidence of a CB2-mediated reduction of TNF-α release and iNOS expression in a model of hypoxic-ischemic brain damage. In addition, we have also described for the first time that CB2 participated in the reduction of glutamate release by WIN, involving them in the modulatory effect of cannabinoids on excitotoxic brain damage. Our results support the possibility of a cannabinoid-based therapeutic intervention, free from psychotropic effects, as CB2 receptors do not mediate the psychoactive effects of cannabinoids (39).
Interestingly, the neuroprotective effect of WIN, a CB1/CB2 agonist, was greater than that of selective CB1 or CB2 agonists. In fact, LDH efflux was similar in WIN+SR1 and JW, as well as in WIN+SR2 and ACEA. These data suggest that simultaneous activation of both CB1 and CB2 receptors was more effective in modulating the factors involved in hypoxic-ischemic brain damage than CB1 or CB2 alone. Studies on neuronal and glial cultures have shown that the neuroprotective action of cannabinoids in response to inflammatory or excitotoxic insults is mediated by both CB1 and CB2 receptor-dependent pathways (26). Co-incubation of WIN with SR1 and SR2 did not increase the inhibitory effect of SR1 or SR2 alone, suggesting that WIN might also act on receptor(s) other than CB1 and CB2 (21).
In conclusion, WIN showed a robust neuroprotective effect on 7-d-old rat forebrain slices exposed to OGD, based on the reduction of glutamate release, TNF-α release, and iNOS expression. The effect of WIN was mediated by both CB1 and CB2 receptors. Our results support a major role for cannabinoids in neuroprotective strategies, opening an exciting field of investigation in the role of CB2 receptors in NHIE pathophysiology and therapeutics.
Abbreviations
- iNOS:
-
inducible nitric oxide synthase
- LDH:
-
lactate dehydrogenase
- NHIE:
-
neonatal hypoxic-ischemic encephalopathy
- OGD:
-
oxygen-glucose deprivation
- WIN:
-
R(+)-WIN-55212-2
References
du Plessis AJ, Volpe JJ 2002 Perinatal brain injury in the preterm and term newborn. Curr Opin Neurol 15: 151–157
Hamrick SE, Ferriero DM 2003 The injury response in the term newborn brain: can we neuroprotect?. Curr Opin Neurol 16: 147–154
Grundy RI, Rabuffetti M, Beltramo M 2001 Cannabinoids and neuroprotection. Mol Neurobiol 24: 29–51
Mechoulam R, Panikashvili D, Shohami E 2002 Cannabinoids and brain injury: therapeutic implications. Trends Mol Med 8: 58–61
Howlett AC, Breivogel CS, Childers SR, Deadwyler SA, Hampson RE, Porrino LJ 2004 Cannabinoid physiology and pharmacology: 30 years of progress. Neuropharmacology 47: 345–358
Hansen HH, Schmid PC, Bittigau P, Lastres-Becker I, Barrendero F, Manzanares J, Ikonomidou C, Schmid HH, Fernández-Ruiz JJ, Hansen HH 2001 Anandamide, but not 2-arachidonylglycerol, accumulates during in vivo neurodegeneration. J Neurochem 78: 1415–1427
Nagayama T, Sinor AD, Simon RP, Chen J, Graham SH, Jin K, Greenberg DA 1999 Cannabinoids and neuroprotection in global and focal cerebral ischemia and in neuronal cultures. J Neurosci 19: 2987–2995
Sinor AD, Irvin SM, Greenberg DA 2000 Endocannabinoids protect cerebral cortical neurons from in vitro ischemia in rats. Neurosci Lett 278: 157–160
Waksman Y, Olson JM, Carlisle SJ, Cabral GA 1999 The central cannabinoid receptor (CB1) mediates inhibition of nitric oxide production by rat microglial cells. J Pharmacol Exp Ther 288: 1357–1366
Klein TW, Lane B, Newton CA, Friedman H 2000 The cannabinoid system and cytokine network. Proc Soc Exp Biol Med 225: 1–8
Van der Stelt M, Veldhuis WB, Van Haaften GW, Fezza F, Bisogno T, Bär PR, Veldink GA, Vliegenthart JF, Di Marzo V, Nicolay K 2001 Exogenous anandamide protects rat brain against acute neuronal injury in vivo. J Neurosci 21: 8765–8771
Van der Stelt M, Veldhuis WB, Bär PR, Veldink GA, Vliegenthart JF, Nicolay K 2001 Neuroprotection by Δ9-tetrahydrocannabinol, the main active compound in marijuana, against ouabain-induced in vivo excitotoxicity. J Neurosci 21: 6475–6479
Martínez-Orgado J, Fernández-Frutos B, González R, Romero E, Urigüen L, Romero J, Viveros MP 2003 Neuroprotection by the cannabinoid agonist WIN-55212 in an in vivo newborn rat model of acute severe asphyxia. Mol Brain Res 114: 132–139
Fernandez-Lopez D, Martinez-Orgado J, Casanova I, Bonet B, Leza JC, Lorenzo P, Moro MA, Lizasoain I 2005 Immature rat brain slices exposed to oxygen-glucose deprivation as an in vitro model of neonatal hypoxic-ischemic encephalopathy. J Neurosci Methods 145: 205–212
Johnston MV 2001 Excitotoxicity in neonatal hypoxia. Ment Retard Dev Disabil Res Rev 7: 229–234
Mishra OP, Fritz KI, Delivoria-Papadopoulos M 2001 NMDA receptor and neonatal hypoxic brain injury. Ment Retard Dev Disabil Res Rev 7: 249–253
Breivogel CS, Walker JM, Huang SM, Roy MB, Childers SR 2004 Cannabinoid signaling in rat cerebellar granule cells: G-protein activation, inhibition of glutamate release and endogenous cannabinoids. Neuropharmacology 47: 81–91
Melis M, Pistis M, Perra S, Muntoni AL, Pillolla G, Gessa GL 2004 Endocannabinoids mediate presynaptic inhibition of glutamatergic transmission in rat ventral tegmental area dopamine neurons through activation of CB1 receptors. J Neurosci 24: 53–62
Köfalvi A, Vizi ES, Ledent C, Sperlágh B 2003 Cannabinoids inhibit the release of [3H]glutamate from rodent hippocampal synaptosomes via a novel CB1 receptor action. Eur J Neurosci 18: 1973–1978
Hajos N, Ledent C, Freund TF 2001 Novel cannabinoid-sensitive receptor mediates inhibition of glutamatergic synaptic transmission in the hippocampus. Neuroscience 106: 1–4
Hájos N, Freund TF 2002 Pharmacological separation of cannabinoid sensitive receptors on hippocampal excitatory and inhibitory fibers. Neuropharmacology 43: 503–510
Brown TM, Brotchie JM, Fitzjohn SM 2003 Cannabinoids decrease corticostriatal synaptic transmission via an effect on glutamate uptake. J Neurosci 23: 11073–11077
Hurtado O, Cárdenas A, Lizasoain I, Boscá L, Leza JC, Lorenzo P, Moro MA 2001 Up-regulation of TNF-α convertase (TACE/ADAM17) after oxygen and glucose deprivation in rat forebrain slices. Neuropharmacology 40: 1094–1102
Allan SM, Rothwell NJ 2001 Cytokines and acute neurodegeneration. Nat Rev Neurosci 2: 734–744
Croxford JL, Miller SD 2003 Immunoregulation of a viral model of multiple sclerosis using the synthetic cannabinoid R(+)WIN55,212. J Clin Invest 111: 1231–1240
Molina-Holgado F, Pinteaux E, Moore JD, Molina-Holgado E, Guaza C, Gibson RM, Rothwell N 2003 Endogenous interleukin-1 receptor antagonist mediates anti-inflammatory and neuroprotective actions of cannabinoids in neurons and glia. J Neurosci 23: 6470–6474
Hurtado O, Lizasoain I, Fernandez-Tome P, Alvarez-Barrientos A, Leza JC, Lorenzo P, Moro MA 2002 TACE/ADAM17-TNF-alpha pathway in rat cortical cultures after exposure to oxygen-glucose deprivation or glutamate. J Cereb Blood Flow Metab 22: 576–585
Cárdenas A, Moro MA, Hurtado O, Leza JC, Lorenzo P, Castrillo A, Bodegón OG, Boscá L, Lizasoain I 2000 Implication of glutamate in the expression of inducible nitric oxide synthase after oxygen and glucose deprivation in rat forebrain slices. J Neurochem 74: 2041–2048
Lizasoain I, Moro MA, Knowles RG, Darley-Usmar V, Moncada S 1996 Nitric oxide and peroxynitrite exert distinct effects on respiration by brain mitochondria which are differentially blocked by glutathione or glucose. Biochem J 314: 877–880
Molina-Holgado F, Molina-Holgado E, Guaza C, Rothwell NJ 2002 Role of CB1 and CB2 receptors in the inhibitory effects of cannabinoids on lipopolysaccharide-induced nitric oxide release in astrocyte cultures. J Neurosci Res 67: 829–836
Jüttler E, Potrovita I, Tarabin V, Prinz S, Dong-Si, Fink G, Schwaninger M 2004 The cannabinoid dexanabinol is an inhibitor of the nuclear factor kappa B (NF-κB). Neuropharmacology 47: 580–592
Fride E 2004 The endocannabinoid-CB1 receptor system in pre- and postnatal life. Eur J Pharmacol 500: 289–297
Jin KL, Mao XO, Goldsmith PC, Greenberg DA 2000 CB1 cannabinoid receptor induction in experimental stroke. Ann Neurol 48: 257–261
Parmentier-Batteur S, Jin K, Mao XO, Xie L, Greenberg DA 2002 Increased severity of stroke in CB1 cannabinoid receptor knock-out mice. J Neurosci 22: 9771–9775
Van Sickle MD, Duncan M, Kingsley PJ, Mouihate A, Urbani P, Mackie K, Stella N, Makriyannis A, Piomelli D, Davison JS, Marnett LJ, Di Marzo V, Pittman QJ, Patel KD, Sharkey KA 2005 Identification and functional characterization of brainstem cannabinoid CB2 receptors. Science 310: 329–332
Maresz K, Carrier EJ, Ponomarev ED, Hillard CJ, Dittel BN 2005 Modulation of the cannabinoid CB2 receptor in microglial cells in response to inflammatory stimuli. J Neurochem 95: 437–445
Benito C, Núñez E, Tolón RM, Carrier EJ, Rábano A, Hillard CJ, Romero J 2003 Cannabinoid CB2 receptors and fatty acid amide hydrolase are selectively overexpressed in neuritic plaque-associated glia in Alzheimer's disease brains. J Neurosci 23: 11136–11141
Carlisle SJ, Marciano-Cabral F, Staab A, Ludwick C, Cabral GA 2002 Differential expression of the CB2 cannabinoid receptor by rodent macrophages and macrophage-like cells in relation to cell activation. Int Immunopharmacol 2: 69–82
Howlett AC, Barth F, Bonner TI, Cabral G, Casellas G, Devane WA, Felder CC, Herkenham M, Mackie K, Martin BR, Mechoulam R, Pertwee RG 2002 International Union of Pharmacology. XXVII. Classification of cannabinoid receptors. Pharmacol Rev 54: 161–202
Acknowledgements
We are grateful to Andrew Lumsden for his help in reviewing the manuscript and to Ruth Pazos, Cristina Benito, and Rosa M. Tolón from the Laboratorio de Apoyo a la Investigación of the Fundación Hospital Alcorcón for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by grants from Sociedad Española de Neonatología 2000 (J.M.-O.), FIS-PI021540 (J.M.-O.), FIS-PI030304 (M.A.M.), SAF 2004-00237 (J.R.), and SAF2005-05960 (I.L.).
Rights and permissions
About this article
Cite this article
Fernández-López, D., Martínez-Orgado, J., Nuñez, E. et al. Characterization of the Neuroprotective Effect of the Cannabinoid Agonist WIN-55212 in an In Vitro Model of Hypoxic-Ischemic Brain Damage in Newborn Rats. Pediatr Res 60, 169–173 (2006). https://doi.org/10.1203/01.pdr.0000228839.00122.6c
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000228839.00122.6c
This article is cited by
-
Cytotoxicity associated with acute and chronic administration of synthetic cannabinoids “Strox” in the brain, liver, heart, and testes of male albino rats: histological and immunohistochemical study
Egyptian Journal of Forensic Sciences (2023)
-
Cannabinoid Receptor Type 1 Agonist ACEA Improves Cognitive Deficit on STZ-Induced Neurotoxicity Through Apoptosis Pathway and NO Modulation
Neurotoxicity Research (2019)
-
Cannabinoids in Neurodegenerative Disorders and Stroke/Brain Trauma: From Preclinical Models to Clinical Applications
Neurotherapeutics (2015)
-
Cannabinoid Receptor 2: Potential Role in Immunomodulation and Neuroinflammation
Journal of Neuroimmune Pharmacology (2013)
-
Stimulation of CB1 Cannabinoid and NMDA Receptors Increases Neuroprotective Effect against Diazinon-Induced Neurotoxicity
Neurophysiology (2013)