Abstract
Antenatal glucocorticoids are routinely given to women at risk for preterm delivery. The fetus is protected from excessive glucocorticoids by the placental enzyme 11β-hydroxysteroid dehydrogenase type 2 (11β-HSD-2), which catalyzes the conversion of cortisol to its biologically inactive metabolite, cortisone. We examined the effects of antenatal dexamethasone on the expression of placental 11β-HSD-2 in fetal sheep. Ewes were randomized to receive repeated or single courses of dexamethasone or placebo beginning at 76-78 or 104-106 d of gestation, respectively. In the single course group, the ewes received dexamethasone (6 mg, n = 7) or placebo (n = 6) as four intramuscular injections over 48 h up to 18 h before placental harvest. In the repeated course group, the ewes received the same treatment (dexamethasone, n = 10, or placebo, n = 9) once a week for 5 consecutive weeks starting at 76–78 d of gestation. Placental harvest occurred at 106–108 d of gestation in the four groups. By semi-quantitative RT-PCR, we found that placental 11β-HSD-2 expression was lower in the fetuses of ewes exposed to a single course of dexamethasone than placebo (p < 0.05). Placental 11β-HSD-2 expression did not differ significantly between fetuses of ewes treated with repeated courses of dexamethasone compared with placebo, or a single course of dexamethasone. Fetuses of dexamethasone treated ewes weighed less than those of placebo treated ewes (ANOVA, main effects for dexamethasone versus placebo treatment:F = 14.5, p = 0.007). Fetuses of ewes exposed to repeated courses of dexamethasone weighed less than those of ewes exposed to placebo or a single course of dexamethasone (p < 0.05). We conclude that maternal antenatal dexamethasone treatment reduces placental 11β-HSD-2 expression and fetal weight at mid-gestation in the ovine pregnancy.
Similar content being viewed by others
Main
Glucocorticoids play a major regulatory role in the body's ability to manage physiologic stress, counteract inflammation, and maintain fuel metabolism. Administration of synthetic glucocorticoids to women at risk for premature delivery is an established, evidenced-based intervention known to accelerate the rate of maturation of various fetal organs, such as the lungs, heart, brain, liver, kidney, and gut (1). However, intrauterine growth restriction can be an untoward side effect of antenatal glucocorticoids (2, 3).
Although glucocorticoids are highly lipophilic and rapidly cross the placenta, the fetus usually has lower levels of glucocorticoids than its mother (4). This gradient is achieved by an important bioactive enzyme, 11β-hydroxysteroid dehydrogenase. There are two distinct isoforms of 11β-hydroxysteroid dehydrogenase, 11β-hydroxysteroid dehydrogenase types 1 and 2 (11β-HSD-1 and 11β-HSD-2) (5). In vitro, the two isoforms catalyze opposite reactions, i.e. type 1 acts mainly as an 11-oxoreductase, producing active hormone, cortisol (6), and type 2 works as an NAD+-dependent 11β-dehydrogenase, inactivating cortisol to its inert metabolite, cortisone (7). Although 11β-HSD-1 is found in the fetal ovine liver (8), ontogeny of this enzyme differs among species, and its precise physiologic role remains unknown. 11β-HSD-2 is widely distributed in fetal tissues, including the placenta, where it is highly expressed (9–15). In the placenta, 11β-HSD-2 appears to inactivate maternally derived cortisol, diminishing fetal glucocorticoid exposure (16–18).
11β-HSD-1 and 11β-HSD-2 expression and enzyme activity are reportedly present in the ovine placenta (19, 20). Although Yang et al. showed that 11β-HSD-1 was the main isoform in the ovine placenta (21), they reported that its dehydrogenase activity (conversion of cortisol to cortisone) predominated and speculated that it may have a similar function to 11β-HSD-2 (17). Clarke et al. recently demonstrated that ovine placental 11β-HSD-2 activity decreases with increasing gestational age (20).
Synthetic glucocorticoids, such as dexamethasone, are poorly metabolized by 11β-HSD-2 (22–24), enabling them to cross the placenta into the fetal compartment (25–28). Limited studies in sheep have demonstrated the growth-retarding effects of single and multiple courses of antenatal glucocorticoids (29–31). Further, multiple courses of dexamethasone have been associated with a down-regulation of 11β-HSD-2 expression in adult rat kidney (23). Clarke et al.(20) recently reported a reduction in 11β-HSD-2 activity in the placenta after cortisol was directly infused into late gestation fetal sheep.
The National Institutes of Health Consensus conference on the effects of corticosteroids for fetal maturation has recommended prompt use of antenatal steroids for women at risk for premature delivery (1). Unfortunately, many human preterm deliveries occur in the second trimester shortly after fetal exposure to maternal glucocorticoid treatment. Although randomized controlled trials support the use of antenatal steroids (32), the use of repeated courses of maternally administered antenatal steroids has not been adequately studied (33, 34). Nevertheless, it is not uncommon practice to treat women who are at continued risk for premature delivery with several courses of antenatal steroids (33, 34).
Therefore, in this study, we examined the effects of single and repeated courses of maternal corticosteroid treatment on placental 11β-HSD-2 expression, fetal growth, and cortisol concentrations in mid-gestation ovine fetuses. We hypothesized that single and repeated courses of dexamethasone would reduce fetal growth, cortisol concentrations, and placental 11β-HSD-2 expression. Our study was designed to examine the effects of single and repeated courses of antenatal corticosteroids in doses similar to those used in the clinical setting to treat women at risk for premature delivery.
METHODS
This study was conducted after approval by the Institutional Animal Care and Use Committees of Brown University and Women and Infants' Hospital of Rhode Island and according to the National Institutes of Health Guidelines for use of experimental animals.
Animal preparation.
Surgery was performed under 1% to 2% halothane anesthesia on 22 time-dated Eastern mixed breed pregnant ewes at 99–101 d of gestation as previously described (35). Singleton and twin pregnancies were included; however, when a twin gestation was present, only one fetus was catheterized. The thoracic aorta was cannulated via the brachial artery for blood sample withdrawal. Fetuses of ewes assigned to receive repeated courses of dexamethasone or placebo were catheterized at 98–99 d of gestation after the ewes received four courses of dexamethasone or placebo. The final course of dexamethasone or placebo was given after recovery from surgery. The plasma and placental samples for this study were obtained from animals enrolled in a larger series of studies to examine the effects of antenatal corticosteroids on blood-brain barrier function in ovine fetuses (36).
Ewes were randomly assigned to one of four treatments groups: (1) single course dexamethasone or (2) placebo (3), five repeated courses of dexamethasone, or (4) placebo. The ewes received a 6 mg intramuscular injection of dexamethasone (Fujisawa, Deerfield, IL, U.S.A., concentration = 4 mg·ml−1, 1.5 mL was given to each ewe) or placebo (0.9% NaCl) every 12 h for 48 h starting at 104–106 d in the single course groups, and on days 76, 84, 91, 98, and 105 of gestation in the repeated course groups (Fig. 1, adapted from Quinlivan et al.(37)). The rationale for choosing this treatment regime (i.e. 6 mg of dexamethasone every 12 h for 48 h) was to use doses and a treatment schedule of dexamethasone similar to that currently recommended to enhance fetal maturation in women at risk for preterm delivery (1).
Open squares (□) represent four intramuscular placebo injections (0.9 NaCl) to the ewes every 12 h for 48 h. Closed squares (▪) represent four 6 mg dexamethasone injections to the ewes every 12 h for 48 h. Animals were killed at 106–108 d of gestation after plasma cortisol concentrations were obtained from the fetuses. After sacrifice, fetal weight and plasma cortisol concentrations and placental 11β-HSD-2 expression were determined.
Experimental protocol and methodology.
On days 106–108 of gestation, 18 h after the last dose of dexamethasone or placebo had been given to the ewes, fetal arterial cortisol concentrations were obtained while the ewes were standing quietly in a cart after being acclimatized to the laboratory for 2 h. After plasma samples were obtained, the ewes were anesthetized (ketamine, 50 mg·kg−1 and hysterotomy performed. The fetuses were removed and weighed, and the placental cotyledons were rapidly removed, immediately frozen in liquid nitrogen and stored at −80°C until analysis.
Hormonal analysis.
Cortisol concentrations were measured in duplicate using Clinical Assays™ GammaCoat™ Cortisol 125I-RIA (DiaSorin, Stillwater, MN, U.S.A.). The GammaCoat™ antiserum exhibits 100% cross reactivity with cortisol. The observed coefficient of variation for inter- and intra-assay precision were 10.1 and 7.9%, respectively (38).
RNA preparation.
Total RNA was extracted from approximately 100 mg of placental tissue per sample by the method of Chomczynski and Sacchi (39) using Tri Reagent® (Molecular Research Center, Cincinnati, OH, U.S.A.). Samples were homogenized with 1 mL of Tri Reagent®. Two hundred microliters of chloroform were added to the solution, mixed, stored in room temperature for 15 min, and centrifuged (14,000 rpm; 4°C) for 15 min. The aqueous phase was transferred to a fresh tube and precipitated with 500 μL isopropanol and stored at room temperature for 10 min. Samples were centrifuged for 8 min (14,000 rpm; 4°C), the supernatant was removed, and RNA pellets were washed with 80% ethanol and centrifuged (8,000 rpm; 4°C) for 5 min. The ethanol wash was removed and pellets air-dried for 5 min. RNA pellets were dissolved in 100 μL Tris-EDTA (TE) buffer (pH 7.5) and precipitated with ethanol to purify. RNA samples were then quantified spectrophotometrically at 260 nm and 280 nm (GeneQuant RNA/DNA Calculator, Pharmacia, Cambridge, England), aliquoted and stored at −80°C until further analysis. Five micrograms of total RNA was run on formaldehyde gel to ensure its integrity.
Reverse transcriptase/PCR amplification of placental RNA.
cDNA was synthesized from placental RNA by the SuperScript™ Preamplification System (GIBCO BRL®, New York, NY) for first-strand DNA synthesis according to the manufacturer's instructions, with minor modifications. Briefly, 5 μg total RNA was digested by DNase I, then hybridized with oligo (dT)12–18. The reaction was carried out using SuperScript II reverse transcriptase for 50 min at 42°C. Subsequently, one tenth of the first-strand cDNA reaction was amplified by 11β-HSD-2 specific primers designed according to Leckie et al.(40). GAPDH specific primers, designed according to Mellon et al.(41), were used for internal control of the PCR reaction. The PCR amplification conditions were 95°C, 5 min (95°C, 30 s; 50°C, 30 s; 72°C, 60 s), 32 cycles, 72°C, 10 min. These conditions were chosen after running time-cycled PCR established the range of linearization for both 11β-HSD-2 and GAPDH (Fig. 2). To confirm the identity of the PCR product generated as 11β-HSD-2, the amplified fragment was purified and digested with the three restriction enzymes Hin dII, Sty I and Pst I. The fragments were separated on a 1.2% agarose gel and sizes compared with previously published sequences for sheep (42). The PCR products were visualized on 1.5% agarose gel electrophoresis after ethidium bromide staining. Optical densitometry was analyzed using NIH Imageshare (Version 1.61, Springfield, VA, U.S.A.).
Statistical analysis.
All results are presented as the mean ± SEM. Fetal weights, cortisol concentrations, and the ratio of 11β-HSD-2 to GAPDH were compared using two-way ANOVA for two factors where treatment (placebo or dexamethasone) and groups (single or repeated courses) were the factors. When a significant difference was found by ANOVA, the Newman-Keuls or Duncan's Multiple Range tests were used to identify specific differences among the groups. χ2 analysis was used to compare the number of twin pregnancies among the four groups. The least squares linear regression analysis was used to compare the total weight of the fetuses in each pregnancy to the weight of the ewes. A probability of p < 0.05 was considered statistically significant.
RESULTS
Placental 11β-HSD-2 expression was significantly lower in the fetuses of ewes treated with dexamethasone than placebo (ANOVA, main effects for dexamethasone versus placebo treatment:F = 8.6, p = 0.007). Posthoc analysis revealed that placental 11β-HSD-2 expression was lower in fetuses of ewes treated with a single course of dexamethasone than placebo (Figs. 3 and 4). 11β-HSD-2 expression did not differ between fetuses of ewes exposed to repeated courses of dexamethasone and placebo, or between repeated and single courses of dexamethasone (Fig. 2 and 3). Although placental 11β-HSD-2 expression appeared lower after exposure of the ewes to repeated courses of dexamethasone, statistical significance was not achieved, possibly because of the number of animals examined.
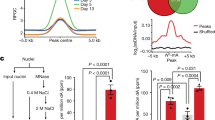
The effect of maternally administered antenatal dexamethasone on the expression of placental 11β-HSD-2 in the fetal sheep. Open bars represent single course placebo, hatched bars represent single course dexamethasone (Single DEX), closed bars represent repeated course placebo, and striped bars represent repeated course dexamethasone (Repeated DEX). Values are mean ± SEM. *p < 0.05 vs fetuses of ewes exposed to a single course of placebo.
Representative ethidium bromide-stained agarose gels containing cDNA amplified from ovine placental RNA. A 100-bp size ladder (M) is shown in the first lane. (A) Lanes 1–3 are fetuses of ewes exposed to a single course of placebo, lanes 4–7 are fetuses of ewes exposed to a single course of dexamethasone; (B) Lanes 1–4 are fetuses of ewes exposed to a repeated course of placebo, lanes 5–11 are fetuses of ewes exposed to a repeated course of dexamethasone. Placental RNA (5 μg) from fetal sheep was reverse transcribed into cDNA and amplified by PCR using 11β-HSD-2-specific primers or GAPDH-specific primers as control for cDNA synthesis. Amplified products were separated on 1.5% agarose gels and stained with ethidium bromide.The 11β-HSD-2 fragment is 657 bp and the GAPDH fragment is 240 bp.
Fetuses of dexamethasone treated ewes weighed less than those of placebo treated ewes (ANOVA, main effects for dexamethasone versus placebo treatment:F = 14.5, p = 0.007). Posthoc analysis revealed that fetuses of ewes exposed to repeated courses of dexamethasone weighed less than those of ewes exposed to both placebo groups and a single course of dexamethasone (Table 1, p < 0.05). Twins were present in 6 of 10 ewes exposed to a single course of dexamethasone, 5 of 9 exposed to a single course of placebo, 4 of 7 exposed to repeated courses of dexamethasone and 3 of 6 exposed to repeated courses of placebo. The numbers of twin pregnancies did not differ among the four groups (χ2, NS), and thus the distribution of twins did not effect the group-wise calculation of body weights. The ewes weighed 70.9 ± 3.1 kg after treatment with a single course dexamethasone, 70.5 ± 3.3 kg after treatment with placebo, 86.0 ± 3.9 kg after treatment with repeated courses of dexamethasone and 72.2 ± 7.6 kg after treatment with repeated courses of placebo. Although it appeared that the ewes exposed to repeated courses of dexamethasone weighed more than the other groups, statistical significance was not achieved (ANOVA, main effects for group treatment:F = 2.45, p = 0.08). There was no correlation between the total fetal weight in each ewe and the weight of the ewes (r = 0.08, p = 0.64).
Fetal plasma cortisol concentrations were lower in the fetuses of ewes treated with dexamethasone than placebo (ANOVA, main effects for dexamethasone versus placebo treatment:F = 5.27, p = 0.03,). Posthoc analysis revealed cortisol concentrations were lower in fetuses of ewes treated with a single course of dexamethasone than placebo (p = 0.01, Table 1). There were no differences in fetal plasma cortisol concentrations when fetuses of ewes exposed to repeated courses of dexamethasone were compared with repeated courses of placebo or a single course of dexamethasone. Plasma cortisol concentrations were lower in the ewes treated with dexamethasone than placebo (ANOVA, main effects for dexamethasone versus placebo treatment:F = 23.26, p = 0.00004). Posthoc analysis revealed the cortisol concentrations were lower in ewes treated with a single and repeated courses of dexamethasone than placebo (p = 0.0002, Table 1).
DISCUSSION
The objective of our study was to examine fetal growth, plasma cortisol concentrations and placental 11β-HSD-2 expression in fetuses of ewes exposed to single and repeated courses of dexamethasone at mid-gestation. The ewes were exposed to repeated weekly courses of dexamethasone or placebo beginning at 76–78 d of gestation and a single course of dexamethasone or placebo beginning at 104–106 d of gestation (full term = 145 ± 5 d). The lower plasma cortisol concentrations in the ewes exposed to both the single and repeated courses of dexamethasone confirmed that corticosteroids suppressed the adrenocortical axis demonstrating that this regimen had a significant effect on the ewes.
A novel finding of our study was that placental 11β-HSD-2 expression was significantly lower after exposure of ewes at mid-gestation to single but not repeated courses of dexamethasone. This was not entirely unexpected as Clarke et al. recently reported that elevations in endogenous fetal cortisol levels and intravascular infusions of exogenous cortisol into late gestation fetal sheep reduced placental 11 β-HSD-2 activity to levels observed in near term fetuses (20). Also similar to our findings, serial doses of dexamethasone administered to rats in late gestation (days 15–22, term = 23) were not accompanied by reductions in placental 11β-HSD-2 activity (43). However, in the adult rat kidney, where 11β-HSD-2 also functions as a dehydrogenase, multiple and consecutive daily doses of dexamethasone were associated with reduced 11β-HSD-2 expression (23). Thus, it appears as if the effect of exogenous steroids on 11β-HSD-2 is dosage, interval and tissue-dependent.
The reason that we detected a significant reduction in placental 11β-HSD-2 mRNA by semi-quantitative RT-PCR in fetuses of ewes treated with a single but not repeated courses of dexamethasone at mid-gestation cannot be discerned by our study. Although placental 11β-HSD-2 expression also appeared to be lower after repeated courses of dexamethasone compared with placebo, statistical significance was not observed. We cannot rule out the possibility that if a larger number of animals had been studied, we might have achieved statistical significance in this group. Nonetheless, repeated courses of dexamethasone did not accentuate the reductions in 11β-HSD-2 observed after a single course of dexamethasone when given to the ewes at mid-gestation. The apparent lack of change in the placental 11β-HSD-2 expression after exposure of the ewes to repeated courses of dexamethasone might reflect glucocorticoid receptor desensitization by repeated exposures to dexamethasone. Glucocorticoids may down-regulate glucocorticoid receptors during the perinatal period as reported by Felszeghy et al.(44).
Ovine placental 11β-HSD-1 appears to be developmentally regulated, with peak dehydrogenase activity at mid-gestation decreasing at term (21). Although ovine placental 11β-HSD-2 activity has recently been reported to decrease between 128–132 d of gestation and term in association with the normal prepartum increase in endogenous fetal cortisol concentration (20), its developmental profile has not been characterized earlier in gestation. We speculate that differences in the developmental regulation of 11β-HSD-2 in the placenta might also account in part for our finding that 11β-HSD-2 expression was decreased in fetuses of ewes exposed to a single course dexamethasone at mid-gestation.
We found that fetal sheep weighed less after dexamethasone treatment, when fetal weight was obtained at 106–108 d of gestation. Our findings are consistent with those of Jobe et al.(30) who found that treatment of ewes with three doses of betamethasone at 104, 111, and 118 d of gestation was associated with reductions in fetal weight when the fetuses were delivered at 125 or 145 d of gestation. In contrast, the same authors did not observe growth restriction in fetal lambs injected directly with betamethasone at mid-gestation and killed at 128 d or at term (45). Further, 72 h of intra-fetal administration of dexamethasone in early gestation lambs, with sacrifice at the end of the infusion, was not accompanied by alterations in fetal growth (46). The findings of our study combined with those of others suggest that 1) the placenta plays an important role in modifying the effect of maternally administered glucocorticoids and 2) the time in gestation of glucocorticoid overexposure and/or the dosing regime have important effects on fetal growth (30, 45, 47–49). It is also important to point out that in our study, a direct affect glucocorticoid excess on fetal growth in fetuses of ewes exposed to repeated courses of dexamethasone is unlikely, because fetal plasma cortisol concentrations did not differ between the fetuses of ewes exposed to dexamethasone and placebo. Instead, an indirect effect of glucocorticoids on the IGF (IGF) axis is possible.
We found that a single but not repeated courses of dexamethasone was associated with decreases in plasma cortisol concentrations in mid-gestation fetal sheep. Consistent with our findings, Tangalakis et al. found that when dexamethasone was infused for 72 h to ewes at 80–90 d of gestation, fetal plasma cortisol concentrations were decreased (47). These authors speculated that at this gestational age, the fetal adrenal gland requires at least 6 h of ACTH exposure to stimulate cortisol secretion. Furthermore, Jobe et al. showed that exposure to antenatal betamethasone early in gestation was not associated with a reduction in plasma cortisol concentration when measured in late gestation or full term fetal sheep (30). Our findings, and those of others (30, 47), suggest the fetal plasma cortisol response to exogenous antenatal corticosteroids depends upon the treatment regimen, the time in gestation at which the exogenous steroids are administered, and the timing of cortisol sampling relative to exogenous steroid administration.
Further, our findings suggest that single but not repeated courses of antenatal glucocorticoids in doses similar to those used in the clinical setting to treat women in premature labor may suppress the fetal hypothalamic-pituitary-adrenal axis at mid-gestation. These findings may be interpreted to suggest that there may be a resetting of the fetal hypothalamic-pituitary-adrenal axis after repeated glucocorticoid exposure, whereby the negative feedback loop is attenuated (50, 51). Moreover, the lack of change in plasma cortisol concentration after exposure to repeated courses of antenatal dexamethasone might also reflect potential down-regulation of central glucocorticoid receptors (44).
CONCLUSION
In summary, we have shown that dexamethasone is associated with fetal growth restriction at 108 d of the ovine gestation. A single course but not repeated courses of dexamethasone given to pregnant ewes is associated with reductions in fetal plasma cortisol concentrations and placental 11β-HSD-2 expression early in the ovine gestation. These results suggest that maternal antenatal glucocorticoids administered early in gestation in doses similar to those used in the clinical setting to treat women in premature labor are associated with significant effects on placental function, fetal growth and the fetal hypothalamic-pituitary-adrenal axis.
Abbreviations
- 11β-HSD-1:
-
11β-hydroxysteroid dehydrogenase type 1
- 11β-HSD-2:
-
11β-hydroxysteroid dehydrogenase type 2
- GAPDH:
-
glyceraldehyde-3-phosphate dehydrogenase
- RT-PCR:
-
reverse transcriptase PCR
- ACTH:
-
adrenocorticotrophic hormone
- ANOVA:
-
analysis of variance
References
Panel NICHD 1995 Effect of corticosteroids for fetal maturation on perinatal outcomes. JAMA 273: 413–418
Benediktsson R, Lindsay RS, Noble J, Seckl JR, Edwards CR 1993 Glucocorticoid exposure in utero: new model for adult hypertension. Lancet 341: 339–341
Reinisch JM, Simon NG, Karow WG, Gandelman R 202 1978 Prenatal exposure to prednisone in humans and animals retards intrauterine growth. Science 202: 436–438
Beitins IZ, Kowarski A, Shermeta DW, De Lemos RA, Migeon CJ 1970 Fetal maternal secretion rate of cortisol in sheep: diffusion resistance of the placenta. Pediatr Res 4: 129–134
Krozowski Z, Li KX, Koyama K, Smith RE, Obeyesekere VR, Stein-Oakley A, Sasano H, Coulter C, Cole T, Sheppard KE 1999 The type I type II 11beta-hydroxysteroid dehydrogenase enzymes. J Steroid Biochem Mol Biol 69: 391–401
Lakshmi V, Monder C 1988 Purification characterization of the corticosteroid 11 beta-dehydrogenase component of the rat liver 11 beta-hydroxysteroid dehydrogenase complex. Endocrinology 123: 2390–2398
Edwards CR, Stewart PM, Burt D, Brett L, McIntyre MA, Sutanto WS, de Kloet ER, Monder C 1988 Localisation of 11 beta-hydroxysteroid dehydrogenase-tissue specific protector of the mineralocorticoid receptor. Lancet 2: 986–989
Seckl JR, Chapman KE 1997 Medical physiological aspects of the 11beta-hydroxysteroid dehydrogenase system. Eur J Biochem 249: 361–364
Bernal AL, Flint AP, Anderson AB, Turnbull AC 1980 11 beta-Hydroxysteroid dehydrogenase activity (E.C. 1.1.1.146) in human placenta decidua. J Steroid Biochem 13: 1081–1087
Blasco MJ, Lopez Bernal A, Turnbull AC 1986 11 Beta-Hydroxysteroid dehydrogenase activity of the human placenta during pregnancy. Horm Metab Res 18: 638–641
Brown RW, Chapman KE, Edwards CR, Seckl JR 1993 Human placental 11 beta-hydroxysteroid dehydrogenase: evidence for partial purification of a distinct NAD-dependent isoform. Endocrinology 132: 2614–2621
Kim EK, Wood CE, Keller-Wood M 1995 Characterization of 11 beta-hydroxysteroid dehydrogenase activity in fetal adult ovine tissues. Reprod Fertil Dev 7: 377–383
Langlois DA, Matthews SG, Yu M, Yang K 1995 Differential expression of 11 beta-hydroxysteroid dehydrogenase 1 2 in the developing ovine fetal liver kidney. J Endocrinol 147: 405–411
Sun K, Yang K, Challis JR 1997 Differential expression of 11 beta-hydroxysteroid dehydrogenase types 1 2 in human placenta fetal membranes. J Clin Endocrinol Metab 82: 300–305
Stewart PM, Murry BA, Mason JI 1994 Type 2 11 beta-hydroxysteroid dehydrogenase in human fetal tissues. J Clin Endocrinol Metab 78: 1529–1532
Benediktsson R, Calder AA, Edwards CR, Seckl JR 1997 Placental 11 beta-hydroxysteroid dehydrogenase: a key regulator of fetal glucocorticoid exposure. Clin Endocrinol Oxf 46: 161–166
Yang K 1997 Placental 11 beta-hydroxysteroid dehydrogenase: barrier to maternal glucocorticoids. Rev Reprod 2: 129–132
Waddell BJ, Benediktsson R, Brown RW, Seckl JR 1998 Tissue-specific messenger ribonucleic acid expression of 11beta- hydroxysteroid dehydrogenase types 1 2 the glucocorticoid receptor within rat placenta suggests exquisite local control of glucocorticoid action. Endocrinology 139: 1517–1523
Yang K 1995 Co-expression of two distinct isoforms of 11 beta-hydroxysteroid dehydrogenase in the ovine placenta. J Steroid Biochem Mol Biol 52: 337–343
Clarke KA, Ward JW, Forhead AJ, Giussani DA, Fowden AL 2002 Regulation of 11beta-hydroxysteroid dehydrogenase type 2 activity in ovine placenta by fetal cortisol. J Endocrinol 172: 527–534
Yang K, Langlois DA, Campbell LE, Challis JR, Krkosek M, Yu M 1997 Cellular localization developmental regulation of 11 beta- hydroxysteroid dehydrogenase type 1 (11 beta-HSD1) gene expression in the ovine placenta. Placenta 18: 503–509
Albiston AL, Obeyesekere VR, Smith RE, Krozowski ZS 1994 Cloning tissue distribution of the human 11 beta-hydroxysteroid dehydrogenase type 2 enzyme. Mol Cell Endocrinol 105: R11–17
Li KX, Smith RE, Ferrari P, Funder JW, Krozowski ZS 1996 Rat 11 beta-hydroxysteroid dehydrogenase type 2 enzyme is expressed at low levels in the placenta is modulated by adrenal steroids in the kidney. Mol Cell Endocrinol 120: 67–75
Siebe H, Baude G, Lichtenstein I, Wang D, Buhler H, Hoyer GA, Hierholzer K 1993 Metabolism of dexamethasone: sites activity in mammalian tissues. Ren Physiol Biochem 16: 79–88
Bayard F, Louvet JP, Ruckebusch Y, Boulard C 1972 Transplacental passage of dexamethasone in sheep. J Endocrinol 54: 349–350
Anderson DF, Stock MK, Rankin JH 1979 Placental transfer of dexamethasone in near-term sheep. J Dev Physiol 1: 431–436
Wintour EM, Alcorn D, McFarlane A, Moritz K, Potocnik SJ, Tangalakis K 1994 Effect of maternal glucocorticoid treatment on fetal fluids in sheep at 0.4 gestation. Am J Physiol 266: R1174–1181
Smith MA, Thomford PJ, Mattison DR, Slikker W 1988 Transport metabolism of dexamethasone in the dually perfused human placenta. Reprod Toxicol 2: 37–43
Ikegami M, Jobe AH, Newnham J, Polk DH, Willet KE, Sly P 1997 Repetitive prenatal glucocorticoids improve lung function decrease growth in preterm lambs. Am J Respir Crit Care Med 156: 178–184
Jobe AH, Wada N, Berry LM, Ikegami M, Ervin MG 1998 Single repetitive maternal glucocorticoid exposures reduce fetal growth in sheep. Am J Obstet Gynecol 178: 880–885
Sloboda DM, Newnham JP, Challis JR 2000 Effects of repeated maternal betamethasone administration on growth hypothalamic-pituitary-adrenal function of the ovine fetus at term. J Endocrinol 165: 79–91
Crowley P, Chalmers I, Keirse MJ 1990 The effects of corticosteroid administration before preterm delivery: an overview of the evidence from controlled trials. Br J Obstet Gynaecol 97: 11–25
French NP, Hagan R, Evans SF, Godfrey M, Newnham JP 1999 Repeated antenatal corticosteroids: size at birth subsequent development. Am J Obstet Gynecol 180: 114–121
Banks BA, Cnaan A, Morgan MA, Parer JT, Merrill JD, Ballard PL, Ballard RA 1999 Multiple courses of antenatal corticosteroids outcome of premature neonates. North American Thyrotropin-Releasing Hormone Study Group. Am J Obstet Gynecol 181: 709–717
Stonestreet BS, Le E, Berard DJ 1993 Circulatory metabolic effects of beta-adrenergic blockade in the hyperinsulinemic ovine fetus. Am J Physiol 265: H1098–1106
Stonestreet BS, McKnight AJ, Sadowska GB, Patlak CS, Petersson KH 2000 Effects of repeated courses of antenatal corticosteroids on blood-brain barrier function in early gestation ovine fetuses. Pediatr Res 4: 470A
Quinlivan JA, Archer MA, Dunlop SA, Evans SF, Beazley LD, Newnham JP 1998 Fetal growth retardation, particularly within lymphoid organs, following repeated maternal injections of betamethasone in sheep. J Obstet Gynaecol Res 24: 173–182
Stonestreet BS, Sadowska GB, McKnight AJ, Patlak C, Petersson KH 2000 Exogenous endogenous corticosteroids modulate blood-brain barrier development in the ovine fetus. Am J Physiol Regul Integr Comp Physiol 279: R468–477
Chomczynski P, Sacchi N 1987 Single-step method of RNA isolation by acid guanidinium thiocyanate-phenol-chloroform extraction. Anal Biochem 162: 156–159
Leckie C, Chapman KE, Edwards CR, Seckl JR 1995 LLC-PK1 cells model 11 beta-hydroxysteroid dehydrogenase type 2 regulation of glucocorticoid access to renal mineralocorticoid receptors. Endocrinology 136: 5561–5569
Mellon SH, Bair SR, Monis H 1995 P450c11B3 mRNA, transcribed from a third P450c11 gene, is expressed in a tissue-specific, developmentally, hormonally regulated fashion in the rodent adrenal encodes a protein with both 11-hydroxylase 18-hydroxylase activities. J Biol Chem 270: 1643–1649
Agarwal AK, Mune T, Monder C, White PC 1994 NAD(+)-dependent isoform of 11 beta-hydroxysteroid dehydrogenase. Cloning characterization of cDNA from sheep kidney. J Biol Chem 269: 25959–25962
Burton PJ, Waddell BJ 1994 11 beta-Hydroxysteroid dehydrogenase in the rat placenta: developmental changes the effects of altered glucocorticoid exposure. J Endocrinol 143: 505–513
Felszeghy K, Gaspar E, Nyakas C 1996 Long-term selective down-regulation of brain glucocorticoid receptors after neonatal dexamethasone treatment in rats. J Neuroendocrinol 8: 493–499
Polk DH, Ikegami M, Jobe AH, Sly P, Kohan R, Newnham J 1997 Preterm lung function after retreatment with antenatal betamethasone in preterm lambs. Am J Obstet Gynecol 176: 308–315
Newnham JP, Evans SF, Godfrey M, Huang W, Ikegami M, Jobe A 1999 Maternal, but not fetal, administration of corticosteroids restricts fetal growth. J Matern Fetal Med 8: 81–87
Tangalakis K, Moritz K, Shandley L, Wintour EM 1995 Effect of maternal glucocorticoid treatment on ovine fetal fluids at 0.6 gestation. Reprod Fertil Dev 7: 1595–1598
Berry LM, Polk DH, Ikegami M, Jobe AH, Padbury JF, Ervin MG 1997 Preterm newborn lamb renal cardiovascular responses after fetal or maternal antenatal betamethasone. Am J Physiol 272: R1972–1979
Jones SA, Brooks AN, Challis JR 1989 Steroids modulate corticotropin-releasing hormone production in human fetal membranes placenta. J Clin Endocrinol Metab 68: 825–830
Seckl JR, Benediktsson R, Lindsay RS, Brown RW 1995 Placental 11 beta-hydroxysteroid dehydrogenase the programming of hypertension. J Steroid Biochem Mol Biol 55: 447–455
Seckl JR, Miller WL 1997 How safe is long-term prenatal glucocorticoid treatment?. JAMA 277: 1077–1079
Acknowledgements
The authors thank Ian Bird, Ph.D., for his helpful suggestions at the onset of these studies and Richard Tucker and John Kazianis for their excellent statistical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by the National Institute of Child Health and Human Development Grant R01-HD-34618.
Rights and permissions
About this article
Cite this article
Kerzner, L., Stonestreet, B., Wu, KY. et al. Antenatal Dexamethasone: Effect on Ovine Placental 11β-Hydroxysteroid Dehydrogenase Type 2 Expression and Fetal Growth. Pediatr Res 52, 706–712 (2002). https://doi.org/10.1203/00006450-200211000-00016
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200211000-00016
This article is cited by
-
Antenatal endogenous and exogenous glucocorticoids and their impact on immune ontogeny and long-term immunity
Seminars in Immunopathology (2016)
-
Maternal Intimate Partner Violence: Relationships with Language and Neurological Development of Infants and Toddlers
Maternal and Child Health Journal (2016)