Abstract
To explore the roles of lactogens in islet function, we generated a stable line of rat insulinoma (INS-1) cells that express rat placental lactogen II (rPLII) constitutively in culture. We used this cell line (Ins-rPLII) to examine the effects of endogenous rPLII on β-cell growth, islet formation, and the expression of glucose transporter 2 (glut-2) and insulin mRNA. Growth and maturation of Ins-rPLII cells were compared with that of cells transfected stably with an empty expression plasmid (control) and of INS-1 cells treated with exogenous prolactin. The Ins-rPLII cells proliferated more rapidly than control cells in serum-free medium and showed distinct morphologic characteristics in culture. Whereas the control cells flattened readily on plastic and formed a branching monolayer, the Ins-rPLII cells remained more rounded, sent out fewer projections, and formed more numerous (p < 0.01) and larger (p < 0.01) β-cell clusters. Larger clusters assumed a spherical form with well-delineated smooth borders and detached more readily from the culture plates. Maturational progression of the Ins-rPLII cells was associated with a 40% increase in preproinsulin mRNA (p < 0.05) and a 2–3-fold increase in glut-2 mRNA (p < 0.01). Induction of glut-2 mRNA was accompanied by a 1.4–2.4-fold increase (p < 0.01) in the uptake of radiolabeled 2-deoxyglucose. Similar effects were observed in INS-1 cells exposed for 48 h to exogenous prolactin. These findings suggest novel roles for the lactogenic hormones in the maturation and growth of pancreatic islets. Lactogen induction of β-cell aggregation coupled with localized β-cell growth may contribute to the expansion of islet mass that occurs in pregnancy and during the perinatal period. The induction of insulin and glut-2 mRNA provides a mechanism by which the lactogens may increase fetal and maternal insulin production and enhance the sensitivity of the pancreas to glucose.
Similar content being viewed by others
Main
The lactogenic hormones placental lactogen (PL) and PRL stimulate DNA synthesis, insulin production, and glucose-dependent insulin secretion in the pancreatic islets of fetal and neonatal rats and mice and human adults (1–9). These actions are mediated through the binding of the hormones to the PRLR. Recent studies of the ontogenesis of pancreatic PRLRs reveal striking changes in receptor expression and distribution during development. In the human fetus and fetal rat and mouse, the PRLR is expressed initially in pancreatic acinar cells and ductular epithelial cells (10, 11). Subsequently, in late gestation and in the postnatal period, the receptor is detected in budding islet cells and in differentiated islets, colocalizing with insulin (12). The advent of PRLR expression in the pancreatic islets during the perinatal period coincides with increases in islet number, β-cell mass, and pancreatic insulin content and with the emergence of glucose-dependent insulin secretion (13, 14). These findings suggest that PL and PRL may play roles in islet differentiation, maturation, and growth.
To explore the roles of the lactogenic hormones in islet maturation and growth, we developed a novel experimental model in which PL is expressed constitutively in pancreatic β cells in culture. The model uses INS-1 cells, a line of differentiated pancreatic β cells derived from a rat insulinoma (15). INS-1 cells express PRLRs (15) and proliferate in response to PRL and hGH (7, 9, 16, 17) and, thus, provide a useful paradigm for the study of lactogen action. To achieve constitutive expression of PL in β cells in culture, we transfected INS-1 cells with an expression plasmid in which the cDNA encoding rPLII is linked to the rat insulin 1 promoter. The resultant cell line (termed Ins-rPLII) was used to examine the effects of endogenous rPLII secretion on β-cell growth, islet formation, and the expression of glucose transporter 2 (glut-2) and insulin mRNA. Growth and maturation of the Ins-rPLII cells were compared with that of cells transfected with an empty expression plasmid and of untransfected INS-1 cells treated with exogenous PRL.
METHODS
Establishment of cell lines.
Rat INS-1 cells were kindly provided by Dr. Maryam Asfari (INSERM, Paris). The cells were maintained at 37°C, 5% CO2 in RPMI 1640 media (11.1 mM glucose; Life Technologies, Grand Island, NY) supplemented with 10% FCS, 50 μM 2-mercaptoethanol, 1 mM pyruvate, 10 mM HEPES pH 7, and a 1% antibiotic-antimycotic solution (complete medium).
To generate an islet cell line that expresses rPLII constitutively in culture, we first isolated a fragment of DNA containing 383 bp of the rat insulin 1 promoter and the first exon and intron and the first 11 bp of the second exon of the rat insulin 1 gene [which precede the initiator methionine (18)]. This DNA fragment was cloned upstream of the rPLII cDNA [generous gift from Drs. May Robertson and Mary Lynn Duckworth, University of Manitoba (19)]. This gene fusion (Fig. 1) was cloned into an expression plasmid (pCR3, In Vitrogen, Carlsbad, CA) that confers G418 resistance. The resulting plasmid was linearized upstream of the insulin promoter and transfected into INS-1 cells by electroporation using a gene pulser (Bio-Rad) set at 270 mV, 960 μF, and infinite resistance. Control cells were transfected with an empty expression plasmid (pCIneo, Promega, Madison, WI) that, like the plasmid containing the insulin promoter-rPLII construct, has a neomycin resistance marker driven by an SV40 promoter. The biologic behavior of the control cells as assessed by cell growth, morphology, and gene expression was similar or identical to that of nontransfected INS-1 cells.
The transfected cells were subsequently grown in complete medium supplemented with 0.5 mg/mL G418 (Life Technologies, Gaithersburg, MD), resulting in the generation of two stably integrated cell lines that we designate Ins-rPLII and control. It should be noted that each cell line represents a population of neomycin-resistant cells; no clonal lines were examined. Nevertheless, all of the neomycin-resistant cells that had been stably transfected with the Ins-rPLII plasmid expressed immunoreactive rPLII (see below).
Northern analyses.
Total RNA was extracted from tissue culture cells by using Tri Reagent (Molecular Research Center, Inc., Cincinnati, OH) according to the manufacturer's protocol. Twenty micrograms of total RNA was electrophoresed in denaturing agarose gels and transferred onto nylon membranes. The cDNA probe for rat preproinsulin-I [(18) kindly provided by Dr. Roger Liddle, Duke University] was a 700-bp Eco RI/ Bam HI fragment containing the entire coding sequence for the peptide. The probe for rat glut-2 [(20) kindly provided by Graeme Bell, University of Chicago] was a 1.5-kb Eco RI fragment containing bases 105–1648 of the glut-2 cDNA. The cDNA probes were labeled with digoxigenin by using the high prime kit (Boehringer Mannheim).
Hybridizations were performed at 60°C overnight in 5X SSC, 0.1%N-lauroylsarcosine, 0.02% SDS, and 1% blocking reagent (Boehringer Mannheim). The membranes were washed at 60°C sequentially in 1) 2 × SSC, 0.1% SDS;2) 0.5 × SSC (750 mM sodium chloride, 75 mM sodium citrate), 0.1% SDS;3) 0.1 × SSC, 0.1% SDS; and 4) malate buffer. The membranes were treated with blocking reagent for 1 h and then incubated with alkaline phosphatase-labeled anti-DIG (digoxigenin) (1:5000) for 30 min. After three malate buffer washes, the hybridization of the digoxigenin-labeled probes was detected by chemiluminescence using 10 μg/mL CSPD (Tropix) in a solution containing 100 mM Tris-HCl pH 9.5, 100 mM NaCl, and 1 mM MgCl2, followed by exposure of the membranes to hyperfilm ECL (Amersham) for 5–30 min. The films and the corresponding ethidium-bromide–stained gels were scanned using an ARCUS II scanner (AGFA). The images were processed for densitometric analysis by using the National Institutes of Health image program from Scion Corporation. The levels of mRNA estimated by densitometric analysis of Northern blots were normalized for the amounts of total RNA loaded on the gels by calculating the ratio of specific mRNA to the corresponding amount of total RNA assessed by ethidium bromide (EtBr) staining. This method was found to be as or more reliable than normalizing for the signal generated by hybridization with a probe for cyclophilin (21).
Western analyses.
Concentrated conditioned media were analyzed by SDS-PAGE according to the method of Laemmli (22). The proteins were transferred to nitrocellulose membranes and probed with a polyclonal antibody (1 μg of protein/mL) raised against rPLII [(23) kindly provided by Drs. May Robertson and Mary Lynn Duckworth, University of Manitoba]. After treatment of the membranes with a horseradish peroxidase-conjugated secondary antibody, the signal was visualized using the ECL detection system (Amersham).
Immunohistochemistry.
Immunohistochemical staining was performed using methods described previously (10, 11). Transfected Ins-rPLII and control cells were washed three times with cold PBS and fixed in 4% paraformaldehyde (in PBS) for 10 min at room temperature. The cells were then washed extensively with PBS and treated with 1% hydrogen peroxide in methanol for 5 min at room temperature and washed an additional five times with PBS. The cells were then incubated for 1 h at room temperature with PBS containing 5% nonfat milk and 4% horse serum; then the cells were incubated overnight at 4°C with anti-rPLII antisera (1 μg/mL) or rabbit IgG in PBS/2% horse serum. After the overnight incubation, the cells were washed extensively with cold PBS and then were incubated for 30 min with a peroxidase-labeled anti-rabbit IgG (1:1000, Amersham) in PBS/2% horse serum. After a 2-h incubation at room temperature, the cells were washed extensively and incubated with diaminobenzidine hydrochloride (200 μg/mL in a solution of 50 mM Tris pH 7.5, and 0.006% H2O2) for 5–10 min at room temperature in the dark.
Cell proliferation assays.
The lactogen-dependent Nb2 lymphoma cell line (24) was kindly provided by Dr. Charles Clevenger (University of Pennsylvania). Nb2 lymphoma cells were passaged in Fisher's medium containing 10% FCS and 10% horse serum. Proliferation of the Nb2 cells and the Ins-rPLII and control cells was measured using the Cell Titer 96 Aqueous Nonradioactive Cell Proliferation Assay (Promega, Madison, WI) according to the manufacturer's protocol.
Morphologic analysis of cells in culture.
To analyze the morphology of the Ins-rPLII and control cells in culture, we plated 105 cells/well in six-well (9 cm2) dishes. The cells were photographed at ×40–400 magnification at various periods of time after plating in complete medium. The aggregation of cells in culture was quantified by two observers working independently. All the cell clusters within six individual wells were counted. A small cluster was defined as an aggregate that measured 5–15 μM in diameter, whereas a large cluster exceeded 15 μM in diameter. In subsequent experiments that examined the effects of exogenous PRL on cluster formation in INS-1 cells growing in monolayer, a small cluster was defined as an aggregate that measured <5 μM in diameter, whereas a large cluster was defined as an aggregate that measured >8 μM in diameter.
Glucose transport assay.
The Ins-rPLII and control cells were washed with PBS and preincubated for 48 h in basal medium (DMEM, 5.5 mM glucose supplemented with 0.1% human serum albumin, 10 μg/mL transferrin, 0.1 nM T3, 50 μM ethanolamine, 50 μM phosphoethanolamine, and an antibiotic/antimycotic solution). The cells were then washed twice and incubated for 30 min at 37°C in glucose-free PBS containing 1% BSA. After two additional washes with PBS, the cells were incubated with 2-deoxy-D-[3H]glucose (1 uCi/mL; Amersham Life Science, Elk Grove, IL) at room temperature for 1, 2, 4, or 16 min. Other cells were incubated with 2-deoxy-D-[3H]glucose in the presence of unlabeled 2-deoxyglucose (Sigma Chemical Co., St. Louis, MO), which was added in 10 000-fold excess to block specific uptake of the labeled 2-deoxyglucose. The uptake of radiolabeled glucose was terminated by washing the cells rapidly with ice-cold PBS containing 0.2 mM phloretin (Sigma Chemical Co.). The cells were solubilized in 0.1% SDS, and aliquots were counted and assayed for protein content by using the Bio-Rad protein assay (Bio-Rad Labs, Richmond, CA). Counts obtained in the presence of excess 2-deoxyglucose were subtracted from those obtained in its absence to quantify specific uptake of the radiolabeled glucose.
Statistical analyses.
Data are presented as the mean ± SE. The levels of mRNA estimated by densitometric analysis of Northern blots were normalized for the amounts of total RNA loaded on the gels by calculating the ratio of specific mRNA to the corresponding amount of total RNA assessed by EtBr staining. Each experiment was repeated at least twice with duplicate or triplicate values within each group. The statistical differences between sample means were tested by ANOVA, followed by the Newman-Keuls test. A p value <0.05 was considered statistically significant.
RESULTS
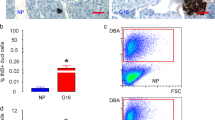
Our initial investigations showed that the rPLII cDNA was expressed by the Ins-rPLII cells in culture. Messenger RNA encoding rPLII was detected in samples of total RNA prepared from Ins-rPLII cells but not from control cells (Fig. 2). Immunohistochemical analysis revealed that all of the Ins-rPLII cells expressed rPLII, albeit at variable levels (not shown). The variable expression may result in part from position-effect variegation in the integration sites of the transfected DNA. Western analysis of cellular conditioned media indicated that the rPLII was secreted from the Ins-rPLII cells (Fig. 2). The rPLII secreted by the Ins-rPLII cells was biologically active, as Ins-rPLII–conditioned media induced cell proliferation of the lactogen-dependent Nb2 lymphoma cell line (Fig. 3).
Expression and secretion of rPLII in the Ins-rPLII cell line. Ins-rPLII and control cells were plated at equivalent densities in serum-containing medium. After 48 h in culture, selected cells were processed for the extraction of total RNA. For the Northern analysis, 20-μg aliquots of total RNA were electrophoresed on denaturing agarose gels, transferred to nitrocellulose membranes, and hybridized with a 0.8-kb digoxigenin-labeled rPLII cDNA probe. For the Western analysis, the cells were washed and incubated for 48 h in serum-free basal medium. Aliquots of cellular conditioned media containing 20 μg of protein were electrophoresed on polyacrylamide gels under reducing conditions, transferred to nitrocellulose, and probed with a polyclonal antibody to rPLII.
Lactogen induction of Nb2 lymphoma cell growth. Ins-rPLII and control cells were plated at equivalent densities in serum-containing medium. After 48 h in culture, the cells were washed and incubated for an additional 48 h in serum-free medium. Fifty-microliter aliquots of the cellular conditioned media were then added to aliquots of Nb2 lymphoma cells (20 000 cells) in a final volume of 100 μL. Cell number was quantified after an additional 48-h incubation. The effects of the conditioned media of Ins-rPLII and control cells were compared with the effects of PRL and of serum-free RPMI culture medium alone.
A comparison of the two cell lines revealed that the Ins-rPLII cells proliferated more rapidly than control cells in serum-free media. Aliquots (20 000 cells) of each line were plated in 96-well dishes and grown for 48 h in serum-containing media; the cells were then washed and incubated in serum-free basal medium for an additional 48 h. During the initial 48 h in serum-containing medium, the two cell lines grew at equivalent rates. However, after 48 h in serum-free medium, the control cells declined slightly in number (−5.5 ± 4.6%, n = 5, p > 0.05) over the next 48 h, whereas the number of Ins-rPLII cells increased by 22 ± 2.9% (n = 5, p < 0.01).
The two cell lines also differed strikingly in their morphologic characteristics and behavior under the experimental culture conditions used. Within the first 24 h after plating in serum-containing media, the control cells had begun to flatten and form projections or spicules (Fig. 4). In contrast, the Ins-rPLII cells remained more rounded, aggregated in clumps, established few projections, and adhered less well to the tissue culture plastic.
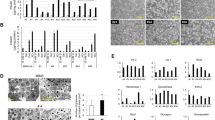
Microscopic analysis of cell morphology. The Ins-rPLII and control cells were plated at equivalent densities and grown in serum-containing medium. Photographs at 48 h were taken at ×100 magnification. The photographs at 96 h were shot at lower power (×40). Note the flattening of the control cells at 48 h, the presence of cellular projections and spicules (arrow), and the generation of a branching monolayer. In contrast, the Ins-rPLII cells aggregate in clumps, display fewer projections and spicules, and form an incomplete monolayer even after 96 h in culture. The larger clumps of Ins-rPLII cells assume a spherical form with well-delineated smooth borders and detach more readily from the tissue culture plate.
During the next 2 to 3 d, the control cells formed an extensive branching network, generating a monolayer interspersed with small aggregates of cells. In contrast, the Ins-rPLII cells remained more rounded, sent out fewer projections, and formed more numerous and larger β-cell clusters. The Ins-rPLII cells generated a 3-fold increase in small (5–15 μM) β-cell clusters and a 10–15-fold increase in large (>15 μM) β-cell clusters (Fig. 5) after 48–72 h in complete medium (p < 0.01). After 4 d in culture, the larger β-cell clusters assumed a spherical form with well-delineated smooth borders. These clusters tended to detach from the tissue culture plate and float freely in the media. Thus, the rate of maturation of these islet-like clusters was enhanced significantly in the Ins-rPLII cell line.
This maturational progression was accompanied by the induction of expression of specific β-cell genes. There was a 40% increase in the levels of preproinsulin mRNA (p < 0.05) and a 2–3-fold increase in levels of mRNA encoding glut-2 (Fig. 6, p < 0.01). Induction of glut-2 mRNA was accompanied by an increase in the number of cellular glucose transporters as shown by an increase in the uptake of radiolabeled 2-deoxyglucose (Fig. 7).
Expression of glut-2 and insulin mRNA in Ins-rPLII and control cells. The cells were grown in serum-containing medium for 48 h, washed, and incubated for an additional 48 h in serum-free medium. Twenty-microgram aliquots of total RNA were electrophoresed on agarose gels, transferred to nylon membranes, and hybridized with digoxigenin-labeled cDNA probes encoding glut-2 or preproinsulin. The levels of mRNA estimated by densitometric analysis of Northern blots were normalized for the amounts of total RNA loaded on the gels by calculating the ratio of specific mRNA to the corresponding amount of total RNA assessed by EtBr staining. ★p < 0.05, ★★p < 0.01.
Glucose transport in Ins-rPLII and control cells. Ins-rPLII and control cells were grown to 80% confluence in serum-containing medium. The cells were then washed extensively and incubated at room temperature in PBS containing radiolabeled 2-deoxyglucose. The specific uptake of radiolabeled 2-deoxyglucose, shown in the Figure, was calculated as the total uptake minus the nonspecific uptake measured in the presence of a 10 000-fold excess of unlabeled 2-deoxyglucose.
The differences in morphology and function of the two cell lines most likely reflect the constitutive expression of rPLII because these properties are manifest in INS-1 cells exposed chronically to the lactogenic hormone PRL. PRL (1 μg/mL) stimulated a 2.7-fold increase in large (>8 μM) β-cell clusters (control: 10.0 ± 0.3 clusters per well, n = 5; PRL: 27.1 ± 1.4 clusters per well, n = 5, p < 0.01) and, as shown in Figure 8, a 2–3-fold increase in preproinsulin mRNA (p < 0.01) and glut-2 mRNA (p < 0.05).
Effects of exogenous PRL on the expression of insulin and glut-2 mRNA in native INS-1 cells. INS-1 cells were grown to 80% confluence in serum-containing medium. The cells were then washed and incubated for an additional 48 h in serum-free medium in the presence (+) or absence (−) of PRL (1 μg/mL). Twenty-microgram aliquots of total RNA were electrophoresed on agarose gels, transferred to nylon membranes, and hybridized to probes encoding the cDNA for preproinsulin or glut-2. The levels of mRNA estimated by densitometric analysis of Northern blots were normalized for the amounts of total RNA loaded on the gels by calculating the ratio of specific mRNA to the corresponding amount of total RNA assessed by EtBr staining. ★p < 0.01.
DISCUSSION
Despite extensive investigation, the factors controlling the production and secretion of insulin in the fetus remain poorly understood (13, 14, 25). The insulin gene is expressed as early as 8 wk of gestation in the human embryo and 11–12 d of gestation in the embryonic mouse and rat. However, fetal pancreatic insulin production and fetal plasma insulin concentrations remain low throughout midpregnancy and fail to respond to glucose, the primary determinant of insulin production during postnatal life. In contrast, the pancreas secretes insulin acutely in response to amino acids and glucagon early in development.
Beginning on d 15–16 in the fetal mouse or d 17.5 in the fetal rat, pancreatic β cells arising from ductal epithelial cells proliferate rapidly, bud from the ductal wall, and aggregate to form differentiated islets (14, 25). Between d 18 and 21 of gestation in the fetal rat, insulin gene expression and pancreatic insulin content increase 100-fold or more, and fetal plasma insulin concentrations increase by 8–10-fold. Glucose-sensitive islet cell DNA replication and insulin production emerge between d 20 and 22, just before delivery (13, 14). The pattern is similar in the human fetus in which pancreatic insulin content increases 8–10-fold between 16 and 36 wk of gestation and in which the insulin response to glucose is minimal before the third trimester (14). The rates of islet formation and growth decline markedly in the weeks after birth and cease shortly after weaning, and the fully differentiated pancreatic islet has low levels of cell turnover and regenerative capacity.
What triggers the proliferation of pancreatic β cells, the dramatic increase in insulin production, and the emergence of glucose-dependent insulin secretion during the perinatal period? Growth factors such as transforming growth factor-alpha (TGF-α), epidermal growth factor (EGF), and IGF-I stimulate ductal epithelial proliferation in postnatal rats but have no effects on islet mass or insulin gene expression (26, 27). Similarly, thyroid hormone, glucocorticoids, and the sex steroids have no effects on or may reduce islet cell insulin production (5, 28–31). In contrast, the lactogens PL and PRL have profound effects on β-cell growth and function. Circulating in fetal as well as maternal plasma (32–34), PL and PRL stimulate the production of insulin in human fetal pancreatic fragments and induce β-cell replication, insulin biosynthesis, and glucose-dependent insulin secretion in isolated islets from fetal and neonatal rats and mice and human adults (1–9). In postnatal and pregnant rats and mice, PL and PRL stimulate β-cell hyperplasia and increase pancreatic insulin content and the insulin secretory response to glucose (1–9, 35, 36). In gestational diabetes, increases in placental size and secretion of PL (37–40) are accompanied by fetal hyperinsulinemia and premature induction of glucose-dependent insulin secretion (13). Conversely, PRL- and GH-deficient Snell and Ames dwarf mice and hypophysectomized rats have reduced islet cell mass and an impaired insulin secretory response to glucose (41–43). Moreover, hypoprolactinemia and GH deficiency in patients with pituitary aplasia are accompanied by hypoinsulinemia and peripheral hypersensitivity to insulin (44). Like PL and PRL, GH stimulates β-cell proliferation and insulin. However, GH is considerably less potent than the lactogenic hormones in parallel experiments (2–4).
The results of the present study add a new and novel dimension to the biologic actions of lactogens in pancreatic islets. Constitutive expression of rPLII, the predominant lactogen in the mid-late gestational pregnant and fetal rat (32, 33), leads to aggregation and localized overgrowth of INS-1 cells. Relative to native INS-1 cells, the rPLII-secreting INS-1 cells adhere less tenaciously to plastic, have truncated branching and spicule formation, form an incomplete cell monolayer, and generate more numerous and larger β-cell clusters. This induction of islet maturation by rPLII is associated with higher rates of insulin and glut-2 expression and cellular glucose transport. Chronic treatment of native INS-1 cells with exogenous PRL produces similar effects, indicating that the behavior of Ins-rPLII cells results from endogenous production of rPLII.
The cellular mechanisms by which PL induces β-cell aggregation are currently unclear. A possible mechanism may include lactogen effects on the expression of cellular adhesion molecules. Recent findings provide support for this hypothesis: the induction by PRL of thymocyte adhesion to thymic epithelial cells is blocked by antisera to fibronectin or laminin (45), and laminin-1 promotes the differentiation of pancreatic β cells from precursor cells in the fetal pancreas (46). Alternatively, PL itself, through binding to PRLR on the surfaces of adjacent cells, may serve as a link between cells to enhance cell-cell interactions. However, acute (1 h) exposure of native INS-1 cells to PRL does not induce obvious cellular aggregation (our unpublished observations).
Of potential relevance is a recent study that showed that lactogenic hormones induce the expression of preadipocyte factor-1 (Pref-1) in neonatal rat islets (47). Pref-1 is a transmembrane protein that contains six EGF-like extracellular domains. Through its binding to a notch-like receptor protein, Pref-1 is thought to function as an antidifferentiation factor, maintaining tissues in a proliferative state (48). Induction of Pref-1 by rPLII in the Ins-rPLII cells may enhance the rate of cellular proliferation, leading to localized overgrowth. Whether or not Pref-1 contributes to the morphologic and functional changes in the Ins-rPLII cells in culture or to their accelerated rate of islet formation is unclear.
The induction of glut-2 and cellular glucose uptake by lactogenic hormones is of interest. Glut-2 is the predominant glucose transport protein in normal β cells and in INS-1 cells and, as demonstrated in glut-2 deficient mice (49), is essential for normal glucose-dependent insulin production and secretion in the perinatal and postnatal periods. The transporter may be of less importance in early- and mid-gestation, when glut-2 protein levels are low and fetal pancreatic insulin production and β-cell replication respond poorly to glucose. Glut-2 protein levels increase significantly during the perinatal period (50–52), coinciding with the emergence of glucose sensitivity. Pancreatic glut-2 expression also increases during pregnancy (53), accompanied by increases in β-cell mass and pancreatic insulin content and an augmented insulin secretory response to glucose.
The common thread that binds pancreatic maturation to pregnancy and to perinatal development may be the induction of PRLR in pancreatic β cells. The expression of pancreatic PRLR mRNA and lactogenic-binding activity increase between d 18 and 22 in the fetal rat (10, 34), and PRLR immunoreactivity in maternal pancreatic islets increases in mid-late gestation (12). In the fetus and the pregnant mother, the pancreatic PRLR is expressed predominantly as the long isoform (16, 21), which activates the Jak-Stat pathway and transduces the biologic signals of lactogenic hormones in target tissues (54). Thus, the induction of pancreatic PRLR in late gestation provides a mechanism by which lactogens may increase fetal and maternal insulin production, glut-2 expression, and pancreatic sensitivity to glucose. Lactogen induction of β-cell aggregation coupled with localized β-cell growth may contribute to the expansion of islet mass that occurs in pregnancy and during the perinatal period.
In summary, constitutive expression of rPLII in INS-1 cells leads to cellular aggregation, islet cluster formation, cellular glucose uptake, and the induction of preproinsulin and glut-2 mRNA. These findings implicate novel roles for the lactogenic hormones in the maturation and growth of pancreatic islets.
Abbreviations
- PRL:
-
prolactin
- PRLR:
-
prolactin receptor
- rPLII:
-
rat placental lactogen II
References
Sorenson RL, Johnson MG, Parsons JA, Sheridan JD 1987 Decreased glucose stimulation threshold, enhanced insulin secretion, and increased beta cell coupling in prolactin-treated rats. Pancreas 2: 283–288.
Swenne I, Hill DJ, Strain AJ, Milner RDG 1987 Effects of human placental lactogen and growth hormone on the production of insulin and somatomedin C/insulin-like growth factor I by human fetal pancreas in tissue culture. J Endocrinol 113: 297–303.
Brelje TC, Sorenson RL 1991 Role of prolactin versus growth hormone on islet β-cell proliferation in vitro : implications for pregnancy. Endocrinology 128: 45–57.
Brelje TC, Scharp DW, Lacy PE, Ogren L, Talamantes F, Robertson M, Friesen HG, Sorenson RL 1993 Effects of homologous placental lactogens, prolactins, and growth hormones on islet beta cell division and insulin secretion in rat, mouse, and human islets: implication for placental lactogen regulation of islet function during pregnancy. Endocrinology 132: 870–887.
Sorenson RL, Brelje TC, Roth C 1993 Effects of steroid and lactogenic hormones on islets of Langerhans: a new hypothesis for the role of pregnancy steroids in the adaptation of islets to pregnancy. Endocrinology 133: 2227–2234.
Brelje TC, Parsons JA, Sorenson RL 1994 Regulation of islet beta cell proliferation by prolactin in rat islets. Diabetes 43: 263–273.
Sekine N, Ullrich S, Regazzi R, Pralong WF, Wollheim CB 1996 Postreceptor signaling of growth hormone and prolactin and their effects in the differentiated insulin-secreting cell line, INS-1. Endocrinology 137: 1841–1850.
Kawai M, Kishi K 1997 In vitro studies of the stimulation of insulin secretion and beta cell proliferation by rat placental lactogen II during pregnancy in rats. J Reprod Fertil 109: 145–152.
Stout LE, Svensson AM, Sorenson RL 1997 Prolactin regulation of islet-derived INS-1 cells: characteristics and immunocytochemical analysis of STAT5 translocation. Endocrinology 138: 1592–1603.
Royster M, Driscoll P, Kelly PA, Freemark M 1995 The prolactin receptor in the fetal rat: cellular localization of messenger RNA, immunoreactive protein, and ligand-binding activity and induction of expression in late gestation. Endocrinology 136: 3892–3900.
Freemark M, Driscoll P, Maaskant R, Petryk A, Kelly PA 1997 Ontogenesis of prolactin receptors in the human fetus in early gestation: implications for tissue differentiation and development. J Clin Invest 99: 1107–1117.
Sorenson Rl, Stout LE 1995 Prolactin receptors and JAK 2 in islets of Langerhans: an immunohistochemical analysis. Endocrinology 136: 4092–4098.
Asplund K, Andersson A, Jarrousse C, Hellerstrom C 1975 Function of the fetal endocrine pancreas. Israel J Med Sci 11: 581–590.
Sperling MA 1994 Carbohydrate metabolism: insulin and glucagon. In: Tulchinsky D, Little AB (eds) Maternal and Fetal Endocrinology. Saunders, Philadelphia, 379–400.
Asfari M, Janjic D, Meda P, Li G, Halban PA, Wollheim CB 1992 Establishment of 2-mercaptoethanol-dependent differentiated insulin-secreting cell lines. Endocrinology 130: 167–178.
Asfari M, De W, Postel-Vinay MC, Czernichow P 1995 Expression and regulation of growth hormone and prolactin receptors in a rat insulin-producing cell line (INS-1). Mol Cell Endocrinol 107: 209–214.
De W, Breant B, Czernichow P, Asfari M 1995 Growth hormone and prolactin regulate IGFBP-3 gene expression in rat beta cells. Mol Cell Endocrinol 114: 43–50.
Soares MB, Schon E, Henderson A, Karathanasis SK, Cate R, Zeitlin S, Chirgwin JM, Efstratiadis A 1985 RNA-mediated duplication: the rat preproinsulin I gene is a functional retroposon. Mol Cell Biol 5: 2090–2103.
Duckworth ML, Kirk KL, Friesen HG 1986 Isolation and identification of a cDNA clone of rat placental lactogen II. J Biol Chem 261: 10871–10878.
Ahn YH, Kim JW, Han GS, Lee BG, Kim YS 1995 Cloning and characterization of rat pancreatic beta-cell/liver-type glucose transporter gene: a unique exon/intron organization. Arch Biochem Biophys 323: 38
Freemark M, Nagano M, Edery M, Kelly PA 1994 Prolactin receptor gene expression in the fetal rat. J Endocrinol 144: 285–292.
Laemmli UK 1970 Cleavage of a structural protein during the assembly of the head of bacteriophage T. Nature 227: 680–685.
Robertson MC, Gillespie B, Friesen HG 1982 Characterization of the two forms of rat placental lactogen: rPL-I and rPL-II. Endocrinology 111: 1862–1866.
Tanaka T, Shiu RPC, Gout PW, Beer CT, Noble RL, Friesen HG 1980 A new sensitive and specific bioassay for lactogenic hormones: measurement of prolactin and growth hormone in human serum. J Clin Endocrinol Metab 51: 1058–1063.
Hellerstrom C, Swenne I 1991 Functional maturation and proliferation of fetal pancreatic beta cells. Diabetes 40: 89–93.
Swenne I, Heldin CH, Hill DJ, Hellerstrom C 1988 Effects of PDGF and IGF-I on the DNA replication of fetal rat islets of Langerhans in tissue culture. Endocrinology 122: 214–218.
Bockman DE, Merlino G 1992 Cytological changes in the pancreas of transgenic mice overexpressing transforming growth factor alpha. Gastroenterology 103: 1883–1892.
Swenne I 1985 Glucose-stimulated DNA replication of the pancreatic islets during the development of the rat fetus. Diabetes 34: 803–807.
Swenne I 1983 Hypothyroidism in the fetal and neonatal rat does not impair the insulin secretory response to glucose. Life Sci 33: 2207–2211.
Karlsson MG, Eriksson UJ, Swenne I 1990 Perinatal hypoadrenalism in the rat does not alter glucose tolerance and insulin secretory response to glucose. Ups J Med Sci 95: 147–155.
McEvoy RC, Hegre OD 1976 Foetal rat pancreas in organ culture: effects of media supplementation with various steroid hormones on the acinar and islet components. Differentiation 6: 105–111.
Ogren L, Talamantes F 1988 Prolactins of pregnancy and their cellular source. Int Rev Cytol 112: 1–65.
Freemark M, Kirk K, Pihoker C, Robertson MC, Shiu RPC, Driscoll P 1993 Pregnancy lactogens in the rat conceptus and fetus: circulating levels, distribution of binding, and expression of receptor mRNA. Endocrinology 133: 1830–1842.
Freemark M 1999 The roles of growth hormone, prolactin, and placental lactogen in human fetal development. Critical analysis of molecular, cellular, and clinical investigations. In: Handwerger S (ed) Molecular and Cellular Pediatric Endocrinology. Humana, Totowa, NJ, 57–83.
Sorenson RL, Parsons JA 1985 Insulin secretion in mammosomatotropic tumor-bearing and pregnant rats: a role for lactogens. Diabetes 34: 337–341.
Parsons JA, Brelje TC, Sorenson RL 1992 Adaptation of islets of Langerhans to pregnancy: increased islet cell proliferation and insulin secretion correlates with the onset of placental lactogen secretion. Endocrinology 130: 1459–1466.
Laurini RN, Visser GHA, Van Ballegooie E, Schoots CJF 1987 Morphological findings in placentae of insulin-dependent diabetic patients treated with continuous subcutaneous insulin infusion. Placenta 8: 153–165.
Mills NC, Gyves MT, Ilan J 1985 Comparisons of human placental mRNA levels from placentas of diabetics and normal term. Mol Cell Endocrinol 39: 61–69.
Gillmer MDG, Beard RW, Oakley NW 1977 Plasma human placental lactogen profiles over 24 hours in normal and diabetic pregnancy. Br J Obstet Gynaecol 84: 197–204.
Lopez-Espinoza I, Smith RF, Gillmer M, Schildmeir A, Hockaday TDR 1986 High levels of growth hormone and human placental lactogen in pregnancy complicated by diabetes. Diabetes Res 3: 119–125.
Parsons JA, Bartke A, Sorenson RL 1995 Number and size of islets of Langerhans in pregnant, human growth hormone-expressing transgenic and pituitary dwarf mice: effect of lactogenic hormones. Endocrinology 136: 2013–2021.
Pierluissi J, Pierluissi R, Ashcroft SJH 1982 Effects of hypophysectomy and growth hormone on cultured islets of Langerhans of the rat. Diabetologia 22: 134–137.
Cavallero C, Dova E 1954 Morphological changes in the islets of Langerhans of the pituitary dwarf mice during induced growth. Acta Pathol Microbiol Scand 34: 201–207.
Gluckman PD 1986 The role of pituitary hormones, growth factors and insulin in the regulation of fetal growth. Ox Rev Reprod Biol 8: 1–60.
de Mello-Coelho V, Villa-Verde DM, Dardenne M, Savino W 1997 Pituitary hormones modulate cell-cell interactions between thymocytes and thymic epithelial cells. J Neuroimmunol 76: 39–49.
Jiang FX, Cram DS, DeAizpurua HJ, Harrison LC 1999 Laminin-1 promotes differentiation of fetal mouse pancreatic beta cells. Diabetes 48: 722–730.
Carlsson C, Tornehave D, Lindberg K, Galante P, Billestrup N, Michelsen B, Larsson LI, Nielsen JH 1997 Growth hormone and prolactin stimulate the expression of rat preadipocyte factor-1/delta-like protein in pancreatic islets: molecular cloning and expression pattern during development and growth of the endocrine pancreas. Endocrinology 138: 3940–3948.
Smas CM, Sul HS 1997 Molecular mechanisms of adipocyte differentiation and inhibitory action of pref-1. Crit Rev Eukaryot Gene Expr 7: 281–298.
Guillam MT, Hummler E, Schaerer E, Yeh JI, Birnbaum MJ, Beermann F, Schmidt A, Deriaz N, Thorens B 1997 Early diabetes and abnormal postnatal pancreatic islet development in mice lacking Glut-2. Nat Genet 17: 327–330.
Hughes SJ 1994 The role of reduced glucose transporter content and glucose metabolism in the immature secretory responses of fetal rat pancreatic islets. Diabetologia 37: 134–140.
Weinhaus AJ, Poronnik P, Cook DI, Tuch BE 1995 Insulin secretagogues, but not glucose, stimulate an increase in Ca2+ in the fetal rat beta cell. Diabetes 44: 118–124.
Tiedge M, Lenzen S 1993 Differential regulation of glucokinase and GLUT 2 glucose transporter gene expression in pancreas and liver from neonatal and 16-day-old rats. Biochem Mol Biol Int 29: 161–166.
Weinhaus AJ, Stout LE, Sorenson RL 1996 Glucokinase, hexokinase, glucose transporter 2, and glucose metabolism in islets during pregnancy and prolactin-treated islets in vitro : mechanisms for long-term up-regulation of islets. Endocrinology 137: 1640–1649.
Bole-Feysot C, Goffin V, Edery M, Binart N, Kelly PA 1998 Prolactin and its receptor: actions, signal transduction pathways, and phenotypes observed in prolactin receptor knockout mice. Endocrinol Rev 19: 225–268.
Author information
Authors and Affiliations
Additional information
Supported by grants from the National Institute for Child Health and Development (National Institutes of Health HD24192), Juvenile Diabetes Foundation (196029), and the Eli Lilly and Genentech Corporations.
Rights and permissions
About this article
Cite this article
Fleenor, D., Petryk, A., Driscoll, P. et al. Constitutive Expression of Placental Lactogen in Pancreatic β Cells: Effects on Cell Morphology, Growth, and Gene Expression. Pediatr Res 47, 136 (2000). https://doi.org/10.1203/00006450-200001000-00023
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200001000-00023
This article is cited by
-
Knockdown of prolactin receptors in a pancreatic beta cell line: effects on DNA synthesis, apoptosis, and gene expression
Endocrine (2014)
-
Tobacco as biofactory for biologically active hPL production: a human hormone with potential applications in type-1 diabetes
Transgenic Research (2011)
-
Effects of lactogen resistance and GH deficiency on mouse metabolism: pancreatic hormones, adipocytokines, and expression of adiponectin and insulin receptors
Endocrine (2007)
-
Glucose regulates LXRα subcellular localization and function in rat pancreatic β-cells
Cell Research (2006)