Abstract
Children treated for acute lymphoblastic leukemia may develop reduced bone mineral density during treatment, but there is little information on the mechanisms involved. In a prospective, longitudinal study on 15 children with ALL, we undertook serial measurements of markers of bone and collagen turnover, insulin-like growth factor (IGF)-I and its binding proteins (IGFBPs)-3 and -2 during the second year of continuing chemotherapy. In eight patients we also measured lower leg length by knemometry. Height SD scores, lower leg length velocity, IGF-I, and markers of bone collagen turnover did not differ significantly from healthy children. However, bone alkaline phosphatase, a marker of the differentiated osteoblast, was lower (mean SD score, −0.64;p < 0.0001), whereas procollagen type III N-terminal propeptide (P3NP, a marker of soft tissue collagen turnover; mean SD score, +0.93, p < 0.05), IGFBP-3 (mean SD score, +0.76;p < 0.01), and IGFBP-2 (mean SD score, +1.24, p = 0.01) were all higher than in healthy children. IGFBP-3 decreased during episodes of afebrile neutropenia (p < 0.05). Within 3 mo after completion of treatment, bone ALP increased in all eight patients, but collagen markers showed little change. IGFBP-2 returned to normal posttreatment, but P3NP and IGFBP-3 remained significantly elevated compared with healthy children (mean SD scores, +1.51 and +1.36, respectively;p < 0.01). We conclude that continuing chemotherapy was associated with normal growth and bone collagen turnover but enhanced soft tissue collagen turnover. Bone bone alkaline phosphatase was low throughout treatment, which suggests impaired osteoblast differentiation resulting from a direct effect of chemotherapy on bone. Although the effect was reversible, the long-term implications for bone health in survivors remain uncertain.
Similar content being viewed by others
Main
There have been many reports of poor growth in children with acute lymphoblastic leukemia (ALL), especially during periods of intensive chemotherapy, but growth may return to normal during less-intensive periods and may show evidence of further catch-up after completion of chemotherapy (1–13). Of greater concern are a number of retrospective cross-sectional studies on survivors of ALL that describe reduced bone mineral density (BMD) at various sites (14–16). This may be associated with increased fracture risk, reduced peak bone mass, and a theoretical risk of osteoporosis in adult life. However, these previous studies reflect the outcome of earlier treatment protocols, most of which included cranial irradiation and are now obsolete. Current protocols generally use more intensive chemotherapy regimens but avoid cranial irradiation in all but a few high-risk cases. Recently, a number of prospective longitudinal studies have reported that the prevalence of radiologic osteopenia and fracture in children with ALL increases and that BMD decreases during chemotherapy, in the absence of cranial irradiation (17–19). However, the mechanisms responsible for these observations remain to be elucidated.
There are a number of biochemical markers that may shed light on the dynamic processes of bone turnover and growth (20). Circulating C-terminal propeptide of type I procollagen (PICP) quantitatively reflects type I collagen synthesis, largely arising from bone, although a small proportion may also emanate from soft tissue; in bone, it is a marker of the osteoblast in its early proliferative stage. Bone-specific alkaline phosphatase (ALP) is a marker of the differentiated osteoblast. The C-terminal telopeptide of type I collagen (ICTP) reflects the breakdown of type I collagen largely, although not exclusively, derived from bone. PICP, bone ALP, and ICTP are all released into the circulation during the modeling and elongation of bone that accompanies growth. The N-terminal propeptide of type III procollagen (P3NP) quantitatively reflects type III collagen turnover in soft tissue. All these markers have been demonstrated to reflect changes in growth in children (20). Insulin-like growth factor-I (IGF-I) is an important regulator of bone turnover at tissue level: it enhances osteoblast proliferation and stimulates both type I collagen production and ALP activity (21). Circulating IGF-I is largely bound to IGF binding protein-3 (IGFBP-3), which controls and modulates its tissue bioavailability and may also regulate cell growth directly (22). Both IGF-I and IGFBP-3 are related to growth hormone (GH) secretion, although other factors, such as nutrition, also influence plasma levels. The role of IGFBP-2 is less well understood but may oppose the effects of IGF-I on bone cell proliferation and collagen synthesis (21–23).
Using these markers, we have previously shown that, at diagnosis, children with ALL have reduced bone ALP, PICP, ICTP, IGF-I, and IGFBP-3, together with increased IGFBP-2 and urinary GH, which suggests low bone turnover state caused by the disease itself and possibly associated with GH resistance (24). During the first year of chemotherapy, periods of intensive chemotherapy were associated with further suppression of the markers of collagen turnover, followed by marked increases during periods of less-intensive treatment (24, 25). These changes apparently were not mediated through circulating IGF-I but by direct action of various chemotherapeutic agents on target tissue. Bone ALP showed similar but quantitatively lesser changes and remained below the population mean throughout the first year of chemotherapy.
We now report the effects of a second year of less-intensive continuing chemotherapy on markers of bone and soft tissue turnover and growth in children with ALL. In a subgroup of the children, we were also able to assess the change in markers following completion of chemotherapy. Our aim in this study was to investigate the degree and nature of any adverse effect of continuing chemotherapy on bone and collagen turnover and whether these effects were reversed after cessation of chemotherapy.
METHODS
Patients
We studied 15 children (10 males, 5 females) with ALL during and after their second year of chemotherapy. The children were already enrolled in the national Medical Research Council randomized trial of childhood ALL treatment, which was performed from 1992 to 1997 (UKALL XI-92). All had previously received induction chemotherapy, followed by two periods of intensification chemotherapy, as previously described (24), and all were in first clinical and hematological remission. None had received cranial irradiation. Eight of the children had previously received high-dose i.v. methotrexate as CNS-directed treatment (24). Six children had received an additional third intensification of eight weeks duration before the period studied here, as previously described (25). The median age of the patients was 4.1 yr (range 2–14.9 yr) at the start of the second year of chemotherapy. The oldest boy was postpubertal (bilateral 25mL testes); the remainder were younger than 10 yr and prepubertal. One patient was retrospectively excluded from the study, owing to testicular relapse, diagnosed one month after the last sample was collected. The study was approved by the local ethics committee, and informed consent was obtained from parents and, if possible, the children.
Drug Treatment, Samples, and Measurements
Continuing chemotherapy was administered as previously described (25) and included monthly administrations of vincristine and prednisolone, weekly administrations of oral methotrexate, and daily administrations of mercaptopurine. They were administered in three monthly cycles: we studied the four cycles (cycles 5–8) that comprised the second year of chemotherapy. Height was measured using a stadiometer at the beginning of cycle 5, at completion of chemotherapy and (in 5 children only) 3 mo after completion of chemotherapy. Lower leg length measurements and blood sampling were scheduled to take place at monthly intervals to coincide with the patients' attendance at hospital for vincristine administration. In eight patients, we obtained additional samples 2–3 mo after completion of chemotherapy. Samples were collected between 1100h and 1500h to minimize the effects of circadian variation. Plasma and serum were stored in aliquots at –70°C until analysis.
We measured lower leg length by knemometry in 8 children who were old enough to cooperate; in three of these children we also made serial measurements at monthly intervals during the three month period following completion of chemotherapy. Measurements were made in the morning, using the random zero method (26); the median technical error (one SD from the mean of a set of triplicate measurements) was 0.15mm.
Analytical Methods
Collagen marker assays.
We measured PICP, ICTP. and P3NP in plasma by RIA (Orion Diagnostica, Espoo, Finland), as previously described (25, 27–29). Between-run coefficients of variation were 7.8% and 5.2% at 94 μg/L and 320 μg/L for PICP, 6.3% and 9.2% at 8.7 μg/L and 33.8 μg/L for ICTP, and 5.6% and 6.4% at 4.6 μg/L and 10.4 μg/L for P3NP, respectively.
Bone ALP.
Bone ALP was measured in plasma by wheat germ lectin affinity electrophoresis, as previously described (30). Between-run coefficients of variation were 2.2, 3.5, and 1.9% at 251, 349, and 435 U/L, respectively.
IGF-I.
IGF-I was measured in serum with a specific RIA (Mediagnost, Tübingen, Germany) as described (25, 31). Between-assay coefficients of variation were 8.5, 6.5, and 8.0% at 69, 140, and 118 μg/L, respectively.
IGFBP-3.
IGFBP-3 was measured in serum using a specific RIA as described (25, 32). Between-assay coefficients of variation were 7.3% and 6.9% at 2772 μg/L and 3545 μg/L, respectively.
IGFBP-2.
IGFBP-2 was measured in serum using a specific RIA as described (25, 33). The between-assay coefficient of variation was 10.7%.
Reference Data
All the markers in this study varied with age and sex. We used our own published age- and sex-specific reference data for bone ALP (34), IGF-I, IGFBP-3, and IGFBP-2 (35). For collagen markers in children older than 5 yr, we also used our own published age- and sex-specific reference data (36). To obtain reference data for collagen markers in younger children, we collected surplus plasma remaining after routine clinical biochemistry testing had been completed from 57 children younger than 5 yr, who presented mainly to the casualty and outpatient departments of our institution with various minor conditions that were considered not to have either a short- or long-term effect on growth; children with intercurrent infections were specifically excluded. All collagen markers were log-normally distributed and were therefore log-transformed to fit a Gaussian distribution. There were no differences between males and females for any of the markers in this age group. In general, circulating concentrations of all three collagen markers were higher than in older children (36). Table 1 shows the log-transformed means and SDs compared with our previously published data from older children (36).
Data Analysis
We expressed height as SD scores, using published data for the U.K. (37). Height velocities during cycles 5–8 were also calculated. For the knemometry data, we calculated lower leg length velocity (LLLV) for each treatment cycle by statistical regression of all lower leg length measurements during that cycle against time. Results were expressed in millimeters per week. Because we observed no apparent trends from cycles 5–8, we then calculated the overall mean LLLV during the second year of treatment for each patient. Posttreatment LLLV was calculated similarly.
We expressed all biochemical data as SD scores relative to our reference groups to compensate for variation with age and sex and to facilitate comparisons among markers. The distributions of serum concentrations of collagen markers IGF-I and IGFBPs in healthy children are log-normal (35, 36). We therefore transformed measured concentrations to their logarithms before calculating age- and sex-specific SD scores, based on our own published data (35, 36), and the data reported here for collagen markers in children younger than 5 yr (Table 1). Bone ALP did not require log transformation; SD scores were calculated in relation to our own published data (34). SD scores were calculated as follows:MATH where x was the measured concentration of the analyte.

We calculated the mean analyte SD score for each treatment cycle in each patient. Because there was no consistent trend in any of the markers from cycles 5 to 8 by analysis of variance, we then calculated the overall mean for each analyte in each patient during the second year of treatment. We also calculated the mean SD score for each analyte 2–3 mo after completion of treatment (for those patients in whom these data were available). Group data were expressed as mean and 95% confidence intervals for the mean. Comparison with our normal reference group (with a mean SD score of zero) was by the one-sample t test. Comparisons between unmatched groups were made using unpaired t tests. Comparisons of measurements made in the same patients during and after treatment were by paired t tests. Relationships among variables were explored using the Pearson correlation coefficient, r. All statistical tests were two-tailed;p < 0.05 was regarded as significant.
RESULTS
During treatment.
The median-height SD score at the start of cycle 5 was +0.90 (range –2.8 to +2.1) and changed little throughout the second year of chemotherapy. Median-height velocity during this period was 7.3 cm/yr (range 4.1–9.7 cm/y). There was no overall trend in LLLV from cycles 5 to 8 of treatment. Median LLLV over cycles 5–8 for the eight patients on whom knemometry was performed was 0.48 mm/wk (range 0.34–0.55 mm/wk), similar to that of a group of healthy children studied earlier by us (26).
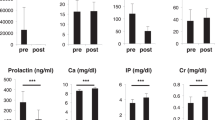
None of the markers showed a consistent trend from cycles 5 to 8 of treatment. Figure 1 shows the mean SD score for each marker over cycles 5–8 for each individual patient. For the group as a whole, mean SD scores (95% confidence intervals) for cycles 5 to 8 were bone ALP, –0.64 (–0.87, –0.40); PICP, +0.36 (–0.26, +0.93); P3NP, +0.93 (+0.06, +1.79); ICTP, +0.21 (–0.26, +0.67); IGF-I, +0.04 (–0.42, +0.50); IGFBP-3, +0.76 (+0.24, +1.28); and IGFBP-2, +1.24 (+0.31, +2.16). Bone ALP was significantly lower than in the reference group (p < 0.0001), whereas P3NP (p < 0.05), IGFBP-3 (p < 0.01), and IGFBP-2 (p = 0.01) were all increased, compared with the reference group. The other markers did not differ significantly from the reference group.
During cycles 5–8 of treatment, none of the markers showed significant correlations with height velocity or LLLV. Significant positive correlations were observed between IGFBP-3 and IGF-I, between IGFBP-3 and ICTP, and between ICTP and P3NP (p < 0.05) but not among other markers.
None of the markers differed significantly between those children who had previously received high-dose methotrexate as CNS-directed treatment and those who had not nor between those children who had previously received a third intensification block of chemotherapy and those who had not.
On 25 occasions in the study, blood samples were collected when the children were neutropenic but afebrile, with a neutrophil count below 1.0 × 109/L. An additional 70 samples were collected when the neutrophil count was above 1.0 × 109/L. Patients remained clinically well during these episodes of neutropenia, but their alanine aminotransferase (ALT) levels were slightly higher (mean 63 U/L; 95% confidence intervals, 12–109 U/L) than when their neutrophil counts were above 1.0 × 109/L (32 U/L; 95% confidence intervals 22–42 U/L, p = 0.05). IGFBP-3 was lower (mean SD score, +0.47; 95% confidence intervals, +0.14, +0.82) during episodes of afebrile neutropenia than when the neutrophil count was above 1.0 × 109/L (mean SD score, +0.95; 95% confidence intervals, +0.72, +1.18, p < 0.05) but was not correlated with ALT. Other markers showed no relationship with neutrophil count.
After treatment.
In the eight patients studied after completion of treatment, mean posttreatment SD scores (95% confidence intervals) were bone ALP, +1.15 (–0.25, +2.55); PICP, +0.22 (–0.60, +1.04); P3NP, +1.51 (+0.68, +2.33); ICTP, +0.49 (–0.68, +1.66); IGF-I, +0.01 (–0.61, +0.62); IGFBP-3, +1.36 (+0.68, +2.03); and IGFBP-2, +0.17 (–1.58, +1.92). After completion of treatment, P3NP and IGFBP-3 were the only markers that remained significantly greater than the reference mean (p < 0.01). IGF-I was correlated positively with IGFBP-3 (r +0.83, p = 0.01), whereas negative correlations developed between IGFBP-2 and both IGF-I (r–0.73) and IGFBP-3 (r −0.72, p < 0.05).
Mean changes in SD scores (95% confidence intervals) from cycle 8 to posttreatment were bone ALP, +1.64 (+0.01, +3.28); PICP, +0.52 (–0.29, +1.33); P3NP, +0.01 (–1.01, +1.02); ICTP, +0.11 (–1.36, +1.58); IGF-I, +0.21 (–0.53, +0.94); IGFBP-3, +0.45 (–0.25, +1.14); and IGFBP-2, –0.60 (–2.23, +1.03). Bone ALP increased after completion of treatment in all patients (p < 0.05, Fig. 2). One 3-year-old boy had a dramatic posttreatment increase in both bone and liver ALP, the latter having the enhanced electrophoretic mobility typical of benign transient hyperphosphatasaemia (38). Overall group changes in the other markers posttreatment did not reach significance. However, individual changes in P3NP after treatment were negatively correlated with the level of P3NP in cycle 8 (r–0.86, p < 0.01) and positively related to individual changes in PICP after treatment (r +0.86, p < 0.01).
For those children in whom height measurements were available 3 mo after completion of treatment, there was a slight but significant increase in height SD score (mean increase +0.16, range 0.0 to +0.3, p < 0.05). For the three patients for whom serial knemometry was available over this period, LLLV increased in all three (from 0.40 to 1.11, 0.67 to 0.83, and 0.49 to 0.93 mm/wk).
DISCUSSION
During treatment.
During the second year of chemotherapy, children with ALL had relatively normal height SD scores, normal height velocities, and normal growth of the lower leg, as previously reported (12, 13). PICP and ICTP levels also indicated normal rates of bone collagen turnover, in agreement with Sorva et al. (39).
We have previously reported that bone ALP, a marker of the mature osteoblast, was low at diagnosis and remained low throughout the first year of chemotherapy (24, 25). This study confirms that bone ALP also remained low throughout the second year of chemotherapy. Because linear growth was relatively normal during this period and PICP, a marker of the osteoblast in its early proliferative phase, was also normal, this suggests that chemotherapy had an adverse effect on osteoblast maturation. The component of chemotherapy most likely to be responsible for this effect was the weekly oral methotrexate. In animal models, methotrexate treatment suppresses osteoblast activity and bone formation, while enhancing osteoclast activity and bone resorption, resulting in reduced bone mass and trabecular bone volume but normal growth (40–42). We have previously demonstrated that high-dose methotrexate administered to children with ALL resulted in lower bone ALP and PICP and increased ICTP, compared with those not so treated (24). It appears that the smaller oral doses administered during continuing chemotherapy may be sufficient to affect osteoblast differentiation (bone ALP) but not its ability to synthesize collagen (PICP) nor the activity of osteoclasts in degrading collagen (ICTP). The consequence is likely to be either ineffective collagen synthesis, in which newly synthesized collagen is degraded without being incorporated into bone matrix, or normal amounts of collagen being laid down in growing bone followed by suboptimal mineralization. Either scenario may be responsible for the fractures and/or reduced BMD observed during chemotherapy (17–19). In our study, samples were taken before each monthly 5-day course of prednisolone, making it unlikely that the suppression of bone ALP was steroid related. We have previously demonstrated that prednisolone treatment resulted in marked suppression of PICP and ICTP but slower and more variable changes in bone ALP (24), a pattern that differs from that seen during continuing chemotherapy.
P3NP tended to be high during chemotherapy. Occult liver fibrosis has been reported as a side effect of methotrexate administration (43) and, in adults treated with methotrexate, increased P3NP has been shown to be associated with liver fibrosis or cirrhosis (44). We have previously shown that P3NP levels were higher in children with ALL and treated with high-dose methotrexate, compared with those not so treated (24). It therefore seems likely those of our patients with higher P3NP levels may have had methotrexate-induced hepatic fibrosis.
During continuing chemotherapy, IGF-I levels were normal but IGFBP-3 levels were slightly increased, mirroring the pattern we observed at the end of the first 6 mo (24) and the first year (25) of chemotherapy. An earlier report found normal levels of IGF-I and IGFBP-3 in children with ALL on maintenance therapy (45). Although circulating IGF-I and IGFBP-3 are both largely determined by GH secretion, the former is more influenced by nutritional factors, which may be of importance in children on chemotherapy. The effects of IGFBP-3 on growth may be both direct and through modulation of the bioavailability of IGF-I to its receptor (22), which may itself be up- or downregulated; in our study, these interacting factors resulted in normal growth.
The high circulating levels of IGFBP-2 that we observed at diagnosis (24) and during the second 6 mo of chemotherapy (24, 25) persisted throughout the second year. There have been previous reports of high pretreatment circulating IGFBP-2 levels in ALL and other malignancies (46–48), probably as a result of production by the tumor itself. However, this seems an unlikely explanation either for its persistence throughout the second year, when all the patients were in remission or for its decrease after stopping treatment, even in a boy (excluded from our study) who relapsed 1 mo later. Instead, IGFBP-2 production or clearance was probably affected directly or indirectly by chemotherapy. IGFBP-2 production appears to be largely independent of GH secretion and is increased in fasting and malnutrition, but its regulators in vivo remain largely unknown (22). Although we did not formally assess nutritional status, weight was normal during this phase of chemotherapy (12). The clinical implications of the high levels of IGFBP-2 are therefore unclear.
We have previously reported that LLLV was lower during episodes of afebrile neutropenia than at other times (13). In the present study, we also observed lower levels of IGFBP-3 during these episodes. The cause of the reduced IGFBP-3 levels in the absence of a reduction in IGF-I is uncertain, because both are largely synthesized in the liver under the control of GH. Although there was evidence of mild hepatocellular damage during some (but not all) episodes of neutropenia, this had no obvious effect on circulating IGFBP-3 levels. The expression of IGFBP-3 in nonhepatic tissues may be influenced by a number of cytokines, growth factors, and hormones, in addition to GH, although the contribution from these nonhepatic sources to circulating IGFBP-3 is probably small (22). Regardless of their etiology, the variations in circulating IGFBP-3 that we observed may have modulated growth either directly or by altering the bioavailability of IGF-I to its receptor.
After treatment.
After chemotherapy was completed, bone ALP increased in all patients. In contrast, the boy excluded from the study because of testicular relapse showed a decrease in bone ALP, consistent with the low levels of bone ALP observed in ALL patients at initial diagnosis (24). Neither absolute levels nor changes in bone ALP posttreatment were related to circulating IGF-I or IGFBPs. The posttreatment increase in bone ALP was therefore likely to be due to removal of the adverse effect of chemotherapy at target tissue level. It coincided with a slight increase in height SD score and an increase in LLLV above that generally observed in normal controls (26).
Although there was little net change in P3NP on a group basis after treatment was stopped, it was striking that those individuals with the highest levels of P3NP in cycle 8 showed a marked decrease after treatment stopped, consistent with the interpretation that the high levels were due to an adverse effect of methotrexate on the liver. Conversely, those with lower levels in cycle 8 showed an increase after stopping treatment, consistent with increased soft tissue turnover associated with increased growth. The posttreatment P3NP reflected the outcome of these two opposing effects. Parallel, but lesser, changes were observed in PICP, consistent with this marker reflecting a combination of bone and, to a lesser extent, soft tissue collagen turnover.
In summary, the second year of continuing chemotherapy in children with ALL was associated with normal growth and normal or high collagen turnover but reduced bone ALP, which suggests impaired osteoblast development and reduced mineralization of bone. After completion of treatment, bone ALP was restored to normal. Although the reduction in bone ALP was reversible, it had been present before treatment was started (24) and throughout the two years of chemotherapy. The consequences for peak bone mass and long-term bone health in these children remains unknown.
Abbreviations
- ALL:
-
acute lymphoblastic leukemia
- BMD:
-
bone mineral density
- PICP:
-
C-terminal propeptide of type I collagen
- ALP:
-
alkaline phosphatase
- ICTP:
-
C-terminal telopeptide of type I collagen
- P3NP:
-
N-terminal propeptide of type III collagen
- IGFBP:
-
IGF binding protein
- LLLV:
-
lower leg length velocity
References
Berglund G, Karlberg J, Marky I, Mellander L 1985 A longitudinal study of growth in children with acute lymphoblastic leukemia. Acta Paediatr 74: 530–533
Möell C, Garwicz S, Marky I, Mellander L, Karlberg J 1988 Growth in children treated for acute lymphoblastic leukemia with and without prophylactic cranial irradiation. Acta Paediatr Scand 77: 688–692
Clayton PE, Shalet SM, Morris-Jones PH, Price DA 1988 Growth in children treated for acute lymphoblastic leukaemia. Lancet I: 460
Marky I, Samuelsson B-O, Mellander L, Karlberg J 1991 Longitudinal growth in children with non-Hodgkin's lymphoma and children with acute lymphoblastic leukemia: comparison between unirradiated and irradiated patients. Med Pediatr Oncol 19: 96–99
Thun-Hohenstein L, Frisch H, Schuster E 1992 Growth after radiotherapy and chemotherapy in children with leukemia or lymphoma. Horm Res 37: 91–95
Tamminga RYJ, Kamps WA, Drayer NM, Humphrey GB 1992 Longitudinal anthropometric study in children with acute lymphoblastic leukaemia. Acta Paediatr 81: 61–65
Hokken-Koelega ACS, Van Doorn JWD, Hählen K, Stijnen T, De Muinck Keizer-Schrama SMPF, Drop SLS 1993 Long-term effects of treatment for acute lymphoblastic leukemia with and without cranial irradiation on growth and puberty: a comparative study. Pediatr Res 33: 577–582
Caruso-Nicoletti M, Mancuso M, Spadaro G, Dibenedetto SP, DiCataldo A, Schiliró G 1993 Growth and growth hormone in children during and after therapy for acute lymphoblastic leukaemia. Eur J Pediatr 152: 730–733
Holm K, Nysom K, Hertz H, Müller J 1994 Normal final height after treatment for acute lymphoblastic leukemia without irradiation. Acta Paediatr 83: 1287–1290
Wallace WHB, Kelnar CJH 1996 The effect of chemotherapy on growth and endocrine function in childhood. In: CJH Kelnar (ed) Baillière's Clinical Paediatrics: Paediatric Endocrinology. Baillière Tindall, London, pp 333–347
Mohnike K, Dörffel W, Timme J, Kluba U, Aumann V, Vorwerk P, Mittler U 1997 Final height and puberty in 40 patients after antileukaemic treatment during childhood. Eur J Paediatr 156: 272–276
Ahmed SF, Wallace WHB, Kelnar CJH 1997 An anthropometric study of children during intensive chemotherapy for acute lymphoblastic leukaemia. Horm Res 48: 178–183
Ahmed SF, Wallace WHB, Crofton PM, Wardhaugh B, Magowan R, Kelnar CJH 1999 Short-term changes in lower leg length in children treated for acute lymphoblastic leukaemia. J Pediatr Endocrinol Metab 12: 75–80
Gilsanz V, Carlson ME, Roe TF, Ortega JA 1990 Osteoporosis after cranial irradiation for acute lymphoblastic leukemia. J Pediatr 117: 238–244
Hoorweg-Nijman JJG, Kardos G, Roos JC, van Dijk HJ, Netelenbos C, Popp-Snijders C, de Ridder CM, Delemarre-van de Waal HA 1999 Bone mineral density and markers of bone turnover in young adult survivors of childhood lymphoblastic leukaemia. Clin Endocrinol 50: 237–244
Warner JT, Evans WD, Webb DK, Bell W, Gregory JW 1999 Relative osteopenia after treatment for acute lymphoblastic leukemia. Pediatr Res 45: 544–551
Atkinson SA, Fraher L, Gundberg CM, Andrew M, Pai M, Barr RD 1989 Mineral homeostasis and bone mass in children treated for acute lymphoblastic leukemia. J Pediatr 114: 793
Halton JM, Atkinson SA, Fraher L, Webber C, Gill GJ, Dawson S, Barr RD 1996 Altered mineral metabolism and bone mass in children during treatment for acute lymphoblastic leukaemia. J Bone Miner Res 11: 1774–1783
Arikoski P, Komulainen J, Riikonen P, Voutilainen R, Knip M, Kröger H 1999 Alterations in bone turnover and impaired development of bone mineral density in newly diagnosed children with cancer: a 1-year prospective study. J Clin Endocrinol Metab 84: 3174–3181
Crofton PM, Kelnar CJH 1998 Bone and collagen markers in paediatric practice. Int J Clin Pract 52: 557–565
Rosen CJ, Donahue LR, Hunter SJ 1994 Insulin-like growth factors and bone: the osteoporosis connection. Proc Soc Exp Biol Med 206: 83–102
Ferry RJ, Cerri RW, Cohen P 1999 Insulin-like growth factor binding proteins: new proteins, new functions. Horm Res 51: 53–67
Kelly KM, Oh Y, Gargosky SE, Gucev Z, Matsumoto T, Hwa V, Ng L, Simpson DM, Rosenfeld RG 1996 Insulin-like growth factor-binding proteins (IGFBPs) and their regulatory dynamics. Int J Biochem Cell Biol 28: 619–637
Crofton PM, Ahmed SF, Wade JC, Stephen R, Elmlinger MW, Ranke MB, Kelnar CJH, Wallace WHB 1998 Effects of intensive chemotherapy on bone and collagen turnover and the growth hormone axis in children with acute lymphoblastic leukaemia. J Clin Endocrinol Metab 83: 3121–3129
Crofton PM, Ahmed SF, Wade JC, Elmlinger MW, Ranke MB, Kelnar CJH, Wallace WHB 1999 Effects of a third intensification block of chemotherapy on bone and collagen turnover, insulin-like growth factor I, its binding proteins and short-term growth in children with acute lymphoblastic leukaemia. Eur J Cancer 35: 960–967
Ahmed SF, Wallace WHB, Kelnar CJH 1995 Knemometry in childhood: a study to compare the precision of two different techniques. Ann Hum Biol 22: 247–252
Melkko J, Niemi S, Risteli L, Risteli J 1990 Radioimmunoassay of the carboxyterminal propeptide of human type I procollagen. Clin Chem 36: 1328–1332
Risteli J, Elomaa I, Niemi S, Novamo A, Risteli L 1993 Radioimmunoassay for the pyridinoline cross-linked carboxy-terminal telopeptide of type I collagen: a new serum marker of bone collagen degradation. Clin Chem 39: 635–640
Risteli J, Niemi S, Trivedi P, Mäentausta O, Mowat AP, Risteli L 1988 Rapid equilibrium radioimmunoassay for the amino-terminal propeptide of human type III procollagen. Clin Chem 34: 715–718
Peaston RT, Cooper J 1986 Affinity electrophoresis of alkaline phosphatase isoenzymes. Clin Chem 32: 235–236
Blum WF, Breier BH Radioimmunoassay for IGFs and IGFBPs 1994 Growth Regul 4 ( Suppl 1): 11–19
Blum WF, Ranke MB, Kietzmann K, Gauggel E, Zeisel JH, Bierich JR 1990 A specific radioimmunoassay for the growth hormone (GH)-dependent somatomedin-binding protein: its use for diagnosis of GH deficiency. J Clin Endocrinol Metab 70: 1292–1297
Elmlinger MW, Wimmer K, Biemer E, Blum WF, Ranke MB, Dannecker GE 1996 Insulin-like growth factor binding protein 2 (IGFBP-2) is differentially expressed in leukaemic T- and B-cell lines. Growth Regul 6: 152–157
Crofton PM 1992 Wheat-germ lectin affinity electrophoresis for alkaline phosphatase isoforms in children: age-dependent reference ranges and changes in liver and bone disease. Clin Chem 38: 663–670
Blum WF 1996 Insulin-like growth factors and their binding proteins. In: MB Ranke (ed) Diagnostics of Endocrine Function in Children and Adolescents. JA Barth, Edition J&J, Heidelberg, pp 190–218
Crofton PM, Wade JC, Taylor MRH, Holland CV 1997 Serum concentrations of the carboxyterminal propeptide of type I procollagen, the aminoterminal propeptide of type III procollagen, the cross-linked carboxyterminal telopeptide of type I collagen and their interrelationships in schoolchildren. Clin Chem 43: 1577–1581
Freeman JV, Cole TJ, Chinn S, Jones PRM, White EM, Preece MA 1995 Cross-sectional stature and weight reference curves for the UK, 1990. Arch Dis Child 73: 17–24
Crofton PM 1988 What is the cause of benign transient hyperphosphataaemia? A study of 35 cases. Clin Chem 34: 335–340
Sorva R, Kivivuori S-M, Turpeinen M, Marttinen E, Risteli J, Risteli L, Sorva A, Siimes MA 1997 Very low rate of type I collagen synthesis and degradation in newly diagnosed children with acute lymphoblastic leukemia. Bone 20: 139–143
May KP, West SG, McDermott MT, Huffer WE 1994 The effect of low-dose methotrexate on bone metabolism and histomorphometry in rats. Arthritis Rheum 37: 201–206
Moëll C, Garwicz S 1995 High-dose methotrexate causes short-term suppression of growth in rabbits. Acta Paediatr 84: 1237–1240
Wheeler DL, Vander Griend RA, Wronski TJ, Miller GJ, Keith EE, Graves JE 1995 The short- and long-term effects of methotrexate on the rat skeleton. Bone 16: 215–221
Nesbit M, Krivit W, Heyn R, Sharp H 1976 Acute and chronic effects of methotrexate on hepatic, pulmonary, and skeletal systems. Cancer 37: 1048–1054
Risteli J, Sogaard H, Oikarinen A, Risteli L, Karvonen J, Zachariae H 1988 Aminoterminal propeptide of type III procollagen in methotrexate-induced liver fibrosis and cirrhosis. Br J Dermatol 119: 321–325
Mohnike KL, Kluba U, Mittler U, Aumann V, Vorwerk P, Blum WF 1996 Serum levels of insulin-like growth factor-I, -II and insulin-like growth factor binding proteins -2 and -3 in children with acute lymphoblastic leukaemia. Eur J Pediatr 155: 81–86
Müller HL, Oh Y, Lehrnbecher T, Blum WF, Rosenfeld RG 1994 Insulin-like growth factor-binding protein-2 concentrations in cerebrospinal fluid and serum of children with malignant solid tumors or acute leukemia. J Clin Endocrinol Metab 79: 428–434
Kanety H, Madjar Y, Levi J, Papa MZ, Pariente C, Goldwasser B, Karsik A 1993 Serum insulin-like growth factor-binding protein-2 (IGFBP-2) level is increased and IGFBP-3 is decreased in patients with prostate cancer: correlation with serum prostate-specific antigen. J Clin Endocrinol Metab 77: 229–233
Lee DY, Kim SJ, Lee YC 1999 Serum insulin-like growth factor (IGF)-I and IGF-binding proteins in lung cancer patients. J Korean Med Sci 14: 401–404
Acknowledgements
The authors thank K. Schmitt for expert technical assistance. We are also grateful to R. Magowan and B. Wardhaugh for their contributions to the anthropometric measurements and for their help in coordinating sample collection. Finally, we would like to thank Dr. P. Shaw for assistance in retrieving data from case notes and Dr. A. Thomas at the Royal Hospital for Sick Children, Edinburgh for allowing her patients to be studied.
Author information
Authors and Affiliations
Additional information
This work was supported by Serono Laboratories (UK), the Child Growth Foundation, and the Jennifer Fund.
Rights and permissions
About this article
Cite this article
Crofton, P., Ahmed, S., Wade, J. et al. Bone Turnover and Growth During and After Continuing Chemotherapy in Children with Acute Lymphoblastic Leukemia. Pediatr Res 48, 490–496 (2000). https://doi.org/10.1203/00006450-200010000-00012
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200010000-00012
This article is cited by
-
The roles of bone remodeling in normal hematopoiesis and age-related hematological malignancies
Bone Research (2023)
-
Bone Turnover Markers in Children: From Laboratory Challenges to Clinical Interpretation
Calcified Tissue International (2022)
-
IGFBP2: integrative hub of developmental and oncogenic signaling network
Oncogene (2020)
-
Physical therapy and chiropractic use among childhood cancer survivors with chronic disease: impact on health-related quality of life
Journal of Cancer Survivorship (2011)