Abstract
The secretion of bile requires the vectorial transport of organic and inorganic solutes from sinusoidal blood to the canalicular lumen. Hydrostatic forces cannot account for biliary secretion, because secretory pressures within bile ducts exceed that of blood within the sinusoidal space. Instead, the process of bile formation requires active transport across the basolateral membrane, transcellular movement through a variety of mechanisms, and then active transport into the canalicular space between hepatocytes. Separate hepatic and ductular transport mechanisms allow for rapid regulation of bile volume and composition required for changing physiologic needs. The array of transport proteins localized to both poles of the hepatocyte have been characterized physiologically and during development. Many have now been cloned and studied further in transgenic models. The recent identification and characterization of several genes that are mutated in inherited forms of cholestatic liver disease have provided new insight into the normal physiology of bile secretion, the pathophysiology of intrahepatic cholestasis, and an unexpected major role for a novel group of P-type ATPases in human biology and disease.
Similar content being viewed by others
Main
The secretion of bile is one of the critical functions of the liver due to its pivotal role as an excretory route for endo- and xenobiotics and in the digestion and absorption of lipids from the intestinal lumen. Important advances have been made in recent years in the understanding of transport processes involved in bile formation as a result of cloning and characterization of several important transport proteins that mediate uptake, intracellular transport, and secretion of organic compounds within the enterohepatic circulation(1). The purpose of this review is to summarize recent advances in our understanding of the molecular mechanisms involved in bile formation and in the pathophysiology of hereditary and acquired cholestatic liver disease.
THE PHYSIOLOGY OF BILE FORMATION
The primary secretory unit of the liver consists of two adjacent hepatocytes which, like other polarized secretory epithelial cells, have two distinct domains: the basolateral (sinusoidal) domain and bile canaliculus defined by the presence of junctional complexes that establish a sealed apical compartment(2). The secretion of bile is the result of the active secretion of osmotically active compounds by hepatocytes into the canalicular space followed by the passive movement of water through the tight junctions(3,4). These osmotically active compounds include organic (bile acids, glutathione, glutathione-conjugated compounds, and glucuronide-conjugated substances) and inorganic anions (bicarbonate and chloride). Many transport systems for these substances have now been identified in both membrane domains of the hepatocytes (Fig. 1). Because bile acids are the major solutes in bile, they are considered the major osmotic driving force in the generation of bile flow. Conventionally, physiologists divide bile flow into bile acid-dependent (i.e. the portion of bile flow generated by the osmotic force of secreted bile acids) and bile acid-independent fractions(the portion of bile flow related to secretion of non-bile acid organic anions and electrolytes). However, this division is artificial because the secretion of bile acids is always present under physiologic conditions. Thus, bile acid-dependent and bile acid-independent fractions of bile flow should be considered interrelated rather than independent components of bile flow(3).
Schematic representation of hepatocyte transporters involved in bile formation. The transport proteins are represented as circles with the arrows showing direction of transport. Ntcp, sodium tauocholate cotransporting polypeptide; oatp1 and 2, organic anion transporting polypeptide 1 and 2; oct1, organic cation transporter 1;SPGP, sister of P-glycoprotein;cBAT, canalicular bile acid transporter; mdr1 and 2, multidrug resistance P-glycoprotein 1 and 2;GSH, glutathione transporter; Mrp2, canalicular multidrug resistance associated protein 2; PFIC1, progressive familial intrahepatic cholestasis gene product; PC, phosphatidylcholine; PE, phosphatidylethanolamine;PS, phosphatidylserine; BS-, bile salts.
Sinusoidal uptake of biliary solutes. Bile flow is the result of vectorial transport of substances from blood to bile. The major cholephilic compounds in sinusoidal blood are bile acids. Their uptake is mediated by Na+-dependent and Na+-independent mechanisms. Three polypeptides have so far been cloned from rat and human liver that are able to confer bile acid transport capacity when expressed in mammalian cells: Ntcp and oatp1 and oatp2(5). In addition to bile acids, oatp1 and oatp2 are able to transport a great variety of other organic anions.
Ntcp is the major bile acid uptake system in the basolateral membrane of rat hepatocytes. It was cloned by Hagenbuch et al.(6) using the Xenopus laevis oocyte expression system. The cloned cDNA sequence predicts a 39-kD polypeptide with five potential sites for glycosylation and seven putative transmembrane spanning domains. Northern blot analysis of Ntcp expression has shown that Ntcp mRNA is exclusively expressed in liver. Experiments using anti-fusion protein antibodies raised against the COOH-terminal of the protein detect a glycosylated ∼50-kD protein on the basolateral membrane of hepatocytes(7,8). Injection of the Ntcp cRNA into X. laevis oocytes or transfection of the cDNA into mammalian cells confers the capacity to carry out saturable Na+-dependent uptake of conjugated and unconjugated bile acids with kinetic parameters similar to those previously defined in liver basolateral plasma membrane vesicles. Antisense experiments have suggested that Ntcp is the predominant and probably the exclusive Na+-dependent transporter for bile acids on the basolateral membrane of the hepatocyte(9). It has also been shown that this transport system is phylogenetically regulated in that it is not present in nonmammalian cells or dedifferentiated cells such as hepatoma cell lines(10). Genomic cloning of the rat Ntcp gene has identified a short DNA sequence of 200 bp as a minimal promoter containing transcription factor binding sites that direct liver-specific expression(11). Finally, the human homologue of rat Ntcp (NTCP) has also been cloned and has similar functional properties, although its affinity for bile acids is higher than that observed for rat Ntcp(12).
The role of Na+-independent systems in the transport of bile acids across the sinusoidal membrane is less clear(5,13). The proteins so far identified in the rat (oatp1 and oatp2) appear to be polyspecific transporters that are able to mediate the uptake of bile acids, particularly unconjugated species, as well as a large number of other compounds differing in charge and structure(14–16). Thus, it is likely that these transport systems play a role in the uptake of xenobiotics by the liver. Oatp1 was cloned using the X. laevis oocyte expression system by Jacquemin et al.(14). Northern and Western blot analysis have shown that this 80-kD molecular mass protein of 670 amino acids is also expressed in tissues other than liver, in particular the kidney and brain. Antisense experiments suggest that it is the predominant sodium-independent uptake mechanism for bile acids in liver but can only partially account for transport of other organic anions as bromosulfophthalein. These data suggest the existence of additional transporters involved in the uptake of organic anions at the sinusoidal pole of the hepatocyte(9). Moreover, although it was initially thought that oatp1 was involved in the uptake of unconjugated bilirubin, the current view is that this polypeptide does not participate in the uptake of this pigment and that other proteins, yet to be cloned, such as bilitranslocase, mediate bilirubin transport into the hepatocyte(1).
Oatp2 is also expressed in liver, brain, and kidney and appears to be important for hepatobiliary and renal excretion of endo- and xenobiotics(17). Oatp2 shares a similar substrate affinity profile with oatp1, with the exception of demonstrating high affinity for digoxin, which may have a role in brain accumulation and neurotoxicity of this cardiovascular drug.
The uptake of cationic compounds at the sinusoidal membrane of rat hepatocytes is thought to be mediated by a recently cloned polyspecific oct1(1). Functional data and the exact role of this transporter, as well as of its human homologue, are still under study.
Finally, the mechanisms underlying the uptake of other biliary solutes are less clear. However, a major advance has been recently made in the elucidation of the uptake mechanism for HDL. The process is important to bile formation because biliary cholesterol originates predominantly from cholesterol present in this lipoprotein. Cloning and characterization of a hepatocyte HDL receptor, the scavenger receptor class A type 1 or SRBI, has shown that this protein may have a critical role in controlling both serum and biliary cholesterol levels(18).
Intracellular transport. The intracellular transport of biliary solutes is not well understood. Most of the available information pertains to the intracellular movement of bile salts(1). These solutes are bound to intracellular binding proteins and undergo rapid monomeric movement to the canalicular pole of the hepatocyte. Teleologically, binding proteins could also serve to prevent the interaction of bile salts with intracellular organelles and subsequent damage due to detergent action of these compounds. Several proteins have been identified as intracellular bile acid binders. In rat liver 3-hydroxysteroid dehydrogenase represents the major cytosolic bile acid binding protein, whereas in humans the predominant protein is a dehydrodiol dehydrogenase(19). The role of vesicular transport in the intracellular movement of biliary solutes is not yet clear. It was previously thought that recruitment of a vesicular transport pathway occurs upon the imposition of a bile acid load to the liver. However, the current view is that a microtubule-dependent vesicular pathway is important in the regulation of canalicular transport capacity of both bile acid and non-bile acid organic anions through the insertion and retrieval of transport proteins in the canalicular membrane similar to that observed in other epithelia(20). Sterol carrier protein 2 and phospholipid transfer protein are involved in the intracellular transport of cholesterol and phospholipids, respectively but the exact details of their action are not well defined(20).
Transport of biliary solutes across the hepatocytes canalicular membrane. Although known to be critical in bile formation, the study of canalicular transport processes has been challenged by the inaccessibility of this space that represents only 13% of the total membrane surface of the hepatocyte. However, with the advent of molecular biological techniques many important advances have been made in the identification of several transport proteins participating in the coordinated secretion of solutes into bile(Fig. 1)(1). In the last decade, research in cancer biology has led to the identification of the multidrug resistance (MDR in human and mdr in rodents) genes which encode proteins that are able to export chemotherapeutic agents out of neoplastic cells(21,22). It soon became apparent that these genes were part of the superfamily of physiologically important transporters, ABC transporters, which function as ATP-dependent export pumps and have a common ATP-binding motif in their protein sequences(23,24). Detection of these proteins in the bile canaliculus raised questions about their role in this location. Subsequent investigations have elucidated the critical role of ABC transporters in the biliary secretion of endo- and xenobiotics(21,22).
Bile acid transport. The secretion of monovalent bile acids into the canaliculus is the rate-limiting step in the overall transport of bile acids from blood to bile. Because this secretory process takes place against a high osmotic and chemical gradient (∼5 µM inside the cell versus 1000 µM in the canalicular space), an active transport system is required(25,26). Although the transmembrane electrical potential was thought to drive bile acid excretion, it has been established recently that an ATP-driven export pump is largely responsible for the canalicular transport of taurocholate and other monovalent bile salts(13,27–29). The exact contribution of the potential driven bile acid transport remains controversial because one study has shown that this system is restricted to the endoplasmic reticulum(30). Several attempts to identify the protein(s) that mediate this secretory event have been made. Purification of a 100-kD protein from rat liver canalicular membrane, later identified as Ecto-ATPase, which conferred bile acid transport capacity when transfected to heterologous cells suggested this protein as a potential candidate for the so-called cBAT(31). However, several investigations have shown that Ecto-ATPase and bile acid transport activities are two different entities so that the role of Ecto-ATPase in bile acid transport in vivo remains to be established. On the other hand, based on functional studies and the structural properties of other export pumps in the liver (like the cMOAT, see below) it is likely that cBAT belongs to the family of ABC transporters(32). In fact, recent preliminary evidence has shown that a canalicular ABC transporter, the SPGP, can effectively mediate ATP-dependent bile acid transport when overexpressed in the insect Sf9 cell line(33). Interestingly, very recent data using positional cloning suggest that mutations in SPGP may play a role in human liver disease (see section "Pediatric Implications"), supporting the concept that is the predominant canalicular bile acid transporter.
Transport of non-bile acid-organic anions. Several functional studies have identified a second ATP-dependent transport system in the canalicular membrane that is responsible for the transport of non-bile acid organic anions as well as sulfated and glucoronidated bile acids(34–36). Several naturally occurring mutant strains of rats have been identified that lack the capacity to excrete several organic anions and conjugated bilirubin(37,38). These animals have the phenotype of mild chronic conjugated hyperbilirubinemia and decreased bile flow secondary to a reduced secretion of glutathione and glutahione conjugates(38). This canalicular multiple organic anion transporter of cMOAT was later identified as an ABC transporter belonging to the family of MRPs(38). A point mutation in the liver isoform of this gene(MRP2) resulting in an stop codon and lack of protein expression was defined in these mutant rats confirming the role of this protein in the excretion of non-bile acid organic anions from the hepatocyte(39). The existence of additional transport proteins sharing substrate affinity with cMRP/cMOAT as well as the role of these proteins in biliary secretion of glutathione conjugates remains to be determined(40). Although a canalicular potential-dependent transport system for glutathione conjugates has been described, its molecular identity is currently unclear(41).
Transport of biliary lipids. Biliary lipid secretion serves an important physiologic role in cholesterol homeostasis because it is the major excretory pathway for this sterol(42,43). In addition, biliary phospholipids play a role on the intestinal absorption of dietary lipids. Moreover, a cytoprotective role of biliary lipids against bile acid-induced injury to hepatocytes and biliary cells has been suggested. The development of mutant mice with a targeted inactivation (knockout) of another ABC transporter mdr2 led to the identification of this protein as a phospholipid translocator(44,45). Mdr2-/- animals do not have detectable phosphatidylcholine in bile and have significant liver pathology characterized by a nonsuppurative destructive cholangitis similar to that seen in some human cholestatic diseases(46). Extensive studies using these mutant animals have shown that secretion of lipids into bile is a result of a coordinate interplay between secretion of bile salts, phosphatidylcholine translocation from the inner to the outer hemileaflet of the hepatocyte canalicular membrane, and detergent extraction by luminal bile salts(47,48). In this theoretical model, cholesterol would diffuse passively from the canalicular membrane into biliary vesicles. Cholesterol transport proteins have not been identified.
Transport of cationic compounds. Our knowledge of canalicular transport of cationic compounds is less complete than for organic anions. The rat mdr1a/mdr1b gene products, also members of the ABC family of transporters, are located on the canalicular membrane and have been suggested to act as transporters of cationic compounds and steroids(21). However, no endogenous substrates have yet been identified for these proteins. Moreover, mdr1a knockout mice do not have significant pathology or changes in biliary composition(21,49). Double knockout mice (mdr1a/mdr1b-/-) also maintain normal bile flow, but have a marked reduction in biliary cation excretion(49,50). Thus, it is likely that these transporters could be important for excretion of xenobiotics and endogenous metabolites.
Hepatobiliary transport of copper, which accumulates in the liver during cholestatic liver disease, is still poorly understood. An ATP-dependent transport system has been described in rat and human liver canalicular membranes, but have not been cloned(51). However, this transport system does not correspond to the recently cloned Wilson's disease gene, designated Atp7b, which codes for a copper transporting ATPase located in the trans-Golgi network(51a). Thus, it is possible that intracellular accumulation of copper leads to impaired expression or function of the copper export pump and a reduced biliary excretion of this metal.
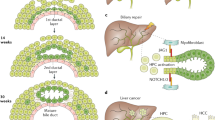
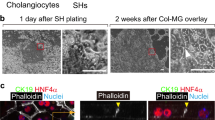
Modifications to bile composition in the biliary tree. Although biliary epithelial cells account for only 3-5% of the overall population of liver cells, they may contribute as much as 40% of the daily production of bile depending on the species by adding fluid and electrolytes to canalicular bile(52). Moreover, the organic and inorganic components of bile may be significantly modified by an array of absorptive mechanisms on the apical membrane of cholangiocytes. There is little information on the functional properties of cholangiocytes during development, but we have recently learned much about the biology of cholangiocytes from normal adult rodent and human livers.
Bile secretion and biliary secretion of bicarbonate are markedly stimulated by the hormone secretin(53,54). Conversely, bile flow and biliary bicarbonate output are decreased by the hormone somatostatin. Both secretin and somatostatin regulate ductal bile flow by interacting with receptors on the basolateral surface of cholangiocytes and effect intracellular levels of cAMP(55). Exocytosis is also stimulated by a cAMP-mediated mechanism. The increase in intracellular cAMP then activates a low conductance chloride channel, probably identical to the cystic fibrosis transmembrane conductance regulator and possibly other cAMP-activated chloride channels(56). As chloride exits the cell, the cholangiocyte depolarizes and facilitates bicarbonate entry through the action of an electrogenic sodium-bicarbonate cotransporter. The rise in bicarbonate concentration stimulates the activity of an apical chloride/bicarbonate exchanger, in which luminal chloride is exchanged for intracellular bicarbonate resulting in the secretion of bicarbonate into bile. In the liver the cystic fibrosis transmembrane conductance regulator has been localized to the apical surface of cholangiocytes but is not expressed in hepatocytes, thus explaining the biliary tract disease which develops in patients with cystic fibrosis(56).
The mechanisms underlying ductal water movement have not been defined completely. Cholangiocytes express the membrane water channel aquaporin at the apical and/or basolateral domains and at least in the rat, it has been demonstrated that cholangiocytes transport water transcellularly via a channel-mediated mechanism(57).
There also seems to be some heterogeneity in the functional properties of cholangiocytes. For example, large but not small intrahepatic bile ducts are involved in secretin-regulated bile ductal secretion(58,59). Correlating directly with physiologic studies, the secretin receptor and chloride/bicarbonate exchanger mRNAs have been detected in large, but not small, intrahepatic bile duct units.
DEVELOPMENTAL ASPECTS OF BILE FORMATION
Functional studies in humans and animals have documented immature biliary excretory function in early life(60). Bile flow and biliary bile acid concentrations are low during fetal and neonatal development, as a result of immature bile acid biosynthetic pathways and transport systems. In addition, hepatocellular transport of several organic anions such as bromosulfophthalein and indocyanine green is delayed in developing compared with mature animals(60). The factors that control the development of the enterohepatic circulation of bile acids are not fully understood. Attempts to dissect the different steps of bile formation during development have been made using plasma membrane vesicles that allow the separate study of the basolateral and canalicular transport processes(60). These studies have shown that sinusoidal uptake of bile acids by the hepatocyte is significantly reduced in the rat during the first month of life and that canalicular ATP-dependent transport of bile acids is also immature at birth (M. Ananthanarayanan and F. J. Suchy, unpublished observations)(61–63). The molecular basis of these developmental processes are being elucidated. Detailed studies on developmental expression of Ntcp have shown that Ntcp mRNA is absent throughout much of rat gestation and first detected at d 20 of fetal life reaching adult levels at d 7 after birth(64). Transcription of the Ntcp gene, as assessed by nuclear run-on studies, is relatively low up to d 21 of gestation with an abrupt increase at d 1 and reaching adult levels by 1 wk of life. Preliminary studies have correlated this pattern of developmental expression with binding activities of critical transcription factors, such as hepatocyte nuclear factor 1, to the Ntcp promoter suggesting that this transcription factor might play an important role in driving the expression of this transporter. In addition, Ntcp protein is detected shortly after birth in a partially glycosylated form that persists up to 4 wk of age(64). Thus, transcriptional and posttranscriptional mechanisms seem to be involved in the developmental regulation of Ntcp expression. mRNAs of other transport proteins participating in hepatobiliary transport including oatp1, cMOAT, and SPGP are also expressed in a developmental stage-specific manner, although available information in this regard is limited(63). Of note, oatp1 and cMOAT are expressed before Ntcp and SPGP, suggesting that bile acid-independent bile flow matures before bile acid-dependent mechanisms. Finally, the ileal bile acid transporter undergoes an biphasic developmental regulation with prenatal onset of expression, repression in the early postnatal period and marked reinduction at weaning(65).
EFFECTS OF HEPATOCELLULAR AND OBSTRUCTIVE CHOLESTASIS ON EXPRESSION AND FUNCTION OF HEPATOCYTE TRANSPORTERS
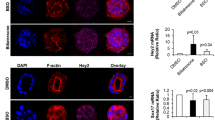
Because uptake and secretion of bile acids and other organic anions are markedly impaired during cholestasis, the expression of several hepatocyte transporters has been investigated in several different forms of experimental cholestasis. Bile duct ligation (obstructive cholestasis) and ethynylestradiol or endotoxin administration (hepatocellular cholestasis) are the most commonly used models. Expression and function of Ntcp is down-regulated in all three forms of cholestasis(66,67). Decreased transcription rates of the Ntcp gene have been observed in obstructive cholestasis and decreased binding activity of a critical nuclear transcription factor, HNF1, required for basal Ntcp gene expression occurs upon the injection of endotoxin(67,68). NTCP mRNA levels are also markedly decreased in infants with biliary atresia and subsequently increase if biliary drainage is restored by portoenterostomy(69).
cMRP/cMOAT expression is down-regulated in both extra-hepatic and hepatocellular cholestasis, whereas the function of the canalicular bile acid transporter is impaired after ethynylestradiol or endotoxin administration(70,71). In contrast, studies assessing the expression of Mdr1b P-glycoprotein have shown that this protein is up-regulated in obstructive cholestasis(71). Without a detailed picture of the mechanisms involved, it is difficult to dissect which of the described changes is potentially pathogenic or merely secondary to cholestatic injury. A speculative but attractive hypothesis is that decreased activity of canalicular transporters for bile acids and organic anions leads to accumulation of bile acids and other potentially toxic substances inside the hepatocyte, which in turn represses transcription of other transporter genes. Thus, decreased expression of Ntcp could represent a protective mechanism to prevent further uptake of bile acids. Several lines of evidence suggest that Ntcp transcription could be under a negative feedback control analogous to that observed for the gene of the key enzyme in bile acid synthesis cholesterol 7 α-hydroxylase (CYP7) giving support to this hypothetical mechanism(11,72). On the other hand, increased expression of P-glycoproteins could represent a secondary response in an attempt to eliminate potentially toxic substances into bile. Owing to their detergent nature, retention of bile acids inside the cell also leads to damage of intracellular membranes, to mitochondrial dysfunction, and ultimately to hepatocyte death. Thus, bile acid retention and bile acid-induced hepatotoxicity are important pathophysiologic mechanisms in cholestatic liver disease.
IMPLICATIONS FOR PEDIATRIC LIVER DISEASE
The molecular basis of several forms of cholestatic liver disease has recently been defined (Table 1). PFIC represents a clinically important group of cholestatic disorders of infancy that often progresses to cirrhosis(73,74). Byler disease or progressive familial cholestasis (PFIC 1) is a rare autosomal recessive disorder in which cholestasis with onset in infancy leads to progressive hepatic fibrosis and death. A locus for PFIC has been mapped to a 19-cM region of chromosome 18 by a search for shared segments, using patients from the Amish kindred in which the disorder was originally described(75,76). Another inherited liver disease, benign recurrent intrahepatic cholestasis, also has been mapped to the same region, suggesting that these two diseases are caused by mutations in the same gene(76). Even though biliary excretion of chenodeoxycholic acid is impaired in Byler disease, no hepatocyte transporters have been mapped to this location(75). It has recently been reported that both benign recurrent intrahepatic cholestasis and PFIC1 are caused by mutations in a single gene, which has been termed FIC1 (for familial intrahepatic cholestasis 1)(77). The FIC1 gene is the first human member of a new subfamily of P-type ATPases which are involved in ATP-dependent aminophospholipid transport. FIC1 is expressed in many epithelial tissues including liver, intestine, pancreas, and kidney. The function of FIC1 is not yet known but could involve regulation of bile acid transport or maintenance of the lipid composition of the canalicular membrane. Other members of this subfamily of P-type ATPases are thought to function in the transport of aminophospholipids from the outer to the inner leaflet of cell membranes.
Among the hereditary forms of human cholestasis, a subtype of progressive familial intrahepatic cholestasis exists in which patients have high serumγ-glutamyltranspeptidase levels. The disorder shares histologic, biochemical, and genetic features with mice lacking the mdr2 gene (mdr2-/- mice), which encodes a phosphatidylcholine flippase(44,45). MDR3 (human mdr2 homolog) mRNA was absent by Northern blotting in the liver of a patient suffering from this form of PFIC, and the biliary phospholipid level in a second patient was substantially decreased(78). In subsequent studies immunohistochemistry revealed the absence of canalicular staining for MDR3 in liver tissue from affected patients. Genomic DNA analysis has demonstrated several mutations in the MDR3 gene that result in stop codons and truncated proteins lacking at least one ABC cassette(79). Thus, the absence of the MDR3 P-glycoprotein is responsible for this type of PFIC, which, as in the murine model, may be due to toxic injury by bile acids to the biliary epithelium because of the lack of biliary phospholipids(46).
A third locus for PFIC has been identified on chromosome 2q24(80). Patients with this variant of PFIC harbor a mutation in the sister of P-glycoprotein gene (R. J. Thompson, personal communication, November 1997), the putative ATP-dependent canalicular bile acid transporter which maps to this locus(33). This is consistent with the phenotype of decreased canalicular excretion of bile salts described in these patients. It is likely that impaired bile acid secretion causes accumulation of bile acids inside the hepatocyte and ongoing hepacellular damage.
Dubin-Johnson syndrome is a rare autosomal recessive liver disorder characterized by chronic conjugated hyperbilirubinemia and a typical dark pigment accumulation in liver parenchymal cells. Patients also have impaired hepatobiliary transport of non-bile salt organic anions and amphiphilic anionic conjugates from hepatocytes into the bile. Selective absence of the canalicular isoform of MRP (MRP2) has been demonstrated in hepatocytes from patients with Dubin-Johnson syndrome by double-label immunofluorescence microscopy(81). Moreover, sequence analysis of MRP2 cDNA from a patient with Dubin Johnson syndrome revealed a mutation leading to premature termination of MRP2 protein synthesis(82).
In conclusion, major advances in understanding of molecular mechanism of bile formation have been made in the last decade by applying techniques of cellular and molecular biology. The impact of this research in pediatric liver disease is becoming apparent and eventually will contribute to the design of more effective forms of therapy.
Abbreviations
- Ntcp:
-
sodium taurocholate cotransporting polypeptide
- oatp:
-
organic anion transporting polypeptide
- ABC:
-
ATP-binding cassette
- SPGP:
-
sister of P-glycoprotein
- cMOAT:
-
canalicular multispecific anion transporter
- MRP:
-
multidrug resistance P-glycoprotein
- PFIC:
-
progressive familial intrahepatic cholestasis
- FIC1:
-
familial intrahepatic cholestasis 1
- cBAT:
-
canalicular bile acid transporter
References
Muller M, Jansen PL 1997 Molecular aspects of hepatobiliary transport. Am J Physiol 272:G1285–G303
Meier PJ 1988 Transport polarity of hepatocytes. Semin Liver Dis 8: 293–307
Nathanson MH, Boyer JL 1991 Mechanisms and regulation of bile secretion. Hepatology 14: 551–566
Boyer JL, Graf J, Meier PJ 1992 Hepatic transport systems regulating pHi, cell volume, and bile secretion. Annu Rev Physiol 54: 415–438
Hagenbuch B, Meier PJ 1996 Sinusoidal (basolateral) bile salt uptake systems of hepatocytes. Semin Liver Dis 16: 129–136
Hagenbuch B, Stieger B, Foguet M, Lubbert H, Meier PJ 1991 Functional expression cloning and characterization of the hepatocyte Na+/bile acid cotransport system. Proc Natl Acad Sci USA 88: 10629–10633
Ananthanarayanan M, Ng OC, Boyer JL, Suchy FJ 1994 Characterization of cloned rat liver Na(+)-bile acid cotransporter using peptide and fusion protein antibodies. Am J Physiol 267:G637–G643
Stieger B, Hagenbuch B, Landmann L, Hochli M, Schroeder A, Meier PJ 1994 In situ localization of the hepatocytic Na+/taurocholate cotransporting polypeptide in rat liver. Gastroenterology 107: 1781–1787
Hagenbuch B, Scharschmidt BF, Meier PJ 1996 Effect of antisense oligonucleotides on the expression of hepatocellular bile acid and organic anion uptake systems in Xenopus laevis oocytes. Biochem J 316: 901–904
Boyer JL, Hagenbuch B, Ananthanarayanan M, Suchy F, Stieger B, Meier PJ 1993 Phylogenic and ontogenic expression of hepatocellular bile acid transport. Proc Natl Acad Sci USA 90: 435–438
Karpen SJ, Sun AQ, Kudish B, Hagenbuch B, Meier PJ, Ananthanarayanan M, Suchy FJ 1996 Multiple factors regulate the rat liver basolateral sodium-dependent bile acid cotransporter gene promoter. J Biol Chem 271: 15211–15221
Hagenbuch B, Meier PJ 1994 Molecular cloning, chromosomal localization, and functional characterization of a human liver Na+/bile acid cotransporter. J Clin Invest 93: 1326–13231
Meier PJ 1995 Molecular mechanisms of hepatic bile salt transport from sinusoidal blood into bile. Am J Physiol 269:G801–G812
Jacquemin E, Hagenbuch B, Stieger B, Wolkoff AW, Meier PJ 1994 Expression cloning of a rat liver Na(+)-independent organic anion transporter. Proc Natl Acad Sci USA 91: 133–137
Kanai N, Lu R, Bao Y, Wolkoff AW, Schuster VL 1996 Transient expression of oatp organic anion transporter in mammalian cells: identification of candidate substrates. Am J Physiol 270:F319–F325
Satlin LM, Amin V, Wolkoff AW 1997 Organic anion transporting polypeptide mediates organic anion/HCO3- exchange. J Biol Chem 272: 26340–26345
Noe B, Hagenbuch B, Stieger B, Meier PJ 1997 Isolation of a multispecific organic anion and cardiac glycoside transporter from rat brain. Proc Natl Acad Sci USA 94: 10346–10350
Rigotti ATB, Babitt J, Penman M, Xu S, Krieger M 1997 Scavenger receptor BI: a cell surface receptor for high density lipoprotein. Curr Opin Lipidol 8: 181–188
Stolz A, Hammond L, Lou H 1995 Rat and human bile acid binders are members of the monomeric reductase gene family. Adv Exp Med Biol 372: 269–280
Crawford J 1996 Role of vesicle-mediated transport pathways in hepatocellular bile secretion. Semin Liver Dis 16: 169–189
Silverman J, Schrenk D 1997 Hepatic canalicular membrane. 4. Expression of the multidrug resistance genes in the liver. FASEB J 11: 308–313
Keppler D, Leier I, Jedlitschky G, Mayer R, Buchler M 1996 The function of the multidrug resistance proteins (MRP and cMRP) in drug conjugate transport and hepatobiliary excretion. Adv Enzyme Regul 36: 17–29
Lomri N, Fitz JG, Scharschmidt BF 1996 Hepatocellular transport: role of ATP-binding cassette proteins. Semin Liver Dis 16: 201–210
Gatmaitan ZC, Nies AT, Arias IM 1997 Regulation and translocation of ATP-dependent apical membrane proteins in rat liver. Am J Physiol 272:G1041–G1049
Suchy FJ 1993 Hepatocellular transport of bile acids. Semin Liver Dis 13: 235–247
Suchy FJ, Sippel CJ, Ananthanarayanan M 1997 Bile acid transport across the hepatocyte canalicular membrane. FASEB J 11: 199–205
Wolters H, Kuipers F, Slooff MJ, Vonk RJ 1992 Adenosine triphosphate-dependent taurocholate transport in human liver plasma membranes. J Clin Invest 90: 2321–2326
Stieger B, O'Neill B, Meier PJ 1992 ATP-dependent bile-salt transport in canalicular rat liver plasma-membrane vesicles. Biochem J 284: 67–74
Meier PJ, Stieger B 1993 Canalicular membrane adenosine triphosphate-dependent transport systems. Prog Liver Dis 11: 27–44
Kast C, Stieger B, Winterhalter KH, Meier PJ 1994 Hepatocellular transport of bile acids. Evidence for distinct subcellular localizations of electrogenic and ATP-dependent taurocholate transport in rat hepatocytes. J Biol Chem 269: 5179–5186
Sippel CJ, McCollum MJ, Perlmutter DH 1994 Bile acid transport by the rat liver canalicular bile acid transport/ecto-ATPase protein is dependent on ATP but not on its own ecto-ATPase activity. J Biol Chem 269: 2820–2826
Luther TT, Hammerman P, Rahmaoui CM, Lee PP, Sela-Herman S, Matula GS, Ananthanarayanan M, Suchy FJ, Cavalieri RR, Lomri N, Scharschmidt BF 1997 Evidence for an ATP-dependent bile acid transport protein other than the canalicular liver ecto-ATPase in rats. Gastroenterology 113: 249–254
Gerloff T, Stieger B, Hagenbuch B, Landmann L, Meier PJ 1997 The sister-P-glycoprotein of rat liver mediates ATP-dependent taurocholate transport. Hepatology 26: 358A( abstr)
Keppler D, Konig J 1997 Hepatic canalicular membrane. 5. Expression and localization of the conjugate export pump encoded by the MRP2 (cMRP/cMOAT) gene in liver. FASEB J 11: 509–516
Keppler D, Konig J, Buchler M 1997 The canalicular multidrug resistance protein, cMRP/MRP2, a novel conjugate export pump expressed in the apical membrane of hepatocytes. Adv Enzyme Regul 37: 321–333
Madon J, Eckhardt U, Gerloff G, Stieger B, Meier PJ 1997 Functional expression of the rat canalicular isoform of the multidrug resistance-associated protein. FEBS Lett 406: 75–78
Ito K, Suzuki H, Hirohashi T, Kume K, Shimizu T, Sugiyama Y 1997 Molecular cloning of canalicular multispecific organic anion transporter defective in EHBR. Am J Physiol 272:G16–G22
Paulusma CC, Oude Elferink RP 1997 The canalicular multispecific organic anion transporter and conjugated hyperbilirubinemia in rat and man. J Mol Med 75: 420–428
Paulusma CC, Bosma PJ, Zaman GJ, Bakker CT, Otter M, Scheffer GL, Scheper RJ, Borst P, Oude Elferink RP 1996 Congenital jaundice in rats with a mutation in a multidrug resistance-associated protein gene. Science 271: 1126–1128
Keppler D, Leier I, Jedlitschky G 1997 Transport of glutathione conjugates and glucuronides by the multidrug resistance proteins MRP1 and MRP2. J Biol Chem 378: 787–791
Ballatori N, Truong AT 1995 Multiple canalicular transport mechanisms for glutathione S-conjugates. Transport on both ATP- and voltage-dependent carriers. J Biol Chem 270: 3594–3601
Verkade HJ, Vonk RJ, Kuipers F 1995 New insights into the mechanism of bile acid-induced biliary lipid secretion. Hepatology 21: 1174–1189
Cohen DE 1996 Hepatocellular transport and secretion of biliary phospholipids. Semin Liver Dis 16: 191–200
Smith AJ, Timmermans Hereijgers JL, Roelofsen B, Wirtz KW, van Blitterswijk WJ, Smit JJ, Schinkel AH, Borst P 1994 The human MDR3 P-glycoprotein promotes translocation of phosphatidylcholine through the plasma membrane of fibroblasts from transgenic mice. FEBS Lett 354: 263–266
Elferink RP, Tytgat GN, Groen AK 1997 The role of mdr2 P-glycoprotein in hepatobiliary lipid transport. FASEB J 11: 19–28
Mauad TH, van Nieuwkerk CM, Dingemans KP, Smit JJ, Schinkel AH, van den Notenboom RG, Bergh Weerman MA, Verkruisen RP, Groen AK, Oude Elferink RP, van der Valk MA, Borst P, Offerbans GJA 1994 Mice with homozygous disruption of the mdr2 P-glycoprotein gene. A novel animal model for studies of nonsuppurative inflammatory cholangitis and hepatocarcinogenesis. Am J Pathol 145: 1237–1245
Ruetz S, Gros P 1994 Phosphatidylcholine translocase: a physiological role for the mdr2 gene. Cell 77: 1071–1081
van Helvoort A, Smith AJ, Sprong H, Fritzsche I, Schinkel AH, Borst P, van Meer G 1996 MDR1 P-glycoprotein is a lipid translocase of broad specificity, while MDR3 P-glycoprotein specifically translocates phosphatidylcholine. Cell 87: 507–517
Schinkel AH, Mol CA, Wagenaar E, van Deemter L, Smit JJ, Borst P 1995 Multidrug resistance and the role of P-glycoprotein knockout mice. Eur J Cancer 31A: 1295–1298
Schinkel AH, Mayer U, Wagenaar E, Mol CA, van Deemter L, Smit JJ, van der Valk MA, Voordouw AC, Spits H, van Tellingen O, Zijlmans JM, Fibbe WE, Borst P 1997 Normal viability and altered pharmacokinetics in mice lacking mdr1-type (drug-transporting) P-glycoproteins. Proc Natl Acad Sci USA 94: 4028–4033
Dijkstra M, Vonk RJ, Kuipers F 1996 How does copper get into bile? New insights into the mechanism(s) of hepatobiliary copper transport. J Hepatol 24( suppl 1): 109–120
Nagano K, Nakamura K, Urakami KI, Umeyama K, Uchiyama H, Koiwai K, Hattori S, Yamamoto T, Matsuda I, Endo F 1998 Intracellular distribution of the Wilson's disease gene product (ATPase7B) after in vitro and in vivo exogenous expression in hepatocytes from the LEC rat, an animal model of Wilson's disease. Hepatology 27: 799–807
Roberts SK, Ludwig J, Larusso NF 1997 The pathobiology of biliary epithelia. Gastroenterology 112: 269–279
Marinelli RA, Larusso NF 1996 Solute and water transport pathways in cholangiocytes. Semin Liver Dis 16: 221–229
Strazzabosco M, Joplin R, Zsembery A, Wallace L, Spirli C, Fabris L, Granato A, Rossanese A, Poci C, Neuberger JM, Okolicsanyi L, Crepaldi G 1997 Na(+)-dependent and -independent Cl-/HCO-3 exchange mediate cellular HCO3- transport in cultured human intrahepatic bile duct cells. Hepatology 25: 976–985
Strazzabosco M 1997 New insights in cholangiocyte physiology. J Hepatol 27: 945–952
Cohn JA, Strong TV, Picciotto MR, Nairn AC, Collins FS, Fitz JG 1993 Localization of the cystic fibrosis transmembrane conductance regulator in human bile duct epithelial cells. Gastroenterology 105: 1857–1864
Roberts SK, Yano M, Ueno Y, Pham L, Alpini G, Agre P, LaRusso NF 1994 Cholangiocytes express the aquaporin CHIP and transport water via a channel-mediated mechanism. Proc Natl Acad Sci USA 91: 13009–13013
Alpini G, Ulrich C, Roberts S, Phillips JO, Ueno Y, Podila PV, Colegio O, LeSage GD, Miller LJ, LaRusso NF 1997 Molecular and functional heterogeneity of cholangiocytes from rat liver after bile duct ligation. Am J Physiol 272:G289–G297
Alpini G, Glaser S, Robertson W, Rodgers RE, Phinizy JL, Lasater J, LeSage GD 1997 Large but not small intrahepatic bile ducts are involved in secretin-regulated ductal bile secretion. Am J Physiol 272:G1064–G1074
Suchy FJ 1994 Bile formation: mechanisms and development. In: Suchy FJ (ed) Pediatric Liver Disease. JB Lippincott, Philadelphia, pp 57–80
Suchy FJ, Bucuvalas JC, Goodrich AL, Moyer MS, Blitzer BL 1986 Taurocholate transport and Na+-K+-ATPase activity in fetal and neonatal rat liver plasma membrane vesicles. Am J Physiol 251:G665–G673
Novak DA, Sippel CJ, Ananthanarayanan M, Suchy FJ 1991 Postnatal expression of the canalicular bile acid transport system of rat liver. Am J Physiol 260:G743–G751
Weymann A, Ananthanarayanan M, Arrese M, Childs S, Ling V, Keppler D, Suchy FJ 1997 Differential development expression of canalicular ABC transporters cMOAT/cMRP2 and sister P glycoprotein. Hepatology 26: 651( abstr)
Hardikar W, Ananthanarayanan M, Suchy FJ 1995 Differential ontogenic regulation of basolateral and canalicular bile acid transport proteins in rat liver. J Biol Chem 270: 20841–20846
Shneider BL, Dawson PA, Christie DM, Hardikar W, Wong MH, Suchy FJ 1995 Cloning and molecular characterization of the ontogeny of a rat ileal sodium-dependent bile acid transporter. J Clin Invest 95: 745–754
Green RM, Beier D, Gollan JL 1996 Regulation of hepatocyte bile salt transporters by endotoxin and inflammatory cytokines in rodents. Gastroenterology 111: 193–198
Gartung C, Ananthanarayanan M, Rahman MA, Schuele S, Nundy S, Soroka CJ, Stolz A, Suchy FJ, Boyer JL 1996 Down-regulation of expression and function of the rat liver Na+/bile acid cotransporter in extrahepatic cholestasis. Gastroenterology 110: 199–209
Trauner M, Arrese M, Lee H, Boyer JL, Karpen SJ 1997 Endotoxin-induced down-regulation of the rat liver gene is mediated by decreased binding activity of hepatocyte nuclear factor 1 (HNF1). Hepatology 26: 535
Shneider BL, Fox VL, Schwarz KB, Watson CL, Ananthanarayanan M, Thevananther S, Christie DM, Hardikar W, Setchell KDR, Mieli-Vergani G, Suchy FJ, Mowat AP 1997 Hepatic basolateral sodium-dependent-bile acid transporter expression in two unusual cases of hypercholanemia and in extrahepatic biliary atresia. Hepatology 25: 1176–1183
Adachi Y, Miya H, Okuyama Y, Kamisako T, Yamamoto T 1996 Hepatocyte canalicular transport of organic anions in bile duct-ligated rats. Int Hepatol Commun 6: 326–330
Trauner M, Arrese M, Soroka CJ, Ananthanarayanan M, Koeppel TA, Schlosser SF, Suchy FJ, Boyer JL 1997 The rat canalicular conjugate export pump (Mrp2) is down-regulated in intrahepatic and extrahepatic cholestasis. Gastroenterology 113: 255–264
Stravitz RT, Hylemon PB, Heuman DM, Hagey LR, Schteingart CD, Ton Nu HT, Hofmann AF Vlahcevic ZR 1993 Transcriptional regulation of cholesterol 7 α-hydroxylase mRNA by conjugated bile acids in primary cultures of rat hepatocytes. J Biol Chem 268: 13987–13993
Riely CA 1987 Familial intrahepatic cholestatic syndromes. Semin Liver Dis 7: 119–133
Bull LN, Carlton VE, Stricker NL, Baharloo S, DeYoung JA, Freimer NB, Magid MS, Kahn E, Markowitz J, DiCarlo FJ, McLoughlin L, Boyle JT, Dahms BB, Faught PR, Fitzgerald JF, Piccoli DA, Witzleben CL, O'Connel 1997 Genetic and morphological findings in progressive familial intrahepatic cholestasis (Byler disease [PFIC-1] and Byler syndrome): evidence for heterogeneity. Hepatology 26: 155–164
Carlton VE, Knisely AS, Freimer NB 1995 Mapping of a locus for progressive familial intrahepatic cholestasis (Byler disease) to 18q21-q22, the benign recurrent intrahepatic cholestasis region. Hum Mol Genet 4: 1049–1053
Van Berge Henegouwen GP 1996 Benign recurrent intrahepatic cholestasis and Byler's disease: one gene, two diseases?[editorial]. J Hepatol 25: 395–397
Bull LN, van Eijk MJT, Pawlikowska L, DeYoung JA, Juijn JA, Liao M, Klomp LWJ, Lomri M, Berger R, Scharschmidt BF, Knisely AS, Houwen RHJ, Freimer NB 1998 A gene encoding a P-type ATPase mutated in two forms of hereditary cholestasis. Nat Genet 18: 219–224
Deleuze JF, Jacquemin E, Dubuisson C, Cresteil D, Dumont M, Erlinger S, Bernard O, Hadchouel M 1996 Defect of multidrug-resistance 3 gene expression in a subtype of progressive familial intrahepatic cholestasis. Hepatology 23: 904–908
Jacquemin E, de Vree JML, Strum E, Cresteil D, Bosma PJ, Aten J, Deleuze JF, Desrochers M, Burdelski M, Bernard O, Hadchouel M, Oude Elferink RPJ 1997 Mutations in the MDR3 gene are responsible for a subtype of progressive familial intrahepatic cholestasis. Hepatology 26: 248A( abstr)
Strautnieks SS, Kagalwalla AF, Tanner MS, Gardiner RM, Thompson RJ 1996 Locus heterogeneity in progressive familial intrahepatic cholestasis. J Med Genet 33: 833–836
Kartenbeck J, Leuschner U, Mayer R, Keppler D 1996 Absence of the canalicular isoform of the MRP gene-encoded conjugate export pump from the hepatocytes in Dubin-Johnson syndrome. Hepatology 23: 1061–1066
Paulusma CC, Kool M, Bosma PJ, Scheffer GL, ter Borg F, Scheper RJ, Tytgat GN, Borst P, Baas F, Oude Elferink RP 1997 A mutation in the human canalicular multispecific organic anion transporter gene causes the Dubin-Johnson syndrome. Hepatology 25: 1539–1542
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Arrese, M., Ananthananarayanan, M. & Suchy, F. Hepatobiliary Transport: Molecular Mechanisms of Development and Cholestasis. Pediatr Res 44, 141–147 (1998). https://doi.org/10.1203/00006450-199808000-00001
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199808000-00001
This article is cited by
-
Non invasive in vivo investigation of hepatobiliary structure and function in STII medaka (Oryzias latipes): methodology and applications
Comparative Hepatology (2008)
-
Hepatobiliary function assessed by 99mTc-mebrofenin cholescintigraphy in the evaluation of severity of steatosis in a rat model
European Journal of Nuclear Medicine and Molecular Imaging (2006)
-
The bile salt export pump: molecular properties, function and regulation
Pfl�gers Archiv - European Journal of Physiology (2004)
-
Role of S-adenosylmethionine on the hepatobiliary homeostasis of glutathione during cyclosporine A treatment
Journal of Physiology and Biochemistry (2000)