Abstract
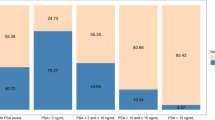
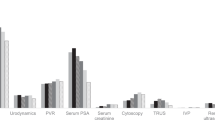
One purported advantage of electronic medical records (EMRs) is to improve patient care. This study uses a search of EMR to identify patients at risk for prostate cancer who were not evaluated by an urologist. The University of Texas Southwestern Medical Center (UTSW) has an institutional outpatient EMR that is used by all providers in all specialties. Since March 2009, all PSA tests were reported with specific interpretative comments including a recommendation for referral to urology for a PSA >2.5 ng ml−1. All PSA tests were performed on campus since institution of these recommendations were analyzed, and charts reviewed for all patients not seen in urology with a serum PSA >2.5 ng ml−1. Of the 2884 non-urology patients that had a serum PSA drawn between March 2009 and February 2010 at UTSW, 293 patients had a serum PSA >2.5 ng ml−1. Of these, 39 patients had known prostate cancer and were seeing an oncologist. There were 59 patients seeing urologists outside the institution. A total of 195 patients were not seen by an urologist and only 11 patients were recommended to see one but did not make an appointment. There were 151 patients with more than one PSA in the system, and of these 103 had a rise in PSA with a median rise of 0.53 ng ml−1 per year. EMR allows identification of patients at increased risk of prostate cancer who are not evaluated. Prospective studies are needed to identify ways to improve appropriate evaluation and detection of prostate cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
National Cancer Institute. Surveillance, Epidemiology, and End Results registry. Available from: http://seer.cancer.gov/.
Hankey BF, Feuer EJ, Clegg LX, Hayes RB, Legler JM, Prorok PC et al. Cancer surveillance series: Interpreting trends in prostate cancer—Part I: evidence of the effects of screening in recent prostate cancer incidence, mortality, and survival rates. J Natl Cancer Inst 1999; 91: 1017–1024.
Feuer EJ, Etzioni R, Cronin KA, Mariotto A . The use of modeling to understand the impact of screening on US mortality: examples from mammography and PSA testing. Stat Methods Med Res 2004; 13: 421.
Etzioni R, Gulati R, Falcon S, Penson DF . Impact of PSA screening on the incidence of advanced stage prostate cancer in the United States: a surveillance modeling approach. Med Decis Making 2008; 28: 323.
Schroder FH, Hugosson J, Roobol MJ, Tammela TL, Ciatto S, Nelen V et al. Screening and prostate-cancer mortality in a randomized European study. N Engl J Med 2009; 360: 11320–11328.
Greene KL, Albertsen PC, Babaian RJ, Carter HB, Gann PH, Han M et al. Prostate-specific antigen best practice statement: 2009 update. J Urol 2009; 182: 2232–2241.
Swan J, Breen N, Coates RJ, Rimer BK, Lee NC . Progress in cancer screening practices in the United States: results from the 2000 National Health Interview Survey. Cancer 2003; 97: 1528–1540.
Sirovich BE, Schwartz LM, Woloshin S . Screening men for prostate and colorectal cancer in the United States: does practice reflect the evidence? JAMA 2003; 289: 1414–1420.
Woolf SH . Screening for prostate cancer with prostate-specific antigen: an examination of the evidence. N Engl J Med 1995; 333: 1401.
Andriole GL, Crawford ED, Grubb III RL, Buys SS, Chia D, Church TR et al. Mortality results from a randomized prostate cancer screening trial. N Engl J Med 2009; 360: 1310–1319.
Draisma G, Boer R, Otto SJ, van der Cruijsen IW, Damhuis RA, Schröder FH et al. Lead times and overdetection due to prostate-specific antigen screening: estimates from the European Randomized Study of Screening for Prostate Cancer. J Natl Cancer Inst 2003; 95: 868.
Thompson IM, Pauler DK, Goodman PJ, Tangen CM, Lucia MS, Parnes HL et al. Prevalence of prostate cancer among men with a prostate-specific antigen level ⩽4.0 ng per milliliter. N Engl J Med 2004; 350: 2239–2246.
Albertsen PC, Hanley JA, Gleason DF, Barry MJ . Competing risk analysis of men aged 55–4 years at diagnosis managed conservatively for clinically localized prostate cancer. JAMA 1998; 280: 975–980.
Barry MJ, Albertsen PC, Bagshaw MA, Blute ML, Cox R, Middleton RG et al. Outcomes for men with clinically nonmetastatic prostate carcinoma managed with radical prostatectomy, external beam radiotherapy, or expectant management. Cancer 2001; 91: 2302–2314.
Richardson TD, Oesterling JE . Age-specific reference ranges for serum prostate-specific antigen. Urol Clin North Am 1997; 24: 339.
Reed A, Ankerst DP, Pollock BH, Thompson IM, Parekh DJ . Current age and race adjusted prostate specific antigen threshold values delay diagnosis of high grade prostate cancer. J Urol 2007; 178: 1929.
University of Texas Health Science Center, San Antonio. Risk of biopsy-detectable prostate cancer. http://deb.uthscsa.edu/URORiskCalc/Pages/uroriskcalc.jsp. Accessed May 14, 2010.
Nam RK, Toi A, Klotz LH, Trachtenberg J, Jewett MA, Appu S et al. Assessing individual risk for prostate cancer. J Clin Oncol 2007; 25: 3582.
Thompson IM, Ankerst DP, Chi C, Goodman PJ, Tangen CM, Lucia MS et al. Assessing prostate cancer risk: results from the Prostate Cancer Prevention Trial. J Natl Cancer Inst 2006; 98: 529.
Schroder F, Kattan MW . The comparability of models for predicting the risk of a positive prostate biopsy with prostate-specific antigen alone: a systematic review. Eur Urol 2008; 54: 274.
Carter HB, Pearson JD . PSA velocity for the diagnosis of early prostate cancer. A new concept. Urol Clin North Am 1993; 20: 665–670.
Hartzband P, Groopman J . Off the record—avoiding the pitfalls of going electronic. N Engl J Med 2008; 358: 1656–1658.
Guerra CD, Jacobs SE, Holmes J, Shea JA . Are physicians discussing prostate cancer screening with their patients and why or why not? A pilot study. J Gen Intern Med 2007; 22: 901–907.
Linder SK, Hawley ST, Cooper CP, Scholl LE, Jibaja-Weiss M, Volk RJ . Primary care physicians’ reported use of pre-screening discussions for prostate cancer screening: a cross-sectional survey. BMC Fam Pract 2009; 10: 19.
McFall SL, Smith DW . Lack of follow-up of prostate-specific antigen test results. Public Health Rep 2009; 124: 718–725.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Erickstad, L., Reed, G., Bhat, D. et al. Use of electronic medical records to identify patients at risk for prostate cancer in an academic institution. Prostate Cancer Prostatic Dis 14, 85–89 (2011). https://doi.org/10.1038/pcan.2010.50
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2010.50